Abstract
Objective:
Vaping, initially a smoking cessation aid, is now a widespread recreational activity sometimes associated with perceived health concerns. This study explored attitudes, harm perceptions and cessation barriers in the context of participants’ vaping behaviours, guided by the theoretical lens of fundamental social causes.
Design and Setting:
The study focused on a subset of 571 current adult vapers from a larger survey investigating vaping attitudes. It analysed open-text survey responses relating to vaping behaviours. To analyse the responses, we employed layered analyses, using deductive conceptual mapping to inform an inductive thematic content analysis.
Results:
Participants mentioned nuanced vaping risks, citing cancer and respiratory concerns, often comparing them to tobacco’s well-known harmful effects. Despite acknowledging vaping’s potential harms, participants perceived the practice to be less harmful than smoking, emphasising relative safety. Some viewed vaping positively for former smokers, contingent on regulated products. This complex attitude balance reflected the intricate interplay between health concerns and social dynamics. Recurrent vaping symbolised consistent engagement, with cravings and widespread availability associated with quitting challenges.
Conclusions:
Participants’ nuanced perceptions of health risks reflect a harm duopoly, resembling illicit drug harm tiering. There is a complex interplay between health knowledge and social influences in the context of vaping behaviours. Study findings underscore the need for messaging interventions discouraging vaping among those who do not smoke tobacco to consider these health and social dynamics, leveraging collaborative design.
Introduction
Since 1 October 2021, nicotine liquid in Australia has been classified as an unapproved prescription-only medicine, with no nicotine vaping devices currently registered on the Australian Register of Therapeutic Goods (Therapeutic Goods Administration, 2022).
Vaping devices, involving the inhalation of aerosol from electronic cigarettes which may or may not contain nicotine, initially emerged in the early 2000s as a smoking cessation aid (Pound et al., 2021) but their use has evolved into a popular recreational activity (Al-Hamdani and Manly, 2021; Trigg et al., 2023). Approximately 10% of Australian adults have tried vaping, with 2.2% identified as current regular users (Australian Bureau of Statistics [ABS], 2023). The perception of e-cigarettes as a safer alternative to tobacco smoking is widespread (Blackwell et al., 2023; Sanchez et al., 2021; Wilson et al., 2023), however, some research indicates negative effects such as respiratory and cardiovascular health risks (Cao et al., 2020; Javed et al., 2022).
Developing effective regulations and policies for vaping is complicated by the diverse motivations behind vaping. These include use as a tobacco smoking cessation aid (Bullen et al., 2013; Famiglietti et al., 2021; Hartmann-Boyce et al., 2021; Pound et al., 2021), a less risky replacement for tobacco products (Famiglietti et al., 2021; Hartmann-Boyce et al., 2023; McNeill et al., 2021; Wilson et al., 2021), and the relative affordability, pleasant flavours and reduced social stigma compared to smoking tobacco (Donaldson et al., 2021; Katz et al., 2022; Sanchez et al., 2021). A range of social factors are also influential, such as ease of access in many countries, social media engagement, and discretion, which have contributed to the widespread adoption of vaping (Rutherford et al., 2023; Trigg et al., 2023), especially among younger populations (Leung et al., 2023; Macleod et al., 2022; Mendelsohn and Hall, 2023). Furthermore, while some engage in vaping for enjoyment, performance and social connection (Donaldson et al., 2022; Katz et al., 2022), others see it as a coping strategy for mental health stressors (Grummon et al., 2022), leading us to believe there are a number of ‘social dynamics’ (Abel et al., 2002) operating.
These social dynamics have been examined in the context of cigarette smoking (Abel et al., 2002), however, in relation to vaping, little is known about the complex social factors and nuanced harm perceptions that influence individuals’ motivations and barriers to cessation, particularly among non-smokers and younger populations. Therefore, this study aimed to address these gaps by investigating how people who vape perceive harm, experience social pressures and navigate barriers to cessation.
