Abstract
Objective:
To analyze the clinical effect of endoscopy-assisted functional rhinoplasty.
Methods:
Endoscopy-assisted functional rhinoplasty was performed in all patients. Deviated nasal septum was corrected, nasal septum cartilage graft was prepared through open access under the assistance of endoscopy, the nasal frame structure was adjusted with the endoscopy-assisted rhinoplasty combined with middle and inferior turbinoplasty, and the patient’s nasal ventilation function and external nose cosmetology were restored. Visual Analogue Scale (VAS), Nasal Obstruction Symptom Evaluation (NOSE), nasal acoustic reflex, and nasal resistance were examined preoperatively and 6 months postoperatively. Rhinoplasty Outcome Evaluation (ROE), nasal appearance deviation value, and morphological measurement of the external nose were used to assess the external nasal appearance. Finally, postoperative satisfaction was used for overall evaluation.
Results:
In terms of nasal ventilation evaluation, the VAS and NOSE scores of nasal obstruction decreased significantly at 6 months after the operation compared with that before the operation (1.96 ± 0.84 vs 6.68 ± 1.28, 4.25 ± 1.80 vs 12.25 ± 2.50; P < .05). Among the objective indexes, MCA1, MCA2 and NV5 were significantly increased whereas RT, MCA1a/MCA1b, MCA2a/MCA2b, MD1a/MD1b, and MD2a/MD2b were significantly decreased compared with those before the operation (P < .05). The MD1 and MD2 levels before and after operation had no significant differences (P > .05). In the evaluation of external nose morphology, postoperative ROE was significantly increased, and the deviation value of nasal appearance was significantly decreased [(16.93 ± 2.61 vs 10.64 ± 3.01), (1.46 ± 1.11 mm vs 5.72 ± 2.30 mm), P < .05]. In terms of postoperative patient satisfaction: 26 cases (92.9%) were very satisfied with nasal ventilation function, 2 cases (7.1%) were satisfied with nasal ventilation function, 24 cases (85.7%) were very satisfied with nasal appearance, and 4 cases (14.3%) were satisfied with nasal appearance.
Conclusions:
Nasal endoscopy-assisted functional rhinoplasty can improve the nasal ventilation function and external nasal morphology at the same time. Moreover, its clinical effect is good, and the patient satisfaction is high.
Introduction
A crooked nose is often accompanied by abnormal nasal structure, which affects facial beauty and causes respiratory dysfunction. Individuals with crooked nose have differences in the cause of nasal pyramid deviation, morphological deformities of external nose, anatomical relationship, and abnormal structure of the nasal cavity, which make crooked nose one of the most challenging deformities for rhinoplasty. 1
The application of nasal endoscopy in the operation of crooked nose has made rhinologists pay more attention to the correction of crooked nose. In this study, we reviewed and analyzed the clinical data of patients with crooked nose and nasal congestion who were treated in our center and compared the subjective and objective evaluations of nasal congestion and crooked nose before and after operation to explore the advantages of nasal endoscopy-assisted functional rhinoplasty in improving nasal congestion and external nasal morphology.
Materials and Methods
Patients and Data
The clinical data of 28 patients with congenital or traumatic crooked nose and nasal obstruction admitted to the Department of Otorhinolaryngology Head and Neck Surgery from January 2018 to December 2022 were retrospectively analyzed. The patients comprised 11 males and 17 females aged 22 to 53 years. All patients provided a written consent for usage of their photographs in scholarly publications.
A routine computed tomography scan and endoscopy were used for the evaluation of nasal structural abnormalities. Crooked nose can be divided into oblique type I deflection, C-type deflection, and S-type deflection. 2
All operations were performed by 1 surgeon. The shape of the external nose for all the subjects was then evaluated by 2 researchers who did not participate in the operation, and a conclusion was drawn according to their consensus.
Evaluation Method
Evaluation of nasal ventilation function
Visual Analogue Scale (VAS) and Nasal Obstruction Symptom Evaluation (NOSE) scale were used to subjectively evaluate the symptoms of nasal obstruction. 3 VAS score is on a 10-point scale, with 0 indicating complete nasal patency and 10 indicating complete nasal obstruction. The NOSE scale has 5 items scored by 0 to 4 (0 = none, 1 = very mild, 2 = moderate, 3 = relatively serious, and 4 = very serious). The higher the score, the more severe the symptoms of nasal congestion.
