Abstract
Evaluating psychosocial outcomes in families of children with chronic health conditions is complicated by heterogeneity in impact across and within conditions. This study used goal attainment scaling to assess individual families’ progress towards child behaviour goals following brief parenting support for families of children (2–11 years) with phenylketonuria (PKU). Twelve hospital-recruited families nominated up to two behaviour goals and completed baseline monitoring before attending two 2-hr Healthy Living Triple P group sessions. Monitoring was repeated at 4-weeks post-intervention and 4-month follow-up. Families reported partial or complete success on 20 of 23 goals by follow-up. Nine goals were PKU-related, focusing on formula intake for younger children and dietary independence for older children; 14 were general, targeting aggression/non-compliance in younger children, with older children’s goals more varied. Goal attainment scaling is feasible and effective for monitoring progress towards individually tailored child behaviour goals, with potential applications in research and clinical care.
Introduction
Phenylketonuria (PKU; OMIM 261600) is an autosomal recessive inborn error of metabolism (IEM) (Scriver & Kaufman, 2001) resulting from a deficiency of the enzyme phenylalanine hydroxylase and characterised by elevated blood phenylalanine (Phe) levels (Enns et al., 2010). Newborn screening and adherence to effective dietary interventions now prevent severe neurological sequelae, although neuropsychological complications are still observed when Phe control is suboptimal (Enns et al., 2010; Singh et al., 2014; Trefz et al., 2011; Vockley et al., 2014). Consistent monitoring of Phe levels and adherence to dietary management are therefore key to successful management of this condition and optimal child health and developmental outcomes (Macleod & Ney, 2010; van Wegberg et al., 2017).
Dietary treatment for children with PKU is individually tailored but typically involves severe restrictions in natural protein intake and supplementation with Phe-free amino acid/glycomacropeptide (GMP) formulas plus or minus the addition of sapropterin for those with a BH4 responsive form of PKU to support adequate nutrition and growth, which can be challenging for children and parents to manage (Simon et al., 2008). Parents play a central role in children's chronic health condition management (Morawska et al., 2015), and it is well-recognised that good PKU management requires a holistic family-centred approach that promotes psychosocial wellbeing and quality of life for children and families (Borghi et al., 2019; Feillet et al., 2010; Medford et al., 2018; Vegni et al., 2010). However, as noted in the broader literature on genetic disorders, there is often an implicit assumption that treatment should primarily be medical, which may contribute to the limited number of behavioural intervention studies in PKU and similar conditions (Hall, 2009; Moskowitz et al., 2011; Zarcone et al., 2008). This trend has been observed in other rare genetic disorders, where behavioural interventions remain relatively underrepresented compared to psychopharmacological approaches (e.g., galactosemia: Finestack et al., 2022; fragile X syndrome: Moskowitz & Jones, 2015; Prader-Willi syndrome: Bedard et al., 2025; Kodra et al., 2016).
Childhood behaviour problems appear to be more intense among children with PKU compared to healthy controls (Ambler et al., 2018; Jusiene & Kučinskas, 2004), and when children with PKU exhibit greater intensity of emotional and behavioural difficulties, these are associated with worse child and parent quality of life (Morawska et al., 2020). While parenting interventions are the gold standard treatment for child behavioural and emotional problems, they have been rarely examined in the context of chronic childhood health conditions (Morawska et al., 2015; Mitchell et al., 2020). One of the challenges of developing and testing interventions for specific childhood health conditions is that while overall numbers of children with chronic health conditions are high (Van Cleave et al., 2010), many individual conditions are relatively rare (e.g., 1 in 10,000 individuals for PKU; Scriver & Kaufman, 2001) and heterogeneous in terms of psychosocial impact and sequelae within and across conditions. This presents a problem for conducting randomised clinical trials of parenting interventions, in part because standardised parent-report measures typically used in the broader parenting interventions literature (e.g., the Strengths and Difficulties Questionnaire, Goodman, 1997; Eyberg Child Behavior Inventory, Eyberg, 1999) may be inappropriate or lack sensitivity to change in these populations. Furthermore, standardized measures developed for populations with developmental disabilities (e.g., Vinelands) are also unlikely to be appropriate for PKU, as children with PKU who are diagnosed and managed from birth typically do not present with adaptive behaviour challenges, global developmental delays, or intellectual impairment. Instead, their challenges are more specific to the unique psychosocial demands of PKU, in particular, emotional and behavioural regulation within the context of dietary management.
An alternative approach is to use individually tailored assessment to evaluate intervention efficacy, such as by applying goal attainment scaling (Kiresuk & Sherman, 1968; Logan et al., 2022). In this approach, parents set individual goals for change in specific child behaviours that are of concern to them, and progress towards these goals is tracked over the course of the intervention and follow-up period. Goal attainment scaling is gaining increasing attention as it enables greater family involvement in treatment planning, allows for more tailored intervention delivery and provides a more detailed evaluation of intervention outcomes (Gaasterland et al., 2016; Krasny-Pacini et al., 2013; Shankar et al., 2019; Vu & Law, 2012). It has been applied in outcome evaluation of parenting interventions in the context of childhood disability (Mazzucchelli et al., 2018), in paediatric rehabilitation (Harpster et al., 2019), and in psychosocial interventions for autism (Ruble et al., 2012). There is evidence that it complements existing validated measures and increases sensitivity of outcome measurement (Steenbeek et al., 2011).
