Abstract
Objectives:
Studies suggest that people experiencing housing insecurity and homelessness (HIH) have varying experiences with food insecurity. We estimated the prevalence of food insecurity and identified the factors associated with it among people experiencing HIH in the United States.
Methods:
We conducted a meta-analysis of the prevalence of food insecurity among people experiencing HIH and a systematic review of associated factors through a comprehensive search of 8 academic databases. We identified 3398 unique articles and included 40 studies in the review that met the following criteria: included observational or experimental data on the prevalence of food insecurity among people experiencing HIH, conducted in the United States, and written in English.
Results:
The overall prevalence of food insecurity was 57% (95% CI, 48%-65%). Most people experiencing HIH had food insecurity, and our estimated prevalence among people experiencing HIH was >4 times higher than the prevalence in the US population. Experiencing symptoms of a mental health condition (eg, depression, posttraumatic stress disorder, anxiety) in addition to HIH was most frequently (7 datasets) associated with increased odds of food insecurity. Social and institutional support was most frequently (5 datasets) associated with decreased odds of food insecurity.
Conclusion:
Our findings suggest that multisector coordination is needed to address individual- and system-level factors associated with food insecurity and HIH.
Individuals experiencing housing insecurity or homelessness (HIH) in the United States face numerous barriers to accessing basic needs. Conventional wisdom often conflates homelessness and food insecurity; however, people experiencing HIH have varying experiences with food access and adequacy.1-4 Housing insecurity exists on a continuum, with secure housing at one end and homelessness at the other end as the most severe form of housing insecurity. 5 Housing insecurity, as defined by the US Department of Health and Human Services, encompasses numerous challenges, such as difficulty paying rent because of cost (≥30% of income spent on housing), frequent moves (≥3 times in 1 year), and overcrowding (≥2 people in 1 room or multiple families in 1 house). 6 Homelessness is defined as “lacking a regular nighttime residence or having a primary nighttime residence that is a temporary shelter or other place not designed for sleeping.” 6 Food insecurity is defined as “uncertain or limited access to adequate food” and is considered a condition distinct from hunger.7,8 High rates of food insecurity may be expected among people who are experiencing HIH because not having a regular place to live may also result in not having regular access to food and having difficulty connecting with public assistance programs. How often these 2 issues overlap and how they might affect each other are unclear. Some homeless service programs offer food pantries and meal services, but many do not. 9
A scoping review that synthesized the relationship between food insecurity and mental health outcomes among people experiencing homelessness found an association between food insecurity and depression. 10 However, the review was limited to adults and was not a meta-analytic review; thus, a need exists for a broader review of the HIH population to estimate the prevalence of food insecurity and identify potential associated factors. The findings would provide consolidated information on this issue, establish prevalence numbers, and help provide potential interventions to help address food insecurity among people experiencing HIH in the United States.
Methods
This systematic review follows the Cochrane Handbook for Systematic Reviews of Interventions. We adhered to the PRISMA guidelines (Preferred Reporting Items for Systematic Reviews and Meta-analyses) and MOOSE reporting checklist (Meta-analyses of Observational Studies in Epidemiology) while considering best practices in systematic reviews of prevalence.11-14 We developed the protocol a priori and registered it with Prospero (CRD42023402438). Institutional review board approval was not necessary per institutional policy at the University of Texas Health Science Center because the review did not involve human data or participants.
For inclusion in the review, studies must have had information on (1) people experiencing HIH as defined by the US Department of Health and Human Services and (2) the prevalence of food insecurity as defined by the US Department of Agriculture, with food insecurity as the numerator and HIH as the denominator.6,8 Multiple tools and questions meeting the definition of food insecurity were included.15,16 We established no date or age limits, although studies must have been conducted in the United States and written in English to decrease heterogeneity in the findings. In addition to published literature, the team included gray literature to reduce the influence of publication bias. We also hand-searched the reference lists of the 40 included studies and relevant systematic reviews identified by our search terms. The full criteria are detailed elsewhere (eTable 1 in the Supplement).
Data Sources
Because of the multidisciplinary nature of food insecurity and HIH research, we searched the Cumulative Index of Nursing and Allied Health Literature, Cochrane Central Register of Controlled Trials, Cochrane Database of Systematic Reviews, PsycINFO, MEDLINE via PubMed, Scopus, ProQuest Dissertations and Theses, and BMC Proceedings in January 2023 with the help of a research librarian. The entire search strategy is detailed elsewhere (eTable 2 in the Supplement). Two team members (C.L.J. and either P.Y. or C.A.H.) independently screened the studies, conducted a full-text review, and made decisions about inclusion in Covidence (Covidence Systematic Review Software), a web-based screening and data extraction tool.
