Abstract
Aim
To discuss the potentials and barriers of establishing a course in facilitating journal clubs among non-medical health professionals (NMHP).
Background
NMHPs and managers had a wish to offer journal clubs. To accomplish this, there was a need of enhancing competences among NMHPs with developmental responsibility, both by education and practice in order to establish journal club in their own department.
Methods
A journal club facilitation course was offered to hospital employed NMHPs. Participants were asked to fill out questionnaires prior to, at midterm, 4 months, and 18 months after, course participation. At the 18-month follow-up, their managers were asked to fill out questionnaires. Results are discussed in an analytic framework inspired from research on conducting journal clubs and learning transfer.
Findings
After 18 months, only three journal clubs were established. Participants and managers mentioned barriers such as time, resources and interest from colleagues. Participants also disputed the management approval. Among the three established journal clubs, the participants stated good management approval, but also a challenge in establishing, preparing and conducting journal clubs.
Conclusion
Facilitation journal club courses have the potential to increase knowledge and skills. To secure implementation, further transfer strategies need to be considered as part of the course.
Introduction
The academic tradition among non-doctors in clinical settings in Denmark is still in its youth. Education at master level was introduced in the early 1990s, and 20 years later the number of PhD degrees is still low compared to medical staff. 1 Internationally the demand for and focus on evidence-based practice has exploded and along with this, the need and wish for practice based research. 2 The concept evidence-based practice is debated, however it is agreed that practitioners should be ensuring that patients receive care based on the best possible evidence.2–4 The combination of a need for production of research in order to enhance evidence-based practice, and the shortage of nurses and other non-medical health professionals (NMHPs) in the future, has led to a focus in the Nordic Countries on initiating non-medical research, capacity-building including strengthening research infrastructure and culture in hospital research strategies. 5 Among approaches to strengthen research culture in clinical settings, the establishment of journal clubs (JCs) is suggested.6,7 On this background, a series of JC facilitation courses was set up at a regional hospital in Denmark. The courses were aimed at clinical nurse specialists and other members of the NMHP-group with similar job profiles.
Background and aim
Research is not a new discipline at the hospitals outside the urban centres in Denmark. Here, the number of doctoral students and published professional and peer-reviewed articles are continually growing, but not to the same extent among NMHPs, where very few have academic degrees at master level and almost no one has doctoral degrees. As an example in the Region Zealand, 262 peer-reviewed articles were published in 2012, among them, five were written by researchers coming from the NMHP-group. 8 Documentation of developmental projects or establishment of JCs is also rare.
According to Honey and Baker,
9
JC can be viewed as: … a mechanism by which health care professionals can update their knowledge, promote critical thinking and research, assess the validity and applicability of the literature, improve skills in critical appraisal, increase the use of literature in clinical practice, and to influence changes in care practices. (p. 825)
JCs can have multiple aims, such as enhancing skills, methodological understanding and enhancing evidence-based practice. The evidence-based process can be described in five steps; Asking the clinical question, searching for the best evidence, critical appraising the evidence, addressing the sufficiency of the evidence, and evaluating the outcome of evidence. 6 In this process, a JC can be an important tool.
These systematic reviews give recommendations, and although Harris et al. 11 has shown positive results regarding improvements in reading habits, increased confidence in critical appraisal and increased ability to use findings in clinical practice, the impact of JCs to enhance evidence based practice is not clear.9,11 The seven recommendations point out important aspects, but it has not been possible to detect any literature regarding how to ensure the implementation of these recommendations and how to overcome the described potential barriers. Such barriers can be insufficient time, no authority to change or not cooperative with changes, statistics not understandable or results not generalizable. 12
Based on questionnaires to participants and their managers (in this article, managers refer to head nurses or equivalent positions), and with analytical inspiration from research on how to conduct a JC and learning transfer factors, the aim of the article is to discuss the potentials and barriers of establishing a course in facilitating JCs among NMHPs.
Setting and purpose of the JC course
This JC facilitator project is an uncontrolled longitudinal case study. 13 It took place at a large suburban hospital setting, employing more than 2,500 NMPHs at three different locations, among these approximately 2,000 nurses. In 2009, a vision and strategy for developing and supporting research culture among NMHPs were agreed among the head nurses and other leading member of staff. 14
One of the initiatives was a decision to offer a JC facilitation course to all NMHPs with developmental responsibilities. The background was an expressed wish coming from this group and from several managers to offer JCs in the organization. The purpose of the course was to enhance the participant’s competences in facilitating JCs both by education and by practicing, and finally to act as an opportunity in establishing a local network for JC leaders. In order to enhance local networking, and due to the limited amount of time clinicians have, the course was offered at all three locations. Locally-based librarians were connected to each group in order to support the process.
