Abstract
We conducted a retrospective study to reexamine the value of single-photon emission computed tomography (SPECT) in the evaluation of patients with neurotologic complaints, and to assess the intra- and inter-radiologist variability of SPECT readings. Our study population was made up of 63 patients—23 men and 40 women, aged 34 to 91 years (mean: 59)—who had presented to a tertiary care otolaryngology practice and university hospital for evaluation of head trauma, sensorineural hearing loss, tinnitus, and/or vertigo. All patients had undergone brain scanning with SPECT during their evaluation, and almost all had also undergone magnetic resonance imaging (MRI) and standard computed tomography (CT). We compared the findings of all three imaging modalities in terms of their ability to detect neurotologic abnormalities. We found that detection rates were very similar among the three modalities; abnormalities were found in 24% of SPECT scans, 26% of MRIs, and 23% of CTs. Nevertheless, we did find that among 60 patients who underwent all three types of imaging, 13 (22%) exhibited areas of cerebral hypoperfusion on SPECT while their MRIs and CTs were read as either normal or nonspecific. In all, 18 of these 60 patients (30%) exhibited normal or nonspecific findings on all three types of imaging. In addition, when SPECT scans were read by the same radiologist at different times, different results were reported for 17 of the 63 scans (27%). Likewise, when SPECT scans were read by different radiologists, different results were reported for 21 of 63 scans (33%). We conclude that SPECT may be a valuable complementary diagnostic modality for making a comprehensive neurotologic evaluation and that it may detect abnormalities in some patients whose other imaging is read as normal. However, we did not find that SPECT was the most sensitive of the three modalities in neurotologic evaluation, as we had previously found in a preliminary study that the senior author (R.T.S.) published in 1996. In addition, with respect to our radiologists, both their intra- and inter-reader reliability was low, and we recommend additional study on this matter.
Introduction
Single-photon emission computed tomography (SPECT) evaluates tissue metabolism by detecting electromagnetic radiation emitted from intravenous tracers. Technetium-99m hexamethylpropyleneamine oxime (99mTc-HMPAO) is a tracer used to specifically assess brain metabolism. The radioactive 99mTc emits gamma rays, and the hydrophobic HMPAO enables their passage through the blood-brain barrier and subsequent trapping via its hydrophilic conversion. 13 Because the diffusion of 99mTc-HMPAO into brain parenchyma is dependent on blood flow, 99mTc-HMPAO SPECT can be used to infer cerebral perfusion, with local ischemia appearing as areas of hypoperfusion. 2
SPECT is a well-established imaging modality for patients with epilepsy,2,4 cerebrovascular disease,2,5 neoplastic processes,2,6 and dementia.2,7–9 A few studies have also examined its use in head trauma10–13 and traumatic anosmia.14,15 The value of SPECT in these disorders is related to its ability to detect variations in cerebral blood flow, which have been suggested as an etiology for hearing loss,16,17 tinnitus, 16 and vertigo. 18
While SPECT has shown promise for evaluating patients with sensorineural hearing loss (SNHL),19,20 tinnitus,19,21 and vertigo,19,22,23 there remains insufficient evidence to support the routine integration of SPECT into clinical neurotology. The ability of SPECT to augment information provided by magnetic resonance imaging (MRI) and standard computed tomography (CT) requires clarification. To this end, we prospectively compared the results of SPECT, MRI, and CT in patients who presented for evaluation of head trauma, SNHL, tinnitus, vertigo, or a combination of these conditions.
The findings of a previous preliminary study led by the senior author (R.T.S.) had suggested that SPECT was superior to MRI and CT in detecting abnormalities related to these same complaints. 19 The goals of the present study were to see if we could reproduce the findings of our previous study. We also determined the intra- and inter-reader reliability of SPECT interpretations.
Patients and Methods
We reviewed the records of 63 patients—23 men and 40 women, aged 34 to 91 years (mean: 59)—who had undergone SPECT for the evaluation of head trauma, SNHL, tinnitus, vertigo, or a combination of these conditions. Of these 63 patients, 62 also underwent MRI (98%) and 60 underwent standard CT (95%); a total of 60 patients underwent all three. The amount of time required for patients to complete these diagnostic procedures ranged from 1 day to 6 months.
