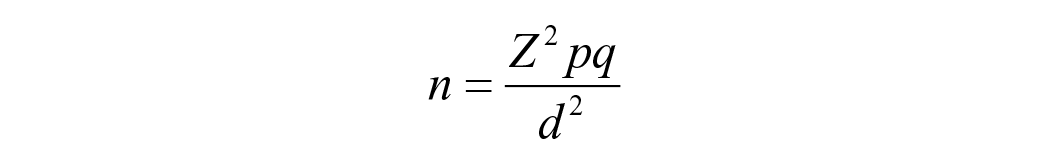Abstract
In 2018, the Ministry of Health and Social Services (MoHSS) introduced acetic acid visual inspection (AAVI) screening program and treatment of cervical precancers with cryotherapy in replacement of Pap smear intervention in Namibia. The study examines the effective use of AAVI-and-cryotherapy treatment on HPV-diagnosed women. Female patients of the reproductive age (20-49 years) group visiting 2 Namibian healthcare facilities for AAVI and cryotherapy treatment were investigated using a cross-sectional approach. The SPSS and coding themes were used to analyze data received through questionnaires and face-to-face interviews from a total of 265 participants. Written informed consent was obtained from participants for treatment and for publication. Among the women that participated in the study, 151 (62%) tested HPV positive, of which 132 (53%) were referred for cryotherapy and 19 (8%) for colposcopy treatments due to Cervical Intraepithelial Neoplasia (CIN I-III) detected. Regardless of the age groups, there was significant evidence of an association between para gravida and HPV positive (χ2(6) = 24.518; P < .001) and HPV negative (χ2(18) = 137.098; P < .001). About 80% of all participants experienced unpleasant pelvic sensations during the examination, with slight abdominal pain during and after the procedure. Ten percent experienced brownish discharges from their pelvis, of which was treated during the cryotherapy treatment. These findings suggest that MoHSS should actively re-evaluate the existing policies to promote AAVI and cryotherapy treatment.
The impact of cervical cancer in women’s health is a global phenomenon. The regular pap tests have limitations, due to the long ques and several visits. Hence overdue cervical cancer screenings jumped from 14% to 23% between 2005 and 2019.
In Namibia, the efficacy of AAVI and cryotherapy screening treatments have not been examined since it was introduced by MoHSS. HIV-positive women screened with AAVI in this study were at higher risk of HPV or chronic Cervical Intraepithelial Neoplasia. Treatment with cryotherapy and colposcopy showed 80% improvement in HPV women.
About 80% of the women experienced unpleasant pelvic sensations during the examination, with slight abdominal pain after the procedure. Outreach strategies need to be set up by MoHSS, in collaboration with health extension workers to prioritize the awareness of AAVI and cryotherapy treatment at free cost to accommodate more population.
Introduction
The human papillomavirus (HPV) is responsible for 90% of cervical cancer occurrences among sexually active women and visual inspection with acetic acid (AAVI) and cryotherapy for detecting cervical cancer is gradually replacing pap smear, especially in low-income countries. 1 With an estimated 530 000 new cases per year, cervical cancer is the third most frequent malignancy among women globally. Cervical cancer affects around 80 000 women in developing countries with limited screening as more than 60 000 women die from the illness. 2 In Namibia, cervical cancer claimed 135 lives in 2018. 3
Pap smear has been the prevalent method for diagnosing cervical dysplasia which uses liquid-based cytology to distinguish between normal and pathological cellularity. 4 However, pap smear is gradually being replaced in Namibia by acetic acid visual inspection (AAVI) and cryotherapy for detecting cervical cancer due to long que that may end up wasting your whole day without being assisted, secondly several visits are requested by the medical doctors before patients are certified free of precancer or not. 5 AAVI and cryotherapy are becoming the preferred treatments for cervical cancer early detection due to simplicity and cost-effectiveness of the procedure that is acceptable to both women and service providers. 6 HPV is the most common viral infection of the reproductive tract that is transmitted through skin-to-skin contacts, such as in sexual contact and open-mouth kissing. There are numerous strains of HPV that affect the vagina, throat, valve, tongue, penis, anus, and cervix. 7 The high prevalence of HPV and its association with cervical cancer makes it important to determine the level of spread in the public. Women between the ages of 18 to 24 years have been reported to be at elevated risk of being infected with HPV.8,9
