Abstract
Objective:
Suicide is one of the leading causes of death of men. This article reports on men’s experiences of using an e-mental health resource, HeadsUpGuys, which was designed to support men’s management and recovery from depression and suicidality.
Design:
Survey methodology was used to report men’s experiences of using the website. Constructs of interest included mental health literacy, stigma, attitudes, taking action, help-seeking and satisfaction with the resource. Survey items were developed specifically for the study.
Setting:
The survey was conducted online.
Methods:
Participants were recruited via the HeadsUpGuys website (headsupguys.org) and invited to participate in the survey if they were (a) male, (b) visiting the site for help with their own health, (c) 18 years of age or older and (d) able to read English.
Results:
A total of 443 men participated in the study. A high proportion indicated that visiting HeadsUpGuys helped improve their knowledge of suicidality among men and better recognise symptoms of male depression. The majority reported a reduction in their stigmatising beliefs about depression and suicidality among men. An increased sense of hope for recovery was reported by many participants. The majority of men also reported feeling inspired to take action towards recovery and having a better understanding of the steps they needed to take. Furthermore, a high proportion indicated they were more likely to seek help from both peers and professionals after visiting the site. Most men reported being satisfied with the HeadsUpGuys resource and would recommend it to others.
Conclusion:
A tailored mental health resource for men has the capacity to facilitate important shifts in constructs that play a critical role in shaping help-seeking behaviours among men. Considering the dearth of free public health resources to support men’s mental health, the HeadsUpGuys programme not only helps to fill this gap, but also provides an example of effective engagement of men to guide the development of other tailored programmes.
In 2019, the World Health Organization reported 759,028 deaths from suicide globally, 523,883 of which were men (Ilic and Ilic, 2022; World Health Organization, 2021), indicating that men account for nearly 70% of suicide deaths internationally. While often referred to as a ‘silent crisis’, male suicide is emerging from the shadows to be appropriately recognised as a serious public health crisis considering its profound social and economic impacts (Cerel et al., 2019; Peterson et al., 2024), which demand gender-responsive attention and action (Ogrodniczuk et al., 2023).
However, despite the increasing acknowledgement of the problem, there persists uncertainty regarding optimal approaches to addressing male suicide. Among the most robust risk factors for suicide is untreated depression (Li et al., 2011), making this a primary target for preventive interventions aimed at reducing male suicide rates. However, empirical evidence indicates a pervasive reluctance among men to seek professional assistance for mental health issues, including depression (Seidler et al., 2016). This reluctance aligns with established understandings of men’s psychological help-seeking behaviour as conflicting with traditional masculine norms including strength, self-reliance and stoicism (Seidler et al., 2016). In addition, concerns regarding the stigma associated with acknowledging the need for mental health care can further deter men from seeking in-person assistance for depression (McKenzie et al., 2022). For example, some men may perceive help-seeking as an act that communicates weakness and failure; consequently, they may fear judgement from others and ostracisation if they seek support (Bennett et al., 2023). More generally, several authors have described that for many men, physical illness represents a legitimate reason for accessing health services, whereas struggling with aspects of psychological illness does not warrant professional help due to the stigma still attached to it (Gough, 2016; Seidler et al., 2016). The admission of ‘unmanly’ depressive symptoms, for example, and the violation of masculine norms of self-reliance and stoicism represented by help-seeking carry with them fears of vulnerability and rejection (Vickery, 2021). As McKenzie et al. (2022) describe it, ‘being on the receiving end of stigma can lead to loss of hope and self-esteem, shame, and disempowerment’ (p. 2). Given the significant social and economic implications of untreated depression in men (White et al., 2011), coupled with persistently high rates of male suicide internationally, there is an urgent need to develop gender-responsive resources that are tailored to meet men’s needs. Such resources should aim to facilitate men’s engagement with their mental health and increase their utilisation of professional services when necessary (Seidler et al., 2018).
