Abstract
Objective:
Disease intervention specialists (DISs) play a crucial role in the public health workforce by conducting essential tasks such as contact tracing, contact interviews, and providing referrals for services to control disease spread. Despite the importance of DISs, research is lacking on the job tasks that they perform and the role that they serve in public health agencies. The objective of this study was to identify the unique skill sets of DISs relative to other public health occupations.
Methods:
We used a national dataset of job postings in the United States to conduct a comparative analysis of the skills required for 3 occupations: DISs, epidemiologists, and community health workers. We examined job listings posted from July 2022 through February 2023 to determine the frequency of certain skills, and we tested for significant differences in skill mentions across these occupations.
Results:
Job postings for DISs were significantly more likely than those for community health workers and epidemiologists to require expertise in areas such as case management (30%), communicable disease control (49%), infectious disease knowledge (33%), and disease prevention techniques (18%).
Conclusions:
This study highlights the specialized nature of DISs in managing disease-related public health interventions and supporting population health. Improved data collection is needed to support workforce planning, training, and policy development to ensure the continued effectiveness and reach of DISs in public health systems.
Disease intervention specialists (DISs) are often categorized as community health workers (CHWs) or epidemiologists in federal workforce studies because of the lack of a specific Standard Occupational Classification (SOC) code for their role.1,2 While DISs perform distinct and specialized tasks—such as case investigation, contact tracing, and patient counseling for communicable diseases—current federal workforce classifications fail to capture these unique responsibilities. 1 This misclassification not only obscures the true size and scope of the DIS workforce but also complicates efforts to assess workforce needs, salary standards, and growth projections specific to this profession. The objective of this study was to measure the differences in job tasks across DIS, CHW, and epidemiologist job postings and highlight the unique role of DISs in the public health workforce.
The Role of DISs in the Public Health Workforce
The DIS role was established in the 1930s under the FDR administration to prevent the spread of syphilis in the United States. 3 Former US Surgeon General Thomas Parran secured funding to implement a program focused on case investigation, free treatment, and health education for affected individuals. 3 Health departments deployed staff to follow up with diagnosed individuals, ensure that they received treatment, and trace their contacts and potential sources of infection. 4 DISs notified these contacts, helped them access care, and in turn helped to contain the spread of disease. Today, the DIS role is recognized as an essential component of public health, disrupting the spread of communicable diseases through targeted individual-level investigations.5,6 Most DISs are employed in state or local health departments, while some DISs work in private health clinics. 7 All 50 states and the District of Columbia have laws that authorize or require the investigation of sexually transmitted infections (STIs), and 67% of jurisdictions extend this requirement to other communicable diseases.8-10 Reported cases of certain diseases trigger the services of DISs, who have data collection skills that are invaluable in providing transmission data for health departments, especially during emerging health threats. 3
The modern definition of a DIS encompasses any public health worker who conducts disease intervention activities: person-centered interviews, enhanced surveillance, community assessment, partner services (including contact tracing), field investigation, directly observed therapy, specimen collection, outbreak response, community outreach, collaboration with medical providers, and navigation of health care systems to ensure evaluation and treatment for those diagnosed with or exposed to infectious diseases.4,9 Relevant program areas include STIs, HIV, tuberculosis, hepatitis, other outbreak investigations, and emergency preparedness and response.11,12
DISs often visit patients in their homes to interview them and identify their physical contacts. They provide a range of services and referrals, frequently bundling services such as syphilis tracing with HIV education and testing resources, preexposure prophylaxis, or connections to housing and food security resources.13-15 After an interview with an initial patient, DISs approach the identified contacts to inform them of their potential exposure, continuing the cycle of intervention and data collection. This work requires not only empathy and sensitivity but also a robust health vocabulary to convey complex laboratory results and treatment plans to patients with varying levels of health literacy. 13 As surveillance databases have expanded in scope and capability, DISs are increasingly required to input detailed interview notes to support case management and future disease investigations. This shift has reduced the time that specialists spend in the field while increasing the computer skills necessary to perform their duties effectively. 4
The objective of this study was to establish the unique role and skills among DISs in the public health workforce relative to CHWs and epidemiologists, 2 occupations that are most often conflated with DISs in workforce research. Limited understanding exists in the size and scope of the DIS workforce, and this research builds on prior studies of DIS job skills and their integration within public health agencies. In this study, we analyzed the skills listed in job postings for DISs, CHWs, and epidemiologists and tested for significant differences in skill frequency across these occupations. We drew on a large-scale vendor dataset of job postings, which allowed us to categorize postings by occupation and specified skills.