The first 2 minimum cross-sectional areas (MCA) of the nasal cavity were determined by a nasal acoustic reflectometer and recorded as MCA1 and MCA2. The distances between nostril to minimum cross‑sectional area (MD) and the MCAs, MCA1 and MCA2, are denoted as MD1 and MD2, respectively. The side with larger MCA and MD values served as the numerator (side a) and the side with smaller values served as the denominator (side b) to calculate the ratio of MCA and MD in the bilateral nasal cavity. The volume of the nasal cavity 5 cm from the anterior nostril (NV5) was recorded. The total resistance (RT) at the narrowest part of the nasal cavity under 150 Pa pressure was measured by a four-quadrant anterior nasal manometer.
Evaluation of external nose morphology
Subjective evaluation of external nasal morphology was performed with rhinoplasty outcome evaluation (ROE). According to the English questionnaire established by Alsarraf et al, 4 referred from the ROE Portuguese questionnaire translated by Izu et al, 5 was translated into Chinese according to the cross-cultural translation method of health-related quality of life assessment proposed by Guillemin et al. 6 The ROE questionnaire consists of 6 questions with 5 answer options on a scale of 0 to 4. A higher ROE score indicates a more satisfactory nasal appearance.
We referred to Guyuron B evaluation of the curative effect of crooked nose and improved it. 7 The exact midpoint of the horizontal line of the medial canthus of both eyes was used as the midline of the facial axis. The distance between the tip of the nose or the back of the nose from the midline was considered the degree of deviation. Deviations of 3 to 5, 6 to 8, and 9 to 12 mm were recorded as mild, moderate, and severe deviations, respectively. A postoperative deviation within 2 mm was considered cured, and a decrease in postoperative deviation by one grade was considered effective.
In addition, a protractor and vernier caliper were used to measure the external nasal morphology. The measurements included (1) nasal length: straight distance from nasal root to nasal tip, (2) nasal root width: straight distance between medial canthi, (3) nasal root height: the distance from the horizontal line of the root of the nose to the intersection of the vertical line of the medial canthi, (4) the angle of the alar of the nose: the angle formed by the nasal alar on both sides, and (5) the angle of the tip of the nose: the angle between the dorsum of the nose and the nasal columella.
Finally, postoperative satisfaction was used to evaluate the nasal ventilation function and external nasal morphology. Postoperative satisfaction was rated as very satisfactory, satisfactory, and unsatisfactory.
Description of the Surgical Procedure
An inverted “V” incision was made at the middle and lower 1/3 of the nasal columella, extending along the lateral edge of the nasal columella (inside the 2 mm of the inner edge of the nostril) to both sides of the nasal alar and the subchondral incision of the nasal vestibule (Figures 1A and 2A). The blood flow was protected to separate the flap and turn the flap upwards, keeping it under the superficial musculo-aponeurotic system (SMAS) layer and separating from the surface of the lower lateral nasal cartilages. The medial crus and lateral crus of the lower lateral cartilage were exposed, then the fornix part was exposed, and the soft tissue connection between the lower lateral cartilage interfornical ligament and the medial crus of the lower lateral cartilage was separated. The bilateral mucoperichondrium was peeled off from the anterior septal angle, and a part of the fibrous connection around the anterior nasal spine was also peeled off. The caudal end of the nasal septum was exposed, the part of the head under the SMAS layer was further separated, and the upper lateral cartilage was exposed. Note that when the keystone area was separated, the mucoperiosteum was longitudinally peeled off, the attachment of the lateral soft tissue was protected, and only the oblique nasal bone cone required for operation was exposed to avoid excessive osteotomy and ensure bone stability.
