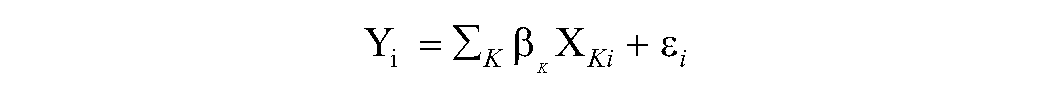Abstract
Numerous studies have explored the relationship between pharmacological treatment regimens and the quality of life (QoL) of type 2 diabetes (T2D) patients. However, there is a dearth of comparative studies focusing on the QoL among rural T2D patients in China across 3 distinct pharmacological treatments: oral antidiabetic drugs (OADs), insulin therapy, and a combination of OADs and insulin. Additionally, the specific correlation between these treatment regimens and distinct dimensions of QoL remains unclear, necessitating further investigation. Data from a survey of rural T2D patients in eastern China were analyzed to calculate QoL scores for different treatment groups. Multivariate linear regression was then used to assess variations in overall QoL and specific dimensions among patients on OADs, insulin, and combined therapy. OADs were most commonly used (70.36%), followed by combined (19.47%) and insulin therapy (10.17%). Patients on OADs reported the highest overall QoL, with reduced physical discomfort, improved psychological well-being, enhanced treatment satisfaction, and fewer medication side effects. Conversely, those on combined therapy had the lowest overall QoL, primarily due to increased physical discomfort. Insulin users had moderately positive overall QoL but lower psychological well-being and treatment satisfaction, along with more adverse reactions. Disparities in QoL and its dimensions exist among rural T2D patients based on treatment regimens. Healthcare providers should prioritize support systems and interventions to help patients manage side effects of insulin and combined therapy, thereby improving their QoL.
Numerous studies have explored the relationship between pharmacological treatment regimens and the quality of life (QoL) of type 2 diabetes (T2D) patients, indicating that different pharmacological treatment regimens may have impacts on the QoL of patients.
Our study underscores the disparities in QoL and its specific dimensions among rural T2D patients using different pharmacological treatment regimens: OADs, insulin therapy, and combined therapy.
Healthcare providers should prioritize the development of support systems or targeted interventions to assist rural T2D patients in effectively managing potential side effects associated with insulin and combined therapy, thereby enhancing their QoL.
Introduction
Diabetes is a metabolic disorder characterized by elevated blood sugar levels due to deficiencies in insulin secretion, insulin action, or both. 1 The escalating global prevalence of diabetes has become a major concern, significantly impacting both morbidity and mortality rates. 2 According to the International Diabetes Federation (IDF) Diabetes Atlas, the global diabetes population was estimated at 537.0 million in 2021, with a projected increase to 783 million by 2045. 3 Type 2 diabetes (T2D) accounts for more than 95% of all diabetes cases. 4 Notably, low and middle-income countries have witnessed a more rapid increase in diabetes prevalence among adults compared to high-income countries. In China, the largest developing nation, the prevalence of diabetes is 12.8%, with projections indicating an increase from 140.9 million in 2021 to 174.4 million in 2045. 5 Furthermore, the number of individuals with prediabetes is on the rise, 6 exacerbating the epidemiological challenge. Although diabetes prevalence is higher in urban areas of China than in rural areas, the risk of mortality is notably more pronounced among rural patients. 7 In recent years, the annual growth rate of diabetes-related deaths among rural residents has significantly surpassed that of urban areas. 8 Consequently, there is an urgent need to intensify efforts on diabetes prevention and treatment, particularly in rural regions of China.
