Abstract
Many religious disaffiliates, similar to immigrants, experience health vulnerabilities. Yet, few studies address their ability to access the healthcare system. This article contributes to filling this void by examining the case of Israeli Jewish ultra-Orthodox disaffiliates. The study analyzes the barriers that hinder these disaffiliates’ access to the healthcare system, adversely affecting their well-being. This research is based on 36 in-depth, semi-structured interviews with ultra-Orthodox disaffiliates, analyzed using qualitative thematic analysis. Six barriers were identified: lack of health-related education and knowledge of the healthcare system, poverty and structural determinants of health, lack of respect for authority, communication gaps, lack of belonging, and stigmas, particularly in mental health. We recommend training healthcare providers and students to better understand and address these barriers and disaffiliates’ unique needs when providing care for them. Specifically, we suggest incorporating this overlooked subject in the frameworks of cultural competency and structural competency, encouraging collaboration between healthcare practitioners and religious disaffiliates to promote equitable and inclusive policies. Implications for community organizations include offering courses, simulations, peer guidance, and consultation for disaffiliates on health-related issues, as well as engaging disaffiliates in self-advocacy. We propose that this study is relevant to disaffiliates from varied insular, high-tension religious communities worldwide.
Keywords
Introduction
Religious disaffiliation, understood as leaving a religious tradition or specific religious affiliation, has become more common over the past few decades (Fenelon and Danielsen 2016; Vargas 2012; Wittberg 2021). Although disaffiliation has clear gains for disaffiliates, such as increased autonomy, this is often an immensely difficult and burdensome process, as individuals who leave their religious communities must learn to navigate their new lives, often without social support. Similar to experiences of new immigrants, disaffiliating can adversely affect mental and physical health, especially if “push” factors—those that compel a person to leave—outweigh “pull” factors—those that compel a person toward a new community (Engelman et al. 2020; Pinchas-Mizrachi and Velan 2022).
Religious disaffiliates’ increased mental and physical health challenges require that these people have access to appropriate healthcare services. However, little is known about the barriers religious disaffiliates face when accessing the healthcare system. Moreover, as Haire (2022) showed, studies that have examined the mental health impacts of disaffiliation lack the specificity and objectivity required to move the results from description to praxis. This article aims to contribute to bridging these gaps by analyzing the case of Israeli Jewish ultra-Orthodox disaffiliates, a rapidly growing social group that has been under-researched. We ask: What are the barriers that hinder Israeli Jewish ultra-Orthodox disaffiliates’ access to the healthcare system? After analyzing six barriers, we illustrate the applied implications and recommendations for healthcare practitioners and community organizations. We propose that this case study can help practitioners to better understand and address the needs and difficulties of ultra-Orthodox disaffiliates, as well as disaffiliates from other insular, high-tension religious communities worldwide. Thus, this study can contribute to promoting more equitable healthcare to varied groups of religious disaffiliates.
Literature Review
Access to Healthcare
According to the National Academies of Sciences, Engineering, and Medicine (formerly known as the Institute of Medicine), access to healthcare is defined as “timely use of personal health services to achieve the best possible health outcomes” (Institute of Medicine 1993:4). Gulliford et al. (2002) identified four dimensions of access to healthcare: availability of services; utilization of services and barriers to access; relevance, effectiveness, and access (access based on healthcare outcomes); and equity and access (healthcare meets the specific needs of the person accessing it). Poor access to healthcare services generally translates to lower rates of service utilization and poorer health outcomes.
A study by Dawkins et al. (2021) identified three primary factors that can affect access to healthcare: a delay in the decision to seek care by the patient, a delay in reaching an adequate facility, and a delay in receiving actual care in a medical facility. The extent to which a population accesses healthcare is contingent to the existence of barriers, such as economic, organizational or cultural barriers that may hinder a person’s ability to utilize healthcare services (Gulliford et al. 2002). Differences between communities, cultural backgrounds, social and structural determinants of health, and unique health needs may affect the access to healthcare of various populations.
Jewish Ultra-Orthodox Society in Israel
Ultra-Orthodox Jews are characterized by their strict observance of Jewish law and insularity from mainstream society. Known in Hebrew as Haredim (Haredi, sing.), they comprise 13.3% of Israel’s population (Malach and Cahaner 2022). The majority live in closed community enclaves. The ultra-Orthodox society struggles for religious sovereignty, maintains its social and spiritual boundaries, and is often suspicious of the outside world, despite a trend of increasing integration in Israeli society in recent years (Caplan and Leon 2023; Vardi, Orr, and Finkelstein 2019). Ultra-Orthodox persons’ strict observance of Jewish law dictates how they dress, what they learn, how they interact with the opposite sex, and what foods they eat (Caplan and Stadler 2012).
The ultra-Orthodox society is characterized by a conservative worldview, commitment to the traditions of their communities of origin, commitment to religious study (“a learners’ society”), a distinct dress code, unique internal discourse and language, separate ultra-Orthodox education systems for boys and girls, and principles of gender separation and modesty (Caplan and Leon 2023; Davidman and Greil 2007). Ultra-Orthodox people use independent sectoral media, supervised by rabbinic committees. Access to the internet as well as non-religious media and books is limited (Orr, Erblich, et al. 2021; Shomron 2022; Shomron and David 2022).
Rabbinic authorities play a key role in community members’ decision-making, including decisions related to everyday life, physical and mental health, and disabilities (Genut et al. 2022; Orr, Unger, and Finkelstein 2021a; Shomron and David 2022). Additionally, askanim (askan, sing.), defined as lay helpers, informal helpers or middlemen, play a role in mediating various aspects of life for members of the ultra-Orthodox community, including healthcare. Though usually having no formal medical education, askanim advise members of the community concerning medical treatment and are viewed as a source of authority (Orr, Unger, and Finkelstein 2021b; Taragin-Zeller, Rozenblum, and Baram-Tsabari 2022; Zalcberg Block and Zalcberg 2023).
