Abstract
Introduction:
Mental health concerns and treatment usually take a backseat when the limited resources are geared for pandemic containment. In this global humanitarian crisis of the COVID-19 pandemic, mental health issues have been reported from all over the world.
Objectives:
In this study, we attempt to review the prevailing mental health issues during the COVID-19 pandemic through global experiences, and reactive strategies established in mental health care with special reference to the Indian context. By performing a rapid synthesis of available evidence, we aim to propose a conceptual and recommendation framework for mental health issues during the COVID-19 pandemic.
Methods:
A search of the PubMed electronic database and google scholar were undertaken using the search terms ‘novel coronavirus’, ‘COVID-19’, ‘nCoV’, SARS-CoV-2, ‘mental health’, ‘psychiatry’, ‘psychology’, ‘anxiety’, ‘depression’ and ‘stress’ in various permutations and combinations. Published journals, magazines and newspaper articles, official webpages and independent websites of various institutions and non-government organizations, verified social media portals were compiled.
Results:
The major mental health issues reported were stress, anxiety, depression, insomnia, denial, anger and fear. Children and older people, frontline workers, people with existing mental health illnesses were among the vulnerable in this context. COVID-19 related suicides have also been increasingly common. Globally, measures have been taken to address mental health issues through the use of guidelines and intervention strategies. The role of social media has also been immense in this context. State-specific intervention strategies, telepsychiatry consultations, toll free number specific for psychological and behavioral issues have been issued by the Government of India.
Conclusion:
Keeping a positive approach, developing vulnerable-group-specific need-based interventions with proper risk communication strategies and keeping at par with the evolving epidemiology of COVID-19 would be instrumental in guiding the planning and prioritization of mental health care resources to serve the most vulnerable.
Background
The World Health Organisation (WHO) declared COVID-19 as a Public Health Emergency of International Concern (PHEIC) on 30 January 2020 (
Mental health concerns and treatment usually take a backseat when the limited resources are geared for pandemic containment. History suggests that any infectious disease outbreak or pandemic brings with itself a major setback in the mental health front. In the case of the Ebola outbreak in the year 2014, symptoms of Post-Traumatic Stress Disorder (PTSD) and anxiety-depression were more prevalent even after 1 year of Ebola response (Jalloh et al., 2018). The global HIV pandemic also provides a similar picture. It has been found that the prevalence of mental illnesses in HIV-infected individuals is substantially higher than in the general population. (World Health Organization, 2008) The risk of PTSD in the aftermath of the pandemic can, therefore, be a huge challenge to the mental health system of the country. Since the healthcare system focuses majorly on emergency services, individuals suffering from substance abuse and dependency disorders may see deterioration in their mental health as a result of this pandemic. (Clay & Parker, 2020) The economic fallout and forecasted recession pertaining to ‘The Great Lockdown’ is feared to be the worst global economic crisis after ‘The Great Depression’ (The Great Lockdown: Worst Economic Downturn Since the Great Depression – IMF Blog, 2020). With many sectors seeing pay-outs and job losses across Europe and America, unemployment can rise to a record 14% in the USA which can worsen to 20% post-pandemic in the future. This can lead to increase in suicide rates among the economically vulnerable (
Methods
The current article reviews the existing literature on mental health issues and interventions relevant to the COVID-19 pandemic. A search of the PubMed electronic database and google scholar was undertaken using the search terms ‘novel coronavirus’, ‘COVID-19’, ‘nCoV’, SARS-CoV-2, ‘mental health’, ‘psychiatry’, ‘psychology’, ‘anxiety’, ‘depression’ and ‘stress’ in various permutations and combinations. A thorough search of all published journal articles, newspaper articles, magazine articles, webpages including World health Organisation, Ministry of Health and Family Welfare- Government of India (MOHFW), State governments and independent websites of various institutions) and non-government organizations, and verified social media portals including -Twitter, Youtube, Facebook, Whatsapp, etc., have been compiled after exclusion of fake and unverified updates. The authenticity of the social media updates has been ensured by thorough search and inclusion of only verified institutional/organisational social media pages and central and state government social media portals. Different combinations of keywords including geographical locations, the vulnerable population were also used for the search strategy. Review was limited to search output up to 31st May 2020.
After review, we synthesized the evidence into two broad headings that is, mental health issues during COVID-19 pandemic particularly in the context of some vulnerable groups and possible reasons thereof, interventions recommended so far at a global level and India. Based on the evidence synthesis, we have proposed a conceptual framework for mental health risk during COVID-19 pandemic and a recommendation framework with reference to Low- and Middle-Income Countries (LMIC) like India
Results
Mental health issues during COVID-19 pandemic
The major mental health issues that have been reported to have been associated with the COVID-19 pandemic are
Strict lockdown laws, social distancing, restrictions in movement could result in increased screen time. Constant misinformation in social media portals may result in a state of panic and anxiety, often resulting in depression eventually. Findings of a study done in Shanghai, China show a high prevalence of mental health problems, which positively associated with frequent social media exposure during the COVID-19 outbreak (Gao et al., 2020).
