Abstract
Heat acclimation is a critical strategy for preventing heatstroke in military personnel, but traditional heat acclimatization relies on natural environments, unfeasible for military training. This study aimed to establish mobile cabin-type thermal rooms in basic-training troops and evaluate the effects of active and passive heat acclimation training in new soldiers. Mobile cabin-type thermal rooms were constructed in basic-training troops. New soldiers underwent heat tolerance tests, and those identified with poor heat tolerance were randomized into active or passive training groups. Following heat acclimation training, participants were re-evaluated, and physiological responses were compared between groups. A total of 1326 male new soldiers participated in the heat tolerance test; 134 (10.1%) were identified with poor heat tolerance. Among them, 70 were assigned to the active training group and 64 to the passive group. All participants completed training and subsequently passed the heat tolerance test. Both groups showed significant improvements in core physiological and stress indices (P < .05), with no statistical differences between groups (P > .05). However, the rise in core temperature and heart rate occurred faster in the passive group, while a higher proportion of soldiers reported comfort in the active group (P < .05). Mobile cabin-type thermal rooms provide a reliable, rapid method for screening and training heat tolerance in basic-training troops. Both active and passive heat acclimation improved heat tolerance, but active training offered better subjective comfort. This approach enables safe and effective preparation for military personnel in hot environments.
Introduction
Humid and hot environment can make human adapt to the heat through certain regulatory mechanisms, and these regulatory mechanisms can be divided into heat acclimatization and heat acclimation just according to whether they are persistent or transient. 1 Heat acclimatization refers to the physiological phenomenon that people who have lived and/or worked in warm-to-hot environments tolerate heat better than those with novel heat exposure. 2 Heat acclimatization has the characteristics of being persistent in life, while heat acclimation is only gradually established under repeated heat stimulation. 3 Therefore the most important method of improving heat tolerance safely under thermal conditions should be inducing heat acclimation in short time. Meanwhile, heat acclimation has become the most important method for military personnel to prevent heatstroke, which is often the most severe condition of heat-related emergencies with a high risk of death. 4 Traditional training methods of heat acclimation depend on strict natural environment, such as temperature of 35ºC to 40ºC, relative humidity of 20% to 60%, as well as a training cycle of 10 to 14 days, otherwise the training effect will be poorly discounted when the above conditions of natural environment are not be obtained. 5 Although there are some proposals of regulating the temperature of micro-environment through clothing, it’s often very difficult to achieve satisfactory training effect in natural environment due to the complexity of climate and the poor safety in actual operation. 6 When military troops are urgently deployed to hot and humid areas, or there is sudden rise in natural temperature, heat acclimation training often cannot be completed in natural environment because of frequent changes of weather. Therefore, it is necessary to establish a training method of heat acclimation that depend on no whether or natural environment.
In recent years, thermal rooms as innovative devices for simulating natural thermal environments have shown significant values and potential in heat acclimation training. The thermal room is not limited by fixed facilities, seasonal climates, and other outer factors, and provides a stable platform for accurate evaluation of any training. In this study, we established mobile cabin-type thermal rooms in basic-training troops of company or platoon units for detection of new soldiers with poor heat tolerance, who were subjected to the following training of heat acclimation in the same thermal rooms to improve their ability of heat tolerance. Here we reported our experience and evaluated the effect of active and passive training methods of heat acclimation.
Participants and Methods
Participants
From January 1, 2025 to February 28, 2025, new male soldiers who were enlisted at the end of 2024 in a tropical region of South China were enrolled in this study. This study was designed as establishing thermal rooms for heat tolerance test which was evaluated by strict monitoring of physiological indicators and subjective feeling, and those who could not pass the test would undertake heat acclimation training in thermal rooms before reevaluated by heat tolerance test. All participants had been well informed of the details of this study, as well as any potential risk in heat tolerance test and heat acclimation training. Each participant made the final choice and signed informed consent. This prospective study was in compliance with the Declaration of Helsinki (Fortaleza, Brazil, October 2013) and approved by the Ethics Committee of Chinese PLA Air Force Medical Center (2020-H3-P101, and the ethic review number AF-07.08/03.2). Those who refused to sign the informed consent form, as well as those who had cold, fever, diarrhea, fatigue, or insomnia in recent 1 week, had all been excluded from this study.