Methods
To assess and measure skills among DISs, CHWs, and epidemiologists, we conducted a study using data from Lightcast, a large-scale data vendor that “scrapes” (gathers) job postings from tens of thousands of sites and aggregates, deduplicates, and analyzes “between 6 and 8 million unique, active postings from more than 90 000 companies” each month.16,17 Deduplication is the process used by Lightcast to identify duplicate job postings; a job posting that had duplicate job postings was counted only once. 18 We conducted 3 separate searches of Lightcast on July 16, 2023, for jobs posted between July 2022 and February 2023: 1 search for job postings with the title “disease intervention specialist,” 1 for “epidemiologist,” and 1 for “community health worker.” Job postings for epidemiologists and CHWs included postings from all employment settings. Lightcast uses a list of >75 000 job titles; in general, job titles are what a person in a role is called. Lightcast uses machine learning tools and natural language processing tools to deduplicate job postings and to code job postings for “sequences of words that indicate skills”; then, it matches them to a “comprehensive taxonomy of more than 32 000 skills collected from hundreds of millions of job postings, resumes, and online profiles” to categorize skills. Skills describe the tasks and competencies expected in performance of the role.”16,17 Skills are organized into common skills (eg, communication, problem solving), which are typical among many occupations and include soft skills and competencies, and specialized skills, which are technical or hard skills that qualify candidates for certain subsets of occupations. We contrasted the skill requirements listed in job postings for DISs, CHWs, and epidemiologists.
We used the 2-sample proportions test (also known as difference-in-proportions test) to test differences in identified skills between DISs and CHWs and between DISs and epidemiologists. The test assessed whether the observed differences in proportions were unlikely to have occurred by chance alone. The test generated a P value, which indicated the probability of observing differences if there were no true differences between the groups. We considered P < .05 to be significant.
We conducted a secondary analysis to test the effect size of the difference between occupations, which we calculated by dividing the difference between 2 means by the pooled SD. The effect size analysis revealed the magnitude of the difference in skills across occupations to determine whether it was large enough to be meaningful. This method can be applied only after identifying significant values (ie, if P < .05). A large difference in percentage may mean substantial disparities in demand of this skill between the 2 occupations. We considered a small effect size to be 0.2, indicating that the difference in skill was minimal. We considered a medium effect size to be 0.5, indicating a meaningful difference that could have implications for job skills, requirements, or expectations. We considered a large effect size to be ≥0.8, indicating a substantial disparity between the groups and a distinct difference in job responsibilities. This study used data from job postings and was not human subjects research; therefore, the University of Minnesota Institutional Review Board considered the study to be exempt from review.
Results
The number of job postings included in the analyses were as follows: 389 unique job postings for DISs, 7003 for CHWs, and 1357 for epidemiologists. The most listed specialized skills for DISs were public health (51%), case management (30%), social work (29%), communicable diseases (49%), epidemiology (35%), and infectious diseases (33%) (Tables 1 and 2). The identified common skills were investigation (52%), communication (37%), management (28%), writing (25%), and planning (20%).
