Abstract
Objectives:
Schools of public health (SPHs) must train students through real-world situations. Practice-based teaching (PBT) uses immediate application for skill development through multiple modes of delivery including virtual collaborations. PBT provides short-term benefits but is less understood long term. We sought to understand the longer-term impacts of PBT on students, public health agencies, faculty, and SPH administration and determine if the reported benefits of PBT outweigh the challenges.
Methods:
We used a mixed-methods pre–post-test evaluation to assess short-term outcomes in spring 2015 and long-term outcomes 3 years later using quantitative and qualitative assessments. The evaluation included 4 PBT courses spanning disciplines in 1 SPH. Participants included students (n = 56), collaborating agencies (n = 9), teaching faculty (n = 7), and SPH administrators (n = 8).
Results:
Students reported acquisition of competencies, application at follow-up, and being workforce ready (91.0%) with greater appreciation 3 years post-semester (78.6%). Collaborating agencies reported successful implementation of deliverables (77.8%) and enhanced networks (88.7%) with cost savings and better outcomes for the communities served. Faculty recognized beneficial outcomes to students including workforce preparation (71.4%), and administration recognized the benefits and worth of PBT to the school for teaching (100%) and research opportunities (87.5%).
Conclusions:
Given the shifting higher education landscape as a result of the pandemic, public health courses are being redesigned to provide opportunities for skill development, regardless of delivery mode, and enhanced connections to the field are essential. PBT is a flexible pedagogy that results in lasting and innovative resources to agencies and prepares public health students with technical skills and professional competencies to be workforce ready.
Keywords
Public health education must be grounded in real-world situations to prepare master of public health (MPH) students for the workforce,1-4 especially considering the changing employment sectors of MPH students. 5 In the context of COVID-19, faculty at schools and programs of public health (SPHs) have struggled to find opportunities for students to apply competencies learned in their program to the field. Proposed updated SPH accreditation guidelines reflect virtual learning, 6 with evaluations of various learning modalities showing equally effective learning outcomes. 7 Practice-based teaching (PBT) combines traditional methods of student learning, immediate application of skills, and agency collaborations to address real-world problems, especially when designed thoughtfully, implemented appropriately, and evaluated rigorously.8-11
PBT courses support students’ learning inside and outside the classroom,12-14 arm students with workplace skills, benefit collaborating agencies and communities,9,15 and can be adapted to delivery modalities, 16 which is necessary in times of natural disasters, pandemics, or other scenarios that rapidly change the public health landscape. 17 This importance became evident in 2020-2021 given the understaffed workforce responding to the COVID-19 pandemic. The student and faculty connection to the public health field, now facilitated by technology, can result in innovative and sustainable solutions. When a need exists to urgently staff the field to address a crisis, 18 pedagogy that incorporates skill building, immediate content application, tailored feedback, group connections and collaborations, and real-time perspectives ensures a ready workforce. In addition, PBT courses provide flexibility, 13 allowing faculty to teach skills through multiple modes of delivery and offering SPHs insight into the most current issues.
The aforementioned benefits are important, but challenges to large-scale adoption and implementation exist. Limited research has measured the long-term effectiveness of PBT in attainment of course competencies and collaborating agency outcomes across multiple public health disciplines. For PBT, conventional methods of assessment cannot effectively measure student achievement,19-21 and evaluations of all academic and community partners should measure impact. 22
We describe an evaluation of 4 PBT courses for MPH students to examine short-term and long-term effectiveness of PBT on academic and community partners. Although an evaluation of PBT courses has been documented and further evaluations of PBT recommended, 22 our study is the first known evaluation of PBT to assess long-term effectiveness of achieving technical public health competencies and professional skills across disciplinary areas. We hypothesized that PBT not only gives students technical and professional skills in the short term but also that those skills are applied and sustained in the long term to contribute to the workplace.
Although this evaluation occurred before the COVID-19 pandemic, the documented outcomes have implications for skill development, especially in a time of increased emphasis on virtual and hybrid learning.12,23 Agency collaborations in this evaluation were mostly virtual, and course content was delivered via in-class lectures, prerecorded content, and virtual meetings. Long-term outcomes documented in this evaluation demonstrate the utility of PBT as a fundamental pedagogy in public health training and argue for more wide-scale implementation, especially as SPHs redesign courses, reallocate resources, and explore alternate pedagogies for successful skill-based delivery in the current higher education landscape.
Methods
We conducted a mixed-methods pre–post-test evaluation during the spring 2015 semester and long-term outcomes 3 years later in fall 2018 to address the PBT cross-disciplinary logic model (Figure 1). The process and outcome evaluation obtained qualitative and quantitative data from students, faculty, agency, and the Boston University School of Public Health. An independent evaluator conducted the evaluation, and the Boston University Institutional Review Board approved all activities.