The AAVI test method does not need more advanced testing conditions as compared to pap smear or cytologic. As per the standard procedure, abnormalities are characterized by examining the cervix without magnification after the use of dilute acetic acid (vinegar). When vinegar is put into abnormal cervical tissue, it momentarily becomes white (aceto-white) for easy and immediate assessment of a positive (abnormal) or negative (normal) result. 10 The AAVI test has been revealed to have a typical sensitivity of 77% and specificity of 86% to detect cervical cancer, however, the use of it is limited in older women or postmenopausal women. 10 Globally, cervical cancer which is the second most common cancer among women develops slowly over a period of 10 to 15 years. 2 Cancer screening uptake continues to be low amongst elderly women in Namibia and South Africa even though there are national guideline recommendations for regular screening to reduce the risk of dying. However, there is a need to advance the availability and affordability of early cervical and breast cancer screening for all women to guarantee successful prevention and control of cervical and breast cancer.11,12 In Namibia AAVI and cryotherapy treatment procedures have been introduced in healthcare facilities in the year 2019. However, no study yet has documented the effectiveness of both AAVI and cryotherapy. Therefore, this study examines the effective application of AAVI and cryotherapy diagnoses on HPV-infected patients attending major healthcare facilities in Namibia. The study focused on the socio-demographic reparations, diagnostic and pathophysiology outcomes, psychological and emotional experiences of AAVI, and cryotherapy procedures.
Methods
SQUIRE Guideline
The study has followed the relevant SQUIRE reporting checklist as guidelines for quality improvement in health care. 13
Study Design, Area, and Data Collection
The study applied a mixed-method cross-sectional design, comprising of quantitative and qualitative techniques using a closed-ended questionnaire as well as face-to-face interviews, respectively. To achieve accurate responds, participants were asked to choose typically one-word answers as “yes/no,” or multiple-choice questions from the questionnaire. Participants were also interviewed one-on-one, giving them the opportunity to explain their answers. The research study was conducted in 2 major healthcare facilities in Namibia for about five (5) months. According to MoHSS, 3 participants (women only) between the ages of 20 to 49 years, especially those previously diagnosed as HIV positive, as well as those with family history of cancer, and those who had epidemiological risk factors are prone to HPV infection, hence were examined on the effective use of AAVI and cryotherapy procedures. Out of all patients visiting these healthcare centers for other regular services, such as HIV care and treatment, Pap smear follow-up, or family planning, 250 patients offered to participate after written informed consent to conduct the research, others declined due to personal reasons. Participants’ social demographics, HIV status, sexual activity, and family history of cancer were determined.
Inclusion and Exclusion Criteria
Female patients between the ages of 20 and 49 diagnosed of HIV positive and negative, who had undergone AAVI and cryotherapy were included in the study. Female patients under the age of 20 and those over the age of 49 were excluded according to MoHSS guidelines.
Sampling Method
The quantitative sample was obtained through Cochran’s formula 14 which is denoted by the following equation:
where: z = 1.96 at 95% confidence level; p (population proportion) = .16; d (margin of error) = .05; q (1-p) = .84. The sample size (n) was calculated as 214, however, to increase the significance probability of research data and findings, the study randomly sampled 250 participants from 2 healthcare facilities. Ten (10) participants were purposively sampled for qualitative analysis as the collected data reached saturation. Data collection was enabled with both closed-ended questionnaires and face-to-face interviews in a conducive environment at the health centers after informed consent. To enhance participant understanding, a local language translator was used. Data collected including demographic information on cervical screening were kept confidential.
Ethics Approval
This study was ethically reviewed and approved by the University (Approval No: Ref: ANM 2020-04). All participants consented before data collection with their participatory decisions being respected. The researcher protected the participants from harm by ensuring anonymity and confidentiality and the collected data was securely stored within lockable locations and a computerized record was secured with a security code.
