Abstract
Thyroglossal duct cyst carcinoma (TGDCCa) is a rare condition with only approximately 300 cases reported to date. There is a lack of comprehensive reporting on its clinical manifestations, ultrasound, contrast-enhanced computed tomography, magnetic resonance imaging (MRI) features, immunophenotyping, procedure, and prognosis following modified Sistrunk’s procedure. This study aimed to address these gaps by analyzing and summarizing the clinical features of 5 cases of papillary carcinoma arising in thyroglossal duct cysts (TGDC).
Five patients with papillary carcinoma in TGDC treated by modified Sistrunk’s procedure were included. Their clinical manifestation, physical examination findings, iconography, pathological findings, treatment, and outcomes were analyzed in aiding the diagnosis and treatment of TGDCCa. Immunohistochemistry was used to confirm the papillary carcinoma subtype. The BRAFV600E mutation was detected in 2 patients. No evidence of cancer recurrence, distant metastases, and malignant changes in the thyroid was found after a mean follow-up of 29.8 months.
The management of TGDCCa with papillary carcinoma in low-risk patients can be accomplished by performing a modified Sistrunk’s procedure along with a regular follow-up imaging of the thyroid and neck. Although postoperative pathological diagnosis is the gold standard for diagnosis, it is equally crucial to comprehend the clinical manifestations and auxiliary diagnostic techniques before surgical intervention.
Keywords
Core Tip
1. Ultrasound revealed mixed echoic mass with microcalcification in all patients.
2. Contrast-enhanced computed tomography showed heterogeneous cystic lesions in the neck at the hyoid and infrahyoid levels.
3. Magnetic resonance imaging showed a cyst in the center of the upper part of the neck. The solid part was slightly enhanced in the enhanced scan.
4. Immunohistochemistry indicated that the tumor specimens were positive for thyroglobulin, cytokeratin 19, thyroid transcription factor 1, galectin-3, and Hector Battifora mesothelial antigen 1.
5. Thyroglossal duct cyst carcinoma with papillary carcinoma in low-risk patients can be successfully managed by a modified Sistrunk’s procedure with regular and timely follow-up.
Introduction
Thyroglossal duct cyst (TGDC) is a frequently occurring midline neck mass of congenital origin and is typically benign. However, thyroglossal duct cyst carcinoma (TGDCCa) is extremely rare and fewer than 300 cases have been reported in the English literature since the first report in 1911.1,2 Approximately 1% of TGDC cases develop into different types of TGDCCa.2,3 More than 90% of TGDCCa cases are papillary carcinomas, and the rest are squamous cell carcinomas or Hürthle cell, follicular, or anaplastic carcinomas.2,4 Since TGDC and TGDCCa share similar clinical manifestations, such as an asymptomatic anterior neck mass near the hyoid bone, distinguishing between TGDC and TGDCCa can be challenging without pathology results following surgical excision.
Various imaging and diagnostic techniques, including ultrasound (US), contrast-enhanced computed tomography (CECT), magnetic resonance imaging (MRI), and fine-needle aspiration cytology are commonly used for the preoperative diagnosis and differential diagnosis between TGDC and TGDCCa.5,6 Among these, US is the most commonly used method in the outpatient setting. 5 Accurate interpretation of the imaging features of these conditions is essential for proper preoperative diagnosis and differentiation between TGDCCa and TGDC.
The optimal management of TGDC with incidentally noted TGDCCa is still a matter of debate. Though modified Sistrunk’s procedure is considered a suitable operation for the treatment of both TGDC and TGDCCa without lymph node metastasis and thyroid malignancy, 6 the need for additional treatments, such as total thyroidectomy, remains controversial, especially for patients with BRAFV600E mutation. 7 To provide further insight into the diagnosis and treatment of TGDCCa, we retrospectively analyzed the medical history and imaging and pathology findings of patients with TGDCCa.
We present the following cases in accordance with the CARE reporting checklist.
Case Presentation
Five patients (3 females and 2 males) with a mean age of 34.2 years were diagnosed with papillary carcinoma following surgical intervention for a painless neck mass. The mean course of the disease was 30.6 months (range 2 months-8 years) (Table 1). All the patients underwent Sistrunk’s procedure for TGDC with no reported complications such as blood vessel or nerve injuries, infections, or bleeding, and the incidence rate of the TGDCCa was 0.84% (5/597).
