Abstract
We studied the behavior of myogenic progenitors from donor desmin+/– LacZ embryos after implantation into tibialis anterior muscle of 2-month-old mouse hosts. Myogenic progenitors were collected from 10-day post-coital mouse embryo somite dermomyotomes (DMs), forelimb buds (LBs), and trunks. The replacement of desmin by the LacZ coding sequence allowed specific monitoring of β-galactosidase expression in donor myogenic cells. Immunostaining for myosin heavy chain and laminin expression was performed together with acetylcholine receptor histochemistry on sections of implanted muscle. Myogenic progenitors generated from DM, LB, and trunk were able to proliferate and adopt a myogenic pathway after transplantation into adult mouse muscle. Although their development appeared to be limited for DM and LB cell transplantation, the differentiation of myogenic progenitors occurred readily with trunk cell injection, suggesting that cell types associated with DM cells were involved in long-term myofiber differentiation (21 day). When neural tube/notochord (NTN) or sclerotomal (S) cells were co-transplanted with DM cells, myogenic nuclei were produced, indicating that both NTN and S are required for the differentiation of DMs grafted into adult muscle. These data are consistent with the differentiation of neural tissues and bone from NTN and S, respectively, and with the development of anatomic relations among all in vivo-differentiated tissues. These results suggest that embryonic trunk cells can be used to repair different types of injured tissues (especially skeletal muscle) under appropriate environmental conditions.
Keywords
S
Skeletal muscle has also been used as a recipient tissue for embryonic cells. De Angelis et al. (1999) injected a cell suspension of freshly dissected dorsal aorta taken from 9-day post-coital (dpc) MLC3F-nLacZ embryos into the leg muscle of SCID/bg mice. At 2 weeks later recipient muscle contained clusters of fibers with many β-gal+ nuclei, indicating that embryonic aorta cells can develop and differentiate in adult muscle. The present study investigated the developmental fate of mouse embryonic myogenic progenitors transplanted into adult muscle. Somite dermomyotomes (DMs) and forelimb buds (LBs) of 10 dpc mouse embryos were chosen as a source of myogenic progenitors. By day 10 myogenic precursors had mainly segregated into DMs derived from dorsal parts of somites (for review see Christ and Ordahl 1995; Stockdale et al. 2000). At this stage the vast majority of myogenic precursors of forelimb bud muscles have already migrated from lateral DMs (somites 9–14) to the forelimb (Houzelstein et al. 1999). Several lines of evidence indicate that signals from adjacent tissues play important roles in the myogenic commitment of somite cells (for review see Brand–Saberi and Christ 1999; Stockdale et al. 2000). It is still uncertain whether signaling pathways are required to maintain or expand a population of myogenic-specified cells on transplantation into an adult muscle environment. To address this question we investigated how a cell suspension from the trunk portion of 10 dpc mouse embryo developed into adult skeletal muscle. In addition to myogenic precursors present in the DMs, the cell suspension contained osteogenic and neural/notochordal (NTN) precursors derived respectively from sclerotome (S), neural tube, and notochord. To determine the possible role of each of these compartments in supporting the myogenesis of grafted myogenic precursors, DM cells were transplanted simultaneously with NTN or S cells. Because the behavior of progenitors in developing organisms is largely determined by environmental factors, grafts were also performed under the skin of the lumbar region to study the influence of the implantation site on the differentiation of grafted cells.
Heterozygous mutant desmin mouse embryos, which possess one copy of the reporter gene encoding nucleus-localizing β-galactosidase (nLacZ) targeted to the desmin locus (Li et al. 1996), were used to monitor the long-term fate of donor-derived myogenic cells. The desmin mutant mouse was chosen for several reasons. Desmin is the muscle-specific member of the intermediate filament family and one of the earliest known myogenic markers in skeletal muscle. Moreover, the mutated gene is activated in myonuclei throughout the prenatal and postnatal life of mutants, whereas no differences in the chronology or morphology of myotome formation or in myofiber differentiation occur during the first 2–3 weeks of postnatal development in mice lacking desmin (Li et al. 1997). We also estimated the differentiation level of grafted embryonic myogenic cells in terms of myofibrillar protein content. At the same time, the osteogenic and neurogenic development of cells transplanted in vivo was characterized through the use of different immunocytochemical markers.
Our results show that embryonic myogenic precursors located in somite DMs can differentiate into myofibers after transplantation into adult muscle. The myogenic rate obtained with trunk cell transplantation indicates that cues emanating from non-myogenic cells (neurogenic and chondrogenic cells) improve the differentiation potential of grafted DM cells. Consistent with these findings, transplantation was found to be more successful when DM cells were grafted simultaneously with NTN or S cells. Therefore, embryonic trunk cells retain their potential to form muscle, bone, and neural tissue after transplantation into an adult host. These findings are of fundamental interest but may also have significant applications after tissue damage.
Materials and Methods
Animals
Two-month-old male Swiss mice were used as hosts for embryonic cell transplantation. Cells were isolated from desmin+/– heterozygous embryos obtained by crossing Swiss female mice with desmin-null male mice (a gift from D. Paulin; Institut Pasteur, Paris). To disrupt the desmin gene in desmin-null mice, a targeting vector was constructed in which an E. coli LacZ gene was inserted in frame into the first exon of the desmin gene (Li et al. 1996). After enzymo-histochemical processing, the inserted lacZ gene allowed myotomal cells (Figure 1) to be recognized and monitored throughout their development. ROSA 26 mice expressing β-galactosidase in all their cell progeny were also used as donors to evaluate the total area occupied by all donor-derived differentiated cells.
Cell Preparation
Pregnant mice were sacrificed by cervical dislocation before removal of embryos at 10 dpc. To prepare the trunks, 10 dpc embryos (Figure 1A) were cut between the anterior and posterior LBs. The viscera and dorsal aorta were discarded and only the dorsal zones of the trunks were kept (Figure 1B). These zones included overlying ectoderm, neural tube and derived neural crest cells, blood vessels, notochord, and somites (Figure 1C). To prepare DMs, NTNs, and Ss, 10-dpc embryo trunks were immersed in a pancreatin solution and tissues were isolated mechanically. DMs in association with Ss or NTNs from each embryo provided a mixed cell suspension in which the ratio of the two cell categories was equivalent to that in the trunk suspension. LBs were isolated bilaterally from 10-dpc embryos. In all series, tissues were fragmented into small pieces and then treated enzymatically with a trypsin solution. Cell preparations were filtered through a 40-μm-diameter nylon cell strainer to eliminate non-dissociated cells that formed aggregates. The cells obtained were centrifuged at 1100 × g for 10 min and resuspended in DMEM. Cell viability was first checked in a hemacytometer using trypan blue as exclusion dye.
