Abstract
Background
External ear canal exostoses are usually bilateral and broad-based, secondary to external ear canal chronic cold exposure, especially water.
Objectives
The objectives were to analyze the influence of the surgeon’s experience on the 3-year recurrence and on the complication. We also studied the influence of prolonged exposure to cold water on the incidence of recurrence.
Material and Methods
This monocentric retrospective study included 98 ears operated for canalplasty between 2009 and 2016 by nine different operators including one senior, a junior, and seven beginner surgeons. Senior, Junior, and Beginner groups were compared.
Results
3-year recurrence rate was higher in the Beginner and Junior groups than in the Senior group (69% and 38% vs 18%, P = .001). Although there was a difference between the Beginner (69%) and Junior (38%) groups, it was not significant (P = .407). Among the recurrences, 48% had continued exposure to cold water while only 7% of the ears without recidivism were still exposed (P < .001, OR = 1.25 [4.4; 36.1]). The complication rates were similar between groups, concerning pain (8% vs 30% vs 12%), per procedure perforation (17% vs 10% vs 16%), scarring disorders (25% vs 20% vs 13%), and osteitis (8% vs 0% vs 1%). Hearing was unaffected.
Conclusions
This is the first study evaluating the risk of recurrence of external ear canal exostoses after canalplasty based on the surgeon’s experience. This risk of recurrence seems to decrease with the surgeon’s experience. There was no difference in complication rates.
Introduction
External ear canal exostoses are usually bilateral and broad-based, secondary to external ear canal chronic cold exposure, especially water. They are mostly asymptomatic, but the obstruction of the external ear canal increases with their growth. Water and epidermal retention phenomena appear, leading to discomfort, hearing loss, or external ear infections. Prevention is based on the use of obturating plugs that prevent exposure to cold water, the main risk factor identified for this pathology.1–3 Aspiration or local antibiotic therapy may be necessary in the case of local super-infection and surgery to prevent the recurrence of symptoms. Exostosis surgery, called canalplasty operations, was described in the second half of the 19th century. 4 This surgery is difficult to learn due to the close proximity of external ear canal to nearby structures. Post-operative complications include meatal stenosis, prolonged healing, tympanic perforation, tinnitus, dizziness, sensorineural hearing loss, and damage to the facial nerve or temporomandibular articulation. Post-operative improvement of symptoms is observed in about 70% of cases. 5 Surgical techniques evolved during the 20th century with the development of different techniques to reduce the morbidity of canalplasty.6–8 However, the role of the surgeon’s experience had never been evaluated and the risk of recurrence was poorly known, with highly variable data depending on the studies.9,10 The main objective was to analyze the influence of the surgeon’s experience on the 3-year recurrence. Secondary objectives were to analyze the incidence of post-operative complications according to the surgeon’s experience, the incidence of recurrence and the influence of prolonged exposure to cold water on the incidence of recurrence.
Patients and Methods
Ninety-eight canalplasty operations for exostoses of 77 patients (6 women and 71 men) were included from January 1, 2009 to August 1, 2016 in this retrospective monocentric study. The mean age was 49 ± 12 years. Post-operative consultations occurred at 1 week, 1 month, 6 months, and yearly. The mean follow-up time was 46 ± 37 months. Clinical recurrence was defined as a finding of restenosis of external ear canal at any stage. Symptomatic recurrence was defined as recurrence of symptoms related to exostoses (water or cerumen retention, hearing loss, and external ear infection). Overall recurrence included all events, clinical or symptomatic. Thirty-three ears (34%) were lost to follow-up before 3 years. The institutional ethics committee (29BRC19.02012) approved the study and all patients expressed their non-opposition to the use of anonymous data. This article followed the STROBE guidelines.