The burgeoning field of eHealth (which refers to virtual, Internet-delivered health services) offers a promising avenue for delivering personalised interventions to men, signalling a growth frontier in tailored healthcare delivery (Linardon et al., 2019). Services and resources delivered via the Internet can permit men to access care in a way that may be less intimidating and confrontational, that maintains confidentiality and anonymity, and does not compromise traditional masculine norms such as being in control, self-sufficient and invincible (Ringrose and Wang, 2022). Studies indicate that young men in particular exhibit a marked preference for accessing health information and interventions through web-based platforms (Pretorius et al., 2019). Numerous eHealth programmes tailored to address diverse health concerns among men (e.g. smoking, prostate cancer, HIV, weight loss) have been developed and shown to have generally positive impacts on acceptability, feasibility, engagement and improved health outcomes (Bottorff et al., 2016; Forbes et al., 2019; Hirshfield et al., 2019; Young and Morgan, 2018). Increasingly, there is growing attention on initiatives focusing on various psychological outcomes (e.g. self-efficacy, resilience, self-esteem, work performance and happiness/quality of life) (Kim and Yu, 2023), although few as yet specifically target men with depression (Fogarty et al., 2017; Opozda et al., 2024b; Young et al., 2021), despite the promising efficacy of eHealth interventions for depression more generally (Luo et al., 2020). Recognising the need for more work in this area, Cheng et al. (2020) advocate for the proactive development of targeted eHealth initiatives tailored specifically for men, with the aim of advancing their mental health self-management, as well as facilitating their engagement with healthcare services (Rice et al., 2018).
Leveraging the potential of eHealth solutions to offer men anonymity in seeking information about depression, a multidisciplinary team comprising researchers, clinicians and mental health advocates developed the HeadsUpGuys platform in Canada (headsupguys.org) (Ogrodniczuk et al., 2021). This initiative emerged from a rigorous development process, including environmental scans, surveys, focus groups and interviews with men who had experienced depression and suicidality, culminating in the launch of this free online resource in June 2015. HeadsUpGuys provides targeted information, practical advice and strategies for managing and recovering from depression, tailored to a male audience, and in doing so, aims to bolster men’s mental health literacy. The choice of language on the website is intentionally non-technical and accessible, aiming to make the content approachable to a broad audience and serving to dismantle stigmatised beliefs about men’s mental health challenges. The platform is crafted to align with men’s preferences for independence, autonomy and self-reliance (Seidler et al., 2024), while also integrating messaging that norm and validate reaching out to peers and/or professionals. The design of HeadsUpGuys adopts a graduated approach to help-seeking, starting from encouraging self-management to norming engagement with external coaching, effectively addressing the gap between men’s propensity for self-directed mental health management and the utilisation of formal healthcare services. This strategy underscores the framing of effective self-management and asking for help to problem solve challenges as embodiments of masculine strength and courageous behaviours, thereby challenging traditional stigmas around men’s vulnerabilities by fore-fronting resiliencies for effective help-seeking (Oliffe, 2023).
A 5-year review of HeadsUpGuys revealed a high and rising volume of users, international reach and unprecedented engagement (Ogrodniczuk et al., 2021). These patterns have continued beyond the 5-year mark. Missing, however, is an assessment of men’s experiences of using the resource. To address this knowledge gap, this study reports men’s experiences of using HeadsUpGuys with regard to mental health literacy, stigma, attitudes, taking action, help-seeking and satisfaction.
Methods
Sample and recruitment
Following University of British Columbia ethics approval (H17-01334), participants were recruited via the headsupguys.org website and invited to participate in the survey if they were (a) male, (b) visiting the site for help with their own health, (c) 18 years of age or older and (d) able to read English. Men who expressed an interest in participating were linked to an independent survey site hosted by Qualtrics, where they were presented with the informed consent page. Those providing informed consent to participate then completed the online survey. Participants were not paid to participate. Participant names were not collected with their survey response data; only IP addresses and study ID numbers were associated with the collected data, which was stored on a secure Canadian server. The quality of the collected data was ensured by checking for duplication in IP addresses, evaluating completion times and screening for response biases (e.g. non-differentiated responding). A total of 443 men met the inclusion criteria and consented to participate in the survey.