Theoretical framing
Policies, knowledge and behaviours shape how technologies, including e-cigarettes, are used and understood (Link and Phelan, 1995). While disparities in health outcomes often arise as those with greater resources benefit more from technological advancements (Link and Phelan, 1995), in the case of vaping, the disparity lies in the widespread adoption of e-cigarettes across various social groups for recreational use, rather than solely as a cessation tool. This shift is driven through social networks, via knowledge dissemination, and the appearance of behaviours that have expanded the use of e-cigarettes beyond their original intent (Chu et al., 2017). Vaping, initially introduced as a smoking cessation aid (Famiglietti et al., 2021), has since evolved into a recreational activity shaped by social factors, such as accessibility, affordability, and social networks (Al-Hamdani and Manly, 2021). To explore these dynamics, we applied the concept of ‘social shaping’ (Link and Phelan, 2009) to understand how perceptions of harm and barriers to cessation are influenced by social contexts. Our study builds on prior smoking research (Link and Phelan, 2009) by examining how these social factors impact vaping behaviour and how they can inform more effective public health interventions. This information could be used to guide targeted public health campaigns aimed at addressing harm perceptions and reducing vaping uptake, particularly among non-smokers.
Methods
Sampling and recruitment
The survey was advertised on social media platforms Facebook and Instagram. The initial sample consisted of 646 participants from across Australia. After screening, we retained 571 participants who provided usable text responses to qualitative survey questions (unusable responses incorporated nonsensical or incomplete data). Recruitment for the survey was promoted through the research team’s social networks and via advertising on platforms like Facebook and Instagram. No specific vaping sites or forums were utilised. All participants we required to be ‘regular’ (i.e. at least weekly) vapers at the time of participation in the study, operationalised through screening regarding their recent vaping behaviours.
Data collection
The survey was designed using the Qualtrics platform. Participants were asked questions related to demographic information (e.g. age, gender, vaping frequency). Following this, they provided answers to a range of open text survey questions: (1) what are your attitudes towards vaping; (2) what do you think are the harms that might arise from vaping and (3) what barriers would arise if you attempted to cut down your vaping? These questions were developed by the authors based on similar approaches within the existing literature regarding tobacco use (Berridge, 2013; Hardcastle et al., 2016; MacDonell et al., 2013; Stark et al., 2008) and vaping harms (Blackwell et al., 2023; Vogel et al., 2021) and participants could opt-in to a prize promotion of one of the two $25 (AUD) gift vouchers. Ethical approval was received from the Human Research Ethics Committee of Griffith University (Approval: H22096).
Data analysis
We adopted a lens of critical realism (Bhaskar et al., 2005) to assist in framing (Fletcher, 2017) the nuanced perspectives of individuals regarding vaping behaviours against the backdrop of public health and policy (Rutherford et al., 2023) regarding this behaviour. This approach aligns with the theoretical framework of social shaping of health disparities (Link and Phelan, 2009), which posits that health advances tend to benefit privileged individuals and groups, perpetuating health disparities. The open-text responses from participants had no capped limit. The depth and complexity of participant responses was consistent with previous research that has demonstrated the dominance of vaping regulation topics across online forums and generally high level of interest and engagement from vaping users (Hardcastle et al., 2016; Notley et al., 2021).
Participant responses varied in length, with some being brief and others more extensive, challenging the predefined sub question parameters and requiring a triangulated analytical approach to analysis (Piatkowski et al., 2021; Turnock et al., 2023) to overcome the pitfalls of more reductionist methodologies (Morse and Mitcham, 2002). Consequently, a comprehensive examination of participant perspectives and experiences required a synthesis of responses across various sub questions, fostering a nuanced understanding of the overarching themes within the dataset. Because of this, we conducted a layered data analysis approach (Campbell et al., 2021), initially employing Leximancer (a text analysis tool) for co-occurring word analysis to extract key concepts from open text responses (see Figure 1). This method, chosen for its suitability for analysing a large sample of responses (Campbell et al., 2021), provided overarching themes via conceptual mapping. Shortcomings of Leximancer include its inability to identify emotive concepts and contextual concepts, potentially limiting the depth of analysis (Engstrom et al., 2022). However, acknowledging the shortcomings of this process (Lemon and Hayes, 2020), we looked to assess these conceptual themes through triangulation of coding using multiple techniques, a process known to enhance rigour and trustworthiness (Engstrom et al., 2022). This step was crucial in reflecting the social shaping theory, as it allowed the analyses to capture the socio-economic and cultural dimensions that influence vaping behaviours.
