Abstract
The microclimate between an individual and their support surface can have a significant effect on skin health. Companies have developed mattress systems designed to regulate the temperature and humidity at the individual-support surface interface, utilizing spacer fabric materials and active airflow systems. However, there has been little formal evaluation of their performance. The aim of this study was to evaluate mattress systems using a lab-based approach.
A physical model tank was applied to each support surface, filled with 20 L of water maintained at 37℃. A continuous network of perforated plastic tubing deposited moisture equivalent to a rate of 1.5 mL/min for 25 minutes. Humidity and temperature sensors, stitched onto the thin cotton sheet, monitored the interface conditions for a total of 24 h. Tests were conducted using a range of support surfaces incorporating spacer fabrics, with and without active airflow.
The results from this study revealed that spacer fabric appears to dissipate heat more effectively than viscoelastic foam (Heat flux 33.6 W/m2 vs. 10.4 W/m2). With no active airflow, the viscoelastic foam and spacer fabric exhibited a limited reduction in relative humidity (RH) at the interface. However, with active airflow, the spacer fabric had the ability to reduce RH over time to basal levels through moisture vapor transfer. This represented a change from saturation (99% RH) to ambient humidity (40%) over a 24-h period (water vapor transfer rate = 0.9 g/m2; h).
Further parametric testing is required to evaluate the optimal combinations of spacer fabric material and airflow systems.
Keywords
There are many situations, both in hospital and community settings, where individuals will be supported by interfaces such as cushions or mattresses for prolonged periods. When vulnerable individuals cannot reposition themselves, pressure and shear forces can cause damage to the underlying skin and soft tissues, resulting in chronic wounds termed pressure ulcers (PUs). A PU is defined as a localized injury to skin and/or underlying tissue, usually over a prominence, as a result of pressure or pressure in combination with shear. 1 PUs vary in severity depending on the depth of the lesion; from non-blanching erythema (category 1) to a full thickness wound down to bone (category 4). 1 In spite of efforts to prevent PUs, the incidence rate remains high worldwide, especially in hospitals and nursing homes,2,3 with a mean incidence in the acute care setting of 17.6% (range 1.4–49%) and in the long-stay setting of 6.6% (range 3.1–8.4%). 3 Recent evidence has shown that the cost of treating wounds in the UK is £5 billion, with PUs accounting for 7% of this total.
In addition, thermodynamic conditions within and around skin tissues, commonly termed the microclimate, strongly influence the risk of soft tissue breakdown and the development of pressure PUs. Indeed, it is well established that both heat and moisture decrease the resilience of the epidermis and hence increase its susceptibility to damage at the skin–support interface in load-bearing regions of the body.4–6 Moisture has also been shown to increase the interfacial frictional forces, which can prove damaging to the skin surface. 7 Traditionally, most active support surfaces designed to minimize the risk of PUs have focused on providing pressure relief and/or redistribution, particularly for those individuals with impaired mobility and sensation. However, there has been recent interest among manufacturers in designing mattresses and cushions that regulate the microclimate. A number of manufacturers have introduced novel fabric technologies and active air flow, e.g. Skin IQ™ MCM Technology (Arjo-Huntleigh), at the patient–support surface interface, which are designed to facilitate the transport of moisture away from the loaded body sites. In addition, technological advances in woven manufacturing techniques have given rise to new three-dimensional (3D) spacer fabrics, which can be incorporated as overlays within mattress systems, e.g. AeroSpacer (Medstrom, UK). These spacer fabrics are composed of co-planar knitted structures that are joined together by yarns of known rigidity to provide a well-defined and pressure-tolerant interspace between the different knitted layers. These fabrics are designed to exhibit superior cyclic compression–recovery properties. 8 In addition, due to the highly porous structure and the open apertures in the surfaces, 3D knitted spacer fabrics usually exhibit high air permeability and low thermal resistance. 9
Relatively few studies have reported validated tests to examine the effectiveness of support surfaces in the management of microclimate. Of the few laboratory-based model studies, Nicholson et al. (1999) described a performance test, based on textile industry protocols, to measure the moisture vapor and heat transport capability from the controlled environment into a mattress cover. 10 A microenvironment of controlled humidity and temperature was established above a sample of fabric of a low-air-loss (LAL) cover to simulate the steady state of moisture diffusion through the fabric at physiological conditions. However, this approach did not incorporate patient body weight on the mattress, and hence their findings reflect vapor transmissibility of the mattress cover as opposed to a simulation of its performance in situ. Reger et al. (2001) examined mattress performance by using a water-saturated patient analog resting on a LAL mattress system to provide moisture and energy inputs. The mattress performance was inferred from measurements of the temperature beneath the analog, reflecting the removal of latent energy for up to 90 minutes. 11 However, this approach only offered a qualitative analysis of moisture transport as the measurements are difficult to interpret. Several studies have been performed on automotive support surfaces, using ISO standards for air permeability (ISO9237), 12 measures of transient and steady-state thermophysical properties and water vapor permeability. 13 However, these do not simulate the clinical scenario of a patient lying in bed or sitting in a chair. In addition, the clinical scenario will typically involve bed sheets covering the support surface and garments on patients, which can influence the efficacy of the microclimate management at the skin surface.