Data Analysis
The IBM® Statistical Software Package for the Social Sciences (SPSS®) version 25.0 was used to analyze quantitative data presented in tables and figures, while qualitative data was thematically analyzed.
Results
Socio-Demographic Analysis
As per age, 69 (27.6%) of the 250 participants were aged 46 to 50 years, 21 (8.4%) were between the ages of 31 to 35 years and 51 (20%) were of 25 to 30 years as shown in Table 1. About 71.2% of the patients who undertook the AAVI and cryotherapy procedures were in their forties. Most of them 43 (17.2%) were from Havana, an informal settlement in Namibia, 36 (14.4%) from Hakahana, 28 (11.2%) from Khomasdal, 15 (6%) from Greenwell, 34 (13.6%) from Ombili, 15 (6%) from Okahandja park, 23 (9.2%) from Okuryangava, 4 (1.6%) from Rocky crest, 16 (6.4%) from Windhoek west and 36 (14.4%) from Otjomuise (Table 1). According to ethnicity, 20 (8%) participants are Kavango, while 36 (14.4%) are Herero, meanwhile, 188 (75.2%) are Oshiwambo, and 6 (2.4%) are mixed ancestry (Table 1). The study observed that 44.8% of the participants were unemployed, followed by 36.8% self-employed, 6% cleaners, 5.6% nurses, 4% housekeepers, 2% secretaries, and 0.8% doctors respectively (Table 1). The total number of 155 (62%) participants that were single but diagnosed of HPV positive or negative were 100 and 55 respectively. About 95 (38%) of the total married women were HPV 51 positive and 44 HPV negative as shown in Table 1.
Demographic Characteristics of the Participants, Including Age, Place of Residence, Ethnicity, Occupation and Marital Status.

HIV Status Per Age Groups
Figure 1 showed that out of the 250 participants, 111 (44.4%) were HIV negative and 139 (55.4%) HIV positive. According to HIV status per age group, a significant difference (P < .001) was observed between 36 (14.4%) HIV negative versus 15 (6%) HIV positive participants, which were of the 25 to 30 age group. Same significant difference (P < .001) was observed for 21 (8.4%) HIV negative participants between the age group of 31 to 35. However, there was no significant difference (P > .05) in 31 HIV negative versus 30 (12%) HIV positive participants of the 36 to 40 age group. Significant differences (P < .001) were noted among 4 (1.6%) HIV negative versus 65 (26%) HIV positive participants of the 41 to 46 age group, and 19 (7.6%) HIV negative versus 29 (11.6%) HIV positive participant of the 46 to 50 age group, respectively.

Comparison between HIV status per age group. ** and * are significantly different at P < .05, respectively; ns are not significantly different (P > .05).
Sexual Activity and the Use of Contraceptives
All the 250 participants were sexually active in addition to each affirming to have only one sexual partner. The participants were negative for pregnancy when screened before the procedures. Meanwhile, 56 (22.4%) patients were using injection type of family planning, and 29 (11.6%) on implantation, while the remaining 165 (66%) patients were not using any type of contraceptive as shown in Table 2.
Family Planning Procedures.

Para Gravida
Among the participants of the 25 to 30 age group, 2, 17, and 13 women had 3, 2, and 1 child(ren) respectively. Moreover, 19 women did not yet have any children. Moreover, for the 31 to 35 age group, 12, 4, 2, and 7 women had 3, 2, 1, and no child(ren), respectively. Meanwhile of the participants from the 36 to 40 age group, 14, 22, 11, 4, and 9 women had 5, 3, 4, 6, and 2 children, respectively. Among the participants of the 41 to 45 age group, 11, 2, 13, 25, and 12 women had 4, 1, 3, 2, and 0 number of child(ren), respectively. Additionally, between the group of participants aged 46 to 50, 14, 14, 7, 10, and 3 women had 2, 3, 4, 6, and 0 number of child(ren), respectively. From the 250 participants, 617 children were born in total as shown in Figure 2. Regardless of the age groups, 151 women were HPV positive while 99 were HPV negative with a maximum of 6 children given birth to. An association analysis was conducted between para gravida and HPV infection. A Pearson’s Chi-Squared test was conducted to assess whether para gravida and HPV infection status were related. There was significant evidence of an association for para gravida and HPV positive (χ2(6) = 24.518; P < .001) and HPV negative (χ2(18) = 137.098; P < .001).

