Abstract
Researchers illuminate the mental health plight of correctional workers by demonstrating a high prevalence of mental health disorders among the group. Yet, structural barriers persist in preventing correctional staff from accessing treatment and support—barriers that may result in more prolonged and pronounced symptoms. We consider correctional staff perspectives on how mental health policies at the organizational level can foster better well-being outcomes for employees. Data are drawn from open-ended survey responses from provincial and territorial correctional employees (N = 870) in Canada. Responses collectively highlight the need for a correctional staff mental health paradigm that reflects the sources of stress among correctional workers, including access to specialized mental health services that are easily accessible, immediately available, and comprehensive in nature. Additional aspects of the work environment were identified as venues for important change, including improvements in work and schedule structures, improved manager–staff relations, and changes to the physical environment.
Keywords
Introduction
Mounting research across diverse contexts documents the adverse mental health outcomes associated with correctional work. Studies focusing on burnout (Kim et al., 2017; Useche et al., 2019), mental health disorders (e.g., posttraumatic stress disorder [PTSD], major depressive disorder, general anxiety disorder; Denhof & Spinaris, 2016; Carleton et al., 2018; Regehr et al., 2019), and other factors tied to well-being and life quality (e.g., work–life conflict; Higgins et al., 2021) shed light on the toll of correctional work on staff. Yet, the literature on correctional worker well-being appears to consistently illuminate poor outcomes, regardless of the operational context.
Although growing measures are in place to improve mental health and well-being among correctional workers, gaps in service and barriers to treatment persist (Brower, 2013; Gurda, 2019). As a result of barriers operating at the individual, social, and organizational levels, there remains much room for improving the mental health interventions and programs available to correctional staff. Recognizing that those directly or indirectly experiencing the mental health impacts associated with correctional work are ideally positioned to identify how interventions can be improved, the current study draws on the perspectives of provincial and territorial correctional staff in Canada to identify mental health initiatives that promote staff well-being.
Literature Review
Contextualizing the Problem and Crisis of Correctional Worker Mental Health
Research on correctional workers has blossomed in recent years, with studies focusing on different facets of mental health and well-being. One subset of research focuses on rates of mental health disorders, with findings consistently indicating higher prevalence rates among correctional workers relative to the general public and other public safety groups (Jaegers et al., 2019; Lerman et al., 2021; Regehr et al., 2019; Stadnyk, 2003). In the state of Washington, James and Todak (2018) found correctional workers have a PTSD prevalence equal to Iraq and Afghanistan veterans and more than police. In the Canadian context, Carleton, Ricciardelli, et al. (2020) have recently found that well over half of correctional workers in the Ontario provincial correctional service screened positive for mental health disorders, most frequently PTSD and major depressive disorder. Researchers also indicate correctional workers are at a higher risk of death by suicide (Stack & Tsoudis, 1997).
Why, exactly, does correctional work take such a toll on mental health? Operational stressors in correctional work, for example, factors related to carrying out one’s job (Denhof et al., 2014), are complex and varied. Over the course of their career, the majority of correctional workers will encounter potentially psychologically traumatic events, including violent incidents, death, self-injury, and other situations involving harm (Barry, 2017; Boudoukha et al., 2011; Viotti, 2016; Walker et al., 2017). Illustratively, James et al. (2017) found that approximately one quarter of correctional workers regularly experienced serious threats to themselves or their families, nearly half witnessed their colleagues endure a serious injury via assault by an incarcerated person, and over half witnessed an incarcerated person die. Following incidents, correctional workers may be involved with all the administrative procedures and/or inquiries that ensue, and must often continue to work in the very atmospheres where they have experienced traumatic incidents (Barry, 2017). If not treated effectively, to withstand these potentially psychologically traumatic stressors and working realities, correctional workers may become desensitized or hypervigilant and alert to danger at all times (Ricciardelli et al., 2018).
What Exacerbates or Remedies Workplace Mental Health Problems?
The effects of correctional work are not temporally or spatially bound to work environments. In addition to studies noting the high prevalence of compromised mental health among correctional workers, a sizable body of research points to how correctional work is associated with different types of work–life conflict. These include time-based (i.e., lack of time for one’s family due to schedules), role-based (i.e., difficulty shifting gears between the work and home personas), and strain-based conflict (i.e., emotional fatigue; Higgins et al., 2021; Lambert et al., 2020; Triplett et al., 1999; Vickovic & Morrow, 2020). Work–life conflict is common among correctional workers, which produces complex outcomes related to job satisfaction, organizational commitment, job stress, and burnout (Lambert et al., 2002, 2006, 2020, 2021).
Alongside operational stressors and logistical challenges are organizational stressors, which speak to the social context in which workers perform their duties. Examples of organizational stressors include perceived poor leadership and interpersonal conflict (Denhof et al., 2014). Whereas negative perceptions of the work environment and organization can serve as a source of stress (Finney et al., 2013), research indicates that perceptions of organizational support can have a positive impact on the well-being of correctional workers (Lerman et al., 2021). Perceived organizational support (POS) refers to how staff feel supported and valued by their employer, which can influence outcomes at the employee level (such as job satisfaction and mood) and factors influencing the organization (such as employee commitment, performance, and behavior; Eisenberger et al., 1986; Rhoades & Eisenberger, 2002; Sun, 2019). In relation to correctional officers, Lerman et al. (2021) found that “the more positively officers perceive supervision and management, as well as the quality and availability of stress management training, the less likely they are to report mental health issues” (p. 182). Thus, organizational structures that are perceived to reflect concern and appreciation for staff may mitigate the impacts of other types of occupational stressors.
