Abstract
Research indicates that the COVID-19 pandemic has had far-reaching repercussions in South Africa, mirroring trends in other countries by affecting health care systems, economies, and overall quality of life, while also profoundly impacting the work and well-being of mental health care professionals. In this context, this study aimed to investigate the psychological distress (K10 > 16) associated with occupational stress among mental health care professionals in private practice during the first wave of COVID-19. A cross-sectional survey was conducted with 284 mental health care practitioners recruited through Medical Pages (Medpages) database and email outreach. Participants completed a SurveyMonkey questionnaire that gathered demographic information, details on occupational COVID-19-related stress, and levels of psychological distress. Univariate and bivariate analyses were employed to describe sample characteristics, assess the prevalence of occupational COVID-19 stress and psychological distress, and explore their association. The majority of participants were male (80%), with a mean age of 49 years. The findings revealed moderate prevalence rates of occupational COVID-19 stress at 66% and psychological distress at 64%. In addition, a moderate positive correlation was found between occupational COVID-19 stress and psychological distress (r = .46; p < .001). These findings suggest the need for continued psychosocial support and self-care by mental health care professionals beyond COVID-19 pandemic.
Keywords
Introduction
The onset of the COVID-19 pandemic, caused by the SARS-CoV-2 virus, emerged in late 2019 and rapidly escalated into an unprecedented global crisis, profoundly impacting health care, economies, and social systems worldwide (World Health Organization [WHO], 2020). Since its first documented case on March 5, 2020, in South Africa, the COVID-19 pandemic has profoundly impacted various aspects of society. These impacts include significant disruptions to public health systems, exacerbation of existing inequalities, and severe economic consequences (Shifa et al., 2022). By late 2023, South Africa had reported over 4 million confirmed COVID-19 cases and more than 100,000 deaths (WHO, 2023). The South African government’s COVID-19 response mirrored global trends through lockdowns, testing, and vaccination campaigns (Kajiita & Kang’ethe, 2024) but was uniquely exacerbated by pre-existing inequalities: high unemployment/poverty, HIV/TB comorbidities, and under-resourced health care infrastructure (Mendelson & Mathema, 2020). These systemic pressures disproportionately burdened health care workers, with mental health practitioners (MHPs) facing heightened secondary trauma from overlapping crises (Harvey, 2023; Nguse & Wassenaar, 2021; Pool et al., 2024). While lockdowns were epidemiologically necessary, they intensified psycholosocial distress across society. This disruption impacted the psychological well-being of both the general population including teachers and health care workers in South Africa as well as other countries, resulting in a significant increase in mental health challenges, in already pre-existing mental health challenges affecting performance at work (Gold, 2020; Nguyen et al., 2020; Petrie et al., 2019; Tawfik et al., 2019), highlighting the urgent need for mental health support (Bendau et al., 2021; Mayisela et al., 2024; van der Westhuizen & Guse, 2022).
Systemic health care inequalities in South Africa marked by disparities in access to care between urban and rural areas and between the public and private sectors, and shortages of resources and staff, were further exacerbated by the COVID-19 pandemic, alongside the high burden of HIV/AIDS and tuberculosis (Mendelson & Mathema, 2020). These challenges intensified pressure on the health care system, resulting in overwhelming demands on health care workers, including extended working hours, increased risks of infection, and disruptions to non-COVID-19-related services (Pappa et al., 2020). Concurrently, research indicates that MHPs experienced a surge in demand for psychosocial support as the population grappled with pandemic-related stress, anxiety, and depression, driven by factors such as fear of illness, grief, and economic hardship (Broche-Pérez et al., 2020; Knight, 2020; Kotowski et al., 2022; Mayisela et al., 2024). MHPs globally experience increased psychological distress suggesting that COVID-19 pandemic has debilitating effects on the practitioners (Kotowski et al., 2022; Murat et al., 2021; Sadek et al., 2021; Salvador et al., 2021). These studies concur with Sadek et al. (2021) who found moderate levels of burnout and psychological distress among MHPs in Canada. Sadek et al.’s (2021) study is supported by the findings in some mental health care practitioners’ published studies (Couarraze et al., 2021; De Kock et al., 2021).
As demand for psychological services surged, mental health care professionals in private practice experienced a corresponding increase in their caseloads. This burden was further intensified by personal concerns about infection, feelings of isolation, financial uncertainty, and emotional distress. Kazadi et al. (2024) found that for health care workers working during COVID-19 was an emotional rollercoaster, physically and mentally exhausting there was a significant rise in client demand for services, with many experiencing heightened emotional distress. This increased demand, combined with the emotional strain of supporting clients through a global crisis, contributed to practitioner burnout and secondary trauma (van der Westhuizen & Guse, 2022).
In addition to managing high workloads, studies show that private health care practitioners also struggled with fears of infection. A survey conducted by Lee et al. (2022) indicated that practitioners in South Africa experienced substantial anxiety regarding potential exposure to the virus, particularly during face-to-face interactions. These concerns were compounded by limited access to personal protective equipment (PPE) at the time and the challenges of maintaining social distancing in therapeutic settings. Furthermore, Knight (2020) argued that the pandemic prompted a shift to telehealth for numerous practitioners. However, this transition was accompanied by obstacles such as unreliable internet connectivity and difficulties in establishing therapeutic rapport remotely. Working remotely and telemedicine were found to be factors contributing to stress leading to depression and anxiety (Almondes et al., 2021; Paolucci et al., 2021). Consequently, this transition led to a reduction in in-person consultations and an increase in cancellations, thereby exacerbating financial strain due to lost income (Pappa et al., 2020).
As much as psychological distress is identified among health care workers working in the public sector, some studies found a high level of psychological distress among health care workers not working in the public health system (Kühlmeyer et al., 2020). In addition, health care practitioners in private practice experienced a sense of professional isolation, which contributed to emotional distress. This isolation stemmed from limited opportunities for in-person engagement with their professional community, which typically offers essential emotional support and supervision, hereby intensifying feelings of burnout and stress (Klein et al., 2020).