The current study is part of a larger project examining the wellbeing of children with PKU and evaluating the efficacy of a brief, group-based parenting program in reducing parenting stress, improving parenting skills, reducing child behavioural and emotional difficulties, and improving the impact of PKU on health-related quality of life for families of children with PKU. Relationships between parenting variables and impact of PKU on quality of life at baseline (Morawska et al., 2020), and primary outcome data from a pre-post intervention study which showed moderate to large intervention effects on parenting style, and also assessed children’s behavioural and emotional adjustment and quality of life (Mitchell et al., 2021), are reported elsewhere. In addition to standardised parent-report questionnaires, the intervention study used goal attainment scaling to assess progress towards individualised child behaviour goals that parents set for their children. This current study examines the types of child behaviour goals that parents set and provides longitudinal data illustrating families’ progress towards both PKU-related and general child behaviour goals across the intervention and follow-up period. The overall aim is to explore the nature and diversity of child behaviour problems experienced by parents of children with PKU and provide a detailed account of the application of goal attainment scaling in this population.
Method
The study employed a single-phase, concurrent, across-participant design using a case series approach. Families of young children who were attending the Queensland Lifespan Metabolic Medicine Service (QLMMS) at the Queensland Children’s Hospital (QCH) for the treatment and management of PKU were invited to participate in a study of a parenting intervention. Eligibility criteria: children (i) aged 2 to 12 years, (ii) diagnosed with PKU, and (iii) currently prescribed a protein-restricted diet and Phe-free amino acid/GMP formula supplementation. Ineligibility criteria: (i) child physical or intellectual disability, (ii) child under care of Department of Communities, (iii) inability of parent to read an English-language newspaper, or (iv) parent disability affecting cognition. The Human Research Ethics Committees of the University of Queensland and Children’s Health Queensland approved the conduct of the research.
Procedure
All potentially eligible families received printed study information and consent forms, and eligibility and willingness to participate were assessed by telephone screening interviews. Consenting parents returned consent forms, completed baseline parent-report assessment measures, and nominated two goals for child behaviour change before being randomly allocated to 1-, 2-, or 3-weeks of pre-intervention child behaviour monitoring. Computer-generated random number lists were used to produce the randomisation sequence, and allocation was concealed from the research team using sequentially numbered opaque envelopes. Envelopes were assigned by the research coordinator in the order in which baseline parent-report assessment measures were completed; however, blinding of researchers and participants to length of child behaviour monitoring was not possible since length of behaviour monitoring depended on group allocation.
Families were booked into intervention group sessions once their pre-intervention (T1) child behaviour monitoring was complete. A further one week of child behaviour monitoring was undertaken at 4-weeks post-intervention (T2), and again at 4-month follow-up (T3). Details of children’s diagnosis and treatment plans, including clinical phenotype and prescribed medications and nutritional supplements, were obtained from the treating team. At the end of the follow-up period, records of routinely-collected blood Phe levels from 6 months pre- to 6 months post-intervention were obtained from the treating team with parental consent. Based on these values, average Phe levels were calculated both pre-intervention and post-intervention for comparison purposes.
Measures
The Family Background Questionnaire (Sanders & Morawska, 2010) was used to collect sociodemographic information (i.e., child, parent and family details) and included additional questions about the child’s PKU diagnosis and management.
The Goal Attainment Scale (GAS) (Turner et al., 2001) was used to assess children’s progress towards parent-nominated behaviour goals. Parents identified specific child behaviours they wished to change; used individualised structured monitoring sheets which were developed with the research coordinator at T1 to establish baseline duration or frequency of target behaviour occurrence; and set goals for change relative to this baseline. Monitoring was repeated at T2 and T3 to enable tracking of behaviour change and evaluation of progress towards behavioural goals over time. Progress is expressed in terms of percentage of improvement, from 0% (i.e., no improvement from baseline) to 100% (i.e., total success/goal attained). The GAS has demonstrated good convergent validity (Hudson et al., 1995; Tellegen & Sanders, 2014; Turner & Sanders, 2006).
Intervention
The intervention comprised two 2-hr Healthy Living Triple P group discussion sessions (Morawska et al., 2018). The intervention draws on the theoretical principles underpinning the Triple P–Positive Parenting Program (Sanders, 2012) and was designed as a cross-diagnostic (i.e., not health condition-specific) brief parenting intervention for families of children with one or more chronic health conditions. As the intervention is designed for families with children with a variety of health conditions, specific topics and thus parent goals can be tailored to during the course of the group sessions. For example, practitioners can tailor the specific examples of strategy application based on the needs to the parents in the group (e.g., praising children for drinking their formula more quickly). The group sessions provide an interactive experience with opportunities for role-play and discussion amongst participants, and proximal intervention targets are parenting skills and confidence. The program aims to enhance parental self-regulation and use of consistent parenting and disciplinary practices to support strong parent-child relationships, child cooperation and use of routine. It also aims to lower child and family stress and parent-child conflict.
