Abstract
Objective:
To investigate the necessity of subsequent dental treatment for patients with odontogenic sinusitis (OS) after endoscopic sinus surgery (ESS).
Methods:
OS patients who received ESS from January 2018 to May 2022 were eligible. Demographic data, medical history, Lund–Mackay (LM) computed tomography (CT) score, Lund–Kennedy (LK) endoscopic score, and OS-specific CT score were recorded and analyzed. All patients were followed up for 6 months after surgery.
Results:
A total of 48 patients (30 males and 18 females) were enrolled. A total of 35 cases (72.9%) were caused by dental diseases (periapical periodontitis), and 13 cases (27.1%) were caused by iatrogenic factors (including tooth extraction or implantation). The overall treatment success rate was 97.9%, and the success rates in the dental disease OS group (97.1%) and the iatrogenic OS group (100%) were not significantly different (X2 = 0.329, P = .729). None of the patients in the dental disease group received treatment of the causative teeth within 6 months after the operation, except for one patient who received tooth extraction treatment 6 months after the operation.
Conclusion:
Without considering the impact of dental disease on patients’ oral health, OS can be completely alleviated by ESS alone, even if no dental treatment is carried out after surgery.
Introduction
Odontogenic sinusitis (OS) is a type of bacterial sinusitis caused by adjacent maxillary dental infection or that occurs secondary to adjacent infectious maxillary dental infection. OS initially occurs in the maxillary sinus but can spread to other paranasal sinuses or structures, including the ostiomeatal complex (OMC), ethmoid sinus (ES), frontal sinus (FS), and even sphenoid sinus (SS).1,2 OS has a high incidence rate, accounting for 40% to 70% of unilateral sinus lesions.3,4 In addition, with the popularity of invasive oral treatment, the incidence of OS has continuously increased.5,6 OS is easily overlooked and misdiagnosed in clinical practice. Wang et al. conducted a systematic analysis of 3031 cases of chronic rhinosinusitis and identified 55 cases of OS, of which only 36 cases showed OS in the imaging report, and the initial diagnostic rate was 65.5%. 7 In other words, approximately 1/3 of OS was misdiagnosed as non-OS sinusitis.
The treatment methods for OS mainly include drug treatment, sinus surgery, and the treatment of causative teeth in stomatology. Sinus surgery includes Caldwell-Luc surgery and endoscopic sinus surgery (ESS); the former has been gradually abandoned and is only used in special cases, while ESS is widely used. 8 The efficacy of ESS for the treatment of OS has been affirmed by scholars, who believe that as long as the surgery successfully restores the ventilation and drainage of the sinuses, good therapeutic effects can be obtained.9,10
For the treatment of OS, it is unknown whether dental treatment is required after ESS. 2 At present, few studies have investigated this question. To draw a conclusion, we reviewed the prognosis of OS patients 6 months after ESS to determine whether the treatment of diseased teeth affected the curative effect of OS.
Methods
Case Collection
The institutional review board of Beijing Chaoyang Hospital approved this retrospective study (NO. 2022-department-50). OS patients who underwent ESS in our hospital from January 2018 to May 2022 were eligible. Their age, sex, medical history, physical examination results, imaging results, surgical content, Lund–Kennedy (LK) endoscopic score, and Lund–Mackey (LM) CT score were reviewed. The LM CT (Table 1) and LK endoscopic scores (Table 2) were evaluated according to previous studies.11,12
Lund–Mackay CT Scoring System*.
