Abstract
Due to the symptom diversity and pervasive function impairments (e.g. in perception, cognition, language, affect, behavior, daily and social functioning and sense of self), recurrent relapses, elevated disability, high rates of (co)morbidity, heightened premature mortality and high burden of care of psychotic disorders, psychosocial interventions are part of patients' standard care. There is growing evidence on the relevance of self-efficacy for well-being and functioning among these patients, but specific coping with stress self-efficacy has rarely been investigated. This study explored the outcomes of an intervention for the improvement of coping resources based on training in coping skills and coping with stress self-efficacy. Fourteen adult volunteers with schizophrenia (
Introduction
More than 20 million people worldwide are diagnosed with schizophrenia spectrum disorders (SSDs). 1 Antipsychotic drug therapy and psychosocial interventions such as cognitive-behavioral therapy (CBT) are combined for the management of the disease.2–4 CBT aims to improve a broad range of skills for facing symptoms and managing daily life challenges to enhance patients' mental health and overall well-being by achieving clinical improvement, enhanced daily functioning, and higher quality of life. It is necessary for clinicians and researchers to continue exploring theoretically grounded and evidence-based psychosocial therapeutic interventions and their efficacy.
The present study presents the outcomes of a CBT intervention for patients with chronic SSDs grounded in three widely accepted theoretical models: Zubin and Spring's vulnerability-stress model in psychotic disorders,5–8 Lazarus and Folkman's person-context transactional model of stress, and coping 9 and Bandura's self-efficacy theory.10,11 These theoretical proposals highlight stress12–15 as well as deficient or maladaptive both symptom-related and general coping for handling stressful events16–21 in the genesis, onset, course, and treatment of psychosis.
Specific self-efficacy beliefs for coping with stress are a powerful resource for coping. 10 Coping with stress self-efficacy (CSSE) refers to the set of beliefs concerning self-confidence in one's own resources to successfully handle challenging and demanding, stressful events and tasks.22,23 Efficacy expectations refer to the individual's perceived ability to carry out particular coping actions; outcome expectations refer to his or her confidence in obtaining the expected positive outcomes by implementing such coping actions. As such, CSSE beliefs are related to an individual's perceived success in preventing and reducing stress, obtaining positive outcomes and controlling undesired consequences.
Specific self-efficacy for coping with stress has not been examined among individuals with SSDs to determine its influence on the patient's real-world behavior in daily life. As research on general self-efficacy in patients with an SSD is extensive, this research is not specifically regarded to coping with stress. To our knowledge, only one study addressed CSSE. MacDonald et al. 24 found that CSSE predicted effective coping, problem-focused coping, and lower negative symptoms. Nevertheless, this study is limited in terms of the sample composition (i.e. a mixed-diagnostic group of young patients with recent-onset disorder), the measurement of CSSE (i.e. an ad-hoc face-valid item) and its descriptive, cross-sectional design. Unfortunately, this line of inquiry was never continued.
Based on the abovementioned conceptual roots, we designed a type of training in coping with stress and CSSE25,26 aimed at reducing psychotic symptoms and the impact of the disease on general functioning in daily life among chronic patients with SSDs. The intervention was expected to help patients acquire coping skills and simultaneously enhance their self-confidence in managing stress, which subsequently was expected to improve the patients' clinical status and overall well-being. As far as we know, no such dual-purpose intervention targeted for patients with psychotic disorders had been implemented. The present study aims at evaluating the influence of such an intervention. We expected a significant increase on CSSE and perceived successful daily functioning—as derived from coping skills enhancement—in the trained patients; further, we expected that these outcomes would remain up to 6 months later. We also expected that the effects of the intervention would translate into enhanced clinical outcomes, as measured by a symptom-based report, through the mediational effect of improvements in daily functioning; that is, we predicted an indirect mediation path between coping self-efficacy and clinical status through daily functioning moderated in turn by study group (i.e. moderated mediation). Thus, trained patients, with stronger CSSE and better perceived psychosocial functioning as derived from the intervention, were expected to benefit more in terms of clinical symptoms.
Materials and methods
Participants
Fourteen adult individuals of age 21–60 years (

Participant flow diagram.
All participants were in a stable or post-acute phase of their disorder receiving outpatient treatment with no hospitalizations or changes in housing or medication within the last month (non-acute exacerbation, non-prodromal, non-relapse period). No modifications were made to the patients’ medications immediately before or during the study. None of the patients had a concurrent diagnosis of organic brain damage, intellectual disability, substance abuse, or any other major medical or psychiatric illness. 27 Table 1 shows their sociodemographic and clinical characteristics, including the antipsychotic drugs taken by the patients.
Characteristics of the participants.

