Abstract
Migrants whose culture and language(s) differ from those of their resettlement country often experience various inequities impacting wellbeing. While this has been explored for some aspects of migrant health, less research has focused on families who have children in resettlement. This reflects a gap in knowledge considering stressors caregivers face across the “First 2,000 Days” (conception to age 5). This study explores how one group of migrant caregivers—from South and Southeast (S/SE) Asia—experience help-seeking and support across the First 2,000 Days in Australia, with a focus on facilitators to culturally responsive care that promotes health equity. Thematic analysis was used to analyze semi-structured interviews with 11 S/SE Asian migrant caregivers and 22 service providers. Findings were explored through Andersen’s Behavioral Model of Health Service Use and the Health Equity Framework. Participants described formal supports for wellbeing as inaccessible and/or not culturally responsive, and caregivers often sought help for wellbeing only when need was severe. Participants noted organizational and community recommendations to address barriers including staff education, culturally responsive communication, and continuity of care (organizational), and collaboration with existing informal networks (community). A model for help-seeking and health equity is proposed for further understanding these experiences for marginalized groups.
Introduction
The First 2,000 Days (defined as the period from conception to age five) are a critical period in which many developmental outcomes for children are established, with associated implications across the lifespan (Heenan et al., 2023; NSW Health, 2019). Therefore, the First 2,000 Days present an opportune time to promote holistic wellbeing (including physical, psychological, social, and spiritual domains; World Health Organization [WHO], 2023) in families (Heenan et al., 2023). This also involves ensuring caregivers have access to culturally responsive formal and informal supports for themselves and the children in their care and are empowered to seek help to support their own wellbeing (Heenan et al., 2023; NSW Health, 2019). However, there is a growing body of research highlighting wellbeing inequities for migrant caregivers and their children in the First 2,000 Days (Billett et al., 2022; Giallo et al., 2017). Compared to the general population, inequities for migrant caregivers include worse wellbeing in general, fewer formal and informal supports and/or less satisfaction with these supports, lower levels of help-seeking for wellbeing, as well as gaps in the provision of culturally responsive care (Heslehurst et al., 2018). While these inequities are well established in the literature, how to promote and facilitate health equity in the First 2,000 Days for migrant caregivers is less well understood. The current study centered on migrants from South and Southeast (S/SE) Asia considering the gap in knowledge related to wellbeing postresettlement particularly for migrants from this region (Aiyar et al., 2023). Specifically, this study drew on interviews with S/SE Asian migrant caregivers and service providers with experience working with this group of caregivers across one or more of the WHO domains of wellbeing (WHO, 2023). The study aimed to explore the help-seeking and formal and informal support experiences of S/SE Asian migrant caregivers in the First 2,000 Days, with a focus on facilitators to culturally responsive care that promotes health equity.
Terminology
In this study, we use “migrant” to describe different subgroups including “migrants” who leave their country voluntarily and may safely return at any point, and “refugees” who have left their country involuntarily, received refugee status, and are resettled in another country (United Nations High Commissioner for Refugees [UNHCR], 2016). While the migration histories and life experiences of these groups are diverse, both may face similar wellbeing challenges and comparable experiences of formal and informal supports across the First 2,000 Days in a resettlement country (Billett et al., 2022; Giallo et al., 2017; Olcoń et al., 2023). As noted above, this study focused on migrant caregivers from S/SE Asia in light of the lack of research on wellbeing in the First 2,000 Days for people from this region (Aiyar et al., 2023). Countries classified under the South Asian subregion include Afghanistan, Bangladesh, Bhutan, India, Maldives, Nepal, Pakistan, and Sri Lanka (World Bank, 2023). The Southeast Asian subregion includes Brunei, Cambodia, East Timor, Indonesia, Myanmar, Laos, Malaysia, Philippines, Singapore, Thailand, and Vietnam (Association of Southeast Asian Nations [ASEAN], 2020).
This study follows the WHO’s definition of wellbeing, where “. . . well-being is a positive state experienced by individuals and societies. Similar to health, it is a resource for daily life and is determined by social, economic and environmental conditions” (WHO, 2021). In addition, wellbeing is considered multidimensional, encompassing physical, mental, psychological, emotional, spiritual, and social dimensions (WHO, 2023). As such, in understanding support experiences for migrant caregivers, this study considers wellbeing—and associated types of support or care—across all these domains.
Background
Prior research has shown that migrant caregivers often experience increased psychological distress across the First 2,000 Days compared to non-migrant caregivers (Giallo et al., 2017; Lansakara et al., 2010). A review of the experiences of S/SE Asian refugee caregivers in the First 2,000 Days noted that they experienced various challenges to physical and emotional wellbeing including concerns around nutrition, breastfeeding, anxiousness, and distress in maternity care settings (Aiyar et al., 2023). S/SE Asian migrant caregivers have similarly reported emotional and mental health challenges in pregnancy and postbirth, often stemming from factors related to being a migrant, including social isolation or separation from family (Mustafa & Kittleson, 2016; Niner et al., 2013).
In addition, previous literature suggests lower help-seeking for mental health for S/SE Asian migrant groups despite the presence of identifiable mental health concerns (Maheshwari & Steel, 2012; Maneze et al., 2016). Factors that may contribute to these reductions in help-seeking include stigma (Maheshwari & Steel, 2012; Maneze et al., 2016), language barriers, unfamiliarity with navigating new systems, and cost or availability of services (Maneze et al., 2016; Saunders et al., 2016). Help-seeking and support-related challenges may also be experienced in terms of other formal or informal supports for wellbeing in the First 2,000 Days (Saunders et al., 2016). Formal support in these contexts typically includes mainstream services—government-funded or private—such as medical or health care (e.g., general practice, psychology, hospital midwifery services); education (e.g., early childhood education and care, schools); and specialist refugee and migrant services (e.g., settlement support, housing). Informal supports generally refer to extended social networks, which may include friends, neighbors, cultural community, or community leaders (Saunders et al., 2016).
In addressing inequities among migrant caregivers in terms of access to support and poorer psychological wellbeing (Giallo et al., 2017; Rees et al., 2019), guidelines in Australia and internationally have underscored the need for culturally responsive care (Care Quality Commission, 2024; Migrant and Refugee Women’s Health Partnership, 2019). Practitioners and institutions that provide culturally responsive care respect the cultural identities, practices, and care preferences of clients and consider how culture shapes clients’ experiences of wellbeing and help-seeking (Markey & Ibeajaero, 2022). An understanding of migrant caregivers help-seeking and support experiences is especially important during the First 2,000 Days in considering the significance of this period for families in relation to lifelong wellbeing. There is also a need for research to explore wellbeing for extended family members who, often in S/SE Asian families, provide care for children (Kurrien & Vo, 2004).
Conceptual Frameworks
In responding to the aims, this study drew upon Andersen’s Behavioral Model of Health Services Use (Andersen, 1995) and the Health Equity Framework (HEF; Peterson et al., 2020).