Many ultra-Orthodox men learn full-time in yeshivot (yeshiva, sing.), schools of religious studies, and do not enter the labor force or academia. Compared to men, more ultra-Orthodox women obtain higher education and participate in the labor market, but on average, their salaries are lower than those of non-ultra-Orthodox employees (Malach and Cahaner 2022). Since participation in the labor market among ultra-Orthodox men is relatively low, and ultra-Orthodox families, on average, are larger and have lower income, there is an overrepresentation of ultra-Orthodox Jews living below the poverty line (National Insurance Institute of Israel 2023).
Poverty is one of the social determinants of health in the ultra-Orthodox society. There are many other sociocultural barriers to health in this society. For example, the ultra-Orthodox population is characterized by low levels of health-promoting behaviors such as physical activity (especially among men) and low awareness of healthy nutrition, which lead to high prevalence of obesity, diabetes, and anemia (Gershoni, Gilboa-Feldman, and Spitz 2023; Leiter et al. 2022; Zalcberg Block and Zalcberg 2023). Furthermore, certain diseases and disabilities are highly stigmatized and may be concealed and undertreated (Gershoni et al. 2023; Orr et al. 2021a; Pikkel and Gershuni 2023). Ultra-Orthodox persons care for large families, leaving little time for self-care and adequate sleep (Leiter et al. 2022). Their minimal exposure to the mainstream media limits their exposure to major health information sources, particularly for women, and their health literacy (Leiter et al. 2022). Moreover, there is a religious prohibition on selective abortions and a limited use of prenatal diagnosis, which lead to high prevalence of health conditions that can be detected during pregnancy (Gershoni et al. 2023).
Despite these sociocultural barriers, health indicators show that ultra-Orthodox have lower mortality rates and better health overall than the general Israeli population (Chernichovsky and Sharony 2015; Pinchas-Mizrachi, Zalcman, and Shapiro 2021). Possible explanations are the increased social and psychological resources in the ultra-Orthodox society (Pinchas-Mizrachi et al. 2021); the beneficial effects that religious attendance has on health behavior (Jung 2022); strong familial relationships; a high level of communal engagement, support, and assistance, including during times of illness, which is manifested in a developed network of charity organizations; a lower rate of smoking; and an extensive use of medical services (Gershoni et al. 2023). Overall, the ultra-Orthodox society is characterized by a high social capital that positively affects many health-related aspects of life (Chernichovsky and Sharony 2015). These findings align with the findings on better self-reported health among other high-cost religious groups that are theologically, socially, and culturally exclusive (Scheitle and Adamczyk 2010).
It is important to note that ultra-Orthodox Jews are not a monolith. There are numerous ultra-Orthodox streams, groups, and sub-groups, which differ from one another in certain aspects of religious practice and belief (Caplan and Leon 2023). The ultra-Orthodox population in Israel can roughly be divided into three main streams: Hasidic, Lithuanian, and Sephardic, each makes up around one third of the ultra-Orthodox population (Engelman et al. 2020; Friedman 2021; Shomron 2022).
Disaffiliation from Ultra-Orthodox Judaism and Other Religious Communities
In Hebrew, ultra-orthodox disaffiliates are known as yotzim beshe’elah, meaning leaving in question. Researchers suggested several reasons why someone from the ultra-Orthodox community would disaffiliate. A prominent reason pertains to questions surrounding their faith and religious lifestyle. For example, in the study of Davidman and Greil (2007) one disaffiliate explained that she could not understand the ways she was taught, and had so many questions she knew she could not ask. Another reason for disaffiliating is criticism toward the ultra-Orthodox community and its institutions. For instance, female disaffiliates felt restricted by and criticized the unequal and discriminatory gender roles (Davidman and Greil 2007). Many disaffiliates described a desire for greater personal autonomy, freedom, and non-religious knowledge. For example, they were inspired by secular books they have read and wanted to learn more (Davidman and Greil 2007). Other reasons include the burden of expectations for ultra-Orthodox individuals; feeling of alienation from the community that prioritizes religion over individual needs; and trauma and victimization, including sexual abuse (Heymann 2015; Horowitz 2018; Miles et al. 2023; Newfield 2020).
Ultra-orthodox disaffiliates face many challenges, some of which are similar to those of new immigrants (Berger 2014; Engelman et al. 2020). They need to adjust to new societal rules and usually lack basic education and skills needed to survive and thrive in the non-ultra-Orthodox world, including how to interact with the opposite sex (Berger 2015). Exacerbating the challenges of this transition, they are also often rejected by their families and former communities (Berger 2014; Shenfeld 2015).
Doron (2013a) showed that ultra-Orthodox disaffiliates often find themselves in a prolonged liminal position, the state of being in-between opposing worlds. Many of them are isolated both from the family, friends, and community they have left, and from the secular society that does not help much in their absorption. This finding aligns with quantitative studies on other groups of religious disaffiliates. These studies found that after disaffiliation, a religious residue persists, and disaffiliates differ both from never religious and currently religious individuals in cognitive, emotional, and behavioral processes (Van Tongeren, DeWall, Chen, et al. 2021). Disaffiliates’ endorsement of moral foundations lies between the never religious and currently religious individuals (Van Tongeren, DeWall, Hardy, and Schwadel 2021). For ultra-Orthodox disaffiliates, the constant liminality has a prominent bodily dimension, given that “Jews are as much a ‘people of the body’ as of the book” (Kasstan 2019:2). The hundreds of ultra-Orthodox bodily inscribed, habitual routines and rituals, which have been central to the lives of disaffiliates as ultra-Orthodox individuals, typically remain with them even after they exit the ultra-Orthodox community (Davidman 2020; Newfield 2020).
Data measuring the extent of disaffiliation in Israel are limited, making it hard to quantify the phenomenon and adding subjective biases to data collection. This is partially because some disaffiliates may eventually “return” to an ultra-Orthodox lifestyle (Horowitz 2018). Based on data from surveys conducted by the Central Bureau of Statistics, however, 10% of ultra-Orthodox adults reported that they disaffiliated, and among adults between the ages of 20 and 40, 7.8% reported that they disaffiliated (Shenfeld 2015). According to Weinreb, 15% of the ultra-Orthodox population disaffiliate (Shtarkman and Georgy 2023). A study by “Out for Change,” an organization that supports disaffiliates, found that 3,500 ultra-Orthodox individuals disaffiliate annually and 16,300 disaffiliated between 2018 and 2022 (Deutsch et al. 2022). This figure includes many ultra-Orthodox disaffiliates who continue to be religious after disaffiliating, choosing a modern Orthodox or traditional (masorti) lifestyle rather than a secular one (Deutsch et al. 2022). The rates of disaffiliation seem to increase in recent years (Regev and Gordon 2021).