Effective T2D management is crucial for blood glucose control and disease progression. Primary pharmacological treatments include oral antidiabetic drugs (OADs), insulin therapy, or a combination of both. In China, OADs are preferred for their convenience and acceptance. 9 The conventional viewpoint posits that the prescription of insulin follows the inefficacy of OADs in diabetes management. 10 However, substantial evidence now suggests the early inclusion of insulin in the treatment regimen is the superior strategy in diabetes treatment. 11 The importance of early insulin use has been emphasized in a joint statement issued by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). 12 A study in China 13 also noted that patients who used insulin within 2 years of diagnosis had better glycemic control than those who started insulin ≥5 years. Moreover, in recent years, a growing consensus within the clinical practice in China has emphasized the imperative of early intervention with insulin in the management of diabetes.14,15 Combining insulin with OADs offers a more comprehensive approach to blood glucose control, reducing the required insulin dosage and mitigating associated weight gain. 16 This combination treatment potentially enhances glycemic control and customization to individual patient needs, thus improving overall diabetes management. 17 In China, 55.0% of T2D patients receive OADs alone, 18.2% are on a combination of OADs and insulin, 17.5% use insulin monotherapy, and approximately 9% opt for non-pharmacological management.17,18
Quality of life (QoL) for individuals with T2D encompasses various dimensions, including physiological, psychological, and social functioning, all of which are significantly affected by the disease and its treatment. 19 Past studies conducted in different countries report divergent views regarding different medication treatment modalities and QoL among individuals with diabetes. While insulin use has been correlated with reduced QoL, including increased neuropathic pain and psychological distress as noted by Tamir et al, 20 Daher et al, 21 and Reis et al, 22 some studies like those by Dąbrowski et al 23 and Al-Taie et al 24 report no significant QoL differences between insulin and OADs treatments. Additionally, previous research has indicated that sociodemographic characteristics (eg, age, employment status, educational attainment, residence, and household income) can potentially predict the QoL of diabetes patients.25 -28 Factors related to diabetes, such as social support, self-efficacy, self-management, and diabetes-related distress, serve as foundational elements that significantly influence the QoL of individuals with T2D.27,29,30
In China, conflicting findings regarding insulin, OAD treatment, and QoL have also been documented. For instance, You Lu et al 31 found that patients on insulin exhibited the lowest EQ-5D Vas. On the contrary, Fan et al 32 reported that patients receiving insulin therapy showed a significantly higher QoL level than those receiving non-insulin therapy, suggesting a potential for insulin therapy to improve quality of life. Like Fan’s finding, Zhang et al 33 reported that individuals with T2D experienced significantly improved overall QoL after initiating basal insulin therapies. On the other hand, a study conducted in the Shanghai community in 2021 reported that elderly patients with T2D treated with OADs had a higher QoL than those not using OADs. 34 Other factors, including duration since diagnosis, concurrent health conditions, age, and educational attainment, have also been linked with QoL in individuals with T2D. 33
Previous research has explored the connection between insulin, OADs, and QoL, but few have compared QoL across all 3 treatments: OADs, insulin, and combined therapy. In rural China, where living standards and medical care may be lower, the impact of these treatments on specific QoL dimensions among T2D patients remains understudied. This study aimed to assess disparities in overall QoL among patients using OADs, insulin, and combination therapy, and to analyze differences in specific QoL dimensions across these treatment groups. Our findings offer valuable insights into the quality of life of rural diabetic patients under different treatment regimens in China.
Methods
Samples and Data Collection
This study utilized data from a survey on the QoL of rural patients diagnosed with T2D in Binhai County, situated in Jiangsu Province, eastern China. We randomly selected 2 townships, Caiqiao and Zhenghong, from the 11 townships in Binhai County. All T2D were enrolled through cluster sampling from the township health center database. A survey was then conducted using questionnaires distributed on-site by the investigators and family doctors. The inclusion criteria involved rural residential registration, aged 18 years or above, confirmed diagnosis of T2D, and a minimum of 6 months of pharmacological treatment. Exclusion criteria encompassed adults with cognitive impairment and mental disorders affecting communication. The final number of participants in this study was 2193. Eligible participants were referred by physicians. Participants were required to sign consent forms and administered self-reported questionnaires at a private room in the clinic. A total of 2193 questionnaires were completed, of which 2095 datasets were deemed valid, resulting in an effective survey return rate of 95.5%. Self-reported questionnaires including Chinese version scales that had shown acceptable reliability and validity previously were used to measure demographic information, socioeconomic status, diabetes specific psychosocial factors, and QoL. Demographic information involved age, gender, education status, and marital status, while socioeconomic factors comprised annual personal income, medical insurance, employment status, comorbidity, and disability. Diabetes specific psychosocial factors encompassed self-efficacy, social support, self-management, diabetes-related distress, and diabetes-related knowledge.