Cell Transplantation
Cell suspensions from DMs, LBs, trunks, and DMs associated with either S or NTN cells were prepared from desmin+/– LacZ heterozygous embryos. Cell suspensions from trunks were also prepared from ROSA 26 embryos. Recipient Swiss mice were anesthetized with an IP injection of a solution of ketamine (10 μg/kg) and xylazine (2 mg/kg). An incision was made in the skin of the leg to make the tibialis anterior muscle accessible. Two superficial injuries were performed by applying a stainless steel rod (precooled in liquid nitrogen three times for 10 sec) at the distal and proximal extremities of the tibialis anterior muscle. At 24 hr later, each damaged area was 1.5 mm thick and 2 mm in diameter, as assessed on histological sections from non-injected muscle. After this lesion procedure, 7 × 105 cells suspended in 10 μl DMEM were injected at a single site in the center of the tibial muscle and the skin was then closed with sutures. The proportion of desmin+ cells at the time of implantation into host muscle was assessed by counting β-Gal+ cells in the suspension.
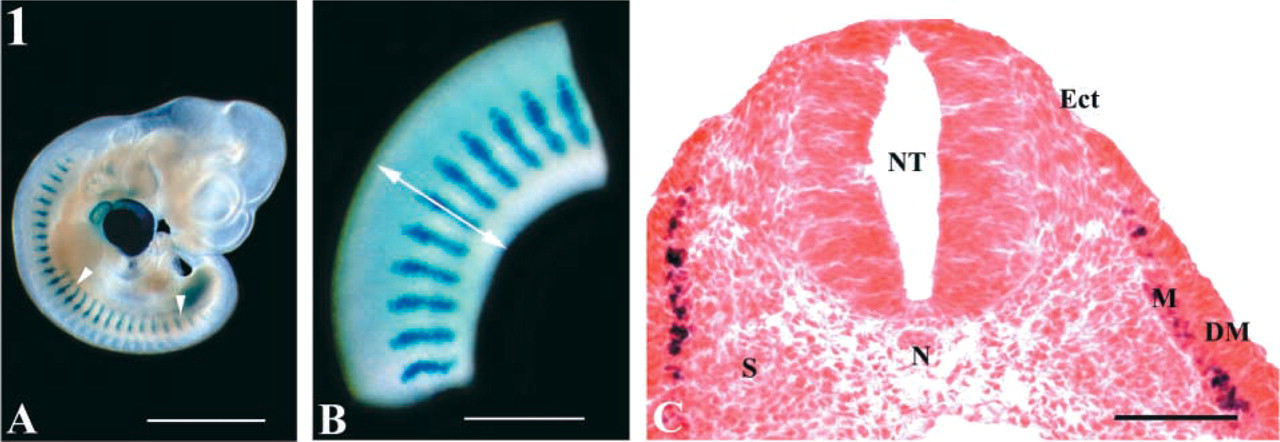
Whole-mount staining for LacZ activity in a desmin+/– mutant mouse examined at 10 dpc (
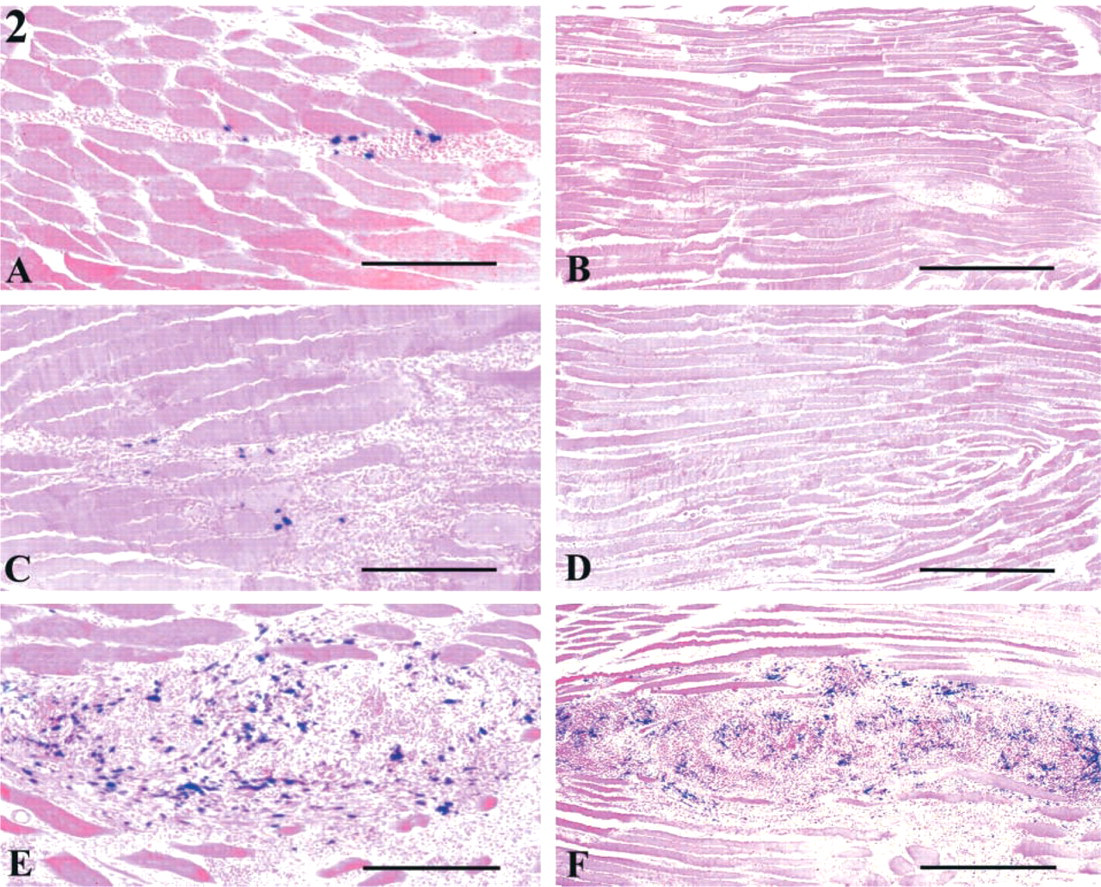
Grafts of 10-dpc desmin+/– mutant dermomyotome (
Trunk cell suspensions from ROSA 26 and desmin+/– LacZ mouse embryos were injected under the skin of the lumbar region. FK506 (kindly provided by Fujisawa GmbH; Munich, Germany), an immunosuppressive agent whose efficiency has been determined in the mouse and monkey (Kinoshita et al. 1996), was administered daily to host mice at a dose of 2.5 mg/kg beginning on the day of grafting and continuing throughout the experiment.