Studies indicate that this population faces clear health risks. Disaffiliation can leave a person with a reduced capacity to cope with stress and is associated with poorer overall well-being compared to their religious counterparts (Engelman et al. 2020; Fenelon and Danielsen 2016). A significant minority report depression and anxiety (Berger 2014; Horowitz 2018; Velan and Pinchas-Mizrachi 2019). Possible reasons for these findings include the loss of community and social support (Fenelon and Danielsen 2016), in addition to the well-established finding that religious individuals have better health outcomes compared to non-religious individuals (Pinchas-Mizrachi et al. 2021; Sullivan 2010). Moreover, since some religions dictate certain health behaviors, those who disaffiliate may no longer subscribe to these health behaviors (Upenieks and Schafer 2020). Additionally, disaffiliates may engage in risky behaviors once they leave, resulting in poorer health.
Scheitle and Adamczyk (2010) found that people who disaffiliate from high-cost religious groups are more likely to report worse health than those who disaffiliate from other groups. For people who exit high-cost, encompassing religious communities, disaffiliation includes an inherent conflict, role loss, and perceived threats to self-identity, which catalyze psychological distress and reduce well-being, followed by a lifetime process of reconstruction and role-identity reset (Haire 2022; Nica 2020; Ransom, Monk, and Heim 2022). For example, disaffiliates from high-cost religious groups in Finland experienced a social identity crisis that led to physical and mental health problems requiring in-patient and out-patient nursing care as well as psychotherapy. Simultaneously, participants described many positive aspects of life after disaffiliation, experiencing freedom, relief, joy, gratitude, and empowerment (Björkmark, Nynäs, and Koskinen 2022). In other cases, the condition experienced by disaffiliates was described as distinct from other mental health disorders, constituting a unique “cultural syndrome” (Brooks 2020).
The increased vulnerability and the liminality of ultra-Orthodox disaffiliates necessitate maximal access to healthcare and minimizing any barriers to healthcare they may face. However, not much is known about these barriers and their implications for practice. The objective of this study is to identify the barriers that hinder the access to the healthcare system by ultra-Orthodox disaffiliates. Identifying these barriers will allow the healthcare system and practitioners to better address them and provide more equitable care to disaffiliates.
Data and Methods
The study relied on interpretative phenomenological analysis to guide the data collection on the lived experiences of disaffiliated young adults who grew up in ultra-Orthodox homes (Eatough and Smith 2017; Smith, Jarman, and Osborn 1999). In keeping with this methodological approach, in-depth, semi-structured interviews were designed to invite participants to share personal accounts and interpretations of their life experiences, focusing on health issues and access to healthcare in relation to the process of moving away from their community of origin (Smith and Fieldsend 2021).
Study Participants and Setting
As reported in Pinchas-Mizrachi and Velan (2022), interviewees were recruited with the assistance of several organizations that help disaffiliates, including “Out for Change,”“Hillel,” and others. After a first set of individuals were contacted, recruitment continued using a snowballing approach in which interviewees recruited other people for the study. The final sample was comprised of 24 males (22–34 years old) and 12 females (20–29 years old), for a total of 36 participants. Inclusion criteria were: disaffiliating from an ultra-Orthodox community 1 to 10 years prior to the interview, studying in an ultra-Orthodox educational institution at least until the age 18, and choosing a secular lifestyle after disaffiliation. Since most disaffiliate at a young age, the year criterion resulted in a relatively young age range of participants. Partially because of this age range, most participants (n = 23) were single. Ten participants were divorced, most of whom divorced following their disaffiliation, and three were married or in a relationship. Nine participants were parents (had one or two children). Participants disaffiliated between the ages of 18 and 29. Most participants (n = 30) were Ashkenazi, that is, descended from European Jews, of which half were Hasidic and half were Lithuanian. The rest (n = 6) were Sephardic or mixed. All but two participants grew up in Jerusalem and Bnei Brak, the two cities with the largest ultra-Orthodox populations in Israel.
All participants received an explanation as to the aims and methods of the study and signed an informed consent form, in addition to providing an oral consent. The ethics committee of Ramat Gan Academic College approved the study in November 2018 (approval number 1318).
The 54 to 120-minute interviews took place in Hebrew between November 2018 and March 2021. Thirty interviews were conducted at the interviewers’ offices in Ramat Gan or Jerusalem or at nearby coffee shops (based on the preference of the interviewee). Due to the Covid-19 pandemic, six interviews were conducted over Zoom. The interviews were recorded, transcribed verbatim, and translated from Hebrew into English by a professional translator. The recordings were stored securely on the researchers’ work computers. (For more information on the participants, please see Appendix 1).
Analysis
After the interviews were transcribed, thematic analysis was conducted to identify significant and recurrent themes in the data that represent common experiences among the participants (Braun and Clarke 2022). We used two simultaneous methods: the first was a manual method conducted by the researchers; the second utilized Atlas software. The two methods yielded very similar results.
The analysis included several stages. First, following a holistic reading of the raw data, each transcribed interview was inductively coded, yielding lists of 20 to 30 statements per interview related to accessing healthcare. Second, in an open coding, we created initial thematic categories. Each researcher classified these themes individually. In most cases, the classification was similar; in the few instances where the classification differed, a discussion to resolve differences ensued. As described in Orr et al. (2023), we subsequently identified connections between the initial categories, refined them, and combined similar categories. We finalized six core categories that comprised the meaningful thematic clusters around which we organized the findings (Corbin and Strauss 2014). Finally, after we formed the conceptual descriptions and explanations, we reread the raw data to confirm that the analysis did not depart from the data.