Summary of studies reporting mental health effects of COVID 19 pandemic and previous pandemics are summarized in Table 1.
Studies on mental health implications of different outbreaks, epidemics and pandemics globally.
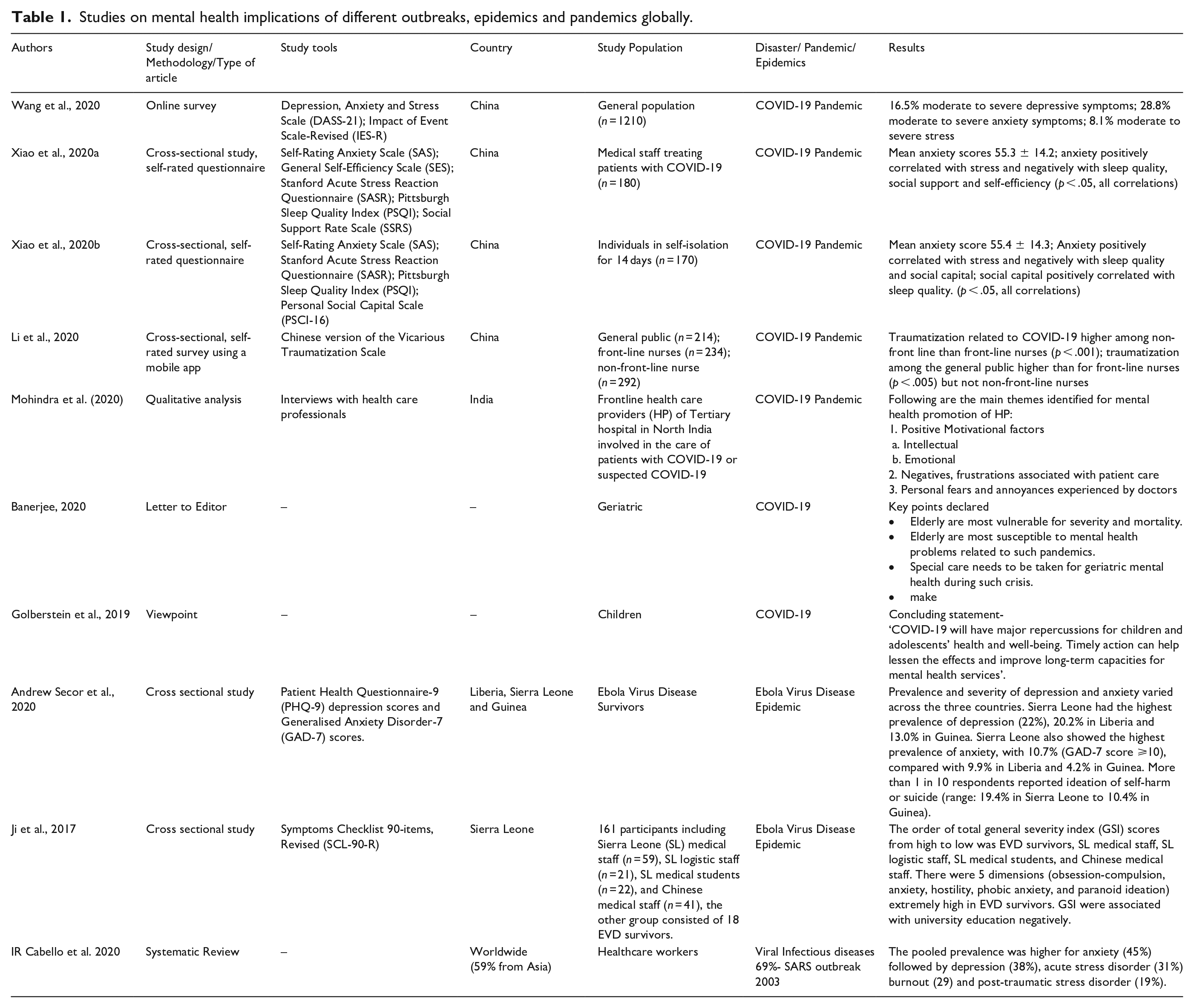
Mental health implications in specific population groups
People with pre-existing mental health illness
It is known that at the rise of an epidemic, generally, people with pre-existing mental health conditions are among the most affected (Chatterjee et al., 2020). The reasons include social stigmatization, risk of infection, low priority to morbidities of mental health etc. These coupled with cognitive impairment, little awareness of risk and diminished efforts regarding personal protection in patients, as well as confined conditions in psychiatric wards could add to the vulnerability of individuals with presenting mental health illnesses during the COVID-19 pandemic (Yao et al., 2020). Discrimination and fear of social isolation due to social distancing worsened by the effects of strict rules of lockdown could add to the cause of their vulnerability. The resulting emotional responses, leading to triggering, relapse or worsening of pre-existing mental health conditions could be another result of the effects of the COVID-19 pandemic. Wandering mentally ill people are at major risk of contracting illness secondary to compromised immune status. Relapse and exacerbation of severe mental health conditions secondary to lockdown and unavailability of psychotropics in rural pharmacies can also pose a hurdle to the health care system.