Tissue Examination
Qualitative Analysis. Recipient mice were sacrificed by cervical dislocation from 2 hr to 21 days after implantation. Injected muscles or subcutaneous grafts were washed in 4% sucrose in PBS and then in PBS + 15% sucrose for 24 hr at 4C before immersion in 30% sucrose/PBS solution overnight and embedding in Tissue-Tek before freezing in liquid nitrogen. They were sectioned longitudinally in a cryostat and all the serial sections (12 μm) were transferred onto gelatin-coated slides. Apoptotic cells were detected by the Tdt-mediated dUTP nick end-labeling (TUNEL) method. For TUNEL, the in situ Cell Death Detection Kit was used according to the manufacturer' recommendations (POD, cat. no. 1684817; Roche Molecular Biochemicals, Dormstadt, Germany). β-Gal histochemical detection was revealed by immersing the sections in a solution containing 2 mM 5-bromo-4-chloro-3-indolyl-β-
Quantitative Analysis. To evaluate the total number of donor blue nuclei per grafted muscle, serial sections were cut from the whole muscle. The number of β-Gal+ nuclei was counted in all 10 sections and then multiplied by 10. The percentages of donor nuclei giving rise to mononucleated myogenic cells and plurinucleated myotubes and fusing with host fibers were estimated with regard to the total number of donor nuclei. To measure the extent of the 2-week-old graft, as well as that of donor muscle fibers and chondrogenic/osteogenic condensations, the larger longitudinal section (n=4) was stained with safranin and then photographed. The different structures were delineated manually using the Adobe Photoshop program, and their areas were compared by counting pixels.
Results
Desmin LacZ Activity of Embryonic Myogenic Cells Deriving from DMs, LBs, and Trunk Cells
Myogenic cells retained in DMs (truncal somites, level 14–24) give rise to back muscles. At day 10, DMs contained mononucleated cells (i.e., myoblasts in proliferative phase), short myotubes, and dermal precursor cells. In addition to all these cells, the trunk cells included progenitors of vertebrae, ribs, and spinal cord, as well as neural crest derivatives. LB cells of 10-dpc embryos contained the progenitors of different muscles and bones of the forelimbs. The DM cell suspension contained about 14% of β-Gal+ cells. Positive cells were very rare in the LB cell suspension, probably because the great majority of myogenic progenitors had just migrated into the forelimb bud and did not yet express myogenic markers (Houzelstein et al. 1999). In the 7 × 105 trunk cell suspension (containing about 16% of DM cells, 64% of SC cells, and 20% of TN cells), 2–3% of cells were β-Gal+. In the three types of graft examined 4 days after implantation, mononucleated myogenic cells, identified by their blue nuclear staining, were located in the injection zone, mostly in interfascicular spaces (Figure 2). Fewer myogenic cells were detected in DM (Figure 2A) and LB (Figure 2C) cell grafts than in trunk cell grafts (Figure 2E). Although host muscles displayed variable amounts of myogenic nuclei, ranging from 0 to 2880 with DMs (n=11), 0–3280 with LBs (n=5), and 12,168–127,344 with trunk cells (n=8), the mean number of positive nuclei per grafted muscle was significantly higher