Clinical Information and Ultrasonic and Pathological Results for the 5 Patients with Thyroglossal Duct Carcinoma in this Study.
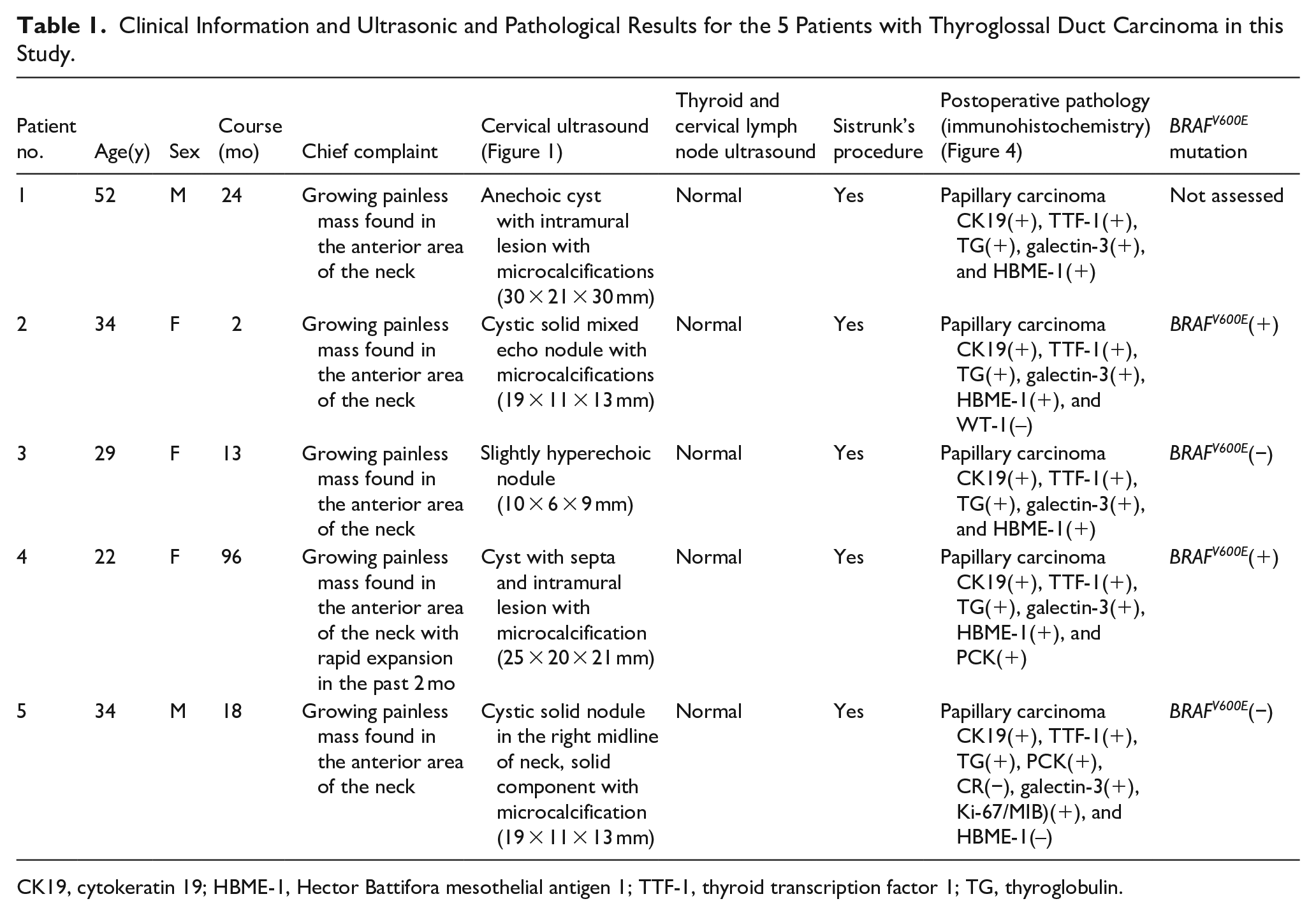
CK19, cytokeratin 19; HBME-1, Hector Battifora mesothelial antigen 1; TTF-1, thyroid transcription factor 1; TG, thyroglobulin.