Frontline workers
The frontline workers including doctors, nurses, community health workers, sanitation workers, policemen, and other volunteers across the world are in an entirely unprecedented situation, having to make impossible decisions and work under extreme pressures. Working under stressful conditions with scarce resources affect not just their personal and family life, but also place them in a situation of moral injury, causing mental health problems. These symptoms can contribute to the development of mental health difficulties, including depression, post-traumatic stress disorder, and even suicidal ideation (Cheng et al., 2004; Duan & Zhu, 2020; Greenberg et al., 2020; Litz et al., 2009; Williamson et al., 2018). Apart from being at high risk of infection, front line healthcare workers including doctors are subject to stigma by community and neighborhoods. Many instances of eviction and harassment from house owners, violence on duties against doctors at the workplace, social isolation, and discrimination have been reported.
Children and older people
The sudden and drastic changes in the day to day routine can be extremely confusing and difficult to cope with the children, geriatric, and quarantined individuals. Closure of schools, recreational outdoor activities, not meeting their peers could take a toll on the mental health of the children. The geriatric population in India has been identified as a vulnerable group to COVID-19. Over 50% of those more than 60 years have at least 1 comorbidity putting them at a much higher risk. The psychological impacts of these populations can include anxiety and feel stressed or angry. Mental health impact can be particularly difficult for older people who are already experiencing cognitive decline, dementia, social isolation, and loneliness. Also, the progression of the disease tends to be more severe in the case of elderlies resulting in higher mortality (MOHFW, 2020).
Probable reasons (both evidence-based and theoretical possibilities) of mental health effects during COVID-19 pandemic among specific vulnerable population groups are summarized in Table 3.
Intervention strategies for mental health issues during COVID-19
Global context
A nationwide survey of psychological distress among Chinese people in the COVID-19 epidemic suggests the following recommendations for future interventions: (a) increased attention needs to be paid to vulnerable groups such as the young, the elderly, women and migrant workers; (b) the availability and accessibility of medical resources and the public health service system should be further strengthened and improved, with lessons from the management of the COVID-19 epidemic; (c) nationwide strategic planning and coordination for psychological first aid during major disasters, potentially delivered through telemedicine, should be established and (d) comprehensive crisis prevention and intervention system should be built including stable surveillance and monitoring systems, screening, referral, and targeted interventions should be built to reduce psychological distress and prevent further mental health problems.
On 27 January 2020, the National Health Commission in Mainland China issued the first comprehensive guidelines on emergency psychological crisis intervention in individuals who were affected by COVID-19; 19 the emphasis was on the delivery of mental health support services to patients and HCW by multidisciplinary teams that consisted of mental health professionals (Ho, 2020). In Singapore, the Ministry of Health, have kept the public abreast of the progress of the outbreak with regular news broadcasts and announcements on social media. Social media channels have also been set up by the state to curb the spread of false information and ‘fake news’ (Ho, 2020). Some interventions used by China, where the pandemic was first reported were, ‘Expert-teacher-coach’ intervention, frequently issuing guidelines for ‘Emergency Psychological Assistance’ by National Health Commission of China, applications like ‘WE-CHAT’ based survey program, online education using ‘WE-CHAT’, ‘WEIBO’ and ‘TIKTOK’. Artificial Intelligence-based ‘Tree hole rescue’ has also been utilized to combat mental health concerns and could be incorporated in other countries including India (Liu et al., 2020).
The Centre for Disease Control (CDC) advises parents to watch for changes in behaviour in their child. Since not all children and teens respond to stress in the same way a thorough and timely lookout for alert signs are important. Some common changes to watch for include the following (
In Italy, many independent (mainly online) initiatives have been established to provide psychological and psychiatric support to health professionals and laypeople, such as the ‘NON SEI SOLO’ [‘YOU ARE NOT ALONE’] and ‘Resilienza COVID-19’ [‘Resilience COVID-19’] projects of Rome’s Fondazione Policlinico Universitario Agostino Gemelli (Sani et al., 2020).