in trunk cells (56,583 ± 15,363) than DM (620 ± 275) and LB (824 ± 635) grafts. Regardless of the type of cell suspension used (DM, LB, trunk), rare apoptotic nuclei were observed at the injection site (data not shown). These observations indicate that the low number of myogenic cells in DM or LB grafts cannot be explained by increased apoptosis during the first hours after cell injection. Furthermore, the differences in the myogenic rates of the three experimental series (DM, LB, trunk cell injections) could not have been due to differences in the extent of fiber damage in host muscle resulting from our injury procedure (see above).
The 7 × 105 trunk cells injected into adult tibial muscle were composed of a mixed cell population, including myogenic precursors deriving from 66 DMs on average. Because each DM consisted of about 1700 cells at the explantation stage, a total of 112,200 DM cells (16% of total injected cells) was contained in the 7 × 105 trunk cells. Despite the fact that about sixfold fewer DM cells (112,200) were injected into trunk than DM graft (7 × 105), enhanced differentiation of implanted muscle progenitors was observed (56,583 vs 620 β-Gal+ nuclei) 4 days after implantation. One week after IM injection of DM or LB cells, no blue β-Gal labeling was detected in recipient muscles (Figures 2B and 2D). Conversely, muscles transplanted with trunk cell suspension contained many blue nuclei at 1 week after injection (Table 1; Figure 2F). Therefore, the differentiation capacities of trunk cells transplanted into an adult muscle environment were further examined from 24 hr to 21 days.
Numbers of donor β-Gal nuclei included in different muscle cell types of a transplanted tibialis anterior muscle
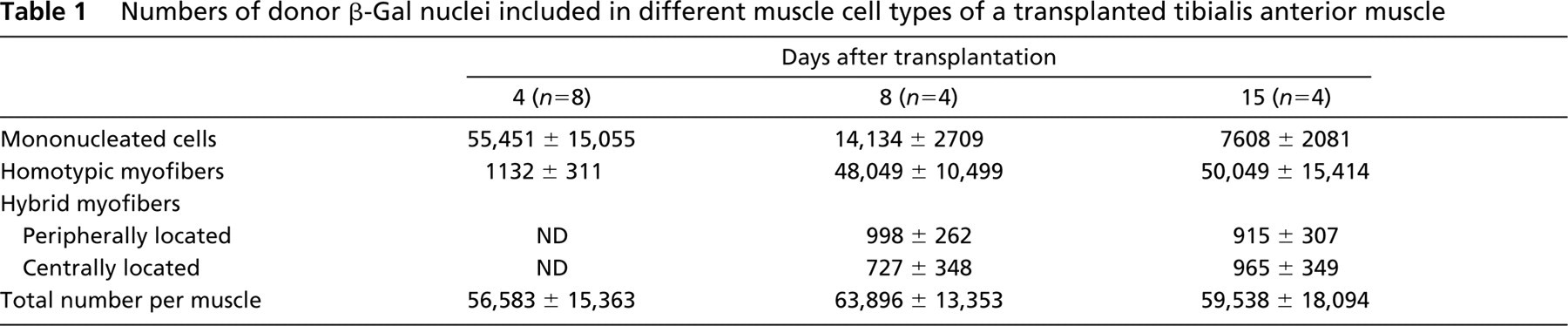
Differentiation of Trunk Cells Grafted into Adult Muscle
Differentiation of the Myogenic Lineage. At 24 hr after surgery, no blue β-Gal labeling was identified (Figure 3A). At 2 days the number of injected cells had markedly increased, and the presence of a few β-Gal+ mononucleated cells among them (Figure 3B) indicated that commitment to the myogenic lineage had occurred. At day 4 after implantation the percentage of β-Gal nuclei observed in mononucleated cells was estimated to be 98% on average (Table 1, Figure 3C). At this time, a few short, thin myotubes, containing three or four blue nuclei resulting from the fusion of donor cells and individually enclosed by basal lamina (identified by laminin staining), were identified (Figures 3D and 3E). Donor blue nuclei were also seen integrating host fibers (Figure 3F). One week after IM injection of trunk cells, the total number of donor β-Gal+ nuclei was similar to that present at 4 days (Table 1). However, the percentage of nuclei identified in mononucleated cells decreased to 22.1% (ranging from 18.7 to 27.4%), whereas the percentage of nuclei included in myofibers markedly increased from 2% to 75.2% (70, 78.1) of the total number of β-Gal nuclei (Figure 4A). Donor myofibers exhibited 10 nuclei on average, which were most often centrally aligned (Figure 4B). The myofibers were positive for neonatal/adult myosin heavy chain (Figure 4C) and expressed large acetylcholine receptor clusters (Figure 4D) that were