Variable Selection
Diabetes specific quality of life
The Diabetes Specific Quality of Life Scale (DSQL) was chosen as the measurement tool to evaluate QoL. The DSQL questionnaire comprises 27 items organized into 4 distinct dimensions assessing the impact of diabetes on patients: physiological dimension (12 items), understanding of the physical discomfort caused by diabetes, impact on sensory function, and effects of complications; psychological dimension (8 items): understanding the impact of diabetes on the psychological well-being of patients and their confidence in disease treatment; social relations dimension (4 items): understanding the impact of diabetes on interpersonal relationships, as well as impact on economic, social, and family status; therapeutic dimension (3 items): understanding patient satisfaction with treatment, impact of medication adverse reactions, occurrence of hypoglycemia, and dietary control. The questionnaire responses were graded using a Likert’s 5-point scale, ranging from 1 (none of the time) to 5 (all of the time), yielding a total score range of 27 to 135. The DSQL scores were categorized as “poor QOL (≥80),” “fair QOL (40-79),” and “good QOL (<40),” with higher scores indicating a greater disease impact and lower QoL. The Cronbach’s α of DSQL was 0.95, widely used by researchers globally, demonstrating good reliability, validity, and responsiveness for assessing the QoL of T2D patients. 35
Self-efficacy
The Self-efficacy for Managing Chronic Disease 6-Item Scale (SECD6) gaged patients’ self-efficacy, comprising 2 dimensions: symptom management (4 entries) and disease co-management (2 entries), totaling 6 entries. It employed a scale of 1 to 10, where higher scores denote higher self-efficacy levels. Cronbach’s α was .83. 36
Social support
The Chronic Illness Resource Survey Scale (CIRS) assessed diabetes patients’ resource utilization, reflecting their social support. This study retained 12 items and 3 dimensions: medical staff (HC), family and friends (FF), and community neighborhood (NC). Utilizing a Likert 5-point score ranging from “never” (1 point) to “very much” (5 points), higher scores indicated better utilization of diabetes resources. Cronbach’s α was .91. 37
Self-care behavior
The Scale of Diabetes Self-Care Activities (SDSCA) measured diabetic patients’ self-management behavior, reflecting 6 aspects: ordinary diet, special diet, exercise, blood glucose monitoring, foot care, and medications. Comprising 11 items, including 10 forward questions and 1 reverse question, the scoring ranged from 0 to 7 points, totaling 0 to 77 points. Higher scores signified better self-management behavior. Cronbach’s α was .76 in this study. 36
Diabetes-related distress
The Problem Areas in Diabetes Scale (PAID) evaluated diabetes-related distress through 20 questions on a 5-point Likert scale (0 for “no problem” and 4 for “serious problem”). Total scores indicated the severity of issues, with higher scores suggesting more serious distress. The scale had consistently high internal reliability (Cronbach’s α = .90). 38
Diabetes-related knowledge
The Audit of Diabetes Knowledge (AD-knowl) served as a validated instrument assessing diabetes-related knowledge. Each question offered 3 response options: “correct,” “inaccurate,” and “don’t know.” Correct answers earned 1 point, while incorrect or “don’t know” responses earned no points. This study used a percentage score to evaluate knowledge. The Cronbach’s α was .909. 39
Detailed descriptions of the variables and scales included in the study are presented as Supplemental Table 1 in the Supplemental Files.
