Abstract
The mechanism(s) responsible for the progression of non-metastatic or borderline ovarian cancer to invasive Grade I/III ovarian cancer is still unknown. An epithelium-restricted integrin, αvβ6, is present in malignant epithelia but not in normal epithelia. We studied the relative expression and distribution of αvβ6 integrin in early and late-stage invasive (Grade I and Grade III) and non-invasive (benign and borderline) ovarian tumors of serous, mucinous, endometrioid, and clear-cell carcinoma subtypes, to assess its potential as a marker for epithelial ovarian cancer progression. Sixty-six specimens, including eight normal, 13 benign, 14 borderline, 13 Grade I, and 18 Grade III tumors were evaluated by immunohistochemistry (IHC) using a monoclonal antibody (MAb) against αvβ6 integrin. Normal ovarian surface epithelium was negative for αvβ6 integrin expression. All 45 carcinomas studied were positive, and the staining intensity significantly correlated with the grade of the tumor. The Grade III carcinomas of all types showed strong staining intensity. Only mucinous benign tissues were positive, and no reactivity was observed in benign serous neoplasms. On the basis of these observations, we hypothesize that the expression of αvβ6 integrin is associated with epithelial ovarian cancer and that a gradual increase in the expression of the molecule may be a correlative index of the progression of this disease.
O
Studies on normal and transformed cells have suggested that after malignant transformation striking changes occur in the ability of the cells to interact with their extracellular matrix (ECM) and other neighboring cells. Much interest in this respect has focused on the rapidly growing integrin family of cell surface receptors (Hynes 1992). The integrins are a group of transmembrane glycoproteins consisting of α- and β-subunits, which are integrated across the plasma membrane to provide a link between the ECM and the cytoskeletal molecules in the cells. There are two major families of integrins. Those in which the β1-chain combines with any one of nine α-chains and the αv group, in which the αv associates with either β1-, β3-, β5-, β6- or β8-subunits. The variable unit in both groups determines the ECM ligand specificity (i.e., fibronectin, laminin, vitronectin, or tenascin) for individual receptors. In addition to their role in cell adhesion, the integrins are also believed to be involved in cell differentiation, gene expression, proliferation, and survival/apoptosis.
αvβ6 integrin is highly expressed in developing fetal tissues and in a number of epithelial carcinomas and cancer cell lines (Breuss et al. 1993). In adult tissues, αvβ6 integrin plays a role in inflammation and wound healing through facilitation of the migration of epithelial cells to traumatized area and in the reestablishment of an intact epithelium at injured sites (Haapasalmi et al. 1996). The expression of αvβ6 integrin has been demonstrated in colon and pancreatic carcinomas, whereas no such expression was found in normal epithelium of the same origin (Weinacker et al. 1994). Increased expression of αvβ6 integrin in a range of epithelial neoplasms has been reported (Breuss et al. 1995). Moreover, recent studies have shown αvβ6 expression in breast and oral squamous carcinomas (Jones et al. 1997, Arihiro et al. 2000) and in premalignant oral epithelial dysplasias (Hamidi et al. 2000), suggesting that this integrin may be involved in malignant transformation. De novo expression of αvβ6 by transfection has also been reported to promote proliferation of colon cancer cells in vitro and increases tumor growth in nude mice (Agrez et al. 1994), consistent with the role of αvβ6 integrin in cancer growth and progression. Hence, the available data concerning the role of αvβ6 integrin support the hypothesis that overexpression of αvβ6 integrin may initiate transformed cells towards a more malignant phenotype, partially through alterations in cell proteolytic activities frequently implicated in metastasis.
The purpose of this study was to examine the expression of αvβ6 integrin in the main subtypes of human epithelial ovarian cancer to evaluate its possible association with histological grade and tumor subtypes. Our results show that αvβ6 expression is associated with ovarian cancer and that the expression of the integrin increases with advancing grade in all epithelial ovarian cancer subtypes. These data are consistent with the expression of αvβ6 integrin in other epithelial cancers.
Materials and Methods
The study was approved by Royal Women's Hospital, Melbourne Human Ethics Committee (HEC#99/32). Resected tissues not required for clinical analyses were obtained from patients who presented for surgery at the Oncology/Dysplasia Clinic at the Royal Women's Hospital, Melbourne, after the provision of participant information statements and only with informed consent. Normal ovaries needed for control comparisons were removed from patients undergoing surgery as a result of suspicious ultrasound images, palpable abdominal masses, and family history. The pathology diagnosis and tumor grade were determined from reports issued by the Department of Anatomical Pathology, Royal Women's Hospital, Melbourne.
The tissues were divided and frozen in cylinders of frozen section embedding medium (OCT) by immersion in isopentane cooled in dry ice. The tissues were then stored at −80C until needed. Frozen sections of the tissues were cut at 5-μm thickness and, if not used immediately, stored at −20C. For staining, sections were fixed in cold acetone for 15 min and held in Tris buffer (100 mM, pH 7.6). Endogenous peroxidase activity was removed using 3% H2O2 in methanol and endogenous biotin activity was blocked using a sequence of diluted egg white (5% in distilled water) and skim milk powder (5% in distilled water), all for 10 min each.