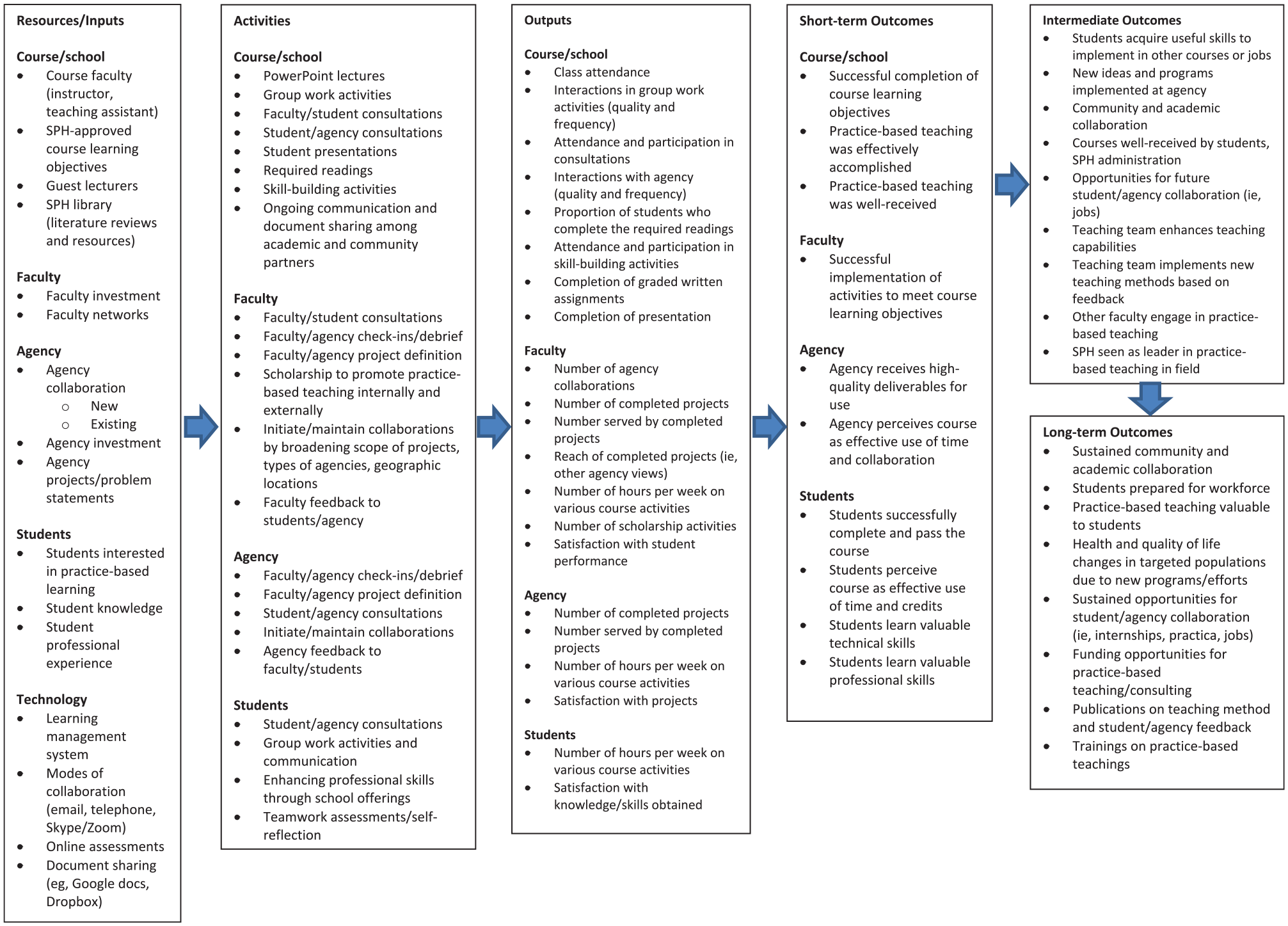
Logic model for cross-disciplinary practice-based teaching in schools and programs of public health (SPHs).
Sample
The sample consisted of 4 PBT courses for MPH students offered in the spring 2015 semester (Table 1). These 4 courses were taught by 4 faculty members experienced in PBT, represented 3 MPH disciplines, and focused on accomplishment of various competencies.
