Abstract
Health personnel have faced highly adverse circumstances in the workplace since the beginning of the COVID-19 pandemic. Prolonged exposure to stressful situations at work is considered to affect the physical, psychological, and emotional health of these workers, as well as job performance. The objective of this study was to analyze the beliefs, attitudes, and feelings of health personnel from one Spanish region towards their work after five waves of the COVID-19 pandemic. A Cross-sectional descriptive study was carried out using an electronic questionnaire, adapted, and validated through the Delphi technique. A convenience sampling of 783 was recruited among health personnel from the Canary Islands during the fifth wave of the pandemic in September 2021. Bivariate analyzes have been performed by the Chi-square test accepting statistical significance (p 0.050). The 94.3% (n=738) of the respondents considered the pandemic to have highlighted the shortcomings of the Spanish health system. A clear level of exhaustion and/or a reduction in the level of commitment can be observed in these workers as the pandemic continues, as participants reported feeling both mentally and physically exhausted when finishing their shifts, and even “burned out by their work”. This study highlights the resilience and vocation of healthcare professionals, who even considering the effects of the pandemic would choose the same profession. On the other hand, these professionals felt undervalued by their institutions, and almost one of every five, precised psychological support in some point during the health crisis.
Introduction
In the period since SARS-CoV-2 was first detected in China in December 2019, health workers around the world have faced constant uncertainty and adverse circumstances, including a lack of personal protective equipment (PPE), ventilators, ICU beds, and medication, staff shortages, overload due to the collapse of national health systems, and home confinements.1–3 In addition, many health professionals have fallen ill while working, and those with elderly people or underage children in their care have experienced a fear of infection or transmission within their homes, especially when no specific treatments or vaccines were yet available to protect against this emerging disease.4,5
Pre-pandemic research on the attitudes of health professionals during similarly unfavorable hypothetical crisis scenarios showed that health professionals were capable of leaving their jobs to safeguard their own health and their relatives.6–9 However, at the beginning of the first wave of the pandemic in Spain in March 2020, these professionals declared that they had a moral obligation to continue working, treating, and caring for their patients, even if this entailed an additional risk to themselves or their families. 10
Nonetheless, prolonged exposure over time to situations of risk and uncertainty is considered to affect the physical, psychological, and emotional wellbeing of healthcare workers, as well as their performance at work.11,12 In fact, there is a consensus that healthcare professionals are at even greater risk of suffering from high levels of stress, anxiety, depression, burnout, substance abuse, and even post-traumatic stress disorder due to their experiences during the pandemic. 13
After two years of the pandemic, it is thus likely that healthcare professionals are exhausted and/or their attitudes towards work have changed. Therefore, this study aimed to analyze the beliefs, attitudes, and feelings of healthcare personnel from one specific region, the Canary Islands, towards their work after the first five waves of the COVID-19 pandemic, and its relationship with gender, age and professional category.
Material and methods
This was a mixed-methodology descriptive and cross-sectional study. It was structured in two phases.
In the first phase, the Delphi technique was used to update the instrument used previously by the authors in a study during full confinement in the first wave in 2020. 10
After adaptation to the current circumstances, the research team generated a first version of the questionnaire that sought to determine the beliefs, attitudes, and feelings of health personnel towards their work after 5 waves of the SARS-CoV-2 pandemic. This first questionnaire was distributed to a group of health experts working in different health services at various levels, who after 2 rounds agreed on the final instrument, evaluating its internal validity. The adapted questionnaire was made up of 78 items divided into 5 dimensions. Thus, the dimensions of the original questionnaire (previously validated by Damery et al. for an influenza pandemic) were kept, only some questions were reformulated following the recommendations provided by the group of experts. 6
The first dimension was focused on the beliefs of healthcare personnel regarding the pandemic, while the second was related to attitudes surrounding the work performed. The third dimension included questions of a personal nature and the fourth included work-related questions regarding the interviewee, while the final dimension was related to feelings towards work. To determine the reliability of the scale, the Cronbach´s alpha coefficient of the 78 items was obtained, and its total value was α = 0.954. Besides this, if we study the reliability of the dimensions independently, we obtained: Beliefs (α = 0.619), Attitudes (α = 0.940) and Feelings (α = 0.962).
