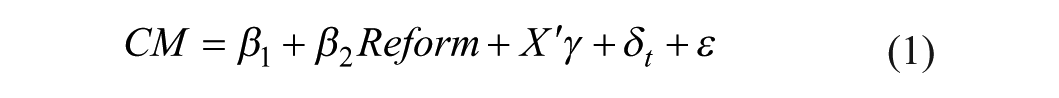Abstract
The Diagnosis–Intervention Packet (DIP) payment reform aims to enhance cost efficiency in healthcare delivery but may also induce adaptive physician behavior. This study examines whether the DIP reform leads physicians to shift conventional medical demand toward traditional medicine. Using patient-level data from a Chinese integrative medicine hospital, we analyze changes in conventional and traditional medicine expenditure structures before and after the DIP reform, with heterogeneity analyses across insurance schemes and age groups. Conventional medicine expenditures decreased significantly, while traditional medicine expenditures increased substantially after the reform, indicating physician-induced service substitution from conventional to traditional medicine. These findings suggest that although the DIP reform effectively contains conventional medicine costs, it may unintentionally transfer excessive medical demand to traditional medicine, underscoring the need for integrated regulatory mechanisms across medical treatment systems.
Keywords
Introduction
As the population ages and demand for healthcare continues to grow, the national health insurance fund of China faces immense pressure, particularly from the unreasonable rise in patient medical expenses driven by physician-induced demand.1,2 Globally, healthcare payment models have been undergoing continuous reform to control rising medical costs and enhance the efficiency of healthcare resource utilization.3 -7 Building on the U.S.-based DRG (Diagnosis-Related Groups) payment reform, China has initiated a pilot reform with the DIP (Diagnosis-Intervention Packet) payment model, aiming to mitigate the issues of excessive medical interventions and escalating costs inherent in traditional fee-for-service models.
DIP, fully named “Regional Budget Point System and Payment by Diagnosis-Intervention Packet,” is a big data-driven innovative medical insurance payment method. Currently, the system is primarily applied to inpatient services, with a single hospitalization episode serving as the settlement unit. Similar to the DRG payment system, DIP follows the core logic of “prospective case-based payment,” whereby cases are categorized according to diagnosis and treatment type, and each group is assigned a relatively fixed payment standard. This design incentivizes healthcare institutions to proactively control costs and optimize clinical pathways in order to improve service efficiency.8 -11 In its specific design, DIP operates under a regional global budget framework: the healthcare insurance authority sets an annual aggregate budget and determines diagnosis-specific point weights based on historical cost data. During actual settlement, the monetary value per point fluctuates dynamically according to the total points accrued from all settled cases across medical institutions in the region. This mechanism achieves the policy goal of “controllable total expenditure and retention of surpluses.” To equitably reflect actual medical resource consumption and better align with the treatment costs of different age cohorts, DIP incorporates a multi-dimensional adjustment mechanism. This includes case severity adjustments based on comorbidity and complication indices, an exceptional case review mechanism for outliers, as well as payment calibrations for specific patient groups. For example, the system applies specialized disease identification and weight adjustments for pediatric patients under 18 years of age according to their developmental stages.
In China, traditional medicine is often integrated as a complementary approach alongside conventional medicine within clinical practice. Notably, the DIP payment system has implemented a pilot policy of “equal payment for equal disease and equal efficacy” for selected disease groups where traditional medicine is clinically advantageous, under which traditional medicine treatments are reimbursed at the same rate as conventional medicine treatments provided that comparable therapeutic outcomes are achieved. This mechanism not only establishes payment parity between traditional and conventional medicine but also creates a financial incentive for healthcare institutions to adopt lower-cost traditional medicine treatment pathways within a fixed payment cap. As a result, the combination of payment equivalence and the relative cost advantage of traditional medicine may encourage physicians to recommend traditional medicine more frequently in clinical decision-making.