Eligibility criteria were intended to allow the construction of a homogeneous sample in terms of clinical status. Inclusion criteria were having schizophrenia or schizoaffective disorder, age 18 years old or older and being in a stable phase of the disease. Exclusion criteria included being in an active phase of the disease, refusing to participate, medication non-adherence, recent changes in medication and the abovementioned comorbidities. In addition to the final participants, two participants belonging to the training group dropped out at the beginning of the study (with lack of interest as a reason for withdrawal) and did not participate in further assessments; consequently, they and their matched controls were reassigned to a general wait-list and excluded from the analyses. Due to eligibility criteria, these two participants were not different to the collaborating patients in clinical status or pharmacological treatment issues at baseline.
Measures
The Coping with Stress Self-efficacy Scale (CSSES)22,23 was used to assess CSSE before and after the intervention, 3 months after the intervention (follow-up 1) and six months after the intervention (follow-up 2). Its eight items assess how confident the individuals are in successfully managing stressful events based on their ability to effectively deal with daily life problems or hassles (efficacy expectations—EE, four items—; out-come expectations—OE, four items—). Responses are given on a Likert-type 5-point scale from 1 = “completely disagree” to 5 = “completely agree.” Partial and global scores are derived by adding the items scores, with higher scores corresponding to a greater perceived self-efficacy for managing stress. Adequate reliability and factorial and construct validity have been found for the CSSES.22,23 Yet of limited value due to sample size, internal consistency (
The Areas of Change Index (ACI) assessed patients’ perceived changes in successful daily functioning at post-intervention and 3-month and 6-month follow-ups. This ad-hoc 9-item self-report assessed perceived outcomes, derived from the intervention in the training group or time passing in the control group, in a broad range of areas related to health and functioning, including overall personal functioning; self-control; problem-solving; managing and solving interpersonal problems; managing and solving marital, family, and domestic problems; managing adherence to pharmacological/psychological treatment; managing clinical symptoms, including negative thoughts and hallucinations; and coping with stress (daily stress prevention and management). The responses were given on a Likert-type 5-point scale from 1 = “no change” to 5 = “extreme change.” A total score was obtained by adding the participant's responses, with higher scores indicating a greater perceived change. Internal consistency (
The ACI also included an overall index of Satisfaction with Changes Index (single-item self-report “Please, indicate your personal satisfaction with the changes you observed in your overall daily functioning”; 1 = “completely dissatisfied” to 5 = “extremely satisfied”) assessed the patient's satisfaction with intervention outcomes and perceived improvements in daily life.
The Expanded Brief Psychiatric Rating Scale (BPRS-E 24-items)
28
was used to assess psychotic symptoms at all study phases. We used this rating scale as a semi-structured interview (all authors had received training in BPRS administration and rating following published suggestions). Symptoms were rated for their intensity during a 1-week timeframe from 1 = not present to 7 = extremely severe. The following symptom dimensions were assessed: positive (psychotic) symptoms, negative symptoms, affective symptoms, symptoms of disorientation, and symptoms of (cognitive) disorganization.
26
Subscale scores were obtained by adding responses in each dimension; a global score was then derived by adding the subscale scores, with higher scores indicating the presence of more severe and clinically significant symptoms. Psychometric properties of the BPRS and the expanded version have been demonstrated29,30 and it is a widely used measure in psychiatric assessment. Internal consistency (
Procedure
Details on recruitment and procedure are described elsewhere. 26 After contacting the collaborating therapeutic center, we provided the responsible parties with pertinent information regarding the study. We then had an initial meeting with the patients and their main carers to briefly explain the key characteristics and objectives of the intervention. Voluntary participation was requested, and each interested patient signed an informed consent before baseline assessment. Those who had consented were then scheduled for baseline assessment and an in-depth interview to confirm eligibility criteria, considering also the clinical reports that the center had for each patient. The patients who met the inclusion criteria were then matched by diagnosis, sex, age, clinical symptoms, and antipsychotic medication regimen. Then, the participants were randomly assigned to each of the study groups. Patients in the training group received an intervention for enhancing daily functioning based on the improvement of coping skills and CSSE, as described below, along with their habitual pharmacological treatment; patients in the control group only received their habitual drug regimen. Thus, we used a combination of “treatment as usual” and “wait list” procedures for higher control.32,33 Once the research was concluded, the second author offered the intervention within the collaborating center, as a part of its caring services, to the control group as well as all the individuals who were excluded for research purposes and newly incorporated patients.