Trustworthiness
To ensure the trustworthiness of this qualitative study, the research team took steps to support the following aspects of trustworthiness: credibility, transferability, dependability, and confirmability (Lincoln and Guba 1985; Shenton 2004). For the credibility aspect, the research was conducted utilizing accepted qualitative research methods. Furthermore, we developed early familiarity with the culture of participants by consulting with organizations that assist disaffiliates, and these organizations helped us contact potential participants, enabling us to gain their trust. We applied triangulation by use of a relatively large sample size for a qualitative study as well as recruitment from a number of organizations. Transferability of this study was strengthened by providing robust context to the phenomenon being studied, as well as methodological information such as the data collection methods, that enable other researchers to compare or replicate our work. Dependability was addressed by the utilization of two analysis methods and conducting the open coding simultaneously and separately by several researchers. Furthermore, peer-debriefing was applied by sharing findings with researchers who did not conduct the interviews. Finally, confirmability was supported by basing findings solely on this study’s data, collected from a relatively large sample, to prevent investigator bias.
Results
Analyzing the transcripts from the interviews, we identified six common themes related to barriers to the access of healthcare. These include barriers related to the disaffiliates’ current life situation, such as poverty, as well as barriers related to their upbringing in the ultra-Orthodox community.
Lack of Health-Related Education and Knowledge of the Healthcare System
Some of the disaffiliates explained that ultra-Orthodox education places great value on health, as a religious commandment.
We were raised on [the commandment] “Take therefore good heed to yourselves.” In the ultra-Orthodox world, if someone is sick, he won’t try to save [money, instead] he’ll go to the best doctor and find a way to pay for it. (Participant 4, male, age 34)
However, disaffiliates also stated that despite this commandment, they were not given any health-related information at home or in ultra-Orthodox schools, which do not place a strong emphasis on secular education. Boys, in particular, were sent to yeshivot, where the majority of the learning revolves around Judaic studies. There are very little secular subjects taught, such as English, mathematics, or science, in yeshivot. This means that ultra-Orthodox men (and to a lesser extent women, as they do receive a basic secular education, though it is censored) have little scientific literacy (Keller et al. 2023; Taragin-Zeller et al. 2022). The interviewees, particularly the young men reflecting on their education, remarked on their lack of understanding of the medical world.
An ultra-Orthodox boy does not know how to manage his life, not even the world of healthcare. Knowledge of the outside [secular] world, including the world of health, is considered to be a negative thing. (Participant 24, male, age 26)
This low health literacy was also evident in relation to the outbreak of the Covid-19 pandemic.
Everyone is talking about this virus and what happens if it comes to the country, but I don’t really know what a virus is. No one ever taught me, how am I supposed to know? (Participant 34, female, age 28)
Further complicating this, disaffiliates do not have personal experience in actively accessing the healthcare system. The ultra-Orthodox are more likely to seek the advice of a rabbinic figure or an askan before approaching a physician or other healthcare provider (Taragin-Zeller et al. 2022; Zalcberg Block and Zalcberg 2023). This translates to limited knowledge of the healthcare system.
The second you leave, you’re lost, health-wise. You no longer have askanim to help you make appointments or give you advice. You’re no longer there. (Participant 32, male, age 30)
Oftentimes, parents preferred to help their children with any encounter with the healthcare system, which was perceived as part of the outside, secular world. As a result, many participants had very limited direct contact with healthcare providers before disaffiliation.
Actually, I did not know any secular people. As a girl, I think the first time I saw secular people was at the health clinic. I was hospitalized when I was 10, and all the contact with the doctor was through my mother and grandmother. In general, I think it’s like this in the ultra-Orthodox world, especially among boys. (Participant 33, female, age 22)
This community and family support does no longer exist after exiting the ultra-Orthodox society, resulting in lack of essential knowledge of the healthcare system.
Poverty and Structural Determinants of Health
Participants told us about different problems that are considered social and structural determinants of health, such as poverty and lack of health insurance. For example, many disaffiliates stated that after disaffiliating and disconnecting from their families, they were unaware that they needed to register themselves to one of the health maintenance organizations in Israel as well as pay for it.
Naturally, until a person disaffiliates, the parents pay [for health insurance], and then when he decides to disaffiliate, he is disconnected from the family, and the father will stop paying his insurance, and the son doesn’t have any health insurance. (Participant 9, male, age 27)
All interviewees noted the poverty they struggled with when they first disaffiliated. Some saw this as a potential barrier to their ability to access the healthcare system, noting that they were more concerned with making a living first, and only then trying to figure out how to navigate the healthcare system (Pinchas-Mizrachi and Velan 2022).
At the beginning of my journey, I was really lost, at a survival level. I wasn’t always sure where I would be sleeping the next night. I was doing any and every job I could. I didn’t have time or headspace to deal with my health problems and it was terrible. (Participant 32, male, age 30)
Additionally, poverty further manifested as an inability to access private healthcare to shorten the wait times for treatment. While Israel has universal healthcare, supported by a health tax, to get any services or care outside the government-defined package of benefits, one must pay for additional coverage.
You know that an appointment to a psychiatrist in the public health clinic can be months away. If you have money, or if someone gives you money, you can go privately, and get better and faster treatment. But we don’t have money. (Participant 31, male, age 29)
Even after a disaffiliate has the resources to pay for private treatment, some disaffiliates explained that the feelings of poverty accompany them for many years.
Currently, I’m functioning well, I work, I earn, I have a car, a house, everything, but it is still something that accompanies me. I save every day, even without realizing it, just in case… That is to say, I’m always anxious. (Participant 4, male, age 34)
Lack of Respect for Authorities
A desire to break with convention and difficulty following instructions was common among disaffiliates. From their perspective, they were raised in a closed society where they were expected to obey everyone—their parents, teachers, and rabbis. After disaffiliating, many described having no will or reason to respect or heed advice from authority figures, to the extent of ignoring the advice of doctors and other healthcare providers, who are unrelated to the closed society from where they came.