Barriers to Treatment and Treatment-Seeking
Increasingly, programs and initiatives to address the mental health needs of correctional staff are available in certain jurisdictions (Brower, 2013). Yet, there remain structural barriers to the treatment of mental health needs among correctional workers; such barriers can mean mental health challenges remain undiagnosed, leading staff to experience symptoms longer and more severely (Stadnyk, 2003). One factor relates to the social systems of meaning surrounding mental health and treatment-seeking within correctional environments. Although somewhat dissipating, there remains pervasive stigma around mental health. Within a field where values such as strength and toughness are valued, mental health and treatment-seeking continue to be linked to perceptions of staff as lazy, weak, deceitful, or not suited for the position (Gurda, 2019; Karaffa & Koch, 2015; Lyons et al., 2017). Here, staff may be deterred from seeking help out of fear of such labels. Furthermore, in workplaces that are understaffed, absences may be frowned upon by colleagues, in turn creating negative connotations associated with using leave (Ricciardelli, Carleton, Mooney, & Cramm, 2020). Limited human resources in the workplace, labor shortages, and pressure to work overtime, and shift work and irregular hours, among other factors, may inadvertently pressure workers to attend work when they are unwell (Brower, 2013; Swenson et al., 2008).
Another barrier to treatment-seeking may be tied to the cumulative and ongoing nature of potentially psychologically traumatic event exposure in correctional work. Compared with physical injuries, some mental health disorders materialize less visibly, which can render the presence of a mental health condition more difficult to identify, both in oneself and others (Ricciardelli, Carleton, Mooney, & Cramm, 2020). The potential psychological trauma to which one is exposed, as well as long-term mental health erosion, may also be normalized in the work environment, or “part of the job” (Carleton, Afifi, et al., 2020; Ricciardelli, Carleton, Mooney, & Cramm, 2020). Work injuries may not only be invisible; they can also be insidious, cumulating over time rather than presenting instantly. Accessing treatment may only become an option when the severity of mental health struggles is no longer tolerable, as noted by Gurda (2019) in a study of barriers to treatment-seeking among U.S. correctional officers.
Gaps in organizational supports and service options are another barrier to the treatment of mental health conditions among correctional workers. Within the work environment, gaps in mental health intervention can include minimal debriefing following exposure to critical incidents, and lack of adequate access to on-site mental health resources, counseling, and treatment (Botha & Pienaar, 2006; Brough & Williams, 2007; Finney et al., 2013; Keinan & Malach-Pines, 2007; Willemse, 2021). More generally, there remains a lack of correctional-specific mental health interventions (Brower, 2013). The gap in effective and timely support can potentially exacerbate the effects of potentially psychologically traumatic and violent incidents on correctional workers. It may even contribute to the development of mental disorders such as posttraumatic stress disorder—a disorder and its comorbidities that is prevalent among correctional workers (Alavi et al., 2021; Finney et al., 2013; Genest et al., 2021; Norman & Ricciardelli, 2021; Regehr et al., 2019; Ricciardelli & Carleton, 2021; Ricciardelli et al., 2018).
Current Study
While the mental health plight of correctional workers is gaining increased attention, minimal academic attention has been paid to understanding the perspectives of workers regarding specific, direct, and practical solutions to mental health–related vulnerabilities. In the current study, we draw on open-ended survey responses to consider the strategies proposed by correctional workers to improve staff mental health and well-being. Respondents were provincial and territorial correctional workers occupying a range of positions in several Canadian provinces and one territory. These employees are responsible for the care, custody, and control of persons remanded in custody (e.g., awaiting trial or sentencing) and persons sentenced to a maximum of 2 years less a day who are either in prison or on conditional release in the community (Ricciardelli, 2019). We discuss how a continuing shift toward addressing the mental health needs of Canadian correctional workers may start to debunk the mental health and treatment-seeking stigma that continues to trouble the profession and is found to be negatively associated with employee experiences of stress, illness, absenteeism, low job satisfaction, high staff turnover, and burnout (Camp & Lambert, 2006; Griffin et al., 2009; Keinan & Malach-Pines, 2007; Ricciardelli, Carleton, Mooney, & Cramm, 2020). We recognize that there is variation in supports offered by correctional services in Canada; however, all services tend to offer Employment Assistance Programs and have some financial benefits to cover additional psychological services for full-time employees. There are variations in resources offered across jurisdictions, such as the availability of peer support programs, and we recognize our study is limited by such variations, which could be affecting participant responses.
Method
Participants
We collected data from Canadian correctional employees working in provincial or territorial correctional services, prior to the onset of the COVID-19 pandemic, using a web-based self-report survey available in English or French. In other work drawing from the same data set (Johnston et al., 2021), our first focus was to identify how workplace culture and occupational environments in prison settings shape the mental health problems and outcomes for many Canadian correctional workers. In the current article, we analyze qualitative, open-ended survey responses from 870 participants who responded to the item, “Please tell us what changes in your current work environment could have a positive impact on your mental health” from the provinces of Manitoba (n = 357), Saskatchewan (n = 362), Nova Scotia (n = 81), New Brunswick (n = 15), Newfoundland (n = 31), and the Yukon Territory (n = 24). 1 In this vein, our hope is to now present the oft-pragmatic solutions, policies, and policy shifts posed by provincial and territorial correctional workers that could potentially remedy the issues and tensions identified in Johnston et al. (2021). Respondents include correctional and probation officers, managers, administrators, nurses, teachers, and other employees within community, administrative, and institutional correctional services. There are discrepancies in sample sizes across the provinces and territories, which in part are due to the differences in the size of each jurisdiction. To exemplify, in 2018/2019, Manitoba had approximately 8,428 adults under provincial correctional jurisdiction on any given day, whereas Yukon had around 348 (Malakieh, 2020). Nevertheless, our sample is broadly, and cautiously, representative of correctional workers working in institutional, administrative, and community in provincial and territorial services in Canada (see Table 1).