All SPECT scans included images obtained in axial, coronal, and sagittal planes. They were obtained at Hahnemann University Hospital with a 99mTc-HMPAO radiotracer (Siemens; Munich) outfitted with a camera (E-Cam, Dual-Head, Signature Series Gamma Camera; Siemens). These cameras were calibrated with daily intrinsic uniformity flood testing, monthly intrinsic uniformity testing, and monthly center-of-rotation quality control to provide the most accurate imaging. As a result, there was very little to no chance of their producing a false-positive result. The MRIs and CTs were performed at various institutions.
SPECT findings were classified as abnormal when perfusion defects were seen in areas that correlated well with the location of the patients chief complaint, such as the temporal lobe, the higher auditory cortex, and the basal ganglia. For purposes of this study, all other observed defects that were not associated with the patient's complaint were classified as normal. This classification protocol represented an important difference between the present study and our previous study 19 because in the previous study, every perfusion defect seen on SPECT was classified as abnormal, regardless of whether it was associated with the patient's presenting sign or symptom. All our study results were tabulated on the basis of first readings rather than subsequent readings.
Analysis of SPECT findings was also performed to assess intra- and inter-radiologist variability. Two radiologists (P.J.C. and J.D.) read all the scans. Intra-radiologist variation was determined by having each radiologist read all the SPECT scans again at a later date and compare the findings with those of the first reading; for their second reading, the radiologists were blinded to the patients personal and clinical data and to the result their initial reading. Inter-radiologist variation was determined by comparing the two radiologists’ interpretation of each SPECT scan.
For both intra- and inter-reader analyses, we chose four categories of outcomes:
Agreement normal: Both radiologists judged that the findings of a particular scan were normal or nonspecific.
Agreement abnormal: Both radiologists found that a particular scan was abnormal.
Disagreement: One radiologist interpreted a particular scan as normal or nonspecific while the other found it to be abnormal.
Partial agreement: Both radiologists found that a particular scan was abnormal, but they disagreed over the degree of the abnormality.
Results
Abnormalities were found in 15 of the 63 SPECT scans (24%), 16 of the 62 MRIs (26%), and 14 of the 60 CTs (23%) (table 1). All SPECT abnormalities were characterized as areas of hypoperfusion. Among the 60 patients who underwent all three imaging investigations, 18 (30%) had normal or nonspecific findings on all three.
We also calculated the sensitivity of each imaging modality according to the patient's presenting sign or symptom (table 2). In all categories, MRI was the most sensitive modality.
Comparison of the Sensitivity of SPECT, MRI, and CT in Detecting Abnormalities

Sensitivity of the Three Diagnostic Modalities According to Chief Complaint
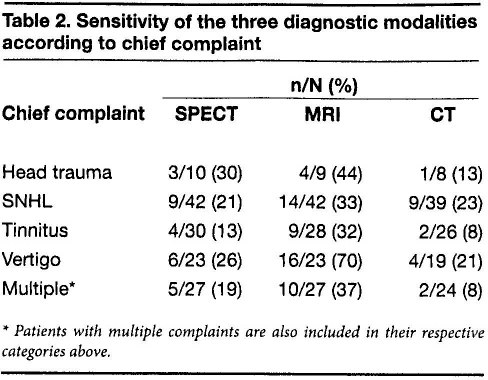
Patients with multiple complaints are also included in their respective categories above.