The sections were incubated for 1 hr in αvβ6 MAb (E7P6; Chemicon, Temecula, CA) diluted 1:200 in 1% BSA in Tris buffer (100 mM, pH 7.6). Antibody binding was amplified using biotin and streptavidin HRP (DAKO; Carpinteria, CA) for 15 min each and the complex was visualized using diaminobenzidine (DAB). Nuclei were lightly stained with Mayer's hematoxylin and the sections mounted and coverslipped. An isotype IgG1, suitably diluted, was substituted for the antibody as a negative control.
Sections were assessed microscopically for positive DAB staining by two trained pathologists. The degree of staining of αvβ6 expression was scored in a blind fashion as (-, 0%), (+, <20%), (++, 20–50%) and (+++, >50%), corresponding to 0%, <20%, 20–50%, and >50% of positive cells in tissue sections. The staining intensity was also scored as negative (0%), weak (<20%), moderate (20–50%), and strong (>50%) immunoreactivity. From each tissue, four sections were studied and the percentage of staining was determined by an average number of positively stained cells in four sections. In addition to the type of staining, tissue and cell distribution of staining was determined. Percentage of tissues having weak, moderate, and strong staining in each particular grade and subtype was scored. Parallel frozen sections were stained with hematoxylin and eosin to confirm the pathological diagnosis. Both hematoxylin and eosin and immunostained sections were reviewed independently by two pathologists with 100% agreement on cell type, grade, and immunohistochemical score.
For statistical analysis, χ2 analyses were used to test the association between the intensity of staining and the histological grade and subtype of tumor.
Results
Figure 1 shows the hematoxylin and eosin staining of normal and Grade III ovarian tumors. Figure 1A shows a thin layer of normal ovarian surface epithelium that is altered and replaced by tumor cells in Grade III tumors (Figures 1B–1E).
Normal Ovaries and Benign Serous Cystadenomas
No αvβ6 expression was observed in normal ovaries (n = 8) or in benign ovarian serous cystadenomas (n = 8) (Figure 2A and 2B) (Table 1).
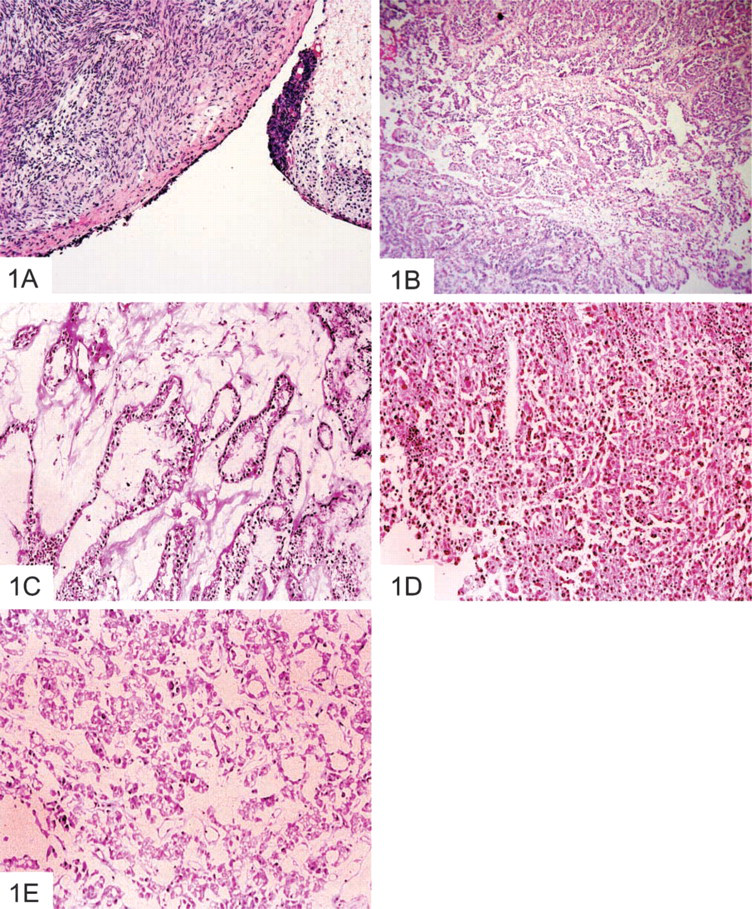
Hematoxylin and eosin staining of (
Borderline Serous Tumor (Tumors of Low Malignant Potential)
Eight patients with low-grade borderline ovarian cancer revealed weak (+) to moderate (++) αvβ6 expression (Figure 2C). Expression varied from strips of low profile cells with solid cytoplasmic staining to small groupings of cells and individual cells with paler, granular cytoplasmic staining. When more solid staining areas were present, these were associated with positive basement membrane staining. In some cases staining was confined to thin “endothelium-like” cells.
Grade I/III Serous Ovarian Adenocarcinomas
Five cases of Grade I tumors were available for examination. Four cases showed some areas of staining (++) that were confined to short strips of strongly staining “endothelium-like” cells with associated basement membrane staining. One case showed extensive strong similar staining. Ten Grade III serous ovarian adenocarcinoma cases were examined and showed moderate (++) to strong (+++) expression of αvβ6 integrin (Figure 2 D). Staining was mostly cytoplasmic or granular, and varied in intensity. In many serous ovarian adenocarcinomas, cell membranes also exhibited strong (+++) staining. Positive staining ranged from involvement of the majority of tumor cells to only scattered positive cells.
