Abstract
Background:
Foreign body aspiration into the trachea is a common occurrence in children. While most foreign bodies in the airways can be removed using rigid tracheoscopy, there are instances where tracheostomy or tracheotomy is needed. This article presents a series of cases in which tracheostomy was necessary to remove foreign bodies, and summarizes the relevant experiences and lessons learned.
Methods:
We reviewed a total of 7 cases in which tracheostomy and rigid tracheoscopy were combined for foreign body removal out of a larger cohort of 1559 cases at Shenzhen Children’s Hospital in Guangdong, China over a 20-year period.
Results:
The combined use of tracheostomy and rigid tracheoscopy resulted in successful removal of foreign bodies in all 7 patients reviewed in this study. Six patients developed complications of tracheotomy, mainly including mediastinal emphysema (5/7), subcutaneous emphysema (3/7), and pneumothorax (1/7). Tracheotomy was temporary in all patients.
Conclusion:
In cases where a foreign body in the trachea is too large or has irregular, sharp edges, is embedded in submucosal tissues with edema, cannot be passed smoothly through the vocal cords, or local endoscopic facilities are inadequate, a tracheotomy may be necessary. However, this approach should be used with caution, and close collaboration with anesthesiologists and careful management of intraoperative emergencies are crucial for improving the success rate of the procedure. Additionally, the complications should be noted, paying particular attention to early complications such as pneumothorax, pneumomediastinum, and bleeding.
Introduction
Bronchial foreign bodies are a potentially life-threatening emergency in otolaryngology, with a higher incidence in rural areas and in males aged 1 to 3 years.1 -3 Previous studies have suggested an age of onset between 2 and 4 years, extending to less than 5 years.1,4 Organic foreign bodies, especially nuts and seeds, are the most common types encountered. Rigid tracheoscopy is the preferred diagnostic and therapeutic modality for foreign bodies in the trachea, with successful removal via the vocal canal in most cases. 5 However, in rare instances, a combined approach of tracheostomy and rigid tracheoscopy may be necessary to ensure optimal patient outcomes. Through this series of cases, we demonstrate the effectiveness and utility of combining bronchoscopy with tracheotomy in specific circumstances. Our findings elucidated the indications and potential complications of this approach.
Case Presentation
Case 1
A 3.5-year-old female child was admitted to the hospital with a complaint of hoarseness that had developed within 4 hours after eating. There were no associated symptoms of fever, cough, or dyspnea. Auscultation revealed coarse and symmetrical breath sounds in both lungs, along with audible laryngeal sounds. X-ray results were negative for any obvious signs of a foreign body. With parental consent, the child was taken to the operating room where a subglottic foreign body was visualized under the laryngoscope. Attempts to remove the foreign body with forceps failed due to the excessive size of the foreign body, and it became lodged under the glottis, resulting in decreased blood oxygen saturation. An emergency tracheotomy was performed, and some fragments of the foreign body were removed through the tracheotomy port. The remaining part of the foreign body was too large to be removed through the tracheotomy port, and it was extracted forcefully from under the glottis. There was significant edema in the glottis following removal, and a tracheal cannula was secured. The foreign body was identified as a hard, sharp, and irregular fruit shell measuring 1.3 cm × 0.8 cm × 0.8 cm. Subcutaneous and mediastinal emphysema developed 2 days after the operation, but it resolved by day 12 when the tracheotomy tube was smoothly removed.
Case 2
A male child, aged 1 year and 2 months, presented with sudden onset of laryngeal wheezing, cyanosis, and choking after accidental inhalation of a foreign body. Upon examination, inspiratory stridor was observed, along with symmetrical respiratory sounds in both lungs. Chest X-ray did not reveal any positive findings. Direct laryngoscopy during the operation revealed a subglottic foreign body, which could not be removed by foreign body forceps and caused a small amount of bleeding in the subglottic area. In view of the potential for airway mucosal injury and vocal cord damage, tracheostomy was recommended by the most qualified doctors. The foreign body was then successfully removed from the tracheotomy with the assistance of a bronchoscope, as it had dislodged into the right main bronchus. The foreign body was identified as a polygonal irregular fish skull measuring approximately 0.5 cm × 0.4 cm × 0.9 cm. The tracheotomy was sutured during the operation. Subcutaneous emphysema, mediastinal emphysema, and a small pneumothorax were observed on chest X-ray on the same day as the operation, and a tracheotomy tube was inserted. The emphysema and pneumothorax resolved after 2 weeks, and the cannula was subsequently removed.