However, existing studies have primarily focused on evaluating the aggregate cost-containment effects of payment reforms, with limited empirical investigation into potential structural shifts in physician behavior across different types of medical services. Specifically, within the incentive framework of DRG/DIP prospective payment—particularly given the cost differences and payment parity between traditional and conventional medicine—it remains unclear whether physician-induced demand could take the form of a substitution effect, shifting from higher-cost conventional medicine services toward lower-cost traditional medicine alternatives. To address this gap, this study utilizes patient-level data from a hospital that offers both traditional and conventional medicine to analyze changes in traditional and conventional medicine expenditures before and after the implementation of DIP.
The significance of this study can be summarized as follows. First, this study enriches the understanding of how payment reform impacts Physician-Induced Demand, particularly across different types of medical services. Second, the findings provide evidence to help policymakers design balanced payment reforms that prevent unintended shifts in physician behavior. At last, the paper offers guidance for the sustainable development of integrative medicine by evaluating the role of traditional medicine under payment reform.
Literature Review
Physician-Induced Demand
Physician-Induced Demand arises when physicians, influenced by economic incentives beyond patient health needs, utilize their informational advantage over patients to recommend higher-revenue treatments.12 -14 This dynamic reflects the inherent conflict between physician income goals and patient welfare, where physicians might increase the volume of specific procedures or substitute services with higher reimbursements to sustain income levels. Research examining responses to income shocks has shown that physicians often react to revenue reductions by amplifying service frequency or adjusting billing practices. 15 For example, in response to fee cuts or declining demand, some studies reveal that physicians may increase high-cost interventions, like surgical procedures,12,16 or engage in “upcoding” to move patients into higher-reimbursement diagnosis groups.17,18
In the Chinese healthcare context, price regulation provides further institutional support for physician-induced demand. Due to the dominance of public secondary and tertiary hospitals, which hold significant market power, price control policies are essential to contain medical costs but can inadvertently encourage demand-inducing behaviors. 19 Without autonomy to set service prices, hospitals may rely on prescribing more pharmaceuticals and consumables to increase revenue, as government-imposed pricing regulations restrict direct service price adjustments. Theoretical studies have demonstrated that when public hospitals lack pricing flexibility, they may compensate by overprescribing medications and devices, 20 which has led to phenomena like “drug mark-up reliance” and “device mark-up reliance.” This practice not only undermines patient welfare by escalating unnecessary healthcare costs but also introduces further market distortions, 21 suggesting that current price regulations alone may be insufficient to curb physician-induced demand in monopolistic or oligopolistic healthcare settings.
In this context, the Chinese healthcare system faces unique challenges due to these structural dynamics and regulatory constraints, which prompt hospitals to offset income losses through increased utilization of pharmaceuticals and high-cost devices. These tendencies highlight the limitations of price regulation in effectively aligning physician behavior with patient welfare, especially when significant market power and restricted pricing autonomy remain key features of the healthcare environment.
DIP Reform
The implementation of DRG payment models can effectively control the growth of healthcare costs and improve the efficiency of health insurance fund operations.9,22 -25 For instance, the U.S. Medicare system has significantly reduced unnecessary hospitalizations through its DRG system, 26 though it has also led to issues such as patient selection by hospitals. 27 In China’s healthcare system, the adoption of the DIP payment model aims to control costs, increase resource utilization efficiency, and gradually drive reform. 28
However, existing literature suggests that due to the fragmented nature of China’s health insurance system, payment reform may enable physician-induced demand to manifest in more concealed forms.29 -31 Physicians may, for example, increase the frequency of expensive diagnostic procedures or encourage the use of medications outside the insurance formulary,32 -34 thus boosting their covert income. In recent years, China’s policies supporting traditional medicine have driven its resurgence, with many patients increasingly choosing traditional medicine for chronic or non-acute conditions. Following payment model reforms, traditional medicine’s lower costs and flexible treatment options have made it an appealing choice for a broader patient base. conventional medicine remains dominant in treating acute conditions and in the application of modern medical technology. However, due to the high costs and standardized nature of conventional medical treatments, both hospitals and patients tend to reduce their use of these services under the new payment reforms.