Two team members (C.L.J. and either P.Y. or C.A.H.) independently extracted data on the publication year, the first author’s last name, and the prevalence of food insecurity (numerator) among people experiencing HIH (denominator). Factors extracted for the secondary objective included the significant and nonsignificant factors associated with food insecurity among people experiencing HIH. We resolved disagreements via discussion or a tie-breaking decision with a third team member (J.T.). One author (C.L.J.) extracted data on the study design, location, food insecurity tool, definition of HIH, and demographic data on people with food insecurity who were experiencing HIH. We synthesized demographic data by calculating mean percentage and mean (SD). We did not include missing or unclear information in the extraction. When multiple publications used the same dataset, the team collated the data and reported the new set as 1 point for the meta-analysis.
Criteria for Assessing Data
We assessed the quality of the studies using the Johanna Briggs Institute Checklist for Prevalence Studies. 17 Two team members (C.L.J. and either P.Y. or C.A.H.) independently rendered a yes or no decision about whether the study adequately met each of the 9 domains. Our team resolved disagreements via discussion and by a tie-breaking vote with a third team member (J.T.). We rated the overall quality as high if all domains met the criteria, medium if 1 to 4 domains failed to meet the criteria, or low if ≥5 domains failed to meet the criteria (eTable 3 in the Supplement). One author (C.L.J.) performed the certainty assessment with 2 authors (P.Y. and C.A.H.) using GRADE (Grading of Recommendations Assessment, Development, and Evaluation) for the prevalence outcomes and GRADE-CERQual (GRADE Confidence in the Evidence From Reviews of Qualitative Research) for the secondary objective of associated factors (eTables 4 and 5 in the Supplement).18,19
The prevalence of food insecurity consists of the number of people experiencing food insecurity as the numerator and HIH as the denominator. We performed the meta-analysis using Stata version 18 (StataCorp) and the Freeman–Tukey double arcsine–transformed proportion method with random effects. We chose the Freeman–Tukey method, which computes the weighted pooled estimate and performs a back-transformation on the weighted estimate, to include proportions close to 0 and 1. 20 We selected the random-effects method to address heterogeneity among studies. We summarized the data using a forest plot. We conducted a subgroup analysis by housing status to further address heterogeneity. We presented the average prevalence for each subgroup and the distribution of the estimates with the I2 statistic, 95% CIs, and prediction intervals.
We had no systematic way to compare the strengths of various factors because of the varying statistical methods used in each dataset; therefore, we examined the 11 datasets for the most common factors and extracted the data whether significant or not. For the significant factors, we examined the number of studies that reported each factor (eTable 5 in the Supplement). We then inspected the factors for themes and grouped them when appropriate.
Results
After removing duplicates, we screened 3398 abstracts from multiple databases in Covidence and relevant reviews and from reference lists of the included studies. After excluding 3283 studies because of nonrelevant abstracts, we reviewed the full text of 115 studies (eFigure 1 in the Supplement). We included 40 journal articles in the review (Table).1-4,21-56 We extracted information on the study location, sample size, population, prevalence of food insecurity, food insecurity screening tool, definition of HIH, and factors associated with food insecurity. Four studies were longitudinal cohort studies,1,48,54,55 and 36 were cross-sectional2-4,21-23,24-47,49-53,56 (eTable 5 in the Supplement). Nine studies were nationally representative,4,21,29,42,44,45,49,50,53 and 31 focused on a specific city or region of the United States.1-3,22,23,24-28,30-41,43,46-48,51,52,54-56 Twenty-three studies exclusively analyzed people experiencing homelessness,1,2,21-23,24,25,27-40 although 2 studies shared the same dataset and were collated.3,26 Eight studies examined people experiencing housing insecurity.4,41-47 Nine studies of people experiencing HIH were collated into 6 datasets, resulting in 36 unique datasets for the review.48-56 Sample sizes ranged from 18 to 10 165 participants. Twenty-three datasets were of adults aged ≥18 years,1-4,21,22,25-27,29-32,34,37,38,41,46-48,51-56 although 5 comprised only college-aged or young adults.1,22,25,28,39 Of 36 datasets, 10 were based on either households or families caring for children aged <18 years.23,24,33,36,40,43-45,49,50 The remaining 3 datasets focused on young people, ranging from age 9 to 24 years because of variable definitions for each study.28,35,39 Only 6 datasets had demographic data on people experiencing food insecurity and HIH.3,21,22,26,38,41,56 A synthesis of the demographic characteristics in the 6 datasets revealed that 61% of participants identified as male, 38% as female, 40% as non-Hispanic White, 52% as non-Hispanic Black, and 28% as Hispanic. The mean (SD) age was 43 (12) years.