Statistical Analysis
Initially, descriptive statistics were employed to analyze participants’ demographic characteristics and variables, presenting the results as frequency and percentage distributions, along with median and standard deviation. Subsequently, the DSQL score was calculated based on different types of pharmacological treatment. One-way analysis of variance (ANOVA) was utilized to compare the differences in DSQL scores among the 3 treatment groups across each dimension. Finally, multiple linear regression models were conducted to assess the association between overall DSQL scores, specific dimensions, and different treatment regimens. Statistical analyses were performed using STATA software (v.17.0; STATA Corp, College Station, TX, USA). The regression model can be represented as follows:
where Yi represents the overall DSQL score or the physiological, psychological, social relations, and therapeutic dimensions of DSQL. Meanwhile, Xk denotes pharmacological treatment regimens and other controlling variables. Additionally, Propensity score matching (PSM) was utilized for a robustness check of the regression analysis, effectively controlling for observable confounders between pharmacological treatment groups. By transforming multidimensional covariates into a propensity score, precise matching of OADs users (control) with insulin (treatment) and combined therapy (treatment) recipients was achieved using 4 established techniques: 1-to-1, 1-to-4 nearest neighbor, radius, and kernel matching. The average treatment effect (ATT) assessed the QoL score disparity, confirming the regression results’ robustness.
Results
Characteristics of T2D Patients
In Table 1, a total of 2095 participants’ data were included in the analysis, of which 1474 (70.36%) were treated with OADs therapy, 213 (10.17%) with insulin therapy, and 408 (19.47%) with combined therapy. In the treatment groups, females (63.70%-62.99%) outnumbered males, with most participants being 65 to 84 years old (64.59%-64.71%), married (82.16%-87.01%), and having an education below the secondary level (91.18%-94.37%). The majority had an annual income under 10 000 yuan (86.76%-91.05%), and no disabilities (91.67%-92.81%). Unemployment was prevalent (61.97%-70.10%), as were comorbidities (61.03%-66.62%). For psychosocial assessments, insulin therapy patients scored lowest in self-efficacy (mean 6.20), social support (mean 3.69), and diabetes-related knowledge (mean 43.44), yet highest in self-management (mean 39.06) and distress (mean 12.85). Combined therapy patients had the highest scores in self-efficacy (mean 6.47), social support (mean 3.74), and diabetes-related knowledge (mean 54.97), contrasting with the OAD group’s lowest scores in self-management (mean 37.41) and distress (mean 11.58).
Description of the sampled rural T2D patients.

Note. OADs = oral antidiabetic drugs; insulin, insulin therapy; Com = combined therapy.
DSQL Scores of T2D Patients With Different Pharmacological Treatment Regimens
Table 2 presents DSQL scores for rural T2D patients, revealing significant variances in overall QoL and its dimensions by treatment regimen, except for social relations. Mean scores for total participants were 48.28 (SD 9.05) for QoL, 24.02 (SD 6.01) for physiological, 14.09 (SD 2.92) for psychological, 5.34 (SD 1.10) for social relations, and 4.82 (SD 1.21) for therapeutic aspects. Insulin therapy yielded the highest overall DSQL score (mean 50.55, SD 10.15), surpassing combined therapy (mean 49.74, SD 9.62) and OADs (mean 47.54, SD 8.62). Notably, insulin patients excelled in physiological (mean 25.38, SD 6.94) and psychological (mean 14.83, SD 2.96) dimensions, whereas combined therapy topped the therapeutic dimension (mean 5.11, SD 1.28). Conversely, OAD patients showed the lowest scores in physiological (mean 23.58, SD 5.73), psychological (mean 13.92, SD 2.84), and therapeutic (mean 4.71, SD 1.14) dimensions. The data indicate that OAD-treated patients report a better QoL across all dimensions compared to insulin and combined therapy patients, with the exception of social relations, which did not differ significantly among the groups.
DSQL Scores for Each Dimension.

Note. OAD = oral antidiabetic drug; insulin, insulin therapy; Com = combined therapy.
