Abstract
Objective
Parotid tumors are rare neoplasms in adults but are exceedingly infrequent in adolescents. We aimed to determine the clinical characteristics and outcomes of parotid tumors in adolescents under 20 years old.
Methods
Between 1999 and 2020, 979 cases of benign parotid tumors and 236 cases of malignant parotid tumors were treated surgically in our department. Of these, 12 benign cases (1.2%) and 9 malignant cases (3.8%) were in adolescents. There were no benign or malignant cases for those aged under 10 years.
Results
Regarding the histological type, all benign tumors were pleomorphic adenomas. About half of malignant tumors were mucoepidermoid carcinomas, and excluding one high-grade case, the grade of malignancy was all low/intermediate. The accuracy of fine-needle aspiration cytology among adolescents showed no significant difference with that of adults. In contrast to adults, adolescent benign tumor cases showed a markedly high rate of pleomorphic adenomas and no postoperative facial nerve palsy. Malignant tumors in adolescents had a different trend than adults; low/intermediate-grade malignancies were common and thus few symptoms/signs of malignancy could be observed. As well, the accuracy of fine-needle aspiration cytology was poor. All cases had a good prognosis and are disease-free survival.
Conclusion
Parotid tumors in adolescents are rare but have several characteristics that are distinct from adults. As long-term observation is required posttreatment in adolescent patients, recurrence in benign pleomorphic adenomas and poor long-term prognosis in malignant tumors, especially for those with low/intermediate-grade malignancy, are more likely to be observed.
Introduction
Around 3–10% of all head and neck tumors occur in children, and about 5% of these are salivary gland tumors.1,2 The majority (60–80%) of pediatric salivary gland tumors are benign and are generally pleomorphic adenomas. 3 Among all pediatric malignancies, .5% are salivary gland tumors. 4 Malignant salivary gland tumors are reported to be more common in children than in adults; the proportion of malignant salivary gland tumors is 25–50% in children compared with 15–25% in adults. 5
Pleomorphic adenomas are known to recur despite their benign nature, with recurrence occurring in 1–4% for superficial parotidectomy and 40–50% for enucleations. 6 Recurrent pleomorphic adenoma occurs a mean of 7 to 10 years after initial surgery, and long-term observation is required in pediatric cases. As such, the importance of definitive removal of the tumor has more relevance than in adults. 7 Additionally, long-term observation cases are reported to have a higher risk of malignant transformation of pleomorphic adenomas. 8 On the other hand, malignant tumors in children tend to have a lower grade of malignancy than in adults, with low/intermediate grades being the most common. 9 The long-term prognosis is important for low/intermediate-grade malignant tumors because of the long time to recurrence. As long-term prognosis needs to be considered in children and adolescents, this leads to the issue of whether the intensity of treatment should be the same as in adults. In adults, postoperative radiotherapy is generally performed for advanced cancer and high-grade malignancies, but indications for adjuvant radiation treatment remain unclear for pediatric cases.
Thus, parotid tumors in children have somewhat distinct characteristics from those in their adult counterparts. Due to its low incidence, the accumulation of cases requires a long time. Reaching an accurate conclusion is also challenging unless the diagnosis and treatment strategies are consistent over the collection period. In our department, 979 cases of benign parotid tumors and 236 cases of malignant parotid tumors were treated in the past 21 years, and the diagnosis and treatment strategies have been consistent over this period. Here, we categorized patients under 20 years old as adolescents and examined their clinical characteristics to discuss issues that exist in pediatric cases.