Andersen’s Behavioral Model of Health Services Use
Andersen’s (1995) model has been widely used in previous literature in understanding health service utilization across different populations and cultural groups (Alkhawaldeh et al., 2023). Other conceptual framings that relate to accessing services and that consider the role of culture include Kleinman’s explanatory model, which views health and illness as directly related to culture and specific contexts (Kleinman, 1980). In addition, the Levesque et al. (2013) framework explores access to health care, accounting for social and cultural factors in exploring the suitability of specific health care. However, neither of these models speaks to help-seeking as an experience and behavior, situated within specific systems. This is relevant given this study centered on help-seeking for S/SE Asian migrant caregivers in the First 2,000 Days, to understand the experiences and choices of migrants despite the potential challenges they may face within health systems (Burford-Rice et al., 2022; Shafeek Amin & Driver, 2022). As such, this study drew upon Andersen’s (1995) model to conceptualize help-seeking, following previous research regarding wellbeing for migrants (e.g., Due et al., 2020).
Andersen’s (1995) model includes three factors that interact to determine an individual’s likelihood to seek help or access services (Figure 1). Predisposing factors include demographic characteristics (e.g., age), social factors (e.g., ethnicity), health beliefs, cultural norms, and community values. Enabling factors are logistical factors related to health services use and include knowledge of services. Need factors prompt help-seeking, generally due to immediate issues such as psychological distress and pain (Andersen, 1995, p. 8).
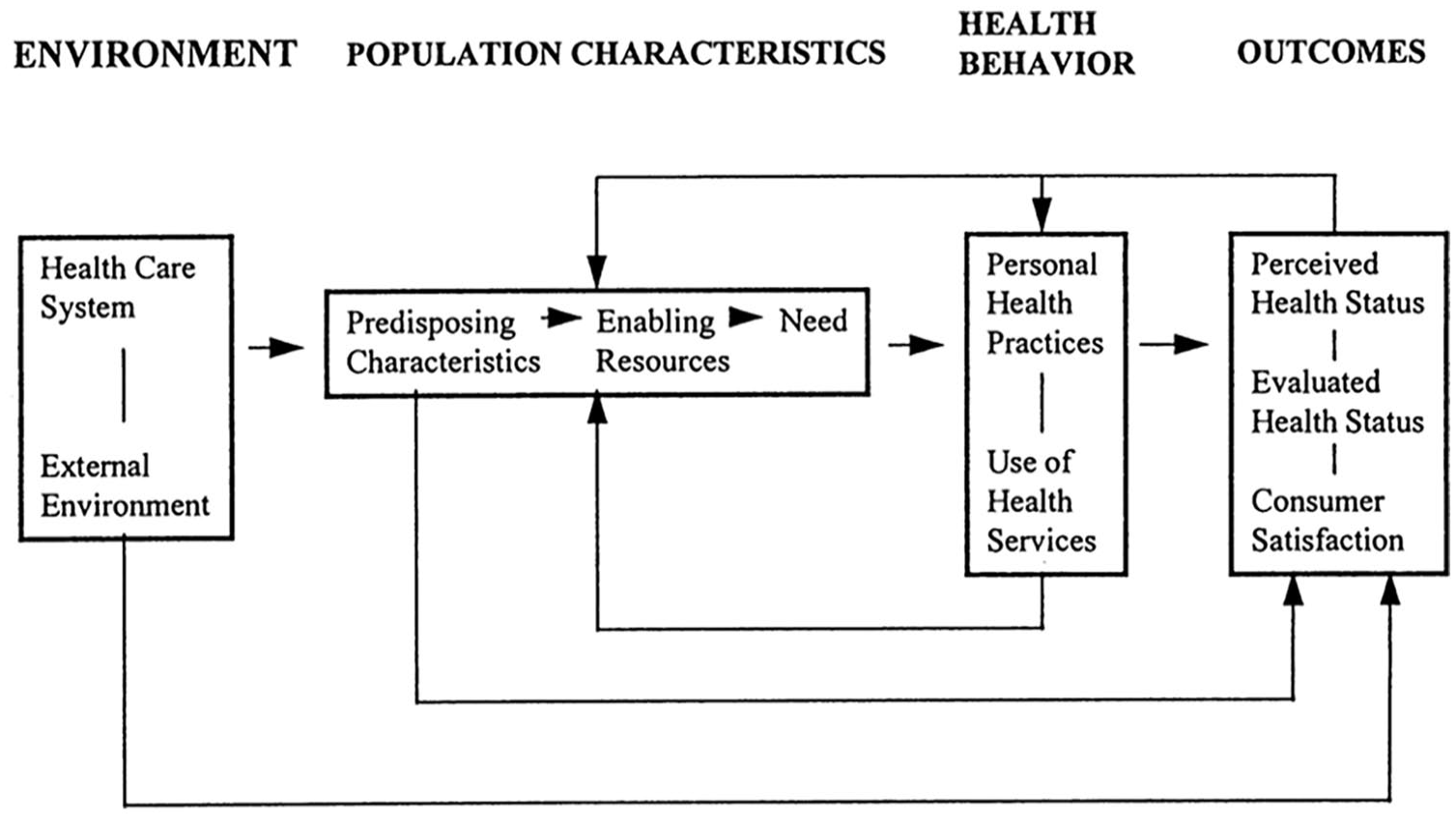
Andersen’s (1995) Emerging Behavioral Model (p. 8).
The HEF
The HEF (Peterson et al., 2020) explains “health equity” as “having the personal agency and fair access to resources and opportunities needed to achieve the best possible physical, emotional, and social well-being” (p. 742). The HEF includes four spheres of influence, representing groups of risk and protective factors for health outcomes: systems of power, relationships and networks, individual factors, and physiological pathways (Peterson et al., 2020; see Supplementary for a visual representation of this framework). The present study specifically used the systems of power, relationships and networks, and individual factors spheres, as they are most relevant in terms of access to support and caregiver wellbeing. The physiological pathways sphere was not included, as physiological responses and factors were out of scope regarding the aims of this study.
The systems of power dimension involve policies and practices that impact fair access to formal health care services. Reformed systems of power may resolve historical and present sources of inequity, advance health outcomes, and promote fair access to care. For systems of power that remain unchecked and where social, economic, or environmental benefits are provided to some groups over others, inequities may intensify (Peterson et al., 2020). The relationships and networks dimension consists of social networks and informal supports such as family or cultural communities. These networks may function as protective sources from unfavorable health behaviors or sources that add to experiences of stigma, which may result in poorer health outcomes (Peterson et al., 2020). The individual factors sphere reflects how people use their attitudes, skills, or behaviors to respond to social, economic, or environmental situations. Health equity may be promoted by addressing individual-level attitudes, skills, or behaviors that strengthen personal or community health (Peterson et al., 2020). The HEF has not been directly employed in previous empirical research with migrant communities but has been used as a framework in research exploring health equity for minority racial groups (Donley, 2023).
Australia’s Health System
In Australia, both federal and state/territory policies inform the health care system. Specifically, Australia’s national government subsidizes most primary health care—typically general practitioners (GPs), who are the first line of practitioners through which people access support, including referrals to specialized services such as mental health care (Fisher et al., 2022). GP services are subsidized by Medicare, Australia’s universal public health care insurance scheme (Fisher et al., 2022). This system means that in terms of maternity, wellbeing, and other relevant support services across the First 2,000 Days, there are often state-level differences in the way health care is organized, as well as the available supports for migrant caregivers and their families across Australia (Fisher et al., 2022).
Where visa conditions for migrants allow access to Medicare, migrant caregivers having their baby through Australia’s public health system may not incur costs (Department of Health and Aged Care, 2022). It is also important to highlight that temporary (often humanitarian) visa holders have faced restrictions in the past in terms of accessing Medicare, a policy that requires migrants to pay substantial fees for almost all formal wellbeing support services (Khatri & Assefa, 2022).