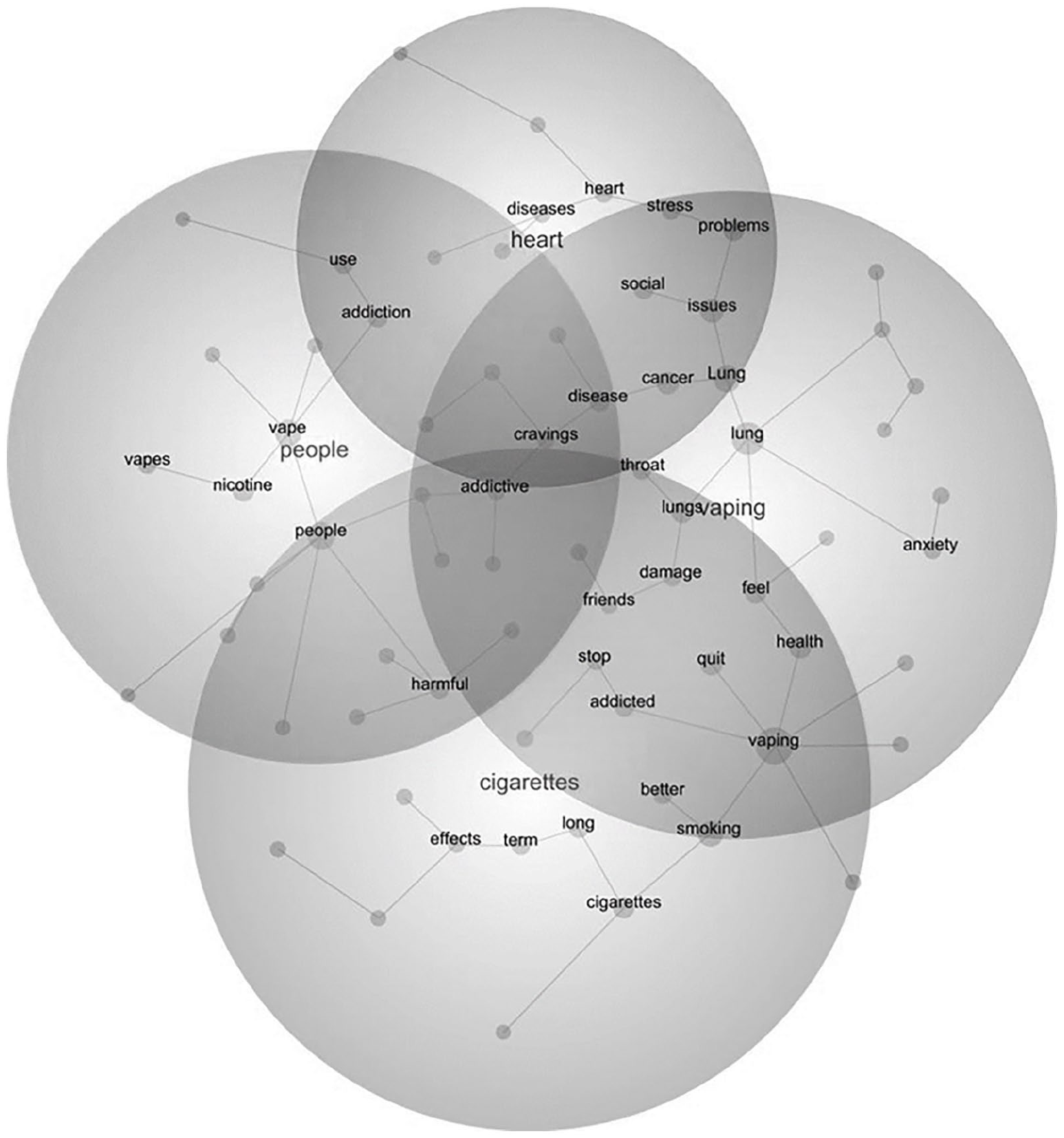
Open-text concept map.