always located near X-Gal-activating nuclei (Figures 4E and 4F). Hybrid fibers, resulting from the fusion of injected cells with host fibers, were observed at the periphery of the implantation site. They were generally of normal diameter and contained one or more β-Gal+ nuclei. After 1 week the percentage of nuclei integrated into host fibers was about 2.7% (1.4, 3.2). These nuclei were centrally located in 42% (26.9, 56.2) of cases or in peripheral position or just below the sarcolemma in 58% (43.7, 66). By the second week no change in the total number of donor blue nuclei was observed, but neomyofibers (more than 15 nuclei/fiber on average) (Table 1; Figure 4G) continued to grow, as indicated by the increased contribution of donor nuclei (84.1%; 79.1, 86.5) and the decreased proportion of β-Gal+ nuclei in mononucleated cells (12.8% on average; 11.7, 16.3). The nuclei seen in hybrid fibers remained relatively constant in proportion (3.1%; 1.8, 4.6) and were situated in central or peripheral position in 48% (50, 54.3) and 52% (50, 46.5) of cases, respectively. Subsequently, the injection site grew markedly (Figure 4H), and donor myofibers displayed larger sectional diameters, clearly defined regular cross-striations, and subsarcolemmal nuclei, some of which bulged from the fiber surface (Figure 4I). Donor myofibers, although well-differentiated, remained one half to one third the diameter of host fibers. Our data indicate that neomyogenesis, which appears to be the predominant fate of implanted embryonic myogenic cells, occurs exclusively at the implantation site.
Differentiation of myogenic cells from 10-dpc desmin+/– mutant trunk cells transplanted into tibialis anterior muscle of a 2-month-old adult mouse. Muscle sections examined (
Differentiation of the Neurogenic Lineage. At the time of extirpation, nerve components included in the trunk cell suspension were mainly composed of neural epithelial cells (including ventral motor, dorsal sensory, and glial cells, future astrocytes, and oligodendrocytes) and neural crest-derived cells (neurons and glia of Schwann cells in peripheral ganglia). In muscles studied 4 days after surgery, neurofilament-positive zones were seen throughout the implantation site, indicating that nerve masses were present. In the following days, many fasciculi of individual nerve fibers and nerve cell bodies visualized because of their neurofilament content were identified (Figures 5A and 5B). The expression of GFAP showed the presence of glial elements scattered over the entire implantation site (Figure 5C). When trunk cells from 10-dpc ROSA26 mouse embryos were transplanted into tibialis muscle, treatment of serial sections with anti-neurofilament antibody and X-Gal showed that neurofilament-positive zones were also blue-stained and therefore of donor origin (Figures 5D and 5E).
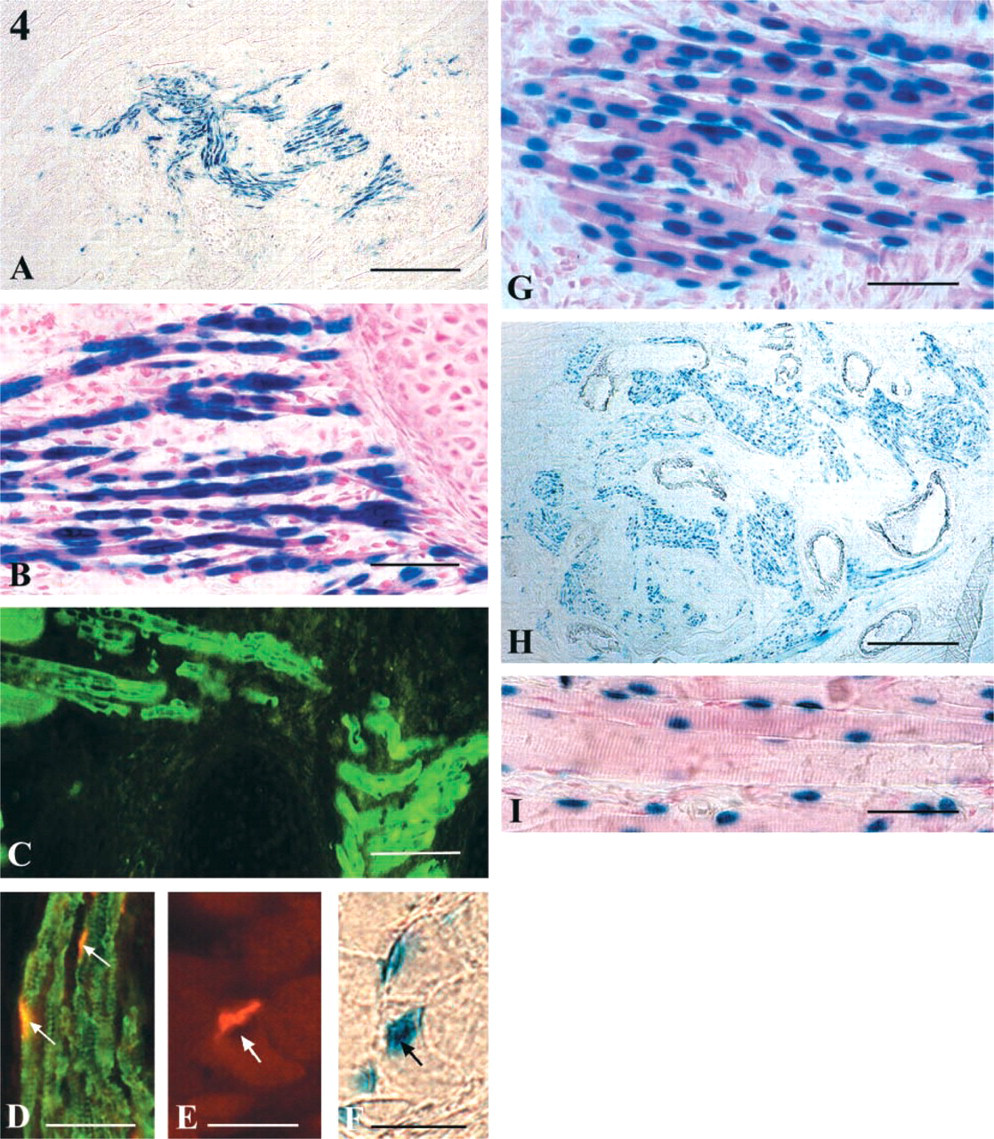
Differentiation of myogenic cells from 10-dpc desmin+/– mutant trunk cells transplanted into tibialis anterior muscle of a 2-month-old adult mouse. Every muscle section examined between 8 and 21 days after surgery was treated for X-Gal activity. (
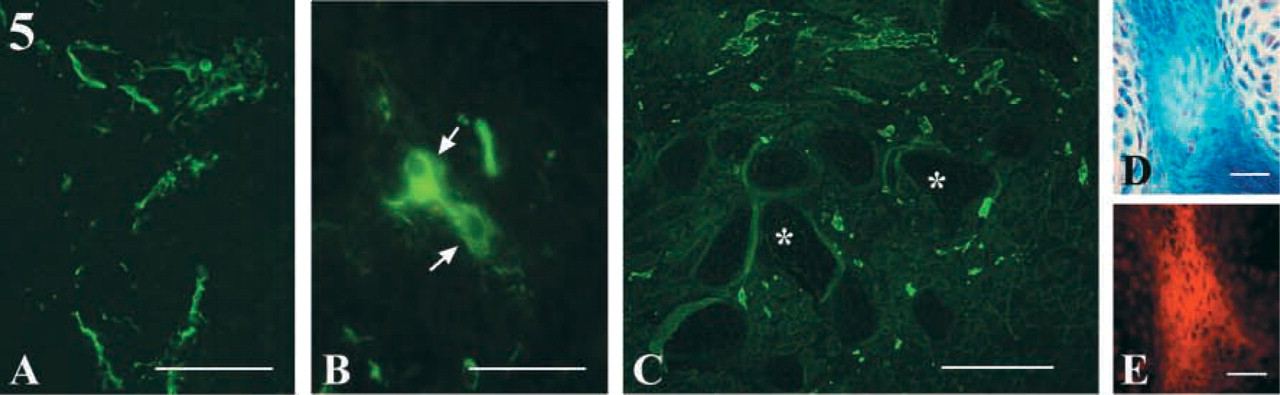