Nine different operators were identified. The seven Beginners operators (2 year’s experience) performed 12 operations (1–3 for each operator), the Junior operator (5 year’s experience) performed 10 operations (10%), and The Senior operator (15 year’s experience) performed 76 operations (78%). The included ears were separated into 3 groups, 1 group of novice surgeons, 1 for the junior surgeon, and 1 for the senior surgeon. Five categories of surgical indications were defined: “otitis” for external ear infection, “entrapment” for water or cerumen entrapment, “hearing loss” for conductive hearing loss due to obstruction, “asymptomatic” for exostoses preventing visualization of the tympanic membrane, “pathological ear” in case of middle ear surgery as the main surgical indication and having required a canalplasty for the approach. The surgical techniques (approach and instrumentation) were studied. All the operators performed a temporal fascia graft and silicone strips for 1 month. No skin grafting or stenting were used. Patients were asked to avoid exposure to cold water. The anatomic data of exostoses were defined, in the absence of a validated classification, by the stage of the stenosis. All patients had a CT-scan before surgery. A ≤30% stenosis defined stage I, between 31 and 60% defined stage II, and 61%≥ defined stage III. Delta bone conduction was defined as the difference in the mean bone conduction threshold measured in before and after surgery on the tonal audiogram at frequencies 250, 500, 1000, 2000, and 4000 Hz. Conductive hearing loss (Delta Air Bone Gap) was defined by the difference of the air bone gap before and after surgery on the frequencies 250, 500, 1000, 2000, and 4000 Hz. Canalplasty on “ pathological ear” were excluded from the audiometric analysis, post-operative audiometric results depending on the procedure performed on the middle ear. Prolonged healing was defined as meatal stenosis, persistent local inflammation or bone exposure more than 6 weeks after canalplasty. Pain persistence at day 7 of the procedure was noted, as well as the occurrence of bleeding.
Characteristics of the patients.
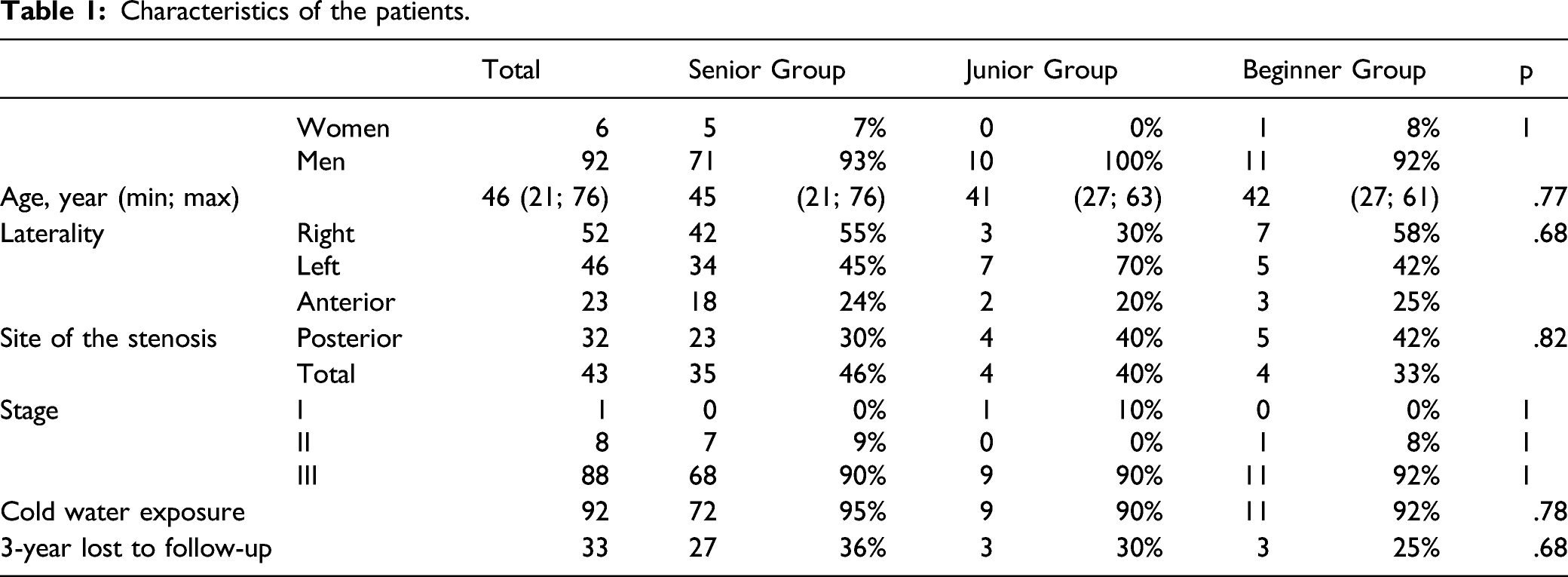
Distribution of surgical characteristics by group.