Benign, Borderline, and Grade I Mucinous Ovarian Tumors
Fifteen mucinous tumors were examined. These included five benign cystadenomas, six borderline tumors, and four classified as Grade I mucinous adenocarcinomas. All benign tumors demonstrated positive staining that was unlike than that seen in the benign serous group (Figure 3A). Smaller endocervical-type cells were strongly positive, whereas taller columnar cells exhibited more diffuse perinuclear staining. The basement membrane was stained in some areas and the glycocalyx was strongly outlined in many columnar cells. Staining patterns in the borderline tumors were similar to those found in the benign group (Figure 3B). In the tall columnar cells, cytoplasmic staining was sparse and mostly perinuclear, but was also found along most of the intracellular borders. The four Grade I mucinous tumors showed similar staining patterns, with large numbers of the epithelial cells staining strongly positive (+++) (Figure 3C).
Intensity of αvβ6 immunoreactivity in 66 normal ovarian and tumor tissues a
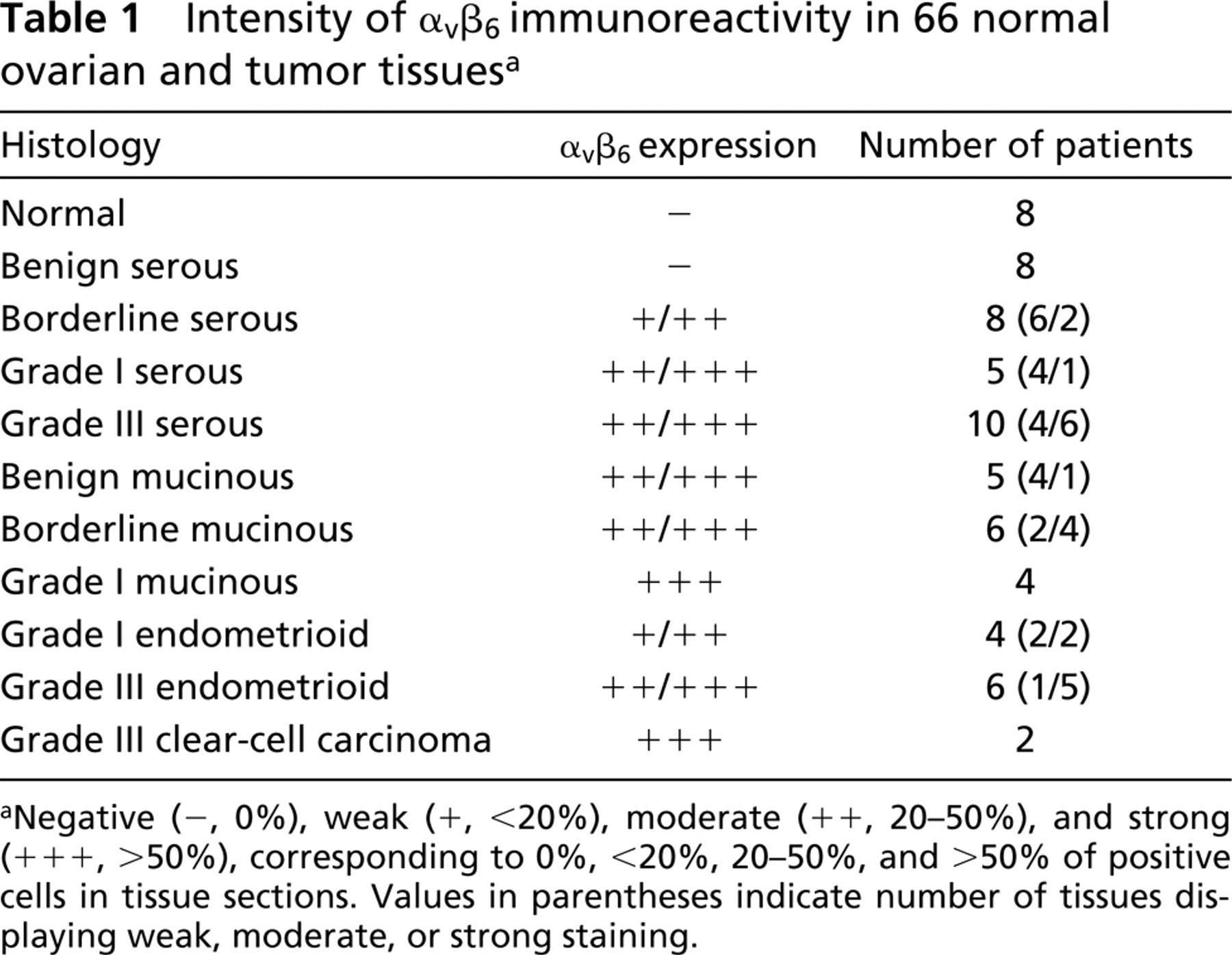

Negative (−, 0%), weak (+, <20%), moderate (++, 20–50%), and strong (+++, >50%), corresponding to 0%, <20%, 20–50%, and >50% of positive cells in tissue sections. Values in parentheses indicate number of tissues displaying weak, moderate, or strong staining.