During the second phase, a quantitative methodological approach was applied through a descriptive cross-sectional study involving an electronic questionnaire distributed in the Autonomous Community of the Canary Islands, Spain. The study period was extended from August 31 to September 23, 2021, during the fifth wave of the COVID-19 pandemic in this region.
The questionnaire was digitized in a “Google Forms” format and was pretested by members of the research team to detect misunderstandings. As the instrument was self-administered, a brief explanation of the study was included in the first part, and express consent to participate in the research was requested. The participants were also informed that the questionnaire was anonymous and were thanked for their participation.
To reach the target population, reference workers from hospitals, healthcare centers, and socio-health centers were contacted, and these professionals managed the dissemination of the questionnaire. The target population of the study was made up of health professionals (doctors, medical interns, nurses, nursing interns, physiotherapists, auxiliary nursing care technicians, emergency medical technicians, radiology technicians, and laboratory technicians) from the Canary Islands who had worked during the COVID-19 pandemic at any public or private health institution. The sample size was calculated considering that 22,882 health professionals worked in the Autonomous Community of the Canary Islands. A sample size of 585 participants was required for a confidence level of 95% with a sample error of 4%. 14
Those individuals who did not give their consent to participate in the study were excluded. In addition, participants who did not respond adequately to a control question were eliminated from the sample to avoid the inclusion of automatic responses.
The statistical analysis was performed with the collaboration of the Research Support Unit at the Maternal and Child Insular University Hospital Complex (CHUIMI) of Gran Canaria using the statistical program R Core Team 2020, version 3.6.3. Frequencies and percentages for the qualitative variables were calculated. Bivariate analyzes have been performed by the Chi-square test accepting statistical significance (p ≤ 0.05).
The authors had no conflicts of interest, and the study was self-financed. This study also had the approval of the Research Ethics Committee/Drug Research Ethics Committee at the University Hospital of Gran Canaria Dr Negrín (CEI/CEIm HUGCDN); Code CEIm HUGCDN: 2021-262-1 COVID-19, and complied with the ethical standards required by the Ethics Commission at the Jaume I University of Castellón de la Plana (file number “CD/112/2021”).
Results
The results presented below belong to the second phase of the study.
Sample profile
A total of 820 responses were recorded. Individuals who did not give their consent for the inclusion of their responses in the study (n = 3) and those who did not adequately answer the control question (n = 34) were excluded, leading to a final sample of 783 health professionals, which means a sample error of 3.44% for a confidence level of 95%. Most were women (n = 603; 77%) with a mean age of 42.2 years. Participants most often lived with their partner and children (n = 329; 42%).
In terms of occupational characteristics, most participants were nurses (n = 403; 51.5%) working in hospitals (n = 298; 38.1%) and in the public health sector (n = 676; 86.3%), and tended to be employed under temporary contracts (n = 347; 44.3%). The mean number of years of experience was 15.83 (SD = 10.81) (Table 1).
Personal and occupational characteristics of the sample (n & %).