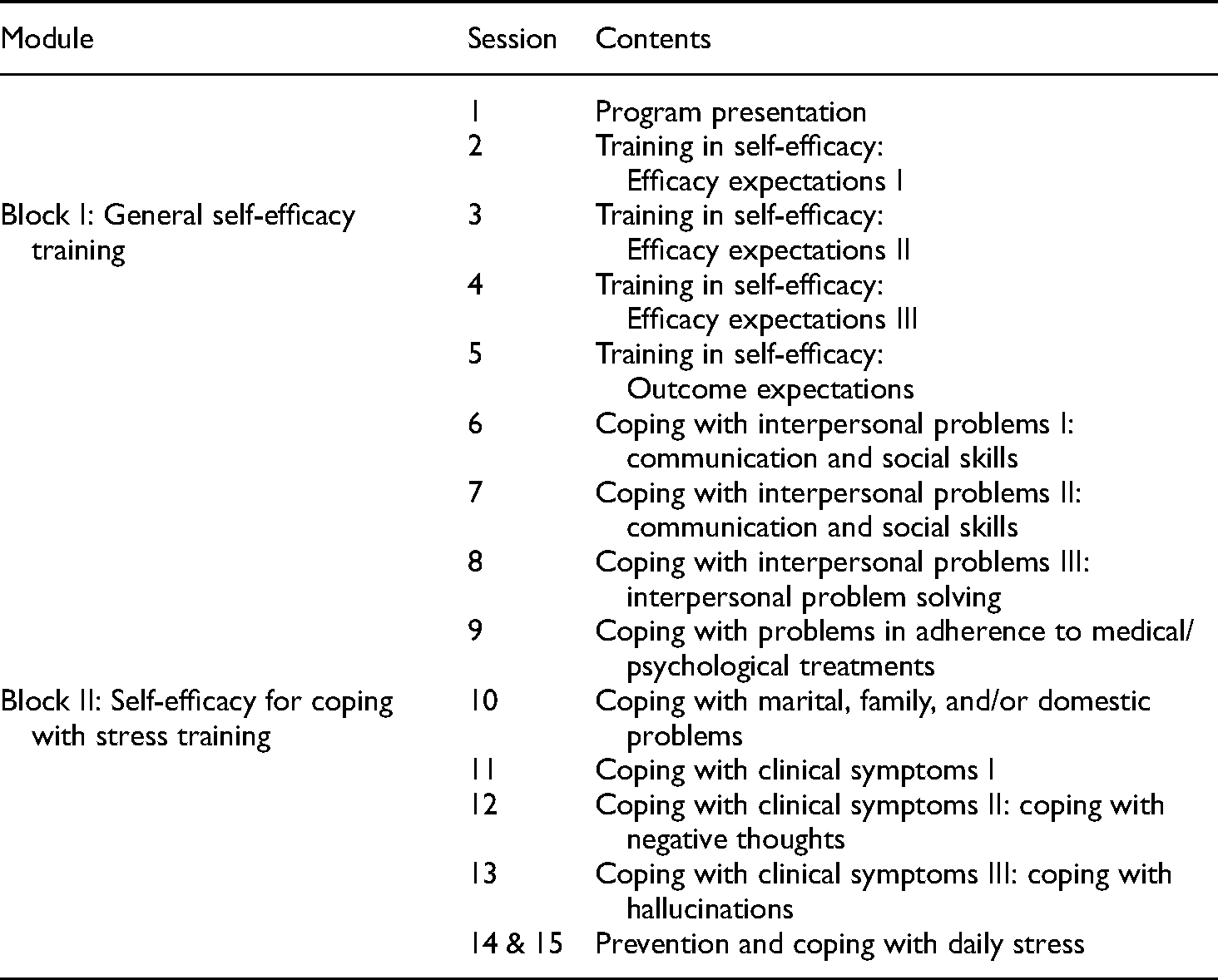
The pre-intervention assessment was conducted during the previous days at the start of the first session of training. The intervention was a training aimed at enhancing successful daily functioning through improving coping resources (including coping skills and CSSE beliefs) over the course of 15 group sessions (8 weeks), with two 150 min sessions per week (with a break within session). An initial block was aimed at explaining and enhancing general self-efficacy and efficacy and outcome expectations, followed by a core-work block aimed at enhancing coping skills and simultaneously increasing beliefs of self-efficacy for coping with stress in several functioning domains. Specifically, the following areas were approached (see Table 2; see also Supplemental file): coping with interpersonal problems; coping with treatment adherence; coping with marital, family, and domestic problems; coping with clinical symptoms; and coping with daily stress.25,26 Personal beliefs in CSSE were enhanced by addressing the main sources of self-efficacy perceptions: enactive mastery experiences, vicarious mastery experiences, verbal persuasion of success, and emotional arousal. 10 The methodology used throughout the program was psycho-education, instruction-guided modeling, and behavioral rehearsal in the framework of problem-solving strategies. As far as we know, no intervention with these characteristics targeted at patients with psychotic disorders had been implemented to date. Our intervention differs from previously published ones in that it includes CSSE as a key element. Post-intervention assessment was conducted immediately following the training and 3 and 6 months later. One of the authors (MLV, supervised by JFG, both conveniently formed and accredited and with clinical expertise in CBT and SSDs) implemented the intervention, whereas one researcher and the clinic staff conducted the assessments with participants' assignment being masked. This study was approved by the authors' institutional ethics committee and followed the international guidelines for research with humans.