In summary, existing research has established 2 key points: (1) physician-induced demand is prevalent and takes distinctive forms within China’s price-regulated healthcare setting; and (2) DRG/DIP payment reforms are effective in containing aggregate costs but may also change the manner in which such demand manifests. A significant research gap remains, however: most studies examine healthcare expenditures or physician behavior in the aggregate, or focus only on changes within a single treatment modality. They have not empirically tested whether—in a context where both traditional and conventional medicine coexist and payment policies introduce new relative prices and incentives—induced demand might undergo a structural shift or substitution between these 2 service types. This study aims to address that gap by analyzing changes in traditional and conventional medicine expenditures before and after the DIP reform, thereby exploring how payment reforms reshape physicians’ referral patterns across distinct categories of care.
Materials and Methods
Policy Background and Sample Selection
This study focuses on the city of X in China, where DIP payment reform was implemented on July 1, 2022. An integrated traditional and conventional medicine public hospital, representative in scale and patient volume within the local healthcare landscape, was selected as the research site. To assess the reform’s impact, we collected patient-level data covering a period from 6 months before to 18 months after the reform (January 1, 2022, to March 31, 2024).
Data on each patient’s demographic characteristics (such as gender, age), insurance type, diagnostic information, treatment plans, and detailed cost information (including conventional medicine and traditional medicine expenses) were collected from the hospital’s electronic medical records and financial reports. All data were anonymized to protect patient confidentiality and comply with ethical standards.
The initial sample included all inpatient admissions during this period. We excluded cases with missing data on any key variables. To mitigate the influence of outliers, we also excluded observations with medical expenditures in the top or bottom 1% of the distribution. The final analytic sample consisted of 20 762 patients. This comprehensive dataset provides a robust foundation for examining service substitution from conventional to traditional medicine following the DIP reform.
Quasi-Experimental Design
The quasi-experimental design is a widely used methodological approach in empirical social science research. Its core rationale lies in leveraging exogenous policy changes or natural experiments to mimic experimental conditions. By comparing differences between treatment and control groups before and after a policy shock, and by employing statistical control strategies to account for potential confounding factors, this design enables credible inferences about causal effects. 35 Following this approach, this study assesses the causal effect of the DIP payment reform on healthcare expenditures. We leverage the reform’s implementation as an exogenous policy shock and adopt a pre-post comparison framework. The core of our identification strategy is to compare patient-level expenditures for conventional and traditional medicine before and after the reform, while controlling for potential confounders. To isolate the net effect of the reform, we estimate the following econometric specification:
The dependent variables are total expenses for conventional medicine (CM) and traditional medicine (TM) incurred during a single hospitalization. The independent variable is the DIP payment reform (Reform), a dummy variable where 0 represents the period before the implementation of the DIP payment reform (January 1, 2022, to June 30, 2022), and 1 represents the period after the reform (July 1, 2022, to March 31, 2024). X is a vector of control variables.
Control variables include patient demographic characteristics, such as age and gender, to account for individual differences that may affect medical expenses. Disease type (DiseType) is included as a control variable based on the ICD-10 three-digit category, which provides a substantially more detailed classification than chapter-level codes. This approach allows us to control for a wide range of specific diagnoses and strengthens our ability to attribute observed cost changes to behavioral responses rather than shifts in the composition of diseases. Patient income is an important factor influencing medical expenses; however, due to the lack of patient income data, this study uses the patient’s insurance type (InsurType) as a proxy and includes it as a control variable in the model. In China, basic medical insurance is divided into 2 types: Urban Employee Basic Medical Insurance (UEBMI), which covers employees, and Urban and Rural Resident Basic Medical Insurance (URRBMI), which covers both urban and rural residents. The former generally has a higher payment capacity than the latter. The InsurType variable is a dummy variable, coded as 1 if the patient is enrolled in UEBMI, and 0 if the patient is enrolled in URRBMI.