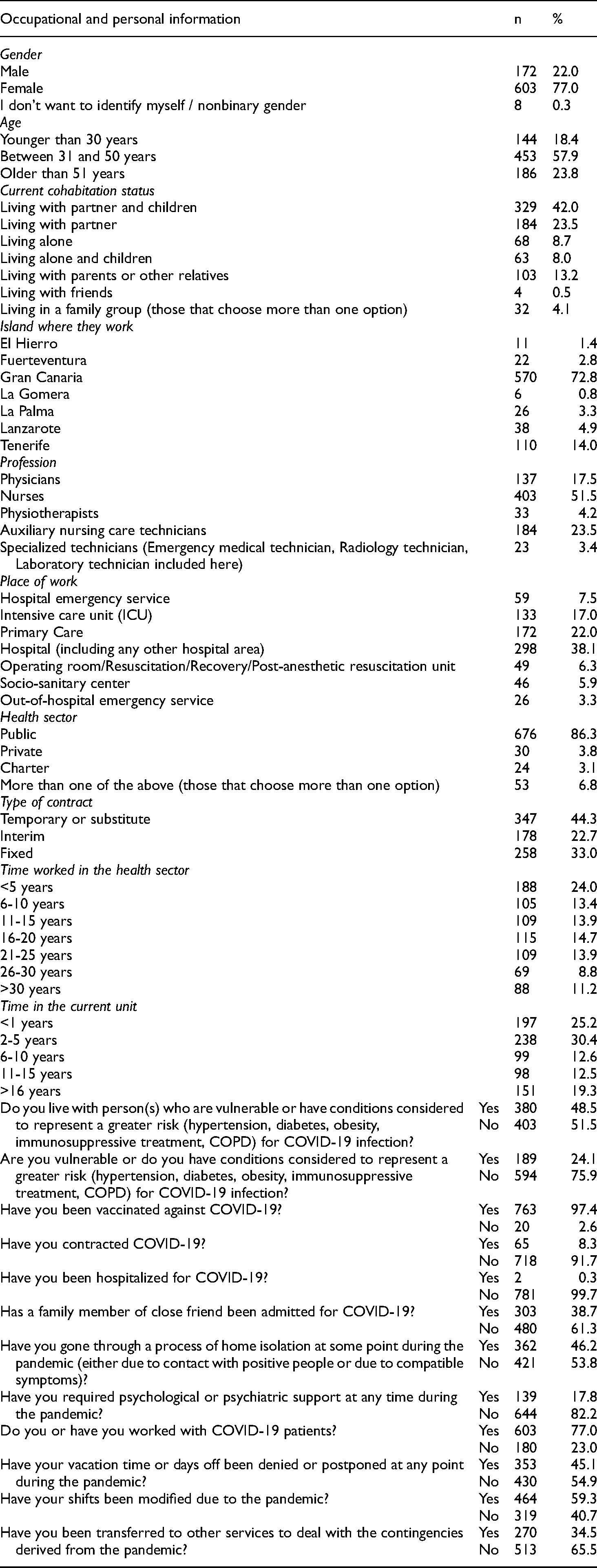

Almost all respondents stated that they had been vaccinated against COVID-19 (n = 763; 97.4%). Overall, 77% (n = 603) were working or had worked with COVID-19 patients, 8.3% (n = 65) had contracted the disease, and 46.2% (n = 362) had been isolated at home after being in contact with people confirmed as positive or because they had symptoms compatible with COVID-19, being the health personnel under 30 years old who worked more with COVID-19 patients (83.3%; p = 0.008) and were also confined in greater proportion (52.9%; p = 0.015).
Compared to other professions, nurses were the most frequently displaced to other services (43.9%; p ≤ 0.001), their work shifts were modified more (65%, p = 0.004) and those who were mostly denied or postponed their vacations or days off (49.9%; p = 0.004).
In addition, 17.8% stated that they had required psychological or psychiatric support at some point during the pandemic (n = 139), being the health personnel under 30 years old who required it the most (21.5%; p = 0.014).
Highlight that health professionals over 51 years of age (44.1%; p ≤ 0.001), male professionals (27.3%; p = 0.018) and auxiliary nursing technicians (34.8%; p ≤ 0.001) were the groups more at risk of COVID-19 infection due to previous pathologies or health conditions. Specialized technicians (65.4%) and auxiliary nursing technicians (58.7%) were the occupational groups where more participants stated to live with people considered vulnerable or at risk of COVID-19 infection due to previous pathologies or health conditions, in comparison for example with physicians (40.9%) (p = 0.004).
Beliefs
In this fifth wave, most respondents considered that they had adequate access to personal protective equipment (PPE) (n = 709; 89.8%). However, many claimed to have lacked this equipment at some point during the pandemic (n = 515; 65.8%) (Table 2).
Beliefs of healthcare personnel from the canary islands after 5 waves of the COVID-19 pandemic.

Regarding vaccines, a large majority considered that all healthcare personnel should be vaccinated against COVID-19 (n = 715; 91.3%). However, less than half (n = 382; 48.8%) believed that current vaccines would help curb the pandemic, male professionals (54.7%; p = 0.013) and the physicians (54.7%; p = 0.016) were the most optimistic.
In terms of health system management, almost all believed that the pandemic had revealed its shortcomings (n = 738; 94.3%), and that its structure should be changed (n = 660; 84.3%). Most of the physicians (64.2%) and the specialized technicians (69.2%) believed that the healthcare system wasn't adequately prepared (p = 0.039).