Materials and Methods
Patients
Histological type of benign and malignant tumors (adults and adolescents) in the study population
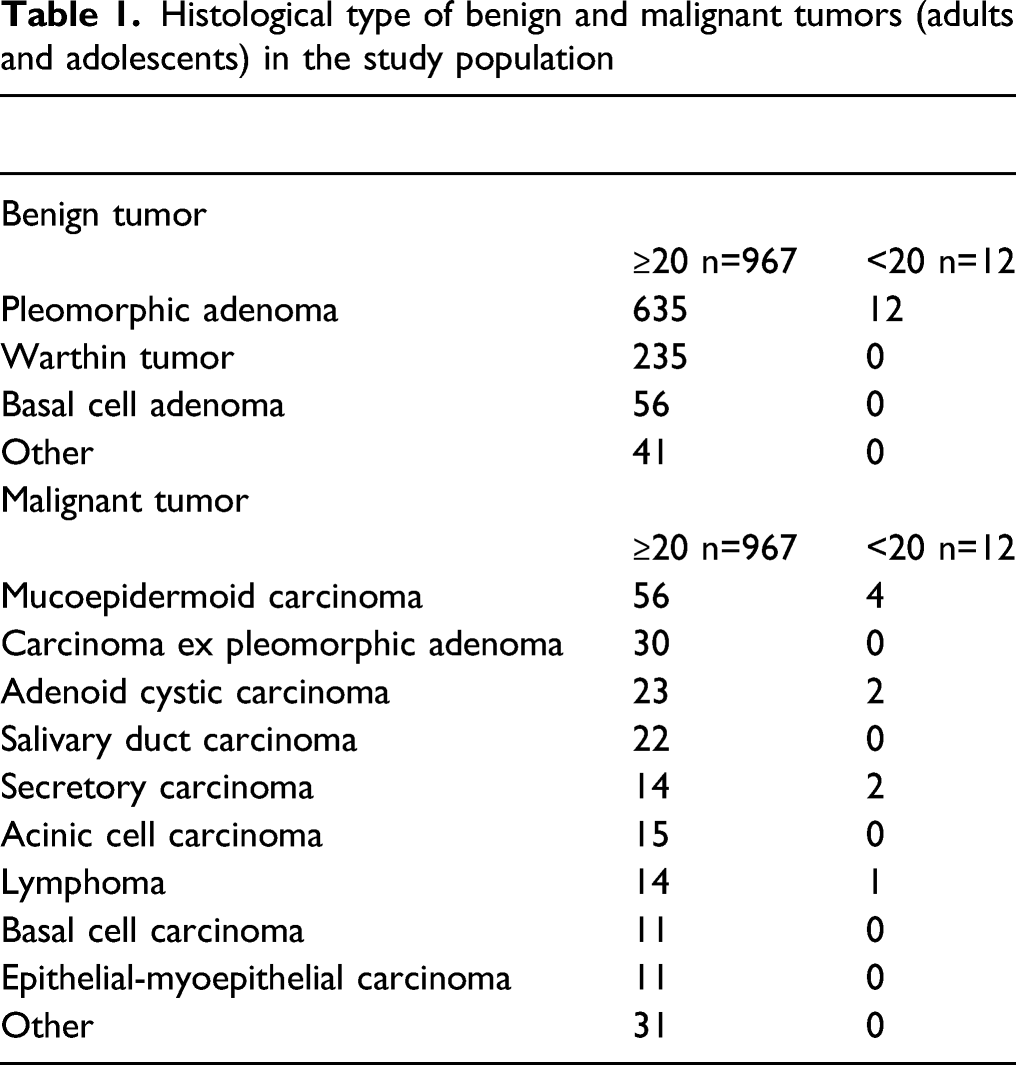
Methods
Benign and malignant tumors were compared in adolescents and adults. For benign tumors, we assessed age, sex, tumor diameter, tumor location, symptoms/signs, surgery, and postoperative facial nerve palsy in adolescent and adult patients. For malignant tumors, we assessed age, sex, symptoms/signs, grade of malignancy, preservation/sacrifice of facial nerves, lymph node metastasis, and outcome in adolescent and adult patients.
Fine-needle aspiration cytology (FNAC) was performed preoperatively, and the results were classified according to the Osaka Medical College (OMC) system. 10 The OMC system classifies cytology results into 11 categories: the FNAC diagnosis (ie, OMC System) was evaluated in 979 benign tumors and 236 malignant tumors, and they were compared between adolescents and adults. Patient background, symptoms, pathology, treatment, and outcomes were examined for adolescent tumor cases for both benign tumors (12 cases) and malignant tumors (9 cases).
Statistical Analysis
The Mann–Whitney U test was used to compare differences between the 2 groups (adults and adolescents) because the following variables did not show a normal distribution: sex, tumor diameter, tumor location, symptoms/signs, operation time, bleeding volume, grade of malignancy, preservation/sacrifice of facial nerves, lymph node metastasis, and outcome. For all analyses, P <.05 was considered statistically significant.