The imaging test results are shown in Table 1, and Figures 1 and 2. US revealed a mixed echoic mass with microcalcification in all patients (Figure 1), without any evidence of cervical lymph node or thyroid gland involvement. CECT (Figure 2) showed heterogeneous cystic lesions in the neck at the hyoid and infrahyoid levels with slight high-density shadow with calcification in the nodular shadow at the edge of the cyst. The boundary of the cysts was clear with no obvious adhesions to the surrounding tissues. MRI of the neck (Patient 5) showed a cyst measuring 19 × 2.1 cm located in the center of the upper part of the neck (Figure 3) with a slight enhancement of the solid part in the enhanced scan.
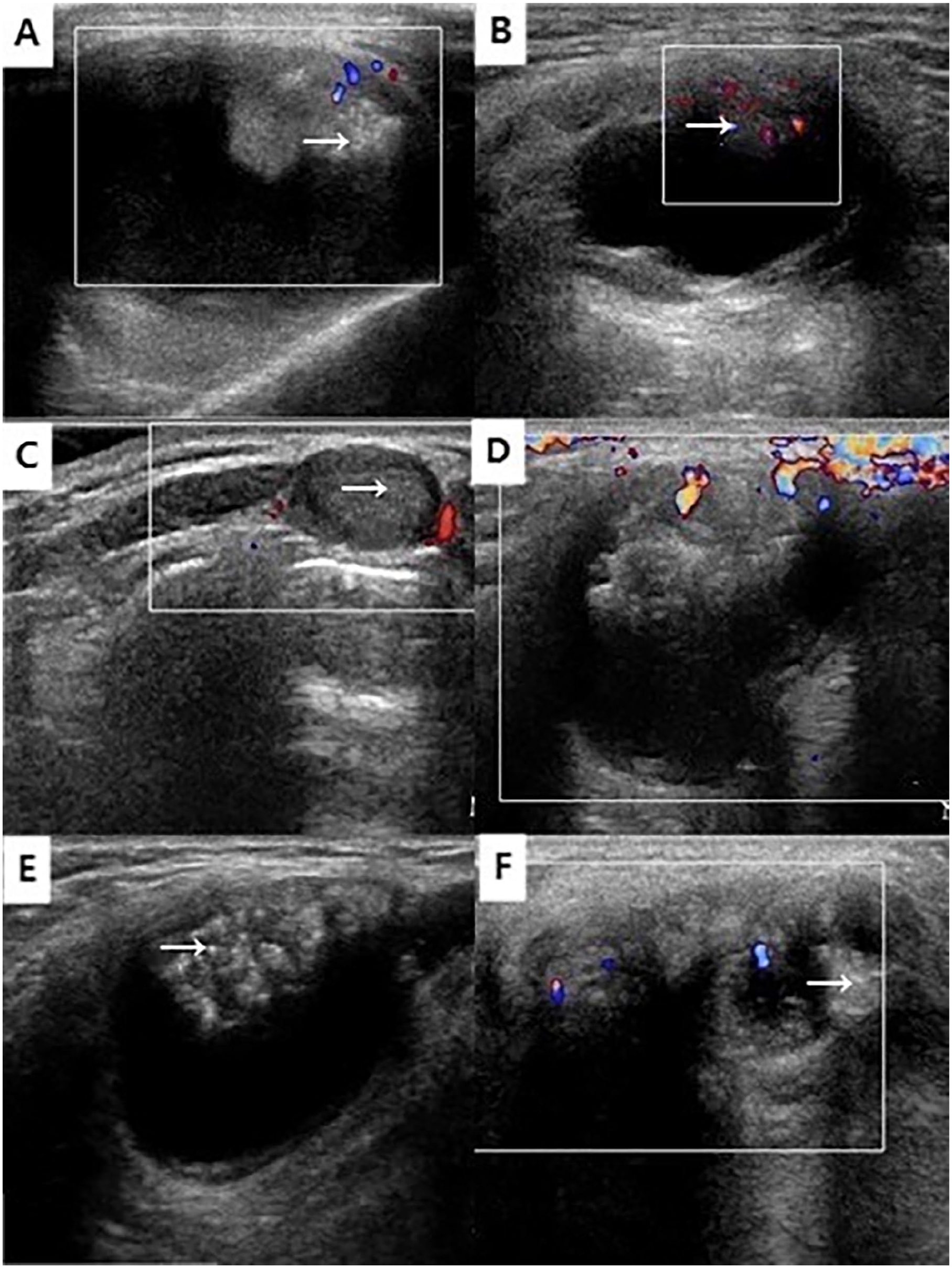
Ultrasound (US) images from patients with thyroglossal duct cyst carcinoma. (A-C, E, and F) are from Patients 1, 2, 3, 4, and 5, respectively, and (D) is a US image of the tumor blood flow signal in Patient 4. US images show that the masses observed in the 5 patients were cystic and solid, mixed-echogenic tumors with clear boundaries and a regular shape. Punctate strong echo can be seen in the solid components in the capsule (white→). Punctate blood flow signals were detected in the tumors and adjacent capsule wall.
