Abstract
Primary solitary extramedullary plasmacytoma is a malignant neoplasm characterized by the monoclonal proliferation of plasma cells outside the bone marrow. The tumor rarely occurs in the sinonasal tract, accounting for about 4% of all non-epithelial sinonasal tumors. Herein, the authors describe a rare case of sinonasal extramedullary plasmacytoma in a 33-year-old man who presented with a 3-month history of progressively increasing nasal mass, causing obstruction. A CT scan showed a soft tissue mass measuring 5*8*3 cm in the right and left nasal cavities, obstructing the nasal airway. The mass extended to the right maxillary sinus. Histopathology and immunohistochemical tests confirmed it to be plasmacytoma. Lymphomas with prominent plasmacytic differentiation and multiple myeloma workups were negative. The patient initially refused treatment. After counseling, the patient consented to undergo surgery and later radiotherapy treatment. At one-year follow-up, the patient is disease-free with no signs of recurrence. Plasmacytomas are either medullary or extramedullary neoplasms. The latter are extremely rare tumors, more commonly presenting in the submucosal tissue of the upper respiratory tract. A mass or swelling causing nasal or pharyngeal symptoms is by far the most common presentation of this entity in the head and neck region. Because these lesions are radiosensitive, radiotherapy is a recommended treatment approach. Further studies are needed to better understand the prognosis and effective treatment regimens.
Introduction
Plasmacytoma is a relatively uncommon malignancy of the plasma cells. 1 Depending on their location and number of lesions, plasmacytomas can be grouped into medullary (if in bone) and extramedullary (tissue other than bone). 2 Plasmacytoma can either be multiple or solitary without evidence of systemic disease; hence, three types are identified: multiple myeloma (MM), solitary bone plasmacytoma (SBP), and extramedullary plasmacytoma (EMP). EMP is a mass-forming lesion of monoclonal plasma cells that occurs outside the bone and bone marrow. 3 By definition, patients with primary EMP do not have evidence of underlying MM. 3 It is estimated that the worldwide incidence of EMP ranges from 0.04 to 3 cases per 100,000 and accounts for only 3% of plasma cell neoplasms and 1% of head and neck tumors. 1
Sinonasal EMP is a rare disease that may present with soft tissue mass, airway obstruction, epistaxis, local pain, proptosis, nasal discharge, regional lymphadenopathy, and cranial nerve palsy. 4 The tumor can attain various sizes and shapes. EMP diagnosis involves physical examination, imaging studies, histopathology, immunohistochemistry, and laboratory blood tests. 5 There is considerable number of published studies in the literature regarding epidemiology, presentations, best management modalities, and prognosis of sinonasal EMP. However, data particularly from sub-Saharan Africa are scanty. 6 Radiotherapy is the treatment of choice, but the optimal dose is uncertain. Combining surgery and radiotherapy has shown the best survival outcomes. Therefore, this case report adds to the body of literature that can later be referred to in building the best treatment guidelines in resource-limited settings. This work has been reported as being in line with the CARE guidelines. 7
Case presentation
In August 2023, a 33-year-old male patient attended the otorhinolaryngology department of the Kilimanjaro Christian Medical Centre in northern Tanzania with a 3-month history of progressive nasal mass. The lesion was associated with spontaneous epistaxis. He had no identifiable allergies, and his past medical history was unremarkable. He had no history of previous surgeries. On local examination, he had a shining mass without a breach in the skin (Figure 1), and it was mildly tender and bleeding easily. Anterior rhinoscopy showed nasal deformity, causing left nasal cavity obstruction. No lymphadenopathy was found, and other systems were essentially normal. His laboratory blood workup test results, including hemoglobin levels, were within the normal limits.