Survey questionnaire
Items were crafted specifically for this study to address participants’ impressions of how visiting HeadsUpGuys impacted their mental health literacy, stigmatising beliefs, attitudes regarding recovery, action-taking and help-seeking and whether they were satisfied with the resource. Most items were rated on a 1 to 5 Likert-type scale (1 = not at all, 2 = very little, 3 = somewhat, 4 = considerably, 5 = very much), while a few used a Yes/No format.
Mental health literacy
Men were asked to rate the extent to which visiting HeadsUpGuys improved three aspects of their mental health literacy on a 5-point scale ranging from 1 (not at all) to 5 (very much). Three items addressed participants’ knowledge of depression in men, knowledge of suicide and suicidal thoughts in men and ability to recognise symptoms of depression (example item: To what extent did visiting HeadsUpGuys help improve your knowledge of depression in men?).
Stigma
To assess stigmatised beliefs, men were asked to rate the extent to which visiting HeadsUpGuys reduced their sense of stigma about both depression and suicide/suicidal thoughts among men on a 5-point scale ranging from 1 (not at all) to 5 (very much) (example item: To what extent did visiting HeadsUpGuys help reduce your sense of stigma about depression in men?). In addition, participants were asked to rate two items that addressed the extent to which visiting HeadsUpGuys helped them feel less alone in their experience of depression and suicidal thoughts, using a 5-point scale ranging from 1 (not at all) to 5 (very much).
Attitudes
To assess men’s attitudes regarding recovery, participants responded to the question ‘After visiting HeadsUpGuys, do you believe men’s recovery from depression is possible?’. Response options included ‘yes’, ‘not sure’ and ‘no’. Participants also rated the extent to which visiting HeadsUpGuys increased their own hope for recovery on a 5-point scale ranging from 1 (not at all) to 5 (very much).
Taking action
To assess HeadsUpGuys’ ability to prompt action among its users, participants were asked to rate the extent to which visiting HeadsUpGuys inspired them to take action towards recovery and better understand the ‘next steps’ needed to recover from depression on a 5-point scale ranging from 1 (not at all) to 5 (very much). They were also asked to rate the extent to which visiting HeadsUpGuys helped them better manage symptoms of depression on a 5-point scale ranging from 1 (not at all) to 5 (very much).
Help-seeking
To assess participants’ help-seeking behaviours, men were asked whether they were more likely to seek support from peers and/or professionals after visiting the website. Response options for these two questions included ‘yes’, ‘no’ and ‘no, had already sought sufficient support/help before visiting’.
Satisfaction with resource
To assess men’s satisfaction with HeadsUpGuys as a resource, participants were asked to rate their general satisfaction with the website on a 5-point scale ranging from 1 (not at all) to 5 (very much). Men were also asked if they would recommend visiting HeadsUpGuys to others in need. Response options for this question included ‘yes, and already have’, ‘yes’, ‘no’ and ‘not sure’.
Data analysis
Analyses were undertaken using SPSS version 27. Descriptive statistics were used to report frequencies and percentages of item rating responses. Responses are summarised below as being at least ‘somewhat’ (rating of 3 or higher) and at least ‘considerable’ (rating of 4 or higher). Exploratory analyses (analysis of variance, bivariate correlation) examined the associations that frequency of visits to HeadsUpGuys (once, twice, more than twice) and age had with the study’s key variables (mental health literacy, stigmatising beliefs, attitudes regarding recovery, action-taking and help-seeking, satisfaction).
Results
Sample description
Participants ranged in age from 18 to 79 years old (M = 45.14, SD = 14.56). The sample was primarily Caucasian (80.4%) and from Canada (76.5%). Most identified as heterosexual (83.7%) and were in a committed relationship and living with their partner (50.1%). The majority had received education beyond high school (80.8%) and worked full-time (51.0%). Among the participants, 48.2% had visited HeadsUpGuys only once, 24.7% had visited the site twice and 27.1% had visited more than twice.