Respondents expected a “second pandemic of post-traumatic stress” among health personnel due to the experiences during this health crisis (n = 584; 74.6%), and female professionals (76.9%) believed it in a greater proportion in comparison with the males (66.9%; p = 0.008). Participants also believed that if more personnel had been on staff the overload would have been reduced (n = 744, 95%).
Attitudes
In total, 38.3% (n = 300) of health professionals reported being willing to work despite a higher-than-usual risk of work-related infection and contracting COVID-19. On the other hand, 50.4% (n = 395) stated that they would most likely not go to work if there was a greater risk of infecting their relatives, and many would not be willing to work if they had to take on tasks for which they had not been trained (n = 406; 51.9%) (Table 3).
Attitudes of healthcare personnel from the canary islands after 5 waves of the COVID-19 pandemic (I).

However, participants reported that they would be willing to work if they received some type of incentive from the institution (n = 520; 66.4%), this response was especially frequent among the health personnel under 30 years old (85.0%; p ≤ 0.001).
They would even work more hours (n = 413; 52.7%), work on their days off (n = 384; 49%), or work at different hospitals or health centers than usual (n = 435; 55.6%). Despite the fact that it was the female professionals (55.0%; p = 0.016) and the health personnel older than 51 years old (54.7%; p = 0.003) who stated in a greater proportion that they probably would work more hours if they were asked to. The male professionals (60.4%; p = 0.015) and under 30 years old (73.8%; p ≤ 0.001) supported that they probably would work at different hospitals or health centers if needed.
The surveyed professionals stated that they would continue working if their coworkers had been infected (n = 539; 68.8%), and even if a colleague from their team (n = 454; 58.0%) or a family member (n = 406; 51.9%) had died from COVID-19.
Overall, 51.9% (n = 406) agreed that all healthcare workers had a duty to work during the pandemic even though there was a greater risk to their health, the male professionals (65.1%; p ≤ 0.001) and those older than 51 years old (67.2%; p ≤ 0.001) were the most who agreed with this affirmation. On the other hand, 44.8% (n = 351) indicated that those unwilling to do so should be sanctioned, the professionals under 30 years old supported the idea of penalizations less (70.1%; p ≤ 0.001) (Figure 1).
