Abstract
Alcohol consumption has been associated with metabolic risk factors (hypertension and diabetes) for non-communicable diseases (NCDS). No studies have been done in Zimbabwe linking alcohol consumption patterns and metabolic risk factors for NCDs. This study sought to compare the prevalence of alcohol consumption levels and practices between rural and urban areas among male adults and assess the relationship between alcohol consumption and metabolic risk factors for NCDs. This study made use of the cross-sectional survey using the WHO stepwise questionnaire. The indicator used in the sample size calculation was based on the proportion of men and women found to be obese when using the standard BMI measurement adopted in the 2010 Zimbabwe Demographic and Health survey. This gave a sample size of 400 with 200 participants from each of the 2 provinces. Regression analysis was performed for relationships between alcohol consumption and blood pressure, blood glucose and demographic variables. The high-income earners consumed more than the low-income earners. Those aged 25 to 34 years were more likely to consume more than those aged 18 to 24 years. The rural group was 79% (0.207 [0.770-0.559] P < .001.) less likely to have consumed 9 or more standard drinks per occasion. Respondents that practised risky alcohol consumption were more likely to have elevated blood glucose; OR, 13.629 (6.274- 29.141) P < .001. The urban group consumed alcohol more that the rural group. Alcohol consumption was significantly associated with elevated blood glucose.
Background
There is generally limited research related to alcohol consumption in Zimbabwe. 1 About 2.6 million deaths globally in 2019 were attributable to alcohol consumption. 2 It is estimated that 6.9% of the disease’s burden in the world in terms of disability-adjusted life-years (DALYs) is attributable to consumption of alcohol among men. 2 Typically, the diseases related to alcohol are non-communicable diseases (NCDs): cardiovascular diseases and cancers. However, the relationship between alcohol consumption and health risk is not linear. Studies have shown that if alcohol is consumed in small quantities, there may be a protective effect for cardiovascular diseases. 3
Studies have shown an inverse relationship between age and alcohol consumption.4 -6 This pattern may be influenced by having many friends who drink and reducing stress from different responsibilities. 4 As people grow older, the problems brought by drinking and negative reactions from family members lead to declines in the consumption of alcohol. 4 A study conducted in Japan concluded that younger people consume more alcohol than their older counterparts. 7 One scholar confirmed this pattern who revealed that younger age groups consume more with 5.1% compared to 4.9% for middle age and 3.1% for older age. 8
Studies have shown that geographical locations present different circumstances and situations that can either promote harmful alcohol consumption or protect against. 9 In Namibia, men and women in rural areas consume more than those in urban areas. 10 Namibians perceived home-brewed beer as food rather than alcohol, which is more common among uneducated people in rural areas. 10 In South Africa, urban dwellers consume more than rural dwellers, with 33.4% and 18.3% consumption levels for urban and rural areas, respectively. 11 Therefore, the patterns differ from 1 country to another, hence the need for updated research on alcohol consumption in Zimbabwe and the risks associated with it.
The NCDs survey of 2005 in Zimbabwe revealed that alcohol consumption was 57.9% for males and 13.3% for females and that males were 4 times more likely to consume alcohol than their female counterparts. 12 The statistics show that the prevalence was higher among men. This is the reason this current study is focussing on men. Further prevalence of diabetes and hypertension combined were highest in Mashonaland East Province and lowest in Bulawayo province. 13 This is the reason this study focussed on these 2 provinces to determine the underlying causes. There is a dearth of studies on the Zimbabwean context investigating alcohol consumption characteristics of urban and rural residents and the link to NCDs. 14 A 2012 Study in Zimbabwe focussed only on rural areas. 1 No studies have been done to compare the prevalence of alcohol consumption between rural and urban areas, the one by the Ministry of Health in 2005 does not differentiate between rural and urban since it compares provinces. This study analysed the alcohol consumption patterns between a rural and an urban setting. In addition, the study conducted by the Ministry of Health and Child Welfare, did not assess the relationship between alcohol consumption and demographic factors and blood glucose and blood pressure. 12 The current study assessed the associations between alcohol consumption and demographic factors, blood glucose, obesity and blood pressure.