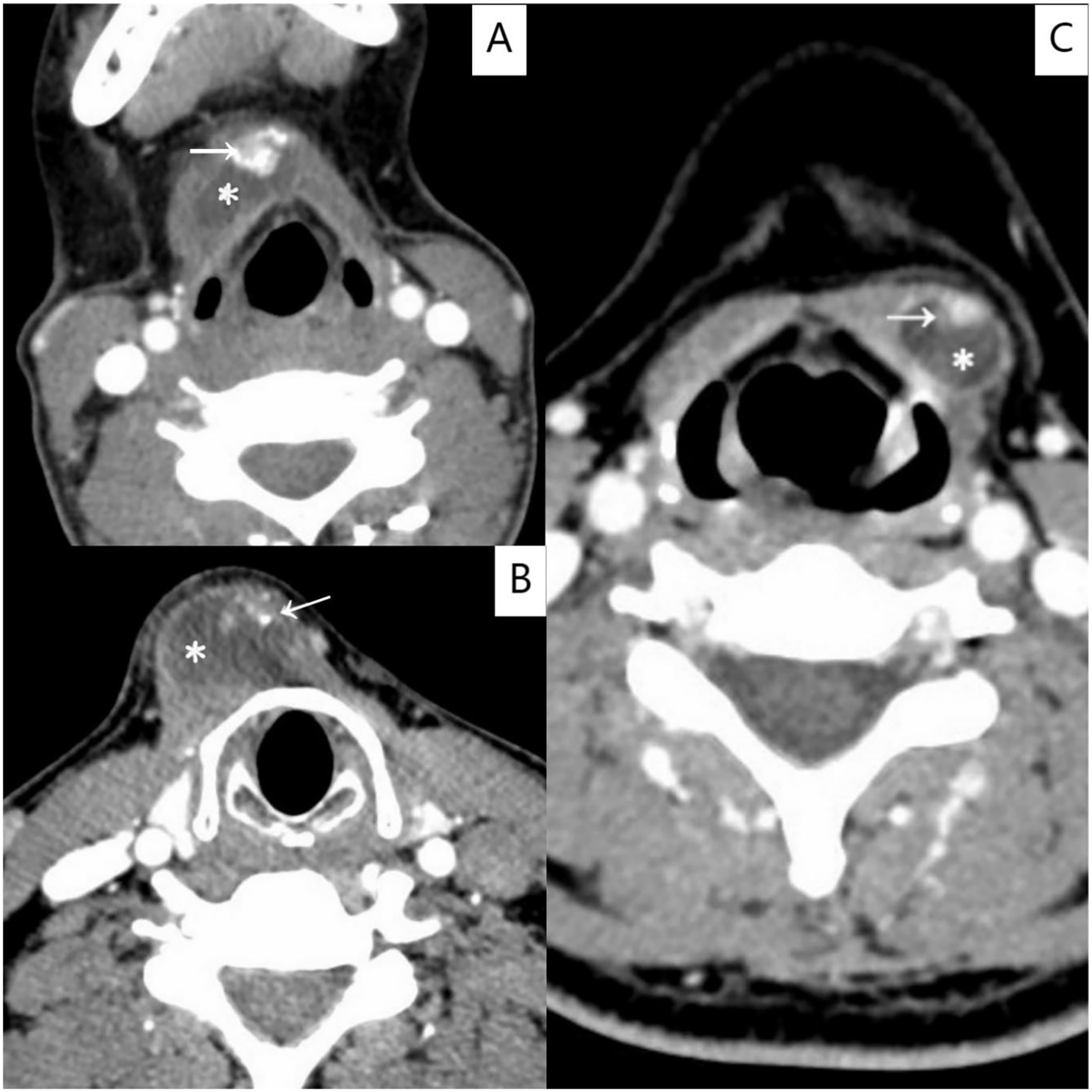
The main features observed with contrast-enhanced computed tomography (CECT) of the neck of Patients 1 (A), 2 (B), and 3 (C). The neck CECT shows cystic masses with homogeneous low density and clear edges (*). The CECT also shows that the capsule and part of the capsule wall are slightly enhanced with focal calcifications (white→).