Structure and contents per session of the training program in coping with stress self-efficacy (CSSE).
Study design and data analyses
This is a longitudinal, randomized controlled study with between-group (training and control groups) and within-group (baseline, post-intervention, 3-and 6-month follow-ups) factors. Consistently with our aims, we decided to use Per Protocol (PP) procedure for data analysis. PP analysis allows a comparison of treatment groups (e.g. intervention vs placebo, usual care, alternative treatment, or other types of control) by including only those patients who completed the treatment originally allocated so that it allows investigating the effect of receiving (instead of being assigned to) the assigned treatment, as specified in the protocol.34,35
Preliminary analyses were conducted to ensure the quality of the database and to determine the analytical tests to be performed. Non-parametric tests were conducted because parametric criteria of normality and homoscedasticity were not reached and due to sample size. Thus, besides descriptive analysis (mean ± standard deviation for continuous variables and
In addition, moderated mediation effects were analyzed with the PROCESS Macro for SPSS, 37 to test whether the influence of post-intervention levels of coping self-efficacy on clinical status after the intervention was mediated by perceived successful functioning and, simultaneously, moderated by the experimental condition (intervention vs time passing). Moderation seeks to determine whether the size or sign of the effect of some putative causal variable or a mediation term on the outcome variable depends on (i.e. interacts with) a moderator variable, so that it establishes how a process operates if the moderator places constraints on how and when that process can function. 37 Moderation effects in a mediation pathway are equivalent to an interaction between any of the paths that define the mediating indirect effect and the moderator, so that the amount to which the mediator translates the effect of the predictor into the outcome depends on the levels of a moderator. Preacher et al.'s approach emphasizes the estimation of conditional indirect effects by bootstrapping those conditional effects. 38 Consequently, for each analysis, 5000 bootstrap random resamples were obtained from the data for parameter estimation, ensuring the stability of the analyses. Bias-corrected 95% confidence intervals (95% CI) were then derived from the obtained distribution of coefficients over the samples, which requires no assumption regarding the underlying distributions because the statistical significance level is determined non-parametrically.
Analyses were carried out without missing data, with a significance level at
We followed the updated Consolidated Standards of Reporting Trials statement for randomized trials of non-pharmacologic treatments for reporting the present research. 39
Results
In the training group, Friedman's within-group comparisons showed significant changes between the four assessment phases for the global score in the CSSES (