Case 3
A 2.5-year-old male was admitted to the hospital due to a half-day history of paroxysmal asthma and coughing with grade I dyspnea, without any prior history of cough or hoarseness. Auscultation revealed low respiratory sounds in the right lung and laryngeal sounds. However, chest X-ray showed no sign of a foreign body. Following consent from the family members, exploratory surgery was conducted under general anesthesia, which revealed a subglottic incomplete white foreign body and highly edematous glottic tissue. There was a high amount of resistance in removing the foreign body and attempts to remove the foreign body using forceps resulted in cyanosis, leading to asphyxia. To address this, the patient underwent endotracheal intubation and tracheotomy. The foreign body, which was an irregular bone fragment measuring 1.0 cm × 0.5 cm × 0.02 cm, was successfully removed from the mouth of the tracheotomy. A tracheal cannula was inserted and fixed, and on the same day after the operation, cervical subcutaneous emphysema and mediastinal emphysema were observed. The emphysema subsided 11 days after the operation, and the tracheotomy tube was successfully removed.
Case 4
A 5-year-old male was admitted to the hospital after accidentally swallowing a plastic whistle, which led to laryngeal discomfort and non-projectile vomiting. The patient exhibited symptoms of silent hissing and coughing and produced whistling sounds during inhalation and exhalation. The patient had no shortness of breath or dyspnea while in a quiet state. The breath sounds in both lungs were coarse and symmetrical. Under general anesthesia, laryngoscope exploration revealed the presence of a subglottic foreign body, which could not be removed despite multiple attempts with foreign body forceps. Therefore, a tracheotomy was performed, and the foreign body was successfully removed from the tracheotomy. The foreign body was identified as a cylindrical, hollow plastic whistle with a diameter of 1 cm and a metal sleeve. Following the operation, the patient experienced hoarseness and subcutaneous emphysema of the neck, which resolved 4 days later. The cannula was removed 1 week after the operation, and the patient fully recovered.
Case 5
An 11-month-old male child was admitted to the hospital after accidentally inhaling a fish bone a month prior. The patient developed cough and slight cyanosis immediately after eating the fish, which subsided after approximately 20 minutes. The patient experienced persistent hoarseness, throat wheezing, and intermittent cough, but no fever was present. Auscultation revealed symmetrical respiratory sounds in both lungs without obvious wheezing and dry‒wet rales. A computed tomography (CT) scan performed at another hospital showed high-density striations in the trachea. Under general anesthesia, subglottic bone-like foreign bodies were visualized under a laryngoscope with the anterior and posterior ends embedded in the mucosa. Attempts to remove the foreign bodies using forceps failed, and subglottic edema was observed. Consequently, a tracheotomy was performed to remove the foreign bodies from the glottis. Mucosal damage and granulation were observed on the anterior and posterior walls of the trachea. The anterior wall of the esophagus was significantly congested, but no perforation was detected. A postoperative chest radiograph showed a small amount of mediastinal emphysema. A 4.5-mm tracheal cannula was placed, which was later replaced with a 3.5-mm tracheal cannula when the tube failed to block. Extubation was successful 1 week after the operation.
Case 6
A 3-year-old male patient was admitted to the hospital due to a suspected foreign body inhalation and presented with cough and stridor for 3 hours. Initially, there was a choking cough and reddening of the face. After about 2 minutes, the symptoms eased, accompanied by intermittent coughing and stridor. The examination revealed weaker breath sounds in the right lung with wet rales in both lungs and no trismus sign. Chest CT confirmed foreign body obstruction in the right bronchus. Despite multiple attempts to remove the foreign body under bronchoscopic guidance, the cylindrical plastic pen cap could not be extracted from the vocal cords, resulting in subglottic swelling. Subsequently, a tracheotomy procedure was carried out to address the situation. The foreign body, measuring 1.5 cm in length and 0.8 cm in diameter, was successfully extracted through the tracheotomy port. A 4.5-mm tracheal tube was inserted, and a postoperative chest radiograph revealed a small amount of mediastinal pneumoperitoneum. Successful tube blocking was achieved 12 days after the surgery.
