Abstract
Keywords
Introduction
Pediatric epistaxis is a common condition with three out of four children experiencing epistaxis at some time in the first two decades of life. 1 Hospital series report a mean age of presentation between 7.25 and 9.1 years.2-6 These figures may not accurately represent the prevalence and distribution of epistaxis in the outpatient clinical setting. Most children with epistaxis never seek medical care as bleeding usually stops spontaneously or with pressure applied to the nasal alae. 7 Still, nasal bleeding is often frightening to parents and caregivers. The formation of clots in the nose may lead inexperienced observers to overestimate the quantity of blood lost. Concern for more serious conditions (e.g., leukemia, tumors, brain hemorrhage) often leads to outpatient visits to pediatricians, hematologists, or otolaryngologists.8,9
The reported incidence of epistaxis varies widely. There are few studies examining epistaxis incidence in children of different ages and fewer still focusing on the office setting. This study aims to determine the incidence of pediatric epistaxis by age in the outpatient setting using a large, representative national sample.
Methods
We performed a cross-sectional analysis using data from the National Hospital Ambulatory Medical Care Survey (NHAMCS) from the years 2007 to 2011. The NHAMCS is a survey study distributed by the Centers for Disease Control and Prevention to 500 nationally representative hospitals and collects information on hospital outpatient visits. 10 These data are collected and submitted voluntarily by the medical providers. The years 2007 to 2011 were chosen as the outpatient publicly available datasets from the NHAMCS were available for these years with consistent variables in the data files that allowed for the merging of data between years. 11 As the NHAMCS is a de-identified, publicly available data set, institutional review board approval was not required under the rules of Temple University’s Human Research Protection Program. The NHAMCS reports basic demographics (age, sex, ethnicity, insurance, region, etc.), reason for visit, date of the visit, associated diagnostic and procedural codes, setting (primary care provider, subspecialty, etc.), and patient comorbidities. Inclusion criteria for our study include patients <18 years of age and only those presenting with a new complaint. Children presenting with recurrent epistaxis and those presenting for a follow-up visit were thus excluded from our study. The International Classification of Diseases Ninth Revision diagnostic code for epistaxis (784.7) was used to identify patients with epistaxis. 12 Only patients with a primary diagnosis code of epistaxis for their new patient visit were included. The incidence rate per person-years was calculated as well as the cumulative incidence of pediatric epistaxis per person over 3-year intervals. Children were divided into 3-year interval age groups (0-2, 3-5, 6-8, 9-11, 12-14, and 15-17). These intervals were consistent with the groupings used in the American Academy of Otolaryngology -Head and Neck Surgery clinical practice guideline for epistaxis. 7 The decision to calculate cumulative incidence in addition to incidence rate per person-years was made to compensate for low values of incidence per year. When examining rates across different seasons, seasons were defined by the following calendar months: winter (January, February, and March), spring (April, May, and June), summer (July, August, September), and fall (October, November, and December); this was similarly characterized by a study by Shay et al. 6 Geographic areas (Northeast, Midwest, South, and West) described by the NHAMCS were defined based on criteria used by the U.S. Census Bureau. 13 A two-proportion z-test was used to compare cumulative incidence rates between age groups. The chi-square test was used to compare categorical variables with the occurrence of epistaxis in a univariate fashion. All statistical analyses were performed using MedCalc® Statistical Software version 20.109 (MedCalc Software Ltd, Ostend, Belgium) and SPSS v28.0.1.1 (Chicago, Illinois, USA). A P-value <0.05 was considered significant.
Results
A total of 55,435,691 patients [mean age 6.93 ± 5.5 years; 52,779,969 (77.2%) white, 27,816,237 (50.2%) male] were included in this study. In all, 135,281 of these patients presented to the clinic as new patients for epistaxis for a cumulative incidence of 2.44 cases of epistaxis per 1000 patients over the span of 4 years. When examining cumulative incidence of epistaxis by age groups, children of the ages 3 to 5 had the highest incidence at 5.0 cases per 1000 patients, followed by children of ages 6 to 8 (3.0 cases per 1000 patients), 9 to 11 (2.0 cases per 1000 patients), 0 to 2 (1.9 cases per 1000 patients), 12 to 14 (1.6 cases per 1000 patients), and 15 to 17 (0.5 cases per 1000 patients) (P < .001) (Figure 1).