Current Study
In light of the lack of literature that focuses on a specific group of migrant caregivers in specific resettlement countries in the First 2,000 Days, the current study aimed to explore the help-seeking and formal and informal support experiences of S/SE Asian migrant caregivers across the First 2,000 Days in Australia, with a focus on facilitators to culturally responsive care that promotes health equity.
Method
Participants
To address the aims and research questions, semi-structured interviews were conducted with two groups of participants: 11 S/SE Asian migrant caregivers (n = 9 mothers, n = 1 grandmother, n = 1 father) and 22 service providers. Table 1 provides information about migrant participants with other details provided in aggregate form below to maintain confidentiality.
Migrant Caregiver Demographics.
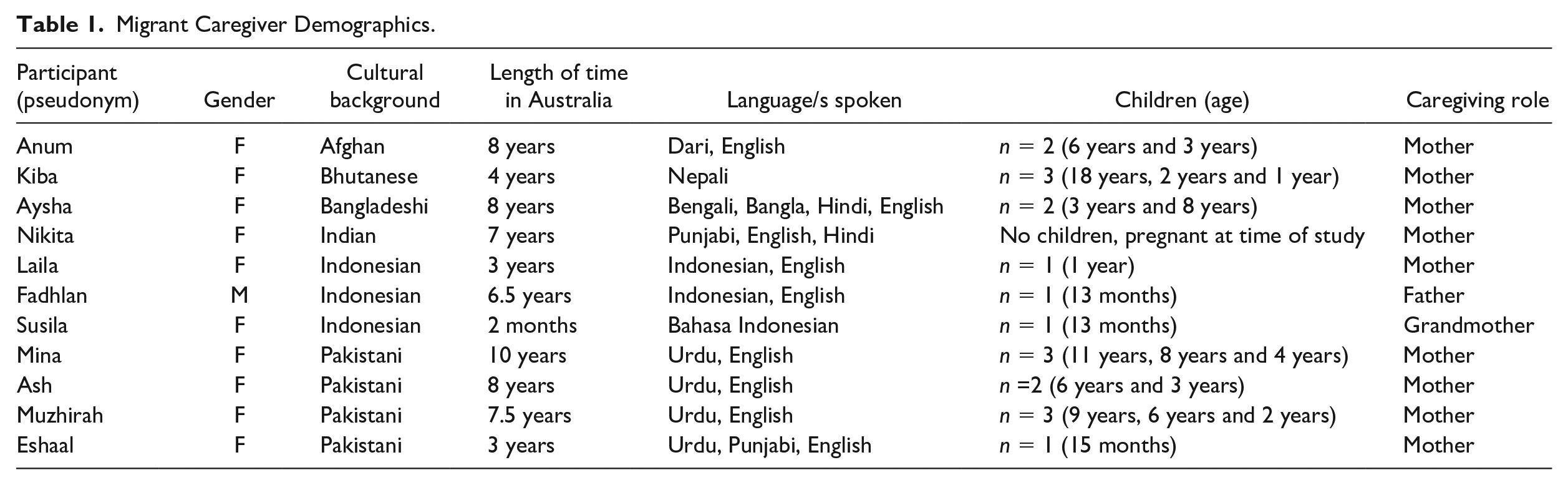
Migrant caregivers, with ages ranging from 26 to 54 years (M = 35.27 years, SD = 8.13), reported a range of residency statuses including Australian citizens (n = 4), temporary migrant visa holders (n = 4), and permanent residents (n = 2), and one person held a permanent humanitarian (refugee) visa. Eight mothers were from South Asian Backgrounds including Afghan (n = 1), Bangladeshi (n = 1), Bhutanese (n = 1), Indian (n = 1), and Pakistani (n = 4). Three participants from Southeast Asia were from Indonesia and included a mother, father, and grandmother from the same family unit (interviewed separately). Bangladeshi, Indonesian, and Pakistani caregivers reported their religious background as Muslim (n = 9), one Bhutanese caregiver reported Christian, and one Indian caregiver reported Hindu.
Criteria for service providers’ field/s of employment were kept broad to include those who had experience supporting S/SE Asian migrant caregivers in the First 2,000 Days broadly related to wellbeing. Service providers had an average of 19.5 years’ experience supporting migrant background clients (SD = 13.18) across various roles including the medical sector in the fields of general practice, nursing, and midwifery; allied health in the fields of counseling, psychology, psychotherapy, physiotherapy, and social work; or in the community services sector including fields related to consumer advocacy, community development, and financial inclusion. Providers ranged in age from 28 to 66 years (M = 47 years, SD = 11.70) and were mostly women (n = 21 women, n = 1 man). Seven service providers were from a South Asian background (Afghan, Australian-Afghan, Bhutanese, Indian, Nepali, and Pakistani) and one from a Southeast Asian background (Vietnamese).
Procedure
Ethics approval was obtained from The Women’s and Children’s Health Network Human Research Ethics Committee on October 13, 2021 (approval number: 2021/HRE00313). Inclusion criteria for caregiver participants were (a) arrival in Australia within the past 10 years as a refugee or migrant (to ensure recency of experiences), (b) S/SE Asian ethnic background, (c) over 18 years of age, and (d) were pregnant, or self-identified as having an active caregiving role for a child less than 5 years old born in Australia. One participant from Bangladesh had birthed overseas; however, her data were included as she reflected on her experiences in Australia during her child’s early years. Inclusion criteria for service providers were that they were over the age of 18 and provided support to S/SE Asian migrant caregivers that broadly involved wellbeing in the First 2,000 Days. In addition, criteria regarding the supports accessed by S/SE Asian migrant caregivers in the First 2,000 Days were kept broad to include various services that commonly provide wellbeing support for caregivers. This therefore included formal supports such as mainstream medical and health care services (e.g., psychology, general practice, maternity care); child care; and specialist refugee and migrant services, and informal supports including community leaders or volunteers, playgroups, or women’s groups (which may also be run through or linked with formal services).
Participants were recruited via convenience and snowball sampling. Study flyers were circulated through community organizations and social media, and the first author attended multicultural community groups. The first author conducted all interviews (M = 41 minutes) between April and December 2022. Three caregivers were interviewed using interpreters from a professional interpreting agency used regularly by the authors. Care was taken to ensure that interpreters were culturally appropriate (e.g., in relation to gender, ethnicity, or dialect). In line with best practice, interpreters were briefed on the study including the sensitive content to ensure the safety of the participants and the interpreters themselves (Gartley & Due, 2017).
Semi-structured interview guides were informed by previous research highlighting an absence of literature regarding understandings of wellbeing and support experiences and factors influencing culturally responsive care for S/SE Asian migrant caregivers in the First 2,000 Days (Aiyar et al., 2023). As such, interview topics related to caregivers’ wellbeing and health care experiences and barriers or facilitators to help-seeking in the First 2,000 Days. These questions were asked in relation to support services for caregiver and/or child wellbeing (e.g., psychological or physical), early childhood education and care, or maternity care. Examples of questions included, “What are some of the things that have helped you or would help you in accessing support for pregnancy, parenting or wellbeing?” (for caregivers) and “How do you think services for these women and their families could be improved?” (for service providers and caregivers). All participants received a $40 AUD shopping voucher. Interviews were audio-recorded and manually transcribed, and participants were assigned a pseudonym.