Based on transport conservation principles, Figliola 14 developed a reproducible test methodology to measure and control the moisture transported into, through and out of a LAL mattress system. The system incorporated a test rig comprising a load, water bladder and moisture reservoir to simulate the human body at its normal temperature and rates of perspiration. The entire system was incorporated within a controlled environment. The input and output airflow was quantified in terms of temperature, mass flow rate and relative humidity (RH) to provide an accurate indicator of the performance of mattress systems in dissipating heat and moisture. It yielded characteristic temporal profiles of the estimated moisture transport, which described the effectiveness of different support surfaces. 14 It further indicates that temperature and, in particular, moisture can be monitored at the microenvironment interface using airflow techniques. This work provides the motivation for the present study, which was designed to evaluate the relative performance of support surfaces incorporating spacer fabrics with varying airflow parameters on the management of a microclimate at a hot and humid interface.
Materials and methods
A lab-based model was developed, based on a previous description,
14
which enabled an assessment of various support surfaces in terms of their ability to control microclimate. The human analog model involved a medium-density polyethylene tank (surface area 0.3 m2) filled with 20 L of water maintained at 37±1℃. The equivalent pressure under the tank was approximately 20 mmHg (2.7 kPa). At the base of the tank, there was a continuous network of plastic tubing (Tygon® laboratory tubing of outer diameter 3.2 mm and inner diameter 1.6 mm), through which water was pumped via a peristaltic pump (Masterflex C/L, Cole-Parmer, UK). Small holes regularly located along the tubing enabled water release under the tank. This is in contrast to the moisture-bearing patient moisture reservoir, made from a non-woven fabric towel, used by Figliola and colleagues.
14
The tank was placed on a cotton sheet, which itself was placed on the support surface (Figure 1).
Schematic (left) and image (right) of the lab-based model used to monitor microclimate.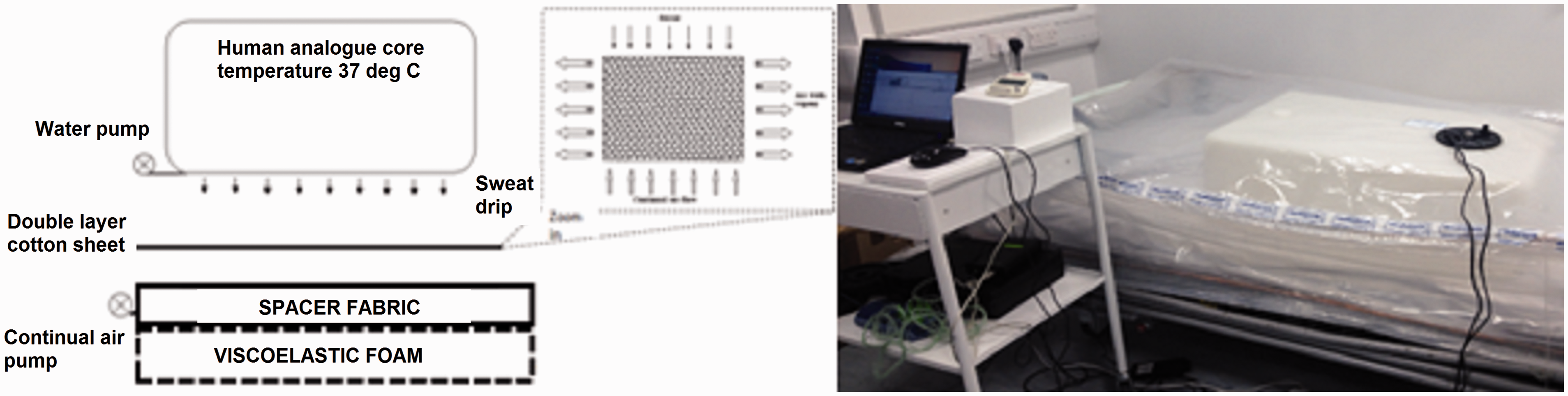
Humidity and temperature sensors, stitched onto a thin cotton sheet, were designed to monitor the interface conditions, acquiring data at 0.5 Hz during and after the simulated sweating phase using a data logger (Model SHT75, Sensiron AG). Two additional sensors were placed away from the analog to monitor ambient conditions. The sensors have an accuracy of ∼ ± 0.5℃ and ±1.8% RH, with their dimensions being 19.5 × 5.08 × 3.1 mm. The complete arrangement was located within a test chamber made of a copper frame surrounded by polyethylene sheeting, with a removable and resealable upper layer of polyethylene creating a sealed environment (Figure 1, right).
Test protocols
The tests, lasting a total of 24 h, utilized a range of support surface combinations, incorporating spacer fabric (Medstrom Ltd, UK), active airflow and ventilated covers (Figure 2). The support surface was comprised of three distinct layers of spacer fabric to create a functional gradient of immersion. Each layer was made of 100% polyester with the following properties:
‐ Layer 1 (superficial); Low Dtex Monofilament with a material density of 25–70 kg.m3, depth 15 mm and weight 500–700 g.m2. ‐ Layer 2 (middle); Medium Dtex Monofilament with a material density of 37–77 kg.m3, depth 20 mm and weight 900–1150 g.m2. ‐ Layer 3 (deep); High Dtex Monofilament with material density of 32–67 kg.m3, depth 20 mm and weight 800–1000 g.m2. Five test combinations of support surfaces incorporating spacer fabrics, with and without active airflow, with a standard viscoelastic foam mattress.