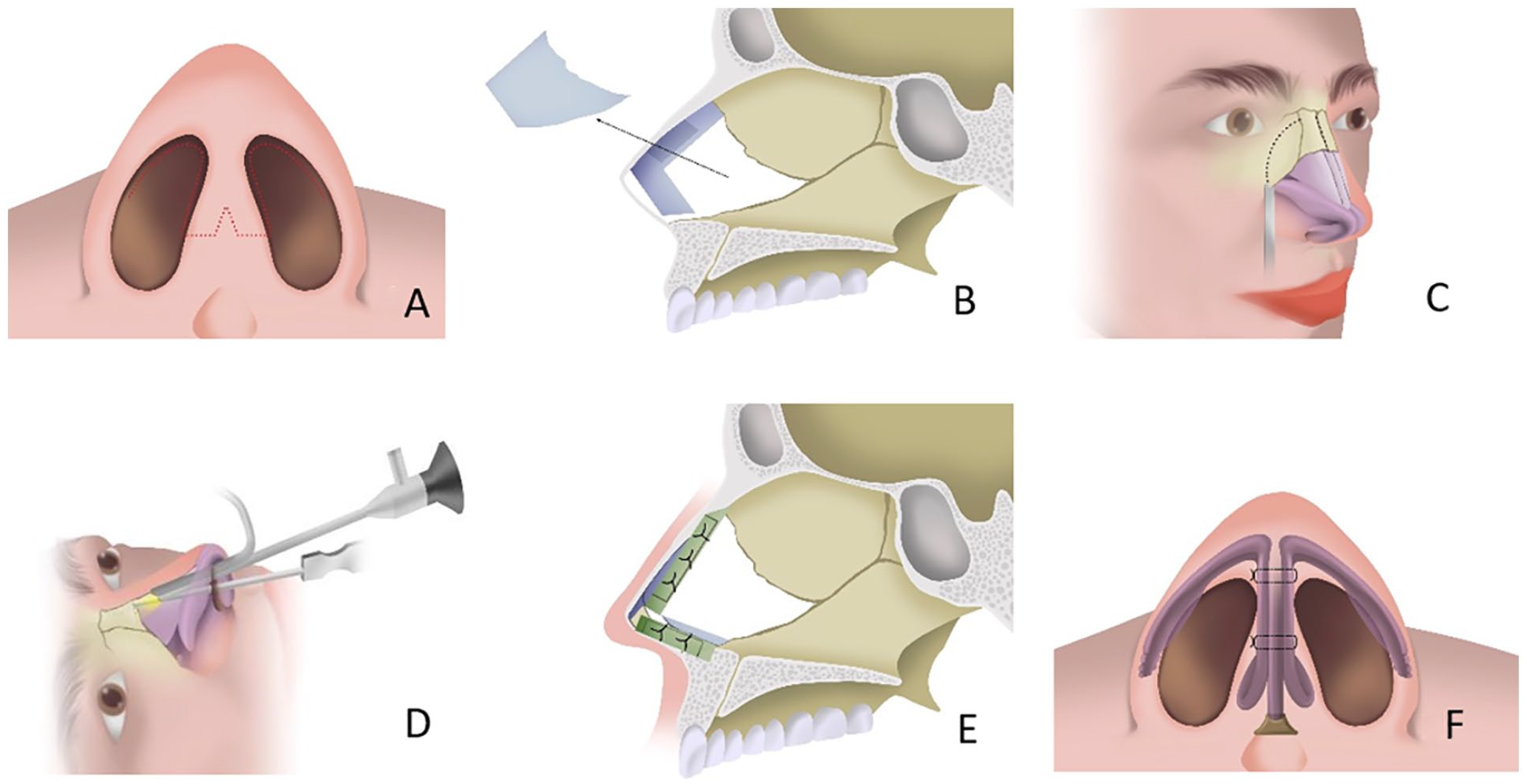
Schematic diagram of nasal endoscopy-assisted functional rhinoplasty. (A) Surgical incision. (B) Nasal endoscopic resection of nasal septum cartilage. (C, D) Lateral and midline osteotomy under nasal endoscopy. (E, F) Implantation of dorsal and caudal grafts.
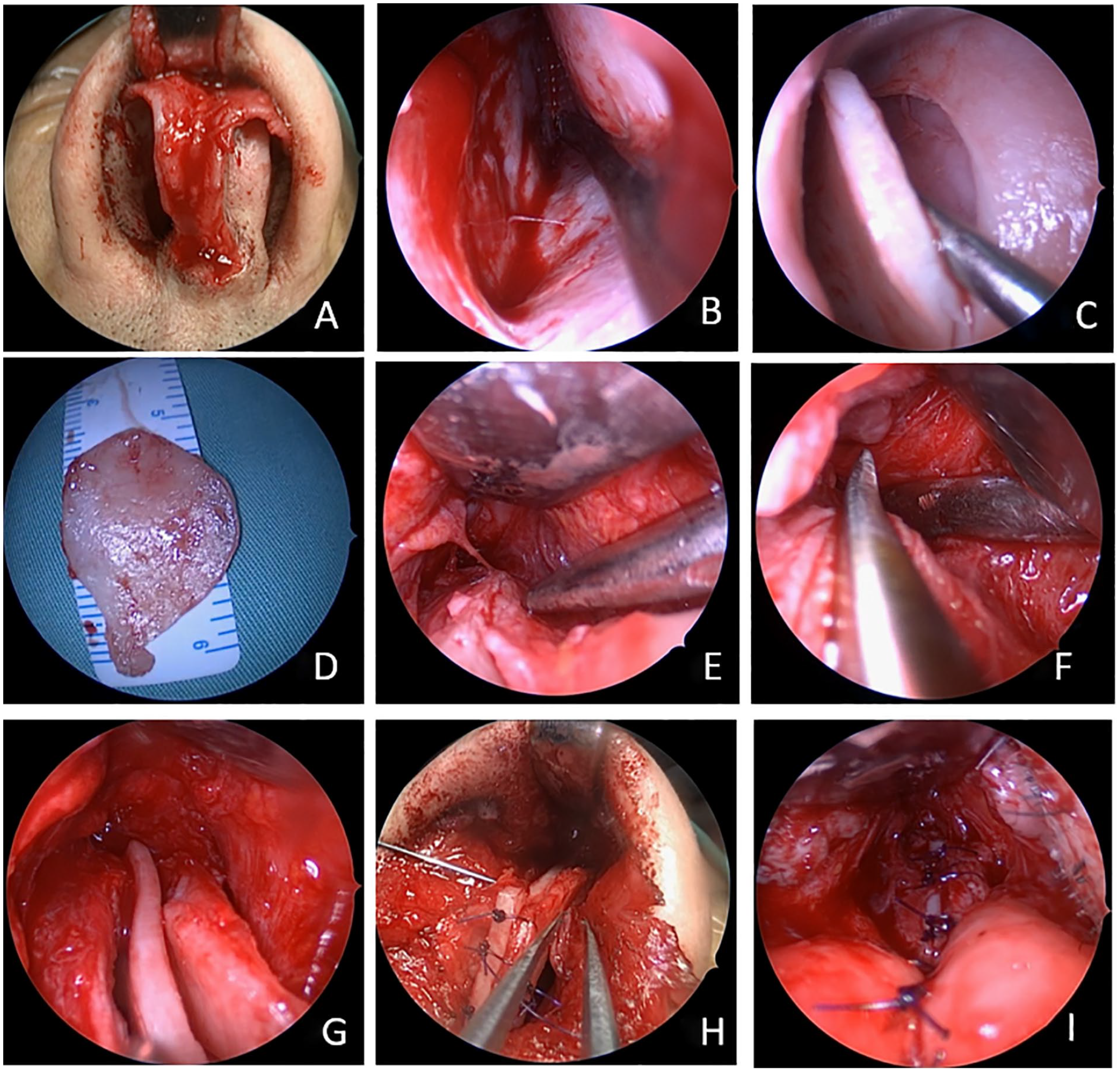
Nasal endoscopy-assisted functional rhinoplasty. (A) Endoscopy-assisted external nasal approach. (B) Nasal endoscopic separation of nasal septum cartilage. (C, D) Preservation of L-shaped stent under nasal endoscopy to remove nasal septum cartilage. (E, F) Nasal endoscopy-assisted osteotomy. (G, H, I) Implantation of dorsal and caudal graft.
Nasal Endoscopic Manipulation
The nasal septum cartilage was separated under nasal endoscopy. The caudal end of the nasal septum was exposed, followed by the junction of the nasal septum cartilage with the vertical plate of the ethmoid bone and the plow bone and the junction of the nasal septum cartilage with the palatal process of the maxilla and the nasal spine of the palate bone. An L-shaped stent that preserves the 10-15 mm at the end and back of the nasal septum was placed to support the back and tip of the nose. The deviated nasal septum cartilage, the vertical plate of the ethmoid bone, the horizontal cartilage strip at the bottom of the nose, and the deviated hyperplastic bone at the bottom of the nose were removed (Figure 2B). The removed cartilage was kept as a spare, and the rest of the nasal septum cartilage was removed to make the graft (Figures 1B and 2C-D).