Rationale
The literature review above indicates that, in addition to impacting health care systems, economies, and overall quality of life, the COVID-19 pandemic has also significantly affected the work and well-being of mental health care professionals (Harris et al., 2011). Despite extensive research on the impact of the pandemic on frontline health care workers such as nurses, doctors, and emergency medical technicians and paramedics, there remains a notable gap in research focusing on the experiences of second-line workers, specifically those providing mental health care in private practice. Second-line workers are health care professionals such as MHPs, therapists, counsellors, and social workers who support individuals dealing with the psychological and emotional impacts of public health crises (Mittal et al., 2023). Mental health challenges among practitioners not only undermine their emotional well-being but also raise concerns about the quality of care they provide to clients during a global pandemic (Klein et al., 2020). Given this backdrop, the present study aimed to investigate the psychological distress associated with occupational stress among mental health care professionals in private practice in South Africa during the first wave of COVID-19. Understanding this association is crucial for identifying the stressors that affect the psychological well-being of private MHPs during a public health crisis, as well as for ensuring the quality of care provided to clients in such unprecedented times. Furthermore, this research may serve as a foundational study for future investigations into the impact of pandemics on mental health care professionals in South Africa and similar contexts.
Theoretical framework
This research is embedded in Engel’s (1977) biopsychosocial theory as the point of departure in understanding the research question, the method towards answering the questions and the data yielded and its analysis. The biopsychosocial theory advocates for the consideration for the social, psychological and behavioural dimensions of illness (Engel, 1977). It refers to the interaction between the individual’s interpretive functioning of the stimulus, based on the environment background and their ontogenetic organisation of a system of units that stack in a continuum from simple to complex. The systematic organisation of an individual as an organism progresses from the minute subatomic units, atom, molecules, organelles, cells, tissue, organ systems, e.g., nervous system, organs and the person. From the system of the individual person, the person forms a system with other human beings as a person-to-person interaction, then the family system, the community system, society, leading to national culture and the biosphere (Engel, 1981; Wade & Halligan, 2017). This research is pursued with the understanding that each individual, the mental health practitioner in this case, is an organism made up of organs, tissues, minute cells made up of atoms and molecules (Engel, 1981; Wade & Halligan, 2017). We argue that the environment and context in which the individual is located, made up of interconnected social systems and the biosphere, calls for the individual practitioner’s adaptation to occupational demands related to rapid response to COVID-19 pandemic. Psychological distress is likely, through a mental interpretive process (psychological processing of the contextual issues), to trigger a cellular stress reaction presenting as biopsychological distress expressed as traumatic symptoms, depression anxiety and more. In the context of this study, the urgent need to adapt to the COVID-19 pandemic served as the occupational stressor that initiated this cycle.
The objectives of the study
To assess the prevalence of occupational stress and psychological distress related to the first wave of COVID-19 among MHPs in private practice in South Africa.
To establish the association between occupational stress and psychological distress related to the first wave of COVID-19 among MHPs in private practice in South Africa.
Hypotheses
Hypothesis 1: Null: MHPs in private practice will not report high prevalence rates of occupational stress and psychological distress (K10 > 16) during the first wave of COVID-19. Alternative: MHPs in private practice will report high prevalence rates of occupational stress and psychological distress during the first wave of COVID-19.
Hypothesis 2: Null: There is no significant association between levels of occupational stress and psychological distress (K10 > 16) among MHPs. Alternative: Higher levels of occupational stress are significantly associated with greater psychological distress among MHPs.
Method
Study design
A quantitative research method, using a survey design, was used to collect data between October 2020 and January 2021.
Participants and sampling strategy
The study participants (n = 284) consisted of MHPs – including psychologists, psychiatrists, and counsellors – registered with the Health Professions Council of South Africa (HPCSA) and practicing in private health care institutions. The initial target sample size of 400 was calculated using a standard population formula at 95% confidence (Noordzij et al., 2011). Ultimately, 284 MHPs (psychologists, psychiatrists, counsellors) registered with the HPCSA and practicing in private institutions completed the survey via SurveyMonkey®. Convenience sampling facilitated nationwide coverage across all nine South African provinces.
Data collection
The researchers distributed the SurveyMonkey questionnaire link with the assistance of the Medical Pages (Medpages) database, a digital platform in which approximately 8,790 South African mental health care professionals were subscribed at the time of the survey (Medpages, September 2020). The self-administered questionnaire included two measures that assessed psychological distress and occupational stress related to COVID-19. To obtain a sense of the composition of the sample, demographic questions related to age, race, gender, category of registration, practice location, and province of practice were added to the questionnaire.
Measures
Psychological distress was measured with the 10-item Kessler Psychological Distress Scale (K10) (Kessler et al., 2003). The instrument was deemed suitable for the study due to its ability to capture information about an individual’s level of distress at the time of the study. The K10 measures psychological distress in the form of depression and anxiety symptoms experienced in the past 30 days with a 5-point Likert-type rating (Kessler et al., 2003). Examples of the items include questions such as ‘In the past 30 days, how often did you feel so restless that you could not sit still?’, with response options in the range of 1 = ‘none of the time’ to 5 = ‘all the time’ (Kessler et al., 2003). Higher scores on the scales were an indication of high psychological distress. To aid in interpretation of the outcome, the K10 psychological distress scale totals were also categorised to show low to very high stress. We used cut-off scores presenting low risk (10–15), moderate (16–29) and high (30–50), to determine severity of distress. The K10 demonstrates strong validity and excellent reliability, with a meta-analytic mean Cronbach’s alpha of .89 across diverse populations (Wojujutari & Idemudia, 2024). In the current study, the scale achieved an internal consistency reliability of α = .80, but validity was not assessed.
Participants’ stress related to COVID-19 was assessed with an occupational stress questionnaire developed by the researchers of the study. The questionnaire was developed by the researchers with the intention to capture only occupational stress that may be related to COVID-19. The questionnaire consisted of 10 questions that enquired about potential work stressors that were related to COVID-19, using a 5-point Likert-type rating (1 = ‘never’ to 5 = ‘most of the time’). Questionnaire items included questions on adaptation to social isolation, working from home, inability to conduct consultations, providing psychotherapy on the phone or a video call, implementation of COVID-19 protocols at work, medical aid payments, fears about contracting the virus at work, financial concerns, and professional inadequacy. High scores on the questionnaire indicated a higher level of occupational stress related to COVID-19, with lower scores indicating lower stress.
