Abstract
Lipomas are the most common soft tissue lesions occurring in the salivary glands but have a very low incidence. Lipomas commonly occur in the parotid gland, and lipomas in the submandibular gland (SMG) are rare. Until recently, ordinary lipomas of the parotid gland and some variants of lipomas of the SMG have been reported. However, few reports of ordinary lipomas occurring within the SMG exist in the literature. We report an extremely rare case of ordinary lipoma within the right SMG of a 65-year-old man. The tumor measured a 2.0 × 1.8 × 2.7 cm, was a well-capsulated homogenous yellow mass, which was composed of mature adipose tissue. A partially mixed area with salivary gland tissue was observed. There has not been much research on lipomatous tumors from the SMG because of their rareness. Most lipomatous tumors in the parotid gland are known as ordinary lipomas, but more research is needed to determine whether they can be applied to the SMG. Thus, this report will be instrumental in the understanding of lipomatous tumors of the SMG.
Introduction
Salivary gland tumors are mostly epithelial in origin and lesions originating from soft tissues are very rare, accounting for 1.9% to 5% of all salivary gland lesions. 1 Lipoma and its variants are known to be the most common salivary gland mesenchymal tumors and most occur in the parotid gland. 2,3 Lipomatous tumors account for 0.5% to 4.4% of all tumors arising from the parotid gland. 4 Until recently, several studies, including case reports, have focused on lipomas of the parotid gland.
However, lipomatous tumors of the submandibular gland (SMG) have a low frequency of occurrence and are rarely included in long-term, large-scale studies on various salivary gland tumors. 1,5,6 Although several cases of sialolipomas of the SMG have been reported since Nagao’s report in 2001, few reports have described or demonstrated ordinary lipomas occurring within the SMG, unlike the parotid gland. 7
Herein, we present a case of an ordinary lipoma originating within the SMG. To the best of our knowledge, no reports describing intra-submandibular ordinary lipoma with images exist in the English literature.
Case Report
A 65-year-old man was admitted with the symptom of swelling in the right submandibular area. It seemed to have appeared about 6 months ago and there were no other symptoms such as pain. There was no underlying medical disease or history of neck trauma and surgery. Bimanual palpation of the oral cavity revealed a soft and nontender lesion on the medial side of the right SMG. The lymph nodes were not palpable on either side of the neck. Computed tomography revealed a 2.0 × 1.8 × 2.7 cm low-density lesion in the right SMG (Figure 1). Submandibular resection was performed using the transcervical approach under general anesthesia.
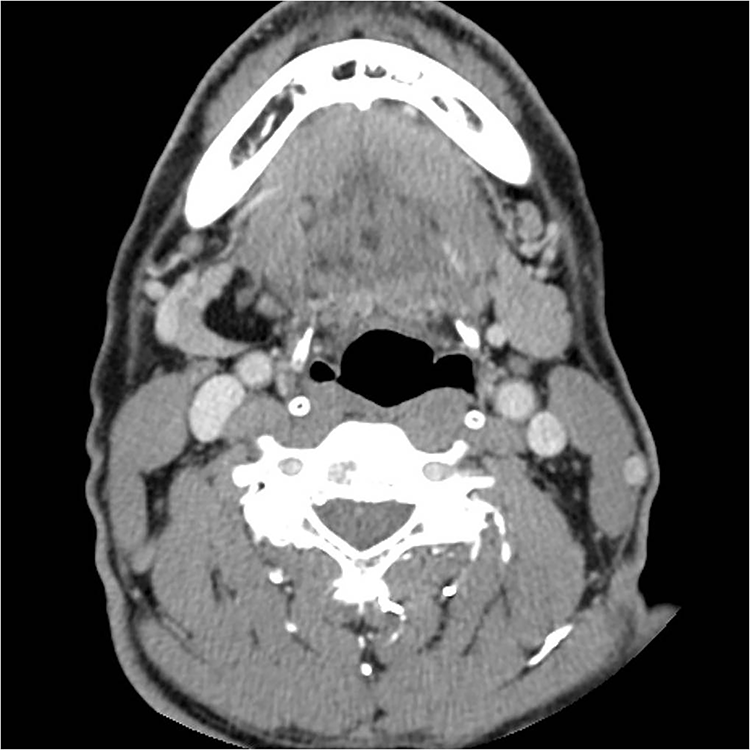
Computed tomography demonstrating a well-demarcated low-density lesion on the medial side of the right submandibular gland.