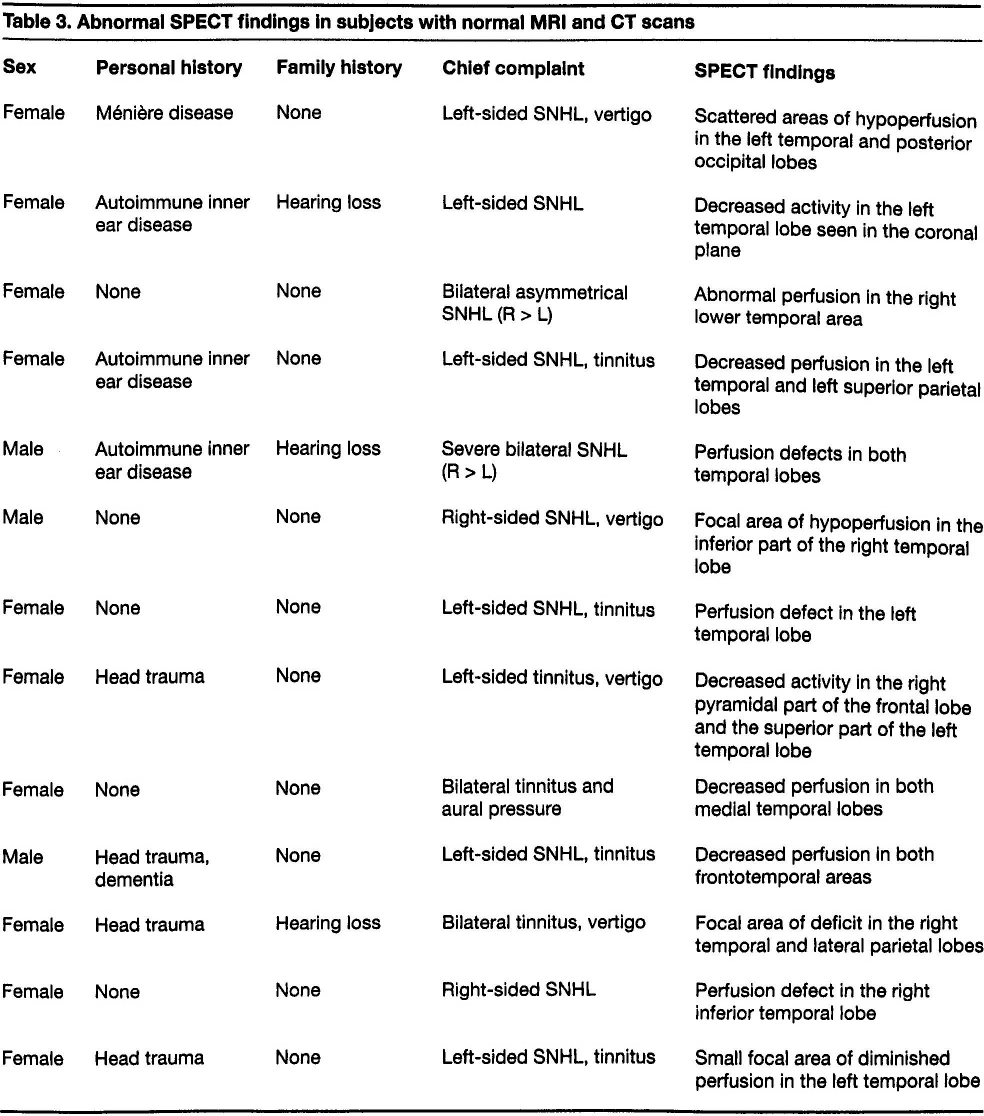
Of the 60 patients who underwent SPECT, MRI, and CT, 13 (22%) exhibited areas of cerebral hypoperfusion on SPECT, but their MRI and CT scans were read as either normal or nonspecific (table 3). Ten of the 13 (77%) had a chief complaint of SNHL, 2 (15%) had a chief complaint of tinnitus and vertigo, and 1 (8%) had a chief complaint of bilateral tinnitus and aural pressure. Of the 10 patients with SNHL, 4 had idiopathic SNHL, 3 had autoimmune inner ear disease, 2 had a history of head trauma, and 1 had Ménière disease. Two of the 10 patients with SNHL had a family history of hearing loss.
Abnormal SPECT Findings in Subjects with Normal MRI and CT Scans
Our analysis of intra-radiologist variability revealed agreement normal on 39 scans (62%), agreement abnormal on 4 scans (6%), disagreement on 17 scans (27%), and partial agreement on 3 scans (5%) (table 4). Combining the first two categories revealed complete agreement on 43 scans (68%), and adding partial agreement raised the total to 46 scans (73%).