To address potential heteroskedasticity, heteroskedasticity-robust standard errors are reported for all regressions. The following diagnostic tests were performed to ensure the reliability of the results: (1) variance inflation factor (VIF) tests confirmed that all VIF values were below 5, indicating no severe multicollinearity; and (2) residual analysis was conducted to examine the linearity assumption and the overall model specification. Moreover, all methods and analyses adhered to the recommendations outlined by the Second Panel on Cost-Effectiveness in Health and Medicine and the Consolidated Health Economic Evaluation Reporting Standards (CHEERS) statement. 36
Table 1 presents the descriptive statistics of the study sample. The average expenditure per hospitalization on conventional medicine was CNY 2005.02, nearly double that of traditional medicine, which was CNY 1045.41. The sample consisted of an equal gender distribution, with 50.0% male and 50.0% female patients. The average patient age was 63.57 years. In terms of insurance coverage, 63.0% of patients were enrolled in the UEBMI, while 37.0% were covered by the URRBMI. Regarding the policy timeline, 68.0% of the encounters occurred in the post-reform period. For disease classification, diagnoses were coded using ICD-10 at the 3-digit level, with codes ranging from 1 to 579.
Descriptive Statistics Results (N = 20 762).

Empirical Results
Expenditure Trends Before and After DIP Implementation
Figure 1 depicts the average expenses per hospitalization for conventional and traditional medicine, along with their respective changes before and after the implementation of the DIP payment reform. Specifically, prior to the DIP reform, the average conventional medicine expense per admission was CNY 2244.13; following the reform, the figure decreased to CNY 1892.84, indicating an average reduction of CNY 351.29 in conventional medicine costs. In contrast, the average traditional medicine expense per admission shows an opposite trend, increasing by CNY 50.26 after the reform. These preliminary observations suggest that the DIP payment reform may have led to substitution effects between the 2 categories of per-admission expenses. However, descriptive statistical analysis alone is insufficient to scientifically explain the causal relationship between DIP payment reform and changes in medical expenses. To provide more rigorous evidence, subsequent sections will employ more stringent statistical methods for a detailed examination.

Comparison of expenditure on CM and TM before and after DIP reform.
Baseline Regression Results
To obtain scientifically credible evidence, we estimated the baseline regressions based on models (1) and (2) to examine the impact of DIP reform on per-admission expenses for conventional and traditional medicine. The results are shown in Table 2 (Baseline regression columns). Columns (1) and (3) report estimates without control variables, while columns (2) and (4) include the full set of controls. For conventional medicine expenses, the coefficient on Reform is significantly negative in both specifications: −511.99 (P < .01) without controls and −494.57 (P < .01) with controls. According to the preferred specification in column (2), the DIP reform reduced per-admission conventional medicine expenses by approximately CNY 494.57. For traditional medicine expenses, the coefficient on Reform is significantly positive: 122.94 (P < .01) without controls and 147.65 (P < .01) with controls. The estimate in column (4) indicates that the reform increased per-admission traditional medicine expenses by about CNY 147.65.
Baseline Regression and Placebo Test Results.

Note. Standard errors are in parentheses.
, **indicate significance at the 1% and 5% levels, respectively.
These results suggest that while the DIP payment reform has effectively contained conventional medicine expenses, it appears to have simultaneously induced a shift toward greater use of traditional medicine at the per-admission level. This shift may reflect the heightened cost-control pressures on hospitals and physicians under the DIP payment system, leading them to favor more cost-effective treatment options. Where traditional medicine is perceived to offer a cost advantage or comparable therapeutic effects, physicians may be more inclined to recommend it. Consequently, although the reform has contributed to lowering overall medical expenditures, it has also altered the composition of care, resulting in a rise in the traditional medicine expenses.