When looking largely at a global scenario, the varied population profile and mental healthcare needs of different countries are different. Therefore the intervention strategies taken up by the other high-income countries may not necessarily be effective in the context of India or similar Low and Middle-Income Countries (LMICs).
Indian context
The mental health issues in the context of the COVID-19 pandemic in India is more complex due to large proportion of socially and economically vulnerable population (children, geriatric, migrant laborers, etc.), high burden of pre-existing mental illness (Murthy, 2017), constrained mental health services infrastructure (Cullen et al., 2020), less penetration of digital mental health solutions, and above all scare created due to tremendous misinformation on social media. Thus, interventions should also be specific and relevant to the circumstances in India. The MOHFW- GOI has issued a tollfree helpline number for ‘Behavioural Health’, The Psycho-Social toll-free helpline-08046110007 can be used by anyone needing mental health assistance during the COVID-19 pandemic. A list of videos, advisories and resource materials on coping stress during COVID, yoga and meditation advice, taking care of the mental health of vulnerable groups, etc. have been provided in the MOHFW-GOI web portal (
The existing mental health-related initiatives include guidelines detailing about mental health and psychosocial considerations during the COVID-19 outbreak developed by the WHO Department of Mental Health and Substance Use, as a series of messages that can be used in communications to support mental and psychosocial well-being in different target groups during the outbreak (
NIMHANS suggests that a ‘Psychological intervention medical team’ can be formed as a standalone team or be part of the general medical team attending to people affected by the pandemic. The staff should consist of psychiatrists, with clinical psychologists and psychiatric nurses participating and the teams should formulate interventions plans separately for different groups for example: (i) Confirmed cases who are hospitalised with severe symptoms (ii) Suspected cases and close contacts of confirmed cases (iii) People with mild symptoms who are in home quarantine (iv) Health care personnel working with people with COVID-19 (v) General public (Cullen et al., 2020) As it is, mental health alone is a global challenge in itself and the COVID-19 pandemic greatly escalated the mental health burden as well.
Another initiative by the GOI is the