Subsequently, we employed NVivo to code the concepts identified through Leximancer (Fletcher, 2017) and to guide thematic content analysis. Leximancer provided four key concepts – vaping, people, cigarettes and heart – along with 67 additional word-like concepts. We focused on the top concepts, such as vaping, lung, people, smoking, health, nicotine and cigarettes, which accounted for over 30% of relevance. In parallel, we incorporated emergent ideas such as health harms and addiction, refining and organising the data into three overarching themes.
Results
The mean age of participants was 22.5 years (SD = 7.4), with the majority of participants being younger and 63% (n = 360) falling below the age of 25. Regarding gender distribution, the study included 55% (n = 314) male participants and 45% (n = 257) female participants.
Among the 571 participants, the majority (53.6%; 306) indicated they were not currently using vaping for the intention for quitting smoking. The majority reporting vaping on an hourly basis (64.7%; 369), followed by daily (22.8%; 130) and weekly (6.5%; 37). Most participants used vapes containing both nicotine and flavour (70.7%; 404), with a significant portion using disposable pods (43.3%; 247). A notable percentage (53.6%; 306) reported not using vaping to quit smoking, while 24.1% (n = 138) did, and 22.3% (n = 127) had done so in the past. A majority (62.2%; 355) had attempted to quit vaping.
Participants’ views on vaping revealed diverse attitudes influenced by health concerns, social norms, and addiction. They expressed perceptions of perceived health risks as well as nuances regarding the challenges of quitting. Overall, the findings highlight the complex factors shaping attitudes and behaviours related to vaping.
Perceptions of vaping-related health risks: ‘I think vaping is better than smoking’
Many participants perceived potential health harms associated with vaping, citing concerns such as cancer, lung diseases, heart problems, respiratory issues, and the likelihood of kidney or liver problems. This widespread recognition indicated their perceived understandings of the health risks attributed to vaping: P15 [18, Female]: Increased risk of cancer, increased risk of heart and lung disease, increased blood pressure and heart rate.
Interestingly, when contemplating the potential health harms, participants commonly framed their concerns by drawing parallels to the well-established long-term effects of tobacco smoking, such as cancer rates. This tendency to contextualise vaping-related health risks in comparison to the known risks of tobacco smoking suggests a cognitive framework in which individuals engage in a harm duopoly, weighing the perceived dangers of vaping against the established health hazards of smoking. This finding shows that people’s attitudes towards vaping are shaped by comparing its harms to those of cigarettes, reflecting how they weigh vaping’s risks and uncertainties: P177 [19, Male]: There is little known about the long-term effects. I have no idea, perhaps similar effects to long term tobacco smokers such as cancer rates. P513 [20, Male]: The comparison of these illnesses to those contracted by long term cigarette smoking is completely inappropriate, as these two [vaping and smoking] are very different.
Some participants articulated the perception that vaping, with appropriate regulation, was less harmful compared to traditional tobacco smoking in its relative safety: P69 [19, Female]: I believe that properly regulated vapes with properly made ingredients are better than smoking cigarettes.
Participants’ belief that vaping was less harmful than tobacco smoke reflects the broader evidence supporting vaping as a healthier alternative to tobacco smoking (Hartmann-Boyce et al., 2023). This perception influences attitudes and behaviours, leading people to understand vaping as a less harmful choice: P249 [29, Female]: Vaping is not a carcinogen and is not harmful like tobacco smoke, it should not fall under the tobacco act.
There were, however, different views offered by participants. Some expressed a positive stance on the health benefits of vaping for former smokers. They highlighted their perception of vaping as a potentially advantageous alternative for those in the process of quitting traditional smoking: P98 [30, Male]: I am very positive about the health benefits of vaping for recovering smokers. I took up vaping to reduce my cigarette consumption. I was able to transition from smoking a pack to a pack and a half of cigarettes daily to using a vape exclusively in the space of less than a week.
