Abstract

The COVID-19 pandemic has been a long and tragic public health crisis. More than 1 million people have died in the United States. Some segments of our population, including those who are African American, Hispanic, American Indian/Alaska Native, and living in low socioeconomic areas, have borne a disproportionate burden of morbidity and mortality. 1 Preexisting health disparities have been exacerbated as people delayed care, deferred prevention, and isolated at home.
During the pandemic, we have become acutely aware of the differences that the social determinants of health (SDOH) play in our lives and our health. SDOH include an array of conditions that affect health in the areas where we live, learn, work, worship, and play, 2 such as access to nutritious food, health care, safe venues for physical activity, and secure, safe, and affordable housing. These conditions also reflect structural barriers that include discriminatory practices that have been deeply embedded in policy and practice. 3
As we emerge from the pandemic, there is a critical need to consider SDOH as we address existing inequities and improve health across our nation. While SDOH are inextricably tied to health equity, they are not one and the same. Unless a conscious effort is undertaken to ensure that SDOH activities are addressed through a health equity lens, some populations may continue to have advantages over others.
Social Needs Versus Social Determinants of Health
As we discuss the SDOH and the approaches different sectors are taking to address them, we need to differentiate individual social needs from broader, population-based social determinants. Both are critical and complementary.
Social needs are experienced at the individual level. 4 A person may have a host of social needs that exacerbate their current health conditions. A person with uncontrolled diabetes or HIV needs access to healthy, affordable food to adhere to medical recommendations. The person may also need housing, transportation, a job, and social services. Many in the health care arena are now embarking on social needs screening and referral processes. If the health system effectively screens and connects individuals to needed resources, health may improve and medical costs may be reduced. For example, the Health Plan of San Mateo calculated a $1.57 return for every dollar it invested, while WellCare calculated a $3.47 return on investment for its CommUnity Impact model. 5
Health plans and even health care systems tend to focus on their patients or enrolled members who arrive at their medical appointments and are screened and referred. But not all individuals have access to health care, and others do not use the health care system. In addition, many health care systems span large geographies that do not correspond to governmental boundaries such as a city or county, making it difficult to address varied social needs given the local nature of social services, policies, and programs.
Social determinants, on the other hand, exist at the community or population level and reflect policies and environments that support or create barriers to health. Within a given community, things that are essential to health are often more or less accessible due to availability, cost, quality, or preexisting policies. For example, a community without a grocery store, a public transportation system, affordable and available housing, or economic opportunities is not a community that can offer an individual the conditions and resources that promote health. Similarly, unhealthy policies and environments resulting in things like pollution or violence are also unevenly distributed. These SDOH, which are broader than individual-level social needs, contribute to resilience and health of communities across geographies and, over time, account for half of the county-level variation in health outcomes. 6
SDOH and Public Health
To address social determinants such as food security, access to green space, transportation, and housing options, among others, multisector partnerships can be an important strategy for addressing root causes. 7 Community coalitions that represent and engage community members have been able to stimulate and lead many of these efforts. 8 Public health organizations are well positioned to work with community coalitions and others to provide the needed knowledge, data, and expertise to produce success. They have long been at the forefront of multisector work and can focus on broad social determinants.9-11 Activities such as integrating available data at the community level, convening multisector partnerships, fostering community trust, and promoting and implementing health-enhancing policies that can lead to systematic and environmental changes fall naturally within the public health domain. A resilient community can make health-promoting opportunities available to all, helping to ameliorate health disparities. 12 Work on social determinants at the community level is a critical complement to work on social needs at the individual or family level. It is time to refocus our attention not only on the social needs of the individual but on the larger SDOH.
Given the complex nature of SDOH, diverse partnerships are beneficial and include, first and foremost, community residents and community representatives from sectors such as education, housing, transportation, and economic development. No single sector alone will ever be able to fully address the SDOH within a community. And no effective strategies will be sustainable without the engagement of community members most affected by these SDOH. Public health organizations, by focusing on upstream, evidence-based interventions, are an essential contributor and partner for SDOH work.
SDOH and the Centers for Disease Control and Prevention (CDC)
CDC, as the nation’s public health agency of the federal government, is committed to addressing health inequities and their root causes. In April 2021, CDC Director Dr Rochelle Walensky declared racism a public health threat, and the agency is currently engaged in an all-encompassing health-equity initiative. 13 This position maintains and enhances CDC’s prior work on SDOH, an example of which has been reported in this journal. 14 Recent agency efforts related to SDOH are wide-ranging and include programming in the National Center for Chronic Disease Prevention and Health Promotion (NCCDPHP) as well as the Health Impact in 5 Years (HI-5) initiative, 15 the Social Vulnerability Index, 16 Community Approaches to Reducing Sexually Transmitted Diseases, 17 the Choose Safe Places Program, 18 and the National Initiative to Address COVID-19 Health Disparities Among Populations at High-Risk and Underserved, Including Racial and Ethnic Minority Populations and Rural Communities. 19 In June 2022, CDC adopted an SDOH agency-wide framework, led by NCCDPHP. The pillars of this framework are data and surveillance, evaluation and evidence building, partnerships and collaborations, community engagement, infrastructure and capacity, and policy and law (Figure).
