Abstract
Several open and arthroscopic techniques for repair triangular fibrocartilage complex (TFCC) tears have been used. The aim of this study, using a cadaveric model, was to compare the biomechanical resistance to the pronosupination movement of arthroscopic repair with anchor and pull-out techniques in TFCC tears of Atzei type II lesions. Eighteen forearms of cadaveric specimens were evaluated arthroscopically, of which 12 were selected according to the inclusion criteria. All specimens were injured with an Atzei type II lesion and were repaired arthroscopically. Six forearms were repaired using the anchor technique and the other six with the pull-out technique. To assess the biomechanical resistance of the repair, the forearms were tested to 300 cycles of 160° pronosupination. Two evaluators independently assessed the repair status every 10 cycles and the modified Desai classification was used to verify the presence of failure. The mean failure of the repair occurred at 41.6 cycles (SD 7.5) for the pull-out technique and at 28.3 cycles (SD 9.8) for the anchor technique, showing a difference of 13.3 cycles (p = 0.025) in favor of the pull-out technique. In all cases, repair failure occurred at the junction of the fibrocartilage with the suture. Arthroscopic repair with the pull-out technique showed greater biomechanical resistance to pronosupination movement in comparison to the anchor technique. Interestingly, the failure of arthroscopic repair of Atzei type II lesions occurs at the junction between the suture and the fibrocartilage.
Introduction
Atzei type II triangular fibrocartilage complex (TFCC) tears are the main cause of pain in traumatic lesions of the ulnar edge of the wrist. 1 These are the most frequent TFCC lesions associated with wrist fractures and also the most frequently repaired ligament lesions.2,3 Current evidence reports that there is no difference in the repair of TFCC lesions performed by open surgery or arthroscopically.4–7 Central TFCC lesions can be treated orthopedically with rest, pronosupination limitation splints, corticosteroid infiltration and changes in daily living activities. 8 In Atzei type II TFCC lesions; surgical treatment includes central debridement, 9 and repair of the injury with the anchor or pull-out technique, performed by open surgery or arthroscopically. 10 Arthroscopic repairs have some advantages, such as less soft-tissue injury, shorter immobilization time, quicker mobility recovery and better esthetic appearance,5,10 and several studies have reported good to excellent clinical results with arthroscopic repair of these types of TFCC lesions.1,3–7,9,11–15
The complication rate of arthroscopic wrist repairs is 5.9% of all cases. 8 The most frequent complications are repair failure, tendon lesions and lesions of the sensory branches of the ulnar and radial nerve. 8 There are a limited number of instances of repair failure that have been reported when open surgery subsequent to arthroscopic repair has been performed. Currently, there are no published studies that have evaluated the biomechanical resistance to the pronosupination movement of TFCC repair with the anchor or pull-out technique.
The main objective of this study is to compare the biomechanical resistance to the pronosupination movement of arthroscopic repair with anchor and pull-out techniques for Atzei type II TFCC lesions in a cadaveric model. The secondary objective is to describe where failure occurs in the repair.
Materials and methods
The cadaveric preparations were provided by the voluntary donor program of the Autonomous University of Barcelona. In each preparation, the segment between the hand and the distal third of the humerus was used. In total, 18 forearms were evaluated by arthroscopy, of which 12 met the TFCC indemnity, we descarted four forearms for traumatic injury from radial border and two for severe degenerative lesion, with only remnants of TFCC.
Diagnostic arthroscopy was performed on each preparation; using an Acumed traction tower (Hillsboro, USA) suspended with medium-sized traction devices from the index and middle fingers with 10 kg. In addition, an arthroscope with a Storz HD camera (Tuttlingen, Germany), 2.7 30° optics (Linvatec-Conmed) and a Shaver 3.0 (Linvatec-Conmed) with a motor were used. In all cases, in order to achieve the correct position of the preparations, the traction tower was fixed to the table with two brackets and the arm segment fixed to the traction tower with plastic clamps (Figure 1).

Biomechanics model.
Dry arthroscopy was performed using portals 3, 4 and 6U. Radiocarpal joint cleaning was performed with 5 ml of physiological serum, an optical trocar syringe and aspirated with the Shaver 3.0 (Figure 2). The presence of traumatic and/or degenerative TFCC lesions was diagnosed was trough a diagnostic arthroscopy using the Arthrex probe.