Characteristics of studies containing the prevalence of food insecurity among people experiencing homelessness and/or housing insecurity in the United States

Abbreviations: —, indicates that no information on factors associated with increased or decreased odds of food insecurity was provided; AOR, adjusted odds ratio; ED, emergency department; HFIAS, Household Food Insecurity Access Scale; OR, odds ratio; SF-12, 12-Item Short Form Health Survey; SNAP, Supplemental Nutrition Assistance Program; USDA, US Department of Agriculture.
Eleven datasets2,3,21, 26,31,32,38,39,41,48-50,54,55 reported factors associated with food insecurity (Table, eTable 5 in the Supplement). Results from the quality assessment are detailed (eTable 3 in the Supplement). Seventeen studies were of high quality,4,21,24,29,34,38-40,42-46,49,50,54,55 and 23 were of moderate quality.1-3,22,23,25-28,30-33,35-37,41,47,48,51-53,56 Most studies were of moderate quality because of sample size or convenience sampling. We had moderate confidence in the prevalence of food insecurity based on the GRADE certainty assessment because of imprecision in the findings, and we had moderate confidence in the majority of factors associated with food insecurity based on the GRADE-CERQual certainty assessment because of some concerns about the adequacy of findings (eTables 4 and 5 in the Supplement).
Prevalence of Food Insecurity
The overall prevalence of food insecurity among people experiencing HIH in the 36 datasets was 57% (95% CI, 48%-65%; for heterogeneity, P < .001; I2 = 99.5%) (Figure). The prevalence of food insecurity among people experiencing HIH ranged from 7% in a cross-sectional study of 55 HIH adults in New York City to 94% in a cross-sectional study of 252 adults in Rhode Island.30,51,52 The study populations were subdivided by housing status into homeless, housing insecure, and HIH, although differences among the groups were not significant (P = .09). The prevalence of food insecurity among people experiencing homelessness was 63% (95% CI, 52%-74%; for heterogeneity, P < .001; I2 = 99.0%); among people experiencing housing insecurity, 51% (95% CI, 33%-69%; for heterogeneity, P < .001; I2 = 99.81); and among people experiencing HIH, 40% (95% CI, 23%-58%; for heterogeneity, P < .001; I2 = 98.0%). Differences between high- and moderate-quality studies were not significant: the prevalence was 52% (95% CI, 40%-64%) in high-quality studies versus 61% (95% CI, 48%-73%) in moderate-quality studies (P = .32).
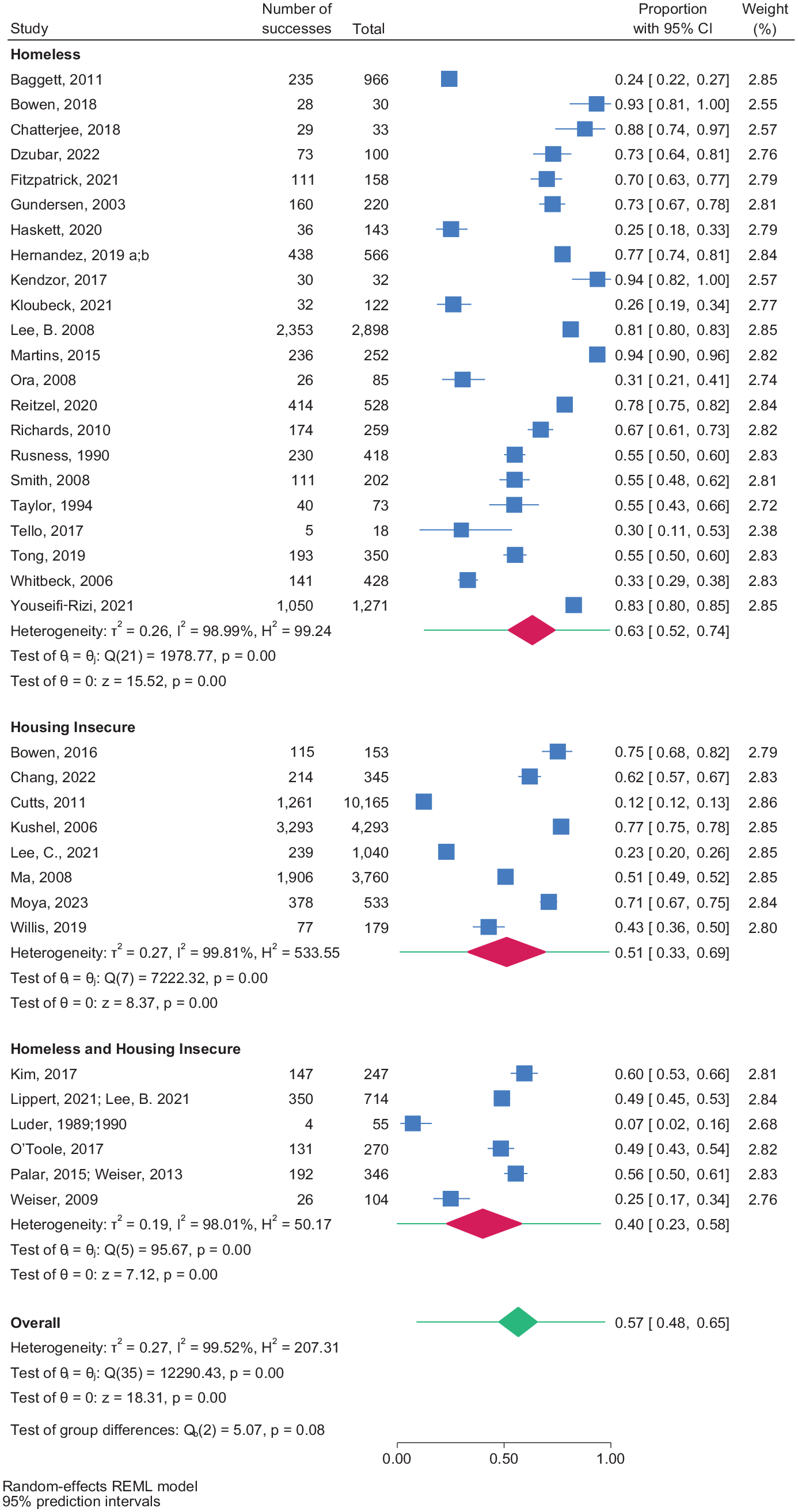
Forest plot of the prevalance of food insecurity among people experiencing homelessness or housing insecurity, in a meta-analysis of 40 studies in a systematic review conducted before January 2023 in the United States.
Factors Associated With Food Insecurity