Data Analysis
The study was guided by Tracy’s (2010) guidelines for methodological rigor in qualitative research. The first author maintained a reflexive journal to document reflections from interviews to assist with analysis, and member reflections including review of transcripts were conducted—resulting in one participant adding additional data around wellbeing and pregnancy. In relation to self-reflexivity (Braun & Clarke, 2021), the first author is an Australian-born South Asian woman with no personal experience of pregnancy. The first author’s ethnicity may have impacted discussions in interviews, as is the case for all interviewer-interviewee dynamics. For example, if caregivers felt the first author was an “insider” and therefore more trustworthy, they may have shared more details, whereas if they felt stigma around a topic, they could have shared less than they might have with an interviewer from a different background (Dwyer & Buckle, 2009). Among the other authors, all are nonmigrant and White-Australian, with and without children. Two are clinical psychologists with experience supporting children and caregivers, of which one has worked with S/SE Asian clients. The experiences and perceptions the authors brought to interviews and analysis were reflected on throughout the process of conducting this study.
Reflexive thematic analysis followed Braun and Clarke’s (2006, 2021) six phases. This approach to analysis was chosen as it enabled us to center lived experiences of participants in understanding their help-seeking and support experiences (Braun & Clarke, 2021). In Phase 1, the first author engaged in familiarization of the data through transcription and repeated reading of transcripts. In Phase 2, initial analysis was inductive and semantic with codes relating to wellbeing and barriers and facilitators to support, whereby coding was grounded in the data rather than informed by existing theories. A deductive coding approach was then taken, and codes were informed by conceptual frameworks related to health equity (Peterson et al., 2020) and health service utilization (Andersen, 1995). In this phase, codes were developed at the latent level for data related to help-seeking experiences and culturally responsive care. This coding led to theme generation in Phase 3, where provisional themes were reviewed by all authors. Final themes were then collaboratively reviewed, defined, and named by all authors in Phases 4 and 5, and we reflected on the key messages of each theme in representing the overall story of the data. The themes mapped onto two dimensions of the HEF, namely the systems of power dimension (Themes 1 and 3) and the relationships and networks dimension (Themes 2 and 4; Peterson et al., 2020). Where relevant, participant experiences consistent with predisposing, enabling, and need factors from Andersen’s (1995) model and the individual factors sphere from the HEF (Peterson et al., 2020) are described.
Results
Four themes were identified (Figure 2). The first two themes highlighted support experiences and help-seeking barriers: (a) “Talk about the barriers!”: Formal supports remain inaccessible and out of reach and (b) “At the last hour”: Interactions between perceived need and help-seeking. The final two themes relate to culturally responsive care and facilitators to support: (c) “We have more pilots than Qantas”: Organizational changes for staff education, information sharing, and continuity of care and (d) Community considerations: “Natural networks” and group-based support.
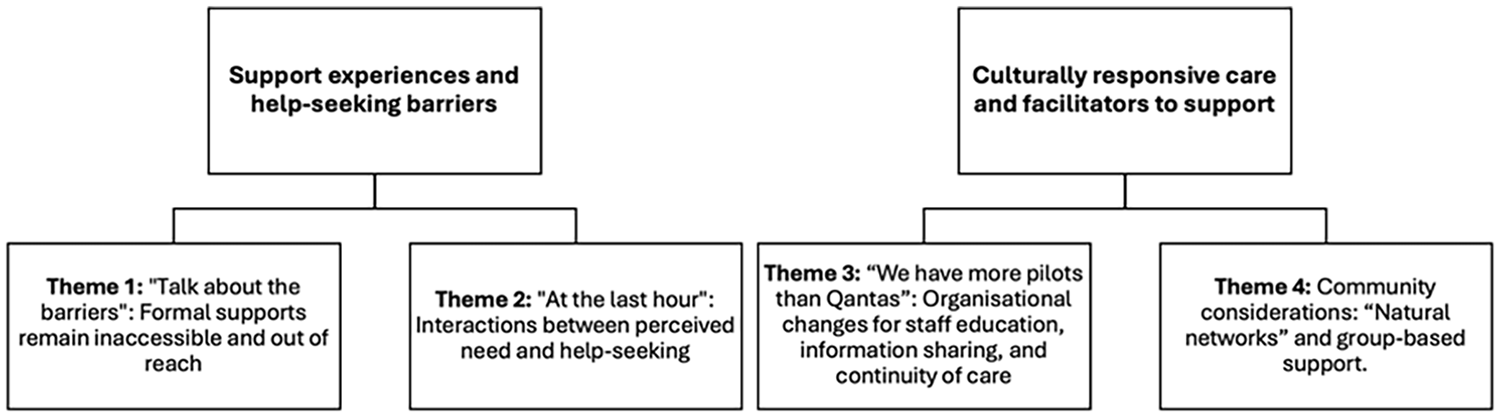
Thematic Map.
Theme 1: “Talk About the Barriers!”: Formal Supports Remain Inaccessible and Out of Reach
Participants discussed issues with formal supports across the First 2,000 Days, highlighting that such supports were often inaccessible and out of reach. Participants gave varied accounts for this, as described in this theme. At a foundational level, migrant caregiver participants explained that they were often simply not aware of available services to support the various domains of wellbeing across the First 2,000 Days. For example, Aysha described not being aware of supports for emotional/psychological domains of wellbeing: . . . that time [pregnancy and postnatally] I didn’t get any emotional support or mental health support because I didn’t know about that you can get some support from NDIS [National Disability Insurance Scheme] as a permanent resident. If I knew that I can have some mental health support for family, I could have got that support, however no one informed me. (Aysha, Bangaldeshi, mother)
Service providers also noted that help-seeking was challenging for caregivers when they were not aware of services. In some cases, this was explained to be due to cultural norms and to reflect cultural behavior such as a tendency toward “humbleness,” in relation to interactions with other people/services: . . . when you look at some people from the Southeast Asian communities, and because, how can I put it, the level of humbleness . . . they’re not going to front up to your service and say, “I should’ve had this, and you should’ve given me this.” That’s not how they work. (Malika, Psychotherapist and Social Worker)
In Andersen’s (1995) model, knowledge of services is a predisposing and enabling factor for health care utilization. Participants indicated that help-seeking experiences and service use were impacted by limited awareness and knowledge of available supports and suggested that this was in part due to a lack of proactive referral. Service provider participants also suggested that help-seeking may be similarly impacted by cultural characteristics (e.g., “humbleness”) in accepting support offered even if the service is poor. These experiences also reflect the individual factors sphere of the HEF (Peterson et al., 2020), in that developing skills and knowledge to scope out and access desired formal supports may prompt caregivers’ help-seeking.