Case 7
The patient, a 9-year-old male, was admitted to the hospital after accidentally aspirating a ballpoint pen cap 5 hours prior. The patient experienced violent coughing, which subsided after a few minutes but was accompanied by pallor, dyspnea, paroxysmal cough, hoarseness, and stridor. An external emergency CT examination revealed a foreign body in the right main bronchus (Figure 1). Physical examination indicated weak breath sounds in the right lung with audible wet rales. The patient underwent rigid bronchoscopy under general anesthesia, during which the pen cap was found to be near the tracheal ridge at the proximal end of the right main bronchus (Figure 2). Alligator forceps were introduced under rigid bronchoscopy to clamp the edge of the pen cap, but the foreign body could not be extracted through the vocal canal due to significant swelling of the vocal canal and subglottic mucosa (Figure 3). Repeated attempts to extract the foreign body using different clamping methods and a supporting laryngeal aid were unsuccessful, leading to the decision to perform a tracheotomy. The foreign body was then successfully removed through the tracheostomy. The pen cap was 1.6 cm long and 1 cm in diameter (Figures 4 and 5). A tracheal tube was inserted, and postoperative examination revealed no dyspnea, subcutaneous emphysema in the neck or chest, or significant asymmetry in the lung breath sounds. The tracheal tube was successfully removed 10 days after the operation. Two weeks after removing the tube, the wound was healed (Figure 6).
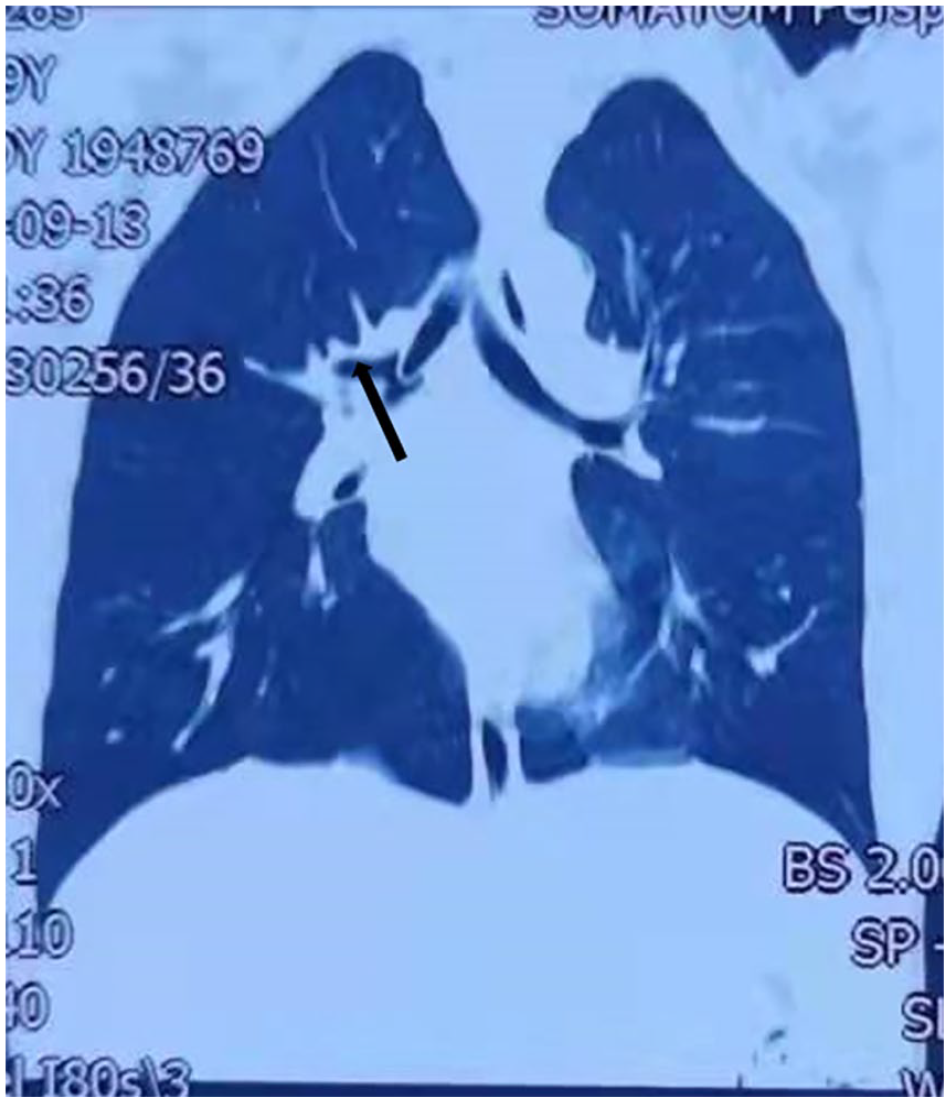
Foreign bodies in the right main bronchus.