Cross-disciplinary evaluation of 4 practice-based teaching courses, deliverables, and collaborating agencies, spring 2015, Boston University School of Public Health
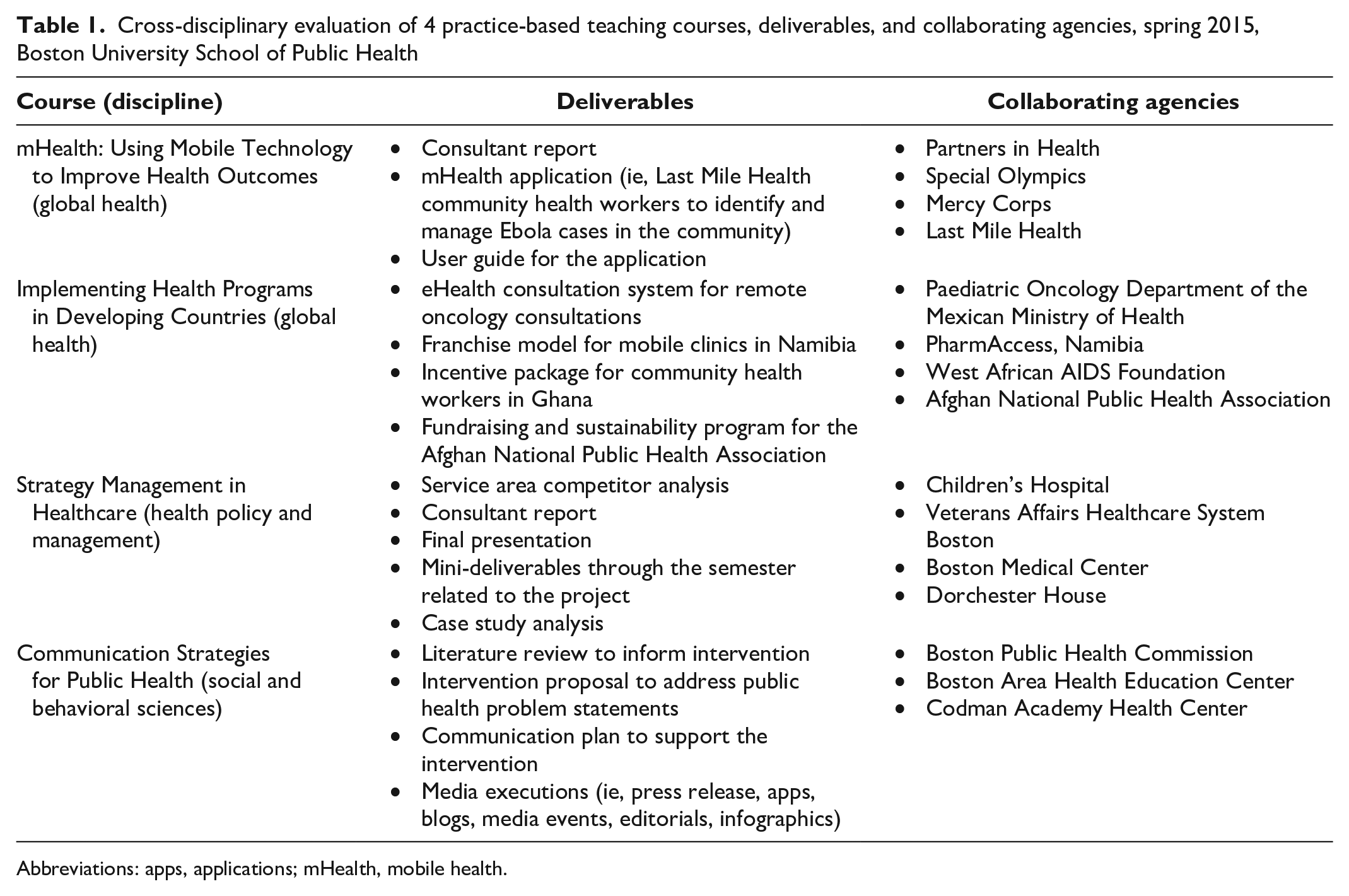
Abbreviations: apps, applications; mHealth, mobile health.
Each course partnered with collaborating agencies (n = 15) that ranged from international to domestic and from local health departments to nongovernmental organizations (Table 1). Students (n = 93) received a scope of work containing deliverables specific to the course objectives from the agency. 9 Teams of 3 to 5 students worked with an agency using flexible communication (in-person meetings, virtual meetings, email exchanges) to produce deliverables for the agency’s use and the course requirements. Agency interaction in 2 courses was entirely virtual and in 2 courses was hybrid. Because of weather conditions, 1 week of all courses was virtual. Deliverables varied and students presented the deliverables to agencies at course completion.
Data Collection and Measures
The evaluation used data collection strategies from students, agencies, faculty, and administration at various time points (Table 2). The evaluator emailed surveys with 3 reminders during a 2-week period. The surveys were anonymous, were voluntary, and took 15 minutes to complete. Survey questions included a 5-point Likert scale (from 1 = strongly disagree to 5 = strongly agree), multiple-choice questions, and open-ended questions.