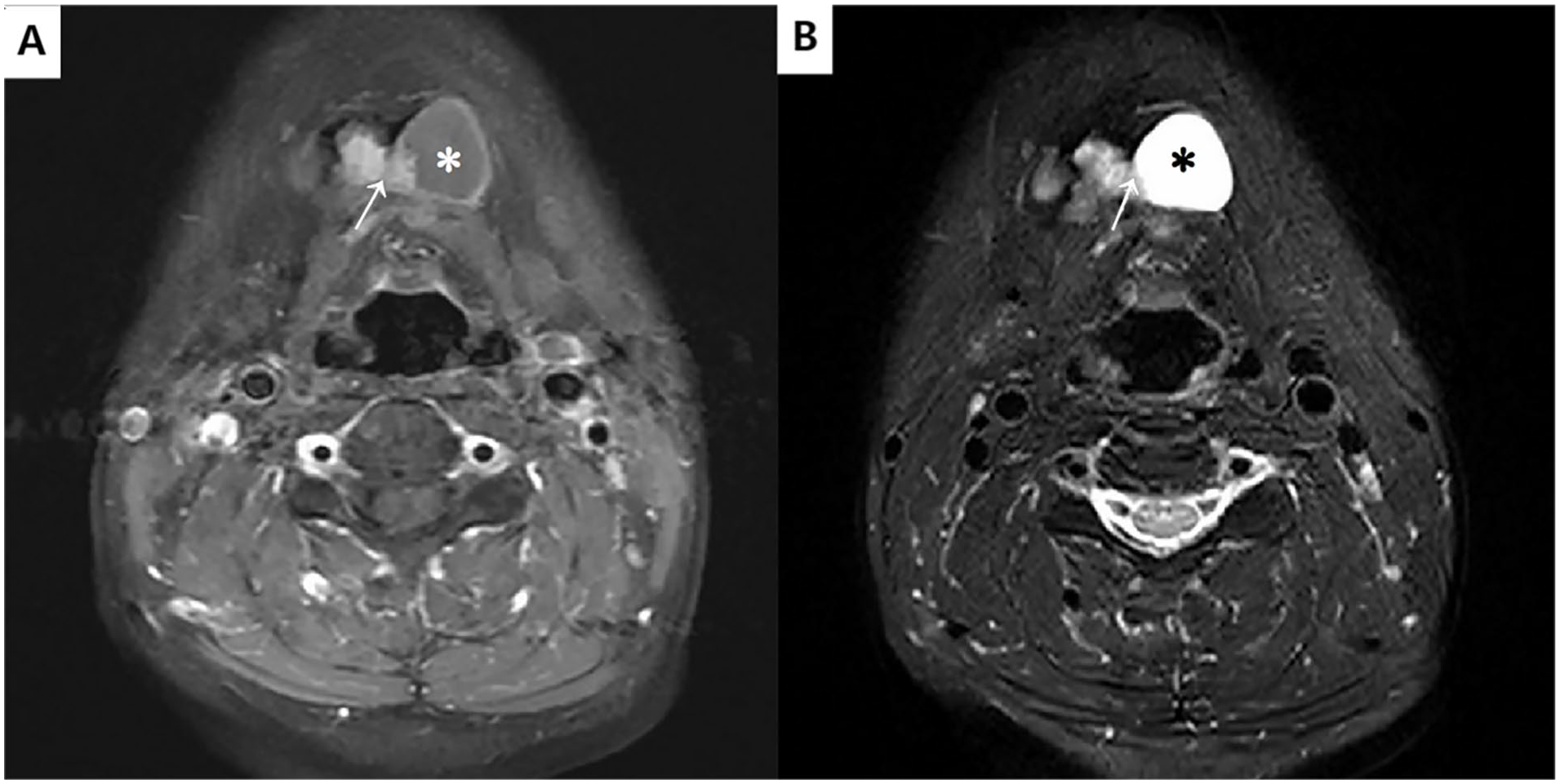
Neck magnetic resonance imaging of Patient 5 shows a cystic component measuring about 19 × 2.1 cm. The lesion showed a hypointense signal in the T1-weighted (A) image (white *) and a hyperintense signal in the T2-weighted (B) image (black *). The solid part is significantly enhanced. The solid nodule at the cyst margin appears hypointense on the T2-weighted image with calcification and appears intermediate on the T1-weighted image (white→).