Difference in shared job skills between job posts for disease intervention specialists and community health workers, United States, July 2022 through February 2023 a
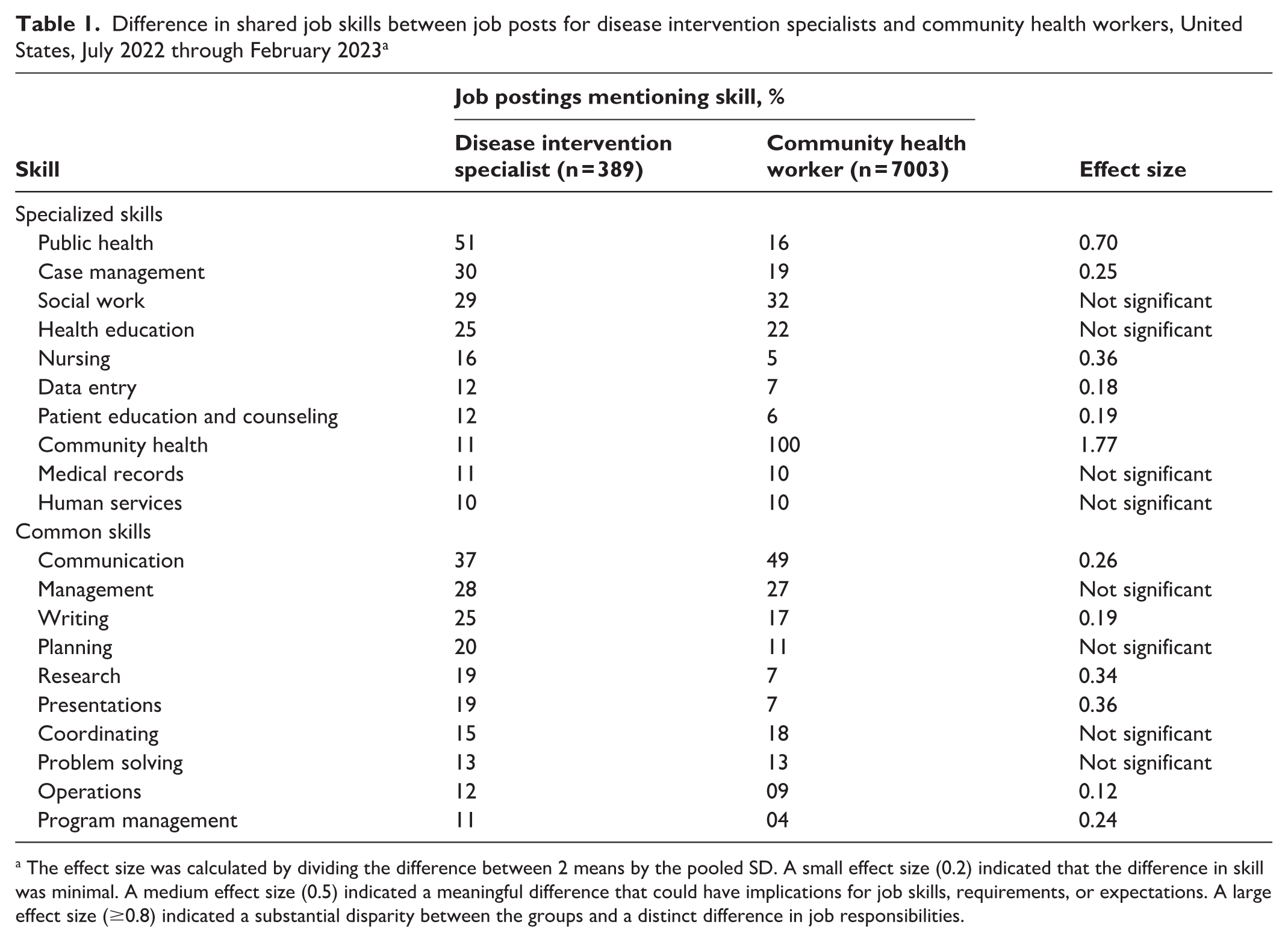
The effect size was calculated by dividing the difference between 2 means by the pooled SD. A small effect size (0.2) indicated that the difference in skill was minimal. A medium effect size (0.5) indicated a meaningful difference that could have implications for job skills, requirements, or expectations. A large effect size (≥0.8) indicated a substantial disparity between the groups and a distinct difference in job responsibilities.