Cross-disciplinary evaluation of practice-based teaching, data collection methods, and timeline, by group, Boston University School of Public Health, 2015-2018
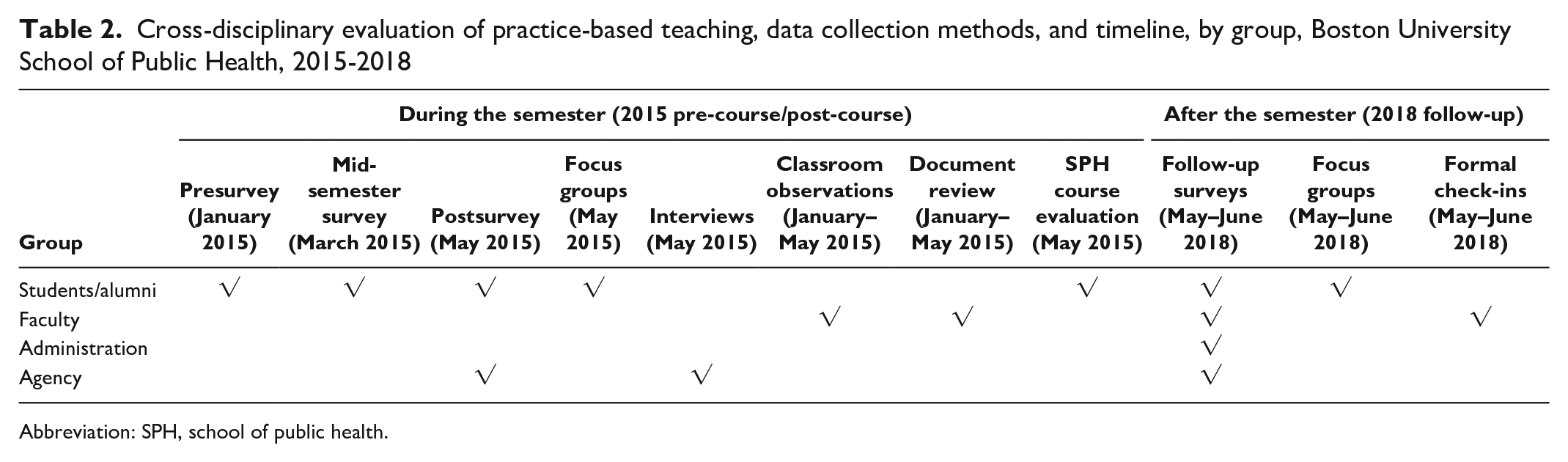
Abbreviation: SPH, school of public health.
The evaluator reviewed course documents to provide context to the course, inform process evaluation measures, and develop targeted surveys, focus groups, and interview questions. Student peer evaluation forms completed at multiple timepoints assessed the quality of student interactions, successes and challenges in teamwork and communication, and areas for improvement and confirmed other data collection. Standardized classroom observations (n = 8, 2 per course) conducted by the evaluator centered on content delivery, student engagement, fidelity to the syllabus, and faculty communication, and observations of student presentations confirmed agency satisfaction.
Surveys
Collaborating agencies (n = 9) completed an initial post-course survey to assess satisfaction with deliverables and course partnership and a post-course survey 3 years later to assess feedback on PBT, collaboration, and utility and quality of the deliverables.
A random sample (n = 48) of full-time faculty engaged in teaching at the SPH received an online survey in fall 2018 to assess perception of outcomes, facilitators, and barriers to PBT for them, students, the agency, and the school. Seven (15%) faculty representing all SPH disciplines responded to the survey.
The evaluator surveyed decision-making administrators at SPHs (n = 22) representing research, education, practice, and administration in fall 2018 to assess perceptions of PBT outcomes and facilitators and barriers to adoption. Eight administrators responded to the survey.
Students completed online pre-course (conducted the first week of the semester) and post-course (administered the last week of the course) surveys with a unique identifier that allowed for matching (n = 56) across timepoints. The pre-course survey assessed student attitudes toward working with an agency, attitudes toward group work, competency with skills (technical and professional), and demographic questions. The post-course survey reassessed those factors along with perceptions of PBT to achieve learning objectives and workforce preparation. Standard SPH course evaluations (n = 46) confirmed the student surveys. The evaluator administered a follow-up survey in fall 2018 with the original 56-student sample to assess application of course competencies to careers, utility of practice-based teaching for workforce readiness and skill development, and benefits and barriers to practice-based teaching; 29 students responded.
Student focus group
The evaluator conducted a 1-hour, in-person focus group with 8 students at the end of the spring 2015 semester to elicit opinions on the PBT format, instructor effectiveness, and agency collaboration. The evaluator conducted a similarly formatted focus group in 2018 virtually with 11 students from the 2015 PBT cohort to discuss applicability of PBT to the workforce. Two students overlapped focus groups, and the remaining students were unique.