Structure and Composition of the Mobile Thermal Cabin
Main Structure of the Cabin
The cabin was designed as the shape of a standard 40-foot container (12.20 m × 2.44 m × 2.90 m) made of welded steel pipes which was convenient for transportation by trailer towing. The side walls, top plates, and bottom plates were made of insulated sandwich panels. The inner and outer layers were stainless steel plates, and the middle layer was filled with insulation material made of ceramic fibers. One large outward-opening door with good sealing and insulation properties was equipped with reliable locking devices. A viewing window made of double-layer hollow insulation glass was set on one side wall for external monitoring. An inlet port and an outlet port were equipped with the ventilation system on the side walls for air exchange at 0.1 to 0.3 m/s during test or training.
Generation of Thermal Environment and the Control System
One oil stove (2500 W) and 4 sets of heating fan (1000 W) with swing function were installed in the cabin to produce a working temperature >50ºC. One set of automatic humidifier (200 W) which could adjust the ambient humidity according to the requirements of tests or training was equipped. The dehumidifying equipment consisted of 3 units of dehumidifier (280 W) which could display and maintain constant humidity in high temperature, and 1 unit of air conditioner with dehumidifying function (1-1.5 horsepower). Because of the typical deviation of uneven distribution of temperature and humidity in trial, a high-power circulating fan (280 W) was installed on roof of the cabin to forcibly drive the air to ensure that the temperature and humidity were more evenly distributed in the cabin. One sensor of WBGT (wet-bulb globe temperature) was installed in the center of the cabin for monitor of the temperature and humidity. The smart control system included: ①the main-control unit, which received sensor signals and controlled start and power output of the heat source, humidifier, and circulating fan according to the preset program; ②human-machine interface, which provided training mode setting, program selection, temperature and humidity curve setting, and timing on/off; ③programmed training mode, which could preset heating or humidification curves, simulating different thermal stress scenarios; ④safety interlock, which provided over-temperature protection, water-shortage protection, and fan-fault protection. Sports equipment consisted of 2 treadmills of commercial grade with the function of adjusting the slope and running speed. High-power input interface equipped with waterproof plug ( 63 A, 380 V) provide power meeting the requirements of high-power appliances.
Personnel Safety Monitoring and Protection System
The cabin floor was treated with anti-slip to prevent slipping when sweating. Internal monitoring cameras were installed in the cabin for real-time observation of the trainee’s condition to ensure safety. Emergency buttons were set inside the cabin, triggering an external alarm and linked control systems. Emergency ventilation system was equipped to ensure that a high-power exhaust fan can be manually or automatically started quickly to discharge hot air in emergencies. Spaces were reserved in the cabin to place the first-aid equipment. The cabin was equipped with fire extinguishers of dry powder or carbon dioxide.