Invitation was sent via email to all leading NMHP staff and all staff with clinical specialist positions, representing 32 different wards. All NMHPs with developmental tasks were offered to participate in the course, and if relevant, leading staff could suggest other NMHPs with, as a minimum, a bachelor degree to attend the course.
Substance and form of the course
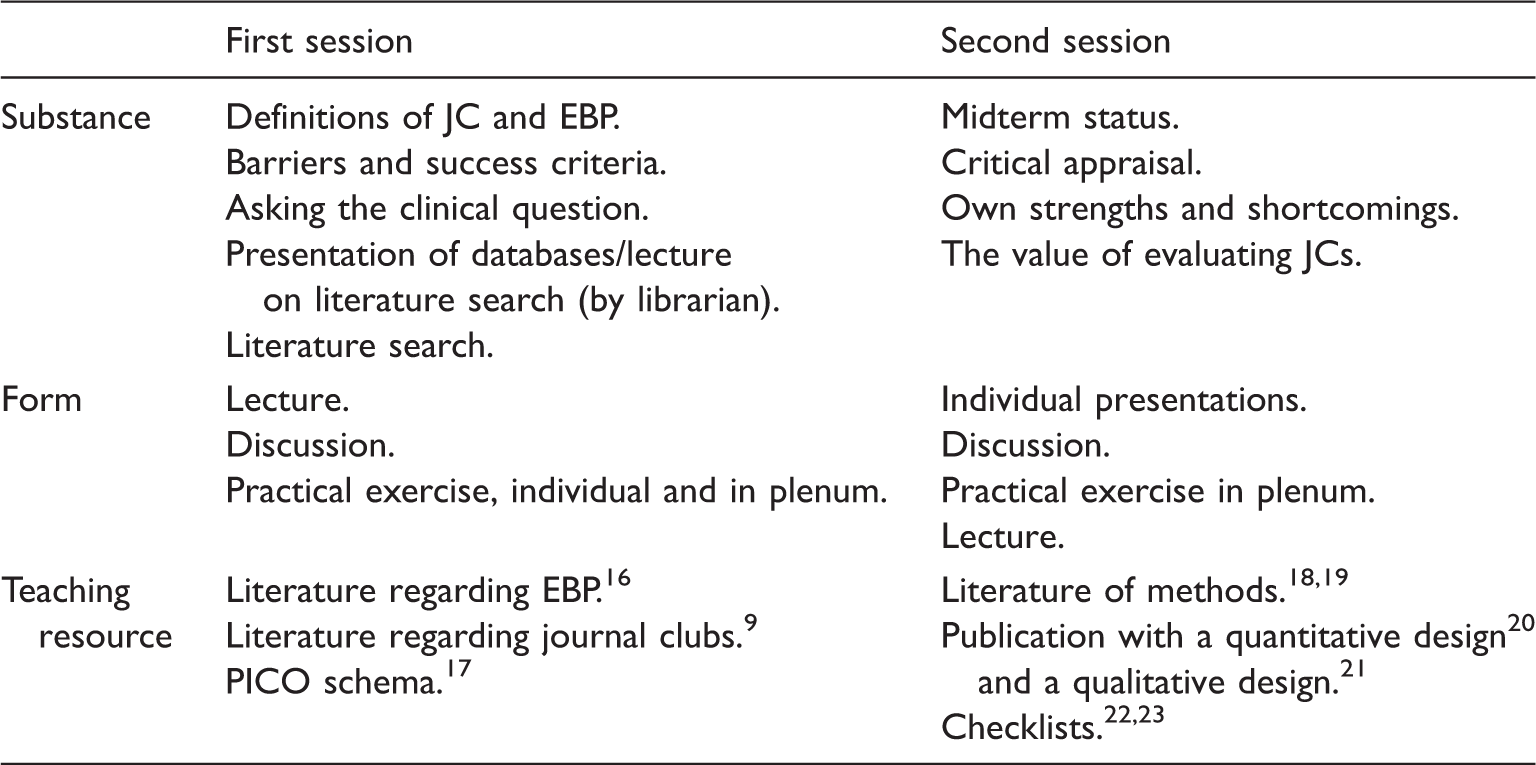
The course consisted of two three-hour sessions presenting and elaborating elements in effective JCs by examples from clinical practice, including examples of conducting JCs and lectures by a librarian on literature search. Insight from systematic reviews9,10 on how to run an effective JC was presented, but like many other educational programmes, it was not explicit planned with reference to transfer theory. 15
Overview of the substance and form of the course consisting of two 3-hour sessions, and the appurtenant teaching resource.