Panel A. Repeated measures for the study groups for CSSE. Panel B. Differences between the study groups for the CSSE.
CSSE, ACI, and SCI within-group and between-groups comparisons for each assessment phase.
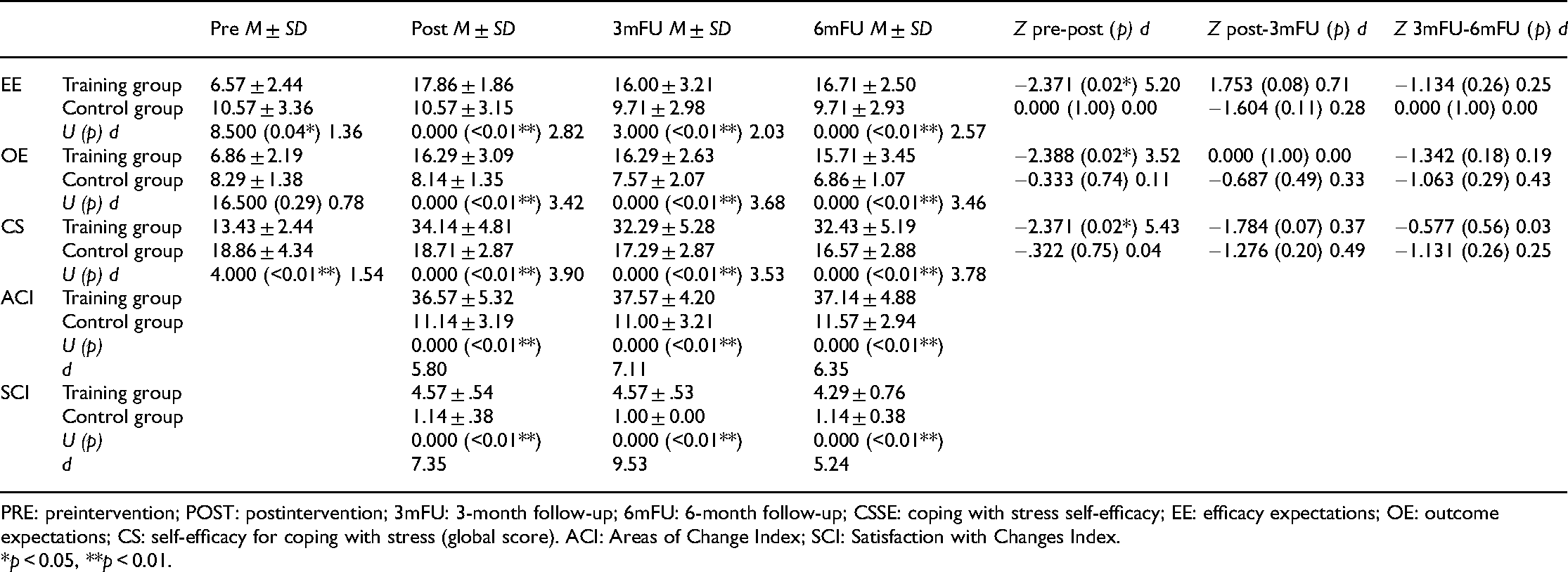
PRE: preintervention; POST: postintervention; 3mFU: 3-month follow-up; 6mFU: 6-month follow-up; CSSE: coping with stress self-efficacy; EE: efficacy expectations; OE: outcome expectations; CS: self-efficacy for coping with stress (global score). ACI: Areas of Change Index; SCI: Satisfaction with Changes Index.
*
Mann–Whitney's
Patients in the intervention group also reported significantly higher perceived positive functioning in daily life as well as higher satisfaction with these changes compared to patients in the control group at post-intervention assessment (see Table 3). These significant differences continued at the 3-month and 6-month follow-ups.
Detailed findings obtained for the BPRS-E are published elsewhere.
26
Attending to the global score, Friedman's (
BPRS-E within-group and between-groups comparisons for each assessment phase.

PRE: preintervention; POST: postintervention; 3mFU: 3-month follow-up; 6mFU: 6-month follow-up; POSIT: positive symptoms; NEGAT: negative symptoms; AFFECT: affective symptoms; DISOR: disorientation symptoms; DISORG: disorganization symptoms; TOT: total score.
In this case it is not possible to calculate the coefficient
*
According to our second hypothesis, changes in clinical status from baseline to post-intervention would be mediated by post-intervention perceived successful functioning (i.e. coping skills used in daily life) as derived from self-efficacy for coping with stress beliefs, and moderated in turn by study group. To test this hypothesis, a moderated mediation analysis was conducted, with differences in scores on the BPRS-E from pre- to post-intervention as the outcome, the CSSES total score at post-intervention entered as the predictor, the ACI score at post-intervention entered as the mediator and the experimental condition entered as a moderator of such a relationship. The results are displayed in Table 5 and Figure 3. The moderated mediation was confirmed. Boot-strapped CIs used for inferring the conditional indirect effect given the values of moderator (intervention vs control group) revealed that this indirect effect is different from zero except among those patients not receiving the intervention, for whom there is no indirect effect of coping self-efficacy on clinical symptoms through daily functioning. Thus, perceived successful functioning in daily life as predicted by stronger coping self-efficacy resulted in higher improvements in clinical status (i.e. higher change) at post-intervention for the trained group, but not for the control group. Moreover, coping self-efficacy could not predict clinical status directly but only indirectly by this moderated mediation effect. Overall, 48% of the variance in BPRS-E changes was accounted for by the entire model.