Differences in shared job skills between job postings for disease intervention specialists and epidemiologists, United States, July 2022 through February 2023 a
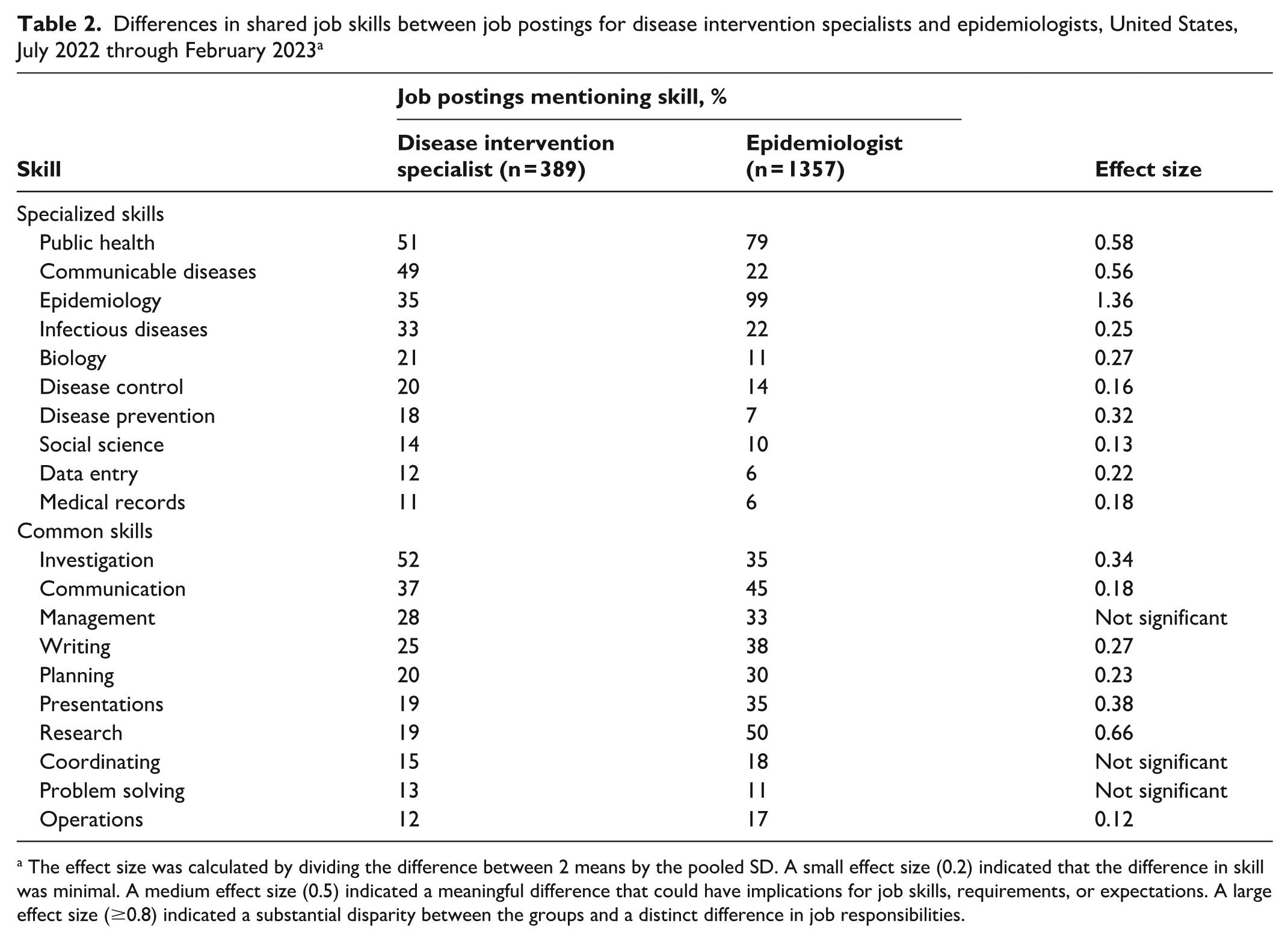
The effect size was calculated by dividing the difference between 2 means by the pooled SD. A small effect size (0.2) indicated that the difference in skill was minimal. A medium effect size (0.5) indicated a meaningful difference that could have implications for job skills, requirements, or expectations. A large effect size (≥0.8) indicated a substantial disparity between the groups and a distinct difference in job responsibilities.
Among specialized skills, DIS job postings were significantly more likely than CHW job postings to identify public health as a specialized skill (51% vs 16%; effect size, 0.75). Thirty percent of DIS job postings and 19% of CHW job postings listed case management as a specialized skill (P < .05; effect size, 0.25). Finally, DIS job postings were significantly more likely than CHW job postings to include the specialized skill of nursing (16% vs 5%; effect size, 0.36). Among common skills, DIS job postings were significantly more likely than CHW job postings to include research (19% vs 7%; effect size, 0.34) and presentations (19% vs 7%; effect size, 0.36).
Among specialized skills, DIS job postings were significantly more likely than epidemiologist job postings to identify communicable diseases as a specialized skill (49% vs 22%; effect size, 0.56). Among common skills, DIS job postings were significantly more likely than epidemiologist job postings to include investigation (52% vs 35%; effect size, 0.34). However, epidemiologist job postings were more likely than DIS job postings to include some skills, including public health and research.