If God can’t tell me what to do, you want me to listen to a doctor? (Participant 11, male, age 28)
Even if a disaffiliate does turn to the healthcare system for treatment, the disaffiliate may also have issues with compliance with treatment. Participants explained that this is their reaction to the extreme obedience characterizing the ultra-Orthodox society.
You grow up in a place where they tell you what to do and you do it. It’s big brother; parents and the rabbis will tell them what to do and everyone does what they’re told. (Participant 18, female, age 29)
However, the disaffiliate has been branded a rebel, and as someone who breaks with community norms. This manifests in the disaffiliate going to the extreme in the other direction from what he was told, after finally breaking out of the ultra-Orthodox community.
The disaffiliate breaks off from God and mom and dad, and the whole family, and from what everyone has been telling him what to do his entire life. They said not to eat unkosher [food], we’ll only eat unkosher [food]; we break all the rules. (Participant 24, male, age 26)
Communication Gaps
The communication process between the healthcare provider and the patient includes both verbal and non-verbal communication, such as behavioral codes, dress, and body language. Disaffiliates shared that they were lacking knowledge related to both verbal and non-verbal language, and this was a significant barrier to care.
A guy goes out into a foreign society, he doesn’t know their codes. Likely when he goes to the doctor, he will be unable to express himself. (Participant 21, male, age 29)
Even among disaffiliates who adopt new dress codes and body language, our study found that the effects of years of modesty education were still prevalent. As a result, there is a risk that a caregiver may read body language incorrectly. This can create disparities in the dialog between the disaffiliate and the provider, who may expect the disaffiliate to be comfortable discussing certain topics and undergoing standard internal exams based on how he or she presents herself.
No one told me to look down, but this is something I’ve been doing since I was a little girl. It’s not accepted here [in the secular society] and is even considered rude. (Participant 16, female, age 25) Up until a year ago, I was an ultra-Orthodox girl going out on prearranged dates [for marriage matches]. How can I go alone to a gynecologist and tell him, and get undressed? (Participant 17, female, age 29) With all the modesty rules, there is a tendency to protect personal privacy among disaffiliates. It’s harder for them to expose themselves during treatments and check-ups. (Participant 30, male, age 31)
The participants expressed their difficulty in sharing feelings with providers, due to cultural norms from the ultra-Orthodox community, where they were discouraged from sharing their feelings, particularly related to mental health.
He comes to the psychologist and doesn’t understand what to say, what can he expose? It’s really hard to share. The education we received at home really closes you off. (Participant 24, male, age 26) At our house, we didn’t talk about our feelings. I’m pretty sure I’m not the only one. In the ultra-Orthodox society, we don’t share, especially not about our feelings and especially not to strangers. (Participant 21, male, age 29) Professionals need to be trained, especially those in mental health, so they understand our issues. They should know it’s hard for us to open up. We’re pros at being mute. (Participant 11, male, age 28)
Finally, there is a language gap with disaffiliates. They will frequently use words not known or commonly used in the secular society. For instance, the Ashkenazi ultra-Orthodox community will frequently use Yiddish in everyday conversations. The interviewees addressed both their lack of understanding of secular language, and the inability of the secular society to understand their language, which can impede their ability to communicate with providers.
Even if he does speak, his terminology is different. So, he may not know how to explain himself to the provider. (Participant 32, male, age 30) It’s like being a new immigrant, but no one knows you’re a new immigrant. You look Israeli, you dress Israeli, and you speak Hebrew, but you’re not really. (Participant 26, female, age 26)
This and other participants emphasized that the providers’ expectations from a disaffiliate patient are identical to their expectations from any secular patient, while the disaffiliate feels and communicates differently.
Lack of Belonging
Participants reported feeling that they do not belong in any world—neither the secular world nor the ultra-Orthodox world.
He’s in a world he really doesn’t know, not really a part of. It’s this constant separation, your body may be physically playing soccer but it’s not really there, doesn’t feel part of it. So how can he open up about things this way? (Participant 28, male, age 23) At least at the beginning of my journey, I felt that no one really cared about me. My family really didn’t care. I mean, I guess if I were dead, they would search for the body to ensure a Jewish burial, but not more than that. You’re really alone with all of your problems. (Participant 32, male, age 30)
Some interviewees raised the issue of the difficulty in seeing an ultra-Orthodox or even a modern Orthodox provider. Others remarked that they had a harder time opening up to secular physicians who are unfamiliar with the ultra-Orthodox community, and even disparage it.
On the one hand, I don’t want an ultra-Orthodox doctor, or even a modern orthodox one. I don’t want to be judged. But someone secular, who doesn’t know our world can also be a problem. (Participant 23, female, age 28) I got Covid-19 and went to the hospital. There were ultra-Orthodox men in the room and a doctor comes in and spoke so condescendingly to them. I never thought I would defend ultra-Orthodox people, but I was so angry at him. I’m not ultra-Orthodox now, but there are some good things in that community. We weren’t raised on trees. (Participant 36, male, age 29)
Some disaffiliates defined characteristics of a caregiver who makes them feel safe. This was primarily a caregiver of the same sex, likely due to the modesty education with which they grew up. A female participant said: It doesn’t matter what treatment; I always prefer a woman. Not just a gynecologist. I’m sure that boys who grew up in yeshiva prefer a man. (Participant 16, female, age 25)
Stigmas
The interviewees described the health-related stigmas with which they were raised as a barrier to accessing healthcare. In particular, disaffiliates stated a fear of words that begin with ‘psycho’, due to stigmas of mental health that prevail in the ultra-Orthodox society.
The disaffiliate, who was raised on that stigma, is terrified of going to a psychologist. (Participant 1, male, age 25)
Furthermore, disaffiliates fear that their family will be judged in the ultra-Orthodox community, and marriage matches for their siblings, which partially rely on familial connections, will be tainted.
Is it not enough that I hurt my siblings’ marriage matches by disaffiliating, I will hurt them even more by being crazy? (Participant 11, male, age 28) During the matchmaking process, people also inquire about diseases in the family. If one of the children has a medical problem, even a small one, it can hurt their siblings’ chance of a good match. If the parents or any of the siblings have any mental health issue, then the chances of getting a good match are even lower. (Participant 27, female, age 29)
Therefore, the privacy of a disaffiliate is of utmost personal importance. The stigmas on which he or she was raised may cause them to feel that if people were to know about their poor well-being, they may judge, and it may hurt their future or the future of their ultra-Orthodox family members, especially younger siblings. This fear may prevent them from seeking care.