The immunohistochemistry results confirmed the diagnosis of papillary carcinoma, which was positive for several markers, including thyroglobulin (TG), cytokeratin 19 (CK19), thyroid transcription factor 1 (TTF-1), galectin-3, and Hector Battifora mesothelial antigen 1 (HBME-1) (Figure 4). HBME-1 was positive in 4 patients. The BRAFV600E mutation was detected in Patients 2 and 4 (Table 1).
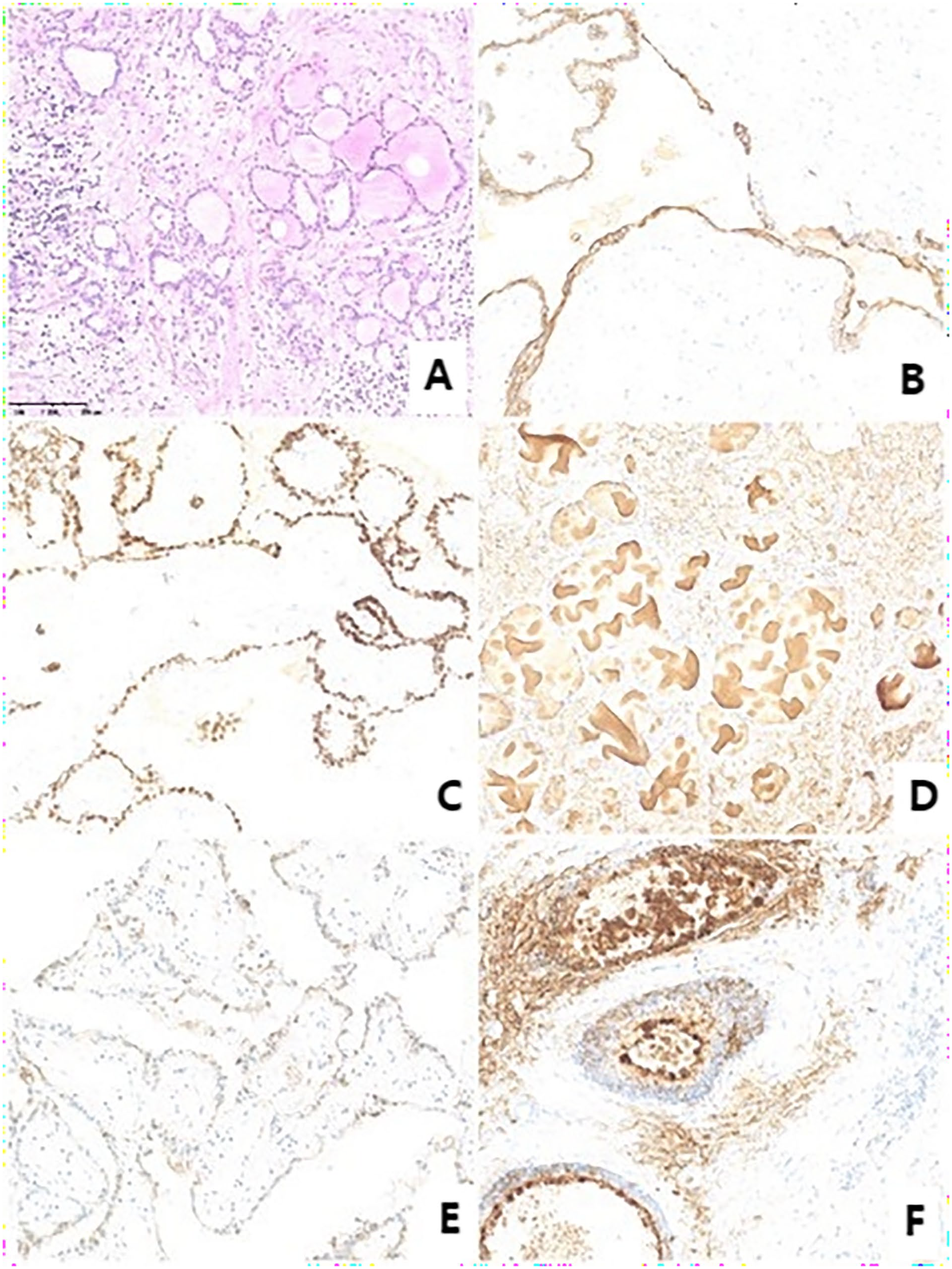
Images of the neck tumor from Patient 2. A shows hematoxylin-eosin staining (×20). B-F show immunohistochemical staining for cytokeratin 19, thyroid transcription factor 1, thyroglobulin, galectin-3, and Hector Battifora mesothelial antigen 1.