Factor analysis results: COVID-19 occupational stress
An exploratory factor analysis (EFA) was conducted using principal factor extraction to investigate the underlying structure of a 10-item occupational stress scale. Prior to analysis, the dataset (n = 278) was assessed for factorability. The Kaiser–Meyer–Olkin (KMO) measure of sampling adequacy was .83, indicating meritorious adequacy, and Bartlett’s Test of Sphericity was statistically significant, χ2(45) = 605.13, p < .001, confirming the appropriateness of factor analysis. The questionnaire demonstrated a reliability of Cronbach alpha .79.
The study utilised the principal-factor analysis (PFA) extraction method with 2.908 for a single factor’s eigenvalue. The scree plot showed a distinct inflection after the first factor, with subsequent eigenvalues forming a near-horizontal pattern, indicating that only the first factor accounted for a meaningful proportion of the total variance. Based on the eigenvalue-greater-than-one rule, scree plot, and parallel analysis, a single factor was retained. This factor accounted for 65.68% of the total variance, suggesting a unidimensional construct underlying the occupational stress items. All items showed substantial loadings on the single factor (range = .52 to .78), supporting its internal coherence. The internal consistency of the full scale was high, with a Cronbach’s alpha of .79, indicating strong reliability. These findings suggest that the COVID-19 occupational stress scale can be treated as a single-factor measure capturing a general dimension of work-related stress among mental health professionals during the COVID-19 pandemic.
Data analysis
Microsoft Excel, STATA 15 and the Statistical Package Software for Social Sciences (SPSS) allowed summary and analysis of the data (Singh, 2022). The missing data rate was below the commonly accepted 5% threshold and considered minimal (Okpara et al., 2022). Descriptive statistics using frequencies and percentages were used to summarise the composition of the sample. In addition, univariate analysis (means, standard deviation, and frequencies) was used to determine the prevalence of COVID-19 occupational stress and psychological distress, while bivariate analysis showed changes in characteristics by psychological distress levels.
An exploratory factor analysis (EFA) was conducted to examine the dimensionality of the 10-item COVID-19 occupational stress scale, with responses measured on a 5-point Likert-type scale (1 = ‘never’ to 5 = ‘most of the time’) using principal factor extraction. Sampling adequacy was confirmed with the KMO measure, and Bartlett’s test of sphericity verified the suitability of the correlation matrix. The number of factors was determined using eigenvalues, the scree plot, and parallel analysis. A single-factor solution was retained, explaining a substantial proportion of the variance. Factor loadings ≥ .40 were deemed significant. Internal consistency was assessed using Cronbach’s alpha, with values ≥.70 considered acceptable.