Heat Tolerance Test and Ability Evaluation
Standardized procedures of pre-test included detailed risk disclosure, avoiding using stimulants for 24 h, adequate sleep, fasting for 2 h, and avoiding a large amount of water 30 min before test. All participants wore only underwear, and adequate hydration and electrolyte replenishment were ensured during the test. Sweat rate was calculated as: (weight loss + fluid intake)/time. After the start of standardized heat exposure, the time when the first appearance of a visible drop of sweat on forehead was observed was recorded as the onset moment of sweating. The temperature in the thermal cabin was controlled between 39.8ºC-40.2ºC, and the humidity was controlled between 35% and 45%. 7 The temperature below the knee was controlled <42ºC, and the head temperature was controlled between 38ºC and 40ºC. 8 Before heat tolerance test, blood pressure and heart rate were measured for each participant, and those with abnormalities were not allowed to participate in the test. A 5-lead electrocardiogram (ECG) monitor was used during the test. Electrode plates of ECG were waterproof to prevent them from falling off because of sweating. Exercise intensity during the heat tolerance test was set as the walking speed of 5 km/h, slope of 2°, and walking time of 2 h on the treadmill. During the test, each participant was repeatedly asked if there was any discomfort, including excessive sweating, dizziness, weakness, nausea, mild muscle spasms, and flushing of the skin. Bedford Thermal Comfort Scale was used for perception of comfort level in heat tolerance test. 9 For measuring rectal temperature, a probe was inserted into the rectum 10 to 15 cm from the anus for continuous monitoring of the rectal temperature. Poor heat tolerance was defined as the occurrence of rectal temperature >38.5ºC or heart rate >150 beats/min lasting for more 3 min in the test, and heat intolerance was defined as rectal temperature >39.0ºC, or heart rate >160 beats/min, or severe arrhythmia, as well as accompanied symptoms such as pale complexion, nausea, vomiting, dizziness, or unsteady standing unable to continue the test. 9 The test was terminated immediately once heat intolerance or poor heat tolerance was confirmed. Standardized procedures of post-test included walking slowly for 5 min in cool outdoor setting, vital signs monitoring, and report of any discomfort.
Heat Acclimation Training and Effect Evaluation
The new soldiers who had been considered as poor heat tolerance by the test were randomly divided into active and passive groups for heat acclimation training. Standardized procedures before training included exclusion of chronic diseases, assessment of basic physical fitness, and personnel status control (the same with the preparation before heat tolerance test). The training was fixed at similar time in the afternoon every day, and all trainee wore only underwear during training with adequate fluid ensured. In the active training group, the trainees continued the exercise of heat tolerance test for 2 h each day, just as the same intensity, environmental temperature, and relative humidity. But once the heart rate reached to 150 beats/min or the rectal temperature reached to 39ºC, or the trainees felt any discomfort, the training of this day was immediately terminated. In the passive training group, the relative humidity in the thermal cabin was controlled at 40%, and the environmental temperature started at 40ºC, with 1ºC increased every day until to 45ºC. The trainees exposed to heat sat quietly for 4 h each day in whatever position they felt comfortable. The training of each group lasted for 7 continuous days. After training, they all participated in the heat tolerance test again for effect evaluation. The average heart rate was calculated in each group at an interval of 5 min for 1 h from the beginning of heat tolerance test, and the average core temperature was calculated at an interval of 10 min for 2 h. The rising rates of heart rate and core temperature were calculated as (peak value-test value)/time. Then physiological stress index (PSI) was used for evaluation of heat acclimation training. The calculation of PSI is: PSI = 5 × (TCt−TC0)/(39.5−TC0) + 5 × (HRt−HR0)/(180−HR0), where 39.5 is the highest temperature the population can endure, 180 is the upper limit of heart rate of the population under high load; TC0 and HR0 are the core temperature and heart rate before exercise, while TCt and HRt are the highest core temperature and fastest heart rate during exercise.10,11
Statistical Treatment
The materials were manually collected and recorded, and then the data were uniformly entered into an Excel spreadsheet. The data were analyzed using SPSS 26.0 software. Metric data were expressed as mean ± standard deviation (x ± s), and counting data were expressed as cases (%). Shapiro-Wilk test was used for normality and Levene’s test for homogeneity of variances in continuous data, and then Mann-Whitney U test was used for inter-group comparison. Two-way repeated measures ANOVA was used for pre-post components between 2 groups and Tukey’s test was used for comparison between 2 groups. Huynh-Feldt corrections was used when sphericity was violated. Cohen’s d (for t-tests) and partial eta-squared were used to quantify practical significance, and 95% confidence intervals were reported for means and differences. P < .05 was considered significant.