Session 1 focuses on strategies to prevent and manage problems with the child’s health condition. Strategies include condition monitoring, adhering to medication/supplements or diets as prescribed, minimising symptoms, problem-solving to promote participation in family/school/recreational activities, supporting siblings, and fostering effective communication between parents, children and other caregivers. Session 2 introduces principles of positive parenting in the context of child chronic health condition management. The reasons why children with chronic health conditions are at increased risk of emotional and behavioural problems are introduced before examining common parenting traps. Multiple effective disciplinary methods are discussed, with a focus on creating environments conducive to caring relationships between parents and children.
Intervention Delivery
Given the broad geographical distribution of participating families, parents could opt to attend sessions in-person (at QCH) or via online videoconferencing. Further details of this are provided elsewhere (Mitchell et al., 2021); however, it is worth noting that no difference in program satisfaction was found between those who attended in-person compared to online. There were three discussion groups in total (two face-to-face, one online). Eleven families participated in face-to-face sessions, and the remaining six families via online delivery. Groups comprised an average of eight parents (M = 8.00, SD = 1.41) from five families (M = 5.33, SD = 0.47). Groups were facilitated by two clinical psychologists, both accredited Triple P practitioners. Catch-up sessions were required for three parents who missed one of their scheduled sessions due to family commitments. During this time, families continued regular medical management. No families reported accessing additional parenting support.
Protocol Adherence
Practitioners delivered the intervention according to a standardised manual (Morawska et al., 2018) and followed treatment delivery protocols. Structured session checklists completed by facilitators indicated that 98.2% of protocol content was covered during sessions. Group sessions were videotaped and 50% were reviewed and independently coded by another trained practitioner to assess protocol adherence, with 100% agreement between the coder and group facilitators.
Statistical Analyses