Arthroscopy.
A complete release of the ulnar insertion of the TFCC was performed, from the apex of the ulna to the fovea. The TFCC was released from its insertion distal and proximal into the ulnar styloid to the fovea from 6U portal using scalpel number 11, which produced a huge lesion similar to the Atzei type II TFCC, under arthroscopic vision from portal 3 to 4. In all cases, the complete lesion was checked with a probe and a Ballottement test. The repairs were performed by two hand surgeons, both with experience level 4 according to the classification of Tang and Giddins. 16 The specimens were randomly assigned to one of the two repair methods under study. Six were repaired with the 2.7 Corkscrew Arthrex titanium anchors and Fiberwire 2.0. The other six were repaired using the pull-out technique (outside-in) with Fiberwire 2.0 braided polyester, in supination and ulnar deviation of the wrist. The two surgeons randomly performed one of the two repair methods. 10 The repair was made with the camera in 3–4 portal and instruments in 6R portal, with forearm in supination position and all case with synovectomy with Shaver 2.5 through 6U portal.
Anchor fixing method
Fixation was carried out with an Anchor Corkscrew 2.7 and Fiberwire 2.0 Arthrex by a small ulnar incision to the 6U portal. Anchor sutures with lasso suture are rescued from the 6U portal under arthroscopic vision, and then a sliding knot is tensioned using knot lowering. A repair resistance check with made with a negative trampoline test probe (Figure 3).
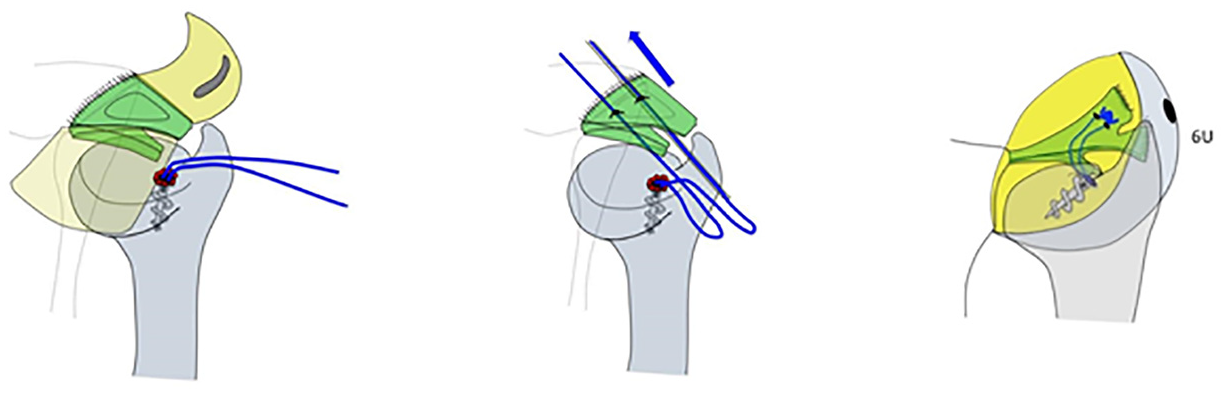
Anchor fixing method.
Transosseus pull-out fixing method
A double bone tunnel is made with a Kirschner wire from the ulnar edge 1.5 cm proximal to the head of the ulna, with 5 mm of separation between tunnels. Fiberwire 2.0 suture passage was through the bone tunnels of the TFCC, returning to the edge of the ulna using hypodermic needle number 18. Tension check of the TFCC was made under arthroscopic vision with traction of the suture ends, four simple knots blocked; a repair check was made using a negative trampoline test probe (Figure 4).

Transosseus pull-out fixing method.
Subsequently, the repairs were evaluated under arthroscopic vision in pronation and supination, verifying reintegration of the TCFF and in clinical form with the absence of the Ballottement test. The preparations were then subjected to pronosupination cycles, for which they were disassembled from the arthroscopy tower and placed on the test stand.
A metal support for the forearms was built in a vertical position with a vertical arch 1.7 m high by 1 m wide and a 1 m3 base capable of resisting the weight and movement of the repaired forearms. The suspension of the forearms was done from the hand, passing the Kirschner wires 2.5 through the diaphysis of the metacarpals, not including the thumb. Subsequently, this was attached to a circular Ilizarov frame with two arches joined by four screws (20 cm diameter, 40 cm height) and a hand fixation to the pre-tensioned lower arch of the Kirschner wire at 200 N in order to increase its resistance to deformation by the weight of the preparations. The movement of the forearms was made by joining the arches of the Ilizarov frame through a central 12-volt motor shaft welded to the vertical support that allows a rotation of 160° at 40 cycles per minute with a turning force of 60 N.
The repaired specimens were subjected to 300 pronosupination cycles and were evaluated by two independent observers every 10 cycles for the occurrence of repair failure and type through portal 3–4. The repair failure was determined by the appearance of a gap that allows the introduction of a 2-mm Arthrex probe between marks. 17 The type of repair failure was classified, using the modified Desai classification, into Type I (loss of ulnar fixation), Type II (loss of radial fixation), Type III (loosening of the nodes), Type IV (loss of the TFCC suture junction), and Type V (suture rupture).
Statistical analysis
All collected data were tabulated using Excel and statistical analysis was performed with the Stata 13.0 program. To choose the statistical test for data analysis, we first evaluated the normal distribution of the data using the Shapiro–Wilk test. To compare the results between groups we used Student’s t-test or the Mann–Whitney U-test for two independent samples; in both cases a significance level of 0.05 was established. The agreement rate between the two observers was calculated using kappa statistics.
Results
The mean age of the cadaveric preparations was 53.4 years (range 52–64 years) and six were female and six male. A total of 12 forearms from the 18 evaluated were selected after meeting the eligibility criteria; of the remaining six, four presented TFCC disinsertion from the radial border and two presented complex degenerative injuries.
Using the previously described method to measure failure cycles and type, the number of cycles until failure was determined with a 0.88 kappa value between both independent observers under arthroscopic observation. Comparison of the results for the two groups is presented in Table 1. The mean failure of the repair was 41.7 cycles (SD = 7.5) with the pull-out technique and 28.3 cycles (SD = 9.8) with the anchor technique, the difference being 13.3 cycles (95%CI = 24.6–2.1) in favor of the group repaired with the pull-out technique (Figure 5). This difference was statistically significant, with a p-value of 0.025.
Comparison of the results between groups.