Finally, simple and multiple linear regression analysis were used to determine the association between COVID-19 occupational stress and psychological distress (K10) among MHPs. We tested the linear regression assumptions and confirmed a linear relationship between COVID-19 occupational stress and psychological distress, independence and normal distribution of residuals (errors), homoscedasticity, and the absence of multicollinearity. This analysis was rerun per individual COVID-19 occupational stress component factor to determine if the association obtained with the compound variable was consistently seen across the component stress variables or not.
Ethical considerations
Ethics approval for the study was obtained from University of Johannesburg, Faculty of Humanities Ethics committee (REC-01-134-2020) and the Humanities Research Ethics Committee of the University of the Witwatersrand (R14/49Mayisela, protocol number H20/07/24). Participants provided informed consent as part of their questionnaire completion on SurveyMonkey. In addition, participants were provided with resources for mental health services for instances where they identified themselves to be psychologically distressed.
Results
Sample characteristics
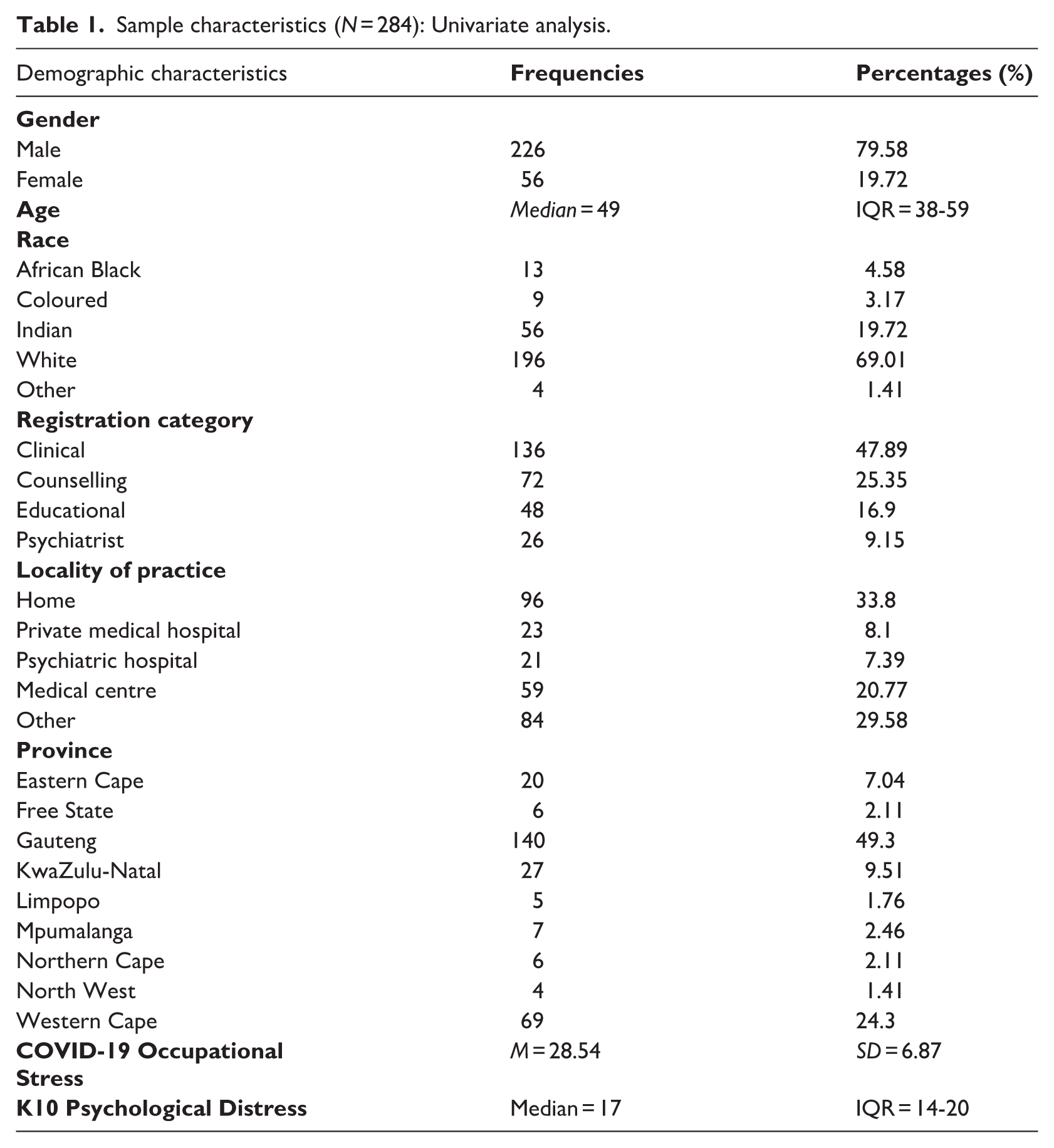
The survey included 284 participants. The descriptive analysis of participants’ demographic characteristics is summarised in Table 1. The majority of participants were male (80%), with a median age of 49 (IQR = 21). Most identified as White (69%), and nearly half were registered clinical psychologists (48%). The primary practice location was home-based (34%), and the largest proportion worked in the Gauteng province (49%).
Sample characteristics (N = 284): Univariate analysis.
Hypothesis 1: prevalence of stress
COVID-19 related occupational stress and psychological distress
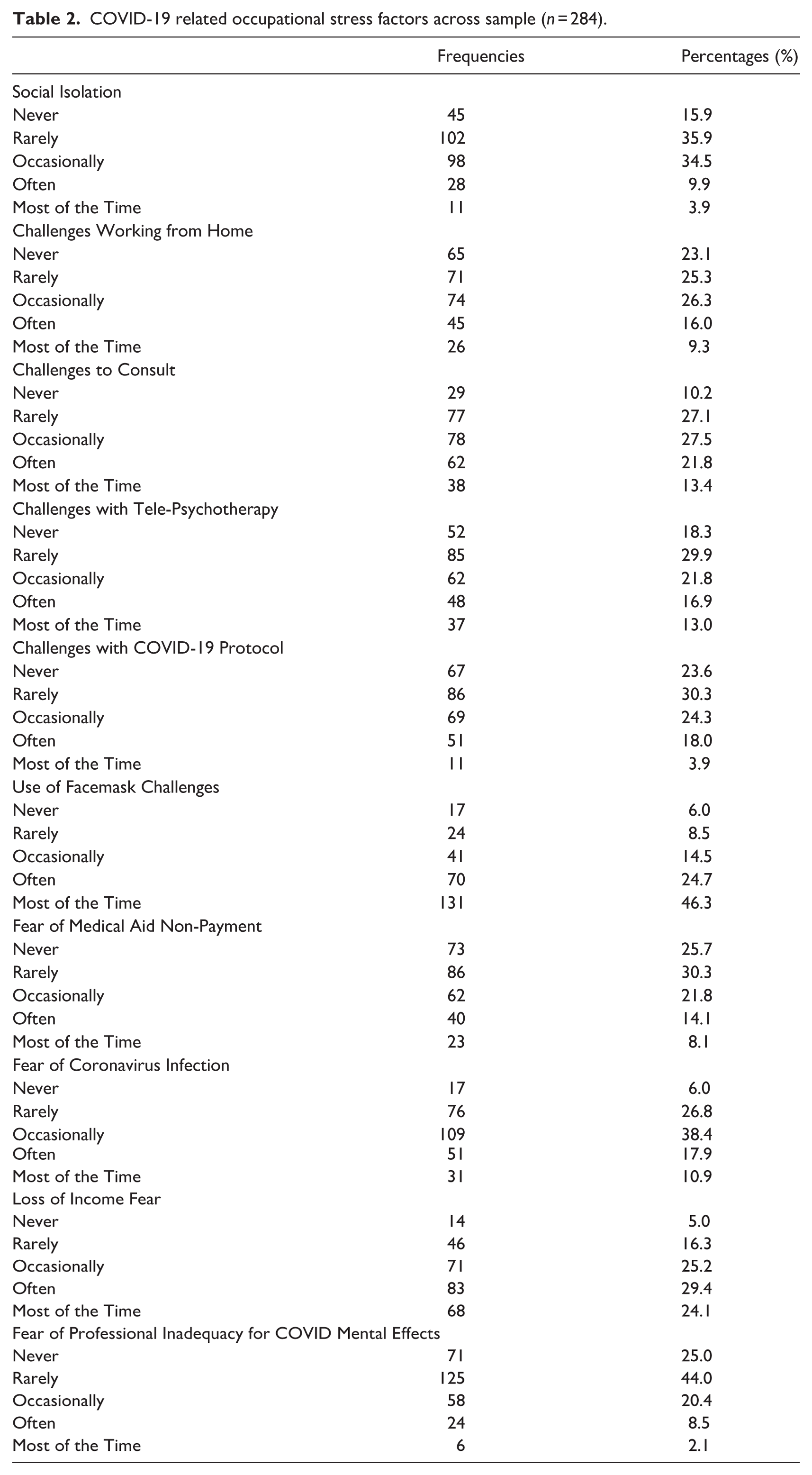
The analysis revealed a high prevalence of COVID-19-related occupational stress, with 66% of participants reporting such experiences (Table 2). The scores on the COVID-19 occupational stress questionnaire ranged from 12 to 45, with a mean of 28.54 (SD = 6.87). All measured occupational stress factors were reported, with MHPs indicating most challenges in four areas: face mask use, fear of losing income, fear of coronavirus infection, and difficulties with patient consultations. In contrast, the prevalence of psychological distress was low at 35% (n = 99). The K10 scores ranged from 10 to 29 and were skewed, with a median of 17 and an interquartile range (IQR) of 6.
