Abstract
A dehiscent high jugular bulb would be a pitfall in middle ear surgery especially for cholesteatoma. We report a case of cholesteatoma attached to a dehiscent high jugular bulb successfully treated with surgery assisted with underwater endoscopy. To the best of our knowledge, no previous study has reported a case of cholesteatoma with dehiscent high jugular bulb treated with surgery assisted with underwater endoscopy. Owing to the risk of jugular bulb injury, underwater endoscopy is a good indication for middle ear cases with a dehiscent high jugular bulb to obtain a clear operative field and avoid an unexpected air embolism.
Keywords
Introduction
The jugular bulb (JB) connects the sigmoid sinus and internal jugular vein. Anatomically, the superior border of the JB lies below the lowest floor of the hypotympanum, with a bony plate separating the dome of the JB from the middle ear cavity. 1 Vascular anomalies in the temporal bone include a high jugular bulb (HJB), a dehiscent JB, a diverticulum associated with JB, an anterior location of the sigmoid sinus, and a dehiscent internal carotid artery. 2,3 The most common vascular anomaly of the petrous temporal bone is HJB. 4,5
A dehiscent JB, defined as a normal venous variant with superior and lateral extensions of the JB into the middle ear cavity through a dehiscent sigmoid plate, 3 is more commonly found in association with HJB. A dehiscent HJB is vulnerable to damage during surgery owing to its incomplete bony covering and resultant lack of protection. 6
We report a case of cholesteatoma attached to a dehiscent HJB that was successfully treated with surgery assisted with underwater endoscopy. Owing to the risk of JB injury, underwater endoscopy is a good indication for middle ear cases with a dehiscent HJB.
Case Report