Mental health literacy
As shown in Table 1, 72% (N = 317) of participants indicated that visiting HeadsUpGuys helped improve their knowledge of depression in men at least ‘somewhat’, with 42% (N = 186) reporting at least ‘considerable’ improvement. Similarly, 74% (N = 329) of participants reported that visiting HeadsUpGuys helped them better recognise depression symptoms ‘somewhat’, with 48% (N = 214) indicating ‘considerably’ better. Two-thirds (67%; N = 297) of participants indicated that their knowledge of suicide and suicidal thoughts among men improved ‘somewhat’ after visiting the website, with 37% (N = 164) reporting ‘considerable’ improvement.
Responses to survey questions (N = 443).
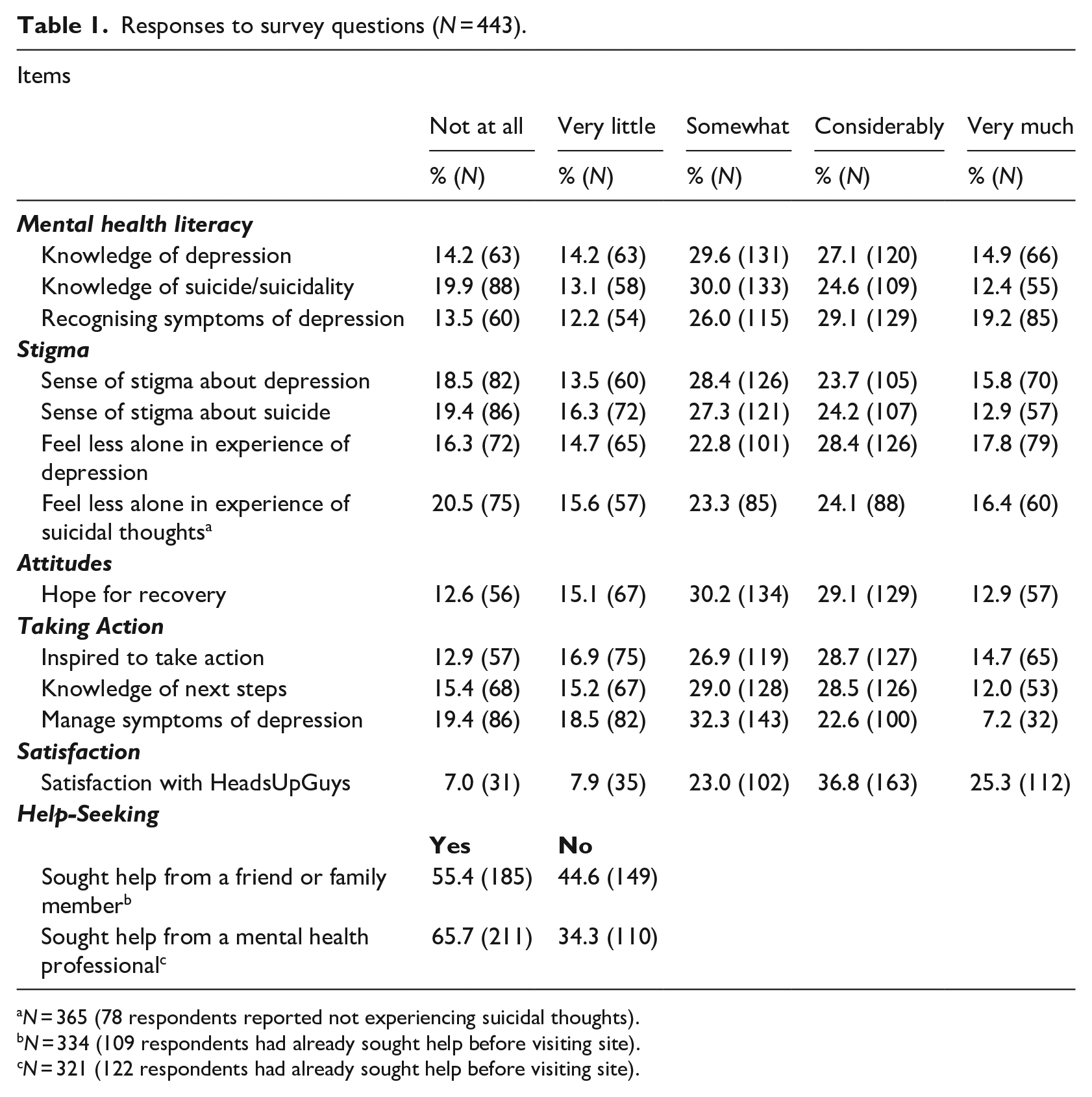
N = 365 (78 respondents reported not experiencing suicidal thoughts).