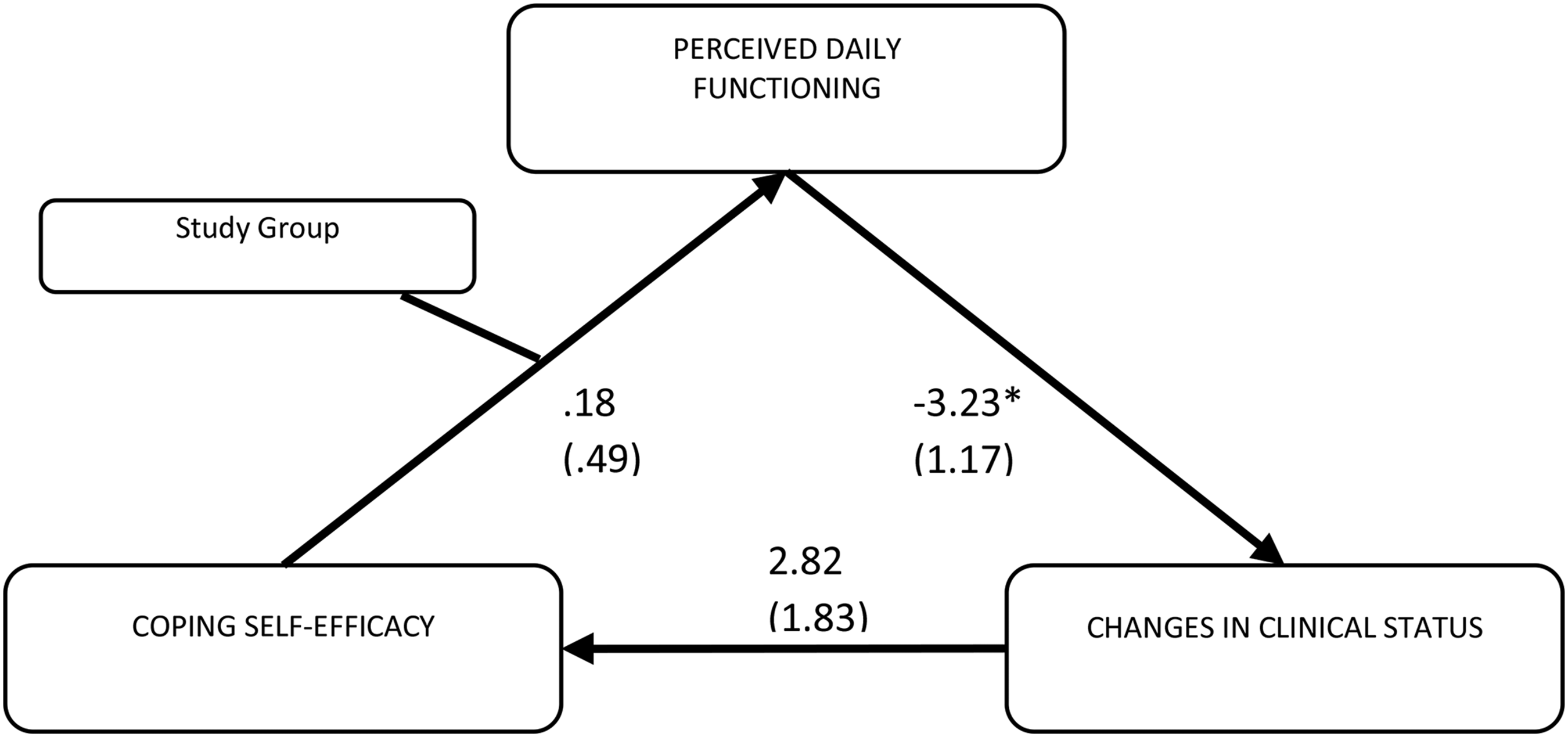
Moderated mediation: study group moderates the indirect relationship of coping self-efficacy and change in clinical status through perceived daily functioning based on coping skills. Non-standardized coefficients. Standard errors are shown in brackets.
Changes in clinical status as predicted by coping self-efficacy mediated by perceived successful functioning based on coping skills and moderated by study group.

ACI: Areas of Change Index; CSSE: self-efficacy for coping with stress (global score); LLCI: lower limit of the 95% CI; ULCI: upper limit of the 95% CI.
*
Discussion
Treatment of SSDs currently involves antipsychotic medication and psychosocial therapies, the combination of which is often helpful for people with psychotic disorders to gain better clinical outcomes and recovery, decrease functional impairment and reduce the number of relapses and hospitalizations. By focusing on modifiable protective psychosocial resources, rather than only on risk and disease factors, it is expected that patients will experience improved clinical outcomes, lower relapse rates and enhanced well-being, quality of life and daily functioning (i.e. personal, familial, social, and work roles). 25 Following this rationale, we implemented a pioneering training program aimed at enhancing coping skills and CSSE in a group of patients primarily diagnosed with SSDs.
Our first aim was to explore whether the intervention increased personal resources for coping with stress, including CSSE, and improved daily functioning by using successful coping skills and by trusting in an enhanced perception of the capability of managing stress. Findings revealed that CSSE significantly increased in the training group after the intervention (effect sizes up to 5.4), and these improvements remained at follow-ups. The percentage of changes and effect sizes are remarkable. In addition, significant differences were found between the intervention and the control groups at all of the assessment phases, which demonstrated that trained patients gained more CSSE, even when they started with comparatively worse perceptions. Moreover, the divergences slightly but progressively increased over time. Trained patients also reported significantly higher perceived positive functioning in daily life as well as higher satisfaction with these changes compared to controls at post-intervention and follow-ups. Furthermore, these improvements were accompanied by a significant reduction in BPRS-E psychotic positive, negative, affective, and disorganization symptoms among trained participants, compared to control patients (effect sizes up to 4.4). This improvement in clinical status was also maintained over time, with further enhancements in several domains. Percentages of change and between-groups differences and effect sizes for all these differences are also noteworthy. In contrast, control participants showed non-significant changes throughout the study for both coping self-efficacy and, in general, clinical status. Thus, no “wait-list” (or “treatment as usual”) effect was observed.