Grade I/III Endometrioid Tumors
Ten endometrioid ovarian tumors were studied. The four Grade I tumors exhibited weak (+) to moderate (++) staining, which consisted of diffuse cytoplasmic staining and basement membrane staining in areas adjacent to the main tumor mass. Five of six Grade III tumors were strongly positive (+++). Multiple nests of cells showed diffuse cytoplasmic staining that varied in intensity (Figure 4A). In many areas the intracellular membranes were highlighted and in some areas the basement membrane appeared to be involved. There were also some individual cells with cytoplasmic staining in stromal areas.
Clear-cell Carcinoma and Transitional-cell Carcinoma
Two other ovarian cancers were examined. One was a Grade III clear-cell carcinoma and the other was a bilateral ovarian tumor, one being a transitional-cell tumor and the other mixed tumor having transitional, serous, and clear-cell phenotype.
The clear-cell tumor contained many scattered positively staining cell groups. Some of this staining was cytoplasmic and some of it was outlining cell membranes (Figure 4B). The pure transitional-cell tumor was negative, and the mixed tumor showed some staining in areas with clear-cell differentiation.
None of the tissues showed any positive staining with IgG1 isotype control.
Statistical Analysis
Specimens from 45 epithelial ovarian cancers were evaluated. αvβ6 integrin was present in 100% of the cases. Of the 45 cases, 14 were borderline and 31 were malignant tumors. Data indicated highly significant αvβ6 expression in malignant (Grade I/III) vs borderline tumors with χ2 = 12.57 (p = 0.01). Strong staining (+++) was present in 72% of Grade III tumors compared to only 28.5% of borderline tumors (Table 2). Weak staining, on the other hand, was present in 43% of borderline tumors vs 0% of Grade III tumors. Approximately 28% of Grade III, 46% of Grade I, and 28.5% of borderline tumors were moderately positive for αvβ6 integrin (Table 2).
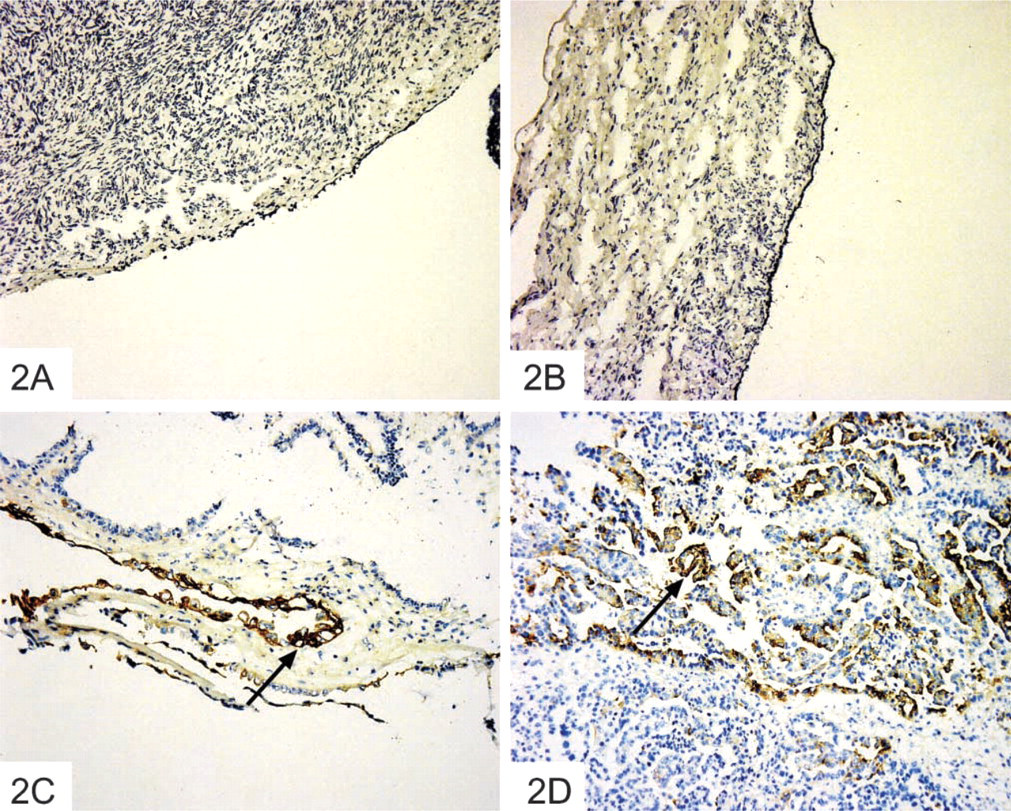
Expression of αvβ6 integrin in normal ovaries and serous ovarian cancer tissues. Cryosections of ovarian tissues were stained by the immunoperoxidase method for the expression of β6 integrin. (
Intensity of staining was compared to the histological subtype of tumors (Table 3). Specimens were divided into three groups: serous (n = 31), mucinous (n = 15), and endometrioid (n = 10). Statistical analysis revealed no significant differences in staining intensity among serous, endometrioid, and mucinous tumor subtypes with χ2 = 6.84 (p = 0.14) (Table 3).