CI 95%: confidence intervals 95%; SD: standard deviation; TFCC: triangular fibrocartilage complex.
p-value obtained with Student’s t-test for independent samples.
p-value: obtained with chi-square test.

Comparison of biomechanical resistance to the pronosupination movement of arthroscopic repair with anchor and pull-out techniques.
When the type of failure was observed, interestingly, in all cases the failure was Type IV, this failure type occurs at the junction between the TFCC and the suture, specifically when the TFCC is torn by the suture, and before 50 pronosupination cycles.
Discussion
The lesion of the ulnar insertion of the fibrocartilage in all the specimens produced radioulnar instability. This was corrected by repairing the fibrocartilage using the anchor and pull-out techniques. In our study, the pull-out technique showed greater biomechanical resistance to pronosupination movement in comparison to the anchor technique. In addition, the failure of arthroscopic repair of Atzei type II TFCC lesions occurred in all cases at the junction between the suture and the fibrocartilage, specifically when the TFCC is torn by the suture.
Regarding the surgical techniques to reinsert the ulnar border of the TFCC, the most common being the techniques with anchors and bone tunnels. In patients operated for instability of the distal radioulnar joint, repair of the TFCC has been defended in the short and medium term, with good results reported in various studies regarding remission of symptoms. However, there are no published studies that have evaluated the clinical and/or arthroscopic correction of instability or the resistance of the repair techniques used. Our study evaluated the resistance of the TFCC repairs until the appearance of a 2-mm gap or repair failure, similar to what was done in another study. 18 Additionally, the arthroscopic repair of Atzei type II TFCC lesions with an outside-in technique has greater resistance to pronosupination using the pull-out technique rather than the anchor technique, and this has not been reported previously in the literature.
In our study, we used the modified Desai classification for the pull-out suture in order to classify the types of failure (knot and tissue failure). 17 This classification identified four of the most frequent types of failure at the level of the TFCC and sutures found in our study. Interestingly, in all our cases, failure occurred at the suture–TFCC junction and before 50 pronosupination cycles. This was used as the basis for the recommendation to limit active movements of pronosupination post-surgery, because it is the movement that most stresses this type of structure. We believe that evaluating the biomechanical repair of Atzei type II lesions allows us to demonstrate the scope of the repair and the sensitive points of failure, as well as to extrapolate the risks of early mobilization.
To our knowledge, this is the first study that assessed the biomechanical resistance to the pronosupination movement of TFCC repair with the anchor or pull-out technique. Despite, the failure that occurs in the two techniques early, there is a significant difference in favor of the pull out technique. We think that these findings are not explained by the type of surgical technique used in the repair. One rational explanation could be that these surgical interventions are dependent operator. This is an important factor because the level of expertise and/or clinical experience could influence the final results in the treatment of each patient.
According to our findings, it is necessary to protect the repair of early pronosupination due to the risk of failure. Additionally, it is necessary to reevaluate the indication for surgical repair in patients over 50 years of age, considering that in our cases 6 out of 18 forearms evaluated present damaged of TFCC.
Our study has some limitations that should be considered when interpreting our findings. The main limitation of our study is the older age of all the specimens used. Additionally, we note that this could condition the type of failure found and that the applied biomechanical forces do not could replicate the circumstances that can occur in clinical conditions.
Conclusion
Arthroscopic repair with the pull-out technique showed greater biomechanical resistance to pronosupination movement in comparison to the anchor technique. Interestingly, the failure of arthroscopic repair of Atzei type II TFCC lesions occurs at the junction between the suture and the fibrocartilage.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
The cadaveric preparations come from the voluntary donor program of the Autonomous University of Barcelona.