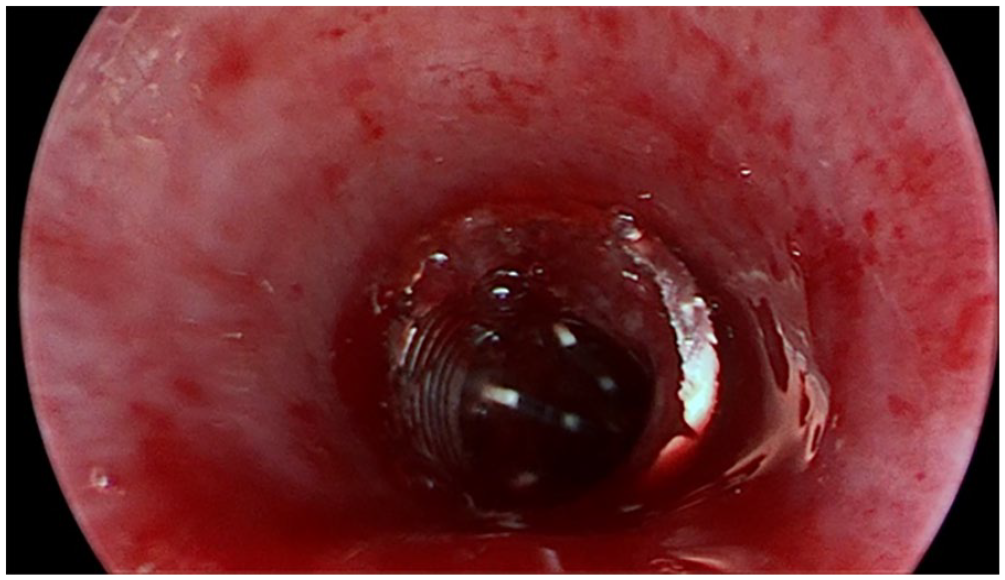
Pen cap was hollow and attached to the bronchial wall.
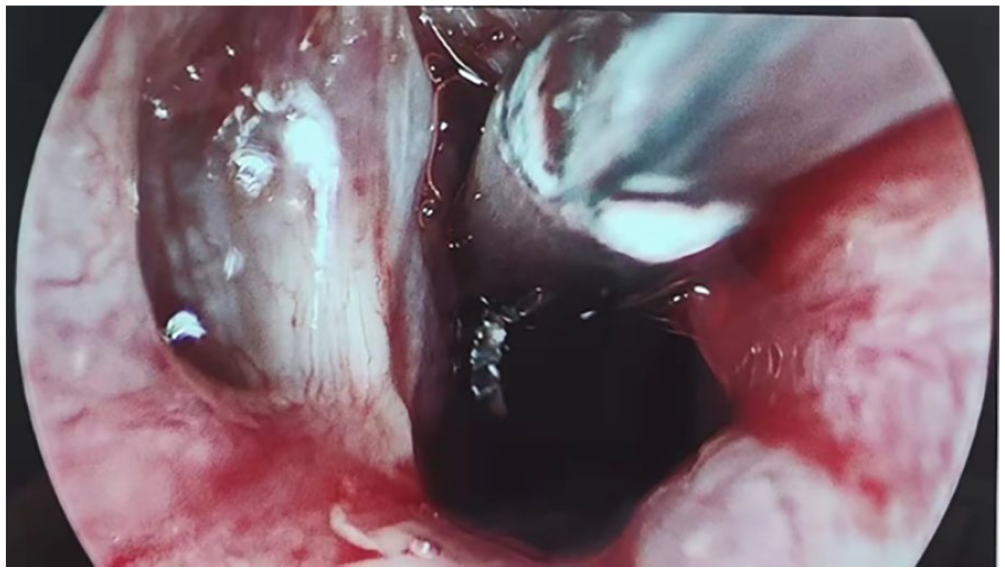
The foreign body is under the glottis and is difficult to remove.