Of the 40 studies in the review, 14 studies2,3,21,26,31,32,38,39,41,48-50,54,55 that collated into 11 unique datasets contained information on factors associated with increased or decreased odds of food insecurity among adults and young people experiencing HIH (Table, eTable 5 in the Supplement).
The most common factor described in 7 datasets was the presence of a mental health condition (symptoms of anxiety, depression, and posttraumatic stress), which increased the odds of food insecurity.2,3,26,38,41,48-50,54,55 Social and institutional support (medical access, jail, shelter, family, or friend support) was the second-most common factor described in 4 datasets and was associated with decreased odds of food insecurity.2,38,39,49,50 Other frequently cited factors associated with increased odds of food insecurity among people experiencing HIH were physical health impairments, substance use/alcohol dependence, and a history of personal or sexual abuse.2,26,39,49 Factors also included high rates of psychiatric/general hospitalization and emergency department use, as well as female gender, oral pain, and history of arrest.2,21,31,38,41,54,55 Because temporality could not be established in most studies, the only causal inference explored was the association of food insecurity and depression, with depression likely resulting from severe food insecurity.48,54,56 Factors uniquely associated with increased odds of food insecurity among HIH children (defined as a child aged <18 y) included families with large numbers of children, children aged >5 years, and parents with temporary employment. Among HIH adolescents aged 16-19 years, factors associated with increased odds of food insecurity included living unsheltered on the street, male gender, and older adolescent age. Social and institutional support was associated with lower odds of food insecurity across all ages.2,38
Discussion
Across 40 studies, the overall prevalence of food insecurity among people experiencing HIH was 57%. This estimate is >4 times the 12.8% estimated prevalence of food insecurity in the general US population. 57 These studies demonstrate that most people experiencing HIH also have food insecurity, and these social determinants of health should be addressed together. For many of these individuals, housing insecurity and food insecurity may have been caused by similar socioeconomic or clinical factors, as found in systematic reviews of risk factors for each condition separately.58-60 The overall prevalence rate that we found can be interpreted another way: many people who experience HIH do not uniformly experience food insecurity, which is an interesting finding that deserves further examination. Many questions remain that warrant further study, such as how those experiencing HIH without food insecurity secure regular food sources and what protective factors keep them from being food insecure.