Intra- and Inter-Reader Variability in SPECT Interpretations
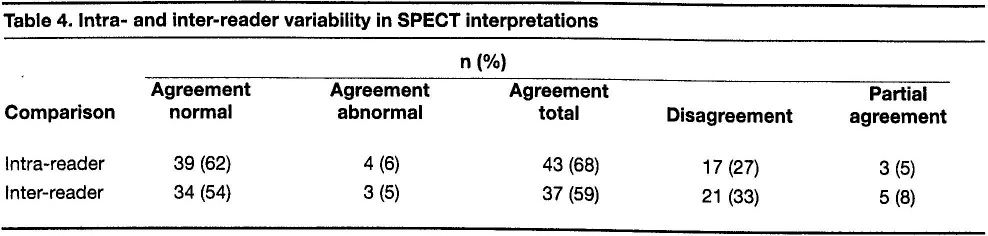
Our analysis of inter-radiologist variability found agreement normal on 34 scans (54%), agreement abnormal on 3 scans (5%), disagreement on 21 scans (33%), and partial agreement on 5 scans (8%) (table 4). Combining the first two categories revealed complete agreement on 37 scans (59%), and adding partial agreement raised the total to 42 scans (67%).
Discussion
SPECT is an intriguing yet poorly characterized diagnostic modality in clinical neurotology. By measuring subtle variations in cerebral perfusion, SPECT can provide insight into disease processes that are undetectable by MRI or CT. However, there remains a paucity of longitudinal, prospective studies that compare the utility of SPECT, MRI, and CT in the evaluation of neurotologic complaints.
Head trauma
The neurotologic complaints of the 4 patients with a history of head trauma began following the trauma and were believed to be associated with it. Authors of previous reports found similar SPECT scan abnormalities in patients with head trauma.11–15
Hearing loss
A number of vascular factors have been proposed as a cause of SNHL, including embolic and thrombotic arterial occlusion, hypotension, vasospasm, vasculitis, and migraine headache. 17 Investigation of the usefulness of SPECT in the evaluation of SNHL is limited. In a previous study, we found that SPECT was superior to MRI and CT for detecting abnormalities in patients with SNHL, with detection rates of 74, 58, and 45%, respectively. 19 Kim et al found that SPECT was able to detect cerebral perfusion defects in patients with SNHL and a normal MRI. 20 Berrettini et al showed that SPECT was useful in the diagnosis 24 and the quantification of disease activity 25 in otosclerosis; they also found that its sensitivity for detecting otospongiotic foci was higher than that of CT.
In our study, we found that MRI appeared to be superior to SPECT and CT for detecting abnormalities in patients with SNHL, with detection rates of 33, 21, and 23%, respectively (table 2). However, an important finding was that SPECT revealed areas of cortical hypoperfusion in 10 patients who had a chief complaint of SNHL, but the MRI and CT findings of these 10 patients were normal. Of these 10 patients, 4 had idiopathic hearing loss, 3 had autoimmune inner ear disease, 2 had a history of head trauma, and 1 had Ménière disease.
The pathophysiology of autoimmune inner ear disease is complex. Immunologic mechanisms—mainly the production of antibodies to inner ear supportive cell proteins—are believed to cause the damage to inner ear structures. In the 3 patients with autoimmune inner ear disease in our study, there was no evidence to suggest this disease could have caused the vascular changes that we saw on SPECT. We suspect that these changes were caused by other pathologies. In these 3 patients, symptoms persisted after treatment with steroids and cytotoxic drugs; there is no way to be certain if this persistence was due to incompletely responsive autoimmune disease or to other coincident pathology.
Although MRI may be more sensitive than SPECT in detecting soft-tissue pathology related to SNHL, these two modalities may complement each other in selected cases, since SPECT is able to detect perfusion defects that can be missed on MRI.
Tinnitus
The pathogenesis of tinnitus remains poorly understood. It has been suggested that vascular insufficiency may be a cause, but the inability of studies to show efficacy with hyperbaric oxygen has brought this hypothesis into question. 26 Tinnitus may be of central rather than peripheral origin, since some patients have reported tinnitus with a normal auditory periphery or after peripheral auditory ablation. 27
Gardner et al reported that SPECT found a higher number of alterations in regional cerebral blood flow among depressed patients with tinnitus compared with those without tinnitus. 28 Specifically, these alterations involved hypoperfusion in the frontal, parietal, and occipital cortex. In a controlled study, Farhadi et al reported a different finding in that tinnitus patients exhibited hyperperfusion of the associative auditory cortex, specifically the middle temporal gyrus and the inferior temporal and temporoparietal areas. 21
In our study, we found that MRI was superior to SPECT and CT for detecting abnormalities in patients with tinnitus, with detection rates of 32, 13, and 8%, respectively (table 2). However, there were 3 patients with tinnitus whose SPECT scan revealed areas of cortical hypoperfusion while their MRI and CT were normal. This again suggests that although MRI may be more sensitive than SPECT for detecting abnormalities related to tinnitus, the two modalities may be complementary.