Placebo Test
To verify the robustness of the baseline regression results, we conducted a placebo test by introducing a dummy variable named P_reform, representing the timing of the DIP reform. This variable is defined to take a value of 1 for the period before a hypothetical reform date (May 2022), and 0 for the period after. We then estimated the model using only the sample from before the actual reform implementation in July 2022. The results, presented in columns (5) and (6) of Table 2, show that the coefficients on P_reform are statistically insignificant at the 10% level for both conventional and traditional medicine expenditures. This suggests that prior to the reform, no systematic pre-existing trends drove the observed changes in medical expenses, thereby supporting the reliability of our main findings.
Heterogeneity Analysis
Service Substitution by Insurance Type
Patients’ payment capacity may influence physicians’ demand-inducing behavior. Compared to patients enrolled in the URRBMI, those covered by the UEBMI generally have more stable employment income or higher pensions, indicating stronger ability to pay. We therefore estimated the effect of the DIP reform on per-admission expenses for conventional and traditional medicine separately by insurance type. The results are shown in Table 3, Panel A.
Heterogeneity Analysis.

Note. Standard errors are in parentheses. Panel A controls: Gender, Age, DiseType. Panel B controls: Age, InsurType, DiseType. Panel C and D controls: Gender, Age, InsurType, DiseType. “Yes” indicates that the full set of controls and a constant term were included. Coefficient estimates for controls are omitted for brevity.
, **indicate significance at the 1% and 5% levels, respectively.
Columns (1) and (2) of Panel A present the results for conventional medicine expenses per admission. The coefficient on Reform is significantly negative at the 1% level for both insurance groups. Specifically, the reform reduced per-admission conventional medicine expenses by CNY 437.38 among UEBMI enrollees and by CNY 605.04 among URRBMI enrollees, indicating a larger reduction for the latter group. Columns (3) and (4) present the results for traditional medicine expenses per admission. The reform increased these expenses by CNY 165.77 (P < .01) for UEBMI patients. Although the point estimate is smaller for URRBMI patients, the increase remains statistically significant. This pattern suggests that, after the reform, a shift toward traditional medicine occurred in both groups, but was more pronounced among patients with higher payment capacity (UEBMI enrollees). Patients with more limited payment capacity may retain a relatively stronger preference for conventional medicine—often associated with shorter treatment cycles and more immediately perceptible outcomes—which could attenuate the magnitude of the shift toward traditional medicine in this subgroup.
Service Substitution by Gender
Table 3, Panel B presents the estimated impact of the DIP reform on per-admission expenses for conventional and traditional medicine, stratified by patient gender. For conventional medicine expenses per admission, the coefficient on Reform is significantly negative for both women (coefficient = −427.80, P < .01) and men (coefficient = −563.71, P < .01), indicating a substantial reduction after the reform. Similarly, for traditional medicine expenses per admission, the coefficient on Reform is significantly positive for both women (coefficient = 103.50, P < .01) and men (coefficient = 193.27, P < .01), reflecting a consistent increase across genders. The direction and statistical significance of these effects are aligned between genders, suggesting no qualitative difference in how the reform influenced medication expenses. This gender-neutral pattern indicates that the financial incentives embedded in the DIP system operate consistently across demographic groups, without systematic bias related to patient gender. Such consistency further supports the generalizability of the reform’s behavioral effects in real-world practice.
Service Substitution by Age Group
This study categorizes age into 3 intervals: 1 to 15 years (pediatric patients), 16 to 59 years (working-age adults), and 60 years and above (elderly). The sample is stratified accordingly for subgroup regression analysis to examine the effects of the DIP reform on per-admission expenses, as shown in Table 3, Panel C.
For conventional medicine expenses, the DIP reform significantly reduced costs for the working-age adults(coefficient = −398.27, P < .01) and the elderly (coefficient = −554.18, P < .01). In contrast, the effect on pediatric patients was negative but not statistically significant (coefficient = −248.23, P > .1). For traditional medicine expenses, the reform led to a significant increase across all age groups. Notably, the magnitude of increase was largest among pediatric patients (coefficient = 272.81, P < .01), followed by the elderly (coefficient = 154.83, P < .01) and the working-age adults (coefficient = 132.64, P < .05).