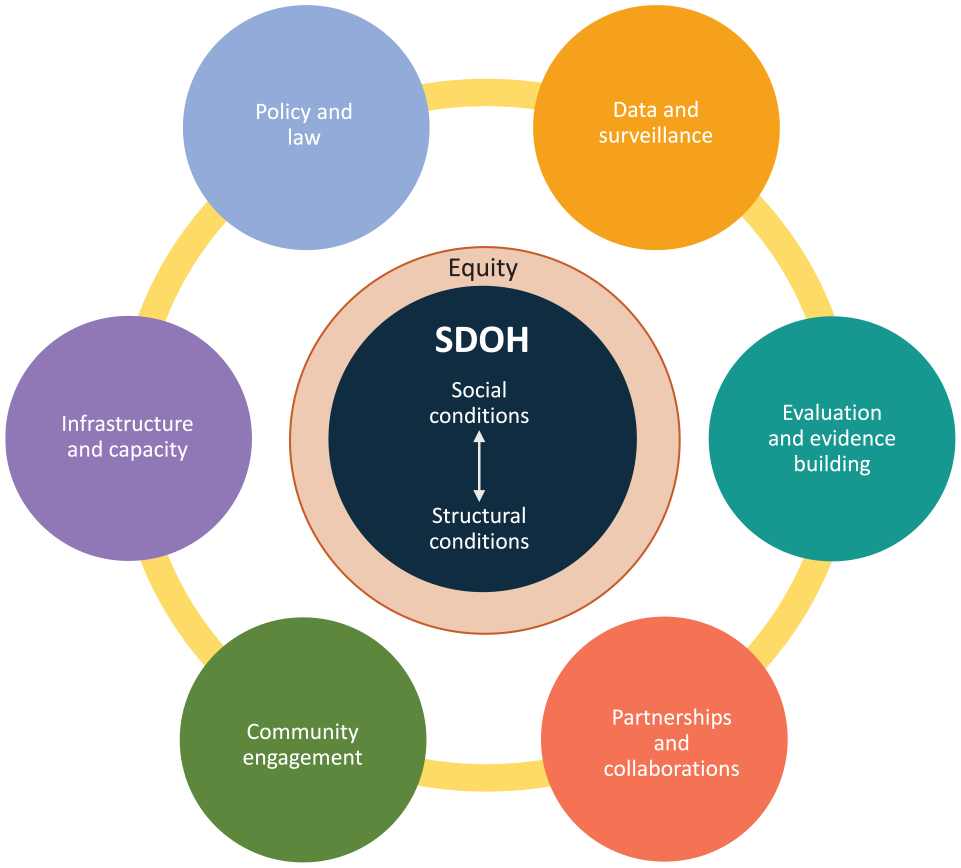
Framework developed by the Centers for Disease Control and Prevention for addressing the social determinants of health (SDOH).
Programmatically, the NCCDPHP has long been involved in efforts to address SDOH. Several programs have been wholly focused on SDOH, including the Racial and Ethnic Approaches to Community Health (REACH) program 20 and the Good Health and Wellness in Indian Country (GHWIC) program. 21 REACH supports 40 grantees using a community-based participatory approach. Recipients work with community partners to address identified needs and connect individuals to clinical care, address the built environment, support tobacco-free living, and promote nutritious food security. The approach works. More than 2.9 million people have better access to healthy food and beverages, more than 322, 000 people have benefited from smoke-free and tobacco-free interventions, and approximately 1.4 million people have more opportunities to be physically active. 22 GHWIC supports 27 grantees serving more than 100 tribes that are implementing holistic, culturally appropriate, and community-driven approaches to chronic disease prevention. 23
In the last few years, NCCDPHP has strengthened efforts to address SDOH and health equity. In 2020, NCCDPHP identified 5 areas related to the Healthy People 2030 SDOH goals 24 that complemented existing work and were related to chronic disease outcomes. These are:
Social connectedness, which is the degree to which individuals have quality relationships to create a sense of belonging and support;
Community–clinical linkages, which connect individuals to the services that they need;
Tobacco-free policy, which includes population-based preventive measures to reduce tobacco use and tobacco-related morbidity and mortality;
The built environment, which refers to human-made surroundings and can include issues related to housing and transportation; and
Food and nutrition security, which exists when people consistently have physical, social, and economic access to food to meet dietary needs for a productive and healthy life.
Several new initiatives support activities in these areas. In 2021, NCCDPHP launched the The Closing the Gap With SDOH Accelerator Plans initiative, 25 which supports multisector collaborations as they create ready-to-implement SDOH action plans. Awards were made to 20 state, local, and tribal recipients. These plans are focused on the SDOH that affect chronic disease. Simultaneously, NCCDPHP embarked on an effort with the Association of State and Territorial Health Officials and the National Association of County and City Health Officials to identify communities that were successfully addressing SDOH. These 42 Getting Further Faster communities are providing practice-based evidence for the field. 26
Advancing SDOH in Public Health
Fully addressing SDOH will require increased attention on evidence-based prevention strategies based on bridge building and coordination with partners. Clarification about the differences between SDOH and social needs will support these activities. After the COVID-19 pandemic, as we rebuild the public health infrastructure, a unique opportunity exists to facilitate a focus on the SDOH to drive population-level improvement in health outcomes, health equity, and general well-being. This focus will demand new skills and resources. Several strategic activities will help the field accomplish these goals:
Make SDOH a core function of public health organizations with appropriate supports,
Expand skills and personnel with relevant expertise for SDOH work,
Link SDOH efforts to health equity to ensure that addressing SDOH also promotes equity,
Strive for mutually beneficial cross-sector partnerships that engage affected communities and effect measurable changes in important health outcomes,
Collect and link data on SDOH at the national level to inform programming at the local level, and
Evaluate efforts to demonstrate value and help set future priorities.
As health care organizations and systems have demonstrated with their work addressing social needs, they are likely to be willing, integral, and ready-made partners in the effort to address SDOH.
The emphasis on health is essential to addressing SDOH and achieving equity. The public health enterprise has a pivotal role to play. Sometimes leading and sometimes supporting, CDC is committed to the field and addressing SDOH. Now, more than ever, we have a unique opportunity to act.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