Data collection
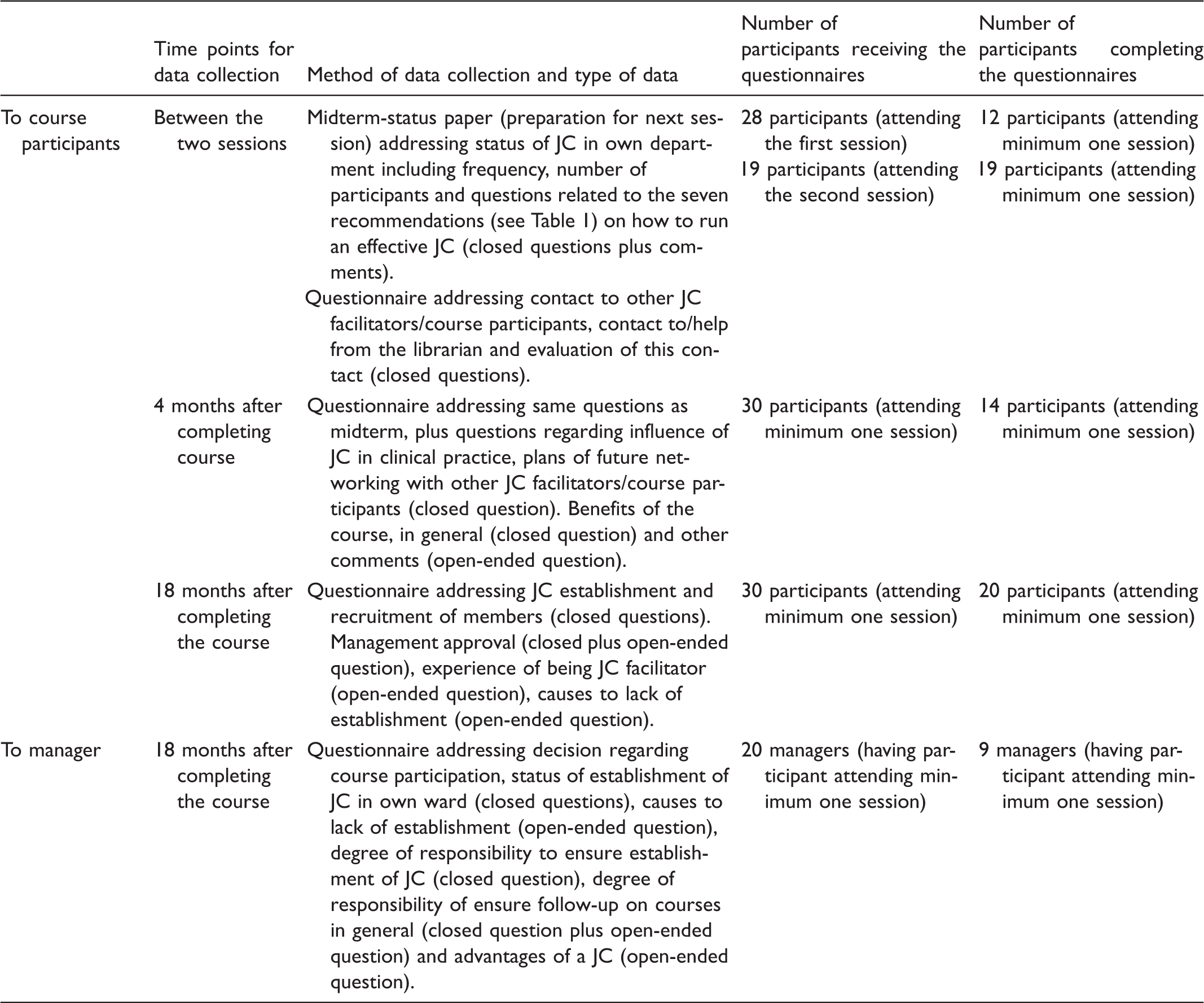
Prior to the course, participants filled out a questionnaire addressing age, gender, profession, working place, years of experience, post-graduate educational level, prior knowledge of databases and experience with JC (closed questions), and finally reflections of becoming a JC facilitator (open-ended question). Between the two sessions, the participants were asked to fill out a midterm-status paper considering their own JC and a short questionnaire. At 4 months and 18 months after participating at the course, all participants were asked to fill out a questionnaire addressing status on the process of establishing JCs. They were also asked to reflect on their experience with being a JC facilitator, if a JC was established. If no JC was established, they reflected on why this was the case. At 18 months after completing the course, the participants managers were also asked to fill out a questionnaire.