Discussion
Ovarian cancer cells bind to various ECM constituents, but the integrin repertoire reported to date encompasses β1 integrin in complex with other integrin subunits such as α1, α2, α3, α5, and α6 (Cannistra et al. 1995). It has also been reported that αvβ3 expression occurs at a significantly higher rate in advanced ovarian tumors than in tumors of low malignant potential (Liapis et al. 1997), but as yet there is no correlation of the expression of αvβ3 integrin with grade and histology of ovarian tumors. It is possible that αvβ3 functions as an angiogenesis factor in ovarian cancer, as suggested for breast cancer (Brooks et al. 1995).
To date, the pathophysiology of the progression of ovarian cancer remains obscure. We have recently demonstrated the expression of αvβ6 integrin in ovarian cancer cell lines but not in normal ovarian cell lines (Ahmed et al. 2002). The expression of αvβ6 integrin in ovarian cancer cell lines correlates with the invasive potential of the cells (e.g., secretion of proteases, degradation of radiolabelled ECM), consistent with the function of this integrin in other cancers (Niu et al. 1998; Thomas et al. 2001). In this study we demonstrate the expression of αvβ6 integrin in neoplastic ovarian tissues but not in normal ovaries. Significant differences could be detected between the expression of αvβ6 integrin in non-invasive borderline tumors and invasive Grade III ovarian