The yellow mass was surrounded by a fibrous capsule surrounding the SMG. On gross examination, the cut surface appeared homogeneous and a partial adhesion with the salivary gland tissue was observed (Figure 2). The lesion was diagnosed as an ordinary lipoma on histopathological examination, which was well-capsulated and was composed of mature adipose cells. Salivary gland cells and adipocytes were partially mixed, and no abnormalities were observed except for the dilated salivary duct in the area corresponding to the adhesion (Figure 3).
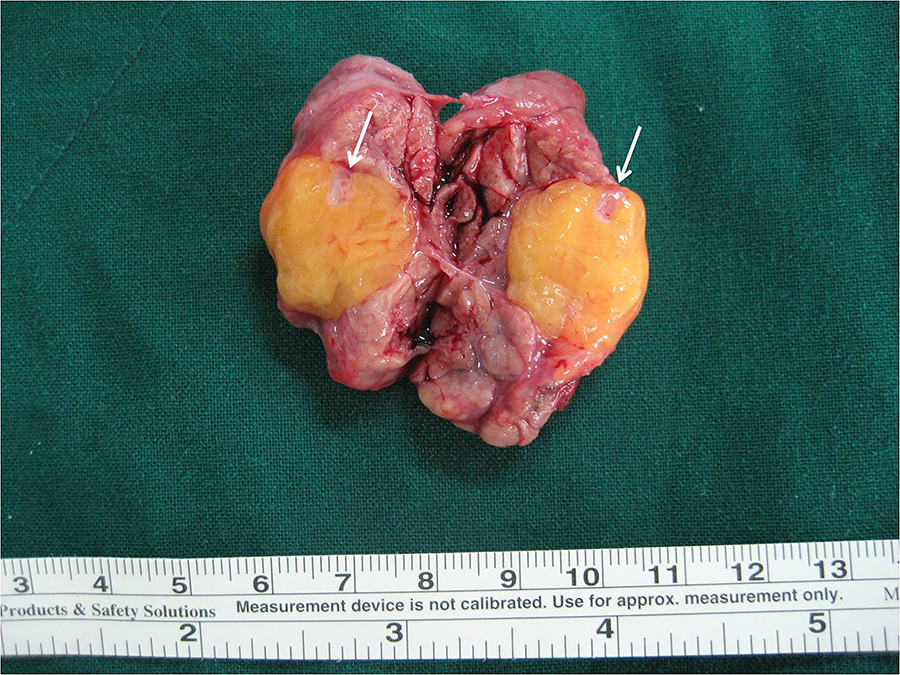
Cut surface of the surgical specimen showing a yellow homogenous lobulated appearance. Note that the tumor is partially attached to the gland (arrows).
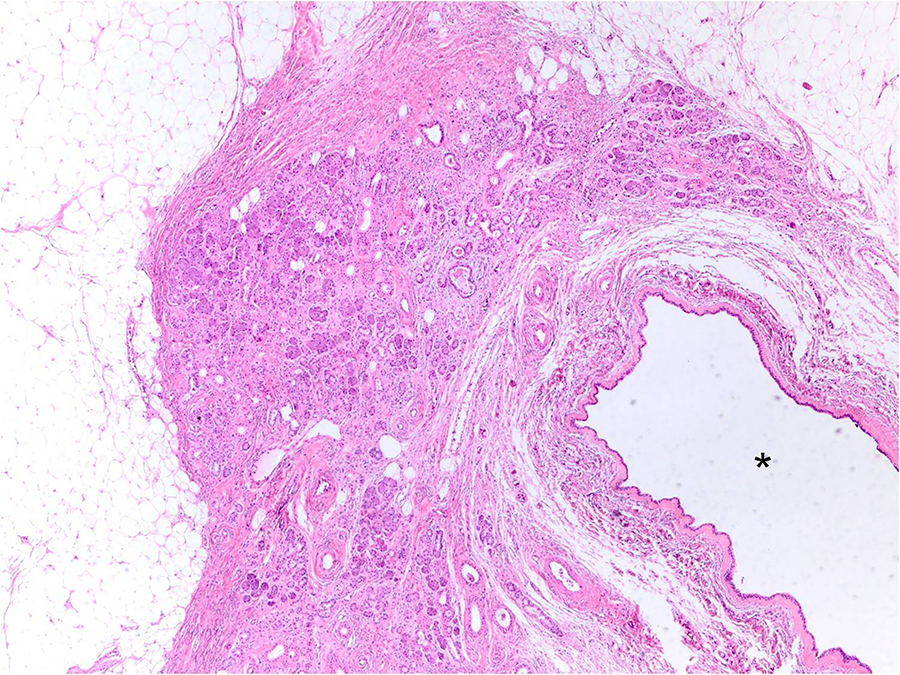
Histopathological examination showing that the tumor is composed of mature adipose tissue separated by thin fibrous tissue, and partly mixed with the parenchyma of the salivary gland containing the dilated salivary duct (asterisk).