You are more concerned that someone may find out, than you are that you won’t get help. (Participant 17, female, age 29)
Discussion
This qualitative study examined the experiences and views of young adults who disaffiliated from the Israeli ultra-Orthodox community, focusing on their ability to access healthcare. Overall, disaffiliation was described as a complex and taxing process associated with reduced mental well-being, communication gaps, and lack of respect for authority, all of which need to be considered when providing care to disaffiliates. A better understanding of disaffiliates’ background and beliefs should increase sensitivity and awareness of potential differences that may pose barriers to access (Gulliford et al. 2002).
Many disaffiliates report poorer overall well-being and experience loneliness, depression, isolation, fear, alienation, excommunication, sense of danger, poverty, and lack of knowledge of secular social norms (Davidman 2015; Levi-Belz and Yalon 2023; Nadan et al. 2021). Disaffiliates come from a society where the community is central and families are large (Malach and Cahaner 2022). Studies have shown that social capital gained by participating in a community can lead to better overall (subjective) health status (Lim 2016). It is not surprising, then, that disaffiliates who lose their original social capital and have a hard time creating new social capital as they adjust to secular life may suffer from poorer overall health (Pinchas-Mizrachi and Velan 2022).
Participants indicated a lack of knowledge related to the healthcare system. In the ultra-Orthodox community, many depend on askanim and rabbis to advise them how to proceed with healthcare decisions. As a result of this dependency, when the disaffiliate must fend for him or herself in relation to healthcare, they are at a loss of how to do so (Taragin-Zeller et al. 2022). This problem is especially prominent among men, who received less secular education than women, in keeping with the finding of Keller et al. (2023) that men reported adverse education experiences at a significantly higher rate than women. Moreover, while the lack of scientific, health-related knowledge is common to both ultra-Orthodox people and disaffiliates, healthcare providers usually know to accommodate to the unique background of ultra-Orthodox, who are visibly recognized as such, whereas disaffiliates do not have any external marker that allows healthcare providers to recognize and be sensitive to their cultural background and accommodate treatment. Furthermore, participants exhibited a lack of respect for authority figures, such as healthcare providers. This lack of respect may stem from their desire to gain a sense of autonomy and independence as the catalyst for their leaving (Berger 2015). It may also stem from their strong self-reliance, which they need in order to survive and thrive outside their insular communities, and their individualism. Thus, disaffiliates have no desire to rely on healthcare professionals as it relates to their health and well-being (Velan et al. 2022).
Communication is a vital aspect in encouraging access to care. The disaffiliates’ lack of knowledge of accepted terminology, as well as their use of “old” terminology from their former lives may lead to miscommunication between disaffiliates and providers. Disaffiliates may not be able to amply describe issues they are experiencing, or exhibit or be comfortable with accepted non-verbal cues for the non-ultra-Orthodox society. Being uncomfortable around ultra-Orthodox or even modern Orthodox clinicians for fear of being judged is another aspect related to the provision of care that must be considered. Disaffiliates pay a high price for leaving their community in lost social support, among other challenges (Berger 2014). Therefore, they may be reluctant to put themselves back in a situation in which they feel judged by someone from their former community for their current life choices. Participants also discussed the issue of privacy, and of the need to make sure that no one knows they need care, particularly for mental health issues. The interviewees stated their fear of being judged by others due to seeking care. It is of the utmost importance for providers to maintain a safe environment for disaffiliates in order to encourage them to engage and continue engaging with the healthcare system.
Providers must also take care to be sensitive to the preexisting beliefs, stigmas, and learned prejudices with which disaffiliates grew up. In particular, the field of mental health is more stigmatized among the ultra-Orthodox than among secular populations (Orr et al. 2021a), with members of the ultra-Orthodox community less likely to openly seek care for fear of bringing shame on their family (Greenberg and Witztum 2013; Rosen et al. 2008). It is not surprising, then, that disaffiliates, even after leaving, are reluctant to seek mental healthcare. This finding aligns with previous studies that show that the former identity of disaffiliates is not abandoned entirely (Doron 2013b; Faulkner 2017; Van Tongeren, DeWall, Chen, et al. 2021) and therefore should not be overlooked by healthcare and welfare professionals. These issues demonstrate that disaffiliates have sociocultural and personal barriers related to the access of healthcare. Providers who care for this population should be aware of these gaps in order to ensure that the provided care is suited to their unique needs.
Limitations
There are several limitations of this study, chief among them possible sampling biases. First, the use of snowball sampling may mean that our sample is not representative of all disaffiliates. Furthermore, our study only included disaffiliates from one sect of Judaism and did not include other disaffiliated Jews, or other religions, nor did it include disaffiliates who chose a modern Orthodox or traditional lifestyle rather than a secular one. These disaffiliates may have different experiences in accessing the healthcare system. Moreover, most of our participants are either single or divorced, and married disaffiliates may have other experiences.
Additionally, most participants are Ashkenazi who grew up in two cities with large ultra-Orthodox populations; there may be differences in the experiences of disaffiliates from Sephardic communities and smaller cities or communities. Our participants were young adults (20–34 year-old) who disaffiliated at a young age (18–29), and their experiences may not represent those of older people who disaffiliated at an older age. Likewise, our sample has overrepresentation of men. However, more ultra-Orthodox men than women disaffiliate. Finally, the interviews took place before and during the Covid-19 pandemic. Changes that have occurred following the pandemic should be explored in future research.
Conclusion, Implications, Recommendations
The healthcare system is a focal point where state, religion, medicine, and health are intertwined and negotiated (Ivry 2010; Kasstan 2022). According to Kasstan (2019), for ultra-Orthodox Jews in England, healthcare constitutes a borderland through which multiple and sometimes opposing understandings of bodily governance and care come into contact. Our findings indicate that for ultra-Orthodox disaffiliates, healthcare continues to constitute a borderland between oft-incompatible sociocultural worldviews even after disaffiliation. The liminality of disaffiliates (Doron 2013a; Van Tongeren, DeWall, Hardy, and Schwadel, 2021) adds another layer to this complexity, forcing disaffiliates to navigate multiple contradictions related to body and health when accessing the healthcare system.