Multiple Liner Regressions on the QoL in Rural T2D Patients
Table 3 presents results from a multiple regression model on overall QoL in rural T2D patients. Insulin therapy (coef. = 1.734) and combined therapy (coef. = 1.891) significantly increased the overall DSQL score compared to OADs, indicating that QoL in patients using insulin therapy and combined therapy is lower than in those using OADs. This effect was more pronounced in patients with combined therapy, suggesting that T2D patients using combined therapy have the poorest QoL among the treatment regimens. Regarding demographic factors, the overall DSQL score was significantly higher in women than in men (insulin: coef. 0.930; combined: coef. 1.015). Elderly individuals were significantly associated with a higher overall DSQL score among patients with insulin therapy and combined therapy (insulin: coef. 2.322, 2.765; combined: coef. 2.286, 3.416). In the socioeconomic status, income level showed a negative correlation with the DSQL score for patients with combined therapy (coef. −1.266); employed patients were significantly associated with a higher DSQL score compared to unemployed patients (insulin: coef. 3.110; combined: coef. 3.353). Rural T2D patients with comorbidities (combined: coef. 0.703) or disability (insulin: coef. 4.474, 7.439; combined: coef. 5.364, 7.477) were significantly related to a higher DSQL score. In terms of diabetes specific psychosocial factors, the DSQL score was negatively associated with self-efficacy score, with the greatest effect observed among T2D patients with insulin therapy (coef. −1.686). The DSQL score was positively associated with diabetes-related distress (insulin: coef. 0.436; combined: coef. 0.481) and knowledge (insulin: coef. 0.025; combined: coef. 0.055).
Multiple Regression on Overall QoL in Rural T2D Patients.

Note. OADs = oral antidiabetic drugs; insulin, insulin therapy; Com = combined therapy.
P < .10. **P < .05. ***P < .01.
The Results of Robustness Testing
We compared the ATTs for QoL scores of patients on OADs with those on insulin therapy and combined therapy, across 4 matching methods. The ATTs for OADs versus insulin were 2.517, 2.047, 1.783, and 2.071, and for OADs versus combined therapy were 1.798, 1.374, 1.146, and 1.139. The findings indicate that patients on insulin or combined therapy have a lower QoL compared to those on OADs. The average ATT for the OADs and combined therapy group was 2.105, higher than the 1.364 for the OADs and insulin group, suggesting that combined therapy is associated with the poorest QoL. These results are consistent with the regression analysis in Table 3, confirming the robustness of the findings. For detailed information, please refer to Supplemental Table 2.
Multiple Liner Regression Model on the Specific Dimensions of QoL in Rural T2D Patients
Table 4 presents a regression analysis of the physiological and psychological dimensions of DSQL scores among rural T2D patients. Insulin and combined therapies significantly elevated physiological dimension scores compared to OADs, with coefficients of 1.019 and 1.343, respectively, indicating greater physical discomfort. Psychological dimension scores were also higher for insulin (coef. = 0.322) and combined therapy (coef. = 0.259), suggesting lower psychological well-being, with insulin showing a more pronounced effect. Demographic influences were noted, with women (insulin: coef. = 0.623; combined: coef. = 0.699) and the elderly (insulin: coef. = 2.010 and 2.612; combined: coef. = 1.967 and 2.820) experiencing higher physiological dimension scores, particularly among insulin and combined therapy patients. Socioeconomic factors such as employment status (insulin: coef. = 1.452 and 0.580; combined: coef. = 1.526 and 0.635) and disability level (insulin: coef. = 3.363 and 1.103; combined: coef. = 3.989 and 1.228) correlated with increased scores in both dimensions, highlighting the impact of socioeconomics on QoL. Regarding diabetes specific psychosocial factors, the DSQL score showed a negative association with self-efficacy (insulin: coef. = −1.041 and −0.501; combined: coef. = −0.908 and −0.430) and a positive association with diabetes-related distress (insulin: coef. = 0.187 and 0.213; combined: coef. = 0.213 and 0.228) in both dimensions. Self-management (insulin: coef. = 0.044; combined: coef. = 0.055) was positively linked to the psychological dimension, underlining the importance of psychosocial factors in diabetes treatment outcomes.
Multiple Liner Regressions on Physiological and Psychological Dimensions of QoL in Rural T2D Patients.

Note. OADs = oral antidiabetic drugs; insulin = insulin therapy; Com = combined therapy.
P < .10, **P < .05, ***P < .01.