No complications such as paralysis of the marginal branch of the facial nerve were observed postoperatively. The patient was followed up for 3 years, without any recurrence.
Discussion
Lipomatous lesions of the parotid gland are rare occurrences, and are even rarer in the SMG. 1,3 -6 Agaimy et al conducted the most recent large-scale study of lipomatous neoplasms of the salivary glands, which included 29 lipomatous tumors of the parotid gland and 2 lipomatous tumors of the SMG. 5 Both the SMG tumors were ordinary lipomas, which occurred on the right side in a 53-year-old man and on the left side in a 62-year-old woman. Serous acini were observed at the periphery of the tumor in the latter patient.
A study that examined the incidence of salivary gland tumors for 20 years in a defined population revealed that only 2 submandibular lipomatous tumors (lipoblastomas) developed during the investigation. 6 Moreover, other studies that focused on soft tissue lesions of the salivary glands did not distinguish between the sites of occurrence or included lesions of the parotid gland only. 1,2,8
There are many studies of lipomatous tumors of the parotid gland, including case reports. Recently, Starkman et al analyzed 70 cases, which is the largest case series to date. 4 According to that study, 90% of parotid lipomatous tumors were ordinary lipomas, and the rest were variants and malignant tumors. About 63% of the tumors were intraparotid and 37% were periparotid, and about 23% of the lesions were well-capsulated.
In the case of SMG, ordinary lipoma occurs in the submandibular space or variant lipomas occurred within the SMG. 7,9 However, there are few reports or studies on ordinary lipomas within the salivary glands. Based on previous studies, we cannot assume that ordinary lipomas occurring inside the SMG are more common than other variants.
Moreover, considering that the types and characteristics of neoplasms of the parotid gland differ from those of the SMG, the fact that most lipomatous tumors that occur in the parotid gland are ordinary lipomas may not be applicable to the SMG. Therefore, the present case may be helpful for future studies on the lipomatous lesions in the SMG, including those on the incidence rate or ratio of ordinary lipoma and its variants.
Trauma is one of the causes of lipoma, and several cases of ordinary lipoma of the parotid gland following trauma have been reported. 10 The fact that the SMG is protected by the mandible, with lesser exposure to the outside environment compared to the parotid gland may be a possible explanation for the difference in the occurrence of ordinary lipomas of the parotid gland and SMG. In this case, the patient denied a history of trauma to the neck and oral cavity, and the tumor occurred in the medial side of the SMG, so the relationship with trauma seems to be negligible.
The treatment of lipomatous masses involves complete surgical resection. 4 Lumpectomy is not recommended for parotid gland lesions, except in some cases, owing to the risk of facial nerve damage. Although tumor resection can be performed for submandibular lesions, submandibular resection was performed in this case, considering the location of the tumor and the needs of the patient, who did not want to undergo a possible reoperation. 7
In conclusion, we treated an intraglandular ordinary lipoma of the right SMG in a 65-year-old man with submandibular resection. Macroscopically, the tumor had a yellow, homogeneous cut surface and with partial adhesion with the gland. Microscopically, it was composed of mature adipocytes, which were separated by thin fibrous connective tissue, and was partially mixed with the parenchyma of the salivary gland. Thus, we believe this report will be very helpful for the understanding of lipomatous tumors of the SMG.
Footnotes
Authors’ Note
This study was approved by the institutional review board of Veterans Health Service Daejeon Hospital. The authors have obtained the patient’s informed consent.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by a VHS Medical Center Research Grant, Republic of Korea (grant number: VHSMC 19026).