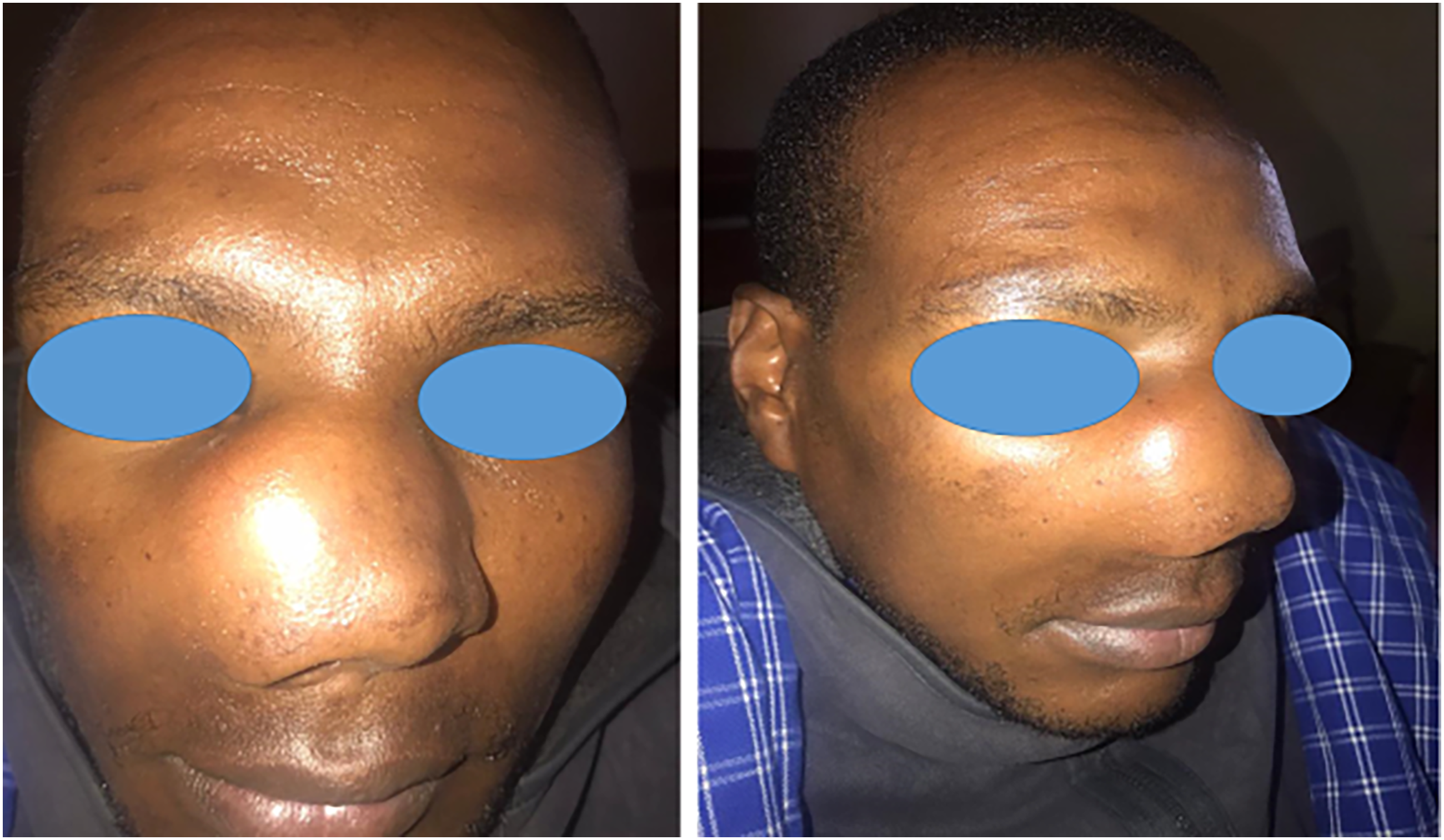
Photographs of the patient prior to surgery highlight the right nasal tumor with intact overlying skin.