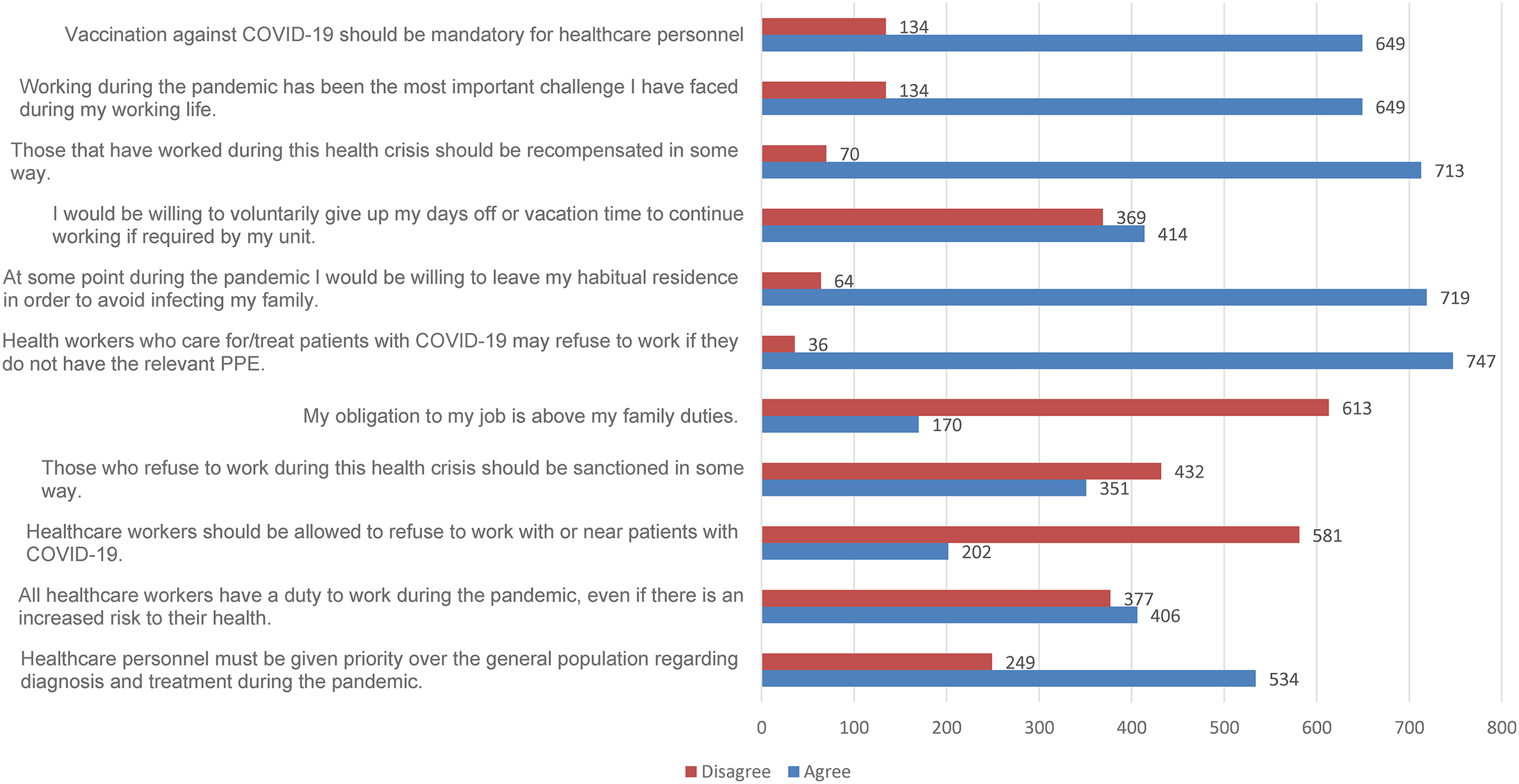
Attitudes of healthcare personnel from the Canary Islands after 5 waves of the COVID-19 pandemic (II).
Most of the participants were even willing to leave their habitual residence to avoid infecting their families (n = 719; 91.8%) and put their duties toward their relatives before their responsibilities at work (n = 613; 78.3%) (Figure 1). Nevertheless, a major proportion of health personnel older than 51 years old put their obligation to their job above their family duties (33.3%; p ≤ 0.001).
The respondents considered this health crisis to be the most important challenge faced during their working lives (n = 649; 82.9%) and stated that they would be willing to voluntarily give up their vacation time or days off to continue working if their unit required it (n = 414; 52.9%). However, it was the health personnel under 30 years old (43.1%; p ≤ 0.001) and physicians (45.3%; p ≤ 0.001) who agreed in a lesser proportion with voluntarily giving up their free time to continue working
Finally, 82.9% considered that vaccination against COVID-19 should be mandatory for health personnel (n = 649). Health personnel older than 51 years old considered a mandatory vaccine the most (91.4%; p ≤ 0.001).
Feelings
In total, 23.4% (n = 183) of healthcare workers stated that their work led them to feel emotionally exhausted on a daily basis, especially the professionals between 31 and 50 years old (26.9%; p ≤ 0.001). In addition, 26.3% (n = 206) felt physically and psychologically exhausted when leaving work and some felt that they lacked the time to finish all their tasks during the workday (n = 136; 17.4%), with some feeling “burned out” by their work (17.8%; n = 139). It should be noted that physicians felt most “burned out” by their current job compared to other professions (21.2%; p = 0.016), and also felt that they didn't have time to perform all their tasks during the working day (31.4%; p < 0.001), as well as professionals older than 51 years (21.0%; p = 0.010).
Health professionals had a daily fear of becoming infected while working (n = 241; 30.8%) but stated that their greatest fear was infecting their loved ones (n = 502; 64.1%). The auxiliary nursing care technicians reported the greatest fear of being infected while working (44.0%; p ≤ 0.001) and they were also the occupational group that stated that their biggest fear of infecting their loved ones (81.5%; p ≤ 0.001), as well as the female workers (67.3%; p ≤ 0.022).