Echoing Andersen’s (1995) model, cost was identified as a barrier to health care accessibility for migrant caregivers. For example, Susila (Indonesian, grandmother) noted cost-of-living as a concern within her community: “Talk about the barriers! [laughs]. . .The [health care] service was excellent . . . But the only thing is the cost . . . And also from the conversations that I have among the Indonesians, everything is all [r]evolve around cost-of-living.” In Andersen’s (1995) model, income and financial circumstances are enabling factors in accessing care. Susila’s experience indicates that service affordability is a key issue for migrant caregivers. Participants also discussed costs of health care processes for their children. Indonesian father Fadhlan who held a temporary migrant visa spoke about the cost of immunizations for his child as a key barrier to accessing health care for physical wellbeing, noting differences in Australia’s state-based immunization services: “. . . so like all the immunisation they are all free [interstate], but unfortunately in South Australia (SA) we have to pay for it because we are not citizen or residents here.” Fadhlan describes being impacted by state-level differences in access to some vaccines (while most are free across Australia, there are some state-level differences which could be linked to residency status; Department of Health and Aged Care, 2023). As such, Fadhlan’s service access was potentially impacted by systems of power policies in which predisposing factors (i.e., residency status) determined his access to health care.
Similar issues were noted by service providers; for example, Nurse and Midwife Alana noted differences in the level of culturally responsive supports between SA and eastern Australian states (which have larger migrant populations and more established services), noting that “it’s quite a stark contrast,” and that SA was particularly lacking in specialist supports related to maternal health. Indian mother Nikita also described how the eastern state she lived in had established supports: “I didn’t have any difficulties and there was a lot of information online about services and support that’s available.” Nikita’s experience outlines the importance of information dissemination as an enabling factor (Andersen, 1995) and culturally responsive resources in enabling migrant caregivers to seek support.
Service providers further described how some formal wellbeing supports were often not inclusive, leading to migrant caregivers experiencing possible discrimination and feeling “unheard.” One service provider discussed this in relation to public postnatal support groups which address a broad range of postnatal wellbeing supports: I know some [S/SE Asian] mums may not attend classes because of language barrier and also may feel as an outsider because they may be seen as being ignorant, so there may be that perception from them, but also maybe the discrimination of other mums because they’re different or they don’t speak the language, or they don’t understand. They may not feel included so they may not attend those classes, or they may miss appointments because they feel that they’re not heard. (Paula, Allied Health Professional)
Consistent with Andersen’s (1995) model, the level of perceived discrimination is a predisposing factor (in this case, barrier) to health care utilization. From an HEF systems of power perspective, perceptions of exclusion combined with limited consideration of factors such as cultural background or language may perpetuate health inequities experienced by migrant mothers.
Overall, this theme outlines how the political and institutional (health care, private organizations) systems that migrant caregivers interact with in the First 2,000 Days maintain health inequities by the exclusion of migrant caregivers from some aspects of the social, economic, or environmental supports provided for carers in the First 2,000 Days (Peterson et al., 2020). This theme also emphasizes individual factors of the HEF in building individual knowledge around service access (Peterson et al., 2020) and highlights predisposing and enabling factors of migrant caregivers in health care utilization and help-seeking (Andersen, 1995).
Theme 2: “At the Last Hour”: Interactions Between Perceived Need and Help-Seeking
A common theme through interviews with both groups of participants was that S/SE Asian caregivers were seen as hesitant to seek formal help for emotional/psychological wellbeing, leaving this until need was severe. Bhutanese community leader Thuy noted that waiting until crisis point for this domain of wellbeing was common among Nepali and Bhutanese caregivers (largely refugees): “. . . and I found some of the families, at the last stage only they come up with they want to seek support. So at the last hour, so it’s very difficult to bring them back [from their mental health struggles].” In terms of potential reasons for this help-seeking behavior, some participants noted that health services in countries of origin impacted some migrant caregivers’ perceptions of services and their help-seeking experiences in resettlement countries. For example, a Nepali Community Volunteer described how health- and help-seeking within her community were low potentially due to the scarcity of mental health support services in Nepal, resulting in caregivers seeking support only when their wellbeing was very poor: . . . another thing is because we come from Nepal and there are not that [many] services easy available like here, and we have that preconception that when the things get worse and only [then] they’re going to the services, the health-seeking behaviour is not that very good in us. (Sanjona, Nepali Community Volunteer)
Kiba, a Bhutanese refugee mother from Nepal and caregiver for three children—including two babies under 2 years of age—also noted that she would generally manage wellbeing issues at home, seeking support only when she felt she “had no choice.” She shared an issue with her husband’s health to illustrate this: Generally I would just deal with the difficulties at home myself. . .But with the little one, my husband has already started taking the medication for his mental health. . .and my husband wasn’t able to help me much, he was struggling, so I had to, I had no choice, I had to discuss all the difficulties that I was dealing with at home, and the midwife she started referring me and she started telling me what supports were available around that I could access. (Kiba, Bhutanese, Mother)
Samrina (Counselor) described a general hesitancy of her clients to seek help for mental health-related issues; so much so that she said the view within some S/SE Asian communities was that you would only seek help when “you actually have gone completely mad and you need help to get you back on track.” Providers also noted that clients were hesitant to disclose mental health issues due to concerns around confidentiality and the perception that their residency status would be affected, and they could be deported. Samrina described how information around mental health support and its impact on visa status could influence help-seeking: . . . so for instance if the government gets to know about their mental health condition or they’re seeking support it may impact or may come in the way of them getting their permanent residency or their citizenship or they may lose their visa when they’re on dependant visa, like on a spouse visa, because they’ve sort of like developed an understanding that if they go and access services, it can disadvantage them and the government has all the right to deport them, or their spouses have the right to deport them. (Samrina, Counselor)
Overall, this theme reflects the relationships and networks sphere of the HEF (Peterson et al., 2020), demonstrating that community understandings of mental health including stigma about seeking support, contributes to understandings about, and impacts migrant caregivers’ help-seeking. Consistent with the individual factors sphere of the HEF (Peterson et al., 2020) and Andersen’s (1995) model, predisposing factors such as health beliefs were seen to impact help-seeking experiences. Participants noted that support was primarily sought when conditions were deemed severe, consistent with the level of symptom discomfort as a need factor highlighted by Andersen (1995) in determining help-seeking and service utilization.
Theme 3: “We Have More Pilots Than Qantas”: Organizational Changes for Staff Education, Information Sharing, and Continuity of Care
This theme highlights organizational recommendations and culturally responsive care to address concerns around accessibility and help-seeking. For example, one service provider noted that staff education and training to understand parenting norms in particular cultures were a significant facilitator for culturally responsive care in formal support settings: . . . there is much more training required to bring some of these cultural norms or appropriateness to the workers who work with different cultures, because sometimes if you don’t have much experience working, you’ll have staff who say, “Oh I’ve never seen an Afghan family before” or “I’ve never worked with a Pakistani family before or a Cambodian family,” so if you haven’t and you don’t have a little bit of an understanding of what’s normal for this culture, sometimes you will misjudge their parenting. (Maria, Clinical Nurse in Maternal Health)
Staff education and training around cultural norms regarding pregnancy, parenting, wellbeing, and building trust with caregivers may address challenges to help-seeking identified in the first two themes connected to predisposing factors such as health beliefs, trust in services, and level of perceived discrimination.