Results
Comparison of Adolescent and Adult Cases
Patient demographics and presentation
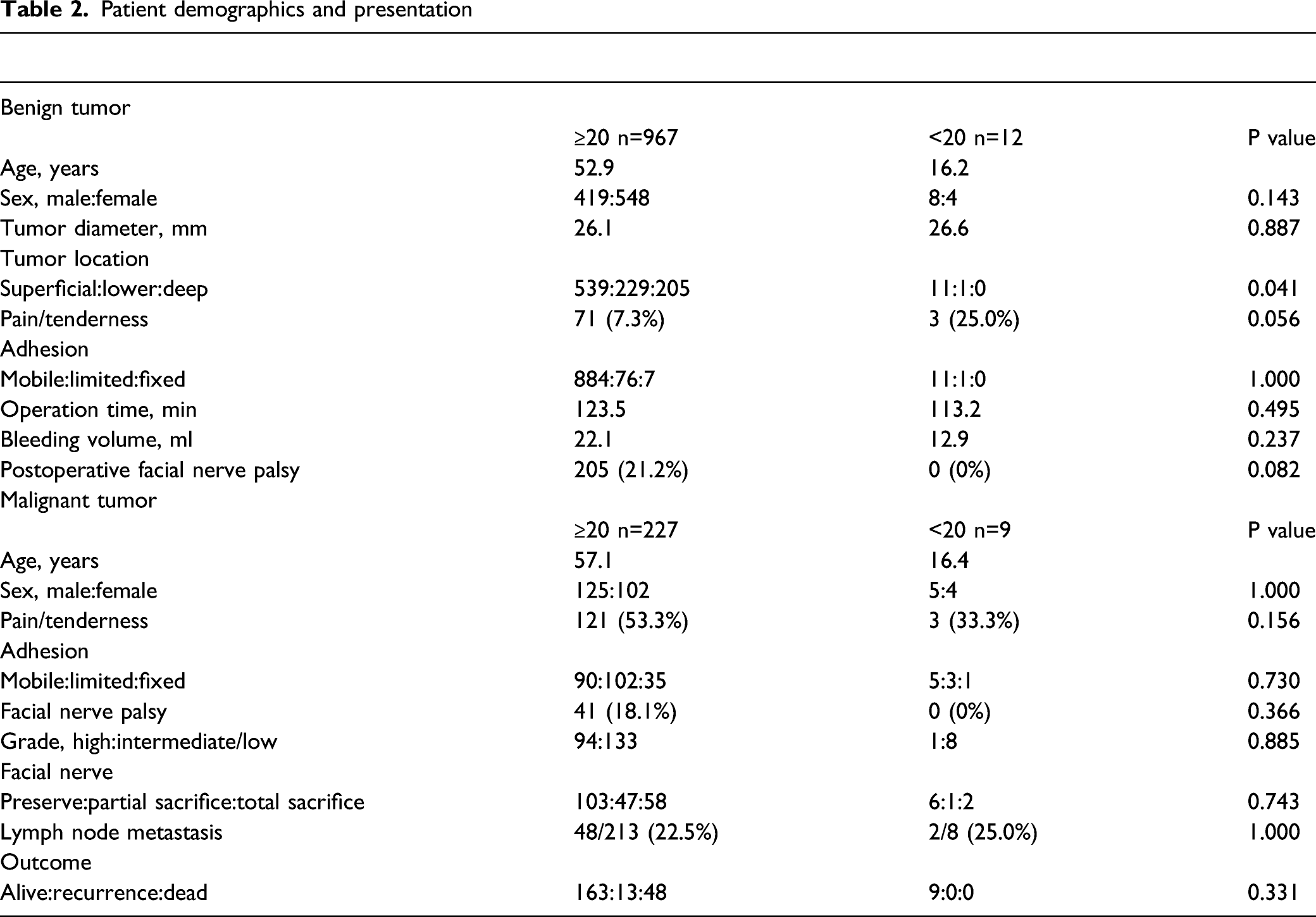
Fine-Needle Aspiration Cytology (OMC Classification) in Adolescents and Adults
In adults with benign tumors, a diagnosis of benign histology was obtained by the OMC system (Category 4-1) in 741 (76.6%) of 967 patients. In adolescents, 11 (91.7%) of 12 patients resulted in a diagnosis of benign histology (all pleomorphic adenomas). Twelve (1.2%) adults were diagnosed as malignant (Category 6), but no adolescent benign cases were diagnosed as malignant.