Regarding their relationship with the healthcare institution, few felt supported by their direct superiors (23% n = 180), their institution (n = 211; 26.9%), and by society as a whole (n = 206, 26.3%). In addition, participants reported that they lacked the possibility of professional promotion in their current position (n = 355; 45.3%) (Table 4).
Feelings of Canary Islands health personnel towards their work after 5 waves of the COVID-19 pandemic.

However, 33.1% (n = 259) were very satisfied with their work and 64.8% (n = 507) stated that given the choice, they would rechoose their profession. It's important to add that the health personnel under 30 years old (22.9%; p = 0.005), physicians (23.4%) and nurses (26.8%) (p ≤ 0.001), stated that they were less satisfied with their job in comparison with other occupations and age groups. There are even those who, to a lesser extent, affirm that they would choose the same profession again (health professionals under 30 years old (56.3%; p = 0.002), physicians (54.7%) nurses (57.8%) (p ≤ 0.001)).
Finally, they felt that, through their work, they positively influenced the lives of other people (n = 435; 55.6%) and were useful to society (n = 617; 78.8%).
Discussion
Epidemiological situation
When the study period began in week 35/2021, the cumulative incidence (CI) was 50.9 at the national level (24,087 cases per 100,000 inhabitants) and 31.4 in the Canary Islands (703 cases per 100,000 inhabitants). 15 The CI decreased over the course of the study period to 24.6 (11,662 cases per 100,000 inhabitants) and 22.5 (503 cases per 100,000 inhabitants) in Spain overall and in the Canary Islands, respectively. 16
Beliefs
Most of the professionals surveyed affirmed that, in this fifth wave, they had access to the appropriate PPE to protect themselves against COVID-19. This perception was substantially different from that at the beginning of the pandemic, when they had felt fear due to a lack of such protection. 10 Similar results have been described by other authors, who found higher scores relating to the availability of PPE in their centers during successive waves of the pandemic as compared to the first. 17
We must not forget that worldwide, Spain had the highest number of infections recorded among health personnel during the first wave, with more than 15% of all infections being reported in this population.10,18,19 A greater availability of equipment has clearly helped reduce infections among health professionals.
It is noteworthy that most professionals felt that the COVID-19 pandemic had revealed the shortcomings of the system and considered necessary a reorganization of its structure after the health crisis. This situation has led such authors as García-Basteiro et al. 20 to analyze how it was possible for a country like Spain to suffer so greatly from the consequences of the COVID-19 when its health system was considered one of the best in the world. 21 These authors concluded that the system was fragile before the start of the health crisis in March 2020 given that health services were already at the edge of their capacities, with a high healthcare burden and understaffing.20,22
However, even though Canary Islands Health Services increased the number of healthcare professionals hired during 2021 by 130% as compared to 2018 (22,882 vs 17,475 staff),14,23 those surveyed reported a shortage of professionals. Almost all participants believed that having more staff on board would have helped reduce work overload. As an example, in the case of nursing staff, Spain has a ratio of 5.9 nurses per 1000 inhabitants, well below the European standard, which stands at 9.3.23,24
Attitudes
The obtained results allow us to observe a certain degree of burnout and/or a lower level of commitment among health personnel as compared to during the first wave, as the percentage of professionals who were willing to work in conditions of higher infection risk was significantly lower, and there was a reduced willingness to work longer hours, at other centers, and in tasks for which they had not been educated/trained. 10
The possibility of infecting relatives continued to be a determining factor in terms of going to work, and participants were willing to leave their habitual residences to avoid infecting family. Both at the present time and the beginning of the pandemic, health professionals put their responsibility to their families before their work, as shown in studies previously published by this research team.9,10
Regarding the attitudes of these workers on the COVID-19 vaccine, most agreed that vaccination should be mandatory for healthcare professionals. Although only 15–25% of health professionals in Spain were estimated to have received the flu vaccine annually before the pandemic, 25 it does not appear that vaccination needs to be imposed in this group, as 97.4% claimed to have been immunized. When the study period ended, the objective of vaccinating 70% of the population had already been exceeded. 26
A clear dichotomy can be seen between the job prospects of the health personnel according to their age. We highlight two different profiles, the first ones are those that we would call the most involved or committed to their work, since they are willing to voluntarily give up their days off or vacations to continue working, they agree that those who are not willing to work should be penalized and there are even those who put their duty as a health worker before their families. This group mainly includes those over 51 years of age.