Data Analysis
The evaluator recorded, transcribed, and managed focus group conversations using NVIVO version 12 (QSR International). We analyzed qualitative data using thematic analysis to identify and compare themes across data sources. 24 We used inductive coding for themes because of the exploratory nature of the evaluation questions. Data source triangulation 25 of participants allowed for a comprehensive understanding of perspectives, especially across data sources. We analyzed quantitative and survey data using SPSS Statistics version 22 (IBM Corporation); we removed missing responses from analyses. We examined Likert-scale questions by using proportions and continuous variables by using means and SDs. We conducted paired t tests on the matched student surveys for skills, value, and reflections, with P < .05 considered significant. Because of small sample sizes, we grouped the 5-point Likert-scale survey results as strongly agree/agree, neither agree nor disagree, and strongly disagree/disagree. We organized findings by student, agency, faculty, and administration and describe data collection methods and time points.
Results
Students
Consistent across the 4 courses, students (n = 93) represented all SPH concentrations, and 56 (60.2% of enrolled students) students completed the pre-course and post-course surveys. Most respondents were female (89.3%, n = 50), were aged 22-25 years (55.4%, n = 31), had full-time student status (69.6%, n = 39), had <5 years of work experience (92.8%, n = 52), and were working <20 hours per week (69.6%, n = 39); most students were not working.
In fall 2018, 29 former students (30% of students enrolled in 2015 and 50% of the matched sample) completed follow-up surveys. Most respondents were female (93.1%, n = 27), aged 26-30 years (89.7%, n = 26), and working full-time (86.2%, n = 25). Alumni worked in various industries and held jobs across various functions.
Eight students representing all 4 PBT courses participated in a focus group at the end of the semester (2015) and 11 students at follow-up; findings were consistent with the survey (Table 3).
Practice-based teaching evaluation benefits, barriers, and future implications, by group, Boston University School of Public Health, 2015-2018
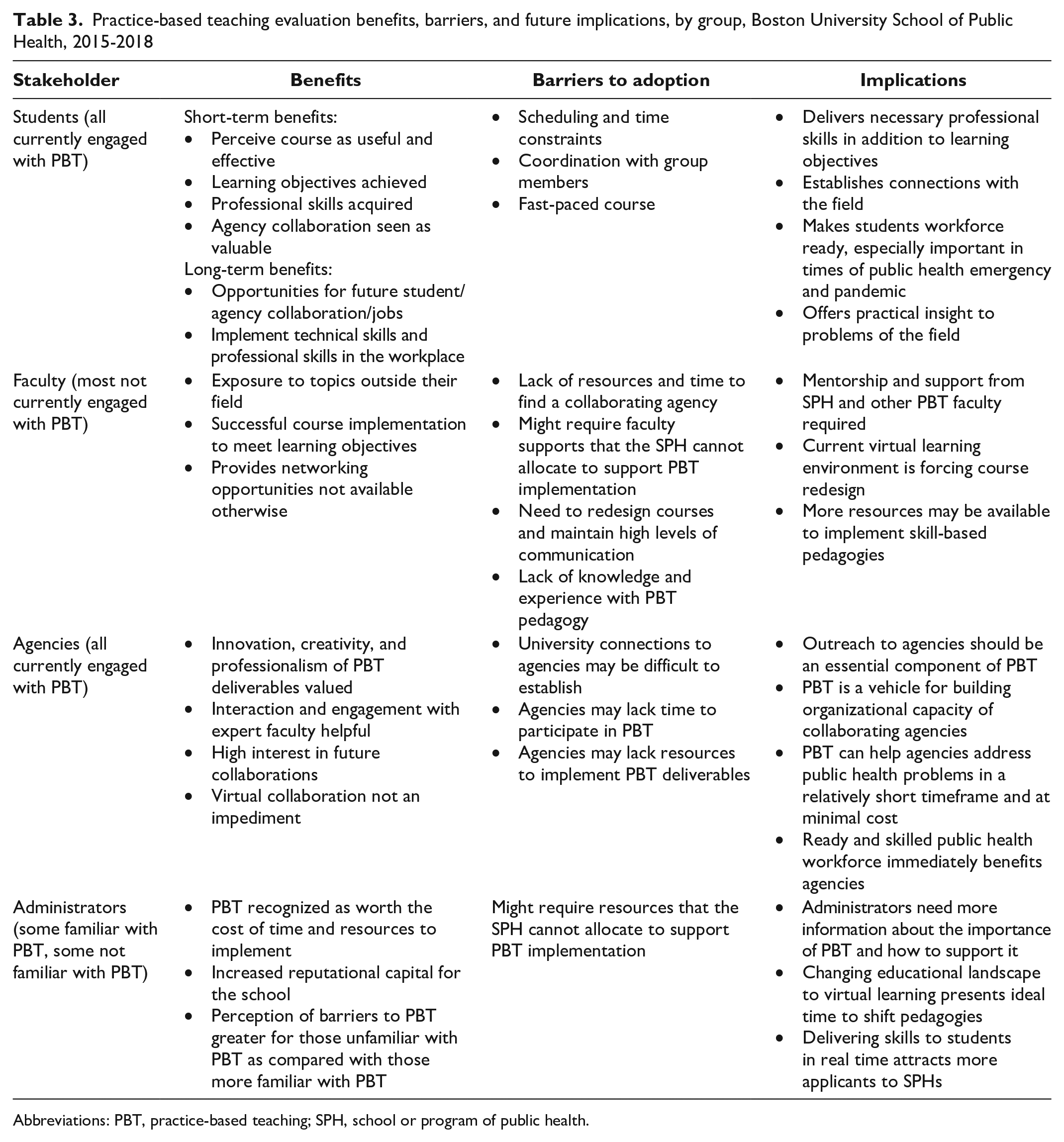
Abbreviations: PBT, practice-based teaching; SPH, school or program of public health.