Table 5 reports the impact of treatment types on the social relations and therapeutic dimensions of DSQL scores in rural T2D patients via multiple regression. Insulin therapy (coef. = 0.314) and combined therapy (coef. = 0.225) notably increased therapeutic dimension scores over OADs, with insulin showing a stronger effect, suggesting reduced therapeutic QoL for these patients. Demographic analysis revealed higher therapeutic dimension scores for women in both insulin (coef. = 0.219) and combined therapy (coef. = 0.229) groups. Socioeconomic status influenced QoL, with employed patients scoring higher in therapeutic (insulin: coef. = 0.179; combined: coef. = 0.253) and social relations (insulin: coef. = 0.898; combined: coef. = 0.939) dimensions. Psychosocial factors related to diabetes showed that therapeutic dimension scores negatively correlated with self-efficacy (insulin: coef. = −0.154; combined: coef. = −0.117) and positively with diabetes-related distress (insulin: coef. = 0.045; combined: coef. = 0.047) and knowledge (insulin: coef. = 0.015; combined: coef. = 0.017). The social relations dimension was negatively linked to diabetes-related distress (insulin: coef. = −0.009; combined: coef. = −0.005) and positively to diabetes knowledge (insulin: coef. = 0.008; combined: coef. = 0.008).
Multiple Liner Regressions on Social Relations and Therapeutic Dimensions of QoL in Rural T2D Patients.

Note. OADs = oral antidiabetic drugs; insulin = insulin therapy; Com = combined therapy.
P < .10, **P < .05, ***P < .01.
Discussion
This study investigated the prevalence of pharmacological treatment regimens for T2D and their association with QoL. The findings revealed that OADs were the predominant treatment modality, utilized by 70.36% of the patient cohort, with combined therapy and insulin therapy accounting for 19.47% and 10.17% of cases, respectively. Patients prescribed OADs exhibited superior overall QoL, characterized by diminished physical distress, enhanced psychological well-being, greater treatment satisfaction, and a lower incidence of medication-related side effects. In contrast, individuals undergoing combined therapy reported the lowest overall QoL, predominantly attributed to heightened physical discomfort. Insulin therapy was associated with a moderate level of overall QoL. The study underscores the importance of considering the impact of various treatment regimens on the multidimensional aspects of QoL in T2D patients, highlighting the need for personalized therapeutic strategies.
The finding of highest overall QoL in patients using OADs is consistent with prior research, 40 whereas those on combined therapy exhibit the lowest. OADs might provide a favorable balance between managing diabetes and minimizing adverse effects, resulting in a relatively better overall QoL. 41 On the other hand, combined therapy, involving multiple medications or approaches, could introduce increased complexities, potential side effects, or added burdens in managing the condition in rural China. Consequently, this might significantly contribute to a comparatively reduced QoL status, potentially even inferior to the QoL experienced under insulin therapy. Nevertheless, the early inclusion of insulin in the treatment regimen is the superior strategy in diabetes treatment according to the existing literatures, 42 which can benefit patients’ glycemic control over a long period of time and delay the occurrence of complications. Therefore, it is recommended that policy efforts focused on establishing support systems, such as counseling services and community resources, be instituted to assist patients, particularly those undergoing combined therapy, in effectively managing potential side effects and treatment intricacies, thereby maximizing the efficacy of insulin or combined therapy.
Considering the physiological dimensions of QoL, our study showed lower QoL for patients on insulin and combined therapy compared with those on OADs. The findings suggest more physical discomfort with injections as against the enhanced convenience of oral medication. 41 The perceived simplicity and convenience of OADs, as opposed to the complexities of insulin or combined therapy, might reduce treatment-induced stress, thereby contributing to heightened confidence in controlling their treatment. 43 Consequently, targeted interventions should be personalized to alleviate physical discomfort in patients undergoing combined therapy, while specific psychological support initiatives need to be designed for individuals receiving insulin therapy to effectively manage their psychological wellbeing. Customized health education can also help manage expectations and improve coping mechanisms during treatment. 44
In the therapeutic dimension of DSQL, patients on OADs showed the highest QoL scores, whereas those on combined therapy had the lowest QoL scores. Insulin yielded less favorable outcomes than OADs, consistent with an existing study. 45 The ease of administering OADs could contribute to heightened treatment satisfaction. 15 Additionally, the compatibility of OADs with patients’ daily routines might facilitate improved treatment adherence, consequently mitigating potential adverse reactions. 24 However, insulin therapy might correlate with a higher occurrence of adverse effects, such as weight gain or fluctuations in blood sugar levels, impacting individuals’ perceptions of treatment satisfaction. 46 Therefore, routine monitoring and scheduled follow-up consultations with healthcare professionals may facilitate early identification and effective management of adverse effects, enhancing the overall patient experience.