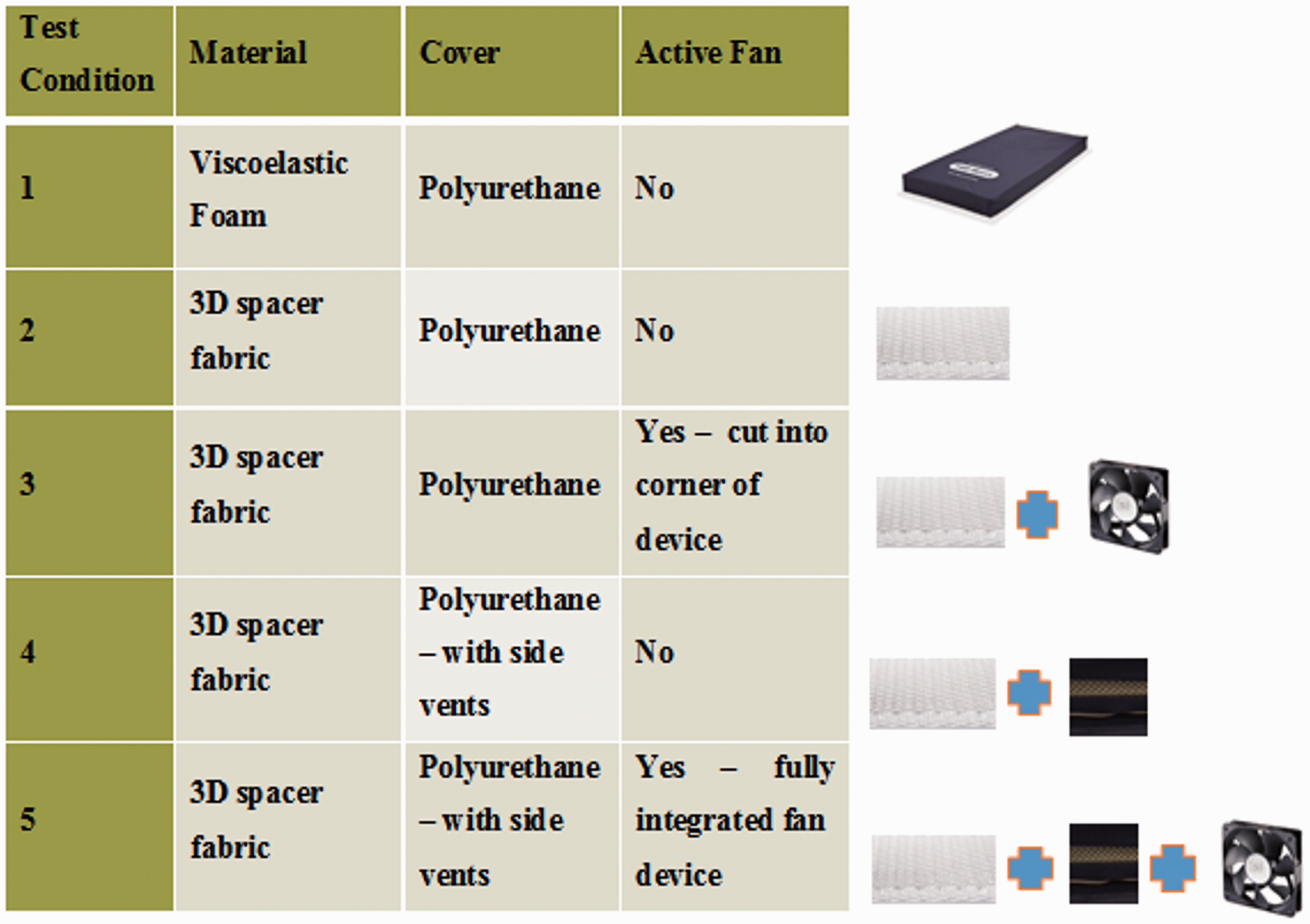
Four separate mattress combinations were examined and compared to a standard viscoelastic foam design. At the start of each test, water was released through the tubing under the tank at rates equivalent to normal physiological sweating of 1.5 or 3.0 mL/min, for a total period of 25 min. These sweat values were chosen to represent the range measured from the collection of human sweat at the sacrum in both loaded and unloaded states. 15 Temperature and humidity data were then recorded for the subsequent period up to 24 h.
Temporal profiles of temperature and humidity were evaluated over the 24-h test period, with specific metrics estimated (Figure 3). The primary outcome measures included: (a) the peak temperature (℃) at the patient–support interface, (b) the peak % RH at the patient–support interface, (c) the overall moisture vapor transfer (MVTR) capability (g/m2.h) of the support surface (i.e. its total evaporative capacity), (d) the heat flux (W/m2) at the patient support interface (i.e. the total heat withdrawal, including dry flux and wet flux) and (e) the area under the curve for the time spent above and below ambient conditions was estimated (Figure 3(c)).
