Abstract
Background:
Studies on mental health and substance use among medical students indicated worrying prevalence but have been mainly descriptive.
Aim:
To evaluate the prevalence of substance use in a sample of medical students and investigate whether mental health variables have an influence on substance use.
Methods:
The data were collected as part of the first wave of the ETMED-L, an ongoing longitudinal open cohort study surveying medical students at the University of Lausanne (Switzerland). N = 886 students were included and completed an online survey including measures of mental health (depression, suicidal ideation, anxiety, stress, and burnout) and use of and risk related with several substances (tobacco, alcohol, cannabis, cocaine, stimulants, sedatives, hallucinogens, opioids, nonmedical prescription drugs, and neuroenhancement drugs). We evaluated the prevalence of use of each substance and then tested the association between mental health and substance use in an Exploratory Structural Equation Modeling framework.
Results:
Statistical indices indicated a four-factor solution for mental health and a three-factor solution for substance use. A factor comprising risk level for alcohol, tobacco, and cannabis use – which were the most prevalent substances – was significantly associated with a burnout factor and a factor related to financial situation and side job stress. There was a significant association between a factor comprising depression, anxiety, and suicidal ideation and a factor related to the use of sedatives, nonmedical prescription drugs and neuroenhancement drugs. Although their use was less prevalent, a factor comprising the risk level of stimulants and cocaine use was significantly but more mildly related to the burnout factor. A factor comprising stress related to studies and work/life balance as well as emotional exhaustion was not related to substance use factors.
Conclusion:
In this sample of medical students, the prevalence of substance use was substantial and poorer mental health status was related with higher substance use risk levels.
Introduction
Mental and addictive disorders affected more than 1 billion people globally in 2016 and caused 7% of all global burden of disease as measured in DALYs and 19% of all years lived with disability (Rehm & Shield, 2019). Medical students have been shown to present poorer mental health compared to the general population and aged-matched peers (Dyrbye et al., 2006; Quek et al., 2019; Rotenstein et al., 2016) as well as a high prevalence of burnout (Erschens et al., 2019; Frajerman et al., 2019). In a recent meta-analysis (Rotenstein et al., 2016) a prevalence of 27.2% for depression and 11.1% for suicidal ideation was estimated among medical students. Furthermore, the prevalence of burnout and other forms of distress in medical students, residents/fellows and early career physicians was shown to be much higher compared with similarly aged college graduates pursuing other careers (Dyrbye et al., 2006). In a recent survey among doctors and medical students in the UK (Bhugra et al., 2019), medical students and junior doctors reported the highest rate of having a formally diagnosed mental health condition in the last 12 months. These findings highlight that the environment in which doctors work, train, and study affects their mental health, and consequently their ability to provide the best possible care for patients.
The use of legal and illegal substances by medical students has also been studied. In a review of the literature (Roncero et al., 2015), medical students were shown to use substances less than university students in general and the general population. However, the authors noted that there were many regional variations. Overall, the substances used were mainly alcohol (24%), tobacco (17.2%), and cannabis (11.8%). The use of hypnotic and sedative drugs also was common (9.9%). The use of stimulants was 7.7% and the use of cocaine was 2.1%; while opiate use was very low (0.4%). The use of substances, except for hypnotics and sedatives, was more common among male than female students. The authors also noted high heterogeneity in methods and research quality.
Recently, a consortium of researchers from 19 countries across the five continents evaluated wellbeing, burnout and substance use among medical students (Kadhum et al., 2022; Molodynski et al., 2021). Their findings indicated a pervasive pattern of high levels of psychiatric symptoms, disengagement, and exhaustion in medical students across these countries. Rates of substance use and identified sources of stress varied largely across cultures. Overall, about 10% reported potential alcohol problems and 14% reported cannabis use. The main source of stress reported by medical students was their academic studies, followed by relationships, financial difficulties, and housing issues.
Most of the studies to date have been descriptive in nature and mainly presented prevalence of mental health and substance use among medical student samples. Fewer studies investigated associations between these dimensions. Some studies descriptively showed that students used substances to deal with mental health symptoms or to feel better. For example, one in three participants were using alcohol, drugs, self-medication, or self-prescribing as a way to cope with their mental health condition in the study among UK doctors and medical students (Bhugra et al., 2019). Among medical students in Paraguay, 9.4% reported using substances to feel better (Torales et al., 2019). In a similar study in Canada, 20% of students reported having taken a non-prescription substance to feel better or regulate their mood (Wilkes et al., 2022). One recent study investigated substance use and mental health problems among Spanish medical students and showed that total scores of self-reported mental health problems negatively correlated with objective academic results and positively correlated with the number of substances consumed in the last 30 days (Atienza-Carbonell et al., 2022). Another recent study focused on non-medical use of neuroenhancement drugs among German medical students (Jebrini et al., 2021). The authors showed that neuroenhancement drugs use was significantly associated with the use of other substances, any psychiatric disorder, feeling pressure to perform in professional/students’ life and in private life, as well as the feeling of pressure to perform to be burdening and harmful to one’s own health.