Endoscopic examination revealed a pinkish tumor filling predominantly the right nasal cavity with a bloody crust and pseudomembrane on the surface involving the right maxillary sinus and a small amount of sinus fluid. The CT-scan images highlighted a soft tissue mass measuring 5*8*3 cm in both side nasal cavities, obstructing the airway. The mass was extending to the right maxillary sinus and was associated with the destruction of the right turbinates, nasal bone, medial wall of the right maxillary sinus, and nasal septum (Figure 2). A needle core biopsy was collected under local anesthesia. Histopathology of the biopsy demonstrated a diffuse infiltrate of neoplastic plasma cells (Figure 3). The tumor cells expressed strong immunoreactivity with CD38 and CD138 (Figure 4), but were negative with CD19, CD20, and CD45. The impression of plasma cell neoplasm with the differential diagnoses of large cell lymphoma with plasmablastic features, extranodal marginal zonal lymphoma, and MM were considered. Lymphomas and MM diagnostic work-ups that included urinary protein (Bence-Jones protein), serum electrophoresis, bone marrow trephine, and a skeletal survey bone scan were all negative. Thus, the diagnosis of EMP was established. The patient was discussed on the multidisciplinary tumor board, where radiotherapy was recommended. However, the patient initially declined all forms of oncological therapy, including radiotherapy treatment. After thorough counseling, the patient accepted surgery, and the procedure was scheduled after obtaining his informed consent. Later, he underwent radiotherapy for better disease control.

The CT scan images of the patient demonstrate the different views of the soft tissue sinonasal mass obstructing the nasal airway.

Histopathology of the tumor demonstrates diffuse proliferation of large atypical plasma cells that are moderately differentiated; H&E staining at 400× original magnification.

Photomicroscopy highlights strong immunostaining of the tumor cells with CD38 (A), and CD138 (B) antibodies respectively.
Surgical procedure
Under general anesthesia, the tumor was removed using a lateral rhinotomy approach sparing of the medial canthal ligament. The procedure was performed by a team of specialist otolaryngologists. An incision through the skin along the side of the nose and folding the external nose toward the opposite side was made to visualize the operation field and the tumor. The side of the nasal cavity was removed by cutting the bone and soft tissue as needed. A wide local excision was not feasible; thus, the tumor was extirpated in piecemeal from the nasal cavity, maxillary sinus, and ethmoid sinus components [Figures 5A-C]. Hemostasis was achieved by gauze compression, bipolar cautery, nasal irrigation, and nasal packing with vaseline gauze bilaterally. The procedure took three hours. The resected tumor specimen (Figure 5D) was submitted for histopathology. The wound was closed with vicryl 3-0 and prolene 6-0 sutures [Figure 5E]. The patient was hospitalized for 5 days, receiving antibiotics and anti-pain medication. The histopathology results of the resection specimen were similar to those of the previous biopsy. On day 7 postoperatively (Figures 5F-H), the wound sutures were removed, and the patient was discharged. After being counseled again, the patient agreed to undergo local radiotherapy (4400 cGy over a 1-month period) for better disease control. Six monthly control CT scan results are normal. To date, a year has passed since the patient completed oncological care; he remains disease-free without signs of recurrence.

Photographs of the patient taken during the operation (A-C), the resected specimen (D), and the appearance of the patient immediately after surgery (E-F) and after one week of surgery (G-H).
Discussion
EMPs in the sinonasal tract are rare, and most published studies are presented as case reports.8–25 The tumors are four times more common in men and tend to affect the elderly, with the highest incidence of new cases reported in the 6th to 8th decade of life, contrary to our patient, who was in the 4th decade of his life. 9 In the head and neck region, approximately 80% of EMP cases occur within the sinonasal cavity. 10 Sinonasal EMP typically presents as an insidiously space-occupying lesion with nonspecific symptoms, such as soft tissue mass, nasal obstruction, and epistaxis. 11 It can delay diagnosis, as evidenced in our patient. Other clinical features include epistaxis, nasal discharge, pain, and vision loss. 5 The common presentations are soft tissue swelling and nasal obstruction. Other clinical features are epistaxis, nasal discharge, pain, proptosis, and cranial nerve palsies. 12
An EMP diagnosis is essentially a diagnosis of exclusion. It should be confirmed through clinical, radiological, biochemical, and histological investigations. 13 It should be distinguished from non-neoplastic lesions and other malignancies. Histopathological examination reveals atypical plasma cells, with immunohistochemistry showing positive demonstrations for one or the other light chains of the immunoglobulins (κ and λ light chains), as well as a positive demonstration of CD138, CD38, MUM1, and CD79a. The tumor cells are negative for CD19, CD20, CD45, and PAX5.