Selected output parameters from temporal profiles of R. (a) Time taken to reach ambient and (b) maximum and minimum temperatures. (c) Estimation of the area above and below the ambient conditions for RH.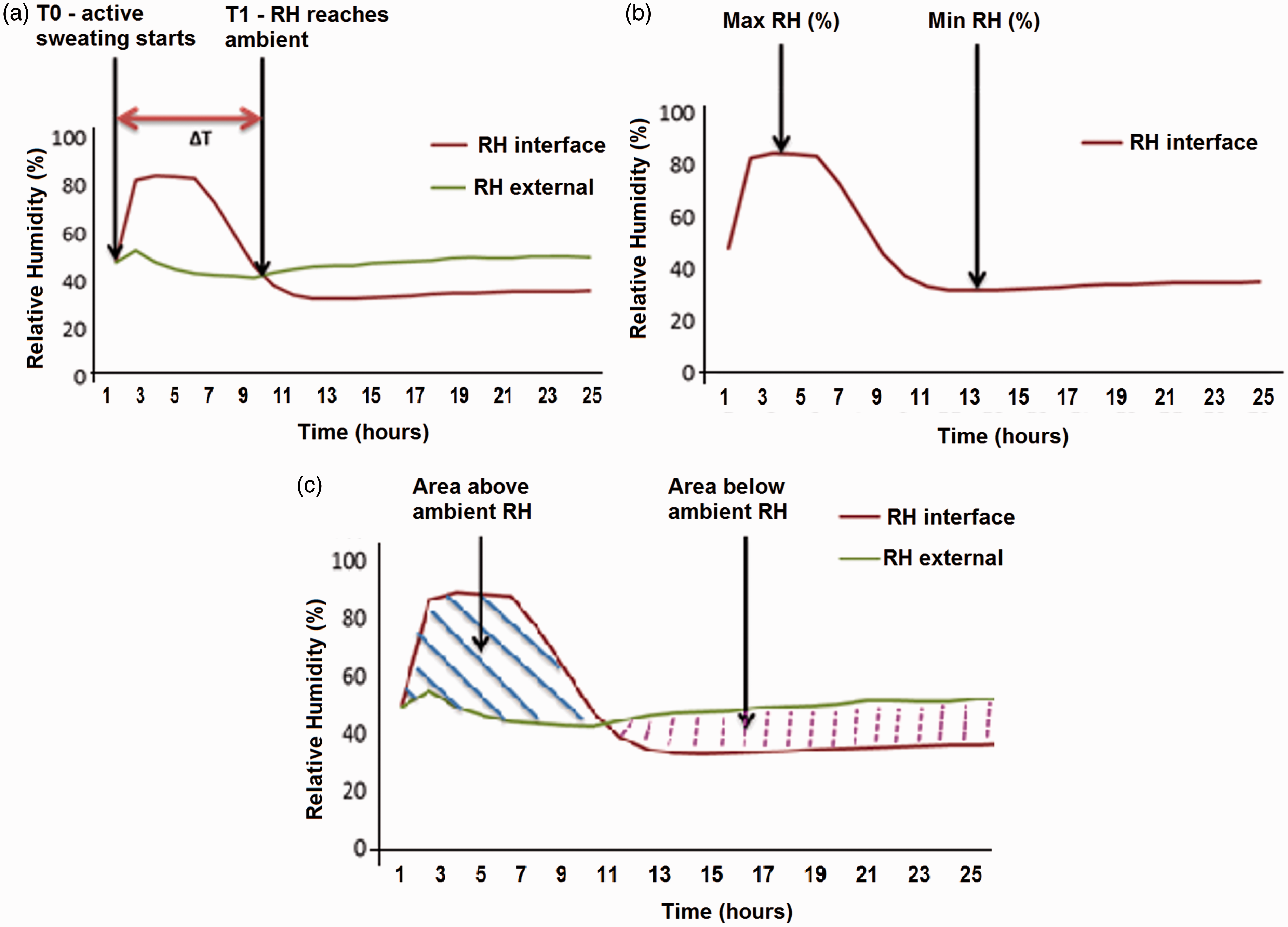
Statistics
Descriptive statistics were used to present the data from the repeat trials. Mean changes in temperature and humidity were estimated for each test condition, and trends were observed between the data sets. Data was analyzed across the test period, with discrete values presented at seven key time points, namely t1 representing baseline values with no phantom and no sweat, t2 and t3 representing 15 and 25 minutes of sweating under the phantom, respectively, and t4, t5, t6 and t7 representing 4, 8, 12 and 24 h post-sweating under the phantom.