COVID-19 related occupational stress factors across sample (n = 284).
Hypothesis 2: the association between psychological distress and COVID-19 occupational stress
A moderate significant positive correlation was observed between COVID-19 occupational stress and psychological distress (r = .46, p < .001; Figure 1). Simple linear regression indicated that occupational stress accounted for 21.5% of the variance in psychological distress scores, R2 = .215, F(1, 258) = 70.54, p < .001; Table 3. The unadjusted model showed that a one-unit increase in occupational stress was associated with a .28-unit increase in psychological distress (β = .28, 95% CI [0.22, 0.35], p < .001).
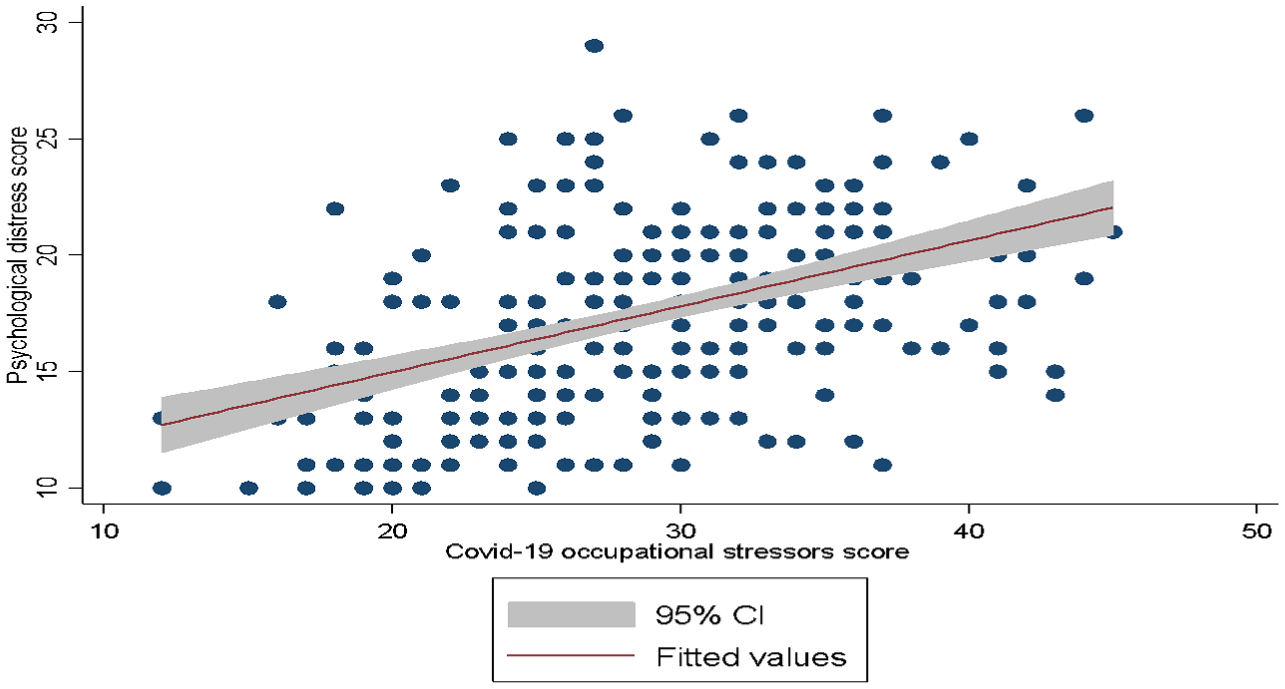
Association between psychological distress and COVID-19 occupational stress (N = 270).