Limitations
It is imperative to acknowledge the limitations of this study. The cross-sectional design of our study presents certain inherent limitations, such as the inability to establish temporality and causality and challenges in controlling for confounding variables. 47 Despite these limitations, our study provides a snapshot of the current state of relationship between various treatment regimens and QoL, pending further longitudinal research for a more in-depth understanding. Moreover, the study’s exclusive focus on a specific rural region in eastern China necessitates caution when generalizing the findings to broader populations. Finally, although appropriate measures have been taken, uneven group sizes in this study may affect the interpretability of our findings to some extent.
Conclusions
Our research reveals that among rural patients with T2D, 70.36%, 10.17%, and 19.47% were treated with OADs, insulin therapy, and a combination of both, respectively. The group treated with OADs exhibited the highest QoL, characterized by reduced diabetes-related physical discomfort, enhanced psychological well-being, increased treatment satisfaction, and fewer medication-related adverse effects. In contrast, those on combined therapy reported the lowest QoL, with the most significant physical discomfort due to diabetes. Patients on insulin therapy alone had a moderate QoL, with lower psychological well-being and treatment satisfaction, and a higher incidence of adverse drug reactions. The implications of these findings suggest a need for the development of support systems or individualized interventions aimed at assisting T2D patients in managing the side effects of insulin and combined therapies, thereby improving their QoL. Our study provides significant insights into the diverse impacts of treatment regimens on the QoL of rural diabetic patients in China.
Supplemental Material
sj-docx-1-inq-10.1177_00469580241288683 – Supplemental material for Association Between Pharmacological Treatment Regimens and Quality of Life Among Rural Type 2 Diabetic Patients: A Comparative Analysis in Eastern China
Supplemental material, sj-docx-1-inq-10.1177_00469580241288683 for Association Between Pharmacological Treatment Regimens and Quality of Life Among Rural Type 2 Diabetic Patients: A Comparative Analysis in Eastern China by Sihan Li, Su Zhao, Lizhu Wang, Xian Wu, Zinan Zhang and Zhonghua Wang in INQUIRY: The Journal of Health Care Organization, Provision, and Financing
Footnotes
Acknowledgements
We would like to acknowledge the Chinese National Health Commission and the local Health Commission of Jiangsu province for their cooperation. We would also like to thank all study participants who gave their time for the interviews.
Abbreviations
AD-knowl: Audit of Diabetes Knowledge
CIRS: Chronic Illness Resources Survey
DSQL: Diabetes-specific quality of life
IDF: International Diabetes Federation
OADs: Oral Antidiabetic Drugs
PAID: Problem Areas in Diabetes Scale
QoL: Quality of Life
SECD6: Self-Efficacy for Managing Chronic Disease 6-Item
SDSCA: Summary of Diabetes Self-Care Activities
T2D: Type 2 Diabetes
Authors’ Contributions
SL led the analysis of the data and wrote the first draft of the manuscript. ZW contributed to the study design and interpretation of the data and helped in the writing of the final draft of the manuscript. All authors have read and agreed to the published version of the manuscript.
Availability of Data and Materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by the National Natural Science Foundation of China (no.72374108), the major research project of philosophy and social sciences in colleges and universities in Jiangsu Province (no.2021SJZDA148) . The funding bodies were not involved in the design of the study, or data collection, analysis, and interpretation or in writing the manuscript.
Ethical Approval and Consent to Participate
This study was approved by the Academic Research Ethics Committee of Nanjing Medical University; reference number: 2022460. All procedures were in accordance with the ethical standards of the Helsinki Declaration. Written informed consent was obtained from the individual (s) for the publication of any potentially identifiable images or data included in this article.
Consent for Publish
Not applicable.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.