This study sought to compare alcohol consumption levels and practices between an urban and a rural setting. It also sought to analyse the relationship between alcohol consumption and demographic factors like income, education level and age. The third objective was to analyse the association between alcohol consumption and prevalence of metabolic risk factors for NCDs that is, blood pressure, blood glucose and obesity.
Methods
Research Design, Study Population and Sampling
This study made use of a household based cross-sectional survey using the WHO-STEPwise methodology. The indicator used in the sample size calculation was based on the proportion of men found to be obese when using the standard BMI measurement adopted in the 2015 Zimbabwe Demographic and Health survey. 15 To measure risk between 2 populations the following elements were included in the sample size calculation:
Alpha: the probability of making a Type I error (-level), that is, the probability of rejecting the null hypothesis when in fact it is true, set at .05 for a 2-sided test to determine if there is a statistically significant difference
Beta: the probability of making a Type II error (-level), that is, the probability of accepting the null hypothesis when in fact it is false, set at .20 power
Proportion 1 (%): the exposed group from the urban province (18.1%)
Proportion 2 (%): The exposed group from the rural province (8.3%)
The calculation gave 184 and 9% was added to cater for non-response to give a sample size of 200 from each province. The calculated sample size was 200 in each province giving a sample size of 400. The 2 provinces were Bulawayo (urban setting) and Mashonaland east (rural setting). A multi-stage sampling procedure was followed. The primary units were the provinces that were broken down to smaller secondary units (districts), from districts to the wards, from the wards to the households and finally, the individuals. In each cluster, simple random sampling was used to select the district, ward and households. Enumeration areas were demarcated in all wards in the provinces prior to the 2012 national census. These enumeration areas had a list and location of all the households. This study made use of a sample of 10 wards (enumeration areas) drawn from the 2 provinces. Random sampling was used to select those eligible in the household, (males aged 18 years and above and those who slept in the household at least 4 nights in the last week). This study used a sample of 10 wards (enumeration areas) drawn from the 2 provinces. In each enumeration area, 40 males from 40 households were sampled. It should be noted that 20% was added to cater for non-responses. The inclusion criteria for participants was any male aged 18 years and above and those that slept in the household at least 4 nights in the last week of the study. Exclusion criteria was any male below the age of 18 years and were visitors that is, those that did not spent at least 4 nights in the last week of the study.
Ethical clearance certificate number BF505/16 was obtained from the biomedical research ethics committee of university of KwaZulu Natal. Permission was sought from the Ministry of Health and Child Care (MMHCC) and all participants were given a consent form and those that agreed and signed participated in the study. As required by the Declaration of Helsinki, a letter was granted to seek consent and voluntary participation from all the respondents. The participants were free to decide whether to participate or decline and were reminded that their participation was voluntary. Anonymity and confidentiality of the participants were preserved by keeping their names and identities away from the research findings and reporting of the study.
Data Collection Tools and Procedures
Alcohol consumption was measured using the 1 standard drink equivalent recommended by the alcohol Policy of Zimbabwe, which would be 1 standard bottle of standard beer (285 ml) or 1 single measure of spirits (30 ml). 16 Using WHO guidelines, a daily intake of 6 or more drinks on occasion once a week was considered high-risk behaviour. 17 Consumption of alcohol above the limit of 15 standard drinks a week or 6 or more drinks on any 1 occasion puts people at risk of NCDs. 17 Low-risk drinking for men was 2 to 3 standard drinks per day with at least 2 alcohol-free days per week. 17 Those who reported drinking 3 or more days a week were categorised as risky consumption, and those who reported drinking more than 6 drinks on 1 or more occasion in the last 30 days.
Following the American Heart Association’s recommendations, blood pressure measurements were done using a blood pressure monitor. 18 The participant was made to sit upright and relax for 5 min before the first reading was taken to measure correct values that are not influenced by any form of exercise since this tends to increase blood pressure. 18 Systolic blood measurement of 140 mmHg and above and diastolic blood measurement of 90 mmHg and above were considered elevated blood pressure levels. Blood pressure for those on treatment was considered under those with elevated blood pressure.