The present study uses data from the ETMED-L project (Berney et al., 2021), an ongoing longitudinal open cohort study surveying medical students at the University of Lausanne’s Medical School (Switzerland) on a yearly basis. In a first article, we reported that N = 886 medical students were included, representing 49.41% of the overall eligible students, and that about 40% of these students were at risk of clinically significant depressive symptoms (Carrard et al., 2022). In the present analysis, we evaluated the prevalence of substance use among medical students, and then investigated whether mental health and burnout variables had an influence on substance use. We hypothesized that poorer mental health status would be related with higher substance use risk levels.
Materials and methods
Participants and procedures
The data were collected as part of the first wave of the ETMED-L, an ongoing longitudinal open cohort study surveying medical students at the University of Lausanne (Switzerland) on a yearly basis. Study procedures have been described in detail elsewhere (Berney et al., 2021). Briefly, all medical students at the University of Lausanne in curriculum years 1 to 6, except external students who are in the university as part of an academic exchange, were eligible for participation during the spring semester of 2021 (N = 1,793). They were informed about the study via an email sent by the Medical School, and then received a link to the online questionnaire. The survey was open between March 5 and April 5, 2021. Questionnaire completion took approximatively 60 minutes. The students received two participation reminders via email and a compensation of 50 CHF (≈50 USD) for their participation. All included students provided informed consent to participate in the online questionnaire. The online questionnaire used a forced answer strategy. Thus, there were no missing data for the participants included in this study. The ETMED-L project protocol was approved by the Human Research Ethics Committee of the Canton de Vaud (protocol number 2020-02474).
Measures
Depressive symptoms were assessed with the French version of the Center for Epidemiological Studies-Depression (CES-D; Radloff, 1977), a 20-item measure of symptoms associated with depression experienced over the past week. We used the French version of the CES-D, which showed good internal consistency as well as adequate structural and construct validity (Morin et al., 2011).
Suicidal ideation was evaluated using two questions of the Beck Depression Inventory (Beck et al., 1961). The BDI is well validated and has been shown to accurately distinguish individuals at risk of suicidal attempts from other individuals (Troister et al., 2015).
General level of anxiety was assessed with the trait subscale of the State-Trait Anxiety Inventory (STAI; Spielberger, 1983). Considerable evidence attests to the construct and concurrent validity of this 20-item scale (Spielberger, 1983).
Stress was measured with six items assessing the level of stress among six domains on a visual-analog scale from 1 ‘none’ to 10 ‘extreme’. The six domains were as follows: (1) family life, (2) financial situation, (3) side job, (4) romantic life, (5) studies, and (6) work/life balance. This questionnaire was used in a previous cross-sectional study of mental health among medical students at University of Lausanne (Unpublished Master Thesis, 2018) and was integrated to the questionnaire for comparability purpose.
Burnout was measured with the French version of the Maslach Burnout Inventory Student-Survey (Faye-Dumanget et al., 2017), an instrument widely used to measure students’ burnout in research. This 15-item scale evaluates three dimensions: Emotional Exhaustion (5 items), Cynicism (4 items), and Academic Efficacy (6 items, reversed dimension).
Substance use was measured using the French version of the WHO’s Alcohol, Smoking and Substance Involvement Screening Test (ASSIST, Humeniuk et al., 2010). The ASSIST is an 8-item questionnaire designed to be useable across a variety of cultures to screen for use of the following substances: tobacco products, alcohol, cannabis, cocaine, amphetamine-type stimulants, sedatives, and sleeping pills (e.g. benzodiazepines), hallucinogens, inhalants, opioids, and ‘other’ drugs. This latter category was selected by 26 participants, mostly to describe neuroenhancement drugs or non-medical use of prescription drugs that were measured separately (see below). We thus excluded this category for further analyses. We also excluded inhalants which were selected by only one participant. A score of prevalence of each substance use was assessed by combining the ASSIST’s Question 1 (lifetime use) and 2 (3-month use). Scores from Questions 2 to 7 were additionally summed to create the so-called ASSIST score for each substance, which provides an indication of the level of risk associated with the respondent’s substance use, and whether use is hazardous and likely to be causing harm. Scores in the mid-range on the ASSIST are likely to indicate hazardous or harmful substance use (‘moderate risk’) and higher scores are likely to indicate substance dependence (‘high risk’).