Providers and migrant caregivers noted that sharing information through audio-visual and verbal channels of communication was also important: “. . . it’s about sharing information, communicating properly and also using video clips, infographics, visual aids. Two cultures. You got reading cultures, you got story telling cultures” (Venus, Consumer Representative/Advocate for Culturally and Linguistically Diverse Families). Pakistani mother, Mina also noted that verbal information regarding emotional/psychological domains of wellbeing would be useful for caregivers in her community postnatally, where caregivers may have extra caring responsibilities with limited time to read written resources: . . . doctors should verbally tell the mothers that it’s a very common thing [depression], it can happen to you, and what are the things you need [to] help. It’s not a mental disease, you can discuss with the doctor . . . they should be aware through verbal communication. Because, when you just pass on the papers and literature to people, they don’t bother reading it, they don’t have time. (Mina, Pakistani, Mother)
These recommendations may be useful in supporting individual factors related to health equity (Peterson et al., 2020) including knowledge generation around service access, as well as in addressing challenges related to predisposing factors such as negative (mental) health beliefs (Andersen, 1995). Providers also noted retention of clients, continuity of care, and funding for programs as key recommendations for sustained support. One service provider reported that this was difficult as most programs for migrant caregivers were pilot projects with limited funding, making it challenging to provide lasting care: It’s really difficult because the funding may be yearly, or two yearly or sometimes it’s less than that . . . a woman said to me, “We have more pilots than Qantas,” because there’s just so much pilot programs that last six months, a year, and then there’s nothing. (Malika, Psychotherapist and Social Worker)
In terms of public maternity care, Nurse and Midwife Alana described continuity of care to ensure that migrant caregivers receive culturally responsive and continued support—particularly important for migrant mothers interacting with the system for the first time, or for caregivers with experiences of trauma: I think there needs to be either a midwife or a group of midwives and obstetricians who are experienced working with [S/SE Asian migrant women] and experienced working around trauma, who can work together and closely with the communities these women are from, to ensure that they have that continuity of care, and that they’re getting that specialised care that they need. (Alana, Nurse and Midwife)
Overall, staff education in culturally responsive approaches to support migrant caregivers and culturally responsive information dissemination (e.g., through verbal discussions) were identified by participants as enabling factors (Andersen, 1995). This may promote individual factors in the HEF such as attitudes or knowledge around help-seeking and service access (Peterson et al., 2020). Funding to keep existing programs (evaluated to be effective) available for clients and continuity of care were cited as important to provide ongoing support.
Theme 4: Community Considerations: “Natural Networks” and Group-Based Support
Another area of culturally responsive care identified by participants was using informal supports such as community leaders to facilitate access to formal support for wellbeing concerns in the First 2,000 days (and beyond). One service provider suggested following a model used to share information around the COVID-19 pandemic with Aboriginal and Torres Strait Islander Elders: . . . actually using the existing community wisdom, I think we need to be doing that a lot more around parenting and education, is actually linking in with the natural networking, and making sure that individuals are connected with those natural networks in a more planned and cohesive manner, and that those networks are refreshed with information about parenting and the services available. (Lisa, Social Worker)
This recommendation emphasizes that relationships and networks are a conduit to promoting health outcomes and service access and use (Peterson et al., 2020). This approach may address (negative) predisposing factors such as stigma due to health beliefs and promote enabling factors such as knowledge of services, information dissemination, and trust and familiarity with services. Community Volunteer Sanjona also noted that Nepali community leaders were the “first point of contact” for caregivers seeking support and described her involvement in organizing Mental Health First Aid training for this group: . . . the community leaders should have the capacity, having the skills of Mental Health First Aid so we recently did training of around twenty community leaders on this topic, so that, you know, we have lots of families coming to ask for support, how to access services. (Sanjona, Nepali Community Volunteer)
Supporting community networks may promote information dissemination and promote migrant caregivers’ knowledge of formal services as enabling factors (Andersen, 1995). From an HEF perspective, community empowerment approaches may also support individual factors in terms of attitudes and behaviors toward help-seeking (Peterson et al., 2020). Group supports were also described by participants as a help-seeking facilitator, especially in relation to women’s groups: . . . women coming together as women is very much accepted. You know, coming into group situations is part of the norm . . . for example the groups run by [refugee service NGOs] for Afghan women, very, very useful for women who are potentially isolated and need some support in a whole range of different ways . . . coming to an environment like that where there are people running the groups who have good information about how to access services or where to go. (Claire, Multicultural Mental Health Nurse)
Pakistani mother Ash also spoke to the importance of a holistic women’s group she had found after moving to a new suburb, where they provided various wellbeing supports and workshops where mothers could connect with other women, conferring benefits including the sharing of parenting experiences: So in [suburb] there’s a women information system, they conduct different workshops. There were six, seven women coming and doing any artwork and talking to each other, and doing other activities, and sharing different parental experiences and all. So at least I was very lucky to have that group with me. (Ash, Pakistani, Mother)
Overall, this theme outlines the ways in which health equity is promoted via the support systems of migrant caregivers which work to reduce inequities created by systems of power (Peterson et al., 2020). Participants noted the significance of drawing from existing informal networks such as community leaders to provide information to migrant caregivers on accessing services.
Discussion
This study explored help-seeking for wellbeing, available support, and culturally responsive care across the First 2,000 Days for S/SE Asian migrant caregivers in Australia. Key findings suggest that services were commonly seen as inaccessible, sometimes due to a lack of outreach to S/SE Asian communities, resulting in limited awareness of available supports. In addition, the findings suggested that cultural norms, particularly related to being humble, also prevented help-seeking for aspects of wellbeing until need became severe. Together with an overall lack of trust with health systems, this cultural trait was seen as leading to low service uptake. Finally, the study highlighted ways to improve health services in the First 2,000 Days, particularly through continuity of care and “natural networks.” Overall, the study found that the HEF (Peterson et al., 2020) provided a holistic and comprehensive view of the factors that impact equity for S/SE Asian migrant caregivers, while the flexibility of Andersen’s (1995) model enabled an understanding of an individual’s predisposition to seek help and support. In this section, these aspects are considered more closely, with a help-seeking and health equity model proposed which considers all elements required for culturally responsive and equitable health care in the First 2,000 Days.
In this study, caregivers and service providers described services related to caregiver wellbeing as out of reach, reflecting previous literature with migrant women (Fair et al., 2020; Riggs et al., 2012). There are a range of contributing factors to this inaccessibility including insufficient culturally responsive supports and limited knowledge among migrant caregivers regarding how to access these services (e.g., Fair et al., 2020). In addition, financial pressures such as cost-of-living and restricted access to subsidized services due to Medicare ineligibility were reported as key issues impacting wellbeing and service access, primarily by caregivers. In previous research, migrant families have also cited financial pressure as a significant stressor to wellbeing and family relationships, particularly by migrant fathers in their role as primary earners (Forget et al., 2018; Okeke-Ihejirika & Salami, 2018).
Furthermore, participants described how help was sought for wellbeing only when need was severe, a finding which both groups of participants saw as typical for S/SE Asian peoples (e.g., a tendency toward “humbleness” or “gratitude”; see also Niner et al., 2013). This reflects previous work on depression, where Vietnamese American women noted that formal support was a “last resort” determined by severity (Ta Park et al., 2017, p. 437). While in this study and in previous research (Niner et al., 2013), this was described as a cultural tendency in some S/SE Asian communities, this may be a feature of collective cultures more generally. For example, a previous study described Middle Eastern women in Lebanon as having a sense of gratitude despite experiencing mistreatment and poor maternity care, which authors noted as “silent endurance” (Kabakian-Khasholian et al., 2022, p. 7). Similarly, in this study, participants described a general hesitancy for some S/SE Asian caregivers to seek help due to mental health concerns being perceived through notions such as “mad[ness]” as has been found for migrants from other communities including African backgrounds, whereby stigma largely influenced help-seeking for mental health (Fauk et al., 2022; Savic et al., 2015). As such, it is important that these concerns are addressed in research and practice for all communities regardless of cultural background.