Results
Twenty trials comprising four repeats of the five test conditions were completed on the support surfaces.
Temperature
Temporal profiles of temperature from the five test conditions over 24 h (mean ± SD from the three test repeats)
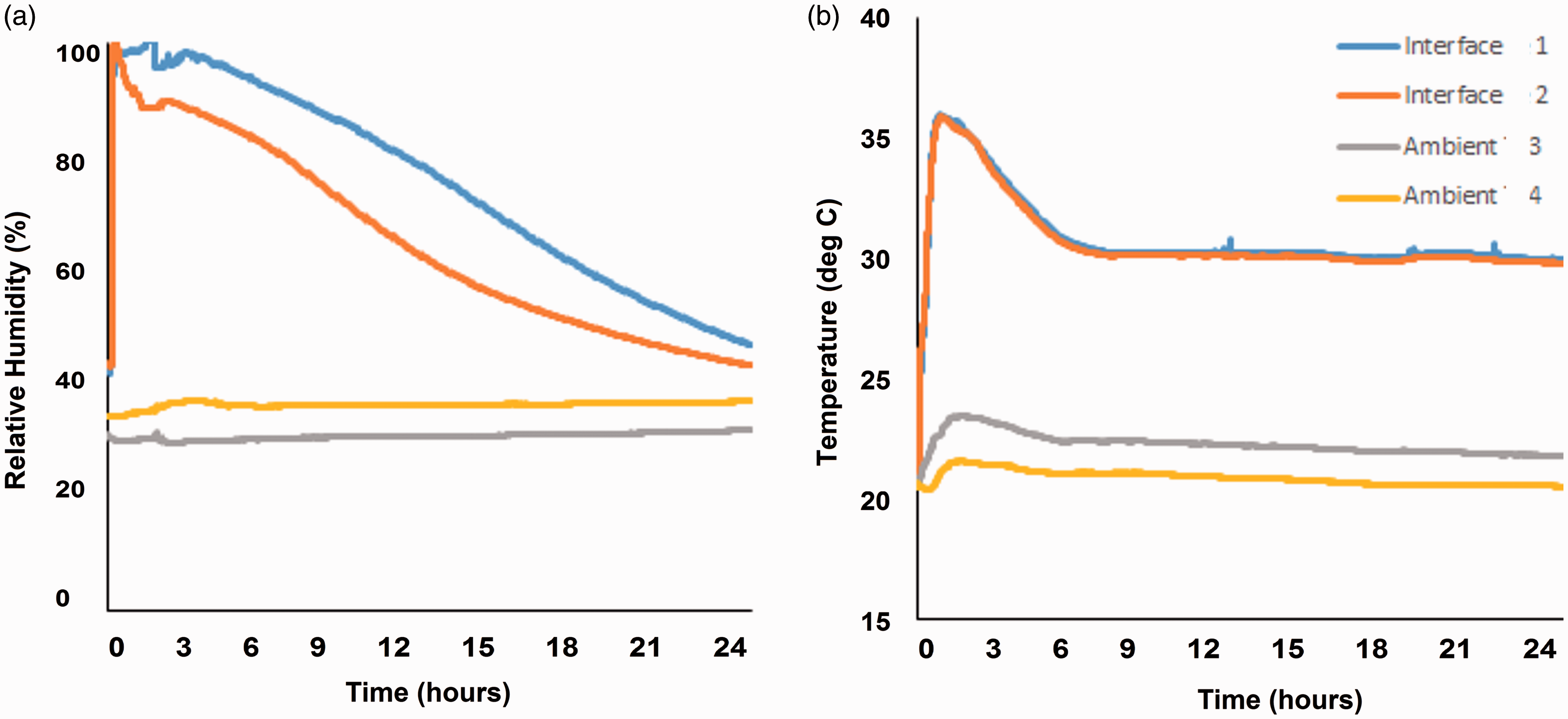
a) Temperature and b) Humidity profiles over the test period for the spacer fabric with active airflow (test condition 2).
Temporal profiles of relative humidity from the five test conditions (see Table 1) over 24 h (mean ± SD from the three test repeats)
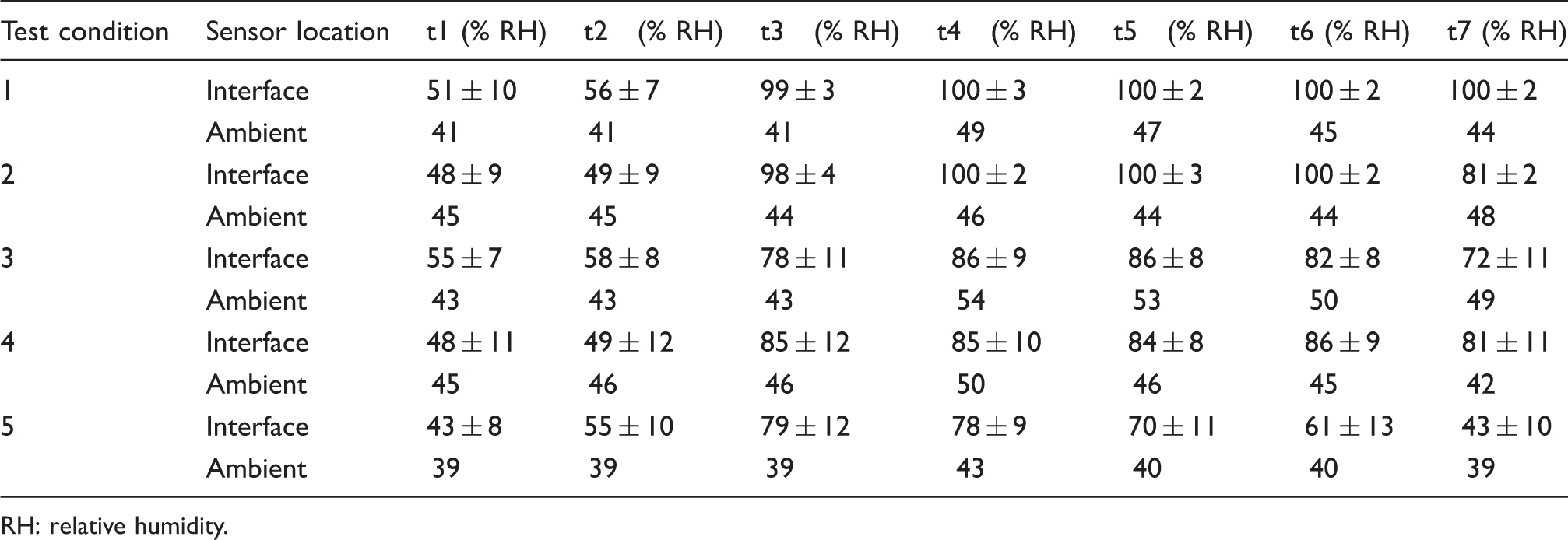
RH: relative humidity.