In addition, we evaluated the use of neuroenhancement drugs, as well as non-medical use of prescription drugs, using items from the Cohort Study on Substance Use Risk Factors questionnaire (Baggio et al., 2014; Deline et al., 2014). The questionnaire described neuroenhancement drugs as medication usually prescribed for specific diseases, but used for other reasons, such as to increase concentration, mental ‘energy’, memory, learning ability, attention span, to reduce stress during exams, or to feel more productive. Participants were asked how often during the last 12 months they had used the following seven types of neuroenhancement drugs: (1) wakefulness medicaments for such sleeping disorders as narcolepsy, for example, modafinil (Provigil®) and armodafinil (Nuvigil®); (2) drugs for ADHD, for example, methylphenidate (Ritalin®), Adderall®; (3) antidepressants, for example, venlafaxine (Effexor®) and fluoxetine (Prozac®); (4) antidiuretic for example, desmopressin, vasopressin (Nocutil®); (5) Alzheimer’s disease drugs, for example, donepezil (Aricept®); (6) Parkinson’s disease drugs, for example, selegiline (Jumexal®); and (7) beta-blockers for cardiac troubles, for example, atenolol (Tenormin®). Non-medical use of prescription drugs was described as the use of prescription drugs without a doctor’s prescription or for reasons other than those indicated. Participants were asked how often during the last 12 months they had used the following six types of prescription drugs: (1) sleeping pills, for example, benzodiazepine (Dalmadorm®, Rohypnol®), barbiturate, chloralhydrate (Nervifène®), zopiclon, zolpidem (Stilnox®); (2) tranquilizers and anxiolytics, for example, benzodiazepine (Valium®, Xanax®, and Temesta®) and muscle relaxing drugs); (3) strong painkillers, for example, buprenorphine (Tamgesic®), codeine (Benylin®), opioids (Fentanyl®, Oxycontin®, and Vicodin®), and DXM (Bexin®), but over-the-counter painkillers such as Aspirin® and Paracetamol® were excluded; (4) stimulants, for example amphetaminsulphate (Aderall®), atomoxetine (Strattera®), methylphenidate (Ritalin®); (5) antidepressants (e.g. Remeron®, Fluoxetine®); and (6) beta-blocker, for example, propranolol (Inderal®). For both neuroenhancement drugs and non-medical use of prescription drugs, answers were collected on an 8-point scale (0 = never, 1 = once, 2 = 2–3 times a year, 3 = 4–9 times a year, 4 = 1–2 times a month, 5 = 3–4 times a month, 6 = 2–3 times a week, and 7 = 4 times a week or more). Prevalence of use over the past 12 months was obtained by dichotomizing ‘never’ versus at least one type once for neuroenhancement drugs and non-medical use of prescription drugs separately, as in Baggio et al. (2014) and Deline et al. (2014). Additionally, a continuous risk score was computed by summing the points obtained on the 0 to 7 scale for each type of (a) neuroenhancement drugs and (b) non-medical use of prescription drugs.
Statistical analysis
We first evaluated the prevalence of use of each substance by computing frequencies. Then, we tested the association between mental health measures and substance use in an Exploratory Structural Equation Modeling (ESEM) framework. This approach was selected as there were important correlation patterns between variables of interest and as we did not have a priori hypotheses of the factor structure. In a first step, we conducted an Exploratory Factor Analysis (EFA) separately for (a) mental health measures and (b) substance use measures, in order to determine the number of factors to extract. Both EFA models were computed in Mplus version 8.3 (Muthén & Muthén, 1998/2017), using maximum likelihood estimation with robust standard errors and oblique geomin rotation. For both models, solutions with one to six factors were compared. To determine the number of extracted factors, we considered Kaiser’s criterion with eigenvalues greater than 1, Chi-square comparison of k-factor against [k − 1]-factor models, as well as three fit indices to assess how well the models fit the data (van Zyl & ten Klooster, 2022): the Root Mean Square Error of Approximation (RMSEA, with values <0.08 indicating marginally acceptable fit and <0.06 indicating excellent fit), the Comparative Fit Index (CFI, with values >0.90 indicating marginally acceptable fit and >0.95 indicating excellent fit), and the Standardized Root Mean Squared Residual (SRMR, with values <0.08 indicating marginally acceptable fit and <0.06 indicating excellent fit). In a second step, we computed an ESEM model while specifying the number of factors indicated in the first step analyses and testing the effect of mental health factors on substance use factors. Finally, we repeated this model while adjusting for age and self-identified gender.