Vertigo
The vascular etiologies of vertigo include migraine disorder, cerebrovascular accidents (particularly in the vertebrobasilar system), neurovascular compressive disorders, vasculitis, and ischemia from aging and other causes, among others. 18 Krishna et al reported that SPECT could reveal areas of ischemia from such vascular disorders earlier than MRI could. 23 According to Arai et al, SPECT in conjunction with magnetic resonance angiography can be useful in distinguishing peripheral vestibular disorders from central vestibular disorders. 29
Several studies have shown that SPECT was superior to MRI and CT in detecting perfusion abnormalities in patients with vertigo. 22 Our previous study found detection rates of 74, 58, and 48%, respectively, in patients with vertigo. 19 In our present study, however, we found that MRI was superior to SPECT and CT in this regard, with detection rates of 70, 26, and 21%, respectively (table 2). However, there were 3 patients with vertigo whose MRI and CT were normal but whose SPECT revealed areas of cortical hypoperfusion.
SPECT interpretation
Interpretation of SPECT scans is subjective. Given the difference in the results between our present study and our previous study, we decided to analyze the intra- and inter-radiologist variations in SPECT readings. It remains unclear whether the radiologists in our earlier study over-read the scans or if subtle vascular abnormalities are missed routinely by SPECT scans at most other institutions. None of the radiologists involved in our previous study was involved in the present investigation.
When we analyzed intra-reader variability by combining the totals for agreement normal, agreement abnormal, and partial agreement, we found that our radiologists made the same interpretation of a given SPECT 73% of the time and an opposite interpretation 27% of the time (table 4). The results of inter-reader variability were similar, as the two radiologists agreed with each other's interpretation of a given SPECT 67% of the time and disagreed with each other 33% of the time.
These intra- and inter-reader results were lower than what would be expected. Based on our findings, perhaps new protocols should be considered within radiology departments so that SPECT scans are routinely read by more than one radiologist. We suspect that differences in interpretation may contribute significantly to the differences and inconsistencies in the literature related to the value of SPECT. We feel it is important to convey our findings to encourage further study of the reliability of SPECT imaging reports and to highlight the limitations of this modality so that these scans might be interpreted more carefully in patients with neurotologic disease.
Conclusion
The present study did not confirm the results of our previous study, 19 which showed that SPECT was superior to MRI and CT for the evaluation of neurotologic complaints. We recognize that our small sample size is a significant shortcoming of the present study. Indeed, the neuropsychological evaluation appeared to be more sensitive than SPECT, MRI, and CT, but no meaningful conclusions can be reached regarding its applicability to the evaluation of neurotologic complaints because of the sample size. We also recognize that the fact that a fair percentage of patients had multiple neurotologic complaints might have affected our results. However, our present study does support the conclusion we reached in our previous study that SPECT can be a valuable adjunct to MRI and CT in the diagnosis of neurotologic complaints.
In some patients, SPECT allowed for the detection of abnormalities that were missed by MRI and CT. Our findings also contribute to our understanding of neurotologic conditions in that they support the theory that hearing loss, tinnitus, and vertigo may be caused by, or at least be associated with, changes in regional cerebral blood flow.
Unfortunately, the somewhat disappointing rates of intra- and inter-radiologist agreement in interpreting SPECT scans suggest that SPECT's value may be limited in neurotologic evaluation. However, we believe that the reliability and validity of SPECT can probably be improved by adopting protocols that require routine independent readings by more than one radiologist. Improving the specificity of SPECT scan interpretation is crucial to advancing the diagnostic capacity of this imaging modality so that it can be integrated successfully into the standard evaluation of patients with neurotologic complaints. Further study of this recommendation and of the neurotologic value of SPECT is encouraged.