This study has shown that disaffiliation among ultra-Orthodox young adults is associated not only with unique health needs, but also with special sociocultural challenges to accessing healthcare. Their backgrounds affect how they approach care, how they decide to receive care, from whom they are willing to receive care, and how they view the role of a physician. We suggest that these findings are relevant also to other groups of people who disaffiliated from insular, encompassing, high-tension religious communities in other parts of the world, such as Mennonites, Amish (Faulkner 2017), Jehovah’s Witnesses (Ransom et al. 2022), and Mormon (Albrecht, Cornwall, and Cunningham, 1988; Brooks 2020; Hinderaker 2020). This relevance is evident despite substantial differences between the exit narratives of ultra-Orthodox and Christian disaffiliates (Davidman 2020).
The disaffiliates’ difference is externally invisible and therefore is usually disregarded by healthcare providers. To the extent that providers who care for the disaffiliate population are aware of their unique needs and concerns, they can begin to address some of their barriers to access. However, to date, healthcare providers do not receive any training to understand and address these needs and concerns, and consequently, they fail to address these barriers. We recommend incorporating a systematic, in-depth training in the curricula of medical schools, nursing schools, and other health professions schools, as well as in the continuing education of these professionals. Special courses that will be offered by organizations that provide healthcare services to disaffiliates, such as hospitals and health maintenance organizations, may also help health practitioners seeking to bridge cultural differences.
Moreover, the issues discussed in this article should be routinely integrated in cultural competency training for healthcare and welfare professionals. Cultural competency in healthcare is “the ability of systems to provide care to patients with diverse values, beliefs and behaviors, including tailoring delivery to meet patients’ social, cultural, and linguistic needs” (Betancourt, Green, and Carrillo 2002:v). Cultural competency improves providers’ communication and increases patient satisfaction, compliance, and healthcare access (Betancourt et al. 2002; Campinha-Bacote 2002; Schuster, Elroy, and Rosen 2018). In the past decade, the needs and challenges of ultra-Orthodox people in Israel have been increasingly acknowledged in the framework of culturally competent healthcare (Freund, Cohen, and Azaiza 2019; Genut et al. 2022; Orr et al. 2023). Yet, the needs and challenges of religious disaffiliates have been completely ignored in this framework. The disaffiliates’ barriers to access care presented in this article should become an element in cultural competency training programs in Israel and other countries. This will likely increase the knowledge and awareness of healthcare providers about disaffiliates and may even mainstream this issue in the healthcare system. In addition, services that are considered part of a culturally competent care, such as professional interpretation services, can be adapted and expanded to the needs of religious disaffiliates, with state funding and state regulation on their implementation.
Some of the barriers identified in this research are social and structural drivers of health and healthcare, such as poverty and access to public and private health insurance. Hence, we recommend incorporating these issues in future structural competency training. As described in Orr et al. (2023:3), structural competency refers to the health practitioners’ trained ability to recognize and address the upstream structural drivers of health, such as laws, public policies, and economic systems, and the ways they affect healthcare and create and perpetuate health disparities (Metzl and Hansen 2014; Neff et al. 2020; Orr et al. 2022). To date, this emerging conceptual framework, which has become increasingly prevalent in many countries, does not refer to religious disaffiliates, and we suggest adding this subject to structural competency training programs.
A key element in structural competency is critical consciousness and reciprocal collaboration and allyship between health practitioners and disadvantaged community members to foster equitable and inclusive policies (Grossman et al. 2021; Melino 2022). The trained health practitioners should collaborate with religious disaffiliates to promote structural changes, for example, changing state policies that do not support disaffiliates and their integration in society the way they support ultra-Orthodox or new immigrants, thus increasing their poverty and marginalization, adversely affecting their access to healthcare. Many disaffiliates are characterized by profound critical consciousness and can even partake in training healthcare providers. This collaborative work can also reduce providers’ burnout and apathy (Downey and Thompson-Lastad 2023).
Moreover, while health promotion programs address the specific health needs and health behaviors of religious minorities, including ultra-Orthodox (e.g., Leiter et al. 2020), similar programs for religious disaffiliates are lacking and can be developed by community organizations based on the six barriers found in this study. Such programs can include, for example, courses on the healthcare system, how to access it, and patient’s rights; workshops aiming to deconstruct stigmas in health and mental health; simulations on inter-personal communication, particularly with healthcare providers; peer guidance and mentoring from people who disaffiliated earlier, who will not be viewed as unwelcome “authorities”; individual consultation of a trained nurse or social worker on dealing with bureaucratic issues in the healthcare system, especially for those who do their first steps outside the ultra-Orthodox society; workshops focusing on peer learning and group support in health issues; self-advocacy and policy change activism in major healthcare organizations and governmental agencies that would leverage the disaffiliates’ strong self-reliance, independence, and critical perspective to promote systemic solutions to structural problems.
Thus far, we have begun to implement these suggestions in a small scale. We have incorporated these issues in the postgraduate curriculum of the Jerusalem College of Technology nursing school. Experienced nurses who graduated from this program have implemented these ideas in a local community-based organization for disaffiliates in Jerusalem called Hachazer Shel Yuda. We hope that these community-based initiatives would constitute a pilot for national programs in Israel and globally. Future directions may be to track if the health education training will help disaffiliates acclimate to the healthcare system more comfortably. We also recommend that future research build upon our study to examine these issues in diverse sociocultural contexts worldwide.
Footnotes
Appendix
Characteristics of Research Participants.