An 84-year-old man visited a nearby otolaryngologist with a 4-month history of otorrhea in the right ear. He had right hearing loss for many years but had no history of surgical interventions such as myringotomy or ventilation tube insertion. He was referred to our department because of suspected attic cholesteatoma.
Clinical examination on presentation revealed retraction and debris accumulation in the pars flaccida and a pulsatile bluish mass of the tympanic membrane in the right ear (Figure 1A). Pure-tone audiometry of the right ear revealed mean air-conduction hearing levels of 78.3 and 40.0 dB at 500, 1000, and 2000 Hz, respectively. Computed tomography (CT) revealed a soft tissue shadow in the mastoid, epitympanum, and mesotympanum (Figure 1B and C). The incus was eroded by the cholesteatoma, and the JB without a bony plate was connected to a soft tissue shadow in the mesotympanum. We made a diagnosis of cholesteatoma with a dehiscent HJB.
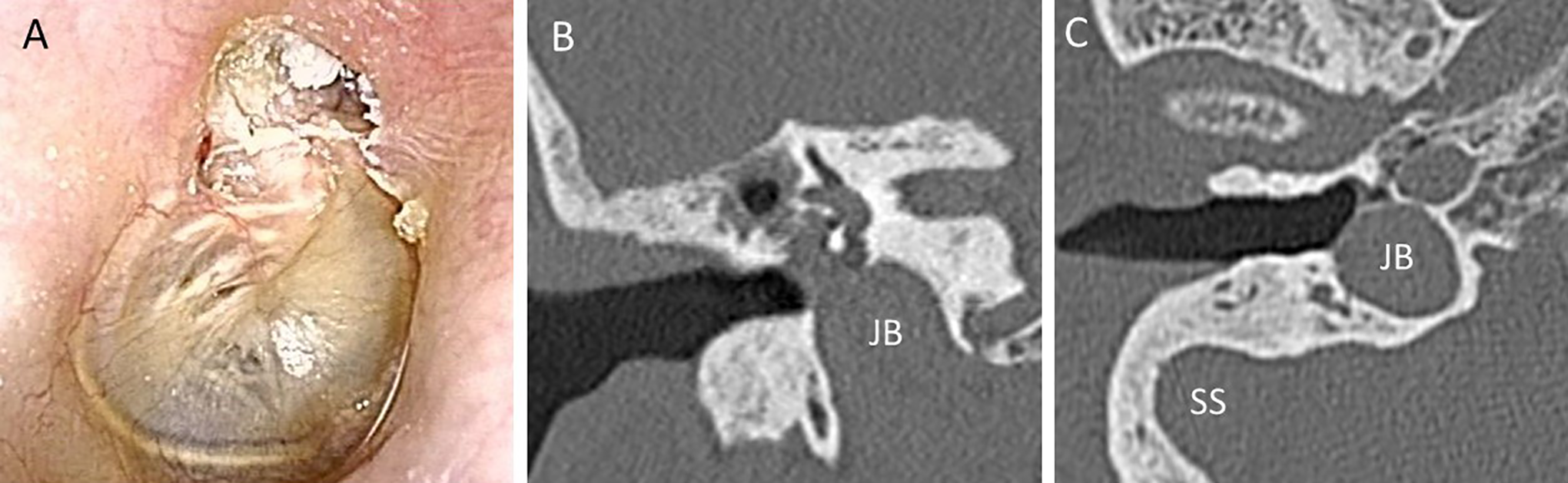
A, Retraction and debris accumulation in the pars flaccida. A pulsatile bluish mass can be observed mainly in the posteroinferior quadrant. The margins of the cholesteatoma and dehiscent high jugular bulb are not clear in the otoscopic finding. B, Preoperative CT image of the right ear showing a destructive lesion in the mastoid extending to the mesotympanum. The jugular bulb, the dome of which lacks the bony plate, possibly blocks the round window, preventing aeration between the cholesteatoma and the dehiscent high jugular bulb. C, The jugular bulb is adhering to the tympanic membrane. CT indicates computed tomography.
During surgery, a postauricular skin incision was completed under general anesthesia. A cholesteatoma was identified during canal wall down mastoidectomy (Figure 2A). The JB, adhesively attached to the tympanic membrane, was identified without a bony plate. The cholesteatoma extended inferiorly to the level of the dehiscent HJB and posteriorly to the stapes (Figure 2B). During cholesteatoma removal, an underwater endoscopy technique was used especially