Notably, for pediatric patients, the DIP reform did not produce a statistically significant reduction in per-admission conventional medicine expenses, while it was associated with a significant rise in per-admission traditional medicine expenses. This pattern may stem from multiple factors. First, medical demand among pediatric patients tends to be less elastic, and guardians may be less willing to compromise on the perceived quality or immediacy of conventional medicine, which could attenuate the reform’s cost- containment effect on conventional medicine expenses for this group. Second, within the fixed payment cap of a DIP bundle, providers have a financial incentive to adopt treatment pathways with lower variable costs. For the pediatric subgroup, traditional medicine may present a relatively lower-cost alternative within the allowed budget, prompting a more pronounced shift in its use. Additionally, the specific disease profile of this age group or a perceived comparative advantage of traditional medicine for certain pediatric conditions could further amplify this substitution effect.
Service Substitution by Disease Severity
This section analyzes whether the impact of the DIP payment reform varies by disease severity and assesses whether the observed effects could be attributed to changes in patient case-mix, such as the possibility that hospitals admitted milder cases after the reform. We calculated a simplified Charlson Comorbidity Index (CCI) based on the primary diagnosis and stratified the sample into 3 subgroups: mild (CCI = 1), moderate (CCI = 2), and severe (CCI = 3). Regression results are presented in Table 3, Panel D.
The analysis reveals systematic variation in the reform’s effects across severity levels. For patients with mild conditions (CCI = 1), the reform significantly reduced per-admission conventional medicine expenses (coefficient = −339.88, P < .01) while increasing per-admission traditional medicine expenses (coefficient = 140.06, P < .01). For those with moderate conditions (CCI = 2), the effects were more pronounced, showing a greater reduction in conventional medicine expenses per admission (coefficient = −1269.92, P < .01) and a larger increase in traditional medicine expenses (coefficient = 266.80, P < .01). In contrast, for patients with severe conditions (CCI = 3), no statistically significant effect was observed for either conventional medicine (coefficient = −270.65, P > .1) or traditional medicine expenses (coefficient = −159.18, P > .1).
These results reveal a distinct gradient and a clear clinical boundary in the reform’s impact. The policy shifted medication expenses for patients with mild and moderate conditions, with the most pronounced effect observed in the moderate group. This pattern suggests that the reform’s incentives were most effective where greater clinical flexibility existed. Conversely, the absence of significant effects among severe patients is consistent with more rigid treatment pathways and limited clinical discretion, which delineates the scope of the reform’s applicability. Crucially, the observed non-monotonic pattern, where effects did not intensify as disease severity decreased, rules out the alternative explanation that findings were driven by a systematic shift toward admitting less severe patients. Therefore, this subgroup analysis confirms that the observed changes in medication expenses reflect genuine behavioral adjustments in clinical practice induced by the DIP reform, rather than changes in patient composition.
Discussion
This study provides evidence that the DIP reform led to a significant reduction in conventional medicine expenses and an increase in traditional medicine expenses per admission, providing evidence of physician-induced service substitution. The heterogeneity observed across patient subgroups offers insights into the underlying mechanisms. The more pronounced substitution among pediatric patients may reflect both specific payment adjustments and greater clinical flexibility in this population, while the larger effect among patients with moderate versus mild conditions suggests that substitution is not merely driven by disease severity shifts. The absence of significant effects among severe patients aligns with the expectation that rigid treatment pathways limit behavioral responses.
To address the physician-induced service substitution emerging from the payment reform, several policy interventions can help balance the supply and demand for different medical services. One approach is to strengthen the regulation and standardization of traditional medicine treatments. Enhanced oversight is needed to ensure the necessity and rationality of these services. This can be achieved by developing clearer treatment standards and cost regulations to prevent excessive or unnecessary treatments. Policies could also require traditional medicine treatments to undergo professional evaluation, ensuring that care is based on clinical needs rather than induced substitution.