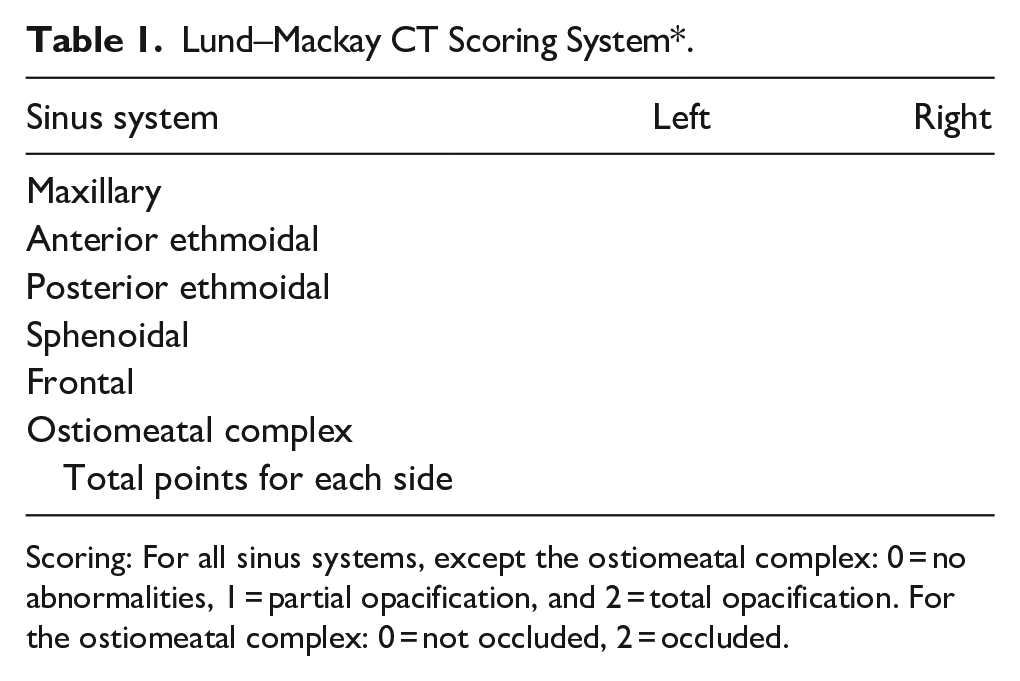

Scoring: For all sinus systems, except the ostiomeatal complex: 0 = no abnormalities, 1 = partial opacification, and 2 = total opacification. For the ostiomeatal complex: 0 = not occluded, 2 = occluded.
Lund–Kennedy Endoscopic Scoring System*.
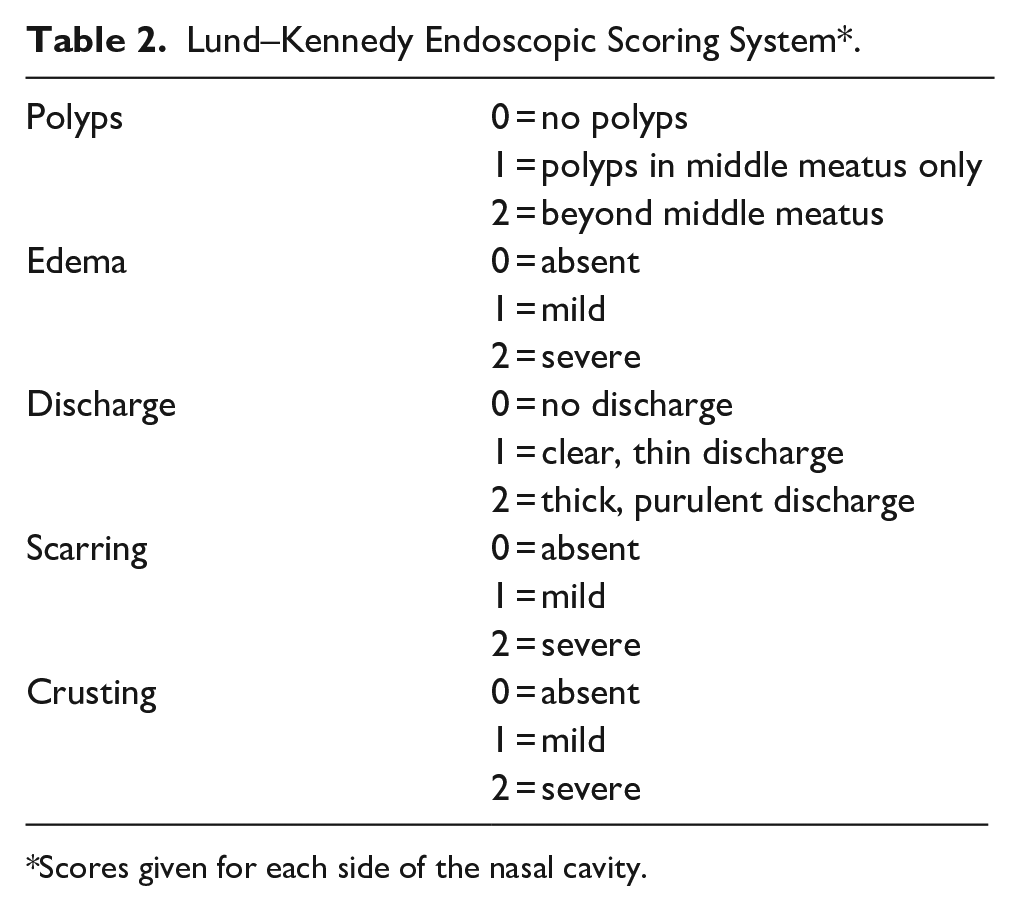
Scores given for each side of the nasal cavity.