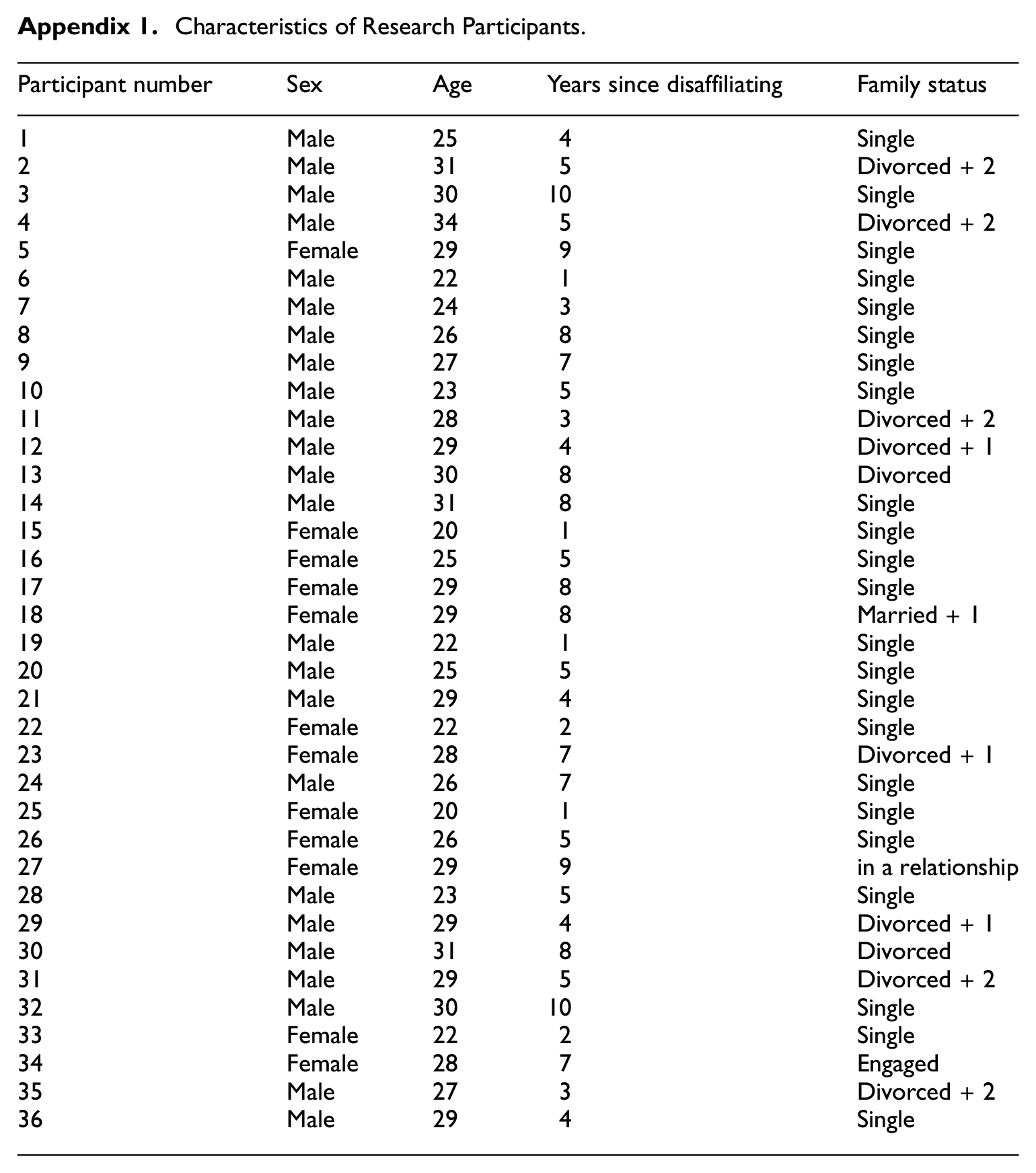
| Participant number | Sex | Age | Years since disaffiliating | Family status |
|---|---|---|---|---|
| 1 | Male | 25 | 4 | Single |
| 2 | Male | 31 | 5 | Divorced + 2 |
| 3 | Male | 30 | 10 | Single |
| 4 | Male | 34 | 5 | Divorced + 2 |
| 5 | Female | 29 | 9 | Single |
| 6 | Male | 22 | 1 | Single |
| 7 | Male | 24 | 3 | Single |
| 8 | Male | 26 | 8 | Single |
| 9 | Male | 27 | 7 | Single |
| 10 | Male | 23 | 5 | Single |
| 11 | Male | 28 | 3 | Divorced + 2 |
| 12 | Male | 29 | 4 | Divorced + 1 |
| 13 | Male | 30 | 8 | Divorced |
| 14 | Male | 31 | 8 | Single |
| 15 | Female | 20 | 1 | Single |
| 16 | Female | 25 | 5 | Single |
| 17 | Female | 29 | 8 | Single |
| 18 | Female | 29 | 8 | Married + 1 |
| 19 | Male | 22 | 1 | Single |
| 20 | Male | 25 | 5 | Single |
| 21 | Male | 29 | 4 | Single |
| 22 | Female | 22 | 2 | Single |
| 23 | Female | 28 | 7 | Divorced + 1 |
| 24 | Male | 26 | 7 | Single |
| 25 | Female | 20 | 1 | Single |
| 26 | Female | 26 | 5 | Single |
| 27 | Female | 29 | 9 | in a relationship |
| 28 | Male | 23 | 5 | Single |
| 29 | Male | 29 | 4 | Divorced + 1 |
| 30 | Male | 31 | 8 | Divorced |
| 31 | Male | 29 | 5 | Divorced + 2 |
| 32 | Male | 30 | 10 | Single |
| 33 | Female | 22 | 2 | Single |
| 34 | Female | 28 | 7 | Engaged |
| 35 | Male | 27 | 3 | Divorced + 2 |
| 36 | Male | 29 | 4 | Single |
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Research Division at Ramat Gan Academic College under Grant no. 2017-1.
Ethics Approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of Ramat Gan Academic College (Approval no. 1318) in November 2018.
Consent to Participate
Written and oral informed consent was obtained from all individual participants included in the study.
Availability of Data and Material
The research data is available but not shared. This study utilized qualitative data obtained via in-depth interviews with participants, who provided consent for data to be collected and used only by the researchers.