Linear regression of psychological distress score.
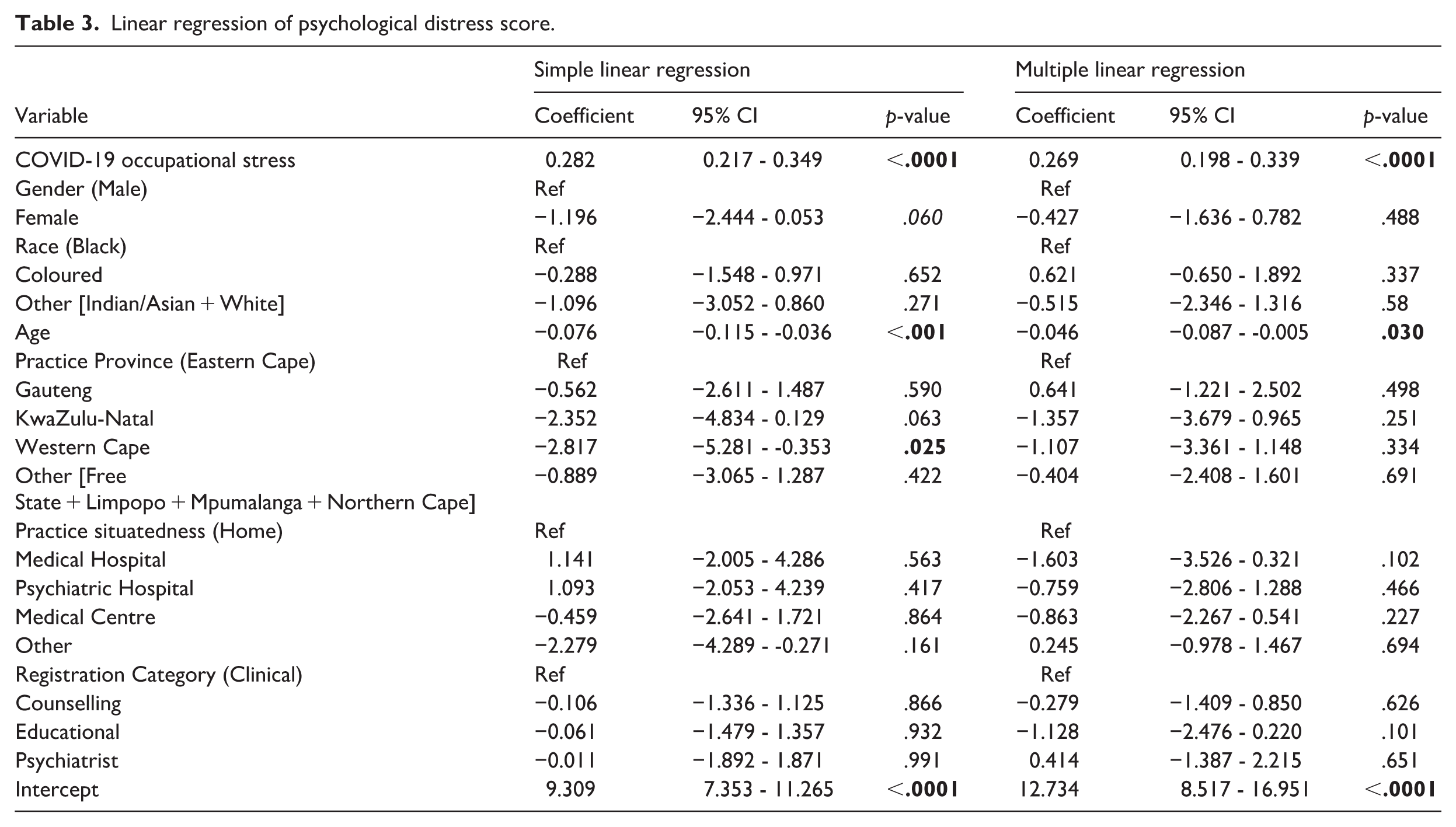
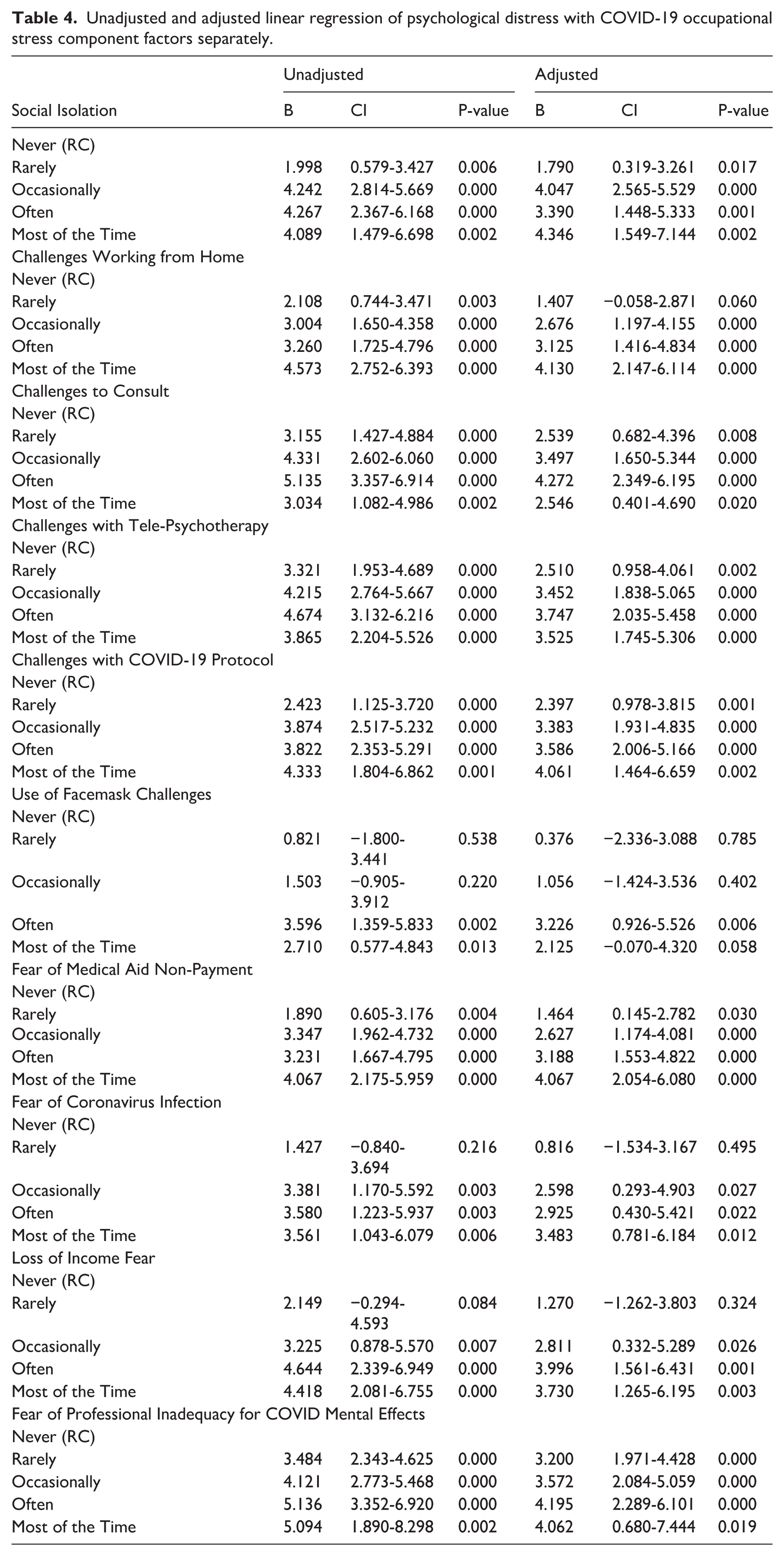
This association persisted after adjusting for key demographic variables, including gender, age, race, province and situatedness of practice, and registration category. The multiple linear regression model was significant and explained 24.6% of the variance in distress, R2 = .246, F(16, 230) = 6.02, p < .001. With all variables in the model, a one-unit increase in occupational stress remained significantly associated with a .26-unit increase in psychological distress (β = .26, 95% CI [0.19, 0.33], p < .001). The results of the association between separated covid-19 occupational stress factors and psychological distress are shown in Table 4 Appendix.