Statistical analyses were conducted using IBM SPSS 25. Visual inspection of the data examining trends for change in GAS scores was used to determine change. GAS scores were calculated based on baseline (T1) occurrence of the target child behaviours; progress towards goal attainment (0%–100% success) at T2 and T3 was calculated by comparing behaviour duration/frequency to the target goal duration/frequency. Success was coded such that 0% success represented no change or a worsening in the behaviour from baseline and 100% success represented total goal attainment or exceeding the behavioural goal. Goals were set by parents and GAS success scores were coded by two researchers independently, with 100% agreement among the researchers on obtained scores. Prior to coding, the duration/frequency of behaviour that represented 50% success was established for each behaviour goal; this represented a duration/frequency that was halfway between the baseline and the behaviour goal (100% success), with 25% and 75% success representing mid-points in between. Partial success was coded as either 25%, 50% or 75% dependent on which score the behaviour monitoring data were closest to.
Results
Participants
A flow diagram of participants can be seen in Figure 1. Forty-two potentially eligible families received study information and all but six were able to be contacted for screening interviews. Fourteen families declined to participate in the intervention due to time constraints, lack of perceived necessity or previous completion of a Triple P program. Of the 22 interested families who received T1 questionnaires, three did not complete them. The remaining 19 families were randomly assigned to 1-, 2- or 3-weeks of baseline monitoring. A further two families withdrew from the study prior to the intervention, resulting in an overall sample of 17 families.
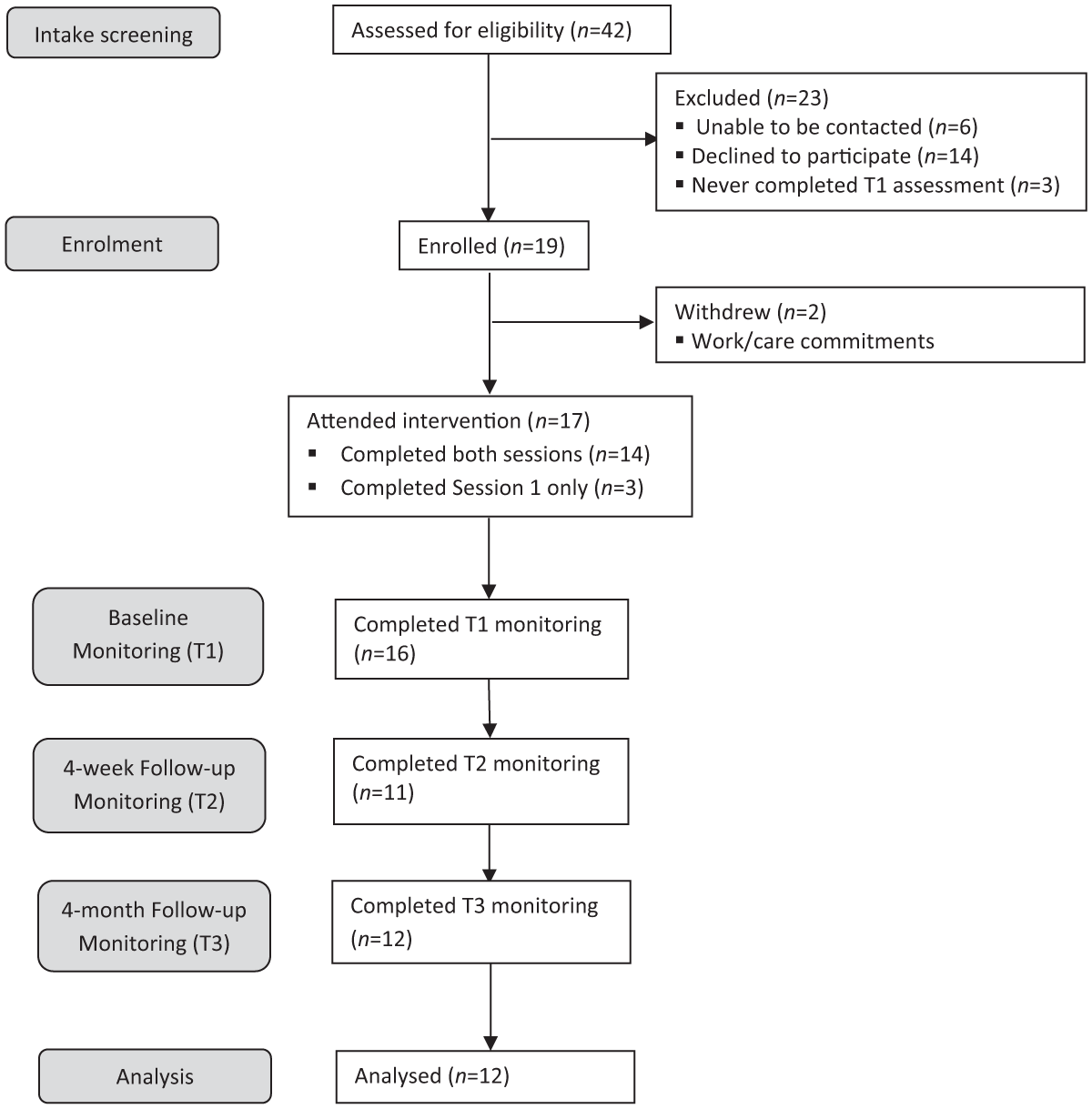
Flow diagram of participants throughout study.
Of these 17 families, five families were not included in analysis; four of these families completed monitoring at T1 only and one family provided no behaviour monitoring data. The remaining 12 of the 17 families completed child behaviour monitoring at multiple time points and were included in analysis. Eleven of these families completed child behaviour monitoring as per protocol, and one family provided monitoring data at T1 and T3 only.
Demographic information for participating families can be seen in Table 1. Children’s ages ranged from 2 to 11 years (M = 6.1 years, SD = 3.6). PKU diagnosis category is based on blood Phe level at time of diagnosis. In this sample, five children (41.7%) had classical PKU (blood Phe > 1,200 μmol/L), four (33.3%) had mild PKU (600–1,200 μmol/L), and three (25.0%) had hyperphenylalaninaemia (hyper-Phe; 360–600 μmol/L). Children’s lifetime Phe levels (mean of all routinely-tested Phe level results from birth to the current age) ranged from 182 to 429 μmol/L (M = 289.7 μmol/L, SD = 71.7).
Participant Characteristics (N = 12).
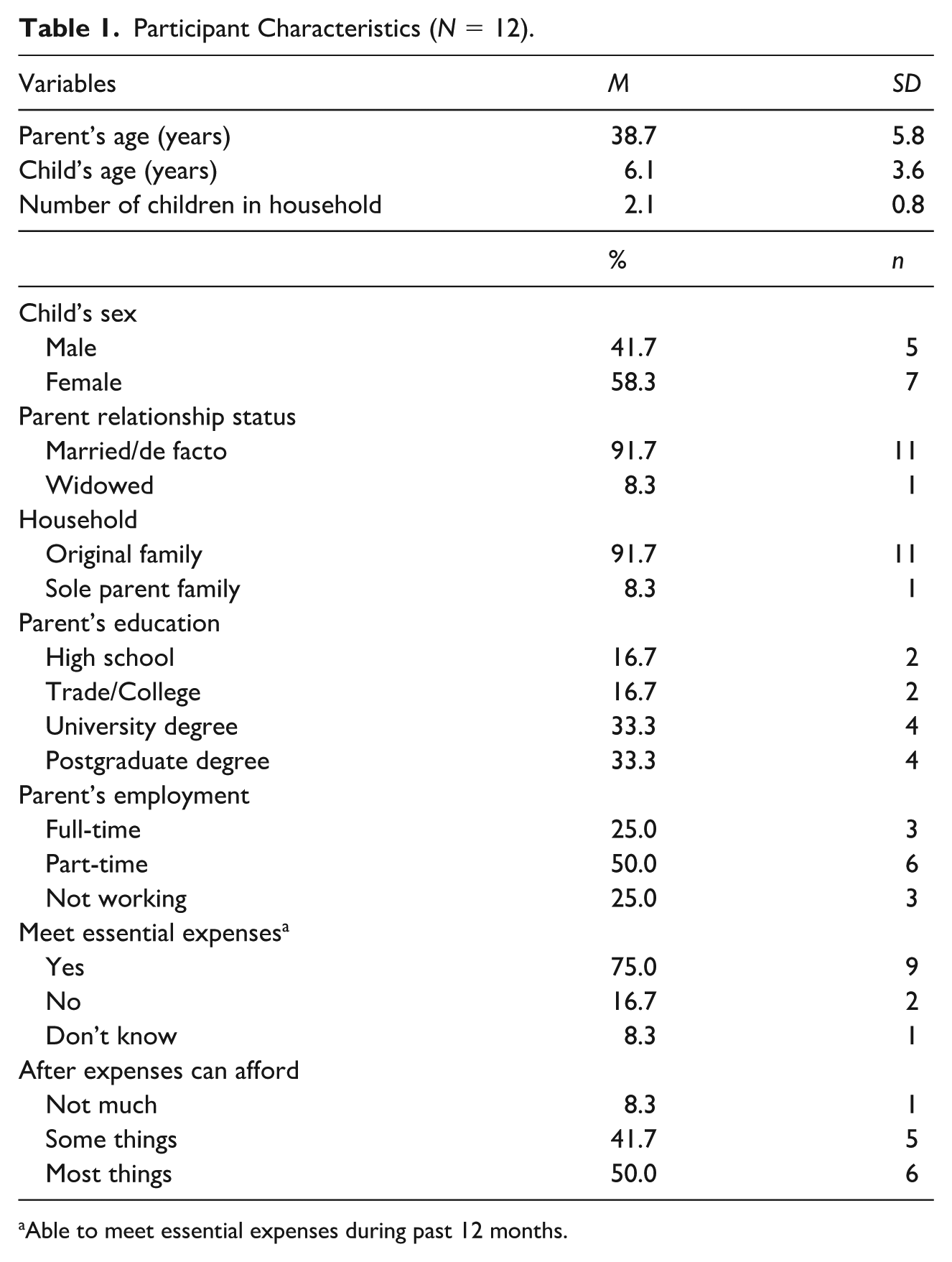
Able to meet essential expenses during past 12 months.