The length is about 16 mm.

The diameter is about 10 mm.
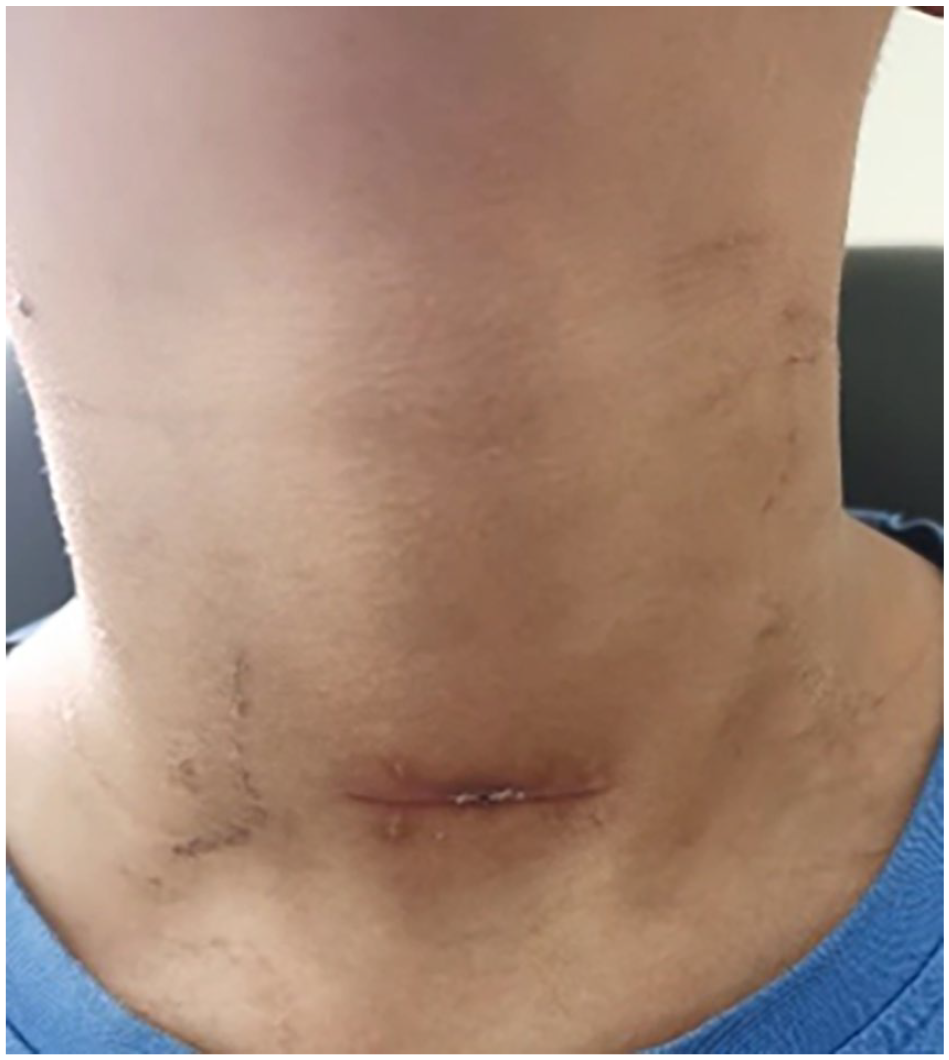
Incision healing after extubation.