Among the demographic covariates, only age was a statistically significantly associated with psychological distress (β = −.04, p = .030), indicating a slight decrease in distress scores with increasing age. No other demographic variables demonstrated a significant association with the outcome.
Discussion
This study investigated the psychological distress associated with occupational stress among mental health care professionals in private practice in South Africa during the first wave of COVID-19. The demographic profile of participants reflected the broader composition of psychologists registered with the HPCSA, particularly those in private practice, where available data indicate significant gender and racial disparities. HPCSA (2017) records indicate that nearly 80% of psychologists and psychiatrists in private practice are male and 74% White (HPCSA, 2017). This limited representativeness underscores the need for greater demographic transformation within the South African mental health care profession.
The findings reveal a complex picture of how work-related stressors translated into psychological outcomes for this cohort. Regarding Hypothesis 1, the results present a notable divergence. A high prevalence of COVID-19-specific occupational stress was observed (66%), while the prevalence of general psychological distress was lower (35%). This suggests that while MHPs were acutely impacted by pandemic-specific challenges, such as infection fears, financial insecurity, and patient consultation difficulties, they may have possessed psychological resources or coping strategies that buffered against more severe, generalised distress. The elevated occupational stress aligns with global research identifying pandemic work stress as a primary driver of burnout (Couarraze et al., 2021). That general distress was not higher may reflect the specific context; while health care workers often exhibit pre-existing mental health vulnerabilities (Gold, 2020; Nguyen et al., 2020; Petrie et al., 2019; Tawfik et al., 2019), the general K10 psychological distress measure may not have fully captured the work-specific manifestations of distress more directly assessed by the occupational stress questionnaire. This interpretation is supported in research indicating significant psychological distress among health care workers outside the public health system (Kühlmeyer et al., 2020).
The relationship proposed in Hypothesis 2 was strongly supported. The significant association between occupational stress and psychological distress remained stable after demographic adjustment, underscoring workplace factors as significantly linked to mental health outcomes. This aligns with international findings where COVID-19 work stress consistently predicted distress (Shi et al., 2020) and mirrors patterns in other South African frontline professions (Kazadi et al., 2024; Mayisela et al., 2024). Specific stressors like infection fear and moral dilemmas about infecting family (Broche-Pérez et al., 2020), compounded by the isolation of remote work, provide a plausible biopsychosocial explanation for this link. The rapid adoption of telemedicine, while essential for service continuity (Almondes et al., 2021), may have been a double-edged sword, as remote working arrangements have themselves been identified as risk factors for psychological distress (Paolucci et al., 2021). However, since the measured factors explained only 21.5–24.6% of the variance in distress, the substantial residual variance underscores the significant role of unmeasured resilience factors. Variables such as social support, individual coping strategies, or professional identity may have critically moderated the pathway from occupational stress to broader psychological distress.
Collectively, these findings emphasise that supporting MHPs requires structural and occupational interventions that extend beyond fostering individual resilience. Targeted strategies must address the specific work-related stressors inherent in providing care during public health crises, particularly those related to safety, practice viability, and professional isolation, to mitigate their impact on mental well-being.
Conclusion
This study, guided by the biopsychosocial model, demonstrates that the COVID-19 pandemic constituted a multifaceted crisis for South African mental health care professionals in private practice. The findings highlight that the pandemic’s social and occupational disruptions – including risks to safety, professional isolation, and practice viability imposed a significant occupational and psychological burden, with a clear link established between these specific stressors and broader mental health outcomes. The robust link between occupational stressors and distress underscores that mental health practitioner wellbeing is not merely an individual concern but is fundamentally shaped by systemic and contextual factors.
However, several limitations should be noted. Recruitment primarily via a single platform likely skewed the sample towards older, White, male professionals, limiting generalisability. The sample was also geographically concentrated in Gauteng and Western Cape provinces, despite national representation. The cross-sectional quantitative design allowed measurement of distress levels and associations but was unable to determine predictors and causality due to simultaneous collection of exposures and outcomes. Also, the study did not explore how these variables interact or the contextual factors involved. Future research should seek broader demographic and geographic representation and employ mixed methods and a longitudinal design to gain deeper insights into the complex relationships and lived experiences underlying distress during crises situations. Finally, the COVID occupational stress scale developed for this study requires further testing, beyond the exploratory factor analysis that we conducted, to determine measurement validity.
Given the high prevalence of occupational stress, it is crucial to support mental health care professionals with accessible mental health services. If such services are readily available, further investigation into barriers to access and their effectiveness is warranted. Mental health care workers are known to face elevated secondary trauma from patient care (Killian, 2023), and addressing this trauma is essential to maintain their well-being and productivity.
The moderate association between occupational stress and psychological distress highlights the need for better preparation of mental health care professionals before resuming patient care during crises. Although these professionals are expected to remain composed in challenging situations, this can contribute to internalised trauma manifesting later as psychological distress (İnci et al., 2025). Recognising that mental health care workers are vulnerable to the negative effects of trauma is vital.
The COVID-19 pandemic placed significant strain on health care workers who continued working despite infection risks and restrictive social and economic conditions. This study highlights the substantial psychological and occupational vulnerabilities experienced by MHPs during the pandemic. Its findings and recommendations aim to inform strategies to mitigate the impact of future disasters and pandemics on this population.