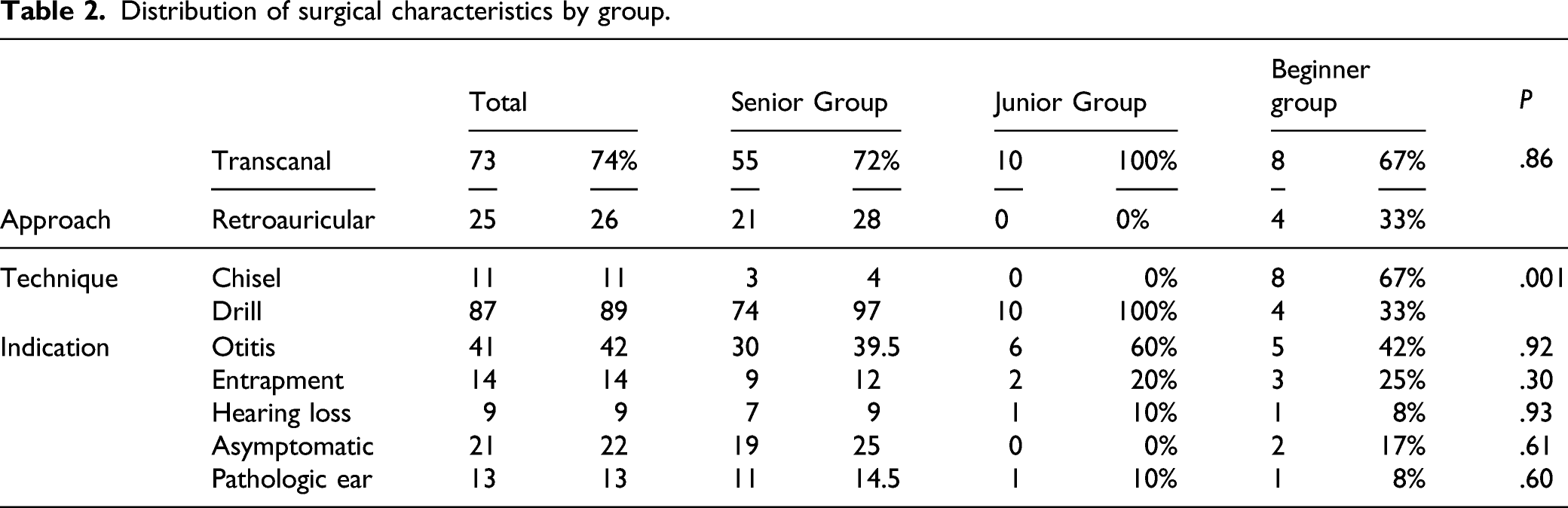
Results
3-year overall recurrence was higher in the Beginner and Junior groups than in the Senior group, with rates of 69% CI95 (54%–84%), 38% CI95 (21%–55%), and 18% CI95 (9%–27%), respectively. The difference was significant between Beginner and Senior groups (P = .001), and between Junior and Senior groups (P = .001), but not significant between Beginner and Junior groups (P = .407) (Figure 1). Lost to follow-up ears were similar between groups: 3 ears (25%) in the Beginner group, 3 (30%) in the Junior group, and 27 ears (36%) in the Senior group (P = .757). The clinical and symptomatic recurrence rates were, respectively, 17% CI95 (5%–29%) and 