Skills that we identified that were unique to DISs included activities involved in the prevention of sexually transmitted diseases, phlebotomy, risk reduction, infection, venipuncture, syphilis, contact tracing, auditing, laboratory testing, and prevention of HIV/AIDS (Figure). In general, skills that were unique to DISs focused on infectious diseases. Unique CHW skills focused on case management, care coordination, and community-based care, while skills that were unique to epidemiologist job postings focused on data analysis methods and software. Skills in DIS job postings that overlapped with skills in job postings for CHWs and epidemiologists included public health, data entry, medical records, community health, health risk assessment, and chronic diseases.
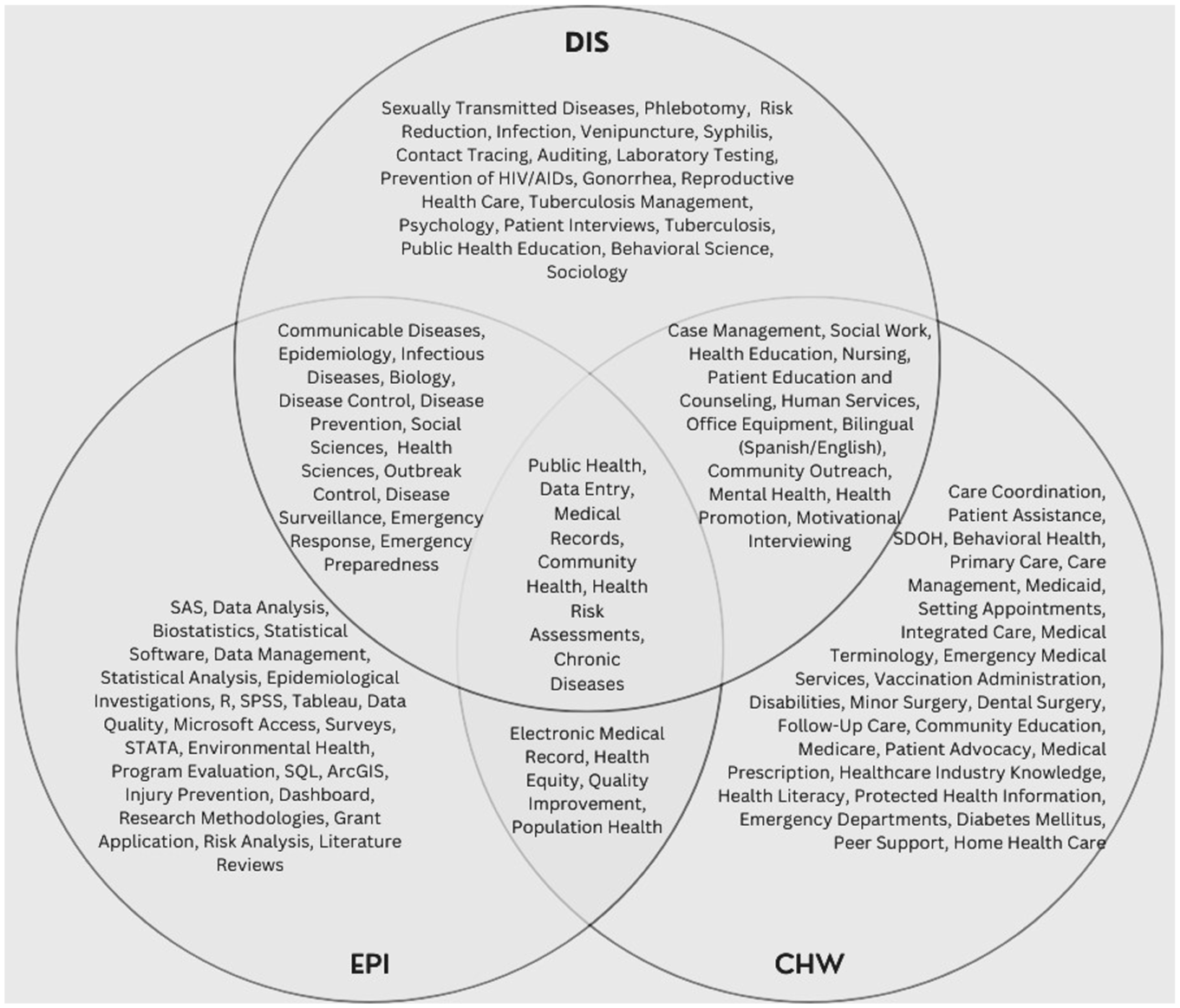
Venn diagram of job skills in job postings for disease intervention specialists (DISs), community health workers (CHWs), and epidemiologists (EPIs). The sample included 389 unique job postings for DISs, 7003 for CHWs, and 1357 for epidemiologists. Abbreviation: SDOH, social determinants of health.
