Abstract

Introduction
Tapia syndrome is characterized by extracranial ipsilateral paralysis of the hypoglossal nerve and the recurrent laryngeal branch of the vagal nerve. 1 This syndrome can occur after any surgical procedure that is performed by general anesthesia, mask ventilation, or the use of laryngeal mask airway probably due to a neuropraxic response to the pressure of the inflated cuff of the tube or mask. 2 The common symptoms in patients with Tapia syndrome are hoarseness, dysphonia, and difficulty in swallowing. 3
Case Report
A 36-year-old woman was consulted to our otolaryngology department due to hoarseness, swallowing difficulty and deviation of the tongue following a total thyroidectomy operation due to multinodular goiter. In physical examination, there was deviation of the tongue to the left side (Figure 1) and left vocal fold paralysis. According to the patient’s file, before the thyroidectomy, she had a 2-cm nodule on the right thyroid lobe and a 3-cm nodule on the left thyroid lobe. She underwent total thyroidectomy 1 day ahead. According to the surgical report, neuromonitoring for recurrent laryngeal nerve had been used, initially the left lobe was resected, and after monitoring the normal function of the left recurrent laryngeal nerve function, the right lobectomy was performed and the superior pedicle of the left thyroid lobe did not reach the region of the carotid bifurcation and the anatomical route of the hypoglossal nerve. The patient’s neurologic examination, evaluation of computed tomography and magnetic resonance imaging images were performed by a neurologist to exclude central nervous system pathologies. Methylprednisolone 1 mg/kg oral steroid was given for 10 days empirically. To avoid the aspiration due to paralysis of hypoglossal and vagal nerves together, the patient received nutrition through a nasogastric tube for a month until the vagal nerve recovery. The hypoglossal nerve gradually recovered 3 months after the surgery.
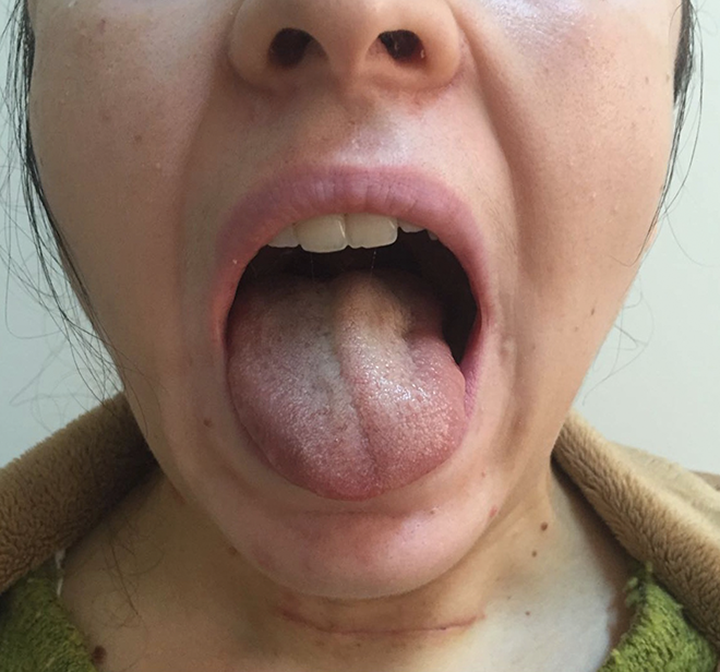
Deviation of the tongue to the left side.
Discussion
Anatomically, on the most lateral prominence of the anterior surface of the transverse process of the first cervical vertebra, the hypoglossal nerve lies and crosses the vagal nerve. 4 This close relationship between vagal and hypoglossal nerve may reveal the most plausible mechanism of concomitant nerve damage in a patient. If hyperextension of this joint occurs, it is likely that these nerves would be stretched and pressed against this prominence.
Thyroidectomy is a quite often performed surgical procedure and has various complications such as postoperative bleeding, hypocalcemia, unilateral, or bilateral vocal folds paralysis. 5 In a thyroidectomy patient, the differentiation of the cause of vocal fold paralysis could be difficult. The most common reason is a direct injury to the nerve while another rare reason is Tapia syndrome. The recognition of Tapia syndrome is much easier after other surgical procedures without nerve manipulation. Although the surgeon is confident that the recurrent laryngeal nerve is not damaged, such a complication may put him in a difficult position until the nerve function recovers. To the best of our knowledge, this is the first case report in the literature reported after thyroidectomy operation.
To avoid such a problem, maximum attention should be paid for proper localization of the head during surgery. This situation is particularly important when surgery includes areas located close to the vagal and hypoglossal nerve anatomic routes. Therefore, perioperative nerve monitorization should be done in surgeries working close to these nerves.
Footnotes
Authors’ Note
Written informed consent was obtained from the patient for publication of this case report and accompanying images.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