Results
Substance use prevalence
As illustrated in Figure 1, alcohol was the most widely used substance in the sample. More than 86% had already used it and about 40% used it at least weekly. Tobacco was the second most used substance, with about one third of the sample having already used it, and 13% using it at least weekly. This was the substance the most frequently used on an everyday or almost everyday day basis (7%). Cannabis was the most widely used illicit substance with about one quarter having already used it and about 10% using it monthly or more. Other substances were much more scarcely used. Only 1% to 2% had previously used substances such as cocaine, stimulants, hallucinogens, or opioids. About 0.3% used stimulants and opioids monthly or more. The use of sedatives was somewhat higher (7% ever used and 3% using monthly or more). About 16% had had a nonmedical use of prescription drugs during the last year and about 4% had used neuroenhancement drugs over the same period.
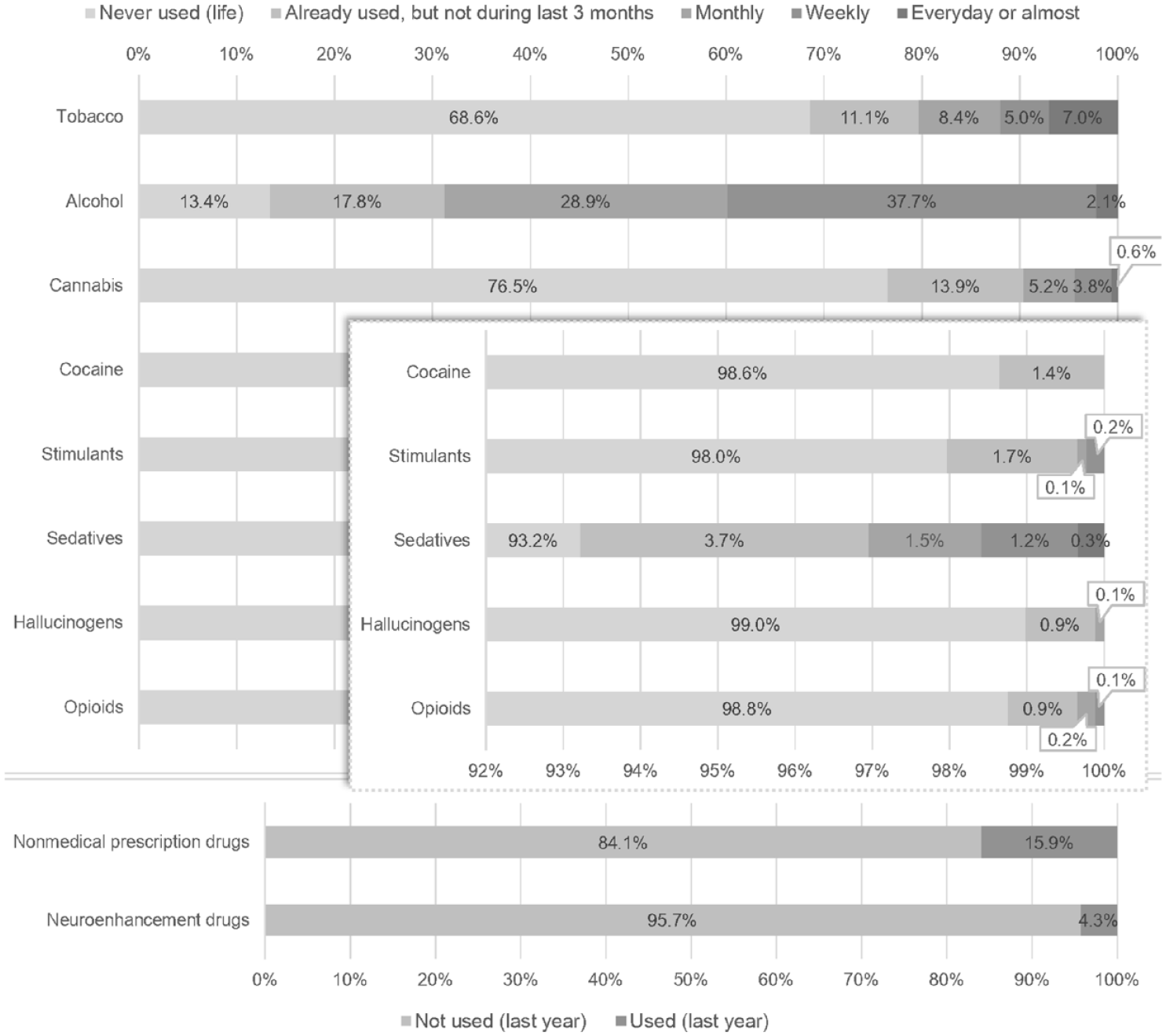
Prevalence of substance use within the collected sample.