Time points, method of data collection, type of data and number of participants/managers receiving and completing the questionnaires.
Ethical considerations
From the beginning the participants were informed about the evaluation study, that their contributions were anonymized and that they had the right to withdraw from the study. Since no sensitive information was included, the study was not registered at The Danish Data Protection Agency.
Data analysis
The flow of the attending NMHP and a description of the midterm status (status paper and questionnaire) will be presented.
Reflection of becoming a journal club leader (based on the open-ended question in the questionnaire at assignment), stated profits of the course (based on the open-ended question in the questionnaire in the 4-month and 18-month follow-ups) and stated reflections about causes to lack of establishment of JC (bases on the open-ended question in the 18-month follow-up).

As no other literature regarding implementation of JCs was found, it was decided to perform a double analysis in order to illustrate the complexity in the succeeding factors. Consequently, the data from the 18-month follow-up (based on open-ended questions) from participants and managers point of view was analysed inspired by the concept learning transfer15,24,25 (Table 5) and in a frame as suggested by Merriam and Leahy,
15
including interdependent factors related to:
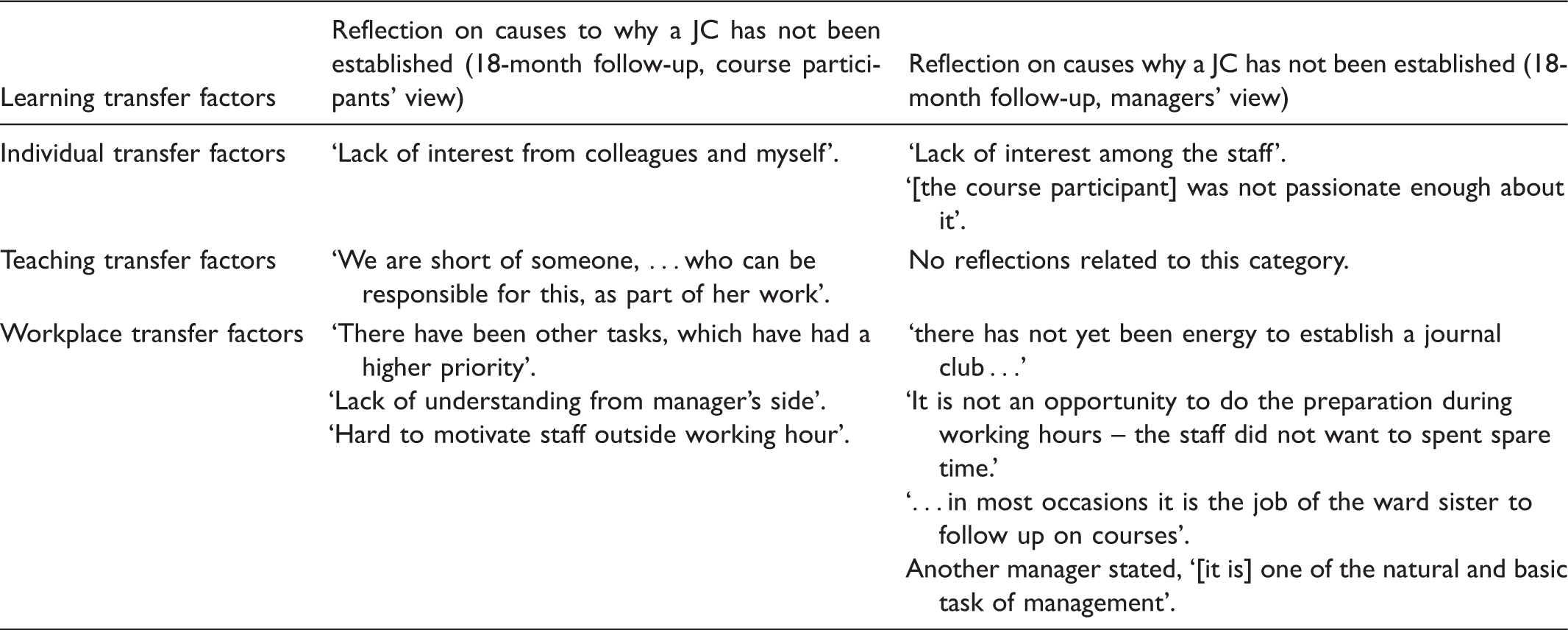
The individual learner, such as motivation, ability to set goals for own work and self-efficacy. The teaching, such as ensuring, that what is taught is learned so well that one is able to use it. The workplace, such as the transfer climate consisting of possibilities to use what is learned in a supportive social environment or culture. Learning transfer factors in relation to reflections on causes to why JCs have not been established, from course participants and managers point of view, respectively.