tumors. Invasive Grade III ovarian tumors showed strong expression throughout the entire tumor, whereas non-invasive borderline tumors showed localized staining confined to epithelial cells at the edges. Restricted expression of αvβ6 integrin in only neoplastic ovarian tissues may be important for cell migration and invasion because increased expression is found at the tips of migrating epithelial cells during wound healing (Larjava et al. 1996) and is closely associated with increased expression of fibronectin and tenacsin (Haapasalmi et al. 1996).
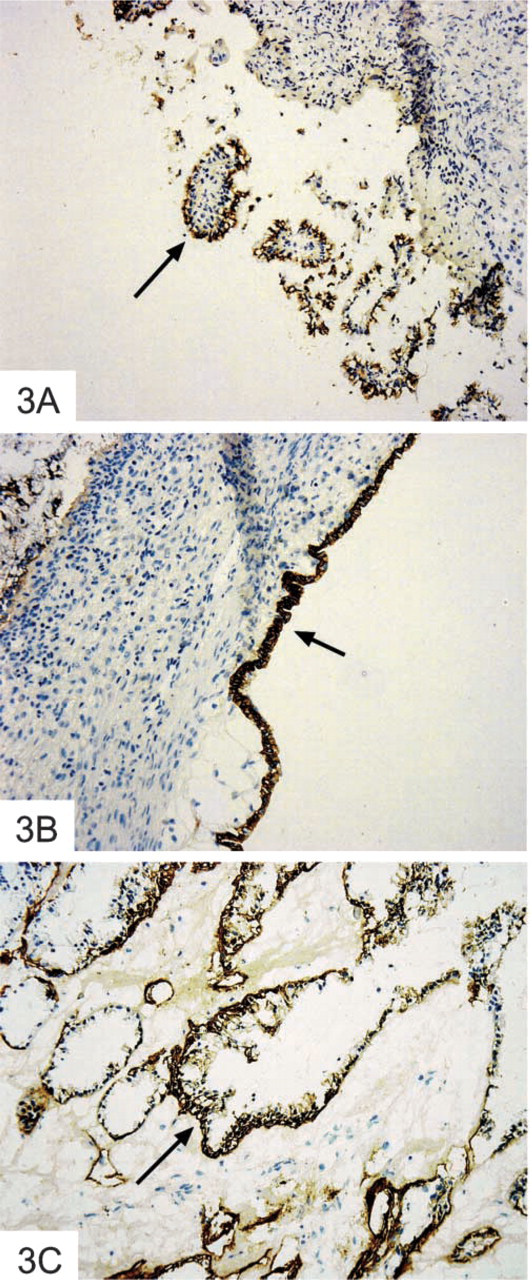
Expression of αvβ6 integrin in mucinous ovarian cancer tissues. Cryosections of ovarian tissues were stained by the immunoperoxidase method for the expression of β6 integrin. (
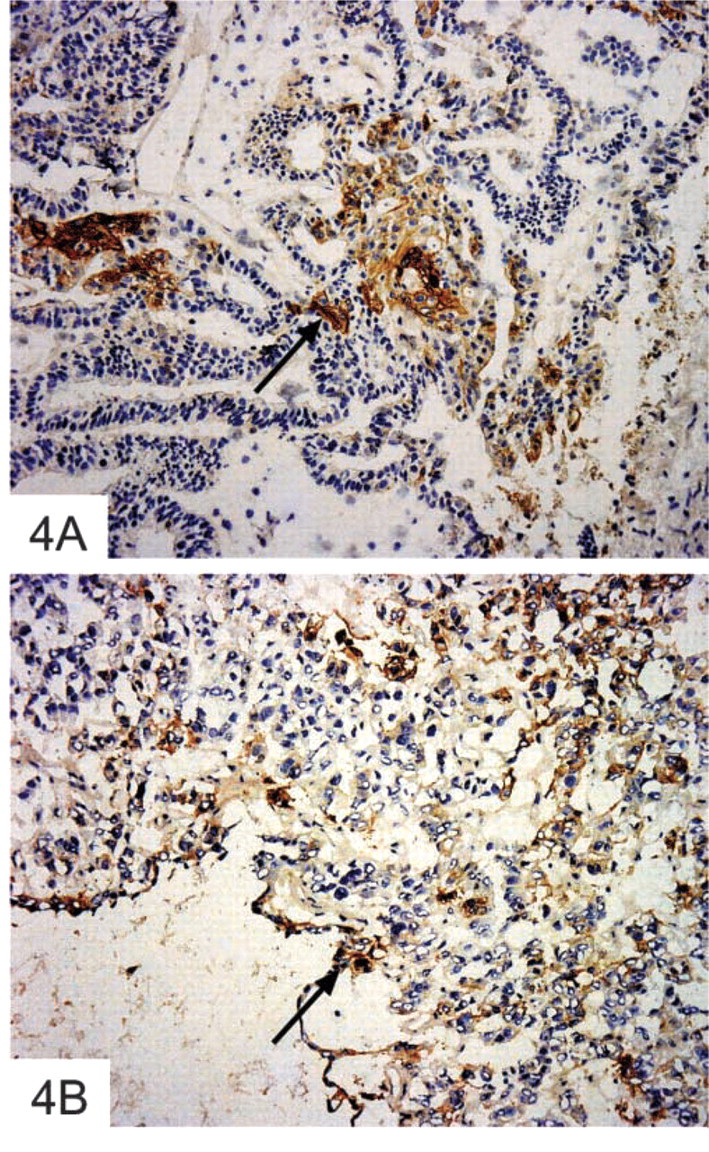
Expression of αvβ6 integrin in (
Intensity of αvβ6 integrin stain and tumor grade in serous, mucinous and endometrioid ovarian cancera
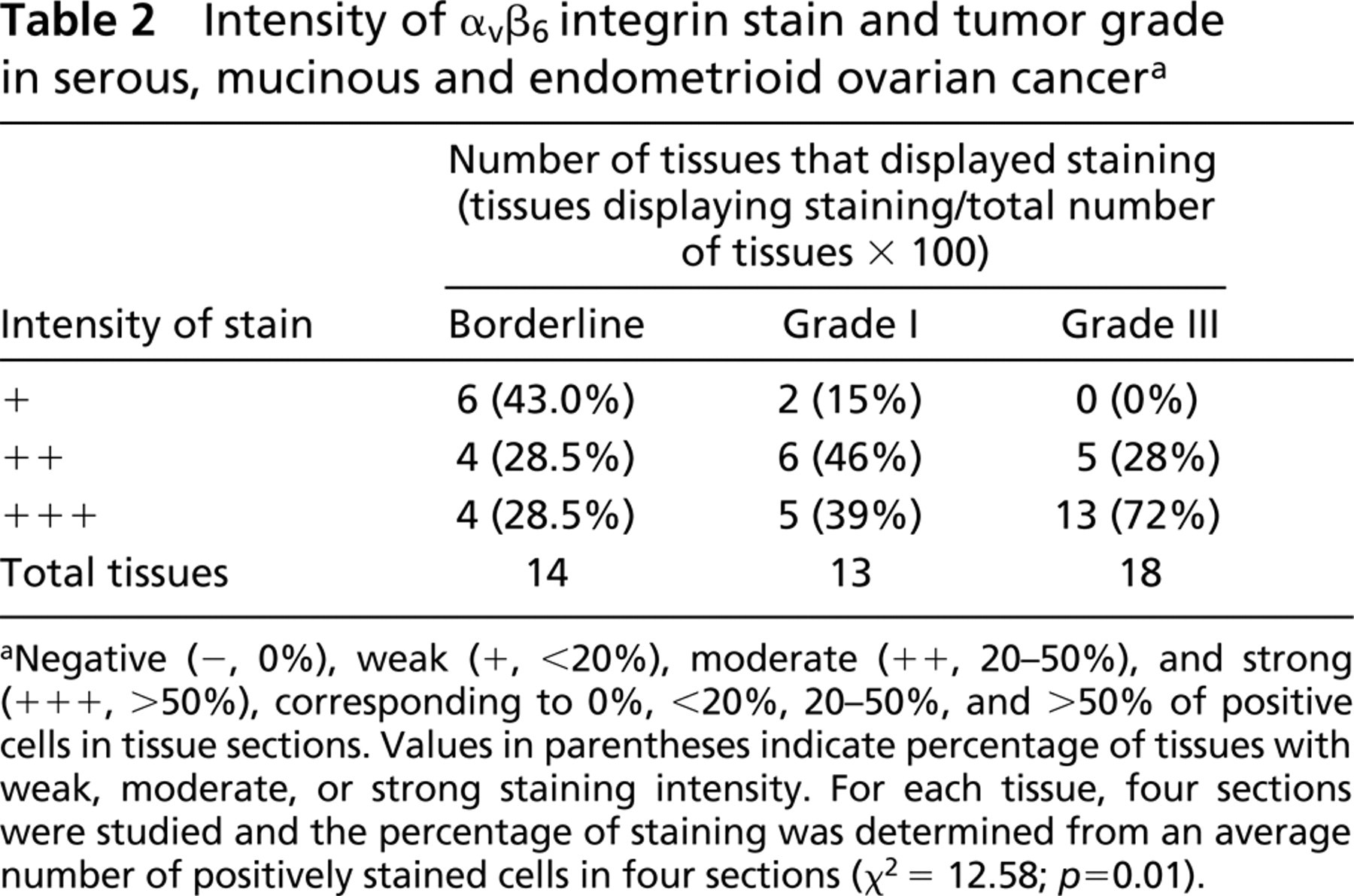
Negative (−, 0%), weak (+, <20%), moderate (++, 20–50%), and strong (+++, >50%), corresponding to 0%, <20%, 20–50%, and >50% of positive cells in tissue sections. Values in parentheses indicate percentage of tissues with weak, moderate, or strong staining intensity. For each tissue, four sections were studied and the percentage of staining was determined from an average number of positively stained cells in four sections (χ2 = 12.58; p = 0.01).