Number of kids per participant and per age group. Erro bars show significant evidence of an association for para gravida and HPV positive (χ2(6) = 24.518; P < .001) and HPV negative (χ2(18) = 137.098; P < .001).
Family History of Cancer
Figure 3 shows the significant difference (P < .05) of family history of cancer. Forty-three (17.2%) participants acknowledged the presence of cervical cancer, 26 (10.4%) with prostate cancer, while 63 (25.2%) were not sure and 135 (54%) recognized that there was no history of any form of cancer in their families. However, one or combination of more than one of skin, blood, bone, and throat cancer(s) was or were found (P > .05) among participant families.

Family history of cancer. ****; ***, ** and * are significantly different at P < .05, respectively; ns are not significantly different (P > .05).
Diagnostic and Pathophysiology Outcomes of HPV-Infected Patients
Among the 250 patients assessed, 151 were HPV positive and 99 were HPV negative. Of the 250 patients evaluated, 155 (62%) participants were single with 100 (64.51%) recorded to be HPV positive and 55 HPV negative, meanwhile 95 (38%) were married to 51 (53.68%) patients observed to be HPV positive and 44 HPV negative. Out of the 151 tested HPV-positive patients, 132 were referred for cryotherapy and 19 for colposcopy treatments. Table 3 shows the results of 19 patients from both hospitals who went through the colposcopy treatment procedure due to chronic cervicitis and Cervical Intraepithelial Neoplasia (CIN) that were diagnosed based on the biopsy results (Figure 4). Results show that the dysplasia affected one-third of the epithelium, leading to the development of CIN I and CIN II. The most severe kind of CIN detected was CIN III, which affected more than two-thirds of the epithelium.
Colposcopy Results of the 19 Patients From Both Hospitals Who Were Diagnosed of Chronic Cervicitis and Cervical Intraepithelial Neoplasia (CIN).


(A) Biopsy results of the Cervical Intraepithelial Neoplasia (CIN 1-111) diagnosed from HPV patients and (B) Chronic cervicitis inflammation of the cervix.
Psychological and Emotional Experiences
Screening implications
When patients were asked about how they received the information on the new procedure of AAVI, 103 (41.2%) responded that they were referred by medical doctors, 92 (36.8%) were informed by people in the community and 55 (22%) find it out through their routine Pap smear follow up. When participants were asked to give their impression of the pain during and after the procedure, about 80% responded that they did not experience any pain, though they were scared and anxious, with the thought of being embarrassed by the outcome after the procedure. They also mentioned that they experienced unpleasant pelvic sensations during the examination, with slight abdominal pain after the procedure. Another side effect mentioned by 10% was brownish discharge from their pelvis which makes them uncomfortable for about a week thereafter, though was treated during the cryotherapy treatment. Above all, patients gave a negative notion that they reacted emotionally due to a lack of understanding of the examination process and awareness of cervical cancer prevention measures, making them believe that the objective of the screening is to discover cancer rather than prevent cancer.
Discussion
According to MoHSS, Namibia women rarely seek out cervical cancer screening, however, when they visit health facilities for other services, such as HIV care and treatment, family planning, and immunization for children, then they are informed about cervical cancer and are offered the chance to be screened. This study revealed that 178 (71.2%) out of the 250 patients who sought the AAVI and cryotherapy treatments, were between 40 and 50 years of age. This finding is consistent with the study conducted by Malagon et al. 8 and Amukugo et al., 9 thus, indicating that the high risk for developing invasive cervical carcinoma is more common among women aged between 40 and 50 years. However, researchers have argued that HPV can proliferate at any sexually active age group. 10 It was noted that 137 (54.8%) participants that were infected with HPV, hailed from informal and density areas as compared to those in medium to low-density areas. This is in line with a study that reported that women from developing and low-resource countries are unable to afford regular screening for HPV infection. 11 This may be because of a lack of awareness of the health services available, or ignorant of the symptoms, fear of the outcome, and stigma that might be attached to them by friends, hence they miss the opportunities to screen for HPV infection and to be adequately treated for cervical cancer. However, Phaswana-Mafuya and Peltzer 12 also alluded to the fact that in South Africa, residents of informal settlements were less likely to have access to cancer screening than those living in metropolitan regions, hence the affected population might seem low than reality.