Mental health and substance use factors
Descriptive statistics and correlations between variables of interest are presented in Table 1. Eigenvalues, Chi square test of k against k − 1 solution, and fit indices consistently indicated a three-factor solution for substance use measures in EFA (see Supplemental Table 1). Solution for mental health measures was less consistent. Eigenvalues indicated a three-factor solution, but Chi square test of k against k − 1 solution and RMSEA and CFI indices indicated that a four-factor solution was better. We selected this solution as the most balanced and clinically relevant.
Descriptive statistics and correlations between variables of interest.
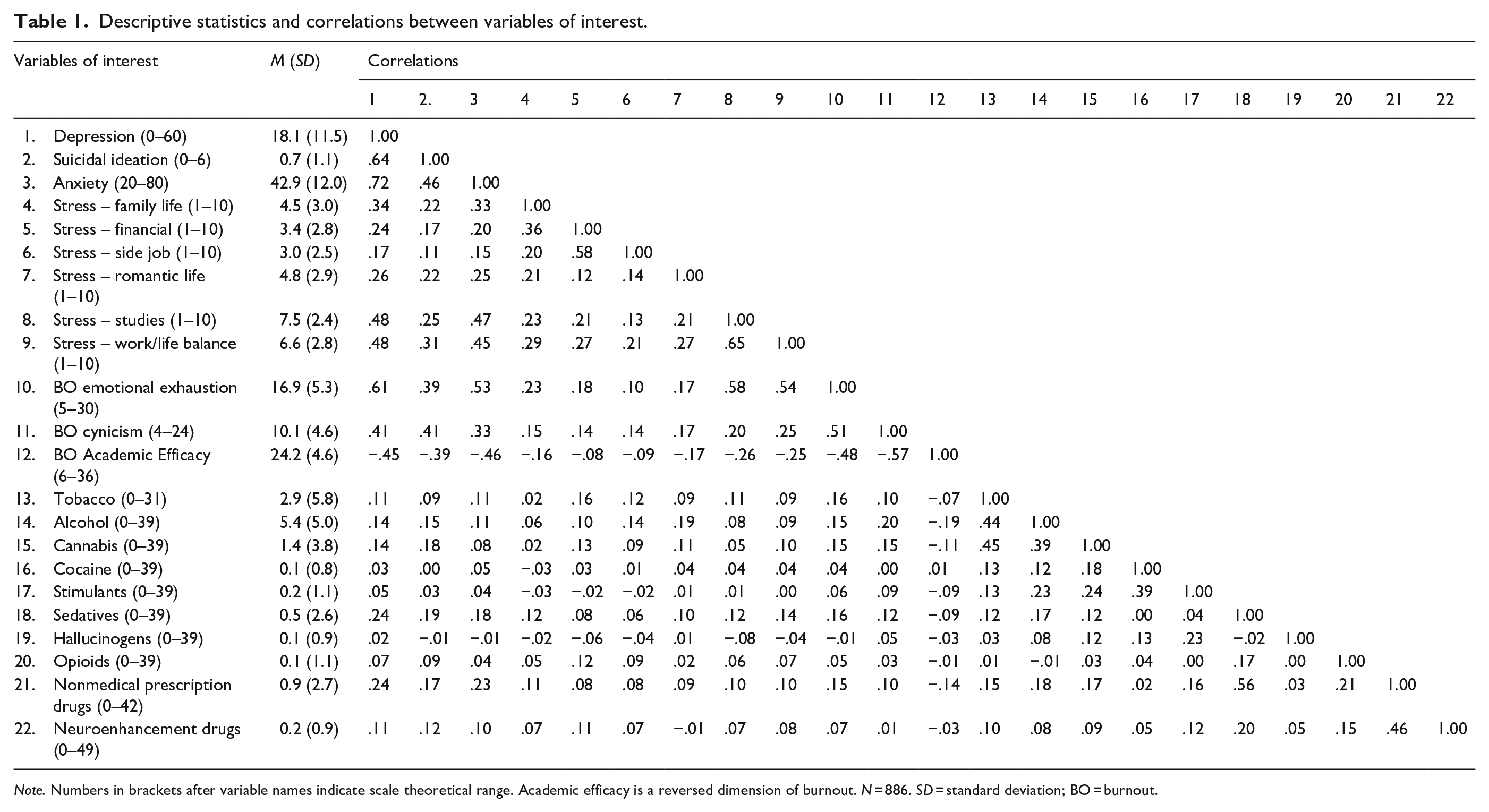
Note. Numbers in brackets after variable names indicate scale theoretical range. Academic efficacy is a reversed dimension of burnout. N = 886. SD = standard deviation; BO = burnout.