Surgical Technique
Following successful administration of general anesthesia, the child’s spontaneous breathing is maintained, and supplemental oxygen is provided until sufficient oxygen reserves are established. If repeated attempts to remove the foreign body through the glottis are unsuccessful or if there is subglottic edema or impracticality in glottic removal, a tracheotomy is performed. At this time, 2 well-trained teams are needed: one is responsible for opening the trachea and removing the foreign body from the tracheal incision, and the other is responsible for bronchoscopy examination to catch the foreign body and pull it to the tracheotomy area.
The patient is positioned in a supine posture with the head hyperextended, and the patient is supported beneath the shoulders. A transverse skin incision, approximately 25 mm in length, is made between the second and third transverse cervical lines, exposing the cervical region. The subcutaneous tissue, anterior cervical fascia, and anterior cervical strap muscles are meticulously dissected longitudinally along the median neck to expose the anterior tracheal fascia and address any bleeding, as necessary. After confirming the precise positioning of the trachea, a longitudinal incision is made through the third tracheal ring. With the guidance of rigid tracheoscopy, the foreign body is carefully grasped using a specialized clamp and maneuvered toward the tracheotomy site via the glottis. Under direct visualization, the foreign body is extracted through the tracheotomy opening, and an appropriate tracheal cannula is inserted and securely fastened. To close the wound, sutures are applied at each end of the transverse skin incision.
Postoperatively, a cervicothoracic X-ray is performed to verify the proper placement of the inferior end of the cannula in relation to the carina, while also confirming the absence of pneumothorax or pneumomediastinum.
Approximately 1 week after the procedure, provided there are no complications or once any complications have fully resolved, an attempt is made to remove the cannula. Decannulation is performed only if the cannula remains closed for a continuous 48-hour surveillance period without the need for reopening.
Discussion
General Management of Tracheal Foreign Bodies
Foreign body aspiration is a common cause of acute respiratory distress in children and is often linked to improper chewing and swallowing habits, as well as the habit of placing objects in the mouth. Patients typically present with choking, breath-holding, shortness of breath, and diminished breath sounds, although loss of voice, dysphonia, or increased salivation may also occur. Prompt recognition and treatment of tracheal foreign bodies are essential to minimize the potentially severe and even fatal consequences. 6 A clear history of foreign body aspiration and typical symptoms and signs can help in the diagnosis. Ancillary tests can also help in diagnosis and subsequent treatment. In the past, chest radiographs were commonly used as an aid, but they had a low positive rate for foreign body identification. In the case presented in this article, the absence of significant positive signs on the chest radiograph may be due to the location of the foreign body. Currently, CT examination is considered a better method for identifying airway foreign bodies. CT examination not only shows the location and exact shape of the foreign body in the airway 7 but also identifies pulmonary complications such as emphysema, pulmonary atelectasis, pneumonia, mediastinal emphysema, subcutaneous emphysema, and other sequelae. 8 According to the literature, plain CT scans have a sensitivity of 98.3%, a specificity of 93.6%, a positive predictive value of 99.2%, a negative predictive value of 86.5%, 9 and a positive rate of 95.5% for spiral CT. 10 CT also presents certain limitations. First, it is not a therapeutic tool and cannot directly remove foreign bodies. In cases where children exhibit severe respiratory distress, prompt examination or even resuscitation takes precedence over CT imaging. Second, there is a risk of the child’s condition deteriorating during the examination. Cooperation from the child is necessary, and sedation is often required for uncooperative individuals. However, violent coughing or vomiting during the examination or sedation can lead to changes in the foreign body’s position or the potential aspiration of vomit, exacerbating respiratory distress. 2 Third, false positives can occur due to endogenous sputum clots, airway infections, tracheobronchial softening, airway tumors, or tracheobronchial stenosis. Last, it is important to consider the potential radiation risk associated with CT scans, especially in pediatric patients.8 -11
Rigid bronchoscopy under general anesthesia is widely considered the gold standard for diagnosing and treating airway foreign bodies 12 due to its safety and effectiveness. 13 However, other tools such as flexible bronchoscopy, 14 ultrafine cryoprobe, 15 reverse grasping forceps, electrocoagulation, mesh baskets, and balloons 16 are also available and have been indicated to be useful in removing foreign bodies, as reported in relevant articles.