For the frontline workers fighting against this global crisis, routine support activities should be made available and must efficiently incorporate and include a briefing on moral injuries. It should also focus on raising awareness of other causes of mental ill-health and what to look out for.
Apart from these, mental health interventions have been issued by different states, NGOs and organisational bodies, some of which are listed in Table 2.
Some specific mental health interventions or initiatives taken by different states and institutional/ organizational bodies.
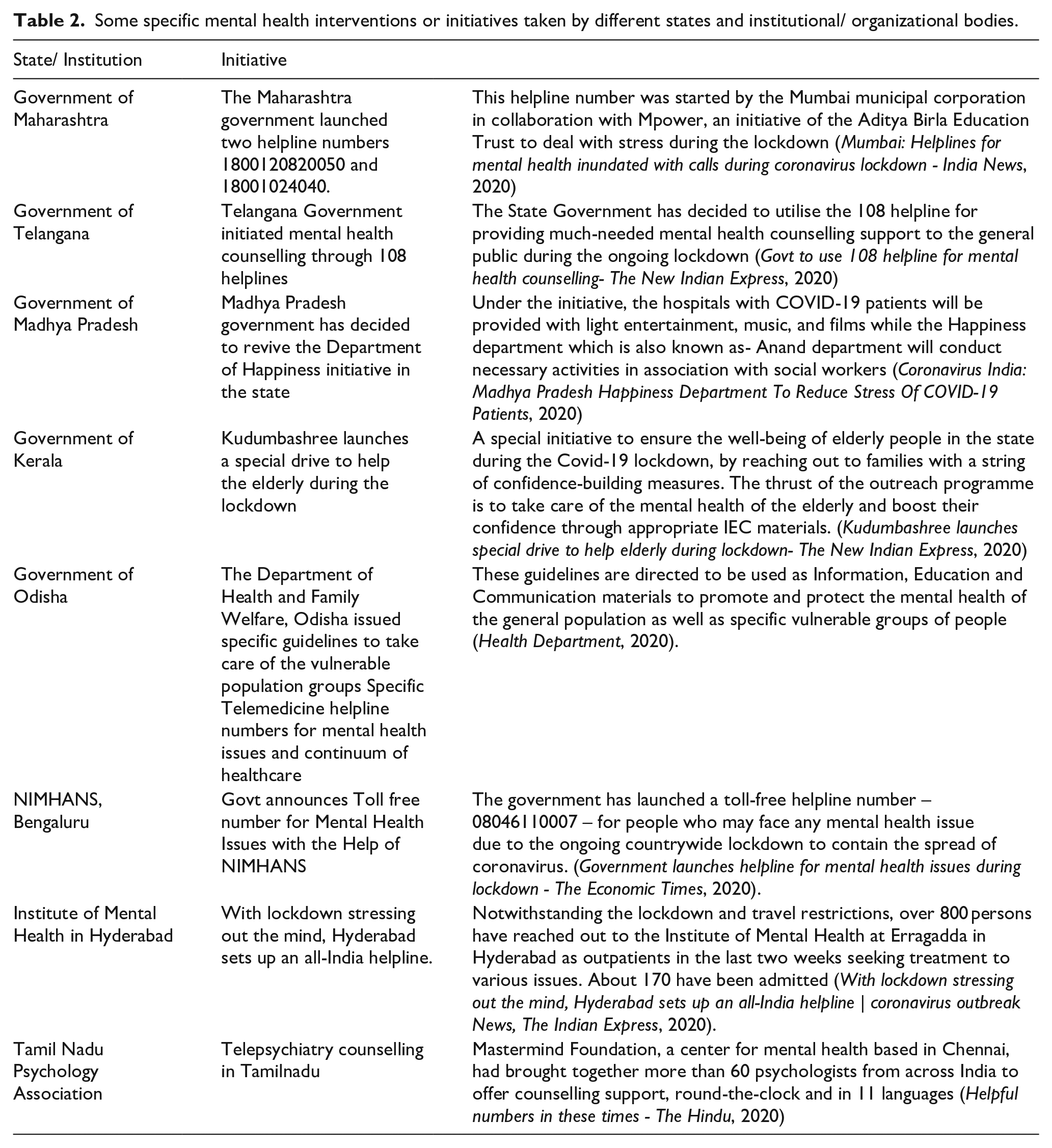
Discussion
Previous research has revealed a profound and broad spectrum of psychological impact that outbreaks can inflict on people. We found in this review that stress, anxiety, depressive symptoms, insomnia, denial, anger and fear were the major mental health manifestations of the COVID 19 pandemic. Anecdotal evidences and newspaper report also suggest an increasing trend of suicide in the community, people with COVID 19, and people in quarantine and isolation.
Fear of disease can precipitate new psychiatric symptoms in people without mental illness, aggravate the condition of those with pre-existing mental illness and cause distress to the caregivers of affected individuals. Regardless of exposure, people may experience fear and anxiety regarding falling sick or dying, helplessness, or blame people who are ill, potentially triggering off a mental breakdown (Ho et al., 2020). Anxiety and fear related to an infection can lead to acts of discrimination. For example, People from Wuhan were targeted and blamed for the COVID-19 outbreak by other Chinese people and Chinese people have since been stigmatized internationally, for example, use of the term ‘China virus’ and the use of terms such as ‘Wuhan virus’ and the ‘New Yellow Peril’ by the media (Usher et al., 2020).
The news of a pandemic is no less than a news of death and morbidity. In the case of COVID-19, we have tried to micro conceptualize based on the concept of ‘Breaking bad news’ and how the news of the pandemic was perceived globally could be very well classified according to stages of grief. Figure 1 shows how the stages of the COVID-19 pandemic could be placed into the Kubler-Ross stages of grief (
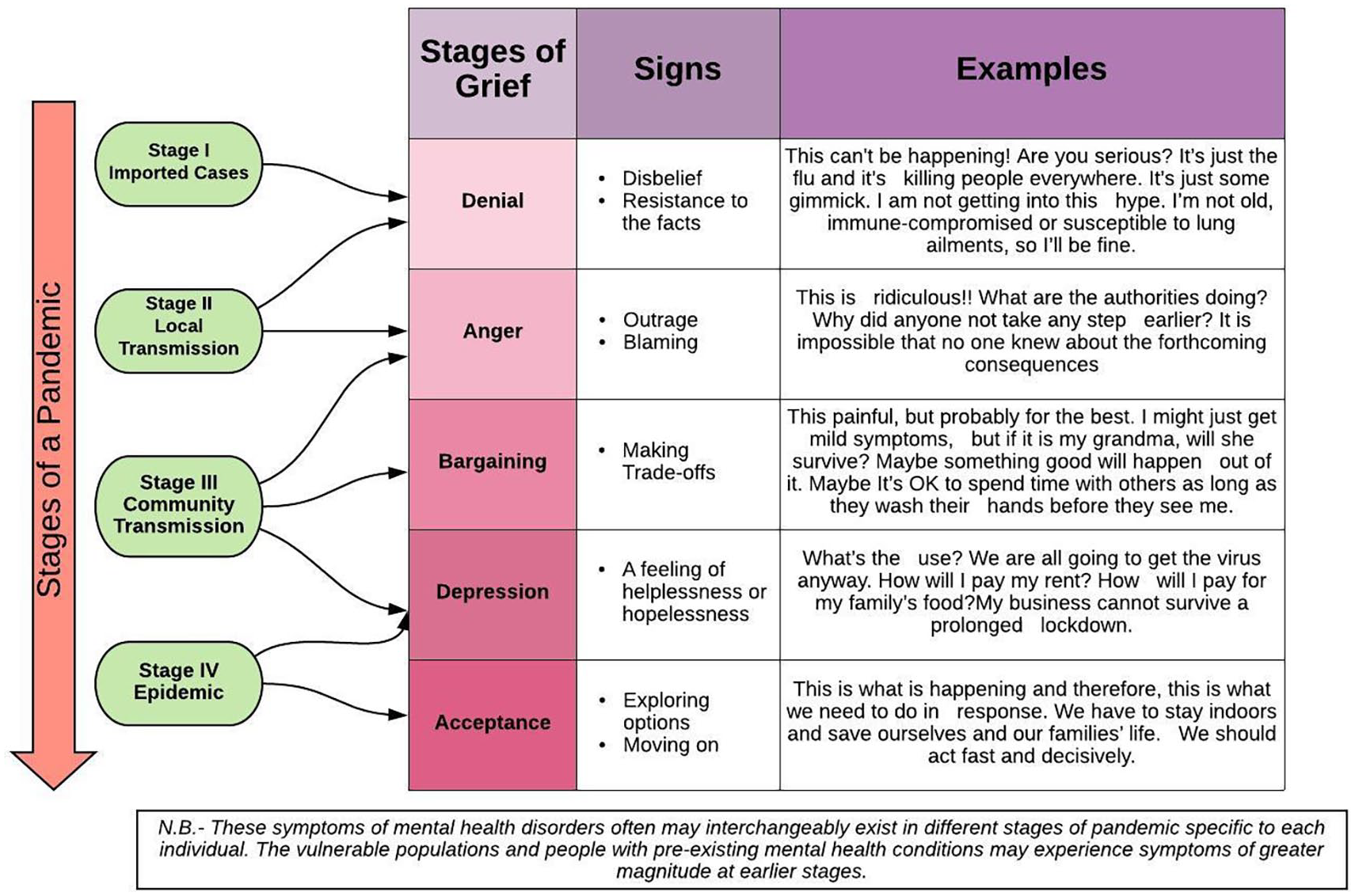
The stages of COVID-19 pandemic explained according to Kubler-Ross model of stages of grief.