Sociodemographic Information (N = 870)
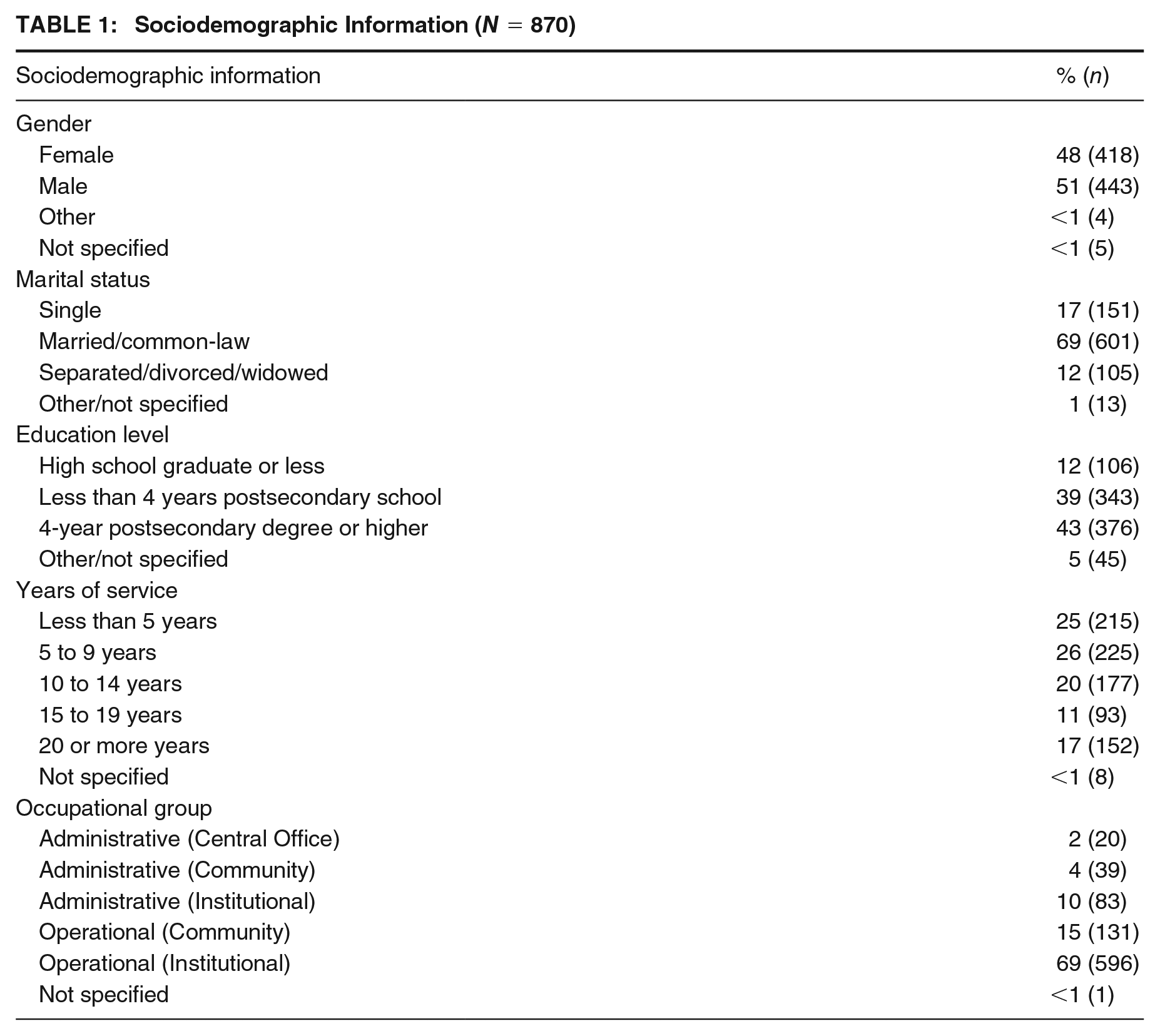
Procedures
Ministerial correctional and union representatives invited their employees/membership to participate in an anonymous and confidential online survey in 2018 and 2019 via their email listserv. Given the overlap between listservs, it is not possible to estimate the sampling frame or calculate the response rate on the survey. All surveys closed prior to/or at the onset of the COVID-19 pandemic. Upon receipt of the circulated survey email, interested respondents were provided with a link that directed them to the project consent form, study information page, and survey. Participation was voluntary and possible during paid work hours. Respondents were able to complete the survey over multiple sittings, if desired, and the survey took approximately between 25 and 40 minutes on average to complete. Research ethics boards at the University of Regina and Memorial University of Newfoundland approved the study.
Responses to the open-ended question varied in length, from a few words to several paragraphs. Using NVivo, data were coded using a constructed semi-grounded emergent theme approach that involved transforming codes into primary, secondary, and tertiary themes (Charmaz, 2014; Glaser & Strauss, 1967). Data pertaining to the question under analysis were then grouped into one document and discussed by the research team to get a sense of the data as a whole and to identify key themes across responses (Corbin & Strauss, 2015). Interrater coding was achieved because the data were, under the supervision of the second author and Principal Investigator, initially coded by research assistants as part of a large working research team. The first author then read through, re-coded, and categorized predominant themes found across all 870 responses to the question under study. The document created from this procedure was then sent to the Principal Investigator, who subsequently discussed the key themes presented by the first author, and how best to represent them in this article. We present the results by showcasing selected and representative quotations to illustrate the concrete themes and voices of respondents. Without compromising meaning or tone, the quotations we cite have undergone minor edits, without affecting vernacular, to correct spelling and grammar for readability.