Acquisition of Skills
Fifty-six students reported significant increases in all skills including consultation techniques (P < .001), literature reviews (P < .001), communication plans (P < .001), presentations (P < .001), program evaluation (P < .001), public speaking (P = .02), and mobile health (P < .001) and a nonsignificant increase in leadership (P = .16). When asked to what extent PBT positively impacted acquisition of skills (answers: not at all, somewhat, or quite a bit), 38 (67.9%) students reported “quite a bit” and 17 (30.4%) reported “somewhat”; the responses were similar for all 4 courses.
At follow-up, students overwhelmingly reported that PBT was important in applying skills (Figure 2) and application 3 years later. One student reported, “It [PBT] gives you a real-life learning experience that cannot be substituted by any other form of learning method.” The acquisition of skills remained high, with some variation from post-course to 3-year follow-up (Table 3).
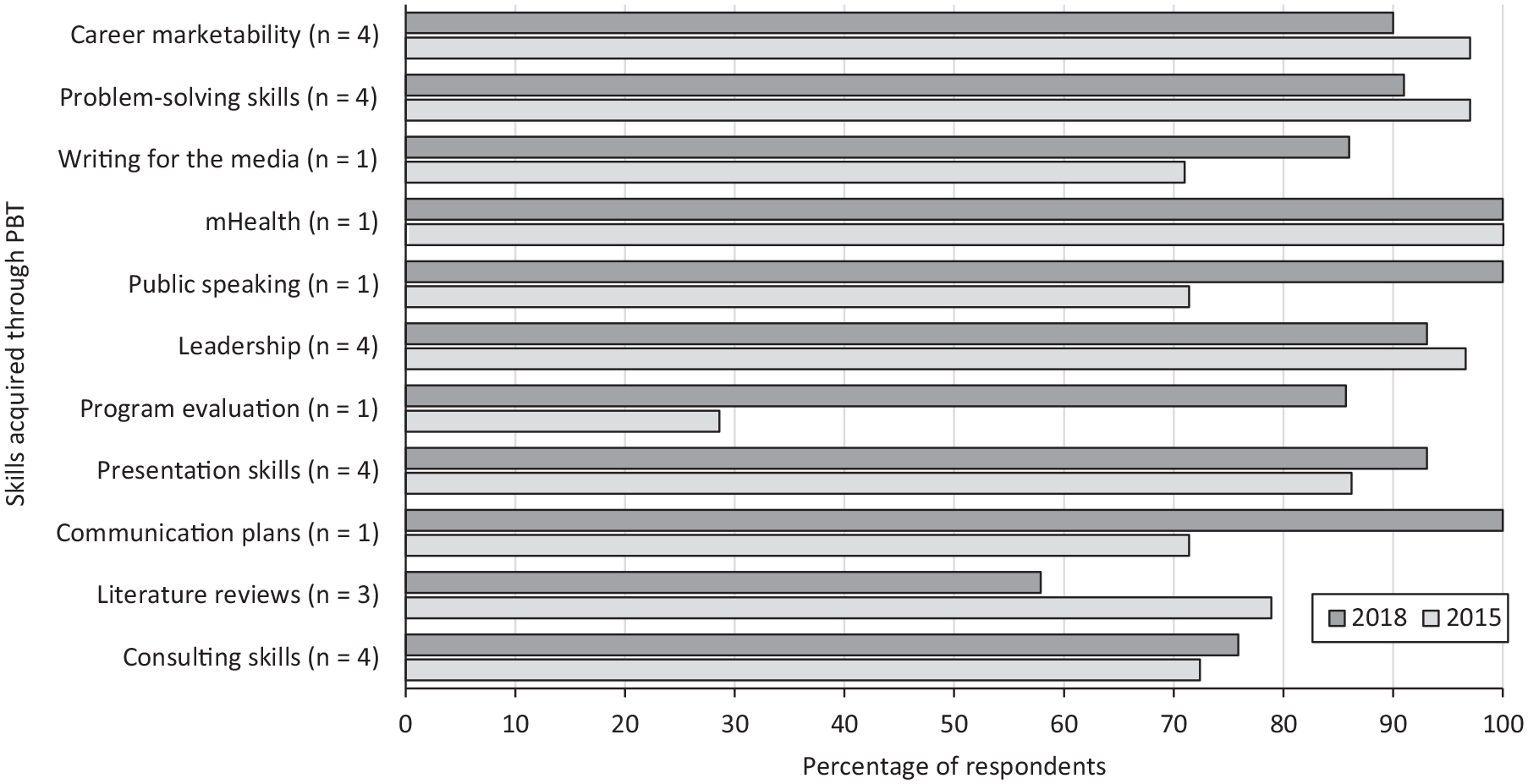
Self-reported acquisition of skills (matched), post-course and follow-up, among students (n = 29) enrolled in practice-based teaching (PBT) courses, Boston University School of Public Health, 2015-2018. Numbers represent the number of PBT courses that addressed that skill. Percentages represent the students who reported acquiring the skill. Abbreviation: mHealth, mobile health.