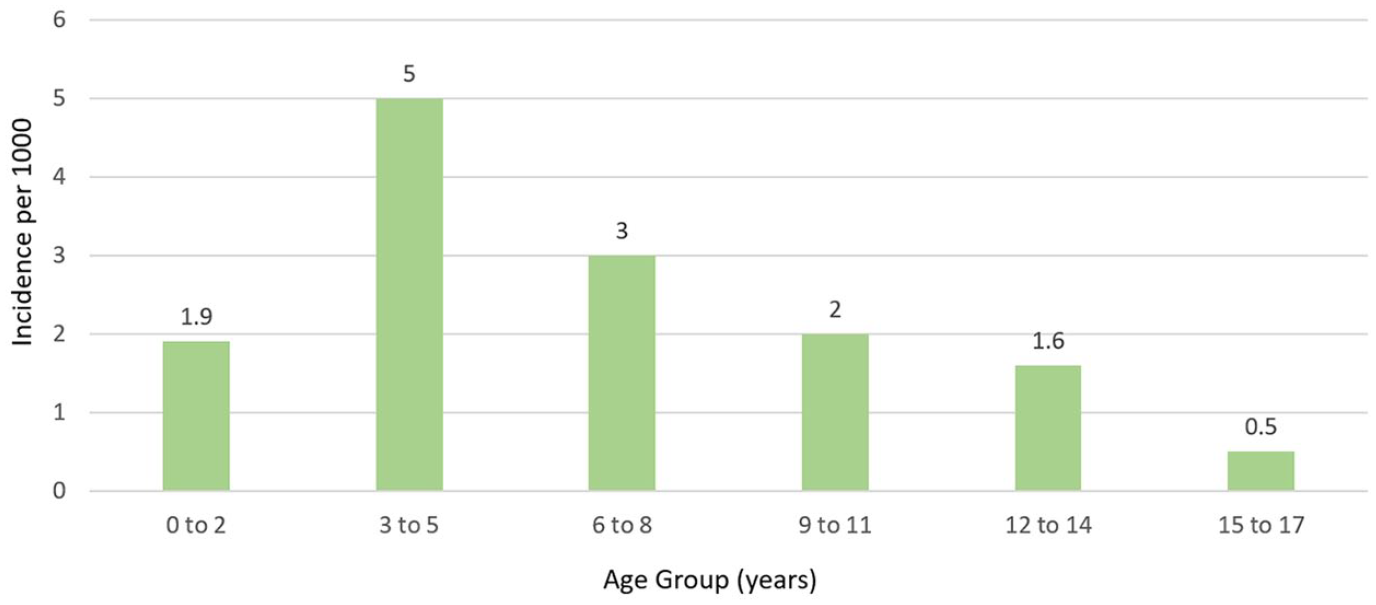
Incidence of epistaxis per age group.
Of the 135,481 children who experienced epistaxis, 87,093 (64.3%) were white and 99,477 (73.4%) were males (Table 1). The majority presented to a general medicine/pediatric clinic (92.9%), whereas 9588 (7.1%) of patients presented to a surgery clinic. In addition, 7319 (5.4%) had comorbid rhinitis, 892 (0.7%) had von Willebrand disease, and 6246 (4.6%) had a history of facial trauma.
Overview of Included Patients With Epistaxis.

The occurrence of epistaxis was examined over each calendar year included in the study, with 2007, 2008, 2010, and 2011 having an incidence of 2 per 1000 epistaxis; during the year 2009, there was a 4 per 1000 rate of epistaxis (P < .001).
The rates of epistaxis were examined across different seasons. Of the 135,481 patients who experienced epistaxis, 31.2% presented during the summer season, followed by 27.0% in the spring, 22.4% in the fall, and 19.4% in the winter (P < .001).
There were slight geographic differences in rates of epistaxis, with both the South and West having an incidence of 3 per 1000 cases of epistaxis, whereas the Midwest and Northeast had an incidence of 2 per 1000 cases of epistaxis (P < .001).
Discussion
Epistaxis is common in children. 6 Most episodes are spontaneous and self-limited in nature. There have been several studies examining the demographics of children presenting to the emergency department or inpatient setting for pediatric epistaxis. Little is known, however, about the epidemiology of pediatric epistaxis in the outpatient setting.6,8 Our analysis of pediatric epistaxis used a nationally representative database with a large sample size (55,435,691, weighted). This contrasts with several existing studies that included mixed pediatric and adult populations. 14 Existing studies that did focus on pediatric patients are limited to single-cohort groups or regional databases (New York, Florida, Iowa, and California).4,6,15 Our study demonstrated a higher cumulative incidence than that found in previous studies conducted in the emergency department setting (1.7 epistaxis cases per 1000 patients in the emergency department). 14 The reasons for a higher incidence of epistaxis in the outpatient setting are unknown. We speculate that children seen in the outpatient setting may have less severe presentations—not necessitating an urgent visit to an emergency department with associated costs and inconvenience.