The inclusion criteria were as follows: (1) OS patients who underwent ESS surgery in our hospital; (2) age ≥ 18 years; (3) postoperative pathology confirmed chronic inflammation; and (4) paranasal sinus CT in our hospital system, which could be used for review and reconstruction. Exclusion criteria: (1) OS patients with fungal sinusitis and (2) OS patients with inverted papilloma.
The OS diagnostic criteria were as follows1–4: (1) abnormal odor or foul smell in the nasal cavity; (2) history of tooth disease or oral treatment on the corresponding side; (3) white purulent secretions in the middle nasal meatus, which could be accompanied by polypoid oedema, medial wall of maxillary sinus moving inward or swelling on endoscopy; and (4) odontogenic lesions, including root protrusion into the sinuses, apical abscess, periapical inflammation, destruction and defect of the maxillary sinus floor, oral maxillary sinus fistula, and foreign bodies and implant protrusion into the sinuses after dental treatment on CT. The basis for determining the diagnosis was to meet (4), with or without meeting criteria (1), (2), or (3). The final diagnosis was made by 2 senior doctors with a rich experience in rhinology.
OS-Specific CT Score
To define the scope of inflammation more accurately, the CT inflammation classification was further refined. The reference was mainly based on the presence or absence of sinus abscess, the thickness of sinus mucosa, and the proportion of abscess or mucous membrane thickness in the whole maxillary sinus. In addition, when it extended beyond the maxillary sinus, such as the OMC, FS, and ES, OS inflammation must follow the path of OMC-ES-FS. FS and ES always have inflammation when the OMC is involved, and the drainage is not smooth. Therefore, an incremental scoring strategy was adopted, with a total score of 0 to 12 points, which we named the OS-specific CT score (Table 3, Figure 1).
OS-Specific CT Score.

Abbreviations: ES, ethmoid sinus; FS, frontal sinus; MS, maxillary sinus; OMC, ostiomeatal complex; OS, odontogenic sinusitis; SS, sphenoid sinus.
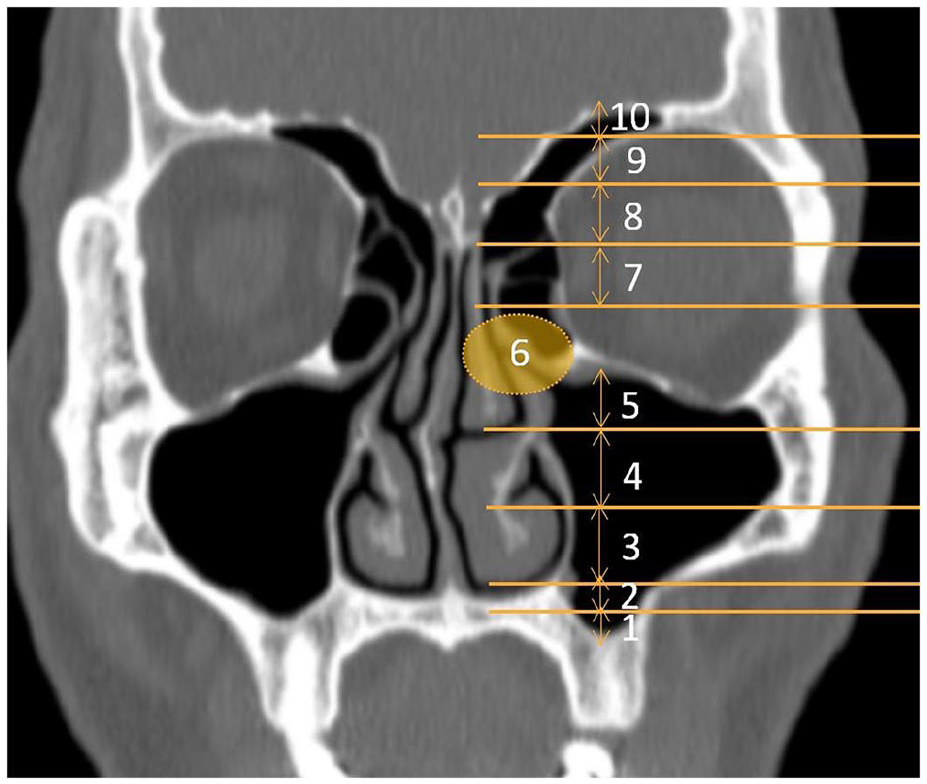
OS-Specific CT score.