Value of PBT
Fifty (89.3%) students reported that working with an agency enhanced their comprehension of course content, and 54 (96.5%) students reported that working with an agency enhanced the quality of deliverables. Students highlighted the value of PBT to future careers: “[PBT brings] so many skills and abilities together . . . because it is not abstract, it creates hands-on skills, and allows the student to experiment and get a taste of the real thing” (Table 3).
At follow-up, students were asked the value of PBT to their current work environment, and 51 (91.1%) students reported the agency collaboration helped them develop problem-solving skills, enhanced their leadership skills, made them more marketable, allowed acquisition of job-appropriate skills, enhanced teamwork skills and appreciation for the field, and better prepared them to enter the workforce. A focus group participant stated, “Currently in my job there are many times I know how to do something because I did it in my practice-based class . . . it’s very important to . . . the growth of the student professionally” (Table 3).
Challenges with PBT reported in the 2015 focus group included frustration with scheduling group meetings, the fast-paced nature of the course, and communication with the collaborating agency. PBT was less valued for clarifying career plans (69.6%, n = 39), finding networking opportunities (53.6%, n = 30), and securing a practicum opportunity (37.5%, n = 21) or volunteer opportunity (21.4%, n = 12).
Reflections on PBT
Upon reflection, 54 (96.5%) students agreed that a PBT course was worth the time investment. Fifty-one (91.1%) students disagreed that they would have gained the same skills, and 46 (82.1%) students disagreed that they would have gained the same knowledge if traditional teaching methods had been used. One student shared, “It is extremely important for courses to bridge the gap between classroom-style/academic teaching and what the real world is like. Practice-based teaching does exactly that” (Table 3). Forty-four (78.6%) students appreciated the utility of PBT 3 years after the course, and 54 (96.5%) students said more MPH courses should use PBT.
Agencies
Value of deliverables
Of the 9 agencies, 7 reported utility of the evidence-based information, recommendations, and novel ideas provided by the students, and 6 agencies successfully implemented the deliverables within 3 years. Eight agencies reported cost savings for their organization, and 6 agencies reported more targeted programs with better outcomes for their community. One agency reported new or continued funding opportunities after the semester, and 5 agencies reported positive changes in the community served by their organization because of the collaboration.
Value of PBT
Agencies reported gaining knowledge (n = 7), skills (n = 5), and professional benefits because of the collaboration, including collaborating and networking with an academic institution (n = 8) and faculty (n = 8), having access to course materials and guest lectures (n = 5), and fostering professional development opportunities (n = 5). One agency shared, “One of the best things about our collaboration was that the . . . team was able to develop a product that our . . . team did not have time or resources to tackle ourselves” (Table 3). Feedback also highlighted the hope that more SPHs would use PBT.
Faculty
Benefits of PBT
Most faculty agreed that compared with a traditional course, PBT would expose them to topics outside their expertise (n = 5) and could enhance the school’s reputation (n = 5). Faculty reported PBT could result in professional networking opportunities (n = 4) but to a lesser extent it would result in research, practice, and/or scholarship opportunities (n = 2). Faculty recognized that successful PBT requires mentorship and support from other PBT faculty (n = 6) and considered whether resources existed to support implementation (n = 6).
Faculty recognized beneficial outcomes for students including higher-quality assignments (n = 4), increased acquisition of professional and technical skills (n = 4), better workforce preparation (n = 5), and the ability of agencies to better serve their target populations (n = 4). Increased acquisition of knowledge (n = 3) and better preparation for subsequent courses (n = 2) were less important.
Barriers to adoption of PBT
Most faculty reported interest in implementing PBT but recognized challenges, including not enough time to find a collaborating agency (n = 4), to redesign the course before the semester (n = 4), or to teach a PBT course during the semester (n = 3); the communication and planning for PBT seemed too daunting (n = 5); and a lack of networks in which to find a collaborating partner (n = 5). Other faculty reported a lack of knowledge about what is required of a PBT course (n = 5). One faculty member commented, “As noted, time is the big reason, and . . . lack of coverage for the effort and time investment [is] needed” (Table 3).