Blood glucose levels were determined from the measurements using a glucose metre. Sino care glucose metre was used (brand- Safe Accu). Calibration was performed every time a new batch of strips was used. A test using the control solution was done to check for accuracy. Measurements were done in the morning, before the respondents had breakfast. The advantage was that these readings reflected night measurements and are important for sugars related to diabetes control. Normal blood glucose ranged from 4 to 6 mmol/l, prediabetes ranged from 6.1 to 6.9 mmol/l, and those with more than 7 mmol/l were considered to have elevated blood glucose. Those on treatment for diabetes were considered among those with elevated blood glucose. Participants were asked about when they last ate and measurements were taken for fasting periods of between 8 and 12 h.
Body mass index (BMI) was calculated from height and weight measurements, which was used as an indicator for obesity. For BMI, the ranges used were as follows: 30 and above (Obese), 25 to 30 (overweight), 18.5 to 24 (Normal) and below 18.5 (underweight). Those that were overweight and obese were considered to be at risk.
Data Analysis
The study used the independent samples t test to investigate if there were any significant differences in total consumption between rural and urban areas. Logistic regression was used to investigate differences in alcohol consumption practices between rural and urban settings, the relationship between alcohol consumption and blood glucose level, blood pressure and obesity.
Results
Demographic Characteristics
Table 1 displays respondents’ demographic distribution according to income, age, education level, and marital status. Rural respondents earned less than the urban respondents (were 93% less likely to earn above $600.00 compared to the urban respondents, P < .001). The rural group had a fewer number of respondents with tertiary education (P < .015).
Demographic Characteristics of Study Participants, (n = 400).

Alcohol Consumption Practices Between the 2 Settings
The number of days when alcohol was consumed in the rural setting was less than in the urban setting (Table 2). In terms of binge drinking, the rural group was 2.6% less likely to have consumed 6 or more drinks than the urban group and was also 62% less likely to have consumed 6 or more drinks per occasion at least 4 times in the last 30 days before the survey. Rural respondents were 55% less likely to agree that those that consume alcohol are relieving themselves of stress than respondents in urban areas (Table 2). The rural group was 75% less likely to state that alcohol consumers enjoy their leisure time than the urban group.
Alcohol Consumption Practices Between the 2 Provinces and Perceptions of Study Participants Towards Alcohol Consumption, (n = 400).

Risky Alcohol Consumption and Demographic Characteristics
Contrasted to the age group 18 to 24 years, the age groups 25 to 34 years and 35 to 44 years were 5 times and 10 times more likely to consume alcohol, respectively (Table 3). The divorced and widowed were 2 times more likely to practice risky alcohol consumption behaviours than the singles group. Those with higher education attainments were more likely to consume alcohol beyond the recommended levels than the lower education group. The group earning above $600.00 was 3 times more likely to practice risky alcohol consumption behaviours than those earning below $301.00.
The Relationship Between Risky Alcohol Consumption and Demographic Characteristics of Study Participants, (n = 400).

Distribution of Blood Pressure
The mean systolic blood pressure was higher among the rural group (134.50) than the urban group (130.15), (P < .036). According to Table 3, rural respondents were 70% more likely to have normal diastolic blood pressure than those in urban areas. After combining systolic and diastolic blood pressure, the rural group was 52% more likely to have respondents with elevated blood pressure. Respondents that practised risky alcohol consumption were more likely to have elevated blood glucose; OR, 13.629 (6.274-29.141) P < .001. Those with elevated blood pressure were referred to the nearest health centre to monitor their blood pressure (Table 4).
Distribution of Blood Pressure Characteristics of Study Participants, (n = 400).