Participants perceived regulated vaping products as less harmful compared to cheaper disposable e-cigarettes, which they associated with higher risks. This indicates a nuanced understanding of vaping’s health impact, with many participants recognising that product quality and regulation play significant roles in harm reduction. Their attitudes revealed a blend of optimism towards regulated products and caution regarding those with uncertain risks, reflecting a sophisticated approach to evaluating the comparative health impacts of vaping and smoking: P105 [48, Female]: Although there is limited long term research, I believe it is less harmful than smoking if you use regulated products not the cheap disposable e cigarettes which may contain harmful chemicals.
Health and social dynamics: ‘It’s considered a new norm to society’
Participants exhibited an array of attitudes and emotions towards vaping, showing some duality in their sentiments. Many participants acknowledged the perceived health risks associated with vaping, with concerns about ‘chemicals’ causing harm, mainly isolated to the lungs. Despite an apparent recognition of the detrimental impact on health, the compelling influence of societal expectations revealed an interplay between personal wellbeing and the desire for social acceptance: P132 [28, Female]: Nothing, I know it’s terrible for your health . . . but I also definitely understand the social pressures that come with it.
In this way, the concept of ‘health’ was tethered to the social relations surrounding vaping. Participants expressed understanding of the ‘pressures’ that contribute to vaping behaviour, despite acknowledging the recognised health hazards. The chemical composition of vaping products, sometimes viewed as harmful, was juxtaposed against the role vaping played in stress relief and coping with life pressures, revealing some semblance of dissonance reduction: P26 [19, Male]: They contain so many chemicals that do a lot of harm to your body, especially your lungs. They probably do the same amount, if not more damage than cigarettes. I would lose the ability to release my stress; I use vaping to cope with pressures from uni [university] and friends and family and all problems in my life, and vaping is a break from all of that.
This relationship between health and social dynamics extended beyond physical wellbeing to encompass broader lifestyle considerations. The potential for future deterioration in lung health and the perceived impact on life expectancy was juxtaposed against the valuable and present social functions of smoking and vaping. Peer pressure, societal norms and the desire to be perceived as ‘cool’ contribute to the ongoing practice despite participants perceiving that it is associated with health-related drawbacks: P531 [18, Male]: If it wasn’t vaping, it would be cigarettes. People have always smoked, and they will be for a long time. All cancers from smoking and probably more. Peer pressure by friends to continue. I believe it’s considered a new norm to society and possibly a trend that you’re cool if you vape.
Many participants acknowledged the challenges associated with social influence, underscoring the pervasive influence of social relations on individual behaviour. This observation highlights how peer pressure can strongly reinforce vaping behaviours, often overriding personal health concerns. The desire to fit in with a social group whose members vape frequently outweighed individual health reservations, illustrating the complex interaction between social influences and personal choices: P427 [18, Male]: For me the biggest barrier is being surrounded by people who are constantly vaping . . . the temptation is strongest when people around me are vaping.
Relative indifference towards vaping’s safety and long-term health risks, often accompanied by disinterest in these factors, suggests that social and pleasure-related aspects were prioritised over health concerns. This attitude, expressed by several participants, reflects a focus on immediate social gratification and enjoyment, with participants downplaying health risks in favour of the social and pleasurable benefits of vaping: P13 [18, Male]: I don’t think it’s safe long term or healthy, but I don’t really care.
Cravings and long-term use: ‘I hate it, but I can’t stop’
The recurrent nature of vaping was symbolised by its constant presence in participants’ lives, highlighting a pattern of consistent engagement with this behaviour. Many participants suggested that vaping has become a regular and habitual part of their daily routines or experiences: P116 [18, Male]: [Vaping is] A common reoccurrence and comfort in my life.