After a mean follow-up of 29.8 months (range 11-78 months), the patients showed no evidence of cancer recurrence, distant metastases, or malignant changes in the thyroid or lymph nodes.
The study was approved by the Ethics Committee of the West China Hospital of Sichuan University (No. 2019-357).
Discussion
US is the preferred imaging modality for its simplicity, rapidity, and low cost, while also avoiding radiation exposure. US can highlight suspicious features of a carcinoma such as calcification and abnormal blood flow pattern. 5 In the case of TGDC, US typically reveals either a well-circumscribed, anechoic cyst or a pseudo-solid mass due to proteinaceous fluid content. However, TGDCCa may appear as a cystic mass with a solid component on the wall, occasionally with microcalcification, or as a tumor invading the cyst wall.5,8 US results from all 5 patients in our study showed microcalcification in the capsule of a well-circumscribed cyst. Hypoechoic solid nodules with microcalcification, appearing as sonographic features suggestive of malignancy, were also observed. We also detected blood flow signals in the solid part of the cystic mass in all patients. The presence of a solid component with vascularization should raise suspicion of possible malignancy. 9 US should be performed in every patient to evaluate midline cystic mass, thyroid gland, and cervical lymph nodes. 9
Auxiliary examinations such as CECT and MRI are frequently used in the diagnosis of TGDC and TGDCCa. 2 They play a crucial role in preoperative diagnosis and staging of malignancy by revealing neck masses with invasive characteristics. CECT shows a heterogeneous tumor with a mixed (solid and cystic) composition that is typically located at the hyoid and infrahyoid level near the midline neck, with central hypoattenuation and peripheral enhancement accompanied by small calcification. 10 MRI can efficiently identify cysts in the neck appearing as irregular, solid nodules. The cystic component appears hypointense on T1-weighted images and hyperintense on T2-weighted images, while the solid component appears heterogeneous and is significantly enhanced. The solid nodule at the margin of the cyst appears hypointense on T2-weighted images with calcification and has intermediate intensity on T1-weighted images. 10 Five patients in this study had CECT and MRI findings that were consistent with the tumor morphology reported in the previous literature. 10 CECT and MRI are useful in evaluating abnormal hyperplasia and the vascular shadow of the tumor and foreign body, as well as in determining whether the tumor adheres to the surrounding tissue.
Moreno and Wang 11 used fluorodeoxyglucose positron emission tomography/CT to evaluate the extent of malignant infiltration in TGDCCa. In addition, US, CECT, and MRI can be combined to assist in the distinction between the differentials of TGDC, such as branchial cleft cyst, lipoma, metastatic thyroid carcinoma, dermoid cyst, sebaceous cyst, and enlarged lymph node papillary carcinoma arising from the tip of the pyramidal lobe.