50% CI95 (37%–63%) in the Beginner group, 10% CI95 (0%–19%) and 40% CI95 (39%–51%) in the Junior group, and 16% CI95 (7%–25%) and 8%, CI95 (0%–17%) in the Senior group. Recurrence occurred within a median of 8, 10, and 20 months for the Beginner, Junior, and Senior groups, respectively. Three recurrences within 6 months after surgery were observed in the Beginner group (25%), 2 in the Junior group (20%) vs 3 in the Senior group (4%). There was no difference in recurrence rate by stage of disease (stage 2: 10% CI95 [0%–31%] and stage 3: 18% IC95 [9%–36%], P = .194). 3-year overall recurrence in Beginner, Junior, and Senior groups, and 5-year overall recurrence.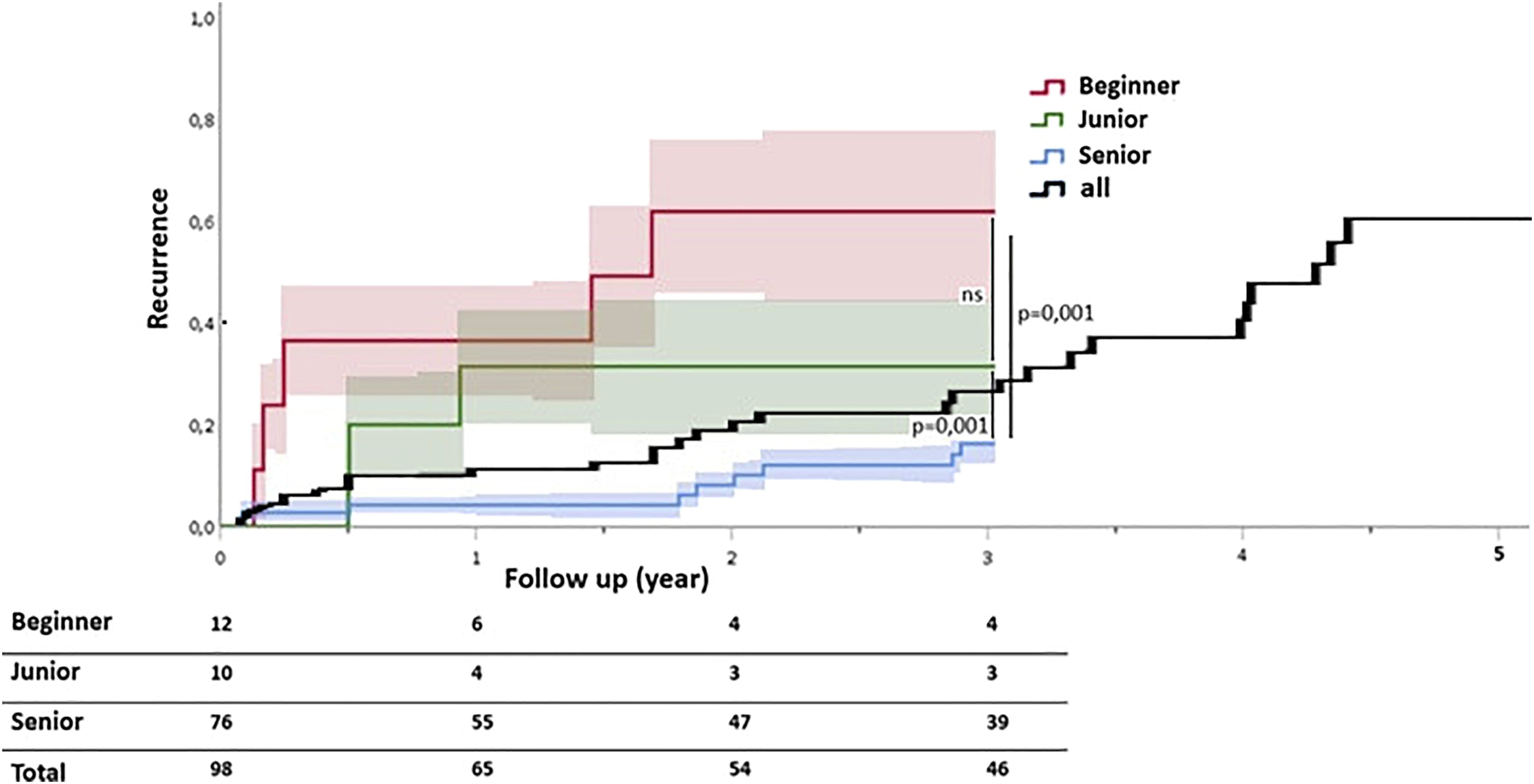