in exploring the stapes from the cholesteatoma and dehiscent HJB (Figure 2C). The incus and head of the malleus were removed with preservation of the chorda tympani. The facial nerve in the tympanic segment was uncovered by the cholesteatoma. Total resection was performed without a JB injury (Figure 3D). Tympanoplasty with meatoplasty was performed with a partial ossicular replacement prosthesis (PORP), and the partial mastoid obliteration was completed with bone pate, auricular cartilage, and temporal fascia using fibrin glue.
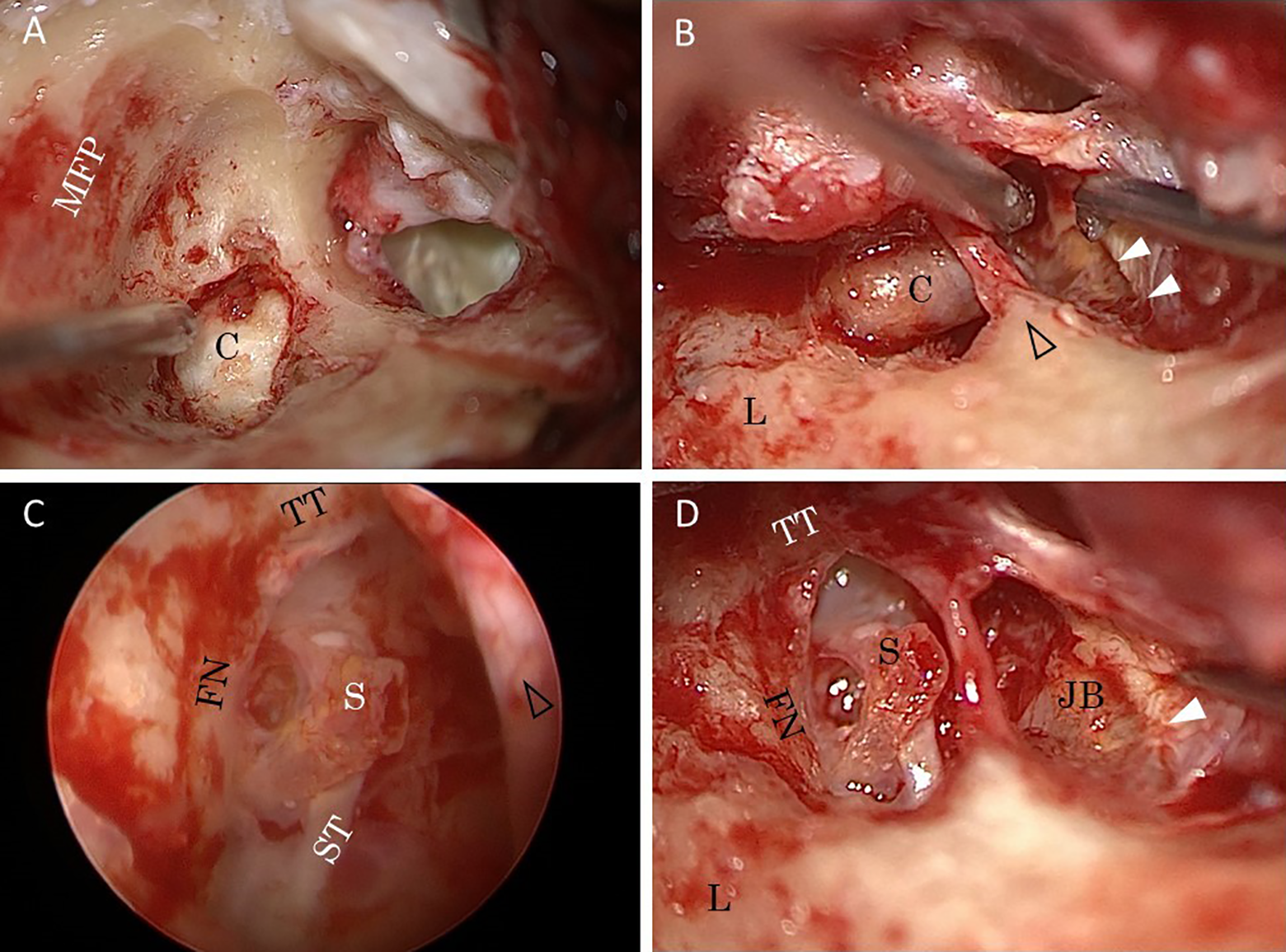
A, A cholesteatoma identified in the mastoid during canal wall down mastoidectomy. B, The cholesteatoma in the mesotympanum extends at the level of the dehiscent high jugular bulb, which is adhesively attached to the tympanic membrane (white arrows). The round window is completely covered by the dehiscent high jugular bulb. The cholesteatoma extends posteriorly to the stapes beneath the chorda tympani (open arrow). C, Underwater endoscopic view. The stapes is clearly observed away from the dehiscent high jugular bulb. The chorda tympani is preserved (open arrow). D, Surgical view after the removal of the cholesteatoma. The dehiscent high jugular bulb, attached to the cholesteatoma, is distal from the stapes. The round window niche is not visualized because the dehiscent high jugular bulb is superimposed. The tympanic membrane is difficult to elevate from the dehiscent high jugular bulb (white arrow).
The patient’s postoperative clinical course was uneventful, with no dizziness, tinnitus, and facial nerve palsy. The right ear cavity had dried within 3 months after operation (Figure 3A), although hearing was not improved postoperatively, demonstrating mean air-conduction hearing levels of 81.7 and 48.3 dB, respectively, at 500, 1000, and 2000 Hz. Postoperative CT revealed the removal of the cholesteatoma and PORP in the tympanic cavity (Figure 3B and C).