Goal Attainment Scale
Parent-nominated behaviour goals and corresponding outcomes on the GAS at T2 and T3 can be seen in Figures 2 and 3. Of the 12 families who provided behaviour monitoring data at multiple time points, four provided the requested amount of monitoring data as per their assigned baseline monitoring condition. Three families provided more days of baseline monitoring data than they had been assigned to, and five families provided less baseline monitoring data than their assigned randomisation condition. Given the small number of families involved, monitoring data were analysed irrespective of the originally assigned length of monitoring.
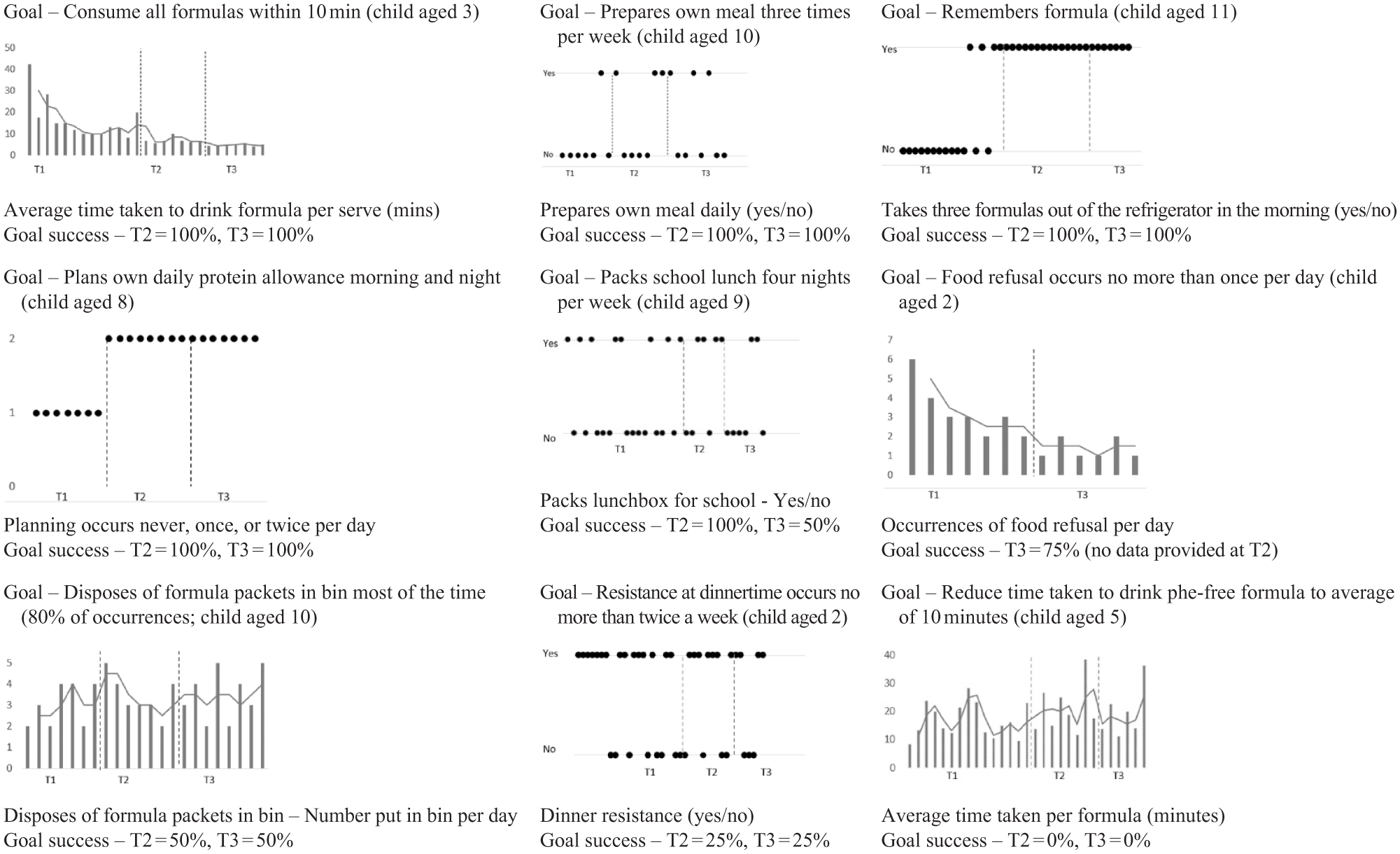
PKU-related behavioural goals arranged in order from most to least % success towards goal at T2 and T3.