We developed a conceptual framework both on the existing evidence and well as theoretical plausibility of mental health implication of COVID 19 pandemic and its response (Figure 2) While, the disease itself has instilled a sense of fear among front line workers, people with COVID 19 and population at large, this effect has been amplified by the overuse of social media which has led to an Infodemic (Orso et al., 2020; Vaezi & Javanmard, 2019). The fear due to disease could affect the population in general whereas it can have a precipitating effect of mental status of people with existing mental health conditions. The response to pandemic has led to a complete or partial restriction of movement in many countries. ‘Lockdown’, closure of educational centers and workplaces can have a significant impact on mental health due to changes in daily routine, social isolation in population, predominantly in children and older people, and people with existing mental health conditions. Abundance evidence is available to suggest that excessive use of social media has a significant impact on mental health (Ahmad & Murad, 2020; Gao et al., 2020; Ni et al., 2020). COVID 19 pandemic and restrictions imposed because of it had led to a surge in screen time as well as social media exposure. Closure of hospitals for non-essential services, in order to meet the surge capacity and halt the disease transmission, has caused serious disruption in routine health care services in many countries including India (Banerjee, 2020; How covid-19 response disrupted health services in rural India, 2020; COVID-19 significantly impacts health services for noncommunicable diseases, 2020). Non-provision of essential services may have a serious impact of older people, people with mental health conditions and chronic conditions. Whereas, a change in working pattern and increase perception of risk of disease can lead to anxiety, depression, stress and burnout among health care workers. Health care workers are also at risk of moral injury apart from recognized mental health conditions such as depression or post-traumatic stress disorder. Moral injury has been explained as a term that originated in the military and can be defined as the psychological distress that results from actions, or the lack of them, which violate someone’s moral or ethical code. People with moral injury are likely to experience negative thoughts about themselves or others as well as intense feelings of shame, guilt or disgust. As we have searched multiple portals to gather information and have also compiled results from various research papers available, the paper gives us a detailed overview of the mental health issues during COVID-19 and its responses, however a limitation of this review could be that, the information regarding data availability or sampling frame was not possible to be explored from every source of information, thus there could be a question about its generalizability to the population.