Treatment of Cartilage Pyramid
The L-shaped stent was trimmed to sharply separate the junction between the upper lateral cartilage and the nasal septum cartilage, and the dorsal graft was sutured and fixed on the dorsal side of the nasal septum and fixed on the raised upper lateral nasal cartilage (Figures 1E and 2G, I). The caudal graft was placed between the medial crus of the pterygoid cartilage and reached the anterior nasal spine (Figures 1F and 2H).
Treatment of Bone Pyramid
According to the deviation of the nasal bone, midline osteotomy and lateral osteotomy were performed to rearrange the skewed nasal bone. The widened nasal bone was pushed inward, the collapsed nasal bone was lifted up, the protruding nasal bone was pressed or ground to the center, and the bridge of the nose was straightened (Figure 1C, 1D and 2E-F).
For those with severe deviation of the caudal end of the nasal septum, the anterior septal angle was entered, the fibrous connections and ligaments around the anterior nasal spine were dissected, the maxillary crest and the base of the nose were exposed, and the caudal end of the nasal septum was completely exposed. Depending on the deviation, wedge resection or septal shortening was performed to release cartilage tension, repositioned to the midline and sutured to the anterior nasal spine. The residual nasal septal cartilage was used to prepare cartilage particles to fill the depression at the back or tip of the nose.