Treatment
All enrolled patients underwent ESS surgery under general anesthesia. The operation procedure opened the maxillary sinus and part of the ES according to the degree of inflammation, and the FS was opened as appropriate. Plasma hemostasis and a small amount of gelatin sponge were used during the operation. During the perioperative period, antibiotics were administered. Mucoactive drugs, nasal sprays, and anti-allergy drugs were also used. The drug treatment in the 2 groups (dental disease group and iatrogenic group) was the same.
Follow-Up
All OS patients who received surgical treatment were followed up for at least half a year. All patients underwent nasal clearance in the first week and the third week after ESS, and the patients were generally cured in the third week after ESS. After that, follow-up and recheck were performed at 2 months and 6 months after the operation, respectively.
Statistical Analysis
The statistical software used was SPSS 20.0 (IBM, USA). The intergroup differences in counting data were analyzed by independent sample t tests, the intergroup differences in measurement data were analyzed by chi-square tests, and the Spearman correlation coefficient was used for correlation analysis.
Results
Basic Information and Evaluation of OS Patients
A total of 48 OS patients were included for further analysis. The patients’ ages ranged from 26 to 77 (47.9 ± 13.5) years old. There were 30 males (62.5%) and 18 females (37.5%), and 26 (54.2%) cases on the left and 22 (45.8%) cases on the right (P > .05) were included. Among them, 35 cases (72.9%) were caused by dental diseases, such as periapical periodontitis; 13 cases (27.1%) were caused by iatrogenic factors, including tooth extraction and implantation.
The preoperative OS-specific CT score was 8.9 ± 2.2; the LM CT score was 7.2 ± 3.0, and the LK score was 3.2 ± 1.3. The vast majority (43 of 48 cases, 89.6%) of OS cases involved sinuses other than the maxillary sinus, 5 of which involved all of the sinuses (10.4%), and only 5 cases were confined to the maxillary sinus (10.4%). The details of the OS patients are shown in Table 4. On CT, the inflammatory expansion of OS presented progressive or sequential characteristics. ES could only affect FS after involvement of the OMC, and the postethmoid sinus (PE) was less involved. For patients with PE, the FS was full of inflammation, indicating that inflammation progressively expands in the anatomical region. If the SS was engaged, all sinuses were involved.
Details of the Enrolled OS Patients.
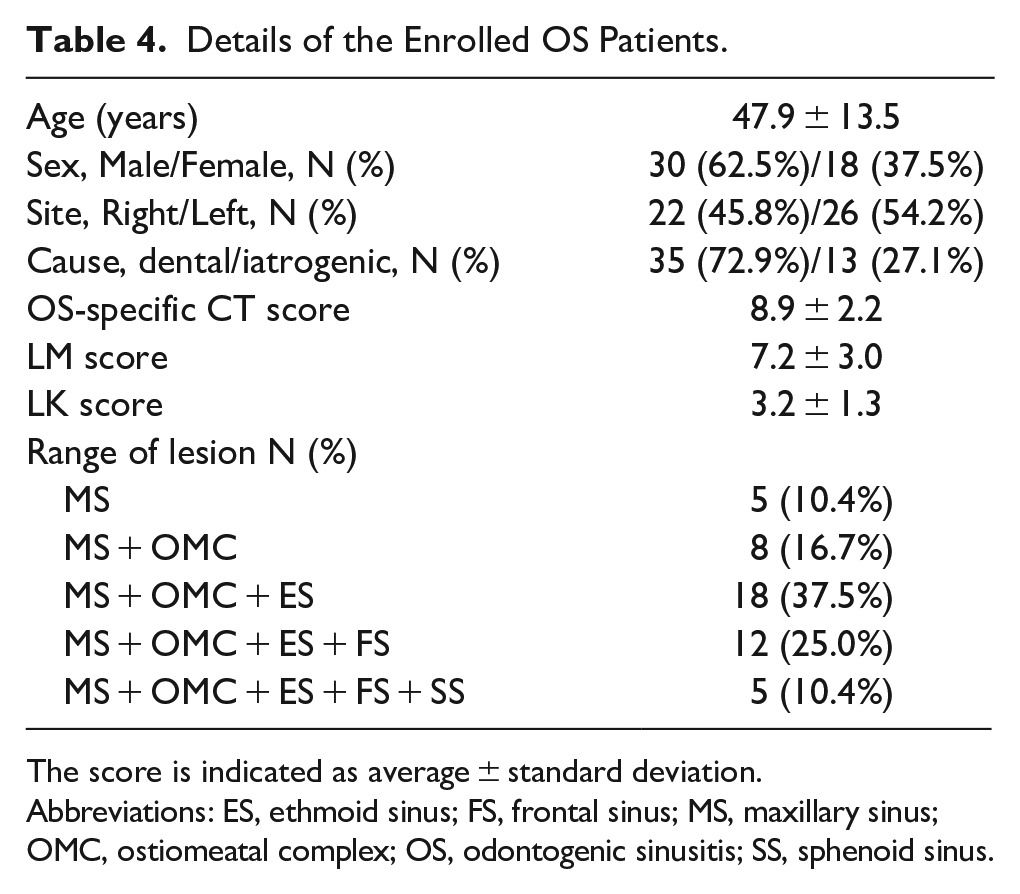
The score is indicated as average ± standard deviation.