Cravings, coupled with the ubiquitous presence of vapes and the ability to use them in locations where tobacco smoking is prohibited (e.g. indoors), made it challenging to resist the urge to vape or cease the desire for it. This dynamic between individual cravings and the widespread availability of vapes indicated that cues in the social environment played a crucial role in sustaining or exacerbating vaping. The constant visibility of vapes likely served as a persistent cue, reinforcing participants’ desire to engage in vaping behaviour: P412 [27, Male]: Addiction/ social triggers. Cravings paired with vapes literally being everywhere makes it hard to avoid them/ stop wanting them.
Accordingly, an underlying theme of problematic vaping was reported by participants, who frequently described patterns of ‘addiction’ in their vaping. They reported the desire to quit was insufficient to overcome cravings and withdrawal, underscoring the struggle individuals face in balancing health concerns with this behaviour: P234 [20, Female]: I hate it, but I hate going without it I feel so unwell all the time I have a lot of commitments . . . I don’t think I could deal with the s**ts I get every time I try and quit right now, I hate it, but I can’t stop.
Participants reflected an understanding of vaping’s role in managing stress or emotional challenges. However, the characterisation of vaping as a ‘slippery slope’ implies an awareness of the potential for unintended consequences and escalation to long-term nicotine addiction: P110 [18, Female]: No, [it’s] more a coping mechanism I think that it’s a bit of an unassumingly slippery slope for most people, it’s very quick and easy to become addicted to vapes, especially the disposable pod kits.
Furthermore, the widespread accessibility of vapes and the social acceptance of vaping, made it challenging for some individuals to disengage from this behaviour. Availability and social acceptance further reinforced the cycle of use, contributing to the persistent challenges faced by individuals who attempted to cease use: P265 [18, Female]: The constant temptation to vape because it is so accessible to me and there is always someone around me with a vape.
Overall, the acknowledgement of vaping’s re-engaging nature reflects the general challenges faced by individuals grappling with long-term use. Participants reported an emotional toll and internal conflict when attempting to quit. This cyclic struggle of attempting to quit and relapsing to vaping highlights the addicting nature of nicotine and the potential barriers when considering cessation of this behaviour: P366 [22, Male]: It’s not great and very addictive and really destroys your self-respect when you keep trying to quit but go back to it.
Discussion
The findings from this study are consistent with broader theoretical frameworks that stress the powerful influence of social dynamics and social relationships on health-related behaviours (Link and Phelan, 1995, 2009; Phelan et al., 2004). In line with the theory of fundamental social causes, our findings indicate that vaping is conceptualised in an integrative manner regarding social factors that permeate social perceptions, risk evaluation processes, and experience of addiction, shaping health decisions and influencing vaping behaviour. This echoes the historical trajectory of smoking cessation strategies (Link and Phelan, 2009), where the dissemination of health-enhancing information was found to be influenced not only by medical knowledge but also by social factors, such as through peer influence and social context. This interplay highlights the need for interventions that address both health knowledge and social influences in the vaping context. These data suggest that effective public health messaging could leverage the harm reduction benefits of regulated vaping products for smokers while emphasising tailored messages to discourage vaping among non-smokers, especially young people. Ensuring the accurate reporting of ingredients in regulated products (Gartner, 2023) is essential for supporting smokers transitioning away from cigarettes and preventing initiation among those who have never smoked.