Differentiation of neurogenic cells from 10-dpc desmin+/– mutant trunk cells implanted into tibialis anterior muscle of a 2-month-old adult mouse. (
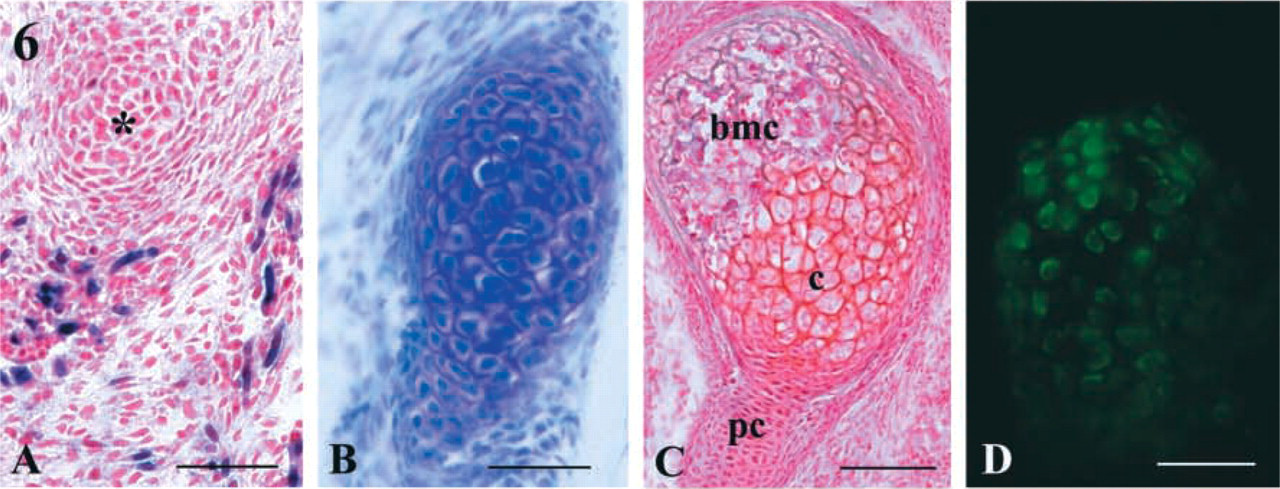
Differentiation of chondrogenic cells from 10-dpc desmin+/– mutant trunk cells implanted into tibialis anterior muscle of a 2-month-old adult mouse. (
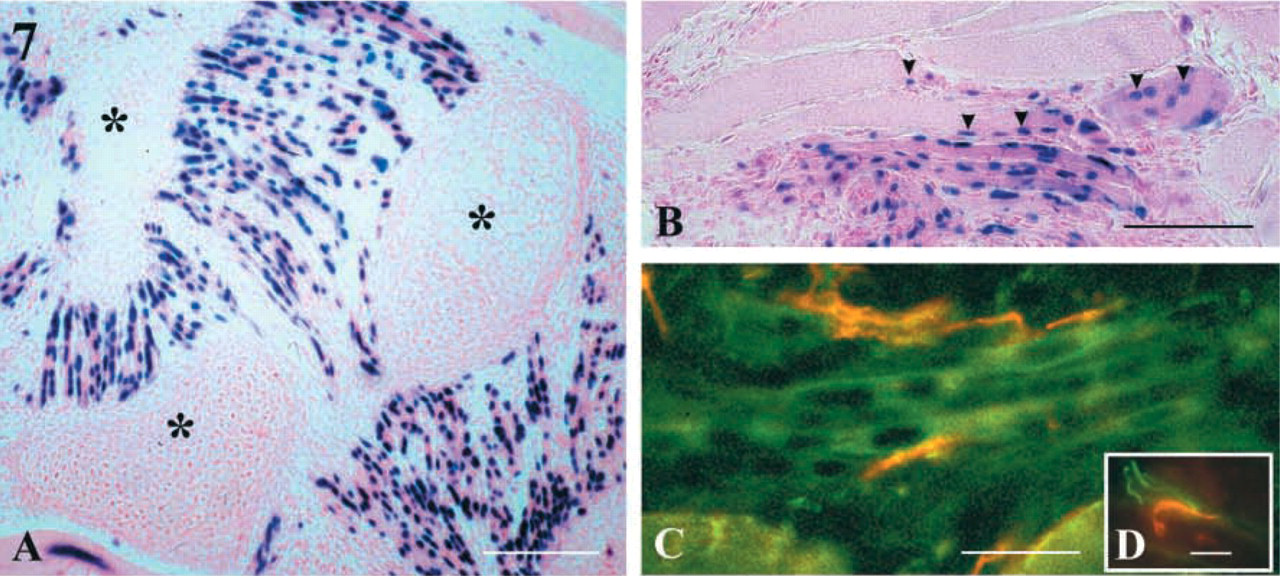
Interaction between the different cell types from 10-dpc desmin+/– mutant trunk cells differentiated in tibialis anterior muscle of an adult mouse host. Sections in the implanted zones were examined 15 days after surgery. (
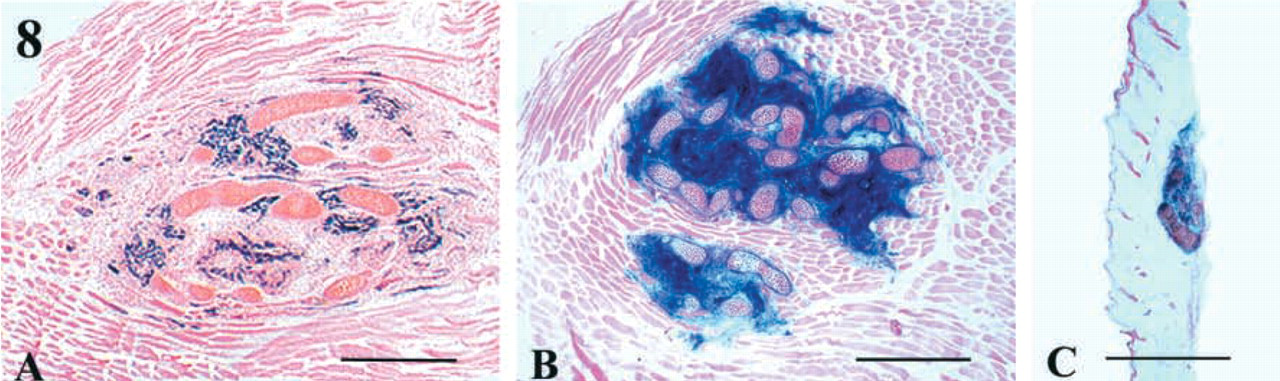
Tibialis anterior muscle of a 2-month-old mouse grafted with 10-dpc trunk cells from desmin+/– LacZ (A) and ROSA 26 (
Differentiation of the Osteogenic Lineage. In addition to myogenic and neurogenic cells, the trunks contained progenitors of skeletal elements of vertebral components and ribs that were located in the ventral zones of somites 14–24 at the time of extirpation. From 4 days, aggregations of mesenchymal cells into prechondrogenic condensations were scattered over the entire graft site. At this time, traces of matrix were present between and around cells (Figure 6A). Between 4 and 8 days after surgery, the prechondrogenic condensed mesenchyme differentiated into chondrocytes, which became hypertrophic and accumulated additional matrix. At 8 days cartilaginous masses elongated, and cells located in the center of these masses were round, often containing two nuclei and apparently arranged transversely to the long axis of the aggregation (Figure 6B). Chondrocyte maturation then led to the formation of a narrow cavity. The outermost cells of these masses lined up parallel to the surface to form the perichondrium.
Figure 6C shows a cartilaginous mass containing cells that reached different steps of chondrogenesis, i.e., pre-chondrogenic condensed mesenchymal cells, differentiated chondrocytes, and bone marrow cells. Osteoblast differentiation was assessed by the expression of osteocalcin, a bone matrix protein (Katagiri et al. 1994). This protein accumulated in all chondrogenic cellular aggregations formed from day 8 after surgery (Figure 6D).
Relationships Among Myogenic, Neurogenic, and Osteogenic Compartments from Trunk Cells Implanted into Adult Muscle. Donor myotubes formed near chondrogenic cells and attached to them. They were often arranged in parallel bundles extending between two cartilage zones and sometimes along them (Figure 7A). Donor myofibers outside these cartilage zones were aligned parallel to host fibers (Figure 7B). Combined anti-neurofilament and anti-myosin heavy chain treatment indicated that some new myotubes might have been contacted by nerve endings (Figure 7C). Staining of acetylcholine receptors (AchR) with α-bungarotoxin, in combination with anti-neurofilament antibody treatment, revealed nerve endings in close proximity to AchR expressed by the new myotubes (Figure 7D). These observations suggest that donor-derived myofibers were innervated.
Two weeks after injection, 28% on average (11 to 39%) of recipient muscle area was invaded by grafted cells (see Materials and Methods). Cartilaginous zones represented 32% on average (14 to 34%), and donor muscle fibers 17% (14 to 19%) of total graft area.