Cytopathology results categorized by the Osaka Medical College (OMC) system after fine-needle aspiration cytology
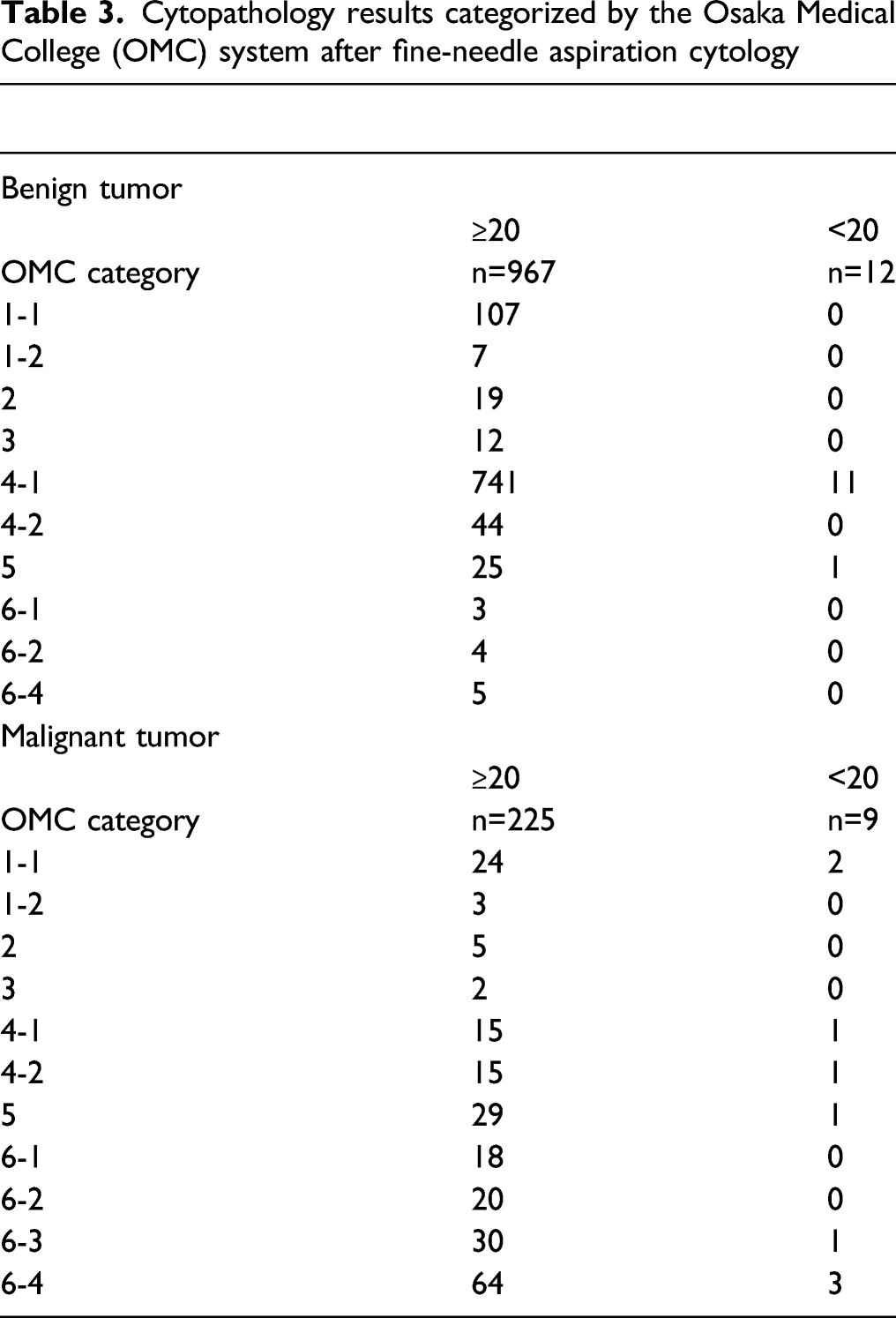
Adolescent Patients With Benign Tumors
Characteristics and treatment of benign parotid tumors in adolescents
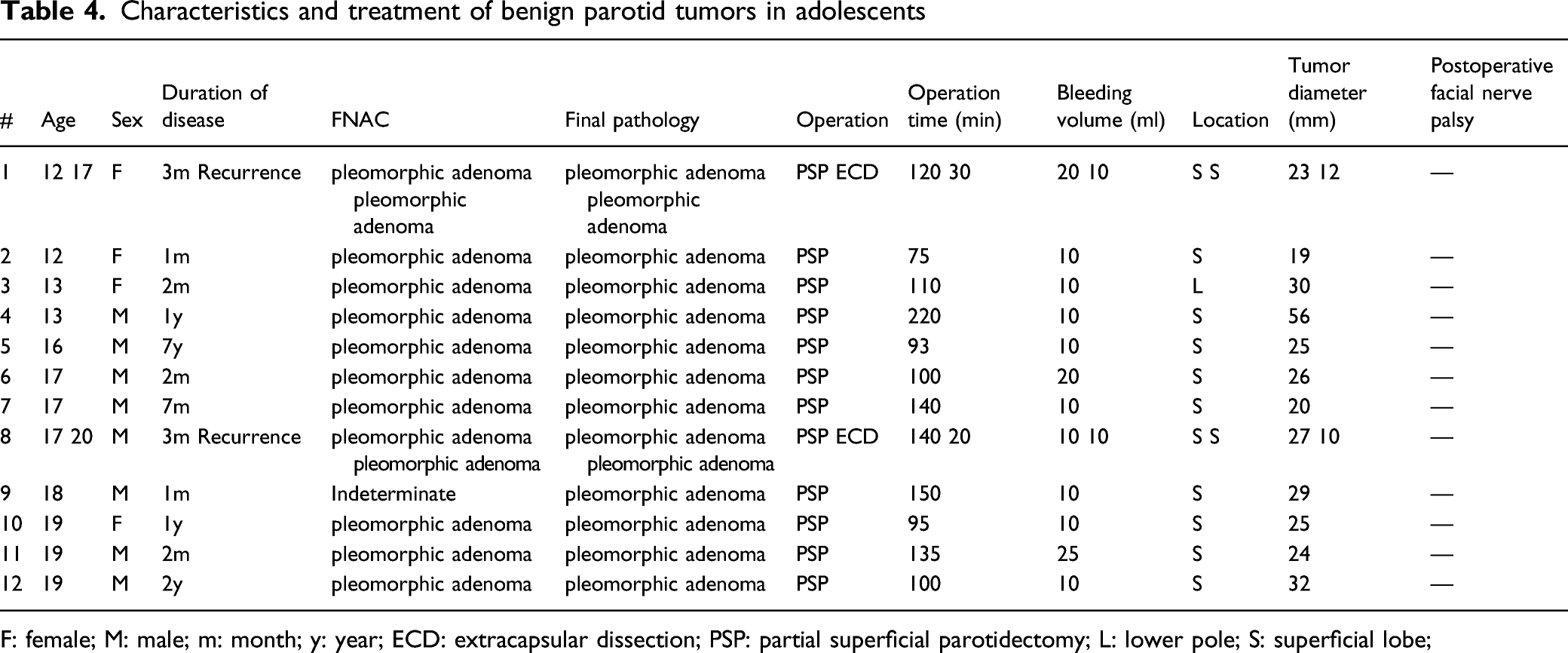
F: female; M: male; m: month; y: year; ECD: extracapsular dissection; PSP: partial superficial parotidectomy; L: lower pole; S: superficial lobe;
Adolescent Patients With Malignant Tumors
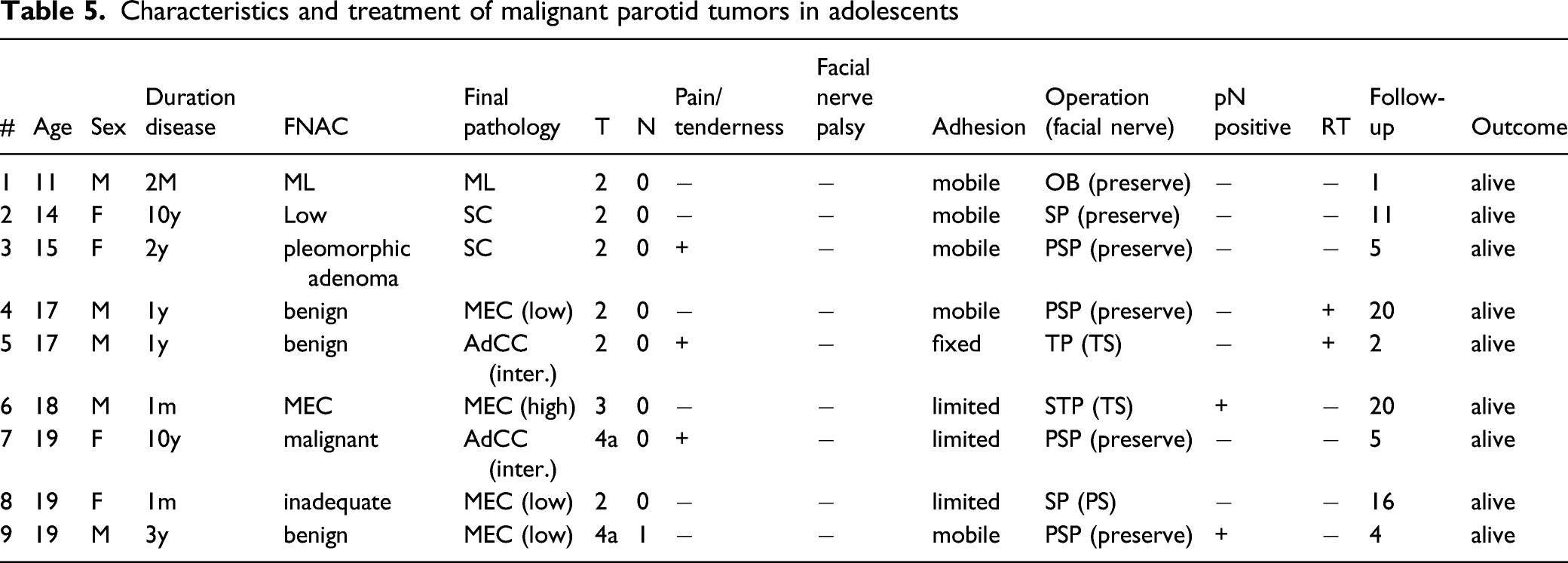
Characteristics and treatment of malignant parotid tumors in adolescents
Discussion
In overseas reports summarizing a large number of cases, parotid tumors in children are reported as rare and occurring in only around 2%.1,2 Moreover, when pediatric parotid tumors are categorized as children (<10 years old) and adolescents (10 to <20 years old), more than 90% occur among adolescents. 2 In the current study, both benign and malignant tumors were all seen in adolescents. Adolescent cases consisted of 12 (1.2%) of all 979 benign tumors. However, when limited to benign pleomorphic adenomas, adolescent cases made up 12 (1.9%) of 647 cases, indicating a slightly higher incidence than for overall benign tumors. In