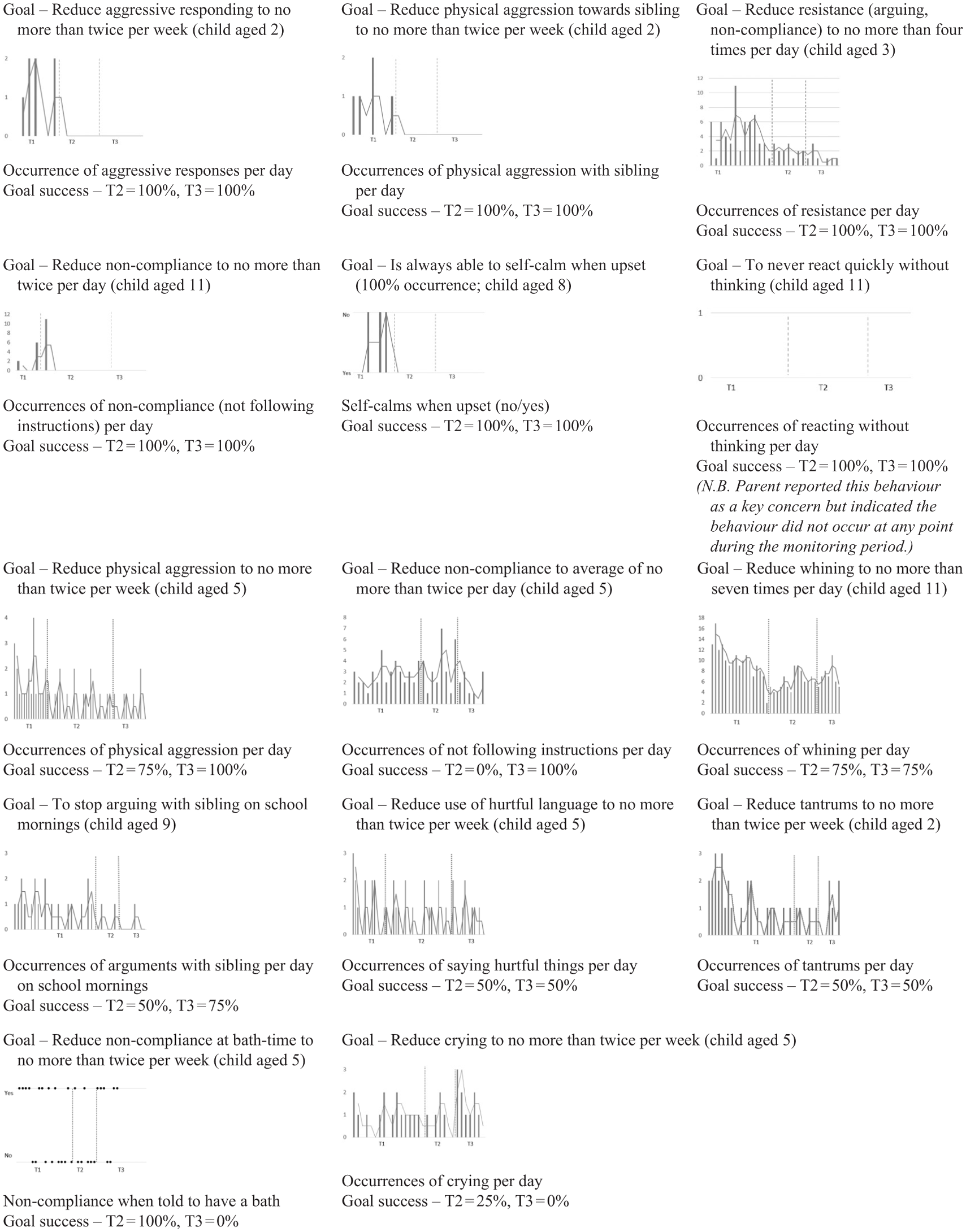
General behavioural goals arranged in order from most to least % success towards goal at T2 and T3.
In total, there were 23 behavioural goals nominated by the 12 families: nine PKU-related behaviour goals and 14 general behaviour goals. Eleven families nominated two goals each, and the remaining family elected to have only one goal as this was their primary and only concern and something they found challenging to manage in light of their child’s PKU. All 12 families achieved partial or complete success with at least one of their goals by T3; overall, families achieved partial or complete success with 20 out of the 23 goals by T3.