The first mental health factor (M1, see Figure 2 and Supplemental Table 2) was mainly explained by higher depression, suicidal ideation, and anxiety scores. It was also linked to stress related to family life and romantic life, as well as emotional exhaustion, but to a lower extent. The second mental health factor (M2) was mainly explained by stress related to financial situation and side job; it was also explained to a lower extent by stress related to family life and work/life balance. The third factor (M3) was mainly explained by stress related to studies and work/life balance, as well as the emotional exhaustion dimension of burnout. It was also related to a lower extent to higher anxiety and higher romantic life stress, and to lower scores of suicidal ideation. Finally, the fourth mental health factor (M4) mainly comprised the burnout items (higher emotional exhaustion, higher cynicism, and lower academic efficacy) and, to a lower extent, higher scores of suicidal ideation. Regarding substance use, a first factor (S1) mainly included alcohol, tobacco, and cannabis risk level. A second factor (S2) was mainly explained by stimulants and cocaine use risk level. Finally, a third factor (S3) was mainly explained by sedatives use risk level, and prevalence of nonmedical prescription drugs and neuroenhancement drugs use.
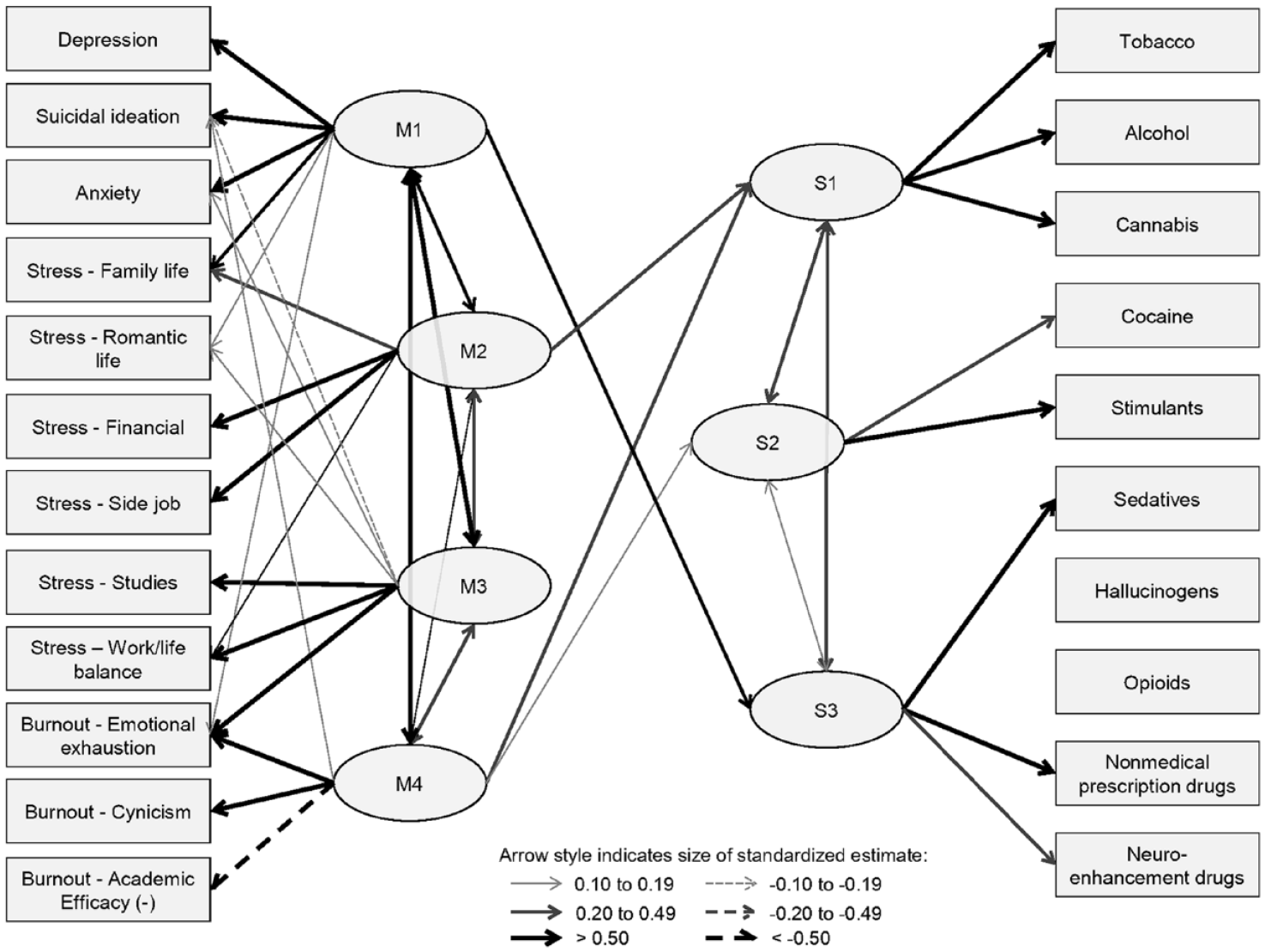
Exploratory structural equation model.
Effect of mental health on substance use
The fit indices of the ESEM model indicated excellent fit (RMSEA = 0.022, CFI = 0.983, and SRMR = 0.024). There were several significant effects when evaluating the effects of mental health factors on substance use factors (see Figure 2 and Supplemental Table 2). Higher scores on the factor related to alcohol, tobacco, and cannabis use (S1) was significantly related with higher scores on the factors related to financial and side job stress (M2) and burnout (M4). Higher scores on the factor related to stimulants and cocaine use (S2) was also significantly related with higher scores on the burnout factor (M4). Finally, higher scores on the factor related to sedatives, nonmedical prescription drugs, and neuroenhancement drugs use (S3) was significantly related with higher scores on the factor related to depression and anxiety (M1). The factor comprising stress related to studies and work/life balance (M3) was not associated with any substance factor.