Complications of canalpasty
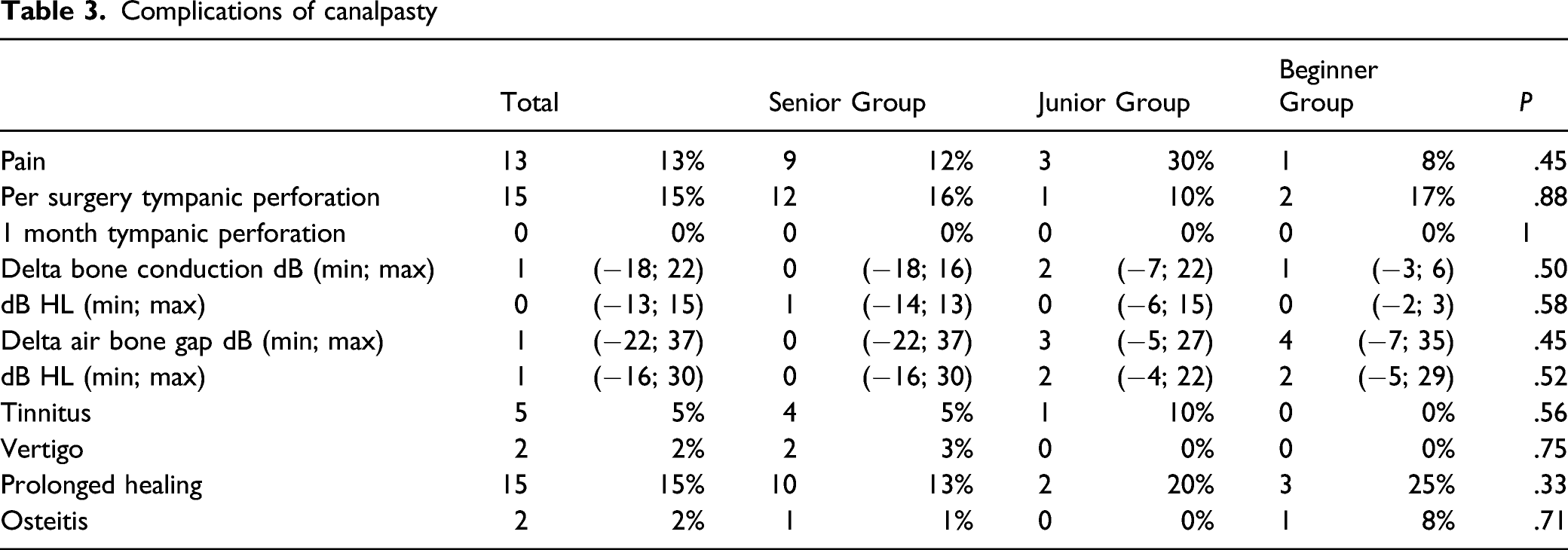
Discussion
Our study is the first to investigate the role of the surgeon’s experience on the recurrence occur of canalplasty for external ear canal exostoses. 3-year recurrence is higher in our series when the surgeon is a beginner or junior. This difference is probably the result of a more complete exostosis removal by the senior surgeon. Indeed, recurrences occurs earlier for beginner and junior operators with an average delay of 8 and 10 months. Nearly a quarter of these recurrences occurred within 6 months, probably reflecting the non-improvement of symptoms more than a real recurrence.