Abbreviations: ES, ethmoid sinus; FS, frontal sinus; MS, maxillary sinus; OMC, ostiomeatal complex; OS, odontogenic sinusitis; SS, sphenoid sinus.
ESS Outcomes of OS Patients After 6 Months
Follow-up results showed that among the 48 OS patients, 47 of them were completely recovered and did not have the causative teeth treated after ESS, and the overall effective rate was 97.9%. One patient experienced recurrence half a year after surgery; this patient underwent tooth extraction, and the symptoms were relieved. Figure 2a and b show the CT scans of an OS patient before and 6 months after ESS.
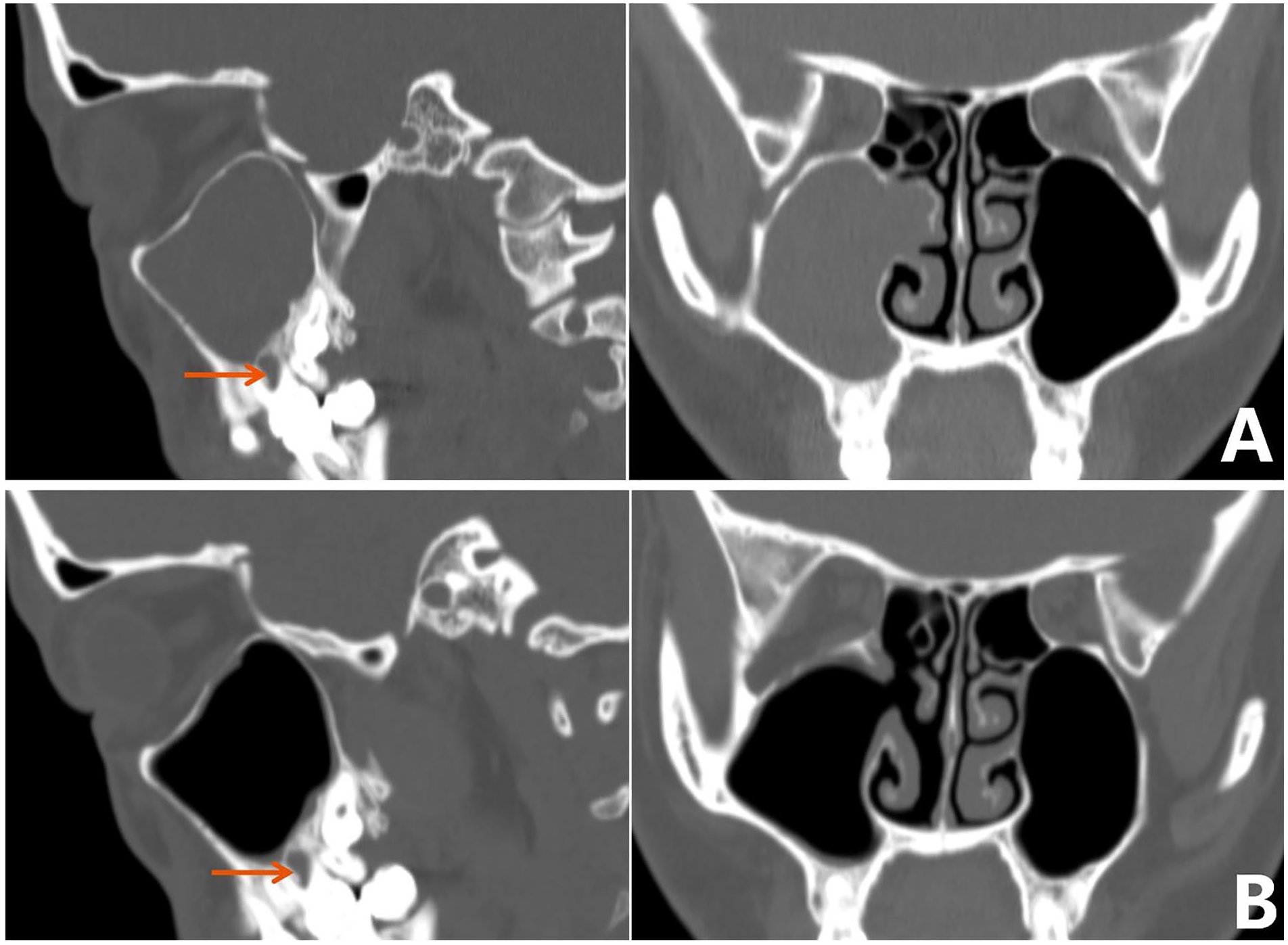
Paranasal CT scan of an OS patient before (A) and 6 months after ESS (B). The arrow shows the causative tooth.