Results
Results of Heat Tolerance Test in New Soldiers
A total of 1326 new male soldiers (19.6 ± 1.5 years) participated in the heat tolerance test. The average height was 174.4 ± 5.2 cm, the average weight was 66.7 ± 7.4 kg. and the average BMI (Body Mass Index) was 21.4 ± 2.6 kg/m2. During the test, 134 participants (19.5 ± 1.1 years) were detected as poor heat intolerance (10.1%), in them 15 participants (0.85%) were considered as heat intolerance. The average height was 174.9 ± 4.8 cm, the average weight was 67.4 ± 8.2 kg, and the average BMI was 21.8 ± 1.7 kg/m2. There was no difference in the demographic data between the overall new soldiers and the poor heat tolerance (P > .05), shown in Table 1. For safety, the 15 new soldiers of heat intolerance were categorized into the passive training group of heat acclimation, only under heat exposure but without any exercise, and the other 119 participants of poor heat tolerance were categorized into the active and passive training groups of heat acclimation at random. A hierarchical randomization method was used to balance the factors of BMI, basic physical condition, and subjective will of the trainee.
Demographic Data of the Overall and the Poor Heat Tolerance.

BMI = body mass index.
Grouping According to the Type of Heat Acclimation Training
Seventy new soldiers of poor heat tolerance were included in the active training group of heat acclimation, and the other 64 new soldiers were included in the passive training group of heat acclimation. Demographic data was shown in Table 2 (median), and no difference was found between the 2 groups. BMI, and duration of heat exposure in the heat tolerance test were shown in Table 2 (mean), and no difference was found between 2 groups.
Demographic and Physiological Data of New Soldiers Before HA Training.

HA = heat acclimation; BMI = body mass index; bpm = beat/minute; BP = blood pressure.
Evaluation of the Effects of Heat Acclimation Training
All these 134 new soldiers detected as poor heat tolerance could complete the training of heat acclimation as scheduled, and including the 15 new soldiers who were regarded as heat intolerance, they all passed the heat tolerance test after training. The improvement of the core physiological index was obvious after training of heat acclimation in each group (P < .05), but there was no statistical difference between active and passive training groups (P > .05). The difference of PSI before and after HA training in the 2 groups was statistically significant (P < .01), and there was no difference in PSI between the 2 groups whether before or after the training of heat acclimation. Table 3 showed the physiological data of the 2 training groups in heat tolerance test. Because the heat tolerance test before heat acclimation was terminated due to the occurrence of coral temperature >38.5ºC or heat rate >150 beats/ min lasting for more 3 min, only the recorded cut-off value of core temperature and heart rate were used as the maximum for statistical analysis.
Comparison of Physiological Data in Heat Tolerance Test Before and After HA Training.

HA = heat acclimation; bpm = beat/minute, BP = blood pressure; PSI = physiological stress index.
P < .05.
Comparison Between Active and Passive Training of Heat Acclimation
The mean core temperature peaked at minute 60 and then plateaued in the active training group during heat tolerance test, while at minute 50 in the passive training group, and the rising rate of core temperature in passive training group was quicker than the active training group (showed in Table 4 and Figure 1). The average heart rate reached the maximum level at 30-min in the active training group, while at 25-min in the passive training group, and the rising rate in passive training group was quicker than the active training group ( showed in Table 4 and Figure 2). There was no statistical difference in the onset time of sweating during heat tolerance test, as well as the decrease rate of heart rate in the first minute after test, between the 2 training groups (P > .05), but the proportion of participants feeling comfortable in the survey of thermal sensation after test was higher in the active training group (P < .05, showed in Table 3).
Comparison of Heat Tolerance After HA Training.

Note. HA = heat acclimation; bpm = beat/minute.
P < .05.