Footnotes
Appendix 1
Unadjusted and adjusted linear regression of psychological distress with COVID-19 occupational stress component factors separately.
| Unadjusted | Adjusted | |||||
|---|---|---|---|---|---|---|
| Social Isolation | B | CI | P-value | B | CI | P-value |
| Never (RC) | ||||||
| Rarely | 1.998 | 0.579-3.427 | 0.006 | 1.790 | 0.319-3.261 | 0.017 |
| Occasionally | 4.242 | 2.814-5.669 | 0.000 | 4.047 | 2.565-5.529 | 0.000 |
| Often | 4.267 | 2.367-6.168 | 0.000 | 3.390 | 1.448-5.333 | 0.001 |
| Most of the Time | 4.089 | 1.479-6.698 | 0.002 | 4.346 | 1.549-7.144 | 0.002 |
| Challenges Working from Home | ||||||
| Never (RC) | ||||||
| Rarely | 2.108 | 0.744-3.471 | 0.003 | 1.407 | −0.058-2.871 | 0.060 |
| Occasionally | 3.004 | 1.650-4.358 | 0.000 | 2.676 | 1.197-4.155 | 0.000 |
| Often | 3.260 | 1.725-4.796 | 0.000 | 3.125 | 1.416-4.834 | 0.000 |
| Most of the Time | 4.573 | 2.752-6.393 | 0.000 | 4.130 | 2.147-6.114 | 0.000 |
| Challenges to Consult | ||||||
| Never (RC) | ||||||
| Rarely | 3.155 | 1.427-4.884 | 0.000 | 2.539 | 0.682-4.396 | 0.008 |
| Occasionally | 4.331 | 2.602-6.060 | 0.000 | 3.497 | 1.650-5.344 | 0.000 |
| Often | 5.135 | 3.357-6.914 | 0.000 | 4.272 | 2.349-6.195 | 0.000 |
| Most of the Time | 3.034 | 1.082-4.986 | 0.002 | 2.546 | 0.401-4.690 | 0.020 |
| Challenges with Tele-Psychotherapy | ||||||
| Never (RC) | ||||||
| Rarely | 3.321 | 1.953-4.689 | 0.000 | 2.510 | 0.958-4.061 | 0.002 |
| Occasionally | 4.215 | 2.764-5.667 | 0.000 | 3.452 | 1.838-5.065 | 0.000 |
| Often | 4.674 | 3.132-6.216 | 0.000 | 3.747 | 2.035-5.458 | 0.000 |
| Most of the Time | 3.865 | 2.204-5.526 | 0.000 | 3.525 | 1.745-5.306 | 0.000 |
| Challenges with COVID-19 Protocol | ||||||
| Never (RC) | ||||||
| Rarely | 2.423 | 1.125-3.720 | 0.000 | 2.397 | 0.978-3.815 | 0.001 |
| Occasionally | 3.874 | 2.517-5.232 | 0.000 | 3.383 | 1.931-4.835 | 0.000 |
| Often | 3.822 | 2.353-5.291 | 0.000 | 3.586 | 2.006-5.166 | 0.000 |
| Most of the Time | 4.333 | 1.804-6.862 | 0.001 | 4.061 | 1.464-6.659 | 0.002 |
| Use of Facemask Challenges | ||||||
| Never (RC) | ||||||
| Rarely | 0.821 | −1.800-3.441 | 0.538 | 0.376 | −2.336-3.088 | 0.785 |
| Occasionally | 1.503 | −0.905-3.912 | 0.220 | 1.056 | −1.424-3.536 | 0.402 |
| Often | 3.596 | 1.359-5.833 | 0.002 | 3.226 | 0.926-5.526 | 0.006 |
| Most of the Time | 2.710 | 0.577-4.843 | 0.013 | 2.125 | −0.070-4.320 | 0.058 |
| Fear of Medical Aid Non-Payment | ||||||
| Never (RC) | ||||||
| Rarely | 1.890 | 0.605-3.176 | 0.004 | 1.464 | 0.145-2.782 | 0.030 |
| Occasionally | 3.347 | 1.962-4.732 | 0.000 | 2.627 | 1.174-4.081 | 0.000 |
| Often | 3.231 | 1.667-4.795 | 0.000 | 3.188 | 1.553-4.822 | 0.000 |
| Most of the Time | 4.067 | 2.175-5.959 | 0.000 | 4.067 | 2.054-6.080 | 0.000 |
| Fear of Coronavirus Infection | ||||||
| Never (RC) | ||||||
| Rarely | 1.427 | −0.840-3.694 | 0.216 | 0.816 | −1.534-3.167 | 0.495 |
| Occasionally | 3.381 | 1.170-5.592 | 0.003 | 2.598 | 0.293-4.903 | 0.027 |
| Often | 3.580 | 1.223-5.937 | 0.003 | 2.925 | 0.430-5.421 | 0.022 |
| Most of the Time | 3.561 | 1.043-6.079 | 0.006 | 3.483 | 0.781-6.184 | 0.012 |
| Loss of Income Fear | ||||||
| Never (RC) | ||||||
| Rarely | 2.149 | −0.294-4.593 | 0.084 | 1.270 | −1.262-3.803 | 0.324 |
| Occasionally | 3.225 | 0.878-5.570 | 0.007 | 2.811 | 0.332-5.289 | 0.026 |
| Often | 4.644 | 2.339-6.949 | 0.000 | 3.996 | 1.561-6.431 | 0.001 |
| Most of the Time | 4.418 | 2.081-6.755 | 0.000 | 3.730 | 1.265-6.195 | 0.003 |
| Fear of Professional Inadequacy for COVID Mental Effects | ||||||
| Never (RC) | ||||||
| Rarely | 3.484 | 2.343-4.625 | 0.000 | 3.200 | 1.971-4.428 | 0.000 |
| Occasionally | 4.121 | 2.773-5.468 | 0.000 | 3.572 | 2.084-5.059 | 0.000 |
| Often | 5.136 | 3.352-6.920 | 0.000 | 4.195 | 2.289-6.101 | 0.000 |
| Most of the Time | 5.094 | 1.890-8.298 | 0.002 | 4.062 | 0.680-7.444 | 0.019 |
Acknowledgements
Nomsa Makobo Machweu who served as a research assistant, Zvifadszo Matsena-Zingoni for serving as a statistical advisor and Megan Moll who served as a language editor for this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by Female Academic Leaders Fellowship (FALF).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