Relationship Among the Clinical Parameters
Spearman correlation was used to analyze the relationship among each parameter. As shown in Figure 3, there was a significant relationship between the OS-specific CT score and the LM CT score (r = 0.97, P = .000). There was no significant correlation between the recurrence rate and any of the parameters, including age, sex, site (left/right), dental or iatrogenic cause, LMCT score, LK score, and OS-specific CT score, all P >.05. The details of the correlation among each clinical parameter are shown in the Supplemental Material.
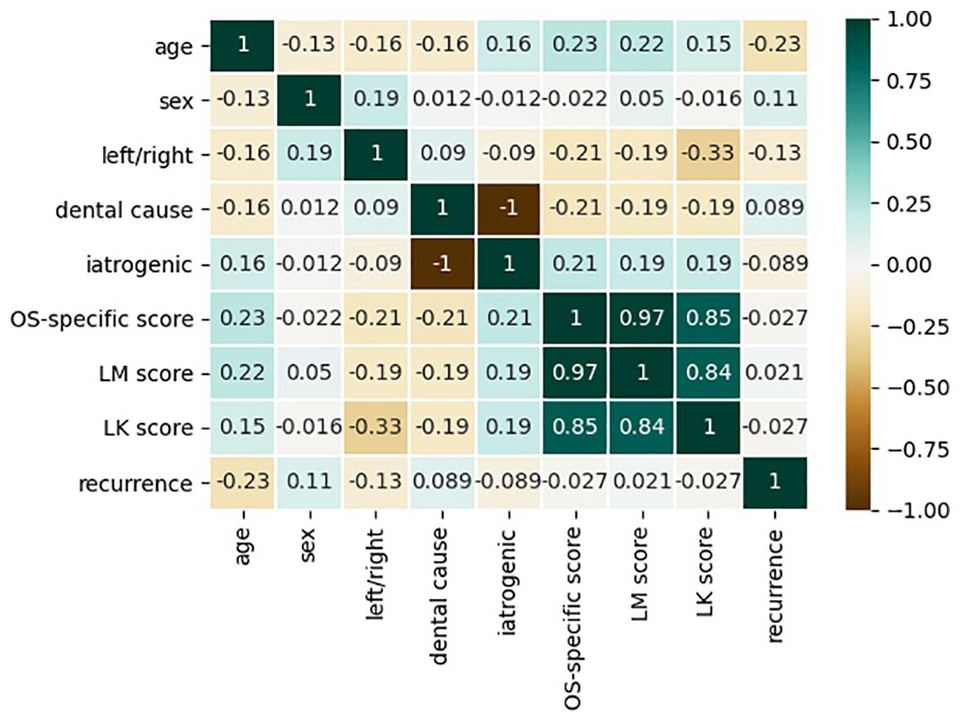
The correlation heatmap of each parameter (Spearman correlation analysis).
Comparison of the Outcome Between the Dental Group and Iatrogenic Group
The differences in the clinical characteristics and ESS outcomes between the dental group and the iatrogenic group were further compared (Table 5), and the results showed that there was no significant discrepancy between the 2 groups in terms of the preoperative OS-specific CT score (9.6 ± 2.1 vs 8.7 ± 2.2, P = .171), LM CT score (8.1 ± 2.8 vs 6.9 ± 3.1, P = .190), and LK score (3.6 ± 1.3 vs 3.0 ± 1.2, P = .156), respectively. There was no obvious difference in the treatment success rate between the 2 groups (97.1% vs 100.0%, P = .729).