We aimed to determine the incidence and age distribution of epistaxis in outpatient pediatric patients. A prior massive database study examining emergency department visits found a bimodal distribution in epistaxis with an early age peak (age <10 years) and then a gradual increase in frequency from age 20 years onward to the elderly. 14 In our outpatient analysis, pediatric epistaxis was most common in children ages 3-5, with an incidence rate of 5 cases per 1000 children of the age group. The average age of children presenting with epistaxis in our study was 5.95 years. This is slightly younger than the mean reported in emergency department studies. Shay et al. 6 reported a mean age of children presenting with epistaxis to be 7.54 years, while Davies et al. reported a mean age of 8.8 years. 4 The cumulative incidence rates in these studies do not break down epistaxis by age. Petruson in 1979 examined the incidence of epistaxis by age group in adults and children using a mix of outpatients, emergency department patients, and inpatients. 15 He reported an increasing incidence of epistaxis by age (0.5/1000 age 0-5 years, 1.6/1000 age 6-10 years, and 1.8/1000 age 11-15 years).
It was our clinical impression that school-aged children presented to our outpatient practice much more often than infants or those in their late teens. Analysis of the NHAMCS database confirms this impression with a peak incidence of epistaxis in children 3-5 years of age and much less common presentations at the upper and lower extremes of the first two decades. Commonly quoted causes of epistaxis include digital trauma and nasal inflammation (recent URIs, allergic rhinitis). While upper respiratory infections are very common in the preschool age group, there is no firm evidence that nose-picking occurs with greater frequency in these children. 16 These variations in epistaxis rates (2.5-fold for infants and 10-fold for ages 15-17) are large enough to trigger suspicion of alternative causes for nasal bleeding for very young children and in those in their late teens with new onset epistaxis. Abuse, 17 foreign body, 18 coagulopathy, or a functional platelet disorder 19 should be borne in mind for infants presenting with epistaxis. Similarly, trauma, 17 coagulopathy, 19 hereditary hemorrhagic telangiectasia, 20 intranasal drug abuse, 21 and nasal tumors22,23 (especially juvenile angiofibroma in teenage boys) 24 should be considered for first presentations or recurrent or severe epistaxis in older teens. Further investigations of the causes of epistaxis in different age groups are certainly needed.
Previous work has demonstrated associations of season,25,26 humidity, and temperature27-29 with rates of epistaxis. Our study demonstrated higher rates of epistaxis during the summer and spring seasons, similar to an analysis of ED visits for pediatric epistaxis by Shay et al. This differs from previous studies that showed epistaxis having the highest incidence in winter months.3,4,30 It has been theorized that the mechanism behind spontaneous pediatric epistaxis may differ from that of the adult population, as most of the studies finding a correlation between the warmer seasons and epistaxis have focused on a pediatric population.6,25,26,28
Interestingly, some studies have seen rates of epistaxis increase with increasing temperature27,29 and others have seen an inverse correlation.31,32 Wei et al. demonstrated moderate temperature zones were associated with lower odds of epistaxis, theorizing that temperature extremes may lead to nasal mucosal dysfunction, increasing the rates of epistaxis. 25
Regarding humidity, Wei et al. also found an inverse association between humidity and epistaxis, with higher rates of epistaxis in dry climate zones for only temperature zones that were moderate, but not in extreme temperature zones. 25 These authors note that temperature may have a greater impact on epistaxis than humidity. By contrast, several other studies have found no correlation between humidity and rates of epistaxis.28,29
Limitations
There are limitations to our study that should be considered during the interpretations of the results. First, our study was retrospective and examined from the time period 2007-2011. These dates were chosen as the diagnostic code for “epistaxis” was included in the NHAMCS database during those years. 10 More recent data might provide different results. Second, using the NHAMCS database, we are unable to evaluate whether patients had visited multiple different practitioners in the same hospital system, potentially falsely elevating our incidence rates. In addition, our study used a database that collected data via patient surveys. As such it depended on the recollections of patients and caregivers rather than collecting contemporaneous information. This may have affected the quality of data included in the database. Finally, this was a survey of hospital-affiliated outpatient practices. A survey of independent practitioners might have yielded different results.
Conclusions
The incidence of epistaxis is highest in children ages 3-5, followed by children ages 6-8, 9-11, 0-2, 12-14, and 15-17. When epistaxis occurs in infants or the late teens, alternative less common causes for nasal bleeding should be considered.
Footnotes
Acknowledgements
None.
Meeting Information
Poster presentation at TRIO Combined Sections Meeting January 25-27, 2023.
Data availability Statement
The NHAMCS is a de-identified, publicly available data set.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Statement
As the NHAMCS is a de-identified, publicly available data set, institutional review board approval was not required under the rules of Temple University’s Human Research Protection Program.
Informed Consent
As the NHAMCS is a de-identified, publicly available data set, informed consent did not need to be obtained.
Trial Registration Number
N/A.
Grant Number
N/A.
Level of Evidence
N/A—National database study.