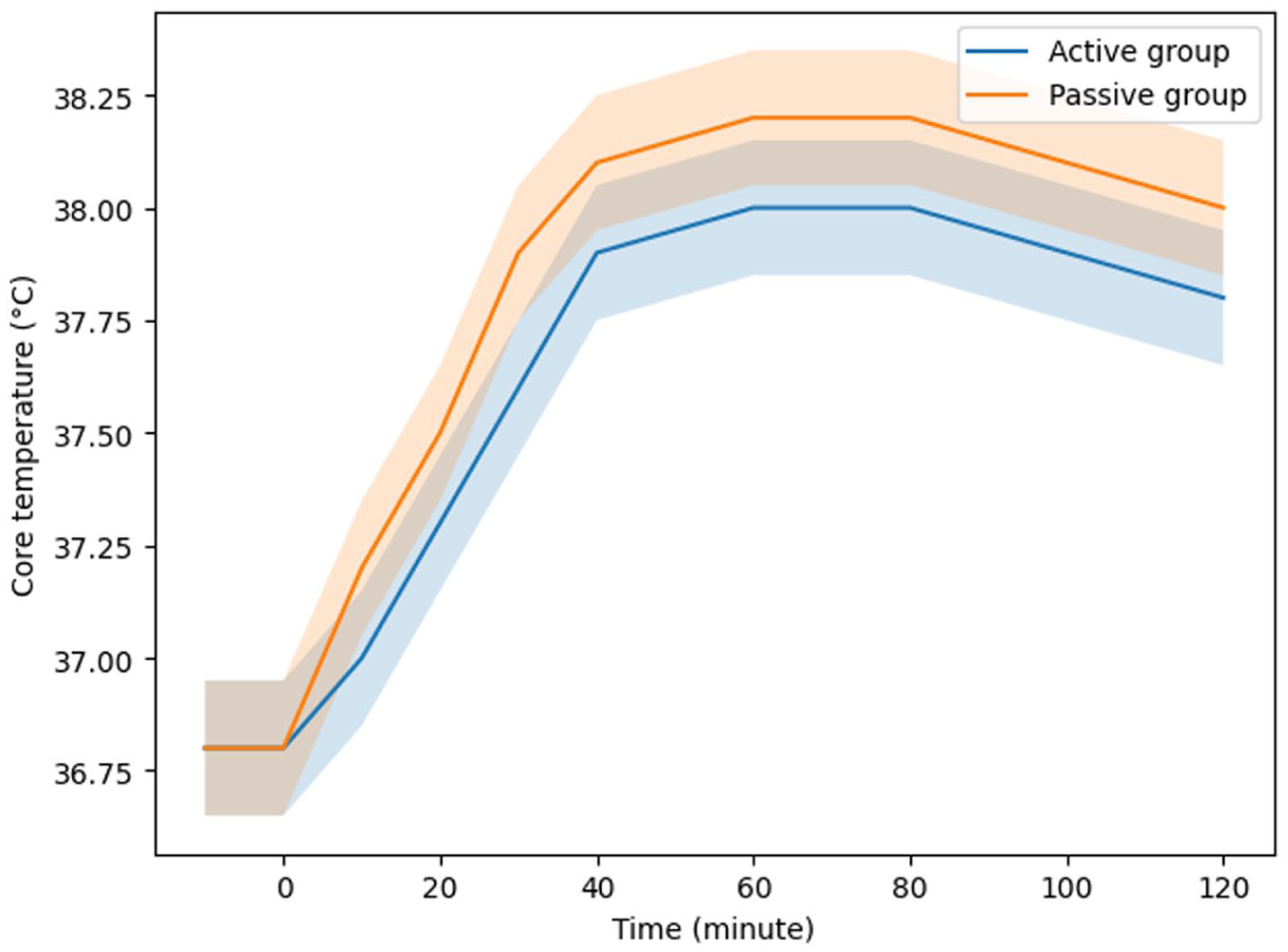
Rising trend of average core temperature in heat tolerance test after heat acclimation training.

Rising trend of average heart rate in heat tolerance test after heat acclimation training.