Certain methodological limitations are worthy of mention. First, analysis of written survey responses is limited to the information presented by participants; we were unable to probe for additional information or clarity. As the nature of our qualitative analysis is interpretative, there may be discrepancy between the intended meanings of respondents and the meanings we ascribe to their words. We mitigated this limitation by discussing the data as a team and ensuring that we came to an agreement over the applied meanings. In this vein, we make no claims to generalizability, especially given the smaller sample sizes in some provinces and territories, but do recognize our sample is rather representative of correctional workers in Canada. The solutions posed by correctional workers may, in fact, be only applicable to the regions in which they work. That said, even if the sample is small, the narratives shared in this study are coming from the frontline experts, namely, correctional workers, some of whom have spent many years reflecting on these issues. Our study is simply mobilizing those voices to propose practical, solution-based strategies to improve the mental health framework of correctional services in Canada. Second, the sampling frame, due to the overlap between institutional and union listservs, cannot be explicitly determined given we cannot confirm a response rate for survey participants. Although we also cannot precisely determine the response rate for different types of corrections personnel, we have acknowledged, represented, and interpreted in this study the voices of many employees working in provincial and territorial correctional services to show the nuances, similarities, and differences in how they try to solve the problem of mental health in correctional work. Despite these limitations, we believe that having the private space to elaborate on a sensitive topic (i.e., mental health needs) allowed respondents flexibility and time to write about their experiences.
Results
On the topic of improving mental health in the workplace, four central recommendations were identified by participants: (a) consistent and funded access to specialized mental health services that are attuned to the realities and needs of correctional workers; (b) changes in work schedules and structures to enhance stability and predictability and reduce work–life conflict; (c) improvements to manager–staff relations; and (d) changes to the physical environment, including on-site spaces designated for personal health needs and wellness activities.
Expanding Correctional Staff Mental Health Resources
To support employee mental health and well-being, respondents across provinces and territories called for consistent and funded access to mental health professionals. Illustratively, a Correctional Officer from Manitoba stated, “More psychiatry hours, and a full-time Psychologist in the building would take a load off my shoulders.” The focus here is on the need for immediate and convenient access to on-site treatment and human resources to help manage and cope with the tensions of, and potential psychological trauma associated with, correctional work.
Some respondents spoke to the need for access to mental health professionals who were specialized in treating the stress injuries tied to correctional work environments: for example, “psychologists who understand the impact of dealing with violent offenders to talk to about workplace trauma” (Correctional Officer, Manitoba). Underpinning such suggestions is a recognition for how the stress and trauma injuries incurred in the context of correctional work may be reflective of highly unique social circumstances, such as regular exposure to violence and potentially traumatic situations. Reflected in participant statements was also the sense that ongoing exposure to potentially psychologically traumatic or stressful events was inevitable; thus, the solution may be containing the psychological impacts of such events through specialized mental health intervention.
The need for specialized services to be easily accessible was also a theme evident in respondents’ accounts, and ties into the specific needs of correctional staff. For example, some respondents proposed the availability of on-site services: “Access to mental health professionals that specialize in trauma disorders and have experience with first responders . . . Improved access to peer counseling services and access to crisis management” (Correctional Officer, Saskatchewan). As well, related to on-site availability of services is the feature of immediacy, whereby staff can access timely support “to help through a traumatic event” (Probation Officer, Manitoba). Here, one respondent described the need for mental health intervention as a component of incident management, specifically calling for the formation of immediate response teams to provide assistance following critical incidents. The respondent noted that the lack of such support “drastically decreases morale during/after incidents” (Correctional Manager, Yukon).
Services that meet the mental health needs of staff were also explained in terms of continuity and robustness—in other words, mental health care that is comprehensive and ongoing rather than episodic and reactive. Regarding comprehensiveness, respondents spoke to limits on existing services or resources (i.e., caps on counseling sessions) as a barrier to effective intervention: More than 7 sessions with a counselor (per year per family). Those sessions get used up very, very quickly, especially when you have a wife that has PTSD. That usually results in the things I’m facing getting no attention at all. (Correctional Officer, Yukon)
In this regard, calls for more comprehensive care reflect a sense that mental health impacts beyond individuals but also families, and possible injuries associated with correctional work cannot be met with quick or simple responses. As a solution, some respondents called for built-in “Annual mandatory mental health check-ins with a professional” (Correctional Secretary, Nova Scotia), occurring at regular intervals, as a preventive measure that can help ensure a healthy workforce. These assessments could, for example, “support early detection of potential PTSD within employees” as a Correctional Manager from Yukon explained.
Changes to Work Structures and Schedules
Given that work stress can be influenced by organizational factors (Denhof et al., 2014), it is perhaps not surprising that some respondents spoke to the need for changes in work structures to improve their mental health and well-being. As respondents’ accounts illustrate, above and beyond operational stressors, certain work features of correctional work can negatively impact well-being and quality of life, including being on-call (e.g., needing to be available to return to work when shifts are short staffed, which is exceptionally common in correctional work), performing shift work, working long hours and irregular schedules, as well as precarity in job status. Rather than buffering the impacts of operational stressors, work structures then can aggravate stress or otherwise fail to alleviate it. This may be particularly so when less stable positions (i.e., part-time, casual) are not associated with benefits.
Greater stability and predictability in work schedules was noted to be one solution to improving well-being and work–life conflict, specifically among correctional officers. As expressed by a Correctional Officer (Manitoba), alternating between day and night shifts can negatively impact well-being: “I think less shift pattern changing would be a good thing, just as your body gets used to days or nights you have to switch to the other and it really messes up your sleeping schedule.” Being on call, often a constant phenomenon for part-time or casual employees, was also deemed to negatively impact well-being, particularly as being on call pertained to maintaining personal lives; “being on call for a decade is stressful for relationships outside of work” (Correctional Officer, Manitoba). Without a permanent and consistent schedule (i.e., for those on call), this participant expresses how planned leave is impossible and relationships with loved ones can become strained by the lack of consistent engagement.