Pathological results remain the gold standard for the diagnosis of TGDCCa. The definitive management of TGDCCa is Sistrunk’s procedure. 12 Whether total thyroidectomy, neck dissection, and postoperative radioactive iodine ablation therapy are necessary for treating papillary carcinoma in a thyroglossal cyst without lymph node metastasis and thyroid malignancy remains uncertain. 13 TGDCs are the most common thyroid developmental anomaly and TGDCCa is a malignant tumor related to the thyroid. 14 Papillary carcinoma accounts for over 90% of TGDCCa cases.2,4 All 5 patients in this study were diagnosed with papillary carcinoma with the immunophenotype of TG(+), TTF-1(+), CK19(+), and galectin-3(+). Some researchers suggested that after modified Sistrunk’s procedure, total thyroidectomy and/or postoperative radioactive iodine ablation therapy are necessary. 9 However, Kermani et al 15 and Carter et al 16 found that total thyroidectomy had no significant effect on overall survival. Srivanitchapoom recommended that these surgical extensions should not be applied routinely to all patients with TGDCCa. 5 Kuzu et al 17 suggested that Sistrunk surgery alone would be sufficient when the cyst wall is well circumscribed, with no tumor invasion outside the cyst wall, no lymph node metastasis, and if the tumor originated primarily from the cyst floor. Lancini et al 18 suggested that risk should be stratified into low, moderate, and high depending on the patient’s age, tumor size, presence of thyroid lesions, involvement of the margins, histological features, multifocality, nodal involvement, and cyst wall involvement. Low risk is defined as age <45 years, no history of radiation exposure, tumor size <4 cm, and the absence of soft tissue invasion, distant or lymphatic metastases, and aggressive tumor histology. For low-risk patients, modified Sistrunk’s procedure can be applied without the need for additional total thyroidectomy, neck dissection, and postoperative radioactive iodine ablation therapy. One patient aged >45 years in our study exhibited no malignant changes in the thyroid and no tumor recurrence or distant metastasis were observed after a follow-up period of 78 months. In TGDCCa cases, it may be wise to consider additional interventions only for high-risk patients. 19
In a study, 80% of patients with BRAFV600E-positive lesions had concomitant thyroid involvement, which confirmed the relationship between mutation positivity and locoregional aggressiveness. 19 The BRAFV600E mutation is the most common genetic alteration observed in papillary thyroid carcinoma and has a specificity of almost 100%.9,19 This mutation is associated with aggressive histopathological features such as extrathyroidal infiltration.20,21 Some researchers have suggested that it is possible to determine whether prophylactic total thyroidectomy is necessary by detecting BRAFV600E in TGDCCa tissue. 7 In this study, BRAFV600E mutation testing was performed in 4 out of the 5 patients, and the gene mutation was found in 2 of them. These 2 patients have been followed up regularly since the operation, but no malignant changes in the thyroid have been found. The need for preventive thyroidectomy in patients with this gene mutation, as mentioned by other researchers, 7 is therefore debatable. However, a longer follow-up period and a larger sample size from multiple centers are required to draw a more robust conclusion.
Conclusion
Long-term US follow-up of the thyroid and neck is important after modified Sistrunk’s procedure in patients with low-risk TGDCCa with or without the BRAFV600E mutation. Papillary carcinoma is usually a low-grade malignancy that can be successfully treated and recurrences reduced with careful patient follow-up. We believe that modified Sistrunk’s procedure with regular and timely follow-up is preferable to long-term thyroxine supplementation and the potential postoperative risks such as parathyroid dysfunction. Although postoperative pathological diagnosis is the gold standard for diagnosis, it is also important to understand the clinical manifestations and auxiliary examination techniques before operation.
Footnotes
Author Contributions
Lei Lei contributed to data collection, data analysis and investigation, methodology, and writing original draft. Min Chen contributed to data collection, investigation, and follow-up. Zong-guo Pang contributed to pathological technological work. Lin Ma contributed to medical imaging technology work. Jian Zou and Jifeng Liu are surgeons. Jifeng Liu and NingYing Song contributed equally to this work, they contributed to the project administration, writing,review, and editing.
Availability of Data and Materials
The datasets used and/or analyzed during the current study are available from the corresponding author upon reasonable request.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval and Consent to Participate
Written informed consent was obtained from the patients to participate in this case report. Our study was approved by Biomedical Ethics Committee, West China Hospital, Sichuan University, and the ethics number is 2019 (357).
CARE Checklist (2016) Statement
The authors have read the CARE Checklist (2016), and the article was prepared and revised according to the CARE Checklist (2016).
Publisher’s Note
Lei Lei and Min Chen contributed equally to this work; Jifeng Liu and NingYing Song contributed equally to this work.