Influence of S Cells and NTN Cells on DM Cell Myogenesis
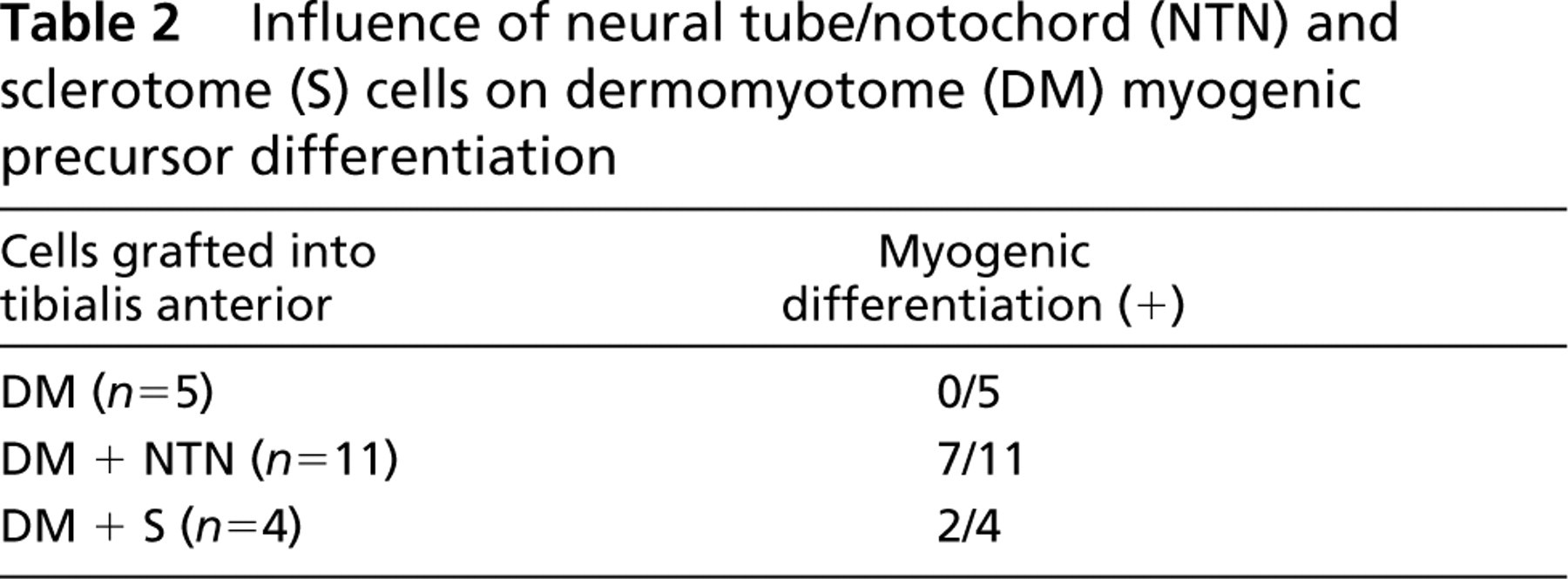
Enhancement of the number of cells undergoing new myofiber formation in trunk cell implantation appeared to reflect the effect of S and NTN cells. To investigate this hypothesis, DM cells were transplanted with either S or NTN cells. At 8 days after implantation, no myogenic blue nuclei were detected in muscles injected with DM cells alone, whereas those transplanted with DM + NTN cells exhibited blue β-Gal+ nuclei in 64% of grafts (7/11). When DM + S cells were grafted, myogenic blue nuclei were present in 50% of cases (2/4) (Table 2). These data support the hypothesis that NTN and/or S cells are required to maintain muscle differentiation. The high myogenic efficiency observed with the trunk cell suspension (100% of grafts contained β-Gal+ nuclei), which included S and NTN cells, suggested that a combination of these two cell types is needed for successful development of myogenic progenitors in transplanted muscle.
Differentiation of Trunk Cells Implanted Under the Skin
As expected from observations of 10-dpc desmin LacZ trunk cell injection (see above; Figure 8A), about one third of recipient muscle area was invaded by ROSA 26 trunk cells, which proliferated and differentiated (Figure 8B). When trunk cells were implanted under the skin, newly formed tissues were found in 50% of cases (2/4) examined 8 days after implantation, and the area occupied by donor-derived cells was about 10-fold less than that of muscle graft (Figures 8B and 8C). Under these environmental conditions, cartilaginous condensations appeared to be predominant (Figure 8C). When desmin+/– LacZ embryonic trunk cells were grafted under the skin, rare desmin LacZ+ cells and a few neurofilament-positive neural bundles were detected in the cases examined (n=4), and the grafts appeared to be constituted essentially of cartilaginous tissue (results not shown). On the whole, these results indicate that adult muscle was readily permissive to trunk cell development, as compared to the subcutaneous site.
Discussion
The purpose of our study was to evaluate the differentiation capacities of embryonic myogenic progenitors from heterozygous desmin+/– LacZ mouse embryos after transplantation into adult mouse muscle. Myogenic progenitors generated from DMs, LBs, and trunk cells of 10-dpc mouse embryos were able to proliferate and adopt a myogenic pathway. Although their development appeared to be limited for DM and LB cell transplantation, the differentiation of myogenic progenitors occurred readily when trunk cells, which associate DM cells with different cell types, were transplanted into adult muscle. In these conditions, not only myogenic cells but also neurogenic (NTN) and chondrogenic (S) cells differentiated. Our data indicate that both S and NTN cells present in the trunk cell suspension promoted myogenic development of DM cells.
Influence of neural tube/notochord (NTN) and sclerotome (S) cells on dermomyotome (DM) myogenic precursor differentiation
Adult Muscle Can Accommodate Myogenic, Neurogenic, and Chondrogenic Differentiation from Embryonic Trunk Cells
Temporal segregation of myoblast types may be the dominant mechanism regulating the normal fates of embryonic, fetal, and adult myofiber formation (Feldman and Stockdale 1992; Hartley et al. 1992; Yablonka–Reuveni 1995). Over the past decade, many experiments have shown that myogenesis during postnatal muscle growth and regeneration arises from satellite cells (adult myoblasts) (for reviews see Grounds 1999; Skuk and Tremblay 2000). Our results indicate that embryonic myogenic progenitors present in the trunk cell suspension retained their myogenic competence when introduced into an adult muscle environment, which was not the case for LB and DM cell suspensions. Embryonic myogenic progenitors contained in trunk cell suspensions were capable of surviving, proliferating, and fusing to form highly differentiated myofibers in adult muscle. Our quantitative analysis indicated that their proliferation was almost achieved 4 days after injection. In fact, the myogenic capacity of embryonic progenitors appears to be distinct from that of adult myoblasts. Other studies have shown that the proliferation of the surviving fraction of adult myoblasts injected into an immunodeficient irradiated mdx mouse host [an optimal environment for adult myoblast transplantation in recipient muscle (Morgan et al. 1990,1993)] ultimately reached 23.5% of the initial population after 4 days (Beauchamp et al. 1999). In addition, the dispersion of transplanted donor myoblasts away from the injection site was enhanced when host muscle was injured (Morgan et al. 1990; Watt et al. 1994). In our transplantation model, the number of donor-derived myogenic nuclei 4 days after injection was equivalent to 50.5% (56,583/112,000) of the initial myogenic population, and there was no evidence of movement of implanted embryonic myoblasts to nearby areas of muscle lesions.
The transplantation of trunk cells into adult muscle also resulted in the survival and differentiation of neurogenic embryonic progenitors. It is conceivable that this phenomenon was due to factors produced by recipient muscle. Indeed, some evidence indicates that skeletal muscle (the natural target or innervating tissue for motor neurons) expresses some of the neurotrophin family members involved in survival, axon growth, and branching of different neuron types (Wright et al. 1992; O'Leary and Daston 1994; Schnell et al. 1994). Robust chondrogenesis and bone formation recapitulating events occurring during skeletal development have also been observed when trunk-derived cells were grafted into adult host muscle. Lee et al. (2000) showed that a clonal population from highly purified myogenic cells genetically engineered to express BMP-2 was able to participate in ectopic bone formation in adult skeletal muscle. Moreover, it is believed that osteoprogenitor cells reside in skeletal muscle (Bosch et al. 2000). Taken together, these observations are consistent with the notion that adult muscle is permissive to differentiation of the chondrogenic as well as the neurogenic and myogenic cells present in trunk cell suspension.