For those who have not obtained full-time or permanent status, the prospect of greater stability and predictability in job status, and thus more stability in schedules, was perceived as out of reach, or without any known timelines. Indeed, some correctional officers expressed that they were unsure when, if ever, they would eventually benefit from a consistent shift rotation and reduced on call hours. Speaking to this, a Correctional Officer (Manitoba) expressed the need for a “realistic timeframe for part-time staff to become full-time employees with full-time benefits and a predictable shift pattern.” In effect, both the nature of precarious work structures and the unknowability of when one will benefit from greater stability can serve as the source of stress.
Respondents also expressed how measures to reduce work–life conflict could enhance staff well-being. Recognizing the spillover effects of work structures and stressors, some spoke to the need for measures in place to reduce adverse impacts on family and private lives. For example, a manager (Saskatchewan) explained the difficulty in prioritizing family health and well-being needs due to their lack of available leave time to attend appointments or otherwise provide support in family crisis situations: Having more time and access to leave when my kids have crisis. As my kids are my priority and they struggle with mental health issues, numerous suicide attempts a year and 3 days spn does not cover the amount of appointments my children / young adult child require support with.
To help mitigate these family predicaments, the employee suggested that an empathetic, adaptive, and flexible response by their employer, perhaps in the form of providing them with the necessary time off even during abrupt circumstances, would go a long way in further developing a mental health partnership among staff working in correctional services. Family-related leave days were also imagined by other respondents as a means of reducing current work–life imbalance titled in favor of work: “Adding Mental Health days accessible for staff, like ‘Family Days’ for emergencies with family” (Correctional Officer, Manitoba).
Work–life conflict is described here not only in terms of family needs, but personal wellness and interpersonal relationships. Some respondents expressed a need for more personal leave time to offset the negative impacts of work stress and promote personal health and prosocial relationships with their family members (i.e., mental health days). In the current work context, some respondents also expressed how narrow perceptions of sickness as pertaining to physical ailments resulted in a lack of recognition of and stigma surrounding mental health injuries requiring leave. In effect, the expectations associated with sick leave can be infused with normative conceptions tied to illness and injury. This was illustrated in the words of a Probation Officer (Nova Scotia), who explained how using leave for mental health purposes was seen as contravening occupational expectations, resulting in “unfair disciplinary action.” They called for “employers to recognize need for mental health days” and “if taking a sick day due to mental health, not to place stigma” or require “that employee must stay confined to house.”
Others similarly expressed how current stigma surrounding mental health leave could deter use of leave for mental health–related matters. Here, respondents pointed to the need for a paradigm shift in the occupational climate surrounding use of leave: for example, having the “ability to take time off for mental health wellness without feeling stigmatized/criticized/feeling guilty for doing so” (Probation Officer, Nova Scotia). A Correctional Officer (Yukon) similarly expressed a sense of “judgement” and being “looked down upon” when using leave for mental health purposes. Tied to perceptions of stigma was the sense of being scrutinized in regard to the reasons for leave, that is, requiring to “prove” that the issues precipitating leave are legitimate. A Correctional Officer (Manitoba) stated the need to have “time off for mental health that isn’t questioned by the employer,” including a shift from scrutinizing the legitimacy of leave, to monitoring the well-being of staff (i.e., “Having the employer contact the staff member for a genuine check in and not have it be about providing doctors notes, or feel like it will be used against you in some way”).
In this context, the emphasis on presentism may deter the use of leave and/or therapeutic responses to mental health injuries. A Correctional Officer (Nova Scotia) explained, “I cannot make myself call in sick no matter how bad I need to out of fear and guilt with the negative stigma.” Here, the systematic barrier to treatment seeking or self-care, inherent in perception of a negative stigma tied to taking sick days/leave, may limit available time for personal care. Guilt and perceived pressures to attend work, both exacerbated by staff shortages and resource limitations, may potentially further compromise mental health and well-being.
Alongside the counseling and aid of trained mental health professionals, these respondents’ words exemplify the willingness of some correctional workers to help manage their mental health and family members’ mental health, if provided the opportunity to invest more time in such practices. Ultimately, mental health leave was seen a measure that would contribute to a better workplace when considering not simply presentism, but the mental state and aptitude of staff who are present, for instance, staff who “feel strong, healthy and ready to tackle our daily duties” (Community Youth Worker, Saskatchewan).
Building Positive Relationships With Management and Staff Solidarity
A common theme threaded throughout responses was that correctional workers perceive that their mental health concerns are unacknowledged or not understood by upper management. A Probation Officer (Nova Scotia) explained this sense of disconnection: “Management is less connected to the field work and thereby less connected to our experiences and workload needs.” Evidenced in participants’ words was the extent perceptions of how management viewed staff influenced occupational outlooks and well-being.
In response to the perceived disconnect with management, some expressed that improved working relationships would positively contribute to the relational atmosphere. This could include a greater presence of management in frontline work situations so as to facilitate communication that is proactive rather than reactive in nature (i.e., “management be[ing] more involved with floor staff to promote positive relationships,” Correctional Officer, Manitoba) and venues for dialogue (i.e., “an open-door policy which allows staff to speak directly with supervisors about feelings of being overwhelmed and stressed,” Correctional Officer, Manitoba). In addition to enhanced communication, respondents emphasized the need for a more solidaristic atmosphere (i.e., “having management work as a team with us”). Such positive staff relations are tied to a sense of wanting to feel respected and “not as a number” (Correctional Officer, Manitoba).