Sinonasal EMPs are radiosensitive tumors; thus, radiotherapy has traditionally been the mainstay of treatment.6,14,24 Local control rates of 80% to 100% have been reported with moderate-dose radiotherapy, with the optimal radiation dose between 40 and 50 Gy. 15 For small, accessible, and localized EMP lesions, surgical excision may be appropriate, although this is often difficult for tumors originating in the sinonasal tract due to the proximity to vital structures and the risk of poor cosmetic results.6,16 However, with larger EMP lesions, as was the case in our patient, a combination of surgery and radiotherapy is suggested for a greater chance of survival.3,6 In line with our case report, Hu et al., established that sinonasal EMP lesions are sensitive to radiotherapy; surgical resection combined with radiotherapy is a more effective treatment. 13 When clear surgical margins are obtained, the rate of local control with surgery alone is similar to that achieved with radiotherapy alone. A combination of radiotherapy and surgery, as evidenced in our patient, has been reported to reduce the tumor volume and consequently the invasiveness of surgery. 18 Similarly, patients receiving any combination of radiotherapy and surgery had significantly better overall survival than patients who received radiotherapy alone or surgery alone. 19 Chemotherapy is not the first go-to therapy due to significant morbidity. Chemotherapy may be considered in patients with refractory and/or relapsed disease and in cases of progression to MM. 20
Surgical approaches to nasal-sinonasal EMP are determined by factors such as tumor location, size, extent of invasion, histological type, and patient condition.21,22 These approaches aim to achieve complete tumor resection with adequate oncological margins while preserving function and minimizing morbidity. The main surgical approaches are: (1) Endoscopic endonasal approach (EEA). This is preferred in small to medium-sized tumors confined to the sinosal region or with limited extension to the skull base, and particularly with tumors without extensive vascular or neural involvement. Important advantages of the EEA are that it is minimally invasive, an enhanced visualization with high-definition optics, reduced morbidity, a shorter hospitalization, as well as a faster recovery. However, difficulty in managing large tumors or those involving critical structures like the orbit or brain are limitations to the EEA approach. (2) Open approaches: (i) lateral rhinotomy and medial maxillectomy; (ii) craniofacial resection (CFR); (iii) midface degloving; (iv) transfacial and transoral approaches. Each of these has different indications, advantages, and disadvantages. (3) Combined approaches; for example, endoscopic and open approaches combined for better resection and reconstruction. 13 This enables comprehensive management of complex tumors, but it increases the surgical time and complexity of the procedure. 22 EMP has a better prognosis than MM, with 5-year survival rates ranging from 31% to 90%. The conversion rate to MM is lower (11% to 50%), with the highest risk in the first two years. Most patients who developed MM received radiotherapy alone. Follow-up radiological and serum electrophoresis is required after treatment to detect recurrences and progression to MM.23–25
Conclusion
Extramedullary plasmacytoma in the sinonasal tract is rare with nonspecific symptoms and radiologic findings. It should be included in the differential diagnosis of a nasal tract lesion. Awareness of this entity is essential, especially for otorhinolaryngologists, since most of these tumors occur in the head and neck region, and, unlike multiple myeloma, they are treatable with local therapy. Our study supports radiotherapy as a treatment of choice, but radiotherapy in combination with surgery may also be considered. A long-term follow-up is important given the possibility of recurrence or transformation to multiple myeloma.
Footnotes
Acknowledgments
The authors wish to thank the patient for allowing us to use his medical information for academic purposes. We are equally thankful to staff in the departments of ENT, Pathology and Oncology as well as the KCMC hospital management for supporting this study.
Author's contributions
Data availability statement
No data were generated from this study.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics statement
The patient provided written informed consent to allow his de-identified medical information to be used in this publication. A waiver for ethical approval was obtained from the authors’ institution review board (IRB) committee since case reports do not need IRB approval.
Funding
The study was in part funded by the Science for Africa Foundation for the Developing Excellence in Leadership, Training, and Science in Africa (DELTAS Africa) program (Del-22-008) with support from Wellcome Trust and the UK Foreign, Commonwealth, & Development Office, and is part of the EDCPT2 program supported by the European Union.