Findings from this study also suggested that support may be sought by some S/SE Asian caregivers “at the last hour,” which may be due to experiences related to health care services in the pre-migration context. For example, some S/SE Asian countries are experiencing chronic shortages in relation to mental health services and practitioners (Maddock et al., 2021), potentially impacting lower help-seeking within these communities. This may also influence understandings around the availability or authenticity of Australian services, where S/SE Asian migrant caregivers may only seek support when need is deemed severe. In addition, caregiver reticence around help-seeking was noted, with fears their residency status would be affected if they disclosed mental health concerns. This is an understandable fear, as Australian policy states that migrants can be deported if it is known that they have health conditions that are considered a significant health cost to the Australian community (Department of Home Affairs, 2021), a position which creates overall mistrust of many services in migrant communities (Au et al., 2019).
In terms of facilitators of service use, consistent with previous research, this study identified that culturally responsive information dissemination such as audio-visual and verbal resources (Riggs et al., 2020), and continuity of care from services offered in the First 2,000 Days (Fair et al., 2020) were important in promoting culturally responsive care and service engagement for migrant caregivers. In relation to the systems of power sphere in the HEF, Peterson et al. (2020, p. 743) argue that while “big policy” concerns such as health care policy are considered contributors to population health, it is also important to establish health equity strategies at institutional levels, including policies that reduce the impacts of potentially exclusionary “big policies” on health inequities. The findings of this study reflect this argument, showing that organizational practices (e.g., commitment to culturally responsive information dissemination) may lessen the effects of exclusionary “big policies” on health inequities (Peterson et al., 2020).
Proposed Model for Help-Seeking and Health Equity
The findings of this study were viewed through Andersen’s (1995) model to identify factors which predisposed and enabled help-seeking and the HEF (Peterson et al., 2020) to acknowledge how systems of power, relationships and networks, and individual factors may promote or prevent health equity for migrant caregivers. These conceptual frameworks were considered more applicable to the present study than other existing models (e.g., Kleinman, 1980; Levesque et al., 2013) which do not center equity or account for help-seeking as an experience and behavior (situated within specific systems) in the way that Andersen’s (1995) model and the HEF (Peterson et al., 2020) do. In terms of Andersen’s (1995) model, this research found that predisposing, enabling, and need factors were present in the data. In particular, migration status (e.g., visa restrictions), knowledge of, and attitudes toward services, level of perceived racial discrimination within services, and individual and community health beliefs were evident for predisposing factors, while information dissemination (e.g., culturally responsive communication) and income/financial circumstances were evident for enabling factors. Finally, individual symptom discomfort and perceived risk related to health concerns were evident as need factors, and often drove engagement. However, Andersen’s (1995) model was not able to account for some aspects of the findings. For example, this research pointed to the central role of cultural attitudes to help-seeking and support as well as the critical importance of culturally responsive care, both of which are largely not considered in Andersen’s (1995) model which, as argued previously, pays little attention to the role of culture at any level (Augsberger et al., 2015). On the contrary, as a model which centers equity, the HEF (Peterson et al., 2020) does consider equity and systemic challenges related to culture with consideration of how systems of power (e.g., health care, government agencies), relationships and networks (e.g., family, community), and individual factors (e.g., individual attitudes) may intensify or mitigate health inequities.
In general, the two models together could account for many of the findings of this study. Specifically, the emphasis on factors salient in an individual’s predisposition to seek support and the flexibility of Andersen’s (1995) model complemented the HEF’s attention on broader facets (e.g., visa conditions; see Ziersch et al., 2021) and cultural elements that may explain inequities in health outcomes (Peterson et al., 2020). As neither model was a perfect “fit” for the findings of this study, we propose an adapted model combining the individual and help-seeking aspects of Andersen’s (1995) model with the health equity lens of the HEF (Peterson et al., 2020) for a comprehensive understanding of the interplay of individual factors and the broader structures that influence help-seeking and health equity (Figure 3).
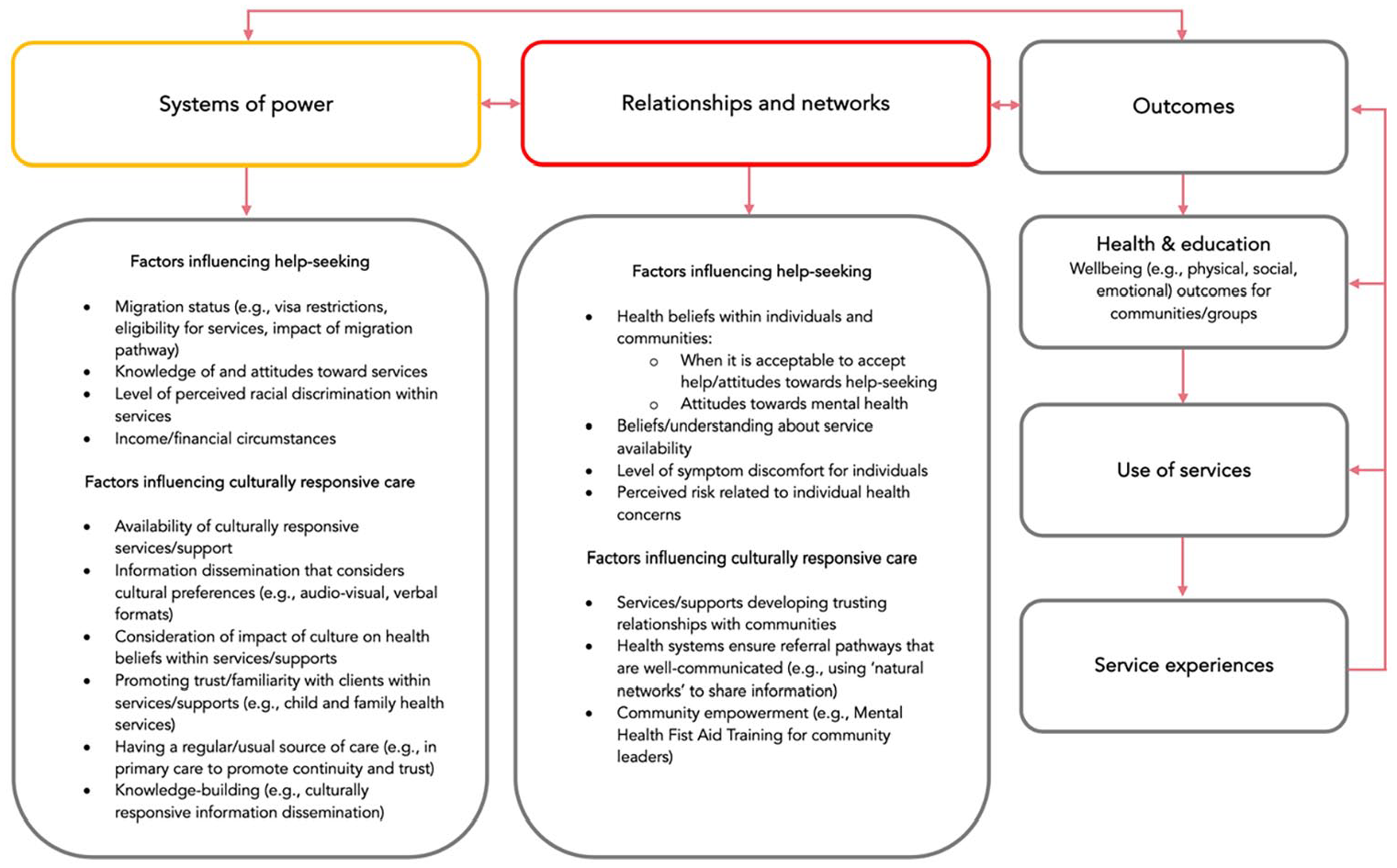
The Help-Seeking and Health Equity Model—a Proposed Model of Help-Seeking and Culturally Responsive Support for Equitable Health Service Delivery in the First 2,000 Days.