The hypertrophic middle and inferior turbinates underwent selective fracture medial and lateral displacement or submucosal partial bone resection under nasal endoscopy.
Statistical Analysis
The measurement data before and after operation were expressed as
Results
Clinical Data
Among the 28 patients with crooked nose, 6 were congenital and 22 were acquired. Seven cases were oblique type (type I), 16 cases were sunken type (type C), and 5 cases were protruding type (type S). All patients were followed up for 6-41 months (mean 15.2 months). Among them, endoscopic submucosal resection of the middle turbinate was performed in 8 cases (11 sides), internal displacement of bilateral middle turbinate fracture was performed in the rest, submucosal partial resection of inferior turbinate was performed in 21 cases (28 sides), and external displacement of inferior turbinate fracture was performed in the rest. In terms of the type of deviation of the nasal septum in this group of cases, 25 (89.3%) patients had evidence of a bony deviation, and 23 (82.1%) patients had a cartilaginous deviation with 20 (71.4%) having both bony and cartilaginous deviations. Anterior and posterior septal deviations were noted in 6 (21.4%) and 9 (32.1%) of the patients, respectively, with 13 (46.4%) patients having both anterior and posterior deviations.
Septal deviations were classified as degree I when the deviation did not reach the lower nasal turbinate, degree II when the deviation reached the lower nasal turbinate, or degree III when the deviation reached the lateral wall and compressed the lower nasal turbinate. This work involved 1 case of degree I, 11 cases of degree II, and 16 cases of degree III. All operations were completed successfully. One patient developed nasal septum hematoma, which improved after debridement and dressing change, and 4 patients developed hypoesthesia and swelling at the tip of the nose, which were relieved within 1-6 months after operation. No complications, such as nasal septum perforation, nasal adhesion, and nasal dorsal collapse, were noted.
Comparison of Nasal Ventilation Function Before and After Operation
The subjective VAS and NOSE scores at 6 months after operation were significantly lower than those before operation (1.96 ± 0.84 vs 6.68 ± 1.28, 4.25 ± 1.80 vs 12.25 ± 2.50; t = 18.765, 16.870; P < .05). Compared with those before operation, NV5, MCA1, and MCA2 increased remarkably, whereas RT, MCA1a/MCA1b, MCA2a/MCA2b, MD1a/MD1b, and MD2a/MD2b decreased considerably (Table 1). No remarkable differences in MD1 and MD2 were found before and after operation. MCA1 was located about 2 cm of the anterior nostril, that is, the nasal threshold and the front of the inferior turbinate, and MCA2 was located 2-5 cm away from the anterior nostril, that is, the area corresponding to the front edge of the middle turbinate.
Comparison of objective indexes of nasal ventilation before operation and 6 months after operation.
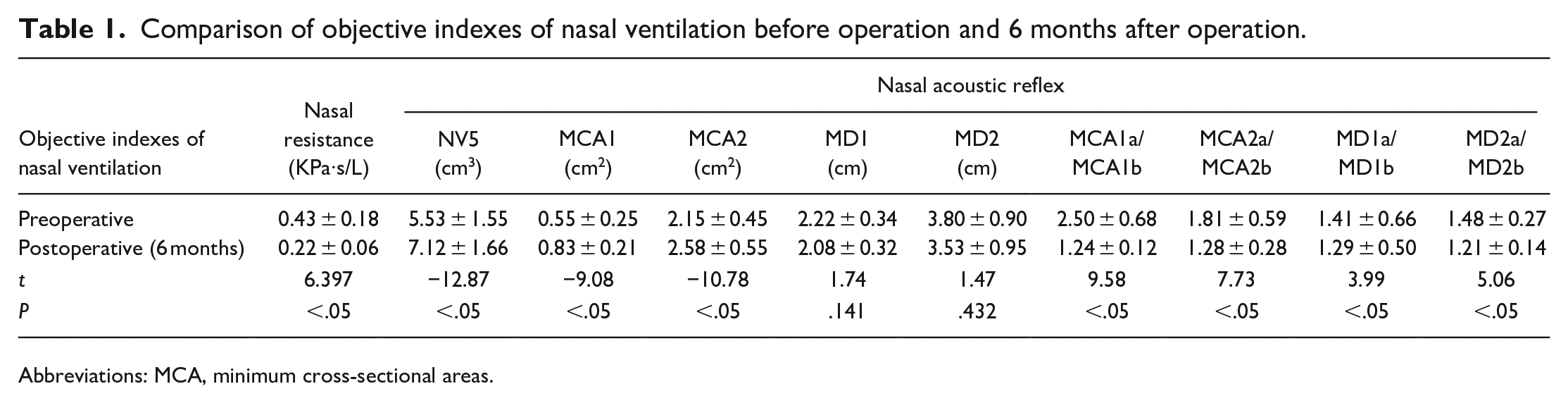
Abbreviations: MCA, minimum cross-sectional areas.