Discussion
Heat tolerance can be significantly improved by heat acclimation training, one of the most effective methods of preventing heatstroke. 12 Establishment of thermal rooms in basic-training troops and heat acclimation training just reflected the philosophy of preventing heatstroke from passive adaptation to active intervention. 13 Traditional heat acclimatization was a slow and unsystematic progress relying on seasonal heat exposure, and exercise in natural thermal environment was greatly limited by climates, tasks, and venues, leading to heat injuries because of insufficient preparation.5,14 The thermal rooms in this study provided an artificial environment in which the training could be conducted actively at any time and in any place without being externally affected. The thermal rooms could embody the philosophy of achieving scientific and precise heat acclimation training through application of advanced technology. 15 From our experience, the key to heat acclimation training was precise monitoring of physiological indicators based on simulation of thermal environment. We have set parameters such as temperature, humidity, wind speed, and solar radiation intensity in thermal rooms to stimulate thermal environments of different areas, and heat acclimation training could start from moderate conditions, with the load gradually increased abiding by safe and effective extent. During heat acclimation training, the core temperature, heart rate, sweating rate, and other physiological indicators could be monitored in real-time, and this system could automatically evaluate the risk of heatstroke and formulate personalized training intensity, achieving the desired purpose of maximizing training benefits and minimizing the risks. By means of heat acclimation training in thermal rooms in this study, the cycle of 2 to 3 weeks required for heat acclimatization in natural environment could be shortened to only 1 week, with better effects of heat tolerance. When military troops receive urgent orders to go to hot areas, they can quickly form combat power and grasp strategic initiative. Heat acclimation can not only prevent heatstroke but also effectively mitigate the negative impact of heat on cognitive functions, such as attention, judgment, and decision-making ability. 16 This allows military personnel to maintain clear mind and tactical skills in extreme environments, which is crucial for operation of modern high-tech equipment. Compared with the heat acclimation training we reported in this study, previous training methods, such as sauna and hot water bath in many units, had many difficulties in regulating the temperature and humidity precisely with more expensive facilities to meet the strict requirement of the training. In addition, thermal rooms were more convenient for medical staff to monitor the heart rate and core temperature during training or test. The mobile cabin-type designed for the thermal room in this study could resolve those defects in previous heat acclimation training effectively and has the potential of widespread application.
The criteria of heat tolerance test used in this study was cited from Israeli and American standard in military personnel, with the purpose of judging the ability of heat tolerance based on the physiological response of body to hot environment. 17 During heat tolerance test, the walking speed set as 5 km/h under slope of 2° was moderate intensity, producing sufficient heat in the body and ensure safety. The upper limit of exercise duration in heat tolerance test was 2 h, which allowed sufficient time for observing the regulation ability of core temperature. Poor heat tolerance in this study was defined as core temperature >38.5ºC or heart rate >150 beats/min lasting for 3 min. Some studies have suggested that the environmental temperature during heat tolerance test should be increased to 45ºC, and the exercise time shortened to 1.5 h. 18 But from our experience in this study, increasing the environmental temperature to 45ºC accordingly increases the risk of heatstroke during the test, while shortening the exercise time may lead to insufficient heat production and can’t reflect the regulatory ability of core temperature. This study showed that the intensity and duration of exercise in heat tolerance test were suitable for military personnel, and poor heat tolerance of new soldiers was significantly improved after active and passive heat acclimation training, without significant difference in training effects between active and passive training groups, which also supported that this test was accurate and reliable.