Improvements in staff culture on the ground were another area deemed ripe for improvements so as to improve staff well-being. Specifically, respondents emphasized the need for respect in their environment, explained in terms of improvements in attitudes and interactions among staff. Illustratively, respondents stated workplace dynamics could be enhanced by improvements or changes such as “less passive aggressive comments” (Correctional Officer, Manitoba): “[a] respectful environment where employees do not talk negatively about each other” (Correctional Teacher, Saskatchewan), and efforts among staff to “be kinder to each other and try to resolve their conflicts with coworkers” (Correctional Manager, Newfoundland). These passages call for a team atmosphere and empathic discourses rather than a more individualist workplace environment. More explicitly, they call for more professional and collegial behavior between co-workers and less negative talk about each other, recognizing that social conflict can have detrimental impacts on well-being and compromise safety in correctional work environments.
Impediments to solidarity among staff were perceived to include lack of predictability, continuity, or control over who one worked with. One Correctional Officer (Manitoba) stated that “a consistent partner would make a world of difference,” as unpredictability in who one works with is “is very stressful.” Continual variation in coworkers was seen as impeding the formation of trust and positive working relations. Other respondents built on these ideas by expressing the need for mentoring programs, whereby less experienced staff would work with mentors who could provide insight when it comes to navigating the often-stressful field of correctional work, including the potentially psychologically traumatic aspects of their work (i.e., “a mentoring program would be a good way for staff who are less confident to have a person to go to when they need,” Correctional Officer, Saskatchewan). Peer-based mentoring programs could assist not only in operational issues, but in matters tied to mental health and well-being, including “opportunity for education both in terms of recognizing secondary trauma, but also in working with individuals who have experienced trauma” (Correctional Officer, Manitoba).
Improvements in the Physical Environment
Although somewhat less common, a small number of participants described how changes to the physical work environment could facilitate mental health and well-being. Some respondents called for the incorporation (or improvement) of spaces intended to promote health and wellness activities within the work setting. One example was the creation of quiet spaces for activities such as meditation; such spaces could provide a small oasis of comfort in an otherwise difficult and challenging workplace environment. To elaborate, a Probation Officer (Saskatchewan) explained that a quiet room could “help escape the tough parts of our job,” noting, “when we feel stressed we could go breathe in peace for 5 minutes.” A Correctional Officer (Manitoba) stated how a “break area away from inmates” would provide them with a small opportunity to relax, de-brief, re-set mentally, and deal with the ongoing fatigue that accompanies working in a consistently challenging environment.
Some also emphasized the need for spaces for physical exercise (i.e., gyms) and to facilitate healthy eating (i.e., kitchens), recognizing the positive impact of physical activity and a healthy lifestyle on mental and physical health, but also impediments to achieving them: “Ability to exercise and stay fit. Incentives to exercise” (Correctional Officer, Newfoundland). As a Probation Officer (Saskatchewan) further explained this issue, “I’m either working at work or working being a parent so there is no time for exercise, and we all know physical activity contributes to well-being.” Similarly, a Correctional Officer (Manitoba) emphasized the need to incorporate “physical health and wellness on site,” such as “having a kitchen and a time to cook in house meals.” The idea here is that spaces in the work environment that are easily accessible not only facilitate forms of activity that promote health and wellness, but also in the words of a Manager from Saskatchewan, “fun.”
Discussion
Recent literature exploring mental health and well-being among correctional workers, including in Canada, reveals a need for organizational policies that improve worker mental health, safety, morale, and general working conditions (Ricciardelli et al., 2018). The organizational context in which operational stressors unfold can mediate the impacts of work stress. Gaps in policy at the organizational level can aggravate the effects of being exposed, sometimes regularly, to potentially psychologically traumatic incidents, which can result in occupational stress injuries (Finney et al., 2013; Willemse, 2021).
Occupational stress injuries occurred in the context of correctional work may be complex, particularly given cumulative exposure to potentially psychologically traumatic events, in effect requiring ongoing and sometimes intensive treatment responses. However, opportunities exist to improve the correctional organizational context, thereby potentially mitigating negative mental health impacts tied to work events and injuries among staff. Regarding mental health interventions, respondents’ accounts of available treatment options point to the need for a special correctional mental health paradigm that reflects the characteristics and sources of stress among correctional workers. There is some recent recognition of this need in the extant literature as Alavi et al. (2021) have identified some of the benefits of delivering an online cognitive behavioral therapy program to address the mental health challenges experienced by correctional workers and other public safety personnel. Our data, in tandem, speak to the need for a model that is responsive to correctional-specific work stressors, available easily and immediately (i.e., in the aftermath of an event), and comprehensive and continuous so as to adequately and sufficiently respond to the complexity of occupational stress injuries. It is unknown, however, how correctional workers feel about online psychological services, which is an area of future research given how participants want to access such services was beyond the scope of the current study. Inevitably, there are undoubtedly challenges associated with such a model, including concerns around privacy, confidentiality, and choice in care provider; however, a correctional staff care model that integrates mental health services into organizational frameworks could possibly assist in challenging the stigma surrounding mental health in correctional services and resulting concrete barriers to treatment-seeking.
Any treatment/intervention/prevention model could include mental health services, including psychological counseling and psychiatric care, provided by staff who are attuned to the unique working realities and occupational stress injuries of correctional workers. As well, services that are easily accessible, particularly in the immediate aftermath of an event, and robust in quantity, reflect the perceived needs of respondents in relation to occupational mental health paradigms. Ease of access was emphasized in the form of on-site services; in addition to being easily accessible, built-in services in the workplace also reflect the connection between work and private lives, specifically the impact of work stress on personal well-being. Although on-site options are not without challenges (e.g., retaining privacy), the suggestion that mental health services should be on-site reflects a perceived connection between work events and mental health—challenging the sentiment that personal mental health is a private matter (Gurda, 2019; Johnston et al., 2021). Recognition of this connection is also particularly notable in an environment where mental health remains stigmatized (Ricciardelli, Carleton, Gacek, & Groll, 2020; Ricciardelli, Carleton, Mooney, & Cramm, 2020).