Comparison of Nasal Appearance Evaluation of Patients Before and After Operation
At 6 months after operation, ROE score was significantly higher than that before operation (16.93 ± 2.61 vs 10.64 ± 3.01, t = −12.821, P < .05). The deviation value of nasal appearance decreased significantly (1.46 ± 1.11 mm vs 5.72 ± 2.30 mm, t = 15.806, P < .05).
Among the 28 patients, 14 cases had mild crooked nose, 11 cases had moderate crooked nose, 3 cases had severe crooked nose before operation. Moreover, 23 cases had normal nose and 5 cases had mild deviation after operation. The cure rate was 82% (23/28), and the effective rate was 100% (28/28). The deviation of the nasal septum was corrected in all patients. Nasal endoscopy showed that the nasal septum was basically in the middle, and the nasal endoscope could enter the posterior nostril smoothly. The nasal alar angle was significantly reduced after operation, and no statistical difference was found in the rest of the external nasal morphology before and after operation (Table 2).
Comparison of objective evaluation of nasal appearance before and after operation.
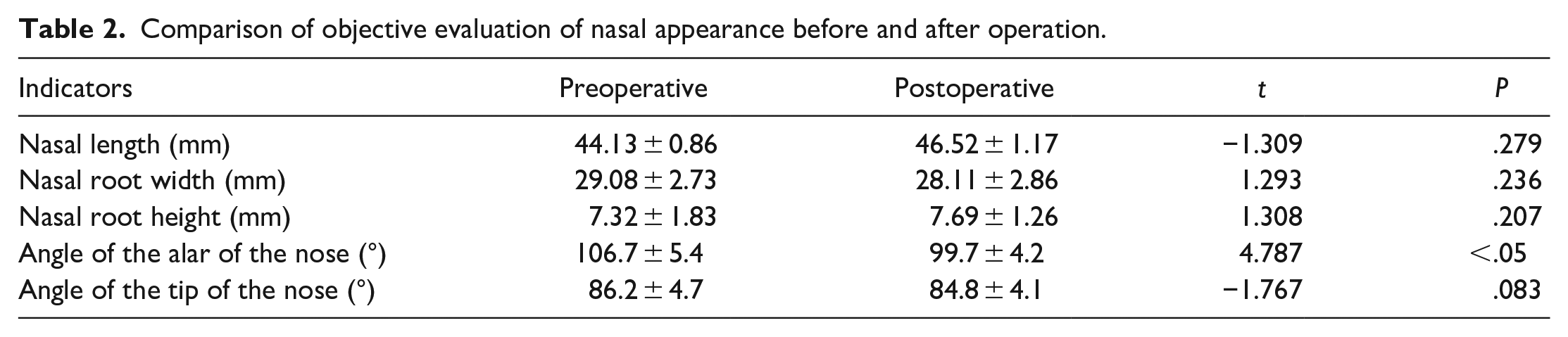
In terms of postoperative satisfaction, 26 cases (92.9%) were very satisfied and 2 cases (7.1%) were satisfied with nasal ventilation function. Moreover, 24 cases (85.7%) were very satisfied and 4 cases (14.3%) were satisfied with nasal appearance after operation. There are no dissatisfied patients (Figure 3 and 4).