This study revealed unique improvements following this theoretically driven intervention. As far as we know, no other intervention aimed at increasing CSSE along with coping skills among individuals with SSDs has been implemented to date, thus it is impossible to compare findings. Self-efficacy perceptions have been found to have an influence on coping efforts and functional or clinical outcomes (see below). Moreover, when self-efficacy trainings have been implemented, or self-efficacy has been addressed by interventions, positive outcomes have been obtained.40–42 These interventions could be effective in increasing patients' self-efficacy to manage their illness and empowering them. The present study contributes to research on self-efficacy and coping with stress among patients with SSDs, complementing the findings obtained by MacDonald et al., 24 as well as on the efficacy of psychosocial therapy, particularly CBT, in the therapy of psychotic disorders. Our findings suggest that it is possible to enhance a sense of agency among individuals with schizophrenia. The sense of being an active agent in managing the disease as well as daily demanding situations may decrease patients' vulnerability to stress and increase their ability to influence the environment, empowering individuals for enhanced independent living, employment, social relationships, and overall well-being. Thus, interventions targeting coping self-efficacy may be beneficial for increasing inner resources in order to manage not only the disease stressful symptoms and the hardships imposed by the illness but also the varied stressful events that SSDs patients encounter in daily life.
The present study further examined whether the indirect effect of coping self-efficacy on clinical status through perceived successful daily functioning by applying coping skills varied as a function of receiving an intervention focused on enhancing coping resources (i.e. whether this mediated relationship occurs at each level of the moderator, study group). Supporting a conditioned effect, findings revealed that only in the intervention group, greater perceptions of personal efficacy for coping with stress contributed to enhanced daily functioning and thus to better clinical status. As previously noted, 43 indirect analyses are especially interesting in prevention and treatment studies, where interventions are designed to change the outcome of interest by targeting process variables that are hypothesized to be causally related to the outcome.
Self-efficacy theory postulates that “self-efficacy is not simply a correlate of functioning, but contributes to it by mediating the relationships between other variables and functioning” (p. 194). 44 Following the self-efficacy theory,10,11 it is possible that self-efficacy, as a protective factor, mediates the effects of coping styles and efforts for coping with psychiatric illnesses on daily functioning and successful adjustment.44,45 It is also possible that it mediates the influences of stressors and disease-related distress on functional and well-being outcomes. 46 However, when mediational indirect effects have been tested for self-efficacy on functional outcomes and illness-related behaviors, generally no support has been obtained,44,47–54 with a few favorable findings.50,55–57 More robust findings have been reported when self-efficacy was considered as a predictor of a patient's functioning when other mediators were considered, such as negative symptoms and illness-related emotional distress.44,51,52,54,58,59 These studies, particularly those supporting the influences of self-efficacy on functioning-related mediators, are in line with our results, which point out that self-efficacy predicts illness-related patient functioning, which in turn predicts clinical outcomes and adaptation. As self-efficacy is domain-dependent, the use of indicators of general self-efficacy instead of domain-specific self-efficacy might have contributed to the mixed results in the schizophrenia research literature. 54 Further exploration of the specific relationships between stress, coping, self-efficacy for coping and health- or functioning-related outcomes is warranted. The present study, using a domain-specific self-efficacy and an experimental, intervention-based design, helps provide a deeper understanding of the predictors and paths of functioning and well-being in SSDs.
Understanding the relationship between self-efficacy and psychosocial functioning has implications for the treatment of SSDs. Clinical research has highlighted the importance of evidence-based psychological interventions to enhance everyday functioning and quality of life by enabling patients to achieve a productive, sustained, independent living, vocational or educational activities, satisfying interpersonal relationships and meaningful lives, not merely the reduction of symptoms and relapses. Strength-based interventions, aimed at enhancing self-agency, coping capacities, personal potential and self-worth are crucial for recovery. If individuals with schizophrenia have the capability to perform daily behaviors but fail to do so because they perceive that they lack the ability, direct attempts at increasing self-efficacy should be included as part of the treatment.44,60 Our findings point out the importance of not only offering the patients effective coping skills but also of improving patients’ confidence in their use and efficacy to enhance their clinical status and adjustment to their disease. Further, specific CSSE may influence patients’ psychosocial functioning, overall well-being and quality of life, which would in turn impact their coping efforts 61 and thus their CSSE beliefs. Interventions such as the one presented in this study are aimed at increasing resources for living as independently and successfully as possible. Increasing self-efficacy beliefs might be essential for patients, as it has been demonstrated that these self-beliefs decrease with chronification of the disorder, probably due to the continued failure to cope successfully with the challenges of the illness and daily living. 51 Establishing the relationships among psychosocial resources such as coping and self-efficacy with indicators of well-being and clinical status allows us to understand the underlying processes of such relationship and to use this information to design effective evidence-based interventions 62 for promoting fulfilling and optimal living and positive clinical status in schizophrenia and related disorders.