Comparison of the Dental Group and Iatrogenic Group.
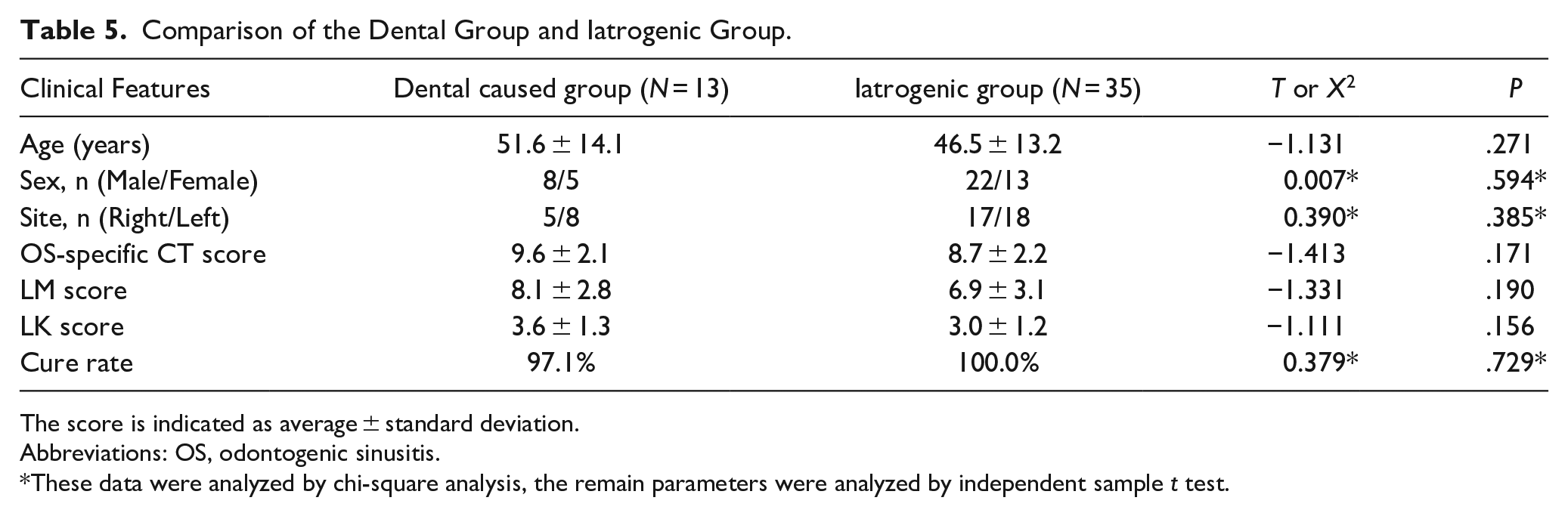
The score is indicated as average ± standard deviation.
Abbreviations: OS, odontogenic sinusitis.
These data were analyzed by chi-square analysis, the remain parameters were analyzed by independent sample t test.
Discussion
In this study, we performed an efficacy analysis of OS patients who did not receive treatment for causative teeth 6 months after ESS. The relationship between OS-related clinical data (OS-specific CT score, LK endoscopic score and LM CT score, site of OS, cause of OS, age, and sex) and the prognosis of OS were also analyzed. The results showed that none of the above clinical parameters were found to be associated with the prognosis of OS patients, and there was no difference between the dental disease and the iatrogenic efficacy rate, indicating that the vast majority of OS patients can achieve satisfactory clinical effects after ESS and that patients do not need further postoperative management of the causative teeth.
Unlike non-OS sinusitis, OS needs a more accurate treatment strategy. Insufficient understanding and treatment of OS may lead to prolonged disease duration and cause unexpected complications. It is necessary to check the course of each patient, including diagnosis, imaging, treatment, and follow-up.13–15 Otorhinolaryngologists generally do not have a sufficient understanding of OS, including the diagnosis, treatment, and prognosis under different treatment methods. An inadequate understanding of OS is one of the main reasons for the poor effect of ESS surgery for such diseases.16,17
ESS surgery is one of the ways to treat OS, and it has been suggested to have excellent efficacy; however, there is still a dispute about whether subsequent dental treatment is needed. Some studies have indicated that ESS and treatment of causative teeth should be carried out for patients simultaneously, while others have provided opposing opinions.18–20 Felisati et al. included more than 250 patients in their study, and the results showed that the success rate after simultaneous ESS and elimination of dental origin was 99%. It is essential to eliminate tooth infection. 18 If the diseased tooth is missing/left, the treatment result is poor or the improvement only lasts for a short time, which requires further revision surgery.