Discussion
Our study demonstrates that DISs have a unique role in the public health workforce. Job postings for DISs focused on infectious diseases such as STIs, risk reduction, contact tracing, and HIV/AIDS prevention, while job postings for CHWs emphasized community-based care. Job postings for epidemiologists were distinguished by data analysis methods and software skills. In their focus on the prevention of infectious diseases, DISs contribute to reducing health disparities. As demonstrated during the COVID-19 pandemic, communities with low socioeconomic status were disproportionately affected by the pandemic.19-21 Low-income and medically marginalized communities have historically faced higher rates of disease incidence than populations with greater resources. 22 DISs are well positioned to support the Healthy People 2030 goals of reducing health disparities through infectious disease tracing and intervention in socioeconomically marginalized populations. 23 They play an essential role in the Foundational Public Health Services24,25 by investigating disease spread through contact tracing, contact interviews, and resource provision.
Policy Implications
The DIS workforce has a long history in public health, leveraging a unique set of skills to trace infectious disease outbreaks and limit disease spread. However, insufficient DIS support may leave state and local health departments struggling to deliver core public health services, such as disease surveillance, control, and prevention, and may constrain the capacity of public health departments to effectively intervene in the transmission of STIs. 4 Under the American Rescue Plan Act of 2021, the federal government allocated >$1 billion in new funding to support the DIS workforce. 25 Yet, much of the funding associated with the DIS workforce grant was rescinded in 2023. 26 Because of barriers in accurately identifying and measuring the DIS workforce in federal employment surveys, we are limited in our ability to measure the investment in the DIS workforce and the withdrawal of these resources. The US Department of Labor’s SOC system, which is used to categorize occupations for workforce projections, salary analysis, and occupational data, lacks a specific code for DISs. 1 As a result, DISs are often classified under various SOC codes that fail to fully represent their specialized work. Creating an SOC code for DISs would allow comprehensive workforce enumeration, facilitating the measurement of investment—and disinvestment—in the workforce.2,27
The rising incidence of STIs and other communicable diseases underscores the urgent need for a clear, standardized classification for DISs in the public health system. The Centers for Disease Control and Prevention’s (CDC’s) 2022 STI surveillance report indicated a 1.9% increase in overall STI diagnoses during a 5-year period, with alarming increases in syphilis and congenital syphilis cases (78.9% and 183.4%, respectively). 28 With each case of congenital syphilis, a child may need lifelong care and special education; preventing even 1 case of congenital syphilis can save thousands of dollars over time, making DISs well worth the investment. 29 Moreover, in 2022, an estimated 32 100 new HIV cases were reported in the United States. One of CDC’s 6 key indicators for ending the HIV epidemic is to increase awareness of one’s HIV status. 30 Currently, of every 100 people with HIV, approximately 13 do not know their status. 31 Maintaining the DIS workforce is a crucial step toward achieving CDC’s goal of 95% status awareness by 2025 because these specialists play a critical role in HIV prevention and early intervention efforts. 32
Conclusion
The role of DISs is indispensable to the public health workforce, especially in addressing communicable disease threats. Identifying and measuring the DIS workforce will strengthen the nation’s capacity to manage ongoing and emerging public health challenges. Improving the visibility of the DIS workforce and data accuracy will enhance the public health infrastructure.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project was supported by the Centers for Disease Control and Prevention and the Health Resources and Services Administration under awards U81HP47167 and UR2HP47371 (total amount $993 239).
Disclaimer
The information or content and conclusions of this article are those of the authors and should not be construed as the official position or policy of, nor should any endorsements be inferred by, the Centers for Disease Control and Prevention, the Health Resources and Services Administration, the US Department of Health and Human Services, or the US government.