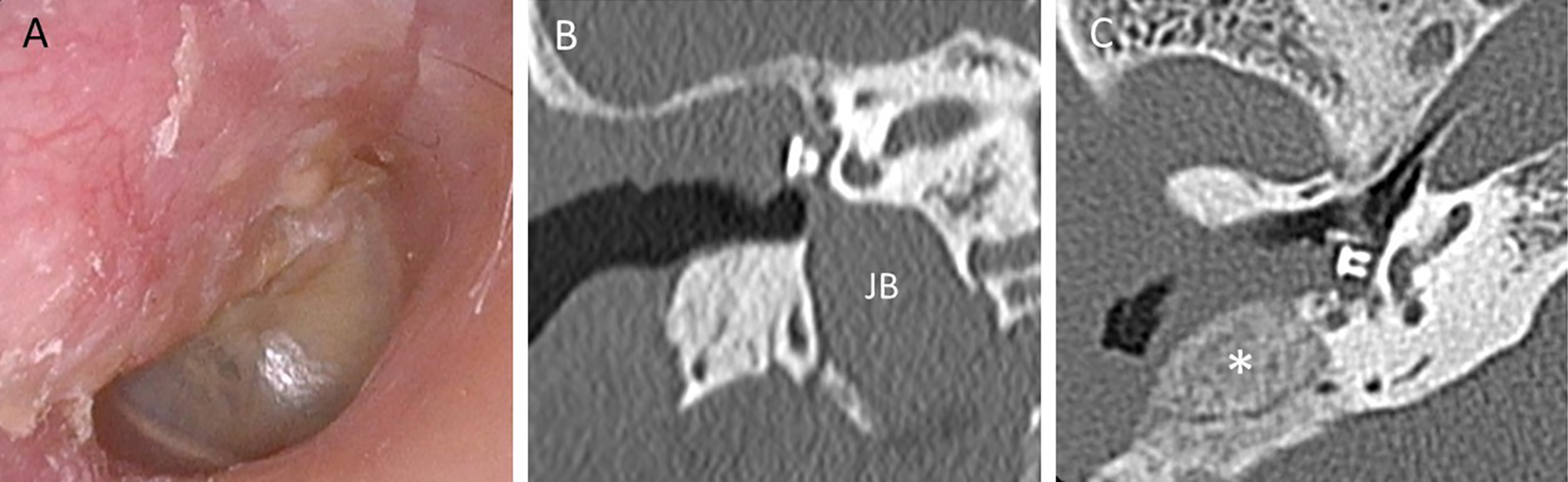
A, Three-months postoperative otoscopy image of the right ear. The retractions in the pars flaccida and mastoid cavity are covered with thin-sliced cartilage. B, The dehiscent high JB is distal from the PORP. During the surgery, a tiny piece of cartilage was placed between the PORP and the JB. C, In the horizontal view, ossified bone (*) can be observed in the mastoid. JB indicates jugular bulb; PORP, partial ossicular replacement prosthesis.
Discussion
High and dehiscent JB is an important anatomical variation during otologic surgery because vascular injuries may lead to serious consequences. Dehiscent JB, the rate of which was reported be 0.5% (10 ears of 1857 operations over a 20-year period) in middle ear surgery, 7 was observed in 2% of temporal bone CT images and defined as a high-risk factor of bleeding. 8 One of the potentially life-threatening complications secondary to sinus and/or JB injury is air embolism. 9,10
While endoscopic middle ear surgery has gained increasing popularity in the late 1990s, 11 a novel technique reported by Yamauchi et al as underwater endoscopic ear surgery was proposed to repair superior canal dehiscence and labyrinthine fistulas with good results and has the advantages of preservation of the inner ear function and clear operative view. 12,13 This technique provides a clear operative field without the need for suction and protects the inner ear from unexpected aeration that might lead to functional damage.
The clinical significance of dehiscent HJB is that it can cause fatal hemorrhage because of inadvertent puncture in patients undergoing myringotomy or tympanoplasty. 14 In chronic otitis media, with or without cholesteatoma, otoscopy and temporal bone CT usually allow preoperative identification of patients at risk of vascular complications. However, surgeons should be aware of the possibility of vascular anomalies being an unanticipated intraoperative finding. 15
Several reports in the literature have described conductive hearing loss related to JB anomalies. Three mechanisms have been proposed as follows: contact between the tympanic membrane and the JB, ossicular chain interference, and round window niche obstruction. 16,17 However, surgical correction of JB anomalies may not lead to hearing improvement and is not recommended. 16,17
In this case, we performed a microscopic ear surgery assisted with underwater endoscopy. Underwater endoscopy, in which the middle ear cleft is filled completely with saline by perfusion, is useful not only for obtaining a clear operative view but also for preventing air embolism secondary to unexpected dehiscent HJB injury. As the middle ear cleft is covered by the delivered perfusate, the possible venous entry of gas is not a risk of air embolism. After the dissection of the cholesteatoma from the stapes and dehiscent HJB, we finished the underwater endoscopy and performed microscopic examination again. Although the round window niche was impeded by the dehiscent HJB, no other surgical procedures such as coagulation or resurfacing with bone cement 18 were performed to avoid injury of the JB and chorda tympani.
Conclusion
We report a case of cholesteatoma attached to a dehiscent HJB treated with surgery assisted with underwater endoscopy. To the best of our knowledge, no case of cholesteatoma with dehiscent HJB treated with surgery assisted with underwater endoscopy has been previously reported.
Owing to the risk of JB injury, underwater endoscopy is a good indication for middle ear cases with dehiscent HJB to obtain a clear operative field and avoid unexpected air embolism.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