Cossu et al. (1995) have suggested that embryonic cells, especially mammalian myoblasts, need to be surrounded by similar cells (in a three-dimensional aggregate) to acquire competence for differentiation (the “community” effect). However, our results indicate that contacts between similar cells are not required initially to induce trunk cells in specific differentiation pathways. If trunk-derived cells do not require a community effect, does this mean that they are able to differentiate independently of their location in the host? To address this question, the trunk cell suspension was injected into a subcutaneous environment, i.e., under the skin of the lumbar region. In these conditions, grafted cells proliferated poorly. Our results therefore imply that the differentiation of transplanted embryonic cells is influenced by environmental cells operating at the implantation site.
Neurogenic and Chondrogenic Cells Promote Myogenic Cell Differentiation into Adult Muscle
The fact that a greater number of myogenic cells formed in 4-day-old trunk cell than DM cell grafts suggests that both NTN and S cells have an initial beneficial effect on DM cells. The persistence of donor-derived myogenic cells after 1 week of implantation required the presence of NTN cells, S cells, or both, which implies that inductive signals from grafted NTN cells are involved in the specification and proliferation of donor myogenic cells. Among all candidate molecules that might account for the effects of NTN cells on somitic myogenesis in embryos, Shh appears to be of particular importance for the development of axial muscle cells. Some studies indicate that Shh induces myogenic differentiation (Munsterberg et al. 1995; Borycki et al. 1999), while others suggest a role in the regulation of muscle cell proliferation and lineage maintenance (Duprez et al. 1998). In addition to these two supposed effects of NTN cells on myogenic cells via Shh, the nerve contacts established at the level of newly formed myofibers may induce other myogenetic signals. Indeed, motor neurons are necessary for the growth, maturation, and survival of muscle cells (for review see Gundersen 1998). For example, shortly after contact is established between a growing motor axon and a differentiating myotube, signaling molecules are released by motor neurons, activating the transcription of muscle genes in synaptic nuclei (for review see Burden 1998). Developing myotubes appear to secrete large amounts of neurotrophic factors (Oppenheim et al. 1993) and NCAM (Covault and Sanes 1985). Because NCAM is implicated in muscle/nerve interactions and final innervation (Landmesser et al. 1988), it is conceivable that its local release by donor-derived developing myotubes in grafts might lead to innervation by host cells as well as neural implanted cells.
A previous study showed that inhibition of chondrogenesis by misexpressing Noggin resulted in a reduced number of muscle fibers, which did not appear to be properly arranged (Pizette and Niswander 2000). Moreover, stretch is an important factor in the organogenic behavior and growth of normal muscle fibers and in the regeneration of muscle in vivo from implanted muscle fragments (Carlson 1972; Vandenburgh 1988). In our grafts, the bone nodules that differentiated in the implantation zone provided anchorage points for newly formed muscle fibers, and parallel bundles of well-developed fibers were observed stretching between them. This implies that the differentiation of muscle tissue can be achieved through experimentally induced interactions between cartilage cores and fibers.
Our experiments indicate that the specific differentiation of myogenic, neural, and chondrogenic lineages is influenced by local cues transmitted by host muscle and by grafted cells themselves. It remains to be determined whether donor differentiated cells derive only from specified cells. Despite the presence of blue β-Gal myogenic cells in the suspension, the first blue cells were only observed 2 days after transplantation. Therefore, a rapid loss of specified myogenic cells occurred after transplantation, and the new myotubes formed in host muscle derived from unlabeled myogenic cells at the time of implantation. Recent studies have described in various types of tissues progenitor cells with a high degree of phenotypic plasticity. Under specific conditions these cells may give rise to different and embryologically unrelated derivatives. Such multipotential cells have been identified in most organ tissues, including hematopoietic, neural, gastrointestinal, epidermal, hepatic, muscle, and mesenchymal stem cells. In skeletal muscle, stem cells can acquire commitment, depending on the recipient tissue (for review see Cossu and Mavilio 2000; Seale et al. 2001; Grounds et al. 2002). This suggests that such cells, capable of differentiating myogenically within the muscle environment, were involved in our transplantation model. This could account for the high myogenic yield obtained from trunk cells. However, this was not the case for sclerotomal or neural tissue, because neural or sclerotomal cells grafted alone into tibialis muscle never differentiated into myogenic cells (data not shown). However, a better understanding of the mechanisms by which neural and sclerotomal precursor cells act on and/or participate in the differentiation of myogenic progenitors is needed to improve the success of embryonic myoblast transplantation in our experimental model.
Although embryonic myogenic progenitors appeared to be capable of fusing with regenerating host muscle fibers to form hybrid muscle fibers, this was a minor phenomenon compared to the large number of homotypic fibers formed by the fusion of donor cells. In hybrid myofibers the peripheral position of donor embryonic nuclei is probably related to the intrinsic characteristics of embryonic myogenic precursors. In growing muscle, these precursors migrate from the center to the periphery of the maturing fiber. Moreover, regeneration from neonatal muscle produces peripherally nucleated muscle fibers, whereas that from older muscle in mice gives rise to permanently centrally located nucleated fibers (Grounds et al. 1980; Morgan et al. 1993; Pastoret and Sebille 1995). Hybrid fibers were detected only at the periphery of the injection site. Although diffusible factors produced by freeze lesions performed at the two extremities of the muscle might induce the fusion of donor cells with hosts (Bischoff 1990), no hybrid fibers appeared near these damaged areas. Several explanations might account for this. First, the cryodamage inflicted on the proximal and distal parts of host muscle may not have been able to induce the dispersion of implanted embryonic myogenic precursors. Second, these precursors may have lost their capability to migrate at this developmental stage (Houzelstein et al. 1999). Finally, because the resident adult myoblasts were healthy, they may have competed with myogenic embryonic precursors for muscle repair. This last hypothesis is consistent with results showing that more donor cells are recruited to contribute to fiber repair and formation when host endogenous adult myoblasts are depleted (Alameddine et al. 1994; Beauchamp et al. 1999). Experiments are ongoing in our laboratory to create optimal conditions for enhancing the fusion of embryonic myogenic precursors with host fibers by reducing the regenerative potential within host muscle through pre-irradiation and by exacerbating the need for repair and regeneration of host muscle resulting from severe injury.
Footnotes
Acknowledgements
Supported by an AFM grant, by the CNRS, and by the University of Nantes.
We are grateful to Denise Paulin and Zenli Li for donating desmin mutant mice, to Fujisawa GmbH for providing FK506, to Maryvonne Zampieri for technical assistance, and to Prof Yablonka–Reuveni for helpful comments.