Sensitivity analysis controlling for age and gender confirmed these findings, with similar pattens of significance and size of effects (see Supplemental Table 2, right-end columns). The effects of age and gender were mostly non-significant, except for a significant effect of gender on the alcohol, tobacco, and cannabis risk level factor (being male related with higher substance use).
Discussion
As hypothesized, the prevalence of substance use among medical students included in this study was substantial and poorer mental health status was related with higher substance use risk levels. In particular, the factor comprising risk level for alcohol, tobacco, and cannabis use – which were the most prevalent substances – was significantly associated with the burnout factor and the financial situation and side job stress factor. There was also a significant association between the factor comprising depression, anxiety, and suicidal ideation and the factor related to the risk level of sedatives use, and the use of nonmedical prescription drugs and neuroenhancement drugs. Although their use was less prevalent, the factor comprising the risk level of stimulants and cocaine use was also significantly but more mildly related to the burnout factor. Importantly, the factor comprising stress related to studies and work/life balance, as well as emotional exhaustion was not related to substance use factors.
Altogether, these findings add support to the literature showing that mental health problems often co-occur with substance use (Alsuhaibani et al., 2021; Carrà et al., 2015; Murthy et al., 2019). This co-occurrence has been already observed among young adults, even if data among this population are inconsistent regarding the direction of this effect (Köck et al., 2022). On the one hand, mental disorders promote the development of substance use disorders, and on the other hand, substance use disorders negatively influence mental health problems (Köck et al., 2022). Recent studies have suggested that substances were used to cope with mental health symptoms, regulate mood, or to feel better among medical students (Torales et al., 2019; Wilkes et al., 2022), as well as among junior doctors (Bhugra et al., 2019). Similar to our findings, other studies observed associations between poorer mental health and higher substance use among medical students (Atienza-Carbonell et al., 2022; Jebrini et al., 2021). Nonetheless, the cross-sectional nature of these data does not allow us to evaluate the directionality of the observed effects and future longitudinal studies are required in this respect.