addition, there were no cases of Warthin tumor in those under 20 years old. In contrast, 9 (3.8%) of 236 patients were adolescents for malignant tumors, showing a proportion 3.1 times higher than benign tumors. 5 When classified by the grade of malignancy, high-grade malignant tumors accounted for 40.3% of all malignant tumors, while only 1 case out of 9 was high-grade in adolescents.
For preoperative diagnosis, the same diagnostic method as that used in adults was used in all cases because this study included only those aged 12 years or older. When a parotid tumor was suspected on inspection and palpation, this was further examined using ultrasound echo and guided FNAC. In our department, FNAC is performed preoperatively in all patients. Of the 12 pleomorphic adenomas, 11 were diagnosed as pleomorphic adenomas by preoperative FNAC. Regarding pleomorphic adenoma in adults, FNAC diagnosed pleomorphic adenoma correctly in about 85% of cases, 11 with a similar rate observed among pediatric cases. On the other hand, only 4 adolescent cases among 9 were correctly diagnosed as malignant by FNAC. The high number of low/intermediate-grade malignant tumors seemed to be the cause; thus, the accuracy rate was lower than that in adults. 12
A systematic review of pediatric malignant tumors, including 427 parotid tumors in patients 0 to 19 years old, reported that 53% were mucoepidermoid carcinoma, 29% were acinic cell carcinoma, and 5% were adenoid cystic carcinoma. 9 Similarly, another systematic review of patients 0 to 19 years old with parotid tumors found that 58% of 2215 patients had mucoepidermoid carcinoma and 25% had adenoid cystic carcinoma. 13 These data are further supported by a database review by Radomski et al, 14 which found that 50% of 220 cases of parotid tumors were mucoepidermoid carcinoma, 40% were acinic cell carcinoma, and 3% were adenoid cystic carcinoma. In our study, mucoepidermoid carcinoma also accounted for half of all cases, and the rest were adenoid cystic carcinoma, secretory carcinoma, and malignant lymphoma. In our department, fusion gene testing is performed for all cases of acinic cell carcinoma to distinguish secretory carcinoma. We found that approximately 50% of acinic cell carcinomas proved to be secretory carcinomas. In addition, secretory carcinomas occurred significantly more than acinic cell carcinomas in adolescents. 15 Therefore, it is possible that about half of the acinic cell carcinomas in previous studies were secretory carcinomas.