The demographic characteristics that we synthesized in our review largely mirrored the demographic characteristics of the homeless population overall. 61 Across all age groups, the most frequently cited factor associated with an increased risk of food insecurity among people experiencing HIH was a mental health condition.2,3,26,32,38,39 This finding is in line with a scoping review that found a bidirectional relationship between food insecurity and mental health conditions among people experiencing homelessness. 10 Many protective factors can be synthesized into 1 common theme—social and institutional support decreases food insecurity among people experiencing HIH. Social support encompasses friends, family, and community members, and institutional support encompasses spending time in a shelter or transitional housing, receiving medical care or childcare, or enrolling in SNAP benefits (Supplemental Nutrition Assistance Program). Social and institutional support intuitively makes sense and is supported by the broader literature that people engaging with others and institutions are more likely than isolated individuals to be provided food or connected with resources.62,63 However, reaching and engaging the most isolated HIH populations is challenging because of the multitude of reasons why people avoid institutional involvement, such as fear of arrest, ineligibility for programs due to immigration status, lack of accessibility, the exclusion of pets, and administrative issues.2,64-67 Addressing food insecurity and HIH together may help improve physical health and decrease acute care and emergency department use.68-70
Public Health Implications
Given the high rate of overlap between housing insecurity and food insecurity, programs can work together to address these challenges.50,71 Currently, programs for food insecurity and HIH are often siloed in part because of a patchwork of funding streams and various administrative management systems, such as the US Department of Housing and Urban Development and SNAP.72,73 Community-based providers have reported a need to improve coordinated governmental efforts to address social needs such as food insecurity and HIH.72,74 This work may be supported by shared evidence-building priorities now required of federal agencies.75,76 In addition, efforts to screen for food insecurity in HIH service settings and for HIH in food insecurity service settings may help identify clients or systems when opportunities exist for interagency collaboration to address both conditions.
Because of the strong association between mental health conditions and food insecurity among people experiencing HIH, mental health clinics located on-site in temporary housing and shelters may increase access to mental health care and potentially decrease health care costs by avoiding the expense of inpatient psychiatric hospitalizations.10,21 Various studies have highlighted the benefits of integrated health care and social services for people experiencing HIH.77,78 Because food insecurity and other issues may remain even after people obtain permanent supported housing, food insecurity should be considered in conjunction with other social needs.79,80 In addition, the protective nature of institutional and social support in decreasing the incidence of food insecurity among people experiencing HIH highlights the importance of person-centered engagement, programming, and outreach efforts.74,81
Strengths and Limitations
This meta-analytic review had several strengths, such as the number of studies analyzed and adherence to the Cochrane Handbook for Systematic Reviews of Interventions. The review also had several limitations. First, we found a large amount of heterogeneity in the prevalence of food insecurity, so we provided prediction intervals. 82 In addition, the measures for food insecurity and HIH varied across studies, which led to difficulties determining whether the most cited factors were simply the most frequently investigated. However, we increased transparency by investigating all of the significant and nonsignificant factors in the studies and reporting the most frequently cited.
Conclusion
Most people experiencing HIH also have food insecurity. Factors most frequently cited as increasing the risk of food insecurity among HIH include a mental health condition, physical health impairment, or a history of physical or sexual abuse. Because social and institutional support was the most frequently cited factor associated with a decreased risk of food insecurity among people experiencing HIH, coordinated efforts are needed to provide shelter, health care, food, childcare, and community among people experiencing HIH.
Supplemental Material
sj-docx-1-phr-10.1177_00333549241305349 – Supplemental material for A Meta-analysis of the Prevalence of Food Insecurity Among People Experiencing Housing Insecurity and Homelessness in the United States
Supplemental material, sj-docx-1-phr-10.1177_00333549241305349 for A Meta-analysis of the Prevalence of Food Insecurity Among People Experiencing Housing Insecurity and Homelessness in the United States by Carolyn L. Jackson, Cody A. Hart, C. Jeff Uribe-Lacy, Phillip Yang and Jack Tsai in Public Health Reports®
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online. The authors have provided these supplemental materials to give readers additional information about their work. These materials have not been edited or formatted by Public Health Reports’s scientific editors and, thus, may not conform to the guidelines of the AMA Manual of Style, 11th Edition.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