Recommendations and Implications for Research and Practice
The help-seeking and health equity model reflects the well-established predisposing, enabling, and need factors of Andersen’s (1995) model but adds feedback loops that link in domains from the HEF to ensure a health equity lens, as well as factors that more overtly relate to culture (Peterson et al., 2020). In combining these two models/frameworks, the proposed model allows for deeper understanding regarding the factors that predispose or enable help-seeking for both individuals and communities/groups. The proposed model also ensures that culture is prioritized as both a critical individual and contextual factor that influences help-seeking for individuals and highlights that health system engagement is dependent upon culturally responsive support for equitable outcomes. In terms of outcomes, the HEF centers on the health and education outcomes of communities and groups (Peterson et al., 2020) and Andersen’s (1995) model on individual’s service utilization. As in previous work exploring refugee health using Andersen’s model (Due et al., 2020), the outcome “service experiences” was added to this new combined model, as multiple spheres of influence in the current study were demonstrated to work together to predispose or explain service and help-seeking experiences. Service experiences may therefore be considered an independent outcome; however, it is also linked to other outcomes (such as service use) and may predispose future health beliefs and help-seeking (Due et al., 2020). The help-seeking and health equity model has implications for research, in that it provides a conceptual base for researchers investigating the intersection of health equity with help-seeking in marginalized groups. The model may be relevant to other contexts with similar populations, where there may be similar predisposing factors (e.g., visa restrictions), enabling factors (e.g., culturally responsive communication), or need factors (e.g., individual symptom discomfort).
This study identified a range of practice-based recommendations and implications which are largely encapsulated in the proposed help-seeking and health equity model (Figure 3). Participants suggested that providing information in ways that consider cultural preferences (e.g., audio-visual and verbal resources) may promote knowledge of services as well as improve communication and ultimately engagement with health services. Similarly, providers suggested funding existing programs—especially those that had been evaluated—to provide ongoing support. This is particularly important for service-level supports that can push back against any inequities in “big policies” (Peterson et al., 2020, p. 743). The proposed help-seeking and health equity model also highlighted a need for organizations to consider the impact of culture on health beliefs within supports/services, and this finding has implications for service provider training and development in supporting S/SE Asian families in the First 2,000 Days. As participants in this study noted the significance of informal supports such as “natural networks,” provision of education and guidance to service providers working in formal support settings may be achieved through partnering with community leaders and/or lived experience advocates with deep knowledge and insight into the norms and preferences of S/SE Asian families.
Participants noted the importance of group support while drawing from “natural networks” to promote health equity and address barriers perpetuated by systems of power. Therefore, the proposed model also highlights the importance of community empowerment approaches to support community understandings around mental health and help-seeking. Focusing efforts within communities where trust is established may therefore be useful; for example, where community members and leaders are equipped with resources (e.g., Mental Health First Aid Training, parenting resources) to offer a form of continuity of care such that caregivers have a regular source of support. In addition, community-based outreach approaches may be useful in destigmatizing help-seeking. This may involve services and providers (e.g., midwives, early childhood services) engaging with S/SE Asian migrant caregivers regarding their strengths and building connections to facilitate a safe space within communities for caregivers to share how they may be feeling in the First 2,000 Days. This is particularly important where help-seeking may be a challenge for individuals and families, due to particular beliefs regarding health and the availability or adequacy of services.
Limitations and Future Research
This study aimed to include the perspectives of broader caregivers considered central in co-caregiving within many S/SE Asian families; however, only two caregiver participants were recruited. Similarly, only one refugee participant was recruited. While the authors had existing connections with groups supporting S/SE Asian caregivers, recruiting refugee participants who may be living in complex environments is challenging, as is recruiting broader caregivers who are not women/mothers (Bilecen & Fokkema, 2022; Forget et al., 2018). Future research should consider targeted recruitment toward the broader caregiving system, given the dearth of evidence in this area. Interpreters were used for a small number of interviews in this study. Using interpreters can be challenging, especially in areas related to mental health, due to potential cultural differences in conceptualizations—and therefore words—relating to mental health (Gartley & Due, 2017). This also reflects the importance of reflexivity across all aspects of the research (Braun & Clarke, 2021). Nevertheless, research with caregivers who do not speak English (or the language of their resettlement country) is important. Finally, further examination of care for migrant families in the First 2,000 Days, which adopts a health equity lens, is needed, including studies that explore the acceptability of the model proposed in this study.
Conclusion
This study explored the help-seeking and formal and informal support experiences of migrant caregivers from S/SE Asia across the First 2,000 Days in Australia, with a focus on facilitators to culturally responsive care. Findings indicated a range of barriers to help-seeking and a perception of formal supports as unavailable and not culturally responsive. Overall findings were mapped to a proposed model of help-seeking (building on Andersen, 1995), centered in health equity. Recommendations from this research include organizational changes to address the inequities perpetuated by systems of power and to facilitate culturally responsive supports, community empowerment approaches to strengthen individual factors, as well as strengthening relationships and networks, and capitalizing on existing “natural networks” to support caregivers’ wellbeing in the First 2,000 Days.
Supplemental Material
sj-doc-1-jcc-10.1177_00220221251320051 – Supplemental material for South and Southeast Asian Migrant Caregivers’ Help-Seeking and Support Experiences Across the First 2,000 Days: A Qualitative Study and Emerging Model of Health Care
Supplemental material, sj-doc-1-jcc-10.1177_00220221251320051 for South and Southeast Asian Migrant Caregivers’ Help-Seeking and Support Experiences Across the First 2,000 Days: A Qualitative Study and Emerging Model of Health Care by Ria Aiyar, Clemence Due, Amanda Taylor and Alyssa Sawyer in Journal of Cross-Cultural Psychology
Footnotes
Acknowledgements
The authors are sincerely grateful to the caregivers and service providers who participated in this project and shared their stories. The authors are also thankful to the local community services and service providers that supported this project.
Author Contributions
RA: Conceptualization, Project Administration, Investigation, Methodology, Formal Analysis, Writing—Original Draft, and Writing—Review & Editing. CD: Conceptualization, Methodology, Formal Analysis, Writing—Review & Editing, and Supervision. AT: Formal Analysis, Writing—Review & Editing, and Supervision. AS: Formal Analysis, Writing—Review & Editing, and Supervision.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: RA is supported by an Australian Government Research Training Program Scholarship. The funding body did not play any role in the design of the study, data collection, data analysis, data interpretation, or in writing the manuscript. This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Ethical Considerations
This study was granted full ethical approval by the Women’s and Children’s Health Network Human Research Ethics Committee on October 13, 2021 (approval number: 2021/HRE00313).
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