Comprehensiveness in care was another principle emphasized by participants, specifically respondents emphasized the need for a sufficient quantity of intervention so as to effectively, and in an ongoing matter, deal with the impacts of work stress. Mandatory psychological assessments and interventions were also highlighted as a means in which to align service paradigms with the mental health vulnerabilities that are tied to correctional work. Such mandatory access and relationship-building with mental health professionals may encourage correctional workers to seek help in confidence more often in the future, possibly before they reach a critical breaking point or become too overwhelmed. Embedded psychological assessments could also serve to normalize treatment-seeking and mental health intervention (see White, 2021).
The notion of mental health paradigms attuned to the needs of public safety personnel is not a novel concept. Police psychology, for example, has become a recognized academic and practical subdiscipline (Brower, 2013). In certain policing services, mental health professionals are specialized in assisting police officers cope with the unique situations and stressors tied to their occupation. However, a similar subdiscipline has yet to be established in relation to correctional workers and many prison services lack embedded mental health services to assist staff in navigating the experiences and mental health impacts they may face at work (Brower, 2013). Yet, the accounts of participants suggest a pressing need for this area of expertise and professional specialization.
As revealed in respondents’ words, work structures in correctional services can contribute negatively to well-being and cause work–life conflict (Armstrong et al., 2015; Swenson et al., 2008). Within correctional work environments, work structures, including schedules, are a complex matter, particularly in institutions, which require constant staff presence, including overnight, on weekends, holidays, and during exceptional circumstances. Given the necessity of 24/7 staffing, features such as overtime, being on-call, and irregular schedules would appear to come with the operational territory. Yet, such work features can take a toll on employees, particularly when the content of their job can involve exposure to various operational stressors, including potential psychologically traumatic events. Reconciling the labor needs and well-being of staff is necessary for the health of staff and the workplace. In addition, it must be recognized that the staff shortages plaguing correctional services may put pressure on staff to come to work, even when they should not. However, many Canadian Correctional Services are understaffed, which in turn results in less consistent shift rotation, more on call hours, and substantial overtime, which clearly perpetuates the cycle of increased job burnout and stress while reducing well-being. Additional human resources, at a full-time capacity with benefits and a regular schedule, are one way to start to remedy this cycle, with the goal of improving the mental health of employees. Of course, resources are few and far between, which requires an investment by governments in correctional service workers, with the recognition that a healthier correctional labor force will also result in a healthier criminalized population.
In addition, recognizing how contextual job factors can influence mental health and well-being, some emphasized how work–life conflict could be improved via measures to increase stability and predictability, including a consistent shift rotation, less on-call hours, and job security. Such features in turn could facility greater stability in one’s personal life, including the ability to make plans and spend uninterrupted time with friends and family. Such a focus in responses captures the extent to which the realms of work and life are interconnected (Higgins et al., 2021), evidenced by work structures that directly impact both the quantity and quality of personal time.
Calls for greater stability appeared to be evident among those in relatively less stable job positions. As in many other occupations (Gross et al., 2018), job precarity may be a reality for correctional workers, which can negatively affect correctional workers’ perceived sense of well-being, morale, and management of their personal lives and family responsibilities. In a demanding occupation where worker absenteeism and turnover are sometimes disproportionately high (Camp & Lambert, 2006; Griffin et al., 2009; Keinan & Malach-Pines, 2007; Kurtz, 2008; Lambert & Paoline, 2010; Trounson et al., 2019), workers may feel pressured to adapt to their shifting and chaotic schedules. Permanent and full-time positions may, to a certain extent, provide staff with full benefits and improve worker mental health, morale, and their family relationships (see Swenson et al., 2008). Reducing major changes in work hours, and thus sleep schedules, could also limit some of the negative physiological, psychological, and behavioral impacts associated with shift work in correctional services (see Swenson et al., 2008).
Even when staff benefit from more stable positions, an ongoing concern remains; specifically, occupational meanings tied to leave, particularly leave for mental health purposes. Perceptions of leave for mental health purposes may be shaped by lingering normative values within correctional workspaces, including stigma around mental health (Ricciardelli et al., 2021) as well as labor dynamics (i.e., staff shortages) that may effectively put pressure on staff to be present even when they feel they should not be. Functioning similarly to “sick time” or emergency leaves of absence, many participants described how access to more leave days may help them to deflate, recover, care for family members, reduce stress, and address their mental health needs. These days off could also possibly reduce adverse mental health challenges from fully materializing and lingering, which would be more financially burdensome for both the employer and individual seeking treatment in the long term. Participant responses also strongly indicate correctional workers’ desire to be able to use mental health days without question, as they express that admitting to a mental health problem in their workplace carries with it some fear of social and occupational repercussion. Experiencing “guilt” or a sense of “judgement” when one does admit to requiring mental health leave may put workers at risk of feeling as though they are at fault for developing a mental health disorder (Johnston et al., 2021). It is not only the availability of leave for mental health purposes that remains a concern for respondents, but the meanings surrounding use of leave for mental health issues that remain an obstacle to well-being. Efforts to counter the stigma tied to mental health leave and help-seeking require more focused attention, as only by reducing stigma can a process like mental health days be impactful, or even helpful, for employees. Likewise, embedding mental health days within leave frameworks was thus put forth as one strategy to normalize use of leave to promote personal health and well-being.