Blood Glucose Distribution and Obesity Levels
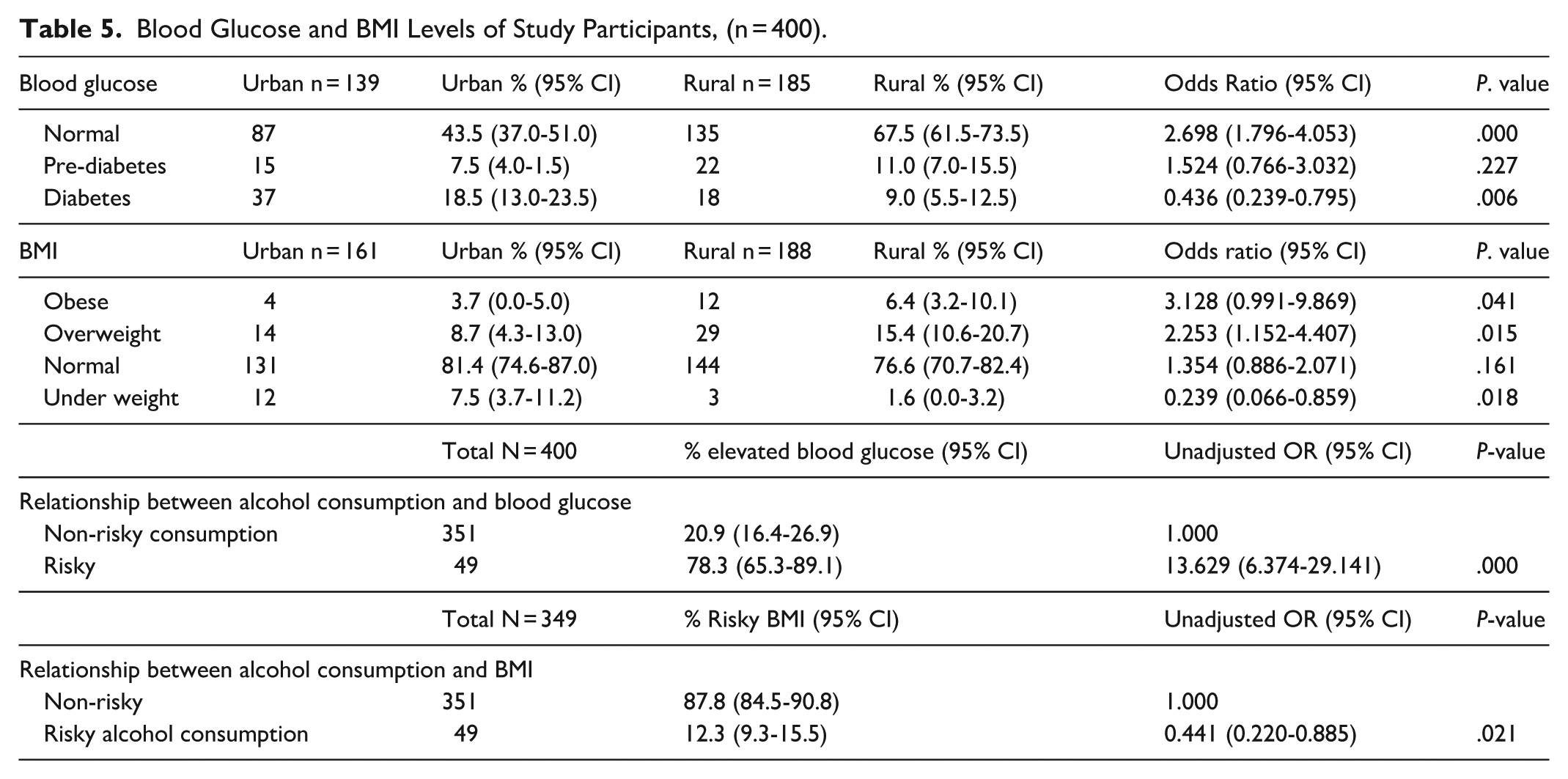
The mean blood glucose for the urban group was higher (6.14) than the rural group (5.5), P < .001. Table 5 shows that respondents in rural areas were 56% less likely to have elevated blood glucose than the urban respondents. The rural group was 213% more likely to have respondents that are obese than the urban group. The rural group were 125% more likely to have people that were overweight. The rural group had higher mean BMI than the urban group (23.5 and 21.7 respectively), t test P < .011. The group that consumed alcohol to the recommended level was 272% more likely to have elevated blood pressure. The group that practiced risky alcohol consumption behaviours was 56% less likely to have high BMI.