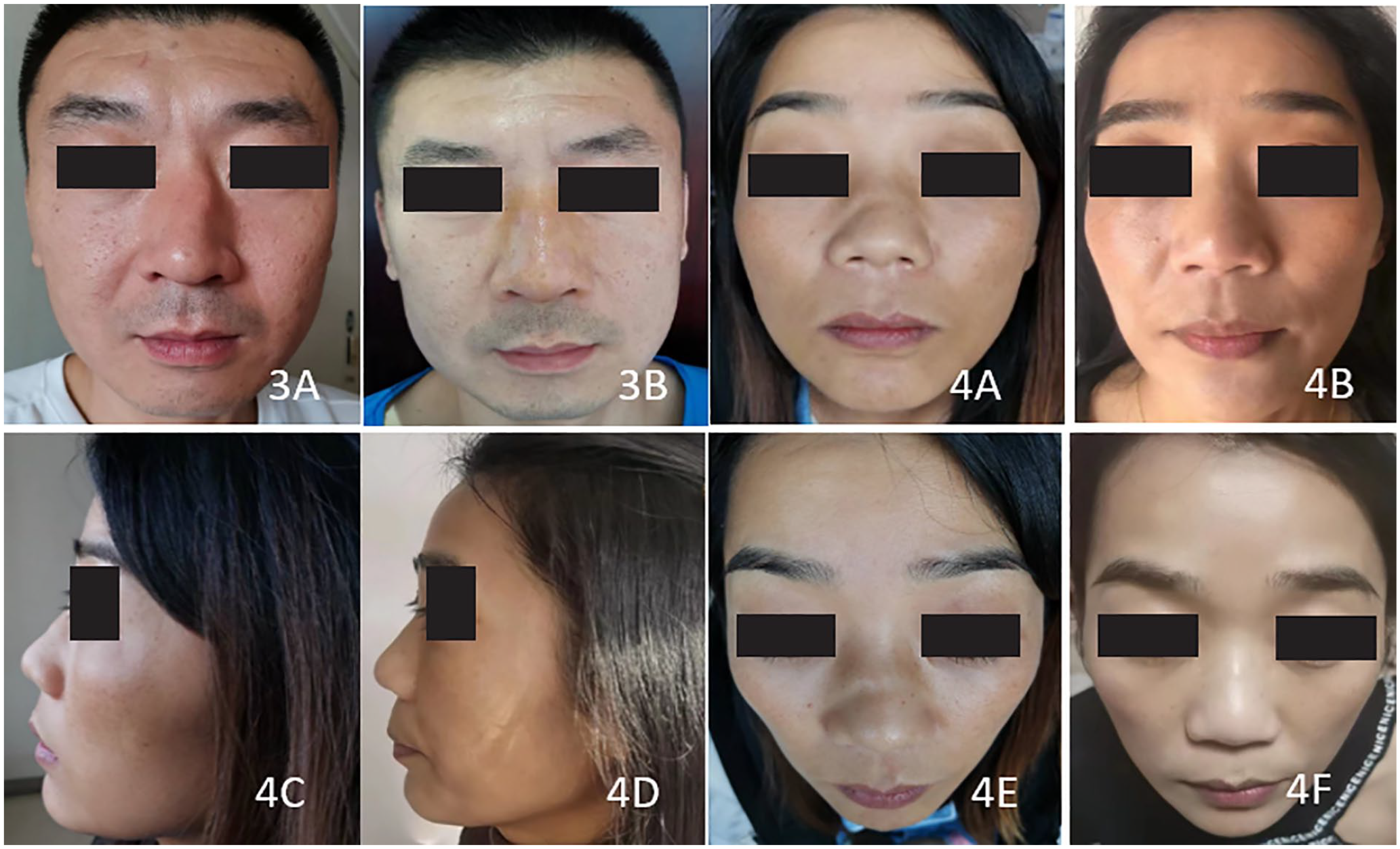
An example of the appearance of functional rhinoplasty patients assisted by nasal endoscope. 3(A), 4(A), 4(C), 4(E): Preoperative views of a patient. 3(B), 4(B), 4(D), 4(F): Postoperative views of the patient after 3 months.
Discussion
Some scholars1,8 have proposed functional rhinoplasty. The core is to adjust the nasal frame structure to correct external nasal deformities and structural abnormalities in the nasal cavity, taking into account nasal cosmetology and ventilation function. Nasal endoscopy can realize visual operation and provide a clear visual field of operation. It can be used in functional rhinoplasty to make the operation more precise, accurate, and minimally invasive.
Endoscopic assistance can make up for the lack of exposure caused by the sheltering of the surgical field caused by pulling tissue. It is especially suitable for the subperiosteal separation of nasal bone, correction of nasal septum and osteotomy and middle and inferior turbinate plasty, where the surgical area is difficult to see directly with the naked eye. After the application of endoscopy, the external nasal incision can be reduced. Some unnecessary separation can be avoided to lessen injury. Moreover, the bony process of the nasal bone can be better removed, and the sunken part can be corrected. 9 Park et al compared traditional rhinoplasty with endoscopic rhinoplasty. Their results showed that endoscopic rhinoplasty has a longer operation time and higher operation cost than traditional rhinoplasty, but the satisfaction rate of patients is higher and the recurrence rate is lower with endoscopic rhinoplasty than with traditional rhinoplasty. 10 Notably, more nasal endoscopic aids have been used in the open approach, making the endoscopy-assisted operation smoother. 11
Functional endoscopic sinus surgery simultaneous rhinoplasty has been considered a safe and effective operation and does not increase the incidence of complications.12,13 It avoids the pain of reoperation and the waste of medical resources and uses the corrected nasal septum cartilage to make grafts, which can avoid the trauma of bone removal in other parts of the body or the rejection of artificial filling materials. In addition, endoscope-assisted functional rhinoplasty can perform fine turbinoplasty for the hyperplastic turbinate bone or concha bullosa, whereas the lack of nasal endoscope-assisted traditional surgery or external displacement of the inferior turbinate fracture may not be able to alleviate the nasal ventilation function of patients.