Despite the strengths (e.g. domain-specific constructs, clinical randomized study, prospective design) and pioneering and inspiring findings presented herein, this study has several limitations to note. First, the small sample size of voluntary patients and the reduced number of individuals with psychotic disorders other than schizophrenia raise cautions on the generalizability of the findings. Nonetheless, to individualize treatment as much as possible and maximize its possible benefits, we decided to offer it to a limited number of patients. Moreover, given the PP nature of the research, these promising results must be replicated in larger samples before firm conclusions about its clinical relevance can be made. Second, further research is needed aiming at establishing long-term outcomes (i.e. over 6 months) after the training. Third, our findings rely on self-reported data, and their validity would be enhanced with other sources of information, such as external informant reports, behavioral observations, or experience-based sampling. In addition, we selected a measure, the CSSES, which had not been used in patients with SSDs previously, and given the sample size its psychometric properties were not fully investigated. Yet it is an uncomplicated measure with items very understandable in their contents, future research is needed exploring its use with this type of patients and its clinical utility in this population. Similarly, the ACI was a measure specifically created for our assessment purposes and for enriching the findings obtained with the BPRS, but its utility in other research or with clinical purposes could be limited. Moreover, we have not considered clinical indicators (e.g. adjustments in medication, relapse rates, information from relatives) other than self-report questionnaires and clinicians’ judgments. Besides, indirect effects analysis is notably less powerful than outcome analysis, 63 which means that only very strong effects would likely be detected in the present study due to sample size. Nonetheless, the robustness of our findings might be questionable due to sample size and composition even when bootstrapping was used to increase the stability of parameters, and future research replicating the present findings with broader samples is warranted. Yet the postulated moderated mediation was demonstrated, the path from coping self-efficacy to perceived successful functioning was not significant. However, recent positions note that the sole requirement to demonstrate a moderated mediation is a significant conditioned indirect effect on either the total or the direct effect.64,65 This training might be associated also with increased awareness of improved overall coping ability, which may be particularly influential for symptom management, clinical improvement, and daily functioning. This could be due to improvements in insight and reduced symptom-related distress due to increased confidence that symptoms, social and life stressors can be successfully navigated which could reduce the intensity of ruminative or delusional thinking. Consequently, training self-efficacy for coping with stress might have broader influences in increasing the functional ability of patients. Future research should explore this or other possible complementary hypotheses. For this, in addition to clinical studies, qualitative research would be very informative. Future research should complement this research with, for instance, interviewing the participants to understand their experience with the disease, the treatment and the outcomes of the intervention, which will also be helpful in refining the intervention.
Conclusions
In conclusion, this longitudinal, experimental-design study with manipulation of coping resources, including CSSE, found that significant improvements in the clinical status of patients diagnosed with SSDs were associated with changes in coping resources. CSSE is revealed as a powerful contributor to clinical status. This study elucidates the mechanisms by which CSSE and coping work together in accounting for patients' functioning in the real world and well-being and thus contributes to the cumulative knowledge on the psychosocial resources for enhanced quality of life in psychosis.
Supplemental Material
sj-docx-1-sci-10.1177_00368504211056818 - Supplemental material for Training coping skills and coping with stress self-efficacy for successful daily functioning and improved clinical status in patients with psychosis: A randomized controlled pilot study
Supplemental material, sj-docx-1-sci-10.1177_00368504211056818 for Training coping skills and coping with stress self-efficacy for successful daily functioning and improved clinical status in patients with psychosis: A randomized controlled pilot study by Débora Godoy Izquierdo and María Luisa Vázquez Pérez, Raquel Lara Moreno, Juan F Godoy García in Science Progress
Footnotes
Acknowledgment
We are grateful to the participants who made this study possible.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was partially supported by the financial aid provided to the Research Group CTS-267 by the Consejería de Innovación, Ciencia y Empresa, Junta de Andalucía (Spain).
Institutional review board statement
The study was conducted according to the guidelines of the Declaration of Helsinki, and approved by the Ethics Committee of Universidad de Granada.
Informed consent statement
Informed consent was obtained from all subjects involved in the study.
ORCID iD
Débora Godoy Izquierdo https://orcid.org/0000-0002-4294-4232
María Luisa Vázquez Pérez ![]()
Supplemental material
Supplemental material for this article is available online.
Author biographies
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