Heat acclimation training can be divided into active and passive types. Active training of heat acclimation is to do aerobic exercise under high temperature and humidity for heat acclimation, while passive training only need heat exposure without doing any exercise. 19 Active heat acclimation can lead to enhanced adaptation of cardiovascular system, because exercise demands efficient function of the cardiovascular system itself, and exercise in thermal environment can increase cardiac output and plasma volume, and optimize blood flow distribution in the skin, leading to more pronounced adaptation. 20 Active heat acclimation combines exercise metabolism with heat stress metabolism, thus can improve the regulatory ability of core temperature and sweating efficiency, leading to superior metabolic adaptation. 21 Perhaps the most important advantage of active heat acclimation is that it’s highly correlated with the actual task, resulting in a direct and significant improvement in maintaining the capacity of exercise in thermal environment, and heat tolerance related to exercise tends to decay more slowly. 22 In addition, exercise under hot conditions helps the military trainee to restore psychological resilience, focus, and tactical execution. However, the disadvantages of active training are also obvious. For example, the dual burden of exercise and heat stress may lead to fatigue and longer time for recovery, and exercise increases the rising rate and magnitude of core temperature, with the risk of heat-related diseases significantly increased under extreme environmental conditions when, hydration is insufficient, monitor is inadequate, or the individual is intolerant to heat. 23 This study showed that active and passive training could achieve the same effect of improving heat tolerance significantly, but active training seemed to achieve better results of heat acclimation than passive training, reflected by the slower rising rates of core temperature and heart rate in active training group, and more trainee in the active group feeling comfortable under hot conditions. Considering the low physical exertion under heat stress without large amount of endogenous heat production from muscle activity, passive training can be conducted with relatively low risk, and is suitable for wider individuals with limited capacity, injuries, or unable to safely exercise in the heat. Therefore, passive heat acclimation training should be the first choice for those regarded as heat intolerance, and can serve as a complement or maintenance when active training is impossible or to maintain some adaptations after heat acclimation.
During heat acclimation training, the blood output from heart is mainly distributed to skeletal muscles to ensure exercise performance, and the reduced blood supply to skin correspondingly weakens the capacity of heat dissipation. Heat acclimation training can increase skin blood flow and improve heat dissipation capacity, and then decrease the basal body temperature, increase sensitivity of thermoregulatory center in hypothalamus, and make the set point of temperature move down, thus preventing core temperature from rising rapidly early in thermal environment and reducing heatstroke.24 -26 PSI is a quantitative index of heat stress in the body. In this study, the PSI of those with poor heat tolerance was >5.0, and after heat acclimation training, the heat tolerance was improved and all PSI was <4.0, significantly reduced after training, suggesting that PSI can be used to measure the heat tolerance, and can also be considered for stratification of heat tolerance. In order to avoid heat dissipation obstacles, the trainees should wear only underwear and adequate hydration and electrolyte replenishment should be ensured during the thermal training or test, which was also an important step of standardization .
The establishment of thermal rooms in basic-training troops for heat intolerance test and heat acclimation training is still a new thing in military fields. Current capacity for thermal rooms to evaluate heat tolerance is only limited in new soldiers or military personnel before special tasks. This study consisted of a small number of samples due to the limitation of new soldiers, and analysis of sample size couldn’t be performed because of the prospective nature of this study. Furthermore, meticulous conclusion should be drawn from more rigorous grouping considering the objects’ basic physical condition, history of heat exposure, and psychological condition. Stricter standardization pre-posttest or training, as well as more physiological indicators recorded, should be considered in the following study.
Conclusion
Mobile cabin-type thermal rooms provide a reliable and rapid method for screening and training of those with poor heat tolerance in basic-training troops. Both active and passive heat acclimation could improve heat tolerance, but active training offered better subjective comfort. This approach enables safe and effective preparation for military personnel in hot environments.
Footnotes
Acknowledgements
The authors thank Dr. Lei He of Chinese PLA General Hospital for helpful suggestions on the data collection and statistical analysis.
Ethical Considerations
This prospective study was in compliance with the Declaration of Helsinki (Fortaleza, Brazil, October 2013) and approved by the Ethics Committee of Chinese PLA Air Force Medical Center (2020-H3-P101, and the ethic review number AF-07.08/03.2).
Consent to Participate
All participants had been well informed of the details of this study, as well as any potential risk in heat tolerance test and heat acclimation training. Each participant made the final choice and signed informed consent.
Author Contributions
Liu L performed data collection, analysis, writing the article and critical revision. Kong YL performed research concept and design, writing the article, and critical revision. Xue LH, Wen DQ and Gu Z performed data collection and analysis. Zhang XY and Li N performed data interpretation. Ning B performed research design and data analysis.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
All data included in this study are available upon request by contact with the corresponding author.*