Mucinous tumors had stronger expression of αvβ6 integrin compared to other categories of epithelial ovarian tumors. These tumors frequently exhibit microscopically an admixture of benign, borderline, and malignant components. As a result, a spectrum of molecules of malignant and non-malignant type is shared by each grade of tumor and can appear in the same specimen (Young et al. 1999). Hence, benign mucinous tumors may contain malignant components, providing an exception to their benign status. Because αvβ6 integrin expression is associated with malignancy, the presence of this integrin in non-homogeneous benign mucinous tumors is not surprising. In addition, mucinous tumors are seldom classified beyond Grade 1. Tumors beyond this grade tend to be placed in an undifferentiated category.
Intensity of αvβ6 integrin stain in histological subtypes of ovarian cancer a
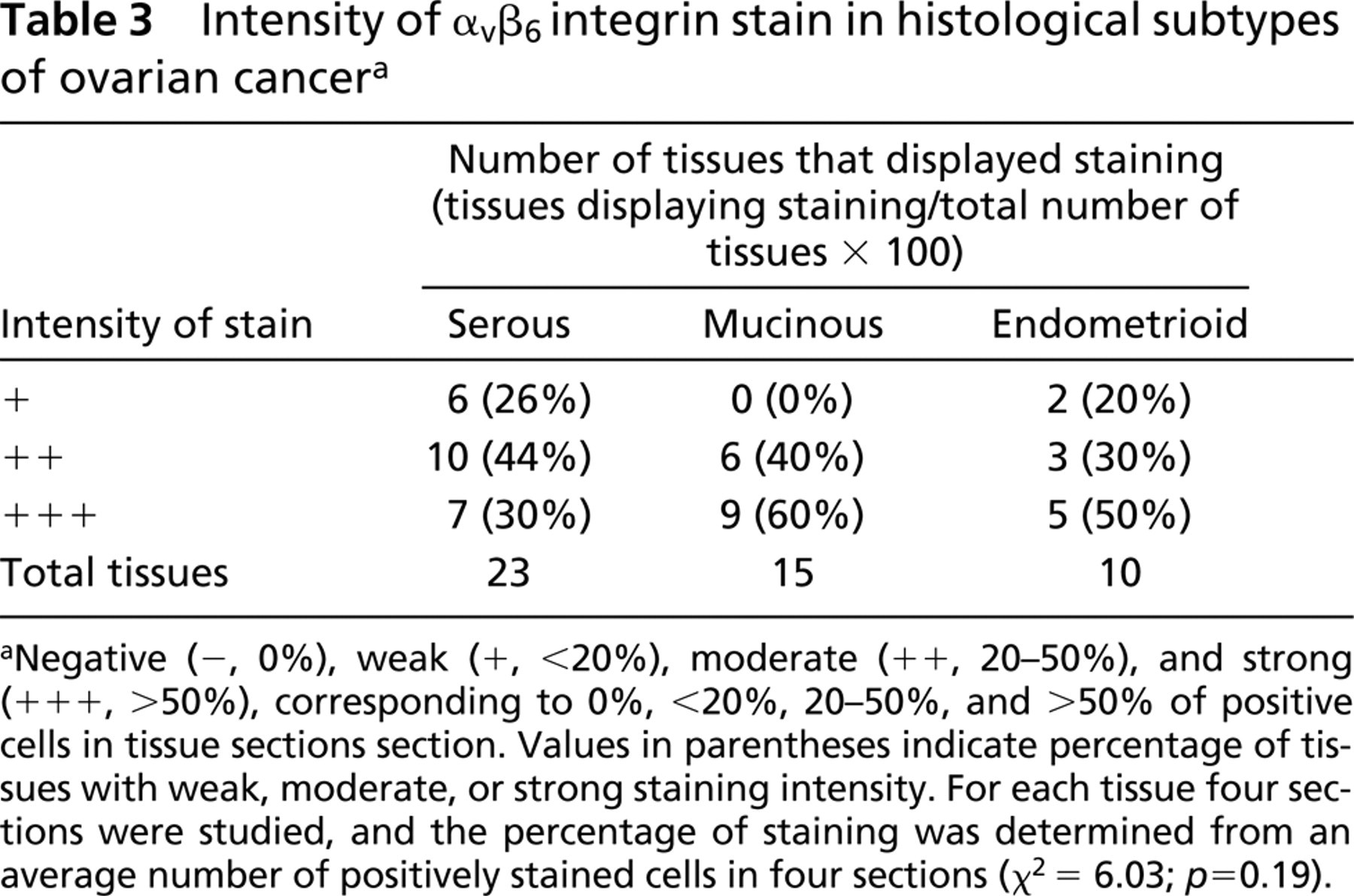

Negative (−, 0%), weak (+, <20%), moderate (++, 20–50%), and strong (+++, >50%), corresponding to 0%, <20%, 20–50%, and >50% of positive cells in tissue sections section. Values in parentheses indicate percentage of tissues with weak, moderate, or strong staining intensity. For each tissue four sections were studied, and the percentage of staining was determined from an average number of positively stained cells in four sections (χ2 6.03; p = 0.19).