In contrast to that group, we find those professionals who work exclusively for economic reasons. They affirm that they would work more if they received some type of incentive from their institution, they are willing to work in more than one health center, less according to the sanctions for those who do not work during the time of crisis and are less willing to resign to their vacations or days off. This group mainly includes those under 30 years of age.
We could find ourselves facing a new social-health paradigm after this pandemic. According to our results, it seems that the younger health workers need more work incentives to continue with their work, since until now it has been the older workers who have sustained the system by working more hours than they were assigned, assuming work overloads and giving up their time off, a situation that young people seem unwilling to accept.
Feelings
Health personnel from the Canary Islands reported being afraid of infection while working and considered their greatest fear to be that of infecting loved ones. Similar results were found in a study carried out in the Basque Country and Navarra, where 44% reported a fear of contagion and of spreading the disease in their homes, and more so if they lived with people at risk. 27
In addition, respondents reported feeling emotionally exhausted both mentally and physically when finishing their shifts, and even “burned out by their work”. Due to their workloads, respondents reported feeling that they lacked the necessary time to complete their tasks during the working day, and in more than half of the cases participants considered themselves to be at the limit of their possibilities at work. One study carried out in the province of Castellón, Spain, found similar results during the first wave, as participants reported that the quality of healthcare had worsened significantly. The authors concluded that the main factor that reduced the quality of healthcare was a high workload, which was in turn related to a lack of personnel and material. 2
However, despite the negative feelings reported by healthcare workers, their resilience and unwavering vocation must be highlighted. Even considering the events experienced during the pandemic, respondents reported that they would choose their profession again given the opportunity and that they were satisfied with their work, feeling their efforts were useful to society. This commitment to society had already been confirmed by the authors of a previous study. 28
Participants did not feel valued by the institutions they worked for. This may be because these workers have not seen any improvements in their working conditions over the course of the pandemic. Zhou et al., concluded in their research in China the importance of the protective effects of organizational support to buffer the negative effect of work-related stressors. In this line, these authors indicated that social support and organizational support had independent predictive effects on the well-being of healthcare workers, with social support seeming more closely related to depression and anxiety and organizational support being more closely related to burnout. 29
To date, no measures have been implemented to resolve the problems that have been endemic to the Spanish health system for some time, such as the continuing temporary nature of contracts and the lack of personnel. As such, healthcare workers do not believe that conditions will change in the short or long term.22,30
Finally, we consider that public administrations must reassess the organization of human resources and health infrastructures, in order to prepare and prevent the collapse of the national health system during situations of a health crisis such as the one we have experienced, so that these events do not cause added stress for professionals or a deprivation of the right to health of the patients with other pathologies.
Limitations
The limitations of this study are those of a cross-sectional study that allowed us to recognize the beliefs, attitudes and feelings of the health personnel towards their work after five waves of COVID-19 at the moment of collecting the data. In addition, the fifth wave affected the distinct regions of Spain differently, and as such, we cannot draw conclusions at the national level.
However, this study provides a “snapshot” of the situation in the Autonomous Community of the Canary Islands at a time when 70% of the general population was vaccinated and there was a low cumulative incidence of COVID-19.
Conclusions
The COVID-19 pandemic has highlighted the shortcomings of the system and the need for reorganization after this health crisis. A clear degree of exhaustion and a reduced commitment of health professionals can be observed as the pandemic continues. Respondents reported feeling both mentally and physically exhausted when they finished their shifts and even “burned out by their work”. Despite this, their resilience and unwavering vocation must be highlighted, as even considering their experiences they would choose their profession again.
Furthermore, we observed that the professionals most committed to the health system itself were those over 51 years old and women. This pandemic has required a large amount of care, and for this reason, nurses have been the most relocated professionals in the health care system. Physicians felt that they have not been able to cope with all the workload that this situation requires, and therefore they are the most overstretched professionals.
Healthcare professionals reported feeling undervalued by their institutions. This is almost certainly because working conditions, far from improving, have worsened despite the events experienced during the pandemic.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