N = 334 (109 respondents had already sought help before visiting site).
N = 321 (122 respondents had already sought help before visiting site).
Stigma
After visiting HeadsUpGuys, 68% (N = 301) of participants reported that their stigmatising beliefs about depression in men had reduced ‘somewhat’, with 40% (N = 175) indicating ‘considerable’ reduction. In a similar fashion, 64% (N = 285) of men reported ‘somewhat’ of a reduction in their stigmatising beliefs about suicide and suicidal thoughts among men, with 37% (N = 164) revealing a ‘considerable’ reduction.
Approximately 7 out of 10 participants (69%; N = 306) reported being helped ‘somewhat’ to feel less alone in their experience of depression, with 46% (N = 205) indicating being helped ‘considerably’. Regarding suicidal ideation (365 men reported having experienced suicidal ideation), 64% of participants (N = 233) reported being helped ‘somewhat’ in feeling less alone in their experience of suicidal thoughts, with 41% (N = 148) indicating being helped ‘considerably’.
Attitudes
Subsequent to visiting HeadsUpGuys, slightly less than two-thirds of participants (61%; N = 270) indicated that they believed men’s recovery from depression was possible, with 2.5% (N = 11) reporting ‘no’, and 37% (N = 162) indicating that they were ‘not sure’. Nearly three-quarters (72%; N = 320) of participants reported that their sense of hope for recovery improved ‘somewhat’ after visiting HeadsUpGuys, with 42% (N = 186) indicating a ‘considerable’ increase in their sense of hope.
Taking action
Seventy percent of participants (N = 311) reported feeling ‘somewhat’ inspired to take action towards recovery after visiting HeadsUpGuys, with 43% (N = 192) indicating feeling ‘considerably’ inspired. A similar proportion (69%; N = 307) reported being helped ‘somewhat’ in better understanding the next steps to take towards recovery from depression, and 40% (N = 179) indicating a ‘considerably’ better understanding. Sixty-two percent of participants (N = 275) indicated that they were ‘somewhat’ better able to manage symptoms of depression after visiting HeadsUpGuys, with 30% (N = 132) reporting being ‘considerably’ better at managing symptoms.
Help-seeking
A quarter of participants (25%; N = 109) had already sought informal support before visiting HeadsUpGuys. Of those who had not previously sought support, just over half (55%; N = 185) reported that they were more likely to seek support from friends or family members after visiting HeadsUpGuys. Forty-five percent (N = 149) indicated that they were not more likely to seek support from friends or family.
Just over a quarter of participants (28%; N = 122) had already sought help from a mental health professional before visiting HeadsUpGuys. Among those who had not, 66% (N = 211) indicated that they were more likely to seek help from a mental health professional after visiting the site, while 34% (N = 110) reported that were not more likely to seek professional help.
Satisfaction with the HeadsUpGuys resource
The vast majority of participants (85%; N = 377) reported being ‘somewhat’ satisfied with HeadsUpGuys as a resource for men who are suffering from depression, with 62% (N = 275) indicating being ‘considerably’ satisfied. Nearly three-quarters (73%; N = 324) indicated that they would recommend HeadsUpGuys to others in need (19% already had), 24% (N = 105) were ‘not sure’, and only 3% (N = 14) indicated that they would not recommend the site to others.
Exploratory analyses
The associations that frequency of visits to HeadsUpGuys (once, twice, more than twice) and participant age had with the visitor impression variables (mental health literacy, stigmatising beliefs, attitudes regarding recovery, action-taking, help-seeking, satisfaction) were examined. In order to reduce the number of analyses conducted, one item that best represented each of the impression variables was selected for the analyses (see Tables 2 and 3).