Another key strategy is to increase payment system flexibility. While controlling costs, policies should accommodate demand for different services types. Alongside DIP, a more tiered payment model could set reimbursement standards according to patient’s health condition, disease type, and treatment needs. This would help control unnecessary conventional medicine treatments while guiding appropriate traditional medicine supply, reducing over-reliance on any single service type and mitigating substitution effects.
Service substitution is often financially motivated. To reduce unnecessary care, strengthening ethical and professional responsibility among physicians is essential. Periodic training, particularly in the post-reform period, should be conducted to help physicians understand reform goals and the importance of health management, thereby encouraging appropriate treatment recommendations.
Increasing patient involvement in treatment decisions can improve understanding of available options and costs. Transparent information platforms could provide details on treatment, costs, and effectiveness. This reduces reliance on physician-driven decisions and supports more informed patient choices, thereby limiting unnecessary care and opportunities for substitution.
Finally, a more rigorous review system can prevent over-treatment. Beyond post-service audits, monitoring and evaluating traditional medicine and conventional medicine treatments should be strengthened. Big data analytics can identify irregular patterns, and third-party agencies can oversee hospital medical practices to ensure reforms are implemented effectively.
This study has several limitations. First, the analysis is based on a single-hospital pre-post design without an external comparison group, which limits causal inference to some extent. To address potential confounding, we controlled for extensive patient-level covariates and included month fixed effects to account for time-specific unobservables. These analytical strategies enhance the credibility of our causal inferences, although residual confounding from unmeasured time-varying factors cannot be entirely excluded. Second, the absence of patient health outcome data prevents assessing whether the observed service substitution has meaningful implications for patient recovery or well-being. Future research incorporating health outcome measures and employing multi-site designs with control hospitals would further validate causal inferences and provide a more comprehensive understanding of the effects of payment reforms.
Conclusion
This study examines the impact of the DIP payment reform on medical expenditure structure using data from a Chinese integrative medicine hospital. The results show that following the reform, conventional medicine expenses per admission decreased significantly, while traditional medicine expenses increased markedly, indicating a service substitution effect. This substitution was more pronounced among patients with higher payment capacity, pediatric patients, and those with mild to moderate conditions. No significant changes were observed for patients with severe conditions, suggesting a clinical boundary to the reform’s impact. These findings suggest that while the DIP reform effectively contains conventional medicine costs, it may unintentionally shift demand toward traditional medicine, highlighting the need for integrated regulatory oversight across treatment systems.
Supplemental Material
sj-docx-1-inq-10.1177_00469580261436361 – Supplemental material for Healthcare Provision Shifts Under DIP Reform: From Conventional Medicine to Traditional Medicine
Supplemental material, sj-docx-1-inq-10.1177_00469580261436361 for Healthcare Provision Shifts Under DIP Reform: From Conventional Medicine to Traditional Medicine by Xiaoqing Pan, Zhiming Dai, Yanqiu Xiao, Chuang Ma, Deli Wang and Jing Wu in INQUIRY: The Journal of Health Care Organization, Provision, and Financing
Footnotes
Acknowledgements
We would like to thank the reviewers for providing professional comments on the manuscript.
Author Contributions
XP and JW conceptualized the study and wrote the original draft; XP, CM and DW developed the methodology, performed software and data curation, and conducted validation; JW carried out the formal analysis and investigation; XQ and DW provided resources and visualization support. The project was supervised by DW and CM, and administered by XQ, CM, and DW. All authors reviewed and approved the final manuscript for submission.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Annual Program for Philosophy and Social Sciences Planning of Henan Province (Grant Numbers: 2024CSH015), the Graduate Education Reform Project of Henan Province (Grant Number: 2023SJGLX004Y), the 2023 Annual Hospital Management Innovation Research Project by the Jiangsu Provincial Hospital Association (Grant Number: JSYGY-3-2023-334), National Social Science Foundation of China (Grant Number: 23BGL297), and the Professional Degree Graduate Teaching Case Program of Henan Province (Grant Number: YJS2026AL043).
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data presented in this study are available on request from the corresponding author.