Regarding substance use prevalence, it seems that substance use within our sample was somewhat lower than in the Swiss population of similar age (20–24 years old; Swiss Health Observatory, 2023). This is particularly the case for tobacco (7% smoking every day or almost every day vs. 26%), but an exception was cannabis (10% with monthly use in both populations). This effect might be expected since substance use is generally lower among people with tertiary level education in Switzerland (Swiss Health Observatory, 2023). Comparison with other samples of medical students is more complicated since measures and timeframe often vary between studies. Previous studies have shown that substance use among medical students importantly varied across cultures (Molodynski et al., 2021). As a tendency, it seems that cannabis use was in the upper level in our sample in comparison with other countries, while on the other hand cocaine was in the lower level (Farrell et al., 2019; Molodynski et al., 2021; Wilkes et al., 2022).
The use of illicit drugs except cannabis was relatively low, but the prevalence of use of sedatives was higher (7% ever used and 3% using monthly or more) and about 16% reported having had a nonmedical use of prescription drugs during the last year. This prevalence seems rather high in comparison with data among young adults in the USA (7.4% among young adults aged 18–25 years in the general population; SAMHSA, 2022) and in Switzerland (6.8% of young men in the general population had non-medical use of painkillers, 3.0% of sleeping pills, 2.6% of anxiolytics, 1.9% of stimulants, and 0.9% of antidepressants; Baggio et al., 2014). On the other hand, the use of neuroenhancement drugs was about 4%, which is in line with other studies in Switzerland (3.8% among 15 to 34 years old in the Swiss general population; 3% among young men in the general Swiss population; Deline et al., 2014; Swiss Health Observatory, 2023). It seems however relatively lower than in other studies among medical students. In a systematic review on stimulant usage by medical students for cognitive enhancement, prevalence was shown to range from 5.2% to as high as 47.4% among medical students across different countries (Plumber et al., 2021).
Similar to effects observed in the present study, the use of neuroenhancement drugs and nonmedical use of prescription drugs have been related to mental health and burnout issues among medical students and young adults. The use of neuroenhancement drugs was significantly associated with having a psychiatric disorder and having higher values of feeling pressure to perform in student and private life among medical students (Jebrini et al., 2021). Nonmedical use of prescription drugs was associated with poorer mental health among young men from the general population (Baggio et al., 2014) and with numerous negative outcomes, including suicidal ideation and attempts among Chinese college students (Juan et al., 2015).
Strengths and limitations
High participation rate and the absence of missing values are important strengths of this study. The use of validated instruments is another strength, except for the measures of stress which were developed and used in a previous cross-sectional study of mental health among medical students at the University of Lausanne (Unpublished Master Thesis, 2018) and was integrated to the present questionnaire for comparability purpose.
One limitation relies in the use of a convenience sample, which might lack generalizability. The cross-sectional design of the study is another important limitation, preventing all interpretation of our findings as showing causality. Future data collection of the ETMED-L project will enable to better understand the potential progression and directionality of effects between medical students’ mental health and substance use. In addition, data were collected in a single site in Switzerland, which might limit transferability to other settings. Finally, the use of Exploratory Structural Equation Modeling comes with statistical limitations. In the present study, an important one was the lack of consistency between indices to choose the most appropriate factor solution. Nevertheless, the consistency and interpretability of the retained solutions foster confidence in their clinical relevance and the final ESEM model showed excellent fit indices.
Conclusion
Altogether, the prevalence of substance use and its relation with poorer mental health and burnout among medical students is worrying and should call for a clinical response. Failing to do so might affect the health and mental wellbeing of medical students themselves, but also indirectly their ability to provide the best possible care for patients at the end of their studies (Bhugra et al., 2019). In the latter study, junior doctors did not get the help they needed even when they asked for it and one in three participants were using substances to deal with their symptoms. Therefore, services must be easily accessible and approachable for students (Molodynski et al., 2021). Promising models promoting well-being and preventing burnout have been and are being developed and should be further considered (Dunn et al., 2008; Edmonds et al., 2023).
Supplemental Material
sj-docx-1-isp-10.1177_00207640241232321 – Supplemental material for Substance use and its association with mental health among Swiss medical students: A cross-sectional study
Supplemental material, sj-docx-1-isp-10.1177_00207640241232321 for Substance use and its association with mental health among Swiss medical students: A cross-sectional study by Jacques Gaume, Valérie Carrard, Sylvie Berney, Céline Bourquin and Alexandre Berney in International Journal of Social Psychiatry
Footnotes
Acknowledgements
We gratefully thank Cristiana Fortini for the careful editing of the manuscript.
Conflict of interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Swiss National Science Foundation [grant number 10001C_197442].
Data availability statement
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