Humidity
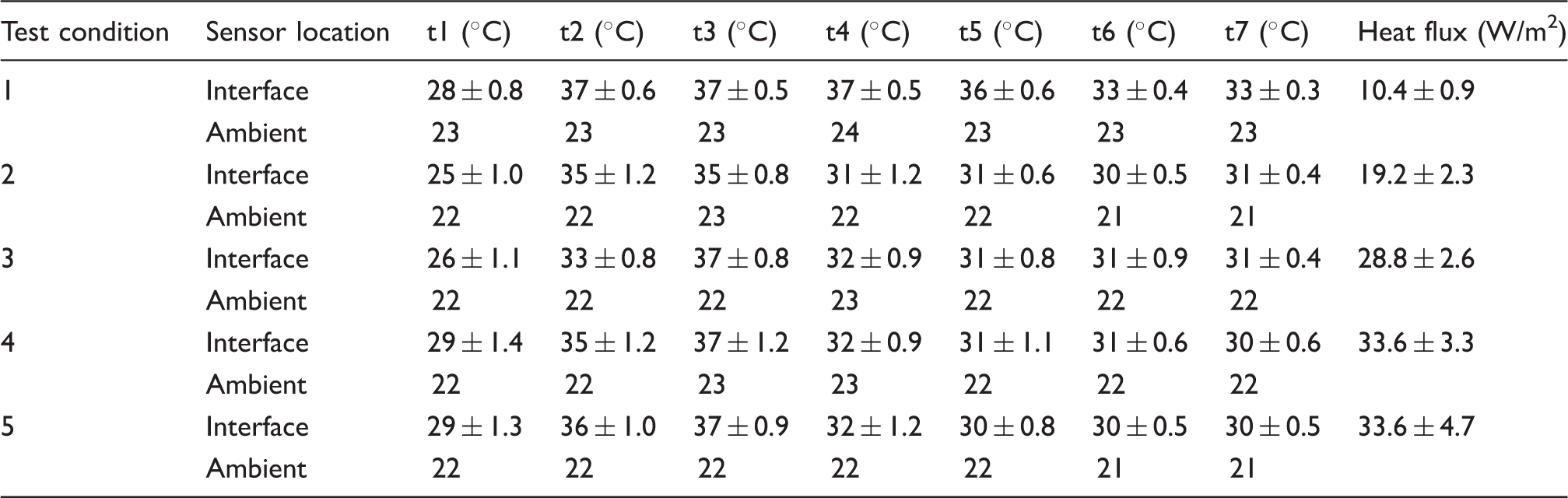
Summary of selected parameters for humidity and temperature from the physical model testing of five test support combinations (average from three repeat tests)
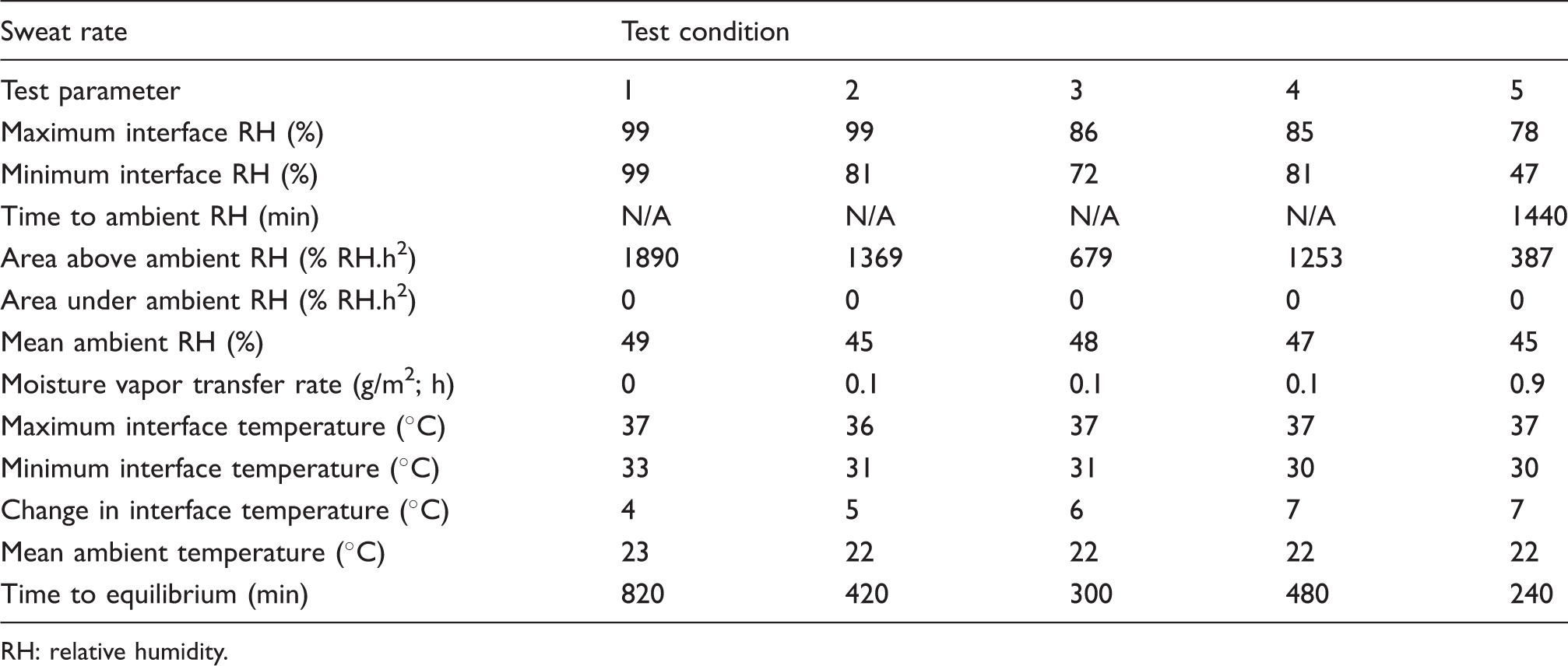
RH: relative humidity.