Associations between frequency of visits and visitor experiences.
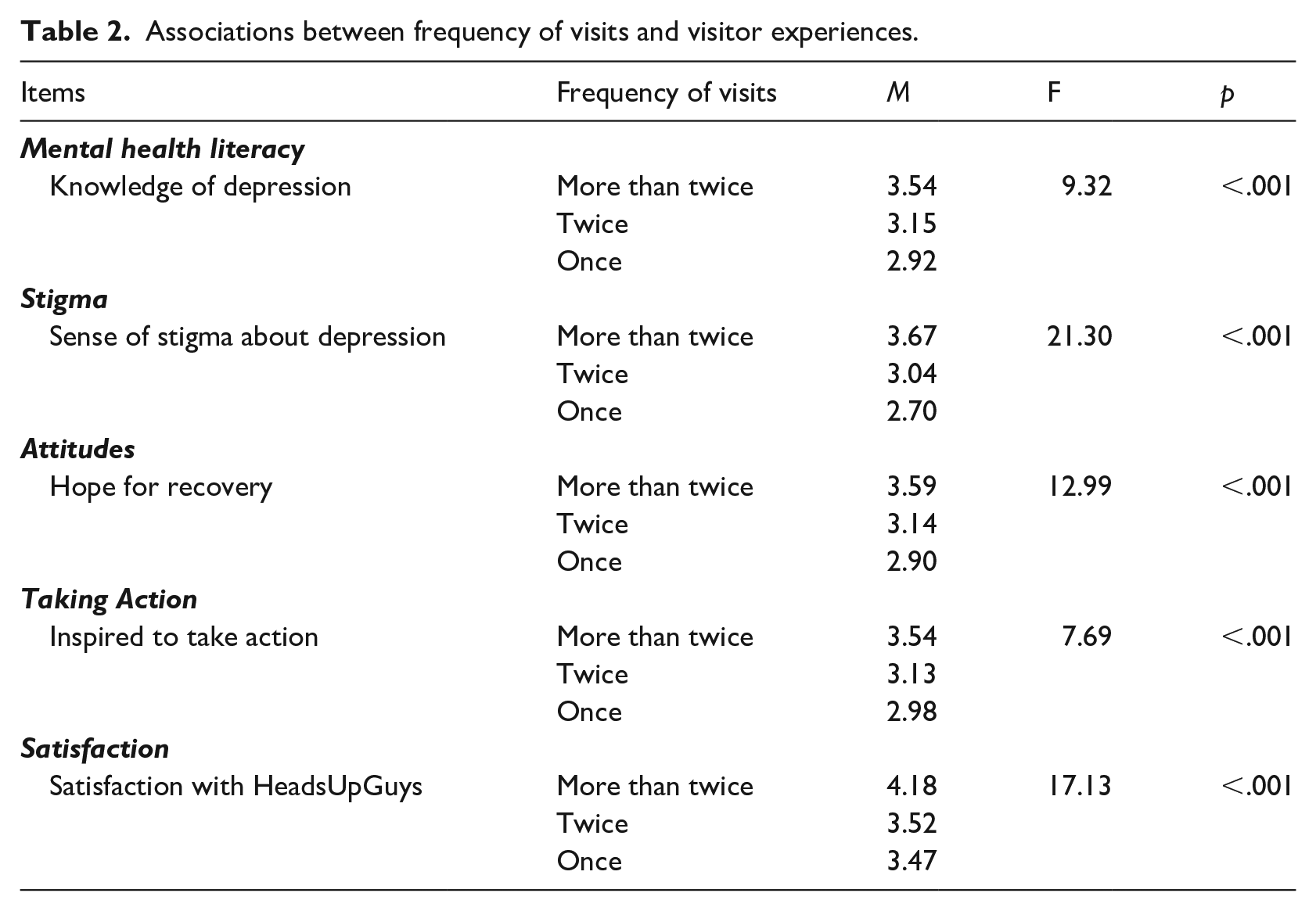
Associations between age and visitor experiences.