Previous studies suggest that malignant parotid tumors in adolescents are frequently low/intermediate-grade, with a high-grade rate of approximately 15%.9,14 Among the 9 cases included in this study, 5 cases were low-grade (mucoepidermoid carcinoma and acinic cell carcinoma), 3 cases were intermediate-grade (cribriform type adenoid cystic carcinoma and lymphoma), and only 1 case was high-grade (mucoepidermoid carcinoma). The observation period ranged from 1 to 20 years, and all patients are surviving cancer-free at the time of this writing. Children generally have a favorable prognosis because the grade of malignancy is often low or intermediate. However, long-term observation is still required for low/intermediate-grade malignant tumors, and Cockerill et al 16 found that when 52 adolescent cases (including 49 parotid tumors) were followed up for a maximum of 60 years, recurrence occurred in 15 (29%) of 52 patients. It should be noted that for most recurrences, the initial surgery was enucleation. As the longest time to recurrence was 45 years in the above study, treatment that takes long-term prognosis into consideration is especially important in pediatric cases.
Pleomorphic adenomas are found at a high rate in pediatric benign tumors, and all cases of benign parotid tumors were pleomorphic adenomas in our study. Among the 967 adult benign parotid tumors, 635 (65.7%) were pleomorphic adenomas, indicating that the rate of pleomorphic adenomas was higher in children. However, there were 17 patients with intraparotid nodules during the same observation period. Surgery revealed them to have inflammatory disease, and 3 of these patients were under 20 years old. Cases of inflammatory parotid nodules likely exist among those who do not undergo surgery. Therefore, inflammatory diseases are an important differentiation to pleomorphic adenoma. Since inflammatory diseases are often accompanied by pain/tenderness, and about half of malignant parotid tumors have pain/tenderness, it is also important to distinguish between inflammatory diseases and malignant tumors. 17
Existing issues of pleomorphic adenoma include recurrence and malignant transformation. Recurrence often occurs 10–15 years after surgery, and a .45% risk of recurrence per year after surgery has been reported for pediatric pleomorphic adenoma. 18 The risk of malignant transformation of pleomorphic adenoma is also thought to increase with time during long-term observation. 8 From this perspective, more attention should be paid to recurrence and malignant transformation in pediatric cases because they require a long follow-up observation than adult cases do. Recurrence is generally thought to be more common in cases of enucleation. 6 In pediatric cases, limited surgery may be selected more often for protection of the facial nerve and aesthetic issues. However, definitive removal may be more desirable because long-term observation is required. The standard operative method would be to perform a PSP where the facial nerve is identified and preserved. It should be noted that 2 of 12 patients with pleomorphic adenoma had recurrences in our study, and the time to recurrence took only 3 years and 5 years, which are relatively short periods of time. The initial surgery was conducted at our department in both patients, and both underwent PSP as with other cases. There were 635 adult cases of pleomorphic adenoma that were operated on within the same time period, of which 34 (5.4%) had recurrences, but the initial surgery was performed at our department in only 2 of these cases. 6 The 2 pediatric cases with a recurrent pleomorphic adenoma in our study were recurrences with single tumor in the superficial parotid gland and were not multiple recurrences by dissemination.
Conclusion
Adolescent patients, defined as under 20 years old, comprised 12 (1.2%) of 979 patients with benign parotid tumors and 9 (3.8%) of 236 patients with malignant parotid tumors; thus, showing relatively more malignant cases. Histopathologically, benign tumors were all pleomorphic adenomas, and mucoepidermoid carcinoma was common among the malignant tumors. Pleomorphic adenomas are known to be associated with recurrence and malignant transformation, and the appropriate resection is desirable in pediatric cases because they require a long-term observation. Although the malignant tumors in this study were of low/intermediate malignancy grade, except for one case, and the prognosis was favorable, further observation over longer periods is required.
Footnotes
Author Contributions
HK, TT, SH, and RK: study designHK, YI, and RK: writing of the manuscriptIK, YA, and AO: literature searchIK, SO, and MH: data analysisRK: final approval of the manuscriptAll authors read and approved the final manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
This study was approved by our Institutional Review Board (Osaka Medical College; #2621-1,2020).