Blood Glucose and BMI Levels of Study Participants, (n = 400).
Discussion
The study sought to analyse alcohol consumption patterns between an urban setting and a rural setting. Urban dwellers consume more alcohol than rural dwellers, and the rural group was 57% less likely to consume alcohol to levels that expose them to the risk of NCDs. This pattern of more consumers in urban areas confirms patterns observed in other African countries and has been attributed to urbanisation.11,19,20 The overall alcohol consumption of 39.8% for both areas is lower than the 58% for 2005 and higher than the 2016 national average.2,12 More people in rural areas in the current study consume alcohol than Cubbins et al, who found 20% in an earlier study in Zimbabwe. 1 This may be due to improvements in access to information brought by social media, making alcohol consumption acceptable in rural areas. Those in urban areas viewed consumption of alcohol as a stress reliever leading to higher consumption levels. The rural group was 75% less likely to state that alcohol consumers enjoy their leisure time than the urban group showing that urban respondents viewed alcohol consumption as a leisure time activity. This could have contributed to higher levels of consumption in an urban setting. The way 1 perceives alcohol consumption has influence on consumption patterns.
The pattern observed differed from Namibia’s experiences. A smaller number of urban dwellers consume alcohol than rural areas, mainly because in rural Namibia, alcohol is part of people’s diet. 10 Similarly, a study on youths in rural Mongolia found higher alcohol consumption rates in rural areas. 21 This was because, in rural areas, it was widely accepted for people to drink alcohol. One in 4 (25%) of urban residents in the current study participated in binge drinking contrasted to 12.5% in rural areas. The figures for both areas are lower than the 2014 national average of 42.5% 22 .
Respondents aged 35 to 44 years were significantly more likely to report risky alcohol consumption patterns than those aged between 18 and 24 years. Scholars have concluded that middle-aged people consume more than the other age groups.4 -6 This is because of the influence from friends that also drink and the need to reduce stress from different responsibilities. 4 It should be borne in mind that this is an economically active group. Those aged above 45 years consumed less than middle-aged people, which confirms findings from other countries.4,7,8 As people grow older, the problems brought by drinking and negative reactions from family members lead to declines in the consumption of alcohol. 4 This was similar to the Mashonaland Central and Midlands province patterns, with the age group 25 to 34 consuming more than the other age groups. 12 However, the pattern is different from patterns observed in Matabeleland South province, where the age group 45 to 64 had the highest rates. 12 The divorced/separated/widowed consumed more than the married. This proves the protective effect of marriage,23,24 related to family roles.25,26 A considerable number of people from the singles group consume to excessive levels (10.5%), showing high consumption rates among young people who are not married. This confirms the pattern observed earlier in Zimbabwe, America, South California, and Japan.1,4,6,7 The high-income earners consume more than the low-income earners, with those earning above $600.00 being 3 times more likely to consume to excess than those earning below $301.00. Urban areas with higher income have more people that consume than rural areas. This pattern is different from findings by other scholars who concluded that those with low income consume alcohol to excessive levels more than those with high income because of stressful living conditions.27 -29 The reason for low rates in rural areas in the current study may be low income since people are struggling to provide for necessities where 90% live below the poverty datum line. 30 The explanation in developed countries is that those in disadvantaged communities have no social support and are isolated from formal job markets and create conducive environments for substance abuse. 31 Thus, the explanations given depend on each setting’s economic environment as results have shown varying relationships.