Changes in the expression and/or function of the integrin receptors have been reported in a number of epithelial tumors (Jones et al. 1997; Korhonen et al. 1992). It has been suggested that loss of function and/or synthesis of these and other adhesion molecules may be strongly favored by selection and may contribute to the uncontrolled pattern of growth typical of malignant tumors. Changes in the expression of β1 and β4 integrins in oral squamous cell carcinomas have also been studied (Jones et al. 1993), and recent studies have suggested that αv integrins are important in modulating the behavior of epithelial cells (Clark et al. 1996). αvβ4 integrin, which normally is a component of hemidesmosomes, is lost or exhibits aberrant expression in various cancers (Juliano and Varner 1993), and αvβ3 integrin is upregulated significantly during the invasive stages of both melanoma and glioblastoma (Marshall and Hart 1996). Localization of the αvβ4 laminin receptor within the cell and the cell membrane in poorly differentiated ovarian carcinomas is changed compared with normal epithelia (Bottini et al. 1993). This change is associated with altered laminin in the cell membrane of ovarian cancer cells, suggesting a relationship between altered production or degradation of ECM components of ovarian cancer cells and the αvβ4 receptor. Moreover, genetic expression of α5β1 integrin in Chinese hamster ovary (CHO) cells resulted in suppression of tumor growth in nude mice (Giancotti and Ruoslahti 1990). Complementing these results, it has been shown that α5-deficient CHO cells manifest increased tumorgenicity, suggesting a role for this integrin in cancer progression (Schreiner et al. 1991). In this study we have focused on αvβ6 integrin, triggered by our finding of the expression of this integrin in metastatic ovarian cancer cells.
There is a gradual increase in the expression of αvβ6 integrin from borderline to malignant tumors. There is also a progression in the intensity of staining from the well-differentiated to the poorly differentiated cancers. This is consistent with increased expression of αvβ6 integrin in oral squamous carcinomas (Jones et al. 1997) and breast carcinomas (Arihiro et al. 2000). In malignant keratinocytes and colon cancer cells, induced expression of this integrin enhances MMP-9 secretion and MMP-9-mediated invasion (Thomas et al. 2000; Agrez et al. 1999). On the other hand, inhibition of αvβ6 function by using inhibitory antibodies results in total abrogation of MMP-9 activation (Thomas et al. 2001), suggesting that the expressions of αvβ6 integrin and MMP-9 are linked, and their coordinate expression appears to promote invasion by squamous and colon carcinoma cells. Recently, we have also shown that the expression of αvβ6 integrin in ovarian cancer cells correlates with enhanced uPA, MMP-2, and MMP-9 secretion and the protease-dependent matrix degradation (Ahmed et al. 2002). Inhibition of αvβ6 function results in complete abolishment of matrix degradation (Ahmed et al. 2002). Although uPA and MMP-9 are not detectable in normal epithelium, their expression has been reported in ovarian cancer tissues (Pujade-Lauraine et al. 1993). Several studies have suggested that uPA and MMP-9 contribute significantly to ovarian cancer progression (O'Toole et al. 1999) and that these proteases have a major functional role in ovarian cancer metastasis (Dolo et al. 1999). These observations are consistent with our hypothesis that the expression of αvβ6 integrin in ovarian cancer tissues may be a prerequisite for the in vivo coordinated changes associated with invasion and migration of malignant ovarian cells.
Whether or not αvβ6 integrin expression in human ovarian cancer is an independent prognostic factor in survival and disease-free period remains to be elucidated. However, because our study demonstrates the absence of αvβ6 integrin in normal ovaries and its presence in all subtypes of ovarian cancer, it poses the possibility of being evaluated as a potential initiator of ovarian cancer progression.
Footnotes
Acknowledgments
We thank the Research Advisory Committee of the Royal Women's Hospital, Melbourne, Ovcare and Jigsaw Women's Fashion Company, and the Jack Brockhoff Foundation, Australia for supporting this work. NA was in receipt of a RoCan Fellowship in Ovarian Cancer and a grant-in-aid from the Anti-Cancer Council of Victoria during the course of the study. The support of the Rotary Club of Williamstown and the Anti-Cancer Council of Victoria is gratefully acknowledged.