Results
Results will first be presented according to the time points of the data collection, divided into responses from participants and from managers, respectively. This is followed by a double frame of analysis based on a literature about JCs and the learning transfer concept. Finally, there will be a description of the answers coming from the three respondents, who actually had established a JC.
Assignment and attendance
There were 38 NMHPs who assigned the course, and 35 of these answered the questionnaire prior the first session. Not all of the assigned NMHP attended. In total, there were 30 NMHPs who attended the course, 17 of these attended both sessions, 24 were nurses, four were midwifes and two of them radiographers. Around 50% of participants had education at master level or above, the rest were bachelors. All were female.
In total, 28 NMHPs participated in the first sessions, and 19 participated in the second sessions. At the first session, the two non-attendees had forgotten the date, and at the second session, eight sent their apologies (two due to illness, one because of a new job, five were unknown) and three participants did not send their apologies.
Midterm status
Twelve participants handed in the midterm status paper. All of them were still in an early stage of the process of planning the JC in their own wards. Only four of them stated that they perceived having management approval at this point. Two participants stated that the JC set up in own department, in general had fallen into place, and two stated that the setting partly had fallen into place. Only a few had made concrete considerations regarding subject, literature search and use of checklists in the set-up of a JC in their department.
Participants’ responses at the 4-month and 18-month follow-ups
In total, 14 participants answered the questionnaire at the 4-month follow-up, and by then only two had conducted a JC session. Another two participants had or were about to enlist members to their JC. One had set the date for the first JC session. The majority (12 participants) had not contacted other JC leaders or had any plans of doing so. Two JC leaders did have contact to others and had plans of having contact in the future. Reasons given for not establishing a JC at this point were lack of time and resources, but also long-term sick leave.
Even though most participants did not manage to plan or try running a JC, several mentioned the same barriers described in the seven recommendations on how to run an effective JC (see Table 1), as explanations to why they did not manage to get to the point where they tried; time, prioritization, management approval and understanding from management level, but also the mangers interfering in choice of subject. Some participants mention lack of interest and motivation from colleagues as an explanation for not establishing a JC (Table 4).
Managers’ responses at the 18-month follow-up
Nine managers responded the questionnaire at the 18-month follow-up (Table 3). Some of them did not regard it as their responsibility to follow up on implementation of skills, which staff members learned at a new course. They also regarded it as the responsibility of the ward sister and/or course participant to establishing a JC after the course. The few managers who had a JC established at their wards responded that it had given professional theoretical input, new insights, and new challenges in form of critical appraisal and implementation of new knowledge in their wards. They also highlighted regular meetings and commitment as central for the success.
Analysis in a frame based on literature about JCs
Table 4 gives an overview of the reflections the participants made regarding becoming a JC leader (data from assignment), the profit of the course (data from the 4-month follow-up), and the participants’ reflections (data from the 18-month follow-up).
Table 4 demonstrates that the participants’ reflections prior to the course follow the seven recommendations given by the literature. As mentioned earlier, the JC facilitation course addressed the seven recommendations, which also is reflected in profits stated by the course participants at the 4-month and 18-month follow-ups (Table 4). Despite awareness and profits, the causes of not having established journal clubs 18 months after completing the course also reflect the recommendations (Table 4).
Analysis in a frame based on a learning transfer concept
Analysing the results in a learning transfer view, it becomes evident that lack of establishment of JC can be related to the three learning transfer factors, both from the course participants’ point of view and from the managers’ point of view (Table 5). These responses show that establishment and thereby implementation is more complex.