When to Remove a Foreign Body From a Tracheotomy
Foreign body aspiration is a life-threatening emergency requiring immediate intervention. In the majority of cases, removal of foreign bodies can be performed through rigid tracheoscopy. However, in certain cases of tracheal foreign bodies, combining tracheotomy with these modalities may be the safest way to remove the foreign body and save the child’s life.17 -24 If not removed in time, children may develop complete airway obstruction, causing acute respiratory distress or even respiratory arrest. Sharp foreign bodies can cause persistent edema and granulomatous hyperplasia. Organic foreign bodies and a retention period of 30 days and over constitute major risk factors for the development of bronchiectasis. 25
In a retrospective study of tracheotomy cases, the indications for the procedure were often related to neuromuscular-related diseases, congenital malformations, accidental injuries, and oncological diseases.26 -28 Tracheotomy is frequently used as a crucial method for breathing support and the management of respiratory insufficiency. However, in some cases, tracheotomy may also be utilized as a technique to remove foreign bodies. In a literature review conducted by Marks et al., 104 out of 5296 cases (2%) required tracheotomy for foreign body removal to save lives. 23 The indications for tracheotomy for foreign body removal are important to consider, particularly in cases similar to those presented in this article. In light of previous literature and the cases presented in this article, we have compiled a summary of the indications for tracheotomy. They are as follows:
1. Giant foreign body: Typically, the narrowest point of the airway is the subglottic region, which can become further constricted due to edema caused by the passage of a large foreign body. In some cases, the shape of the foreign body may allow for passage only in a particular direction, such as with items such as pen caps (case 6 & case 7). Although reverse grasping forceps may be effective in removing such items, tracheotomy remains a viable option. 29 However, due to the high-risk nature of tracheal foreign bodies, the use of steroids to reduce edema prior to surgery is a matter of debate. Organic foreign bodies, such as peanuts and soybeans, can absorb moisture and become swollen, making removal in situ impossible. 24 In such cases, we first attempt to remove the foreign body from the vocal cords. If it cannot be safely extracted from beneath the vocal cords or other airway structures, tracheostomy may be necessary. This technique can serve both as a route for foreign body removal and as a means of ventilatory support. Sometimes, foreign bodies may be difficult to remove via the tracheotomy port and may require forceful extraction through the vocal cords. Dividing the foreign body may be an option, but this approach has its own set of challenges. 24
2. Irregular, sharp-edged foreign bodies: They are usually characterized by multiple sharp edges, which can cause damage to the vocal cords and airway tissue during removal. 23 Importantly, even the most experienced physicians may find it challenging to safely remove such foreign bodies. Wrapping the sharp edges may be necessary before attempting removal to minimize the risk of injury to the airway.
3. Upper airway obstruction: When the foreign body is lodged in the subglottic tissue, it can become embedded and cause subglottic edema, and sometimes even granulation tissue. Repeated attempts to remove a large foreign body can also result in subglottic and laryngeal edema. In a study by Marks et al., 52 out of 102 mesotracheostomy cases were performed due to laryngeal edema caused by foreign body obstruction. 23
4. Limited medical resources and lack of advanced endoscopic equipment: In settings with limited resources, tracheotomy combined with postural percussion has been successfully used as an alternative to rigid bronchoscopy for the removal of inhaled foreign bodies in children. 20
Complications of Foreign Body Removal Through a Tracheotomy Opening
Although removal of a foreign body by tracheotomy is a crucial step in treatment, clinicians must remain vigilant to the potential complications that may arise. Early complications of tracheotomy (<1 week) include bleeding from the incision, accidental decannulation, subcutaneous emphysema (including mediastinal emphysema and pneumothorax), and infection. Long-term complications (≥1 week) may include stenosis of the trachea or stoma, tracheal softening, tracheo-arterial fistula, aspiration pneumonia, dysphonia, dysphagia, tracheoesophageal fistula formation, obstruction, and accidental detubation.