In studies evaluating surgical experience with type 1 tympanoplasty, most of the results suggest better outcomes for senior surgeons compared to residents, with a better myringoplasty graft rate.11,12 Baruah et al find that the learning curve is almost complete after 20 surgeries, in agreement with our study, with 10 surgery for the Junior operator. 13 In endoscopic stapes surgery, the learning curve has also been studied, with similar functional results to those of microscopic surgery, with the same rate of complications.14,15 In Stapedotomy with a standardized laser-assisted surgical technique, Kwok et al found no difference between experienced and novice surgeons (58 vs 12 ears, respectively). 16
One limitation of this study is the difference in population size, with 76 ears in the senior group vs 10 in the junior group and 12 in the beginner group. The only significant difference between the groups was in surgical technique. Transcanal or retroauricular approach were used. 17 Beginner operators used micro-osteotome more often than junior and senior operators, who preferred drilling. These preferences may have influenced long-term post-operative outcomes; however, the choice of technique was also a function of the operator’s experience. It is interesting to note that despite the use of drilling, the junior operator had a higher 3-year recurrence compared to the senior operator.
Drilling and chiseling are the 2 main techniques that have been described and studied since the beginning of canalplasty.4,18 Barrett et al 19 and Hetzler 20 recommend a combined approach combining osteotomy with impact scissors and drilling for a more complete procedure, reducing the risk of auditory complications related to drilling. It would be interesting to be able to observe the learning curve of the junior surgeon to know the number of canalplasties required to acquire this expertise. New techniques have been developed to reduce morbidity: the piezoelectric saw, which is used in maxillofacial surgery for its action on mineralized tissue to preserve soft tissue, could be used to reduce prolonged healing. 7 In a series of 10 exostoses, Haidar et al. did not find any complication. 6 This surgical technique would be interesting to evaluate over a larger series with long-term follow-up.
In our study, the complication rate is not modified by the surgeon’s experience. Fisher et al found a complication rate of 35% for surgeons in training and 21% for trained surgeons. 21 The tympanic perforation rate of 15% in our study is comparable to the literature with rates ranging from 9.5% for Barrett et al 19 to 22.5% for Hetzler 20 The prolonged healing rate is 15%, comparable to the 18% rate found by Fisher and McManus, 21 but higher than 4.7% in Grinblat et al. study. 22 In a series of 254 exostoses treated by drilling, House and Wilkinson 9 found a 4.8% risk of sensorineural hearing loss greater than 15 dB at 4000 Hz. Timofeev et al 10 described sensorineural hearing loss after 3 canalplasties with a cumulative drilling time of 7 hours. In our series, excluding “pathological ears,” we find one case of sensorineural hearing loss with an average loss of 13 dB HL on the bone tonal curve at day 2 of a canalplasty performed by the senior operator. CT-scan showed the stapes dislocated into the vestibule. Five ears (5.1%) showed transient post-operative tinnitus that may be related to labyrinthic trauma.
The clinical recurrence rate was 14% at 36 months in our study, compared to 9% with an average follow-up of 24 months in the House and Wilkinson study. 9 Timofeev et al 10 reported symptomatic recurrence for most ears operated at 10 years, with a rate of 40% at 5 years. In our study, we have a symptomatic recurrence rate of 16% at 3 years. The lack of standardization in the definition of recurrence makes it difficult to compare studies. This high variability is also explained by the difficulties in long-term follow-up of these patients in good general condition with functional pathology. Only 24% of patients with symptomatic external ear canal exostoses consult according to the study by Lennon et al 23
Our study confirms the findings of Timofeev et al 10 and Alexander et al 24 that avoidance of cold water prevents recurrence. This preventive measure is widely known to the main exposed population. Indeed, 60–86% of surfers say they are informed, but only 24–54% of them wear stoppers.25,26 In our series, the rate of eviction from cold water reaches 80.6%, which can be explained by a cohort of ears already operated with greater awareness of this pathology. However, 52% of recurrences occur after stopping exposure. There could be a delayed effect of cold water exposure which would explain almost all recurrences in the 5 years post-operatively in our series. It would have been interesting to know the duration and frequency of cold water exposure prior to ear surgery in our cohort to evaluate whether the intensity of preoperative exposure influenced the recurrence delay after canaplasty.
Conclusion
This is the first study investigating the role of the surgeon’s experience on the risk of recurrence of canalplasty for external ear canal exostoses. The incidence of recurrence appears to decrease with surgeon experience above a certain threshold and with cessation of cold water exposure. We did not find any change in the rates of complication rates pre- and post-operatively according to surgeon experience.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