Established JCs at the 18-month follow-up
At the 18-month follow-up, only three participants, all nurses, stated that they had established a JC as a result of their attendance in the course. There were differences among those three regarding how easy it had been to recruit members to the JC (one state very easy, one state easy and one state difficult). The three participants stated that there was good management approval in form of time to conduct the JC session, but they also mentioned that, when it came to time for preparing and planning, it was not easy. To be a JC leader is challenging regarding finding the relevant literature and it takes time to get hold on the whole set-up. One mentioned that as a leader of a JC you have to ‘… find a balance between being active or laid-back …’, and one experienced that the leader of a JC also has the overall responsibility of the implementation process.
Discussion
The intention of this project was to establish JC facilitation courses giving special attention towards barriers described in the literature. 12 However, 18 months after the course, transfer15,24,25 had not taken place and only three journal clubs had been established. In the following the results will be discussed and related to the intertwined transfer factors at individual, teaching and workplace levels. 24
Individual transfer factors
From the open-ended question prior to the first course, and in the 4-month follow-up about satisfaction with the profit of the course (Table 4), lack of focus on individual transfer factors can explain the lack of success in establishing JCs. Some participants made reflections regarding own role, motivation and competences and found the course had given them insight into what a JC is and what it requires to facilitate one. However, most participants did not manage to establish a JC.
Of the three facilitators of the JCs that were established after the course, all had a master degree. This leads to a reflection of whether a moderate educational level is an essential individual competence. Other important competences might be familiarity with literature searching (other than knowledge and use of databases), reading and critical appraisal of the literature.
Teaching transfer factors
Feedback from the participants suggested, that most of them did not feel comfortable regarding facilitating a JC. Even though the majority had positions with developmental responsibilities, only two of them had tried to participate in a JC prior to the course. This leads to reflection of whether this should have been a requirement for participation. However, such a demand would in this particular context probably have entailed, that relatively few participants had attended the course. Through both sessions there was time for discussion of barriers and how to overcome them, status of JC in own department, and future needs in order to implement and facilitate a JC. Nevertheless, new clubs were not established.
In order to enhance transfer and prevent post-training relapse, 26 the course could have been expanded with further sessions, with more practical training on how to facilitate, initiate, and provide feedback. Another tool could have been post-training 27 by letting the course participant share what is learned with her colleagues and management upon return. However, post-training may cause trainee fatigue. 28
Workplace transfer factors
Ensuring education of staff is among the many tasks that challenge managers. Making sure that the participating staff really is interested, following up on courses, including ensuring a supportive and curious environment, at return from education/course, can be a different and even new task for managers. At the 18-month follow-up questionnaire some managers explained that JC had not been established at their ward because of lack of self-efficacy, energy or passion of the course participants.
Both participants and managers point out that lack of resources, especially time, as a problem, indicating prioritization of other tasks post-course.
Some managers did not consider it their job to ensure course follow-up; this was considered the responsibility of ward sisters. However, one of the managers stated that he found it the natural and basic task of management to follow up. Possibilities to transfer knowledge at workplace level seem difficult in a busy clinical environment, if there is no prior- and post-course prioritization, agreements on an implementation plan or a clear view on who is responsible.
Limitations
One limitation is that relatively few filled in the questionnaires, and unfortunately the electronic set-up was not optimal, since we were unable to detect the individual trace. This was a possibility and anonymization could still have been fulfilled, but we did not utilize this opportunity. Another limitation is that to some point we could have made more felicitous questions, for example in order to achieve further information about the participant’s competences. In that way the intervention could have been more targeted towards the exact participants.
Conclusion
Based on a concrete course on facilitating JCs, it has been our intention to discuss the potentials and barriers of establishing such a course among nurses and other members of the NMHP group. Even though we planned the course with attention to barriers of running a JC, we only got to the point where three out of 30 participants had established one after 18 months. We recovered already known barriers post-course, even though we did pay attention to them, including potential tools to overcome them. This led us to examine the intervention in a broader sense with theoretical inspiration from theories of learning transfer focusing on individual, learning and workplace factors.
Like the participants and the managers, we still believe that teaching a JC course has the potential to increase employees’ knowledge, skills, and abilities to read relevant literature for the benefit of the patients and the organizations. However, we suggest it is wise to consider factors like personal qualifications and motivation, structure of programme including reflections on relevant post-course actions and management support, approval and prioritization if the intention is implementation.
Footnotes
Acknowledgements
We thank the two Librarians; Penille Pless and Anni Friis.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Conflict of interest
The authors declare that there is no conflict of interest.