Most of the patients who had the procedure done were Oshiwambo and Herero speaking with 75.2% (188) and 14.4% (36) respectively. Women from these tribes seem to be well informed as compared to the other tribes investigated in this study. However, outreach strategies have been set up by MoHSS with several community women groups, expert clients, health extension workers, and clinic in-charges with the aim to actively prioritized cervical cancer screening for free cost at least among 70% of women of reproductive age, rather than passively waiting for women to show up at the health facility for testing. Most of the participants or patients who had the procedure done were either unemployed (44.8%) or self-employed (36.8%). Irrespective of any individual’s occupational or financial status, access to regular cervical cancer screening shouldn’t be only for women who have medical aids, but rather for all.15,16 Of the 250 patients assessed in this study, 155 (62%) were single with 100 (64.51%) HPV-positive single women are more likely to have multiple sexual partners. 17 For example, in the Namibian socio-cultural settings single women do not live with their sexual partners. Thus, favoring situations where some sexual partners are likely to have many other sexual partners thus increases the risk of contracting HPV infection. However, in a study conducted in Turkey, 68% of the women who went for cervical cancer screening were married, 18 compared to 38% observed in this study.
HIV-positive women observed in this study 139 (55.6%) were at higher risk of having AAVI testing positive for HPV or having chronic Cervical Intraepithelial Neoplasia (CIN). Untreated women infected with HIV usually have a strong association with high HPV persistence and a higher risk of cervical precancerous lesions and cancer.19,20 Most women of about 60.4% (151) who are HPV infected in the study have more than 3 children, however, there is no correlation between para gravida and HPV infection among women who participated in the study. Theoretically speaking, the more pregnancy and/or childbirths a woman is exposed to, the higher the risk of being infected with the HPV virus and the greater the chance to develop cervical cancer. 21 A similar study done by Tapera et al., 22 concluded that if a woman gives 3 times vaginal birth, she might have a loose birth canal and tore cervical lining, causing open tissue. Thus, the HPV virus might have a higher possibility to contaminate the opening tissue and cause infection. In this study, 27.6% of the participants confirmed a form of family history of cancer, of which 43 (17.2%) participants acknowledged the presence or history of cervical cancer and 26 (10.4%) of prostate cancer. This is in line with a study that reported that cervical cancer may run in some families. 23 If a mother or a sister had cervical cancer, the chances of a next of kin developing the disease are higher than a woman whose family history did not show any form of malignancy. In other instances, women from the same family as a patient that has cancer could be more likely to have one or more forms of cancer compared to non-genetic cancer risk factors families. 24 In this study, 132 (52.8%) women had cryotherapy while 19 were referred for colposcopy treatment, which uses the visual characterization of the magnified cervix to guide biopsy sampling for histologic diagnosis, allowing high-risk women who require treatment to be distinguished from lower-risk women who do not. About 7.6% had colposcopy which showed results of CIN I-III, where the dysplasia aberrant alterations are present up to one-third to two-thirds of the epithelial layer.