PKU-Related Behavioural Goals
Individual case series graphs plotting child behaviour monitoring data for PKU-related behavioural goals at T1, T2 and T3 can be seen in Figure 2. Parents provided monitoring data for eight of the nine PKU-related behaviours at T2; families achieved 100% success with five goals, partial success with two goals and no success with one goal. By T3, families had maintained 100% success with four goals and had partial success with four goals, as one behaviour reduced from 100% success at T2 to 50% success at T3. Only one behaviour did not improve by T2 or T3.
Trends can be seen in the type of PKU-related behaviour goals that parents selected based on their children’s age. As no children in this study were aged 6 or 7, children can be usefully grouped as either between 2 and 5 years old or 8 and 11 years old. For families with children aged 5 years and younger, PKU-related goals targeted either food refusal/resistance or the length of time it took children to drink their Phe-free/GMP formula. For older children, goals predominantly (i.e., for 4 out of 5 families) related to greater child autonomy over their PKU diet and supplement management (e.g., planning their own daily protein allowance and preparing their own meals).
General Behaviour Goals
Individual case series graphs plotting child behaviour monitoring data for general behaviour goals at T1, T2 and T3 can be seen in Figure 3. By T2, families achieved 100% success with seven goals, partial success with 6 goals, and no success with one goal. By T3, families had achieved 100% success with eight goals, partial success with four goals, and no success with two goals. All 14 behaviours saw improvement from baseline by T2 and/or T3. Eleven behaviours improved by T2, and improvement was maintained from T2 to T3; one behaviour only improved from T2 to T3; and two behaviours that had improved at T2 regressed to baseline by T3. It is worth noting that these two behaviours that reverted to 0% success at T3 both belonged to the same family; thus, nine of the 10 families who nominated general behaviour goals reported improvement by T3 compared to baseline.
Six of the seven families who had a child 5 years or younger set at least one goal related to general behaviour (nine goals in total). Of these, four goals were related to reducing physical or verbal aggression (e.g., physical aggression towards sibling) and three were related to reducing non-compliance generally or specifically (e.g., non-compliance at bath-time). Four of the five families with children aged eight to 11 years had at least one general behaviour goal (five goals in total). Unlike in the younger group of children, these five general behaviour goals were more diverse (e.g., self-calming, reducing whining, reducing arguing with siblings), and there were no clear common themes across these goals.
Discussion
Child behaviour problems are common among children with chronic health conditions, including PKU, and can affect adherence to condition management and child and family quality of life (Ambler et al., 2018; Morawska et al., 2020; Remor et al., 2024). This study detailed the use of goal attainment scaling to evaluate progress towards PKU-related and general child behaviour goals set by parents taking part in a brief, group-delivered parenting intervention for families of children with PKU. Behavioural goals that were selected by parents give insight into the daily lives of families of children with PKU and reveal some of the difficulties associated with parenting a child with PKU.
Reducing mealtime difficulties, particularly children’s food refusal/resistance, was a common goal nominated by parents of children aged 5 years and under. While mealtime difficulties are a common experience among the general population of parents of younger children (Mascola et al., 2010), for parents of children with PKU this can be particularly problematic given the necessary dietary restrictions that exist for these children and the importance of ensuring adequate nutrition despite these restrictions. To meet protein/amino acid requirements, children with PKU need to drink a Phe-free amino acid/GMP formula several times per day to supplement their protein-restricted diet. While medically necessary, Phe-free/GMP formula can be unpalatable (Rocha & MacDonald, 2016). Children who do not like the taste may take a long time to consume it (e.g., in the current sample at baseline, this was taking one child up to 42 min per serve), and several parents reported that they could only persuade their child to drink their formula by offering rewards, often in the form of screen time. As such, a PKU-related goal for two of the youngest children was to reduce the time they took to drink their Phe-free/GMP formula. By T3, one family had achieved 100% success with this goal, and average time to consume formula had dropped from 16.47 min to 4.74 min per serving. To our knowledge, this is one of the first studies to evaluate the effect of behavioural intervention on children’s cooperation with Phe-free/GMP formula consumption. This is an important outcome given that parents were typically needing to supervise their children with drinking their formula three to five times a day; this had therefore been taking up a substantial portion of the day and represented a significant source of stress for parents.
For children aged 8 years and older, parents’ PKU-related goals typically focused on increasing children’s autonomy with their PKU management. This reflected a perceived need for children to become more self-reliant as they got older and spent increasing amounts of time away from their parents. Parents expressed concern about their children needing to self-manage their diet given the potential ramifications of poor PKU management on children’s functioning and development, and therefore were very conscious of equipping them with the skills to do so.
In this sample of families, goals related to children’s general behaviour were not dissimilar to child behaviour concerns commonly reported by the general population of parents with children of the same age (Emerson & Einfeld, 2010; Ogundele, 2018). It is worth noting, however, that these common behavioural challenges can exacerbate the difficulty and stress associated with day-to-day PKU management tasks. For example, lack of compliance at bath-time adds extra stress to an already busy evening schedule that typically involves having to prepare a separate and carefully planned meal for the child with PKU that does not exceed their remaining protein allowance for the day.
There are clear benefits to using goal attainment scaling over traditional parent-report questionnaires. Working towards an individually selected goal enhances participant involvement in treatment planning and creates greater meaning and buy-in from participants during the intervention period, as goals act as a motivator for behavioural change (Epton et al., 2017; Killeen & Anaby, 2022). Monitoring also enhances participant insight into the target behaviour: for problematic behaviours, monitoring may help parents to recognise causes that contribute to behavioural difficulties, while, on the other hand, changes in parenting behaviour and other positive habits can be implemented to increase desired behaviours (Germann et al., 2007; Ivory & Kern, 2022). Additionally, participants receive immediate feedback on their child’s progress through the monitoring process and can see how they are tracking towards their goals.