However, some studies have noted that the diseased teeth should only be treated when the symptoms are serious. Mattos et al. noted that conservative treatment is the primary method to control odontogenic sinusitis, and surgical treatment should only be considered after the symptoms continue after conservative treatment. 19 Longhini et al. noted that a good therapeutic effect can be achieved only by pulling out the diseased tooth, but this was questioned because many cases of OS appeared after tooth extraction. 20 In the contrary. Sato et al. confirmed that 83 out of 85 OS patients could be cured by ESS alone, and the success rate of ESS in curing OS was 97.6%. 9
Based on present observations, ESS is a crucial treatment for patients with OS, but perioperative medication may also contribute to the success of ESS. All the OS patients were treated with antibiotics for 3 weeks, mainly metronidazole and cephalosporin, and patients who were allergic to cephalosporin were treated with roxithromycin instead.
The Mucoactive drug that we selected was a eucalyptol-limonene-pinene enteric soft capsule, a Chinese medicine developed from the ferulic acid of ligustrazine, which decreases mucous viscosity and increase mucociliary clearance by acting on the cilia. 21 The nasal spray that we selected was mometasone furoate aqueous nasal spray. Antihistamine drugs have also been used to reduce nasal secretion and improve nasal symptoms in patients. In EPOS 2020, 22 antihistamines are not recommended as first-line treatment for sinusitis due to insufficient evidence, but to improve nasal sneezing and runny nose symptoms, we have used antihistamines in the course of treatment.
The incidence of OS may be related to the sinuses themselves, which also explains why many patients have dental disease but no OS. The ESS operation can reverse the factors inducing sinusitis. Even if dental disease still exists, it will not induce sinusitis again. Furthermore, studies have shown that, unlike chronic rhinosinusitis, the ciliated cells of the affected sinus epithelium were not irreversibly injured, and the ciliated columnar epithelium of the OS was intact, which may be the reason that after ESS, when the drainage channel of the sinuses is successfully established and the purulent secretion is completely aspirated, OS can be relieved. 23
Based on the observation of our study, even if OS involves multiple sinuses, most patients could still obtain a very good prognosis through adequate ESS surgery, and none of the parameters (OS-specific CT score, LK endoscopic score and LM CT score, site of OS, cause of OS, age, and sex) were correlated with the surgical prognosis of OS. This indicates that regardless of how many sinuses are involved in OS, satisfactory curative effects can be obtained through ESS. In addition, we also found that there was no obvious difference in treatment efficacy between the iatrogenic group and odontogenic group, suggesting that ESS may achieve satisfactory efficacy regardless of the pathogenic factor in OS.
In our follow-up study, 1 patient experienced recurrence 6 months after surgery. The patient’s nasal symptoms were significantly relieved after surgery, but OS-related symptoms appeared again 6 months later. Reexamination CT indicated a recurrence of sinusitis, and the patient underwent dental extraction treatment. These results imply that a 6-month follow-up may not be sufficient. Extending the follow-up time may be beneficial for a more accurate understanding of the prognosis of OS after ESS.
In conclusion, the current study showed that the majority of OS patients can be cured by ESS treatment alone, suggesting that ESS should be a first-line therapy for OS, and subsequent dental treatment for OS after ESS is not required in most cases.
Supplemental Material
sj-csv-1-ear-10.1177_01455613231196105 – Supplemental material for The Necessity of Subsequent Dental Treatment for Odontogenic Sinusitis After Endoscopic Sinus Surgery
Supplemental material, sj-csv-1-ear-10.1177_01455613231196105 for The Necessity of Subsequent Dental Treatment for Odontogenic Sinusitis After Endoscopic Sinus Surgery by Xiaochang Zhao, Zufei Li and Jinfeng Liu in Ear, Nose & Throat Journal
Footnotes
Authors’ Contributions
Drafting the article: Xiaochang Zhao, Zufei Li, and Jingfen Liu. Acquisition of data: Zufei Li, Xiaochang Zhao, and Jingfen Liu. Analysis of data: Zufei Li, Xiaochang Zhao, and Jingfen Liu. Revising the article for important intellectual content: Jingfen Liu. Conception and design of the study: Xiaochang Zhao and Jingfen Liu
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
All of the procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This study was approved by the institutional review board of Beijing Chaoyang Hospital (NO.2022-科-50).
Informed consent
Informed consent was obtained from all individual participants and guardians included in this study.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