Participants in the study shared their thoughts on their experiences before and after the operation. Though they were nervous before the surgery, but got relieved afterward, believing that being screened would prevent them from acquiring cervical cancer. Evidence suggests that women who are having a pelvic examination may feel anxious due to the unpleasant sensation that might occur before and throughout the examination, and for several weeks afterward. Furthermore, patients’ negative emotional reactions stem mostly from a lack of understanding of anatomy and awareness of cervical cancer prevention measures, leading them to believe that the objective of screening is to discover cancer rather than prevent cancer. 25 Research study has found that HPV infection may lead to serious mental and psychological issues, including stigma, which prevents generally black women in Africa from being screened. 26 Does it mean that HPV testing is more likely to cause mental worry, due to the brownish discharges and abdominal pain experienced after examination? The same side effects were reported by participants in the study done by (Postolica et al. 27 Other side effects also noted include spotting bleeding and pelvic inflammatory. 28 It is therefore recommended that caution should be taken by medical experts when examining the pelvis for HPV, as some pelvis may so fragile than others. Since AAVI and cryotherapy procedures seem to be faster than a pap smear, then the Department of Health Services should organize community-based health education programs about awareness of their use of cervical cancer examination, addressing the negative behavioral misconceptions and fear toward testing, including building women’s confidence to go for screening to know their status.
Limitations
Most women generally were not willing to be examined due to mental and psychological issues, including the stigma of the disease if they are diagnosed positive. Some women who have gone through the test examination, feel uncomfortable to share their experiences of the test with another, especially “researchers.” The notion of been embarrassed during the interview process was a huge limitation, probably due to the reactions they felt during the screening test. Secondly, thoughts of been stigmatized when people get to know of their positive cervical test results, even though it was well explained that results are completely confidential. However, the HPV-positive participants in this study were happily satisfied after the whole procedure was completed and believed God that their healing process will be faster. However, when participants were asked to give their general impression on the AAVI and cryotherapy procedure for cervix examination, they responded that the process was quicker and affordable, and results are out immediately after the screening.
Conclusion
The study investigates the use of AAVI and cryotherapy procedures on HPV-infected patients attending 2 healthcare facilities in Namibia. The 250 women that participated in the study ranged from 25 to 50 years of age. Most of the women that participated in the study mentioned that screening procedures seem simple, affordable, and sensitive compared to the traditional cytology-based strategies. The findings from this study highlight the experiences of women who underwent AAVI and cryotherapy treatments and should be included in the schools/university’s curriculum to address the importance of cervical cancer screening. The important information on cervical cancer screening, including the findings of this study, can be reproduced in booklets, and distributed to patients in hospitals to create awareness on the necessity of the screening and the new technologies available.
Supplemental Material
sj-docx-1-inq-10.1177_00469580241290041 – Supplemental material for Cervical Inspection With AAVI and Cryotherapy on HPV-Diagnosed Women in Windhoek, Namibia
Supplemental material, sj-docx-1-inq-10.1177_00469580241290041 for Cervical Inspection With AAVI and Cryotherapy on HPV-Diagnosed Women in Windhoek, Namibia by Aune Mbadhi, Yapo Guill Aboua, Larai Aku Akai, Beauty Etinosa Omoruyi, Benjamin Ifeoluwa Okeleye and Vincent Ifeanyi Okudoh in INQUIRY: The Journal of Health Care Organization, Provision, and Financing
Footnotes
Acknowledgements
The author(s) thanked the Ministry of Health and Social Services Executive Director for allowing us to perform the research and the nurses and superintendents of the 2 hospitals (Katutura and Central hospitals) for their technical assistance.
Authors’ Contributions
Conceptualization: AM, YGA, LAA; Data curation: AM, YGA, LAA; Formal analysis: AM, YGA, L.A.A, BEO, BIO, VIO; Investigation: AM, YGA; Methodology: YGA, LAA; Software: AM, YGA, LAA, BEO, BIO, VIO; Supervision: YGA, LAA; Validation: YGA, LAA; Visualization: AM, YGA, LAA; Writing-original draft: all authors; Writing-review & editing: all authors. All authors read and approved the final manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval
This study was reviewed and approved by the higher degree committee of the Namibia University of Science and Technology (NUST) higher degree committee, as well as from the Ministry of Health and Social Services (MoHSS) (Approval No: Ref: ANM 2020-04). All participants consented before data collection with their participatory decisions being respected. The researcher protected the participants from harm by ensuring anonymity and confidentiality and the collected data was securely stored within lockable locations and a computerized record was secured with a security code.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.