Another organizational factor that can contribute to stress among correctional workers pertains to the social relations of work, illustrating the connection between POS and staff well-being (Lerman et al., 2021). In particular, participants felt the perceived disconnection between frontline workers and upper management contributed negatively to the work environment and staff well-being. This type of organizational stressor speaks to a larger disconnect between frontline employees and management that is often pronounced in fields such as correctional services (Bennett, 2012; Chenault, 2010; Crawley & Crawley, 2008). Studies across other contexts have likewise emphasized how frontline correctional staff may feel misunderstood, unappreciated, and not valued (Bennett, 2012; Chenault, 2010; Crawley & Crawley, 2008). Perceptions of feeling replaceable and disposable (i.e., “just a number”) can contribute to negative attitudes in the workplace, including a distrustful mentality that draws skepticism to those outside of frontline worker groups (Chenault, 2010).
Although this mentality has been found to be pervasive within frontline correctional environments, responses in the current study suggest workers recognize that improving top-down relations could positively impact well-being. Specifically, efforts to promote more positive, open, and collaborative interactions were presented as a strategy to improve relations of work. Respondents sought more team-oriented relationships with their superiors, which could be facilitated through small gestures of “encouragement” and a stronger managerial presence on the “floor.” Their suggestions are reinforced by the POS model, whereby staff who hold positive views of management and are supported through stress management interventions are less likely to report mental health problems (Lerman et al., 2021).
Transformational leadership tactics employed managers and supervisors have also been found to increase correctional worker job satisfaction and reduce work–family conflict, particularly when correctional workers feel that they have a voice in decision-making and ownership/autonomy over their job (Abderhalden et al., 2021; Baker et al., 2015). Improving relational dynamics to become more team-based and collaborative could not only enhance well-being at work, but, as participants emphasized, increase awareness among managers regarding the daily work realities faced by frontline staff. Although some frontline correctional employees raised tension with management, we did not find in our data concerns raised by managers or administrators about their own potential challenges supervising, and working with, frontline staff, or any mental health challenges that can arise from such relationships. Thus, this is an important area to consider in future research.
Improving relations among colleagues on the floor was also deemed needed, although few specific strategies to improve the cultural atmosphere within workspaces were offered. Changes at the level of staff culture can be difficult to identify, given the ways in which culture can permeate and become entrenched within systems of interaction. However, one set of concrete changes was tied to greater predictability, continuity, and/or control over work teams. Dynamic environments where staffing compliments are frequently changing due to rotating schedules, turnover, and restructuring mean that staff may be unable to gain a sense of their social environment and benefit from positive social relations. This sense of trust can be particularly important for correctional workers, who may feel a greater sense of safety and security against risks in their environment knowing support is present (Liebling et al., 2011). Having the ability to build lengthier and deeper relationships with colleagues may also help to diffuse any tensions or conflicts that become difficult to resolve without meaningful and frequent communication. A peer mentor program where new workers can tap into the knowledge and expertise of veteran workers who have experienced and sought treatment for mental health could also serve to challenge patterns of suffering in silence driven by the lingering stigma associated with mental health challenges, and potentially alleviate any workplace vulnerabilities.
Finally, a small number of participants spoke to the utility of embedding wellness spaces in the work environment to promote well-being activities, including meditation, exercise, and healthy eating. Wellness spaces embedded in workspaces not only promote but facilitate health coping mechanisms to deal with stress. Convenient access to wellness spaces may be particularly important for staff such as correctional officers who often face work–life imbalance in the form of time-based conflict (Lambert et al., 2006), and who may be at risk of health problems tied to lifestyle (Morse et al., 2011). Positive spaces for mediation or simply quiet time could further assist in facilitating decompression following a stressful incident or otherwise assist in ongoing well-being activities and exercises. Suggestions by respondents regarding changes to the infrastructure of work capture the extent to which the physical work environment can influence both mental and physical health, including the well-being activities that are possible and encouraged within such environments. Embedding spaces within the work environment for wellness activities can serve to imbue work spaces, often marked by negative experiences, with positive meaning, promoting not only individual but group well-being.
Conclusion
The adverse mental health impacts of correctional work are becoming increasingly known (Jaegers et al., 2019; Lerman et al., 2021; Regehr et al., 2019). Despite this enhanced knowledge, ongoing barriers to mental health interventions persist. Correctional workers, like other public safety personnel, may be formally, informally, or socially sanctioned for accessing mental health resources or admitting that they have a problem that requires assistance (Karaffa & Koch, 2015; Lyons et al., 2017; Ricciardelli, Carleton, Mooney, & Cramm, 2020). Organizational factors within correctional services can aggravate, or otherwise fail to mitigate, work-related stress injuries (Finney et al., 2013). However, researchers suggest that organizational support can reduce the adverse mental health impacts of correctional work (Lerman et al., 2021). As conveyed by respondents in the current study, there exist opportunities to promote more nuanced understandings of stress injuries and mental health, provide more robust mental health resources to staff, and engage in other strategies to enhance mental health outcomes.
Shifting from an individual to social sense of responsibility for mental wellness remains a challenge (Johnston et al., 2021). This is particularly the case within correctional environments that, in many cases, remain influenced by traditional elements of staff culture, including an emphasis on control and authority (Crouch & Marquart, 1980). The features deemed necessary to be a “good” correctional worker, particularly for officers, can deter outward behaviors or reactions that may be perceived as weak or emotional. Yet, correctional environments are both emotionally charged and highly emotionally regulated environments (Crawley & Crawley, 2008). In such contexts, staff responses to highly distressing events and situations are often filtered by normative occupational expectations. The incongruity between cultural norms surrounding emotional responses and operational realities is evidenced by high rates of mental health disorders among staff—that is to say, the realities of correctional work do impact workers in a myriad of complex ways. Indeed, findings presented here affirm that correctional staff are keenly aware of the mental health impacts of their work—but also the systematic changes that might effectively curb the growing mental health plight of workers.