Several studies have reported varying rates of complications associated with tracheotomy, ranging from 7.1% to 35.2%. 30 Gumussoy’s follow-up study of 273 patients who underwent tracheotomy suggests that the incidence of subcutaneous emphysema (including mediastinal emphysema and pneumothorax) is higher when using a transverse skin incision as opposed to a longitudinal skin incision. 31 In this study, the majority of tracheotomy-related complications were cases of subcutaneous emphysema (6 out of 7 cases), specifically mediastinal emphysema (5/7), subcutaneous emphysema (3/7), and pneumothorax (1/7). Several types of emphysema may exist in a mixture. It is significantly higher than the reported incidence in the literature. This may be attributed to the nature of tracheotomy and foreign body removal in emergency situations with transverse incisions. However, it is worth noting that these complications can be resolved in the short term.
Bleeding is a common early complication of tracheotomy, as reported in previous studies. 30 However, in the cases presented here, bleeding did not occur, which may be due to the small sample size. An enhanced CT scan can reveal the anatomical relationships between the pretracheal vessels and thyroid gland, which can facilitate a safer tracheotomy procedure and reduce the risk of bleeding and thyroid damage. 32 Although this examination may not be applicable to tracheal foreign body removal, it still provides valuable insight into the possible anatomical relationships of pretracheal vascular tissue.
In most cases, the child can be successfully extubated within 7 to 10 days following foreign body removal, and distant complications are rare. It is important to preserve the tracheotomy site as much as possible after foreign body removal to prevent complications such as mediastinal subcutaneous emphysema. Suturing the tracheotomy site immediately after removal is not recommended, and the tracheal tube should be gradually removed once the child’s condition improves.
Limitations of the Study
The present study has some limitations, including a small sample size and a retrospective design. The conversion from rigid tracheoscopy for foreign body removal to tracheotomy for foreign body removal may be influenced by the clinician’s skills. Intraoperative assessment to determine if changes are needed in the surgical approach is another limitation of this study. The possibility of preoperatively predicting the likelihood of a change in the surgical approach on the basis of the child’s symptom profile, foreign body characteristics, and CT findings is a worthwhile direction for future research.
Conclusion
The primary method for removing tracheobronchial foreign bodies is rigid bronchoscopy, which has a high success rate. However, foreign bodies are difficult to remove when they are too large or irregular, have sharp edges, are embedded in the subglottic tissue with edema, cannot pass smoothly through the glottis, or when local endoscopic facilities are inadequate. In such cases, tracheotomy is an important alternative that requires advance preparation by the surgeon and anesthesiologist. During tracheotomy foreign body removal, 2 well-trained teams should work together: 1 for neck access, tracheal opening, and direct visualization of foreign body removal, and the other for bronchoscopy to grasp the foreign body and pull it to the tracheotomy area. 21 Simultaneous and rapid teamwork is essential to ensure the safe removal of the foreign body. It is also important to be aware of postoperative complications associated with tracheotomy, especially its early complications, such as pneumothorax, pneumomediastinum, and bleeding.
Footnotes
Acknowledgements
Not applicable.
Author Contributions
H.C.W., Y.C.C., Y.S.T., and H.G. P. contributed to the study’s conception and design; data acquisition, analysis, and interpretation; and drafting and critical revision of the article. L.L. contributed to the study design and data interpretation and critically revised the article. All authors provided final approval and agreed to be accountable for all aspects of the work.
Availability of Data and Materials
The datasets used and/or analyzed during the current study are available from the corresponding author (Y.S.T.,
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by Guangdong High-level Hospital Construction Fund Clinical Research Project of Shenzhen Children’s Hospital (LCYJ2022063).
Ethics Approval and Consent to Participate
All procedures performed in this study involving human participants were in accordance with the ethical standards of the institution. Due to all participants included in the study are under 18, informed consent was obtained from all individual participants’ parents and/or legal guardian. As a retrospective study, no ethics approval is required in our institute.
Consent for Publication Written
Informed consent for publication was obtained from the patient’s parents for the use of their medical records and exam images in writing this study.
Competing Interests
All authors declare that they have no conflicts of interest.