Analyses revealed significant associations between frequency of visits and each of the five impression variables. The findings indicated that men who visited HeadsUpGuys more frequently reported greater improvement in knowledge about depression, greater reduction in stigma about depression, greater hope for recovery, greater inspiration for taking action towards recovery and greater satisfaction. Similarly, age was found to be significantly associated with each of the five impression variables, indicating that younger age was related to greater improvement in knowledge about depression, greater reduction in stigma about depression, greater hope for recovery, greater inspiration for taking action towards recovery and greater satisfaction.
Discussion
Given the challenges of successfully and sustainably engaging men with professional mental health care services (Seidler et al., 2018), and the consequence that this carries for male suicide risk (Oliffe et al., 2020), it is crucial that novel means of engagement be developed (and scaled) for men struggling with mental health challenges. A survey of men’s experiences with HeadsUpGuys and the outcomes of their engagement provides evidence that this resource is a step in the right direction. A high proportion of men indicated that visiting HeadsUpGuys helped improve their knowledge of suicidality among men and better recognise symptoms of male depression. The majority reported a reduction in their stigmatising beliefs about depression and suicidality among men. An increased sense of hope for recovery was reported by many. The majority of men also reported feeling inspired to take action towards recovery and having a better understanding of the steps they needed to take. Furthermore, a high proportion indicated they were more likely to seek help from peers and professionals after visiting the site. Importantly, most men reported being satisfied with the HeadsUpGuys resource and would recommend it to others. Not to overstate the findings or imply attribution, but it is, nonetheless, clear that HeadsUpGuys offers important tangible gains for many of the men who access this resource.
Literacy and stigma
The impact of educating men about depression and suicidality was evident, with a significant proportion of participants in the present study indicating that visiting HeadsUpGuys helped improve their knowledge of depression and suicide among men, and better recognise symptoms of depression. Furthermore, the majority reported a reduction in their stigmatising beliefs about depression and suicidality among men. These findings align with results from recent systematic reviews indicating that digital interventions can effectively improve mental health literacy (Tian et al., 2024) and reduce stigma (Goh et al., 2021), although digital interventions focusing on these health-related constructs specifically in men are scarce. As a lack of knowledge about depression and the stigma surrounding men’s mental health are large barriers to entry for men in need of psychological interventions (Oliffe et al., 2016a, 2016b), facilitating change in these areas is key to encouraging (and bridging) men’s engagement with mental health supports and services. Indeed, recent commentaries on the poor state of men’s mental health have positioned the improvement of mental health literacy and reduction of stigma as critical for facilitating men’s uptake of mental health services (Kwon et al., 2023; Rice et al., 2018). By enhancing mental health literacy and reducing stigma through the use of targeted programmes such as HeadsUpGuys, men can be empowered to recognise symptoms, understand treatment options and overcome significant barriers to avail themselves of help.
Attitudes and action
The shift in men’s perspectives observed in this study extended beyond mental health literacy and stigma, with a high proportion of participants reporting that their sense of hope for recovery improved after visiting HeadsUpGuys. Hope plays a pivotal role in the recovery from mental illness (Laranjeira and Querido, 2022), serving as a catalyst for resilience and motivation. Research suggests that men with a more hopeful outlook exhibit greater treatment adherence, coping strategies and overall well-being (Schrank et al., 2011). Cultivating hope thus can significantly enhance mental health outcomes, offering men a sense of agency and optimism amid the challenges associated with depression and suicidality. To this end, future eHealth programme development for men with depression can build on the work of others who have developed hope-inspiring interventions (e.g. Chan et al., 2019) to be delivered as self-directed courses on digital platforms (e.g. websites). Indeed, digital interventions designed to cultivate hope are under development (Uribe et al., 2023), with some found to be effective already (Daugherty et al., 2018), and although none have focused directly on men, they could serve as useful templates for male-specific programmes.
Perhaps emboldened by hope, the majority of men who visited HeadsUpGuys reported feeling inspired to take action towards recovery. Moreover, they indicated having a better understanding of the