Figure 5(a) shows a typical temporal profile in RH with test condition 5. It is evident that there is a sharp increase in RH levels following the sweating period, but that these values gradually decline at a constant rate over the 24-h period. This resulted in a MVTR capability of 0.9 g/m2ċh, in the spacer fabric with active air flow. When the mattress was tested with the fan inactive, there was no effect on the RH levels throughout the test period (Figure 5b). As the other test conditions remained saturated at the support surface interface, it can be assumed that MVTR was negligible. In both cases, the ambient RH values remained constant within a range ±5% during the entire test period.
Relative humidity values from the three-dimensional spacer fabric with (a) a blue vented polyurethane cover with an active fan (condition 5) and (b) without a fan (condition 4).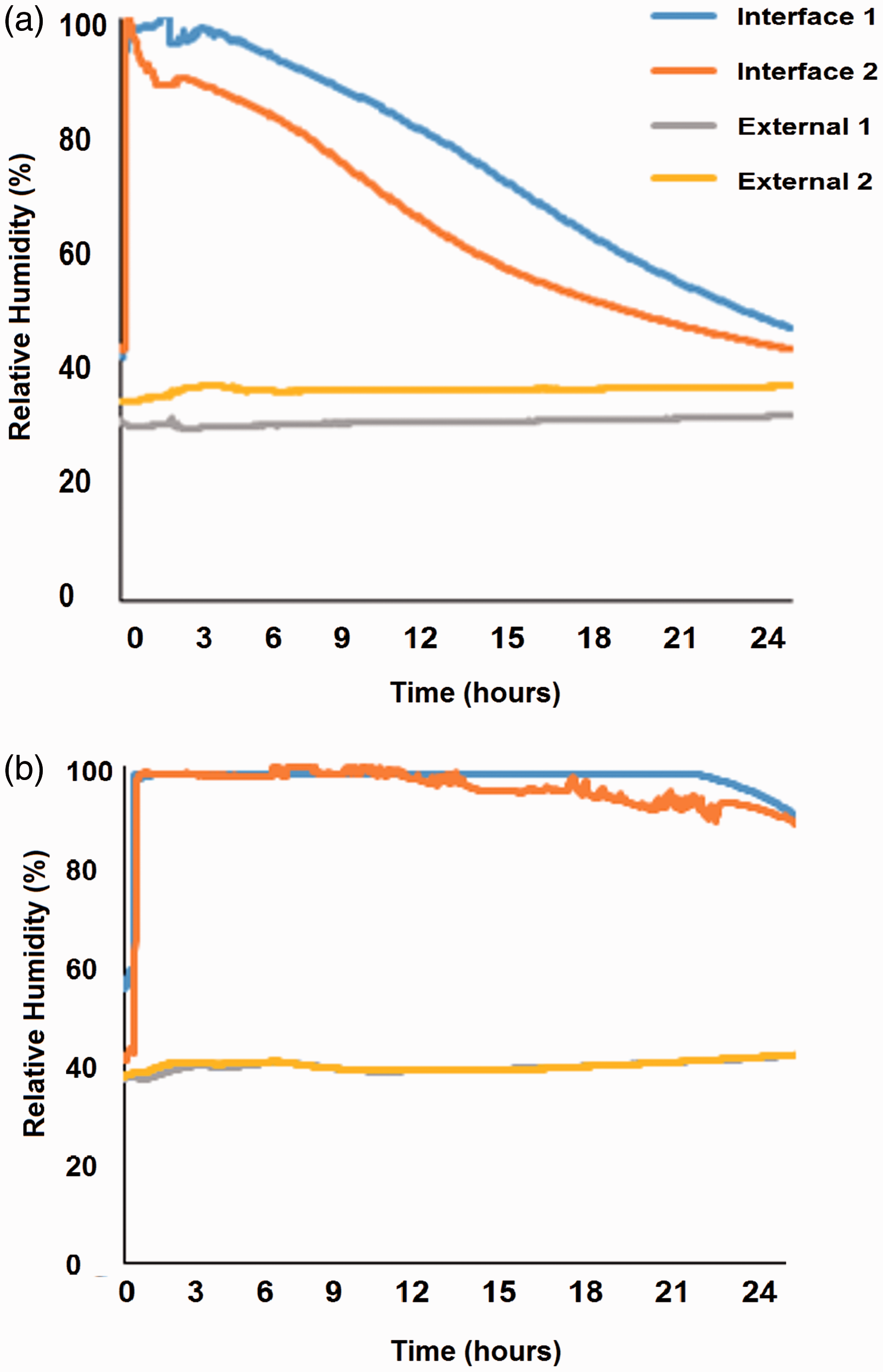
A summary of the output parameters reflecting the microclimate at the model–support interface is indicated in Table 3. It confirms considerable differences between the performances of the test combinations. In particular, the combinations involving active air flow are considerably more effective in controlling the microclimate with, for example, a nine-fold increase in MVTR rate compared with the combinations incorporating the spacer fabric alone.
Discussion
The aims of the study were to evaluate the relative performance of support surfaces incorporating spacer fabrics with varying airflow parameters on the management of microclimate at a hot and humid interface. The design of the human physical analog model proved ideal to deposit moisture uniformly at its interface with the loaded support surface. This resulted in an increase in both temperature and humidity values over the 25-min period of simulated sweating when compared with ambient conditions. The addition of a 3D knitted spacer fabric produced a significant effect on moisture transfer at the interface when an active fan pumped air through the material. This effect was not observed when the fan was inactive.