Education has a positive relationship with excessive alcohol consumption, where those with higher educational attainments were 2 times more likely to consume than those with lower education. The same pattern was observed in Zimbabwe, South Africa, and Taiwan.1,11,32 The reason for such is that those with education secured employment and have income that can allow them to consume alcohol, which is different for those without education who cannot afford to purchase alcohol. 11 The educated in Zimbabwe have higher chances of getting employed and hence can buy more than 6 drinks at once. 1 However, other studies in developed countries like England and Japan have shown that the educated may consume more but do not consume beyond stipulated levels.7,33 The reason was that education influences people’s behaviour positively; however, in this current study, the educated are the ones that can afford to drink to excessive levels. In a society where living standards are too low, the less educated fail to buy alcohol. 34
The urban group had a higher diastolic mean than the rural group (86.61 and 78.83 respectively). However, rural respondents had a higher systolic mean than the urban respondents (134.5 to 130.2), and overall, 27% of urban respondents were hypertensive contrasted to 36% in the rural group. Thus, rural respondents had more people who had elevated blood pressure. This confirms the study findings in Turkey where prevalence was higher in rural areas. 35 This is different from other studies which have concluded that rural areas have lower rates.36 -41 It was interesting to note that those that did not consume to risky levels had higher odds of having elevated blood pressure because of other lifestyle risk factors that were not covered in this current study.
Rural respondents had lower blood glucose levels than the urban respondents (5.5 and 6.14 respectively). These are, however, higher than the national average of 5.3. 12 The current study’s means are higher due to differences in sample sizes (smaller sample size and exclusion of women in the current study). Almost 1 in 5 (18.5%) of the urban respondents had elevated blood glucose levels contrasted to 9% of rural respondents, and no one was on treatment. The urban setting had a higher number of people with elevated blood glucose than the national average of 9%. 12 The pattern is similar to some scholars’ findings who concluded that diabetes was higher in urban areas.41 -43
Those who consume alcohol to excessive levels were more than 10 times more likely to have elevated blood glucose than those who do not consume alcohol. This confirms findings from other scholars who concluded that heavy drinkers have higher chances of having elevated blood glucose because of increased insulin resistance.44,45 Urban respondents were more likely to have elevated blood glucose because they had higher chances of having heavy drinkers than the rural group. Alcohol consumption is the reason for the higher levels in the urban group.
Limitations of the study may include memory lapse since information collected was based on memory, this might have led to collection of biased information. This study collected quantitative data and lacked explanations to the patterns observed because it was a survey that did not collect qualitative data. Data on blood pressure and body mass index could have been influenced by other factors like physical activity and diet which were not analysed in this study. The study findings may not be generalised for the whole population because it only focussed on males.
Conclusion
Results have shown that urban dwellers consume more alcohol than rural dwellers. Binge drinking is common among those in urban areas with high income and higher educational attainments. Alcohol consumption is significantly associated with elevated blood glucose. Urbanisation leads to high alcohol consumption exposing people to metabolic risk factors for NCDs. There is need for health education programmes targeting reduction of alcohol consumption in urban areas focussing on workplace alcohol screening programmes and Integration of alcohol counselling in NCD prevention.
Footnotes
Acknowledgements
We would thank the Ministry of Health and Child Care for permitting us to conduct this study.
Ethical Considerations
Ethical clearance certificate number BF505/16 was obtained from the biomedical research ethics committee (BREC) of a university of KwaZulu Natal. Permission was sought from the Ministry of Health and Child Care (MMHCC) and all participants were given a consent form and those that agreed and signed participated in the study.
Consent to Participate
As required by the Declaration of Helsinki, a letter was granted to seek consent and voluntary participation from all the respondents. The participants were free to decide whether to participate or decline and were reminded that their participation was voluntary. Anonymity and confidentiality of the participants were preserved by keeping their names and identities away from the research findings and reporting of the study.
Author Contributions
NM: conceptualisation, research design, data collection supervision, analysis and interpretation of data, drafting the article, revising for publication. KV: Conceptualisation, analysis and data interpretation, final approval, WNN: Research design, analysis and interpretation of data, revising for publication, NM: analysis and interpretation of data, revising for publication.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Data is available upon request.