Administration
Benefits of PBT
SPH administrators reported that PBT courses benefit the school through enhanced reputation in teaching and/or community engagement (n = 8), professional networking opportunities (n = 7), and research, practice, and/or scholarship opportunities (n = 7). Seven administrators agreed that PBT was worth the resources, recognizing the vast benefits of PBT to students. One administrator noted, “Practice-based teaching enhances the learning experience for students” (Table 3).
Administrators did not agree with as many benefits to faculty; 3 administrators reported that PBT courses may expose faculty to other topics outside their expertise. Administrators did perceive positive agency outcomes, including sustained agency partnerships (n = 6), providing tailored deliverables to communities (n = 7), and products being implemented (n = 5).
Barriers to PBT
Although the perceptions were equally reported by administrators who were more familiar with PBT as a pedagogy (n = 4) and those who were less familiar (n = 4), administrators less familiar with PBT reported more barriers and that PBT implementation would require SPH administration support or PBT faculty mentorship (n = 8). One administrator noted, “Percent effort would have to be increased to cover the time/effort it takes to really do this well” (Table 3).
Discussion
The COVID-19 pandemic has enhanced the need for academic public health institutions to rapidly deploy a well-trained workforce to meet the changing needs of the public health field, which even before the pandemic had shifted employment sectors of MPH graduates. 5 During the pandemic, public health students were deployed to support understaffed local health departments. 18 This effort illustrates the need for training that fosters technical and professional skill acquisition through applied opportunities and real-world situations resulting in innovative and sustainable solutions.26,27 Our evaluation is timely given the current urgency for a trained and ready public health workforce and the shift to virtual and hybrid learning in higher education.
For students, the evaluation demonstrated achievement of learning objectives and acquisition of knowledge and skills acquired during the semester; consistent with other research, 28 students largely attributed the increase to the PBT course. Students received course content through in-person and virtual modalities. Students also more fully appreciated the essential nature of the skills developed—problem-solving, leadership, and teamwork skills—in the PBT course 3 years after being exposed to various functional roles in the workforce. These skills are important, particularly now in the changing public health landscape. These courses delivered competencies in a hybrid approach, with PBT a flexible pedagogy to teach virtually 16 and with increased technology. 29
Collaborating agencies expressed an interest in continuing collaboration, which is especially relevant given our virtual environment. Agencies connected either virtually or in a hybrid format (ie, a combination of virtual and in-person interaction). PBT is not only capable of being delivered through virtual connections with agencies but can be enhanced by technology 12 ; it has the ability to connect the classroom to agencies regardless of geographic boundaries. The longer-term benefits to the agency reported in this study reinforce already documented benefits, including cost savings and more targeted programs with better community outcomes.30-32
Consistent with previous research, faculty recognize the benefits of PBT 33 and that successful implementation requires resources and poses some barriers. 30 SPH administrators also recognized these barriers but reported it was worth the investment to successfully implement the pedagogy. Strategies to support the implementation and sustainability of PBT include time coverage to design or redesign a course for PBT, enhanced networking through alumni and career services offices, mentorship from experienced faculty, and structured trainings with resources.
Limitations and Strengths
This study had several limitations. First, we conducted the evaluation on 1 semester of PBT courses, which may have limited the generalizability of findings, although students in these courses represented all public health disciplines. Second, some sample sizes were small; however, respondents represented a variety of perspectives, and quantitative and qualitative data collection strategies yielded similar themes. Third, follow-up survey response rates were low (30%), but the sample was demographically similar to the students enrolled during the semester.
This evaluation also had several strengths. First, it was conducted by 1 evaluator unaffiliated with the program who examined 4 courses across public health disciplines with various learning objectives, assessments, and deliverables. Second, it examined application of skills in the field 3 years post-course, which is often too resource-intensive to assess. Third, PBT was delivered by 4 faculty members with different teaching styles and backgrounds but all with reliance on virtual connections. Fourth, collaborating agencies represented a variety of public health sectors and issues. Finally, the mixed-methods evaluation, a proposed update to SPH accreditation criteria, 6 resulted in a robust picture of the pedagogy.
Conclusion
The ability to develop and redesign courses that focus on skill development is at the forefront of higher education and will become more relevant as SPHs modify and expand their offerings. Resources are being reallocated to provide hybrid and virtual learning opportunities to students that did not previously exist, technology is more available to connect people, 23 and virtual learning will remain part of our higher education landscape. 34 The barriers that prevented large-scale adoption and implementation of PBT in SPHs will likely be addressed by the increased resources given to virtual, online, and hybrid learning. 26 PBT is a flexible pedagogy that can use a hybrid approach and leverage technology to connect the classroom to the field to prepare a ready public health workforce. Future research should explore the extent of resources needed to design and implement PBT courses, and other courses should be evaluated for short-term and long-term impacts across various delivery models.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