Using the current methodology, further work can be carried out to investigate, for example, the performance of different covers on different foams, gels and spacer fabric mattresses or cushions, and to determine the effects of bed clothing. A parametric evaluation of interface material porosity under load and varying airflow distributions would add significant value to our understanding of microclimate management systems. The present methodology provides opportunities over previous systems 10 in that it can be adapted to provide varying interface conditions (temperature and pressure), as well as sweating rates, over a realistic surface area. However, it is noteworthy that the physical model is limited in terms of the static nature of the assessment. Research has shown that postural changes significantly affect the microclimate at the patient–support surface interface, 16 with lateral lying postures used to relieve vulnerable skin sites such as the sacrum. The physical model distributed moisture in a pattern associated with the orientation of the perforated Tygon tubing. Thus, sweat was deposited in the corner closest to the moisture inlet and then dispersed across the area of the physical model over time. Further technical developments to employ even dispersion over the simulated sweating period would improve the assessment of support surface performance.
The temperature changes over the 24-h period resulted in a heat flux of 10.4 W/m2 for the viscoelastic foam, compared to a heat flux ranging between 19 and 34 W/m2 for the spacer fabrics. These flux values are comparable to previous studies investigating the conductive heat exchange with a gel-coated circulating water mattress, 17 hospital contract mattresses and other microclimate management systems. 10 A previous study revealed that spacer fabric in mattresses generated a thermally comfortable fabric that regulated human body temperature during sleep. The study also revealed that fabric design, fabric tightness and fiber composition were found to be significant on almost all thermal behavior apart from thermal diffusion. 18 The combination of spacer fabric, vented cover and active airflow was able to produce the wicking-away of moisture over the 24-h test period, resulting in a water vapor transfer rate of 0.9 g/m2.h. Although the initial results of reducing humidity appear to be beneficial to skin health, some caution must be noted to avoid excessive drying. Indeed, excessive dryness of the skin also causes challenges for tissue integrity. Dry skin presents with reduced lipid levels, water content, tensile strength, flexibility and junctional integrity between the dermis and the epidermis. 19 However, the values observed in the present study showed that RH reduced to 40% RH, suggesting adequate moisture to maintain skin health.
It is important that advances in support surface construction for PU prevention and management improve thermodynamic and moisture-dissipating properties without limiting pressure-reducing properties. Indeed, the mechanical properties of support surfaces can be altered by heat and moisture. The present study has shown the thermal and moisture transport benefits of 3D spacer fabrics, particularly when air is forced through the 3D matrix. Spacer fabrics offer superior cyclic compression–recovery properties, 8 delamination resistance and fracture toughness characteristics, offering advantages in support surface design compared to traditional materials. The spacer fabrics can also be tailored in terms of fabric orientation and density. 20 The present study used a new support surface with no prior conditioning, which may have influenced the efficacy of its microclimate control. Further longitudinal studies are required to assess the pressure redistribution qualities of spacer fabrics, with simulated mechanical loading to investigate wear characteristics.
In order to support the maintenance of the microclimate, it is important to regularly reposition immobile patients to allow cooling and moisture dissipation from the body/support interface, 16 especially when there is excessive heat and sweat production. More research is needed to optimize support surface design to effectively manage both pressure redistribution and microclimate. Standardized test methods, such as the physical model described in the present study, will provide the means to provide relative performance statistics on support surfaces. This information will need to be translated into a clinically relevant and user-friendly decision tool for clinicians and managers to use during procurement processes. The present study did have some limitations, for example we only assessed the spacer fabric within a mattress. In clinical practice, there are many situations where an individual can be sat in a leisure chair or hospital chair in excess of 8 h, 21 making the interface with the buttocks highly vulnerable. In addition, we limited the test to standard viscoelastic foam and spacer fabrics; future testing should consider a wide range of material properties for support surfaces including foams, gels and spacer fabrics, in addition to the material properties of covers to distinguish the related performance of designs. Future research employing computational modeling techniques could also offer significant insight into the design of support surfaces with respect to microclimate management. 22 Although the deviation in microclimate values within test conditions was low (Tables 1 and 2), further formal evaluation of repeatability would allow for confidence intervals to be estimated. The validity of the test protocol was provided through the standardized use of representative temperatures, interface pressures and sweat rates delivered through the physical model to simulate a sweating patient scenario. 15
Conclusion
This paper reports a modification of a laboratory method used for the simultaneous measurement of the heat- and water vapor-dissipating properties of hospital mattress systems. The results revealed that foam mattresses with standard polyurethane covers have limited capacity to remove heat and moisture away from a loaded interface. The addition of spacer fabrics without active airflow provided limited benefits regarding MVTR. However, with the addition of active airflow, dissipation of heat and MVTR were observed. This was revealed by temporal changes in microclimate conditions at the support–surface interface over a 24-h period. Further parametric studies are required to establish optimal composites of support surface materials with active airflow technologies to maintain the microclimate adjacent to the skin and promote tissue health.
Footnotes
Acknowledgements
Support surfaces were provided by Medstrom Healthcare Ltd. The work was supported by the Engineering and Physical Sciences Research Council-National Institute for Health Research ‘Medical Device and Vulnerable Skin Network’ (Grant Numbers EP/M000303/1 and EP/N02723X/1).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The work was supported by the Engineering and Physical Sciences Research Council-National Institute for Health Research ‘Medical Device and Vulnerable Skin Network' (Grant Numbers EP/M000303/1 and EP/ N02723X/1).