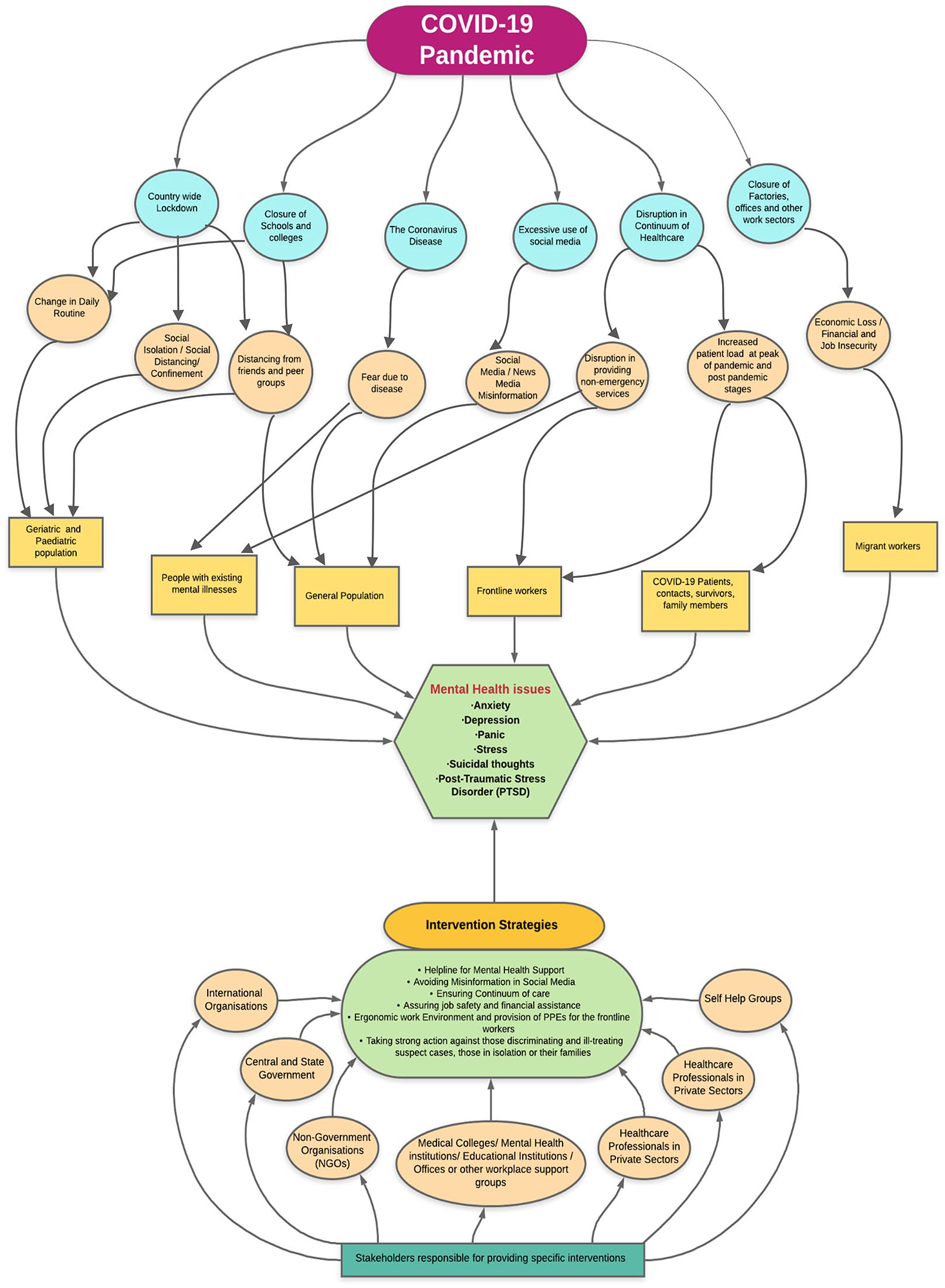
Conceptual framework of mental health issues during COVID-19 pandemic, its risk factors or causes; and some recommended intervention strategies.