In this study, the subjective VAS and NOSE scores were considerably lower after the operation than before the operation. In objective examination, MCA1, MCA2, and V5 were remarkably increased; and RT decreased considerably. The results showed that the nasal cavity widened obviously, the nasal resistance decreased, and the ventilation increased after the operation. Previous studies found that single-index MCA, MD, NV5, and RT are not effective in testing nasal ventilation function and cannot well reflect the structural differences of bilateral nasal cavities. 14 The symmetry between nasal passages on both sides or the balance of airflow is an important prerequisite for normal nasal ventilation.15,16 Therefore, we analyzed the structural difference of the bilateral nasal cavity. We found that the MD1 and MD2 values after operation were lower than those before operation, but the difference was not statistically remarkable. However, the ratios of MCA1a/MCA1b, MCA2a/MCA2b, MD1a/MD1b, and MD2a/MD2b were substantially lower after the operation than before the operation, and the differences were statistically substantial. The results show that the operation effectively restored the symmetry of the structure of the bilateral nasal cavity, rather than blindly expanding the airway of one side of the nasal cavity. The restoration of symmetry marks the effective correction of the abnormal structure of the nasal cavity. On the whole, the subjective and objective evaluations tended to be consistent and showed that the operation effectively improved the nasal ventilation function. The results show that nasal endoscopy-assisted functional rhinoplasty can combine endoscopic rhinoplasty with open rhinoplasty and effectively restore nasal ventilation function.
In this study, we used ROE scale nasal appearance deviation value and morphological measurement of external nose to evaluate the external nasal morphology, subjectively and objectively. The ROE score increased substantially, and the nasal appearance deviation decreased remarkably. Although no statistical difference was found in many external nasal morphological measurements in this group, the nasal length and nasal depth increased after the operation. Moreover, the nasal alar angle after the operation was significantly smaller than that before the operation. Thus, surgery was found to improve the morphology of the external nose.
In the evaluation of postoperative satisfaction, the overall satisfaction was higher, but the satisfaction of nasal ventilation function was higher than that of nasal appearance. Our analysis may be related to the fact that rhinologists pay more attention to the correction of abnormal nasal structure under nasal endoscopy and pay more attention to the treatment of nasal ventilation function.
The fact that only one surgeon performed all surgeries may add to the consistency of the performed procedures, possibly reducing additional bias resulting from a variety of surgical techniques, personal influences, and perioperative management.
Although nasal endoscopy has many advantages, it still has some limitations in practical operation. (1) Endoscopic observation has difficulty of control the shape of the nose as a whole, lacks a 3D sense and may lead to misjudgment during operation. (2) In a relatively narrow operating space, endoscopes are easily contaminated, requiring assistants to constantly rinse the surgical fields and lenses. (3) Suturing the corrected crooked nose is usually more convenient under direct vision. (4) During repeated operation of the nasal endoscope, secretions in the nasal cavity or dirt outside the nose may enter the incision and cause infection.
This study still has many shortcomings, such as the relatively few cases included, the absence of a comparative study on patients undergoing functional rhinoplasty in the same period. The long-term effect of nasal endoscopy-assisted functional rhinoplasty needs to be further observed.
Conclusions
In summary, the application of nasal endoscopy in functional rhinoplasty realizes the visual operation and makes the operation more precise and minimally invasive. Nasal endoscopy-assisted functional rhinoplasty is worthy of continuous improvement and development in clinical practice in the future to improve its clinical effect.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Ethical approval to report this case was obtained from the Institutional Review Board of Qilu Hospital of Shandong University (Qingdao). All the clinical treatments detailed in the manuscript have been conducted in accordance with the Declaration of Helsinki and its later amendments or comparable ethical standards.
Informed Consent
Written informed consent was obtained from the patient for her anonymized information to be published in this article.
Data Available on Request From the Authors
The data that support the findings of this study are available from the corresponding author, upon reasonable request.