Given the emphasis on individually tailored goals that parents determined based on their knowledge of their child’s capability and expectations of their behaviour, degree of goal difficulty or demand differed between participants. Whether the goals selected were indeed realistic for each individual child or not may help explain why some goals saw little or no improvement over the monitoring period. For example, substantially reducing resistance towards eating dinner may be an unrealistic target goal to set for a 2-year-old child with significant dietary restrictions. It is also worth considering whether multiple behavioural goals should be addressed at the same time, as was done in this intervention study, or whether it would be more beneficial to focus on one specific behaviour to target and monitor. The focus on a single behavioural goal may potentially result in more accurate behaviour monitoring as well as greater focus, targeting and, resultantly, more improvement on the child’s behaviour that is of most concern. Further, future research could collect qualitative data on parent experiences of goal attainment and program impact to provide richer insights into how the intervention supports families.
While the potential benefits of using the GAS are apparent, there may also be some drawbacks to reliance on parent-reported observational data. Specifically, as the child’s progress towards the goal can be clearly tracked during monitoring, social desirability could influence parents’ reporting. Additionally, this type of observational data ideally relies on in-the-moment reporting of the occurrence of target behaviours to enhance accuracy. If parents were to complete this reporting retrospectively, it may lead to reduced accuracy. It is worth also noting that this sample of parents constantly needs to track and monitor their child’s formula and protein intake which could result in either more astute monitoring of targeted child behaviour or reduced capacity to consistently monitor behaviour as well as PKU management. Future research could explore the use of ecological momentary assessment (EMA) to capture real-time monitoring data which may enhance accuracy and reduce recall bias compared to retrospective reporting (Russell & Gajos, 2020).
Limitations of the study need to be acknowledged, including the relatively small sample size and the fact that not all parents undertook monitoring and, as such, the sample may not be representative of all parents of children with PKU. Nevertheless, our recruitment of parents to the larger project did encompass a substantive proportion of all eligible families in Queensland, Australia. In addition, while we had randomly assigned families to different lengths of monitoring periods with the aim of implementing a multiple baseline design, we were unable to ensure that families followed the planned protocol. While we did have considerable monitoring data from individual families, a multiple baseline design would have provided a more rigorous approach to evaluating the effect of the intervention on child behaviour. As the study did not include baseline or comparison phases, we cannot draw causal conclusions about the effect of the intervention on child behaviour. Implementing the intervention concurrently across families also limits control over other factors that may have influenced outcomes, such as maturation or life events, and the absence of staggered or replicated phase changes reduces confidence in internal validity. As such, findings should be considered preliminary and useful for generating hypotheses rather than confirming intervention effects.
Conclusions
Parents of children with PKU participating in a brief parenting intervention derived considerable benefit from the program as demonstrated in individually monitored goals. Of note, parents could choose goals relevant to their child and these included both PKU-specific goals as well as more generic child behaviour goals. PKU-specific goal types also differed by child age, with the focus for younger children more on compliance with dietary requirements and for older children more on building autonomy and independence skills. These findings point to the need for clinicians to be aware of the diversity of parenting challenges experienced by this population and the utility of using a GAS approach in routine care.
Footnotes
Acknowledgements
We would like to thank all the families who participated in this research and the staff at the Queensland Lifespan Metabolic Medicine Service for their assistance with recruitment.
Ethical Considerations
This study received research approval from Children's Health Queensland Hospital and Health Service Human Research Ethics Committee (HREC/18/QRCH/162) and The University of Queensland Human Research Ethics Committee (2018001620).
Consent to Participate
All participants provided written informed consent prior to participation, which included permission to use de-identified data in publications.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by a grant from Children’s Health Queensland – Centre for Clinical Trials in Rare Neurodevelopmental Disorders, and Children’s Hospital Foundation Early Career Fellowships (AEM; award ref. no. 50223, ECF0112020). The funders had no role in the study design; the collection, analysis or interpretation of data; the writing of the report; or the decision to submit the article for publication.
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: The Parenting and Family Support Centre is partly funded by royalties stemming from published resources of the Triple P – Positive Parenting Program, which is developed and owned by The University of Queensland (UQ). Royalties are also distributed to the Faculty of Health, Medicine and Behavioural Sciences at UQ and contributory authors of published Triple P resources. Triple P International (TPI) Pty Ltd is a private company licensed by Uniquest Pty Ltd on behalf of UQ, to publish and disseminate Triple P worldwide. The authors of this report have no share or ownership of TPI. Dr Morawska receives royalties from TPI. TPI had no involvement in the study design, collection, analysis or interpretation of data, or writing of this report. Dr Kirby, Dr Morawska, and Dr Mitchell are employees at UQ.
Data Availability Statement
The datasets generated during and/or analyzed during the current study are not publicly available due to participant confidentiality, given the relatively small population from which this sample is drawn. However, data may be available from the corresponding author on reasonable request.
Trial Registration
ACTRN12618001564246