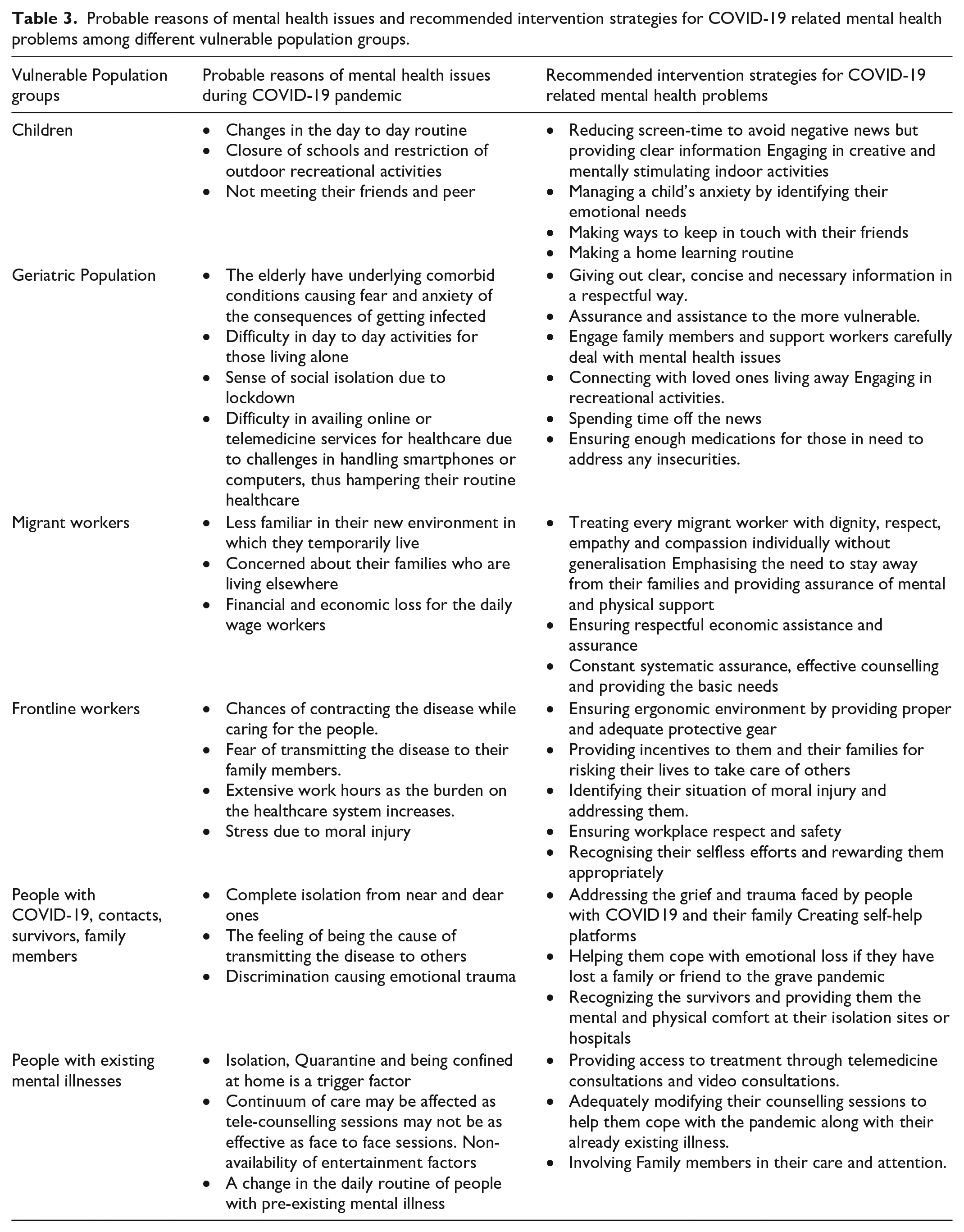
We propose a multi-pronged multi-stakeholder approach based on the experiences and evidence available from India and different countries. International and national organizations, governments, non-governmental organizations, health professionals’ groups and self-help groups are important stakeholders in providing interventions. Multi-pronged approach should comprise of a helpline number for easy access to mental health support, strict control over misinformation in social media, provision of continuum of care services at all level, financial and employment security to vulnerable groups, regulatory and legal provisions against discrimination and stigma of health care workers and other forces involved in pandemic response. We also suggest a framework for interventions and recommendations for specific population groups based on the possible reasons associated with their enhanced risk to mental health problems (Table 3).
Probable reasons of mental health issues and recommended intervention strategies for COVID-19 related mental health problems among different vulnerable population groups.
Conclusion
While the health system struggles to save millions of lives daily, there is probably a risk of a looming pandemic of hidden mental health issues which has a huge potential of shattering the existing mental health infrastructure. To handle the aftermath of the COVID-19 pandemic, the mental health of the people needs to be handled hand in hand and given equal importance along with other strategies to manage and control the disease and the pandemic at large. There is a definite need for specialized psychological intervention and proper and consistent risk communication and crisis communication. An updated, timely, uncomplicated guidelines should be put forth in order to avoid confusion and anxiety among the people. Hence, keeping a positive approach, effective communication strategies and understanding the problem statement, will help in dealing with the mental health issues faced by the world in this hour of crisis. The recommended intervention strategies should therefore be vulnerable group specific and further cause or risk factor specific also. Developing need-based interventions with proper risk communication strategies and keeping at par with the evolving epidemiology of COVID-19 would be instrumental in guiding the planning and prioritization of mental health care resources so that the mental health of most vulnerable groups is well served.
Footnotes
Author Contributions
All the authors contributed to the manuscript. The conceptualization of the study was done by AS, AR and SM, AR and AS contributed to the methodology of the study, AR, AC, AM, OB were responsible for the writing – original draft preparation. AS, AR, SM and AM contributed to the manuscript review, and editing.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