Social perceptions of vaping, including health risks, reveal a complex interplay between awareness of and comparison with that of tobacco smoking and e-cigarettes, consistent with existing work (Al-Hamdani and Manly, 2021; Cooper et al., 2018; Langley, 2019; Manzione et al., 2020; Romijnders et al., 2018; Vogel et al., 2021). For instance, in one study conducted in the USA, 21% of e-cigarette-naïve young adults initiated e-cigarette use during young adulthood, with lower perceptions of health harm and addictiveness predicting initiation among non-smoking college students (Cooper et al., 2018). Acknowledging concerns like respiratory issues (Marques et al., 2021; Romijnders et al., 2018), participants in the current study often framed these risks in a comparative context, establishing a harm duopoly and tethering vaping perceptions to smoking perceptions, either comparatively or contrastingly. Despite recognising potential harms, participants generally understood that vaping is less harmful than smoking, emphasising its relative safety in explaining their vaping behaviours. This perception of reduced harm, however, could be skewed by the type of vaping products used. Participants in our study recognised that regulated e-cigarettes are perceived as less harmful compared to unregulated disposable vapes, which may carry unknown risks. These types of harm ‘tiering’ appraisals have been noted between smoking and e-cigarette use (Wackowski et al., 2016), as well as among people who use illicit drugs (Piatkowski et al., 2023a), something which we have extended specifically to vaping behaviours in the current paper. Overall, this finding aligns with those in previous studies suggesting a harm reduction perspective exists among people who use e-cigarettes (Hart et al., 2018; Jackson and Bullen, 2022; Notley et al., 2018) as well as most vapers (Erku et al., 2020; Wilson et al., 2021). Messaging strategies can leverage this harm reduction perspective by emphasising the benefits of regulated products over unregulated ones. Effective public health campaigns should address the need for regulation to ensure the availability of safer, regulated vaping products and to diminish the influence of unregulated markets. This approach can help clarify the risks associated with different vaping products and enhance the overall effectiveness of smoking cessation strategies. Implementing policy regulations, such as curbing underground vaping markets, is crucial to supporting these messaging efforts and ensuring that consumers are not misled about the safety of the products they use.
Participants’ attitudes towards vaping reveal an interplay between personal health concerns and social influences. The challenges and internal conflicts described underscore the difficulty of addressing what they perceive as ‘problematic’ vaping. In this way, our findings extend the broader discourse surrounding smoking, e-cigarettes and vaping, where individuals navigate a landscape of health concerns, social influences and harm perception (Dai et al., 2022; Grummon et al., 2022; Hartmann-Boyce et al., 2021; Jackson and Bullen, 2022; Vogel et al., 2021; Yong et al., 2022). The harm duopoly, whereby participants weigh vaping risks against those of tobacco smoking, offers insights into how individuals rationalise their choices within the context of well-established smoking-related health hazards. For instance, in a recent study conducted among adults who smoke in the UK, although many people correctly viewed e-cigarettes as less harmful than combustible cigarettes, approximately 41% considered them equally or more harmful, or were unsure (McKeganey et al., 2023). Qualitative analyses showed that these perceptions were influenced by a complex mix of beliefs, fears and uncertainties about the long-term impact of e-cigarettes and their likely increased usage compared to combustible cigarettes (McKeganey et al., 2023). This is consistent with evidence from cohorts of UK smokers who do not vape, who were found to express significant misperceptions about e-cigarette harm (Svenson et al., 2021). Fortunately, there is evidence to indicate that these misperceptions can be corrected via the use of informational videos. For instance, participants who viewed a video featuring e-cigarette experts had the most accurate harm perceptions and knowledge, with 67% indicating they would try e-cigarettes in a future quit attempt, compared to lower rates in other groups (Svenson et al., 2021). Future campaigns could utilise participant perspectives to inform collaboratively driven harm reduction strategies both including and beyond informational videos. This type of collaborative work with consumers has demonstrated increased community receptivity for public health initiatives (Piatkowski et al., 2023b, 2024) and approaches in this licit sector (Harden et al., 2001) may adopt similar frameworks for curbing vaping initiation among non-smokers (Stalgaitis et al., 2023).
Limitations
Limitations of this study include a reliance on self-report data, and a sample predominantly consisting of young adults from one geographic region, limiting generalisability. In addition, using an online survey with specific, closed questions may have restricted the depth of responses and missed perspectives beyond the predefined concerns about harm. The open-ended nature of the responses, while providing some insight, did not fully capture the nuances and complexities of participants’ attitudes towards vaping. Despite these constraints, the findings offer insight into the complex interplay between social dynamics and vaping behaviours. In conclusion, addressing vaping-related health disparities necessitates nuanced interventions that acknowledge the complex intersection of health knowledge and social influences. Future research should consider more in-depth qualitative approaches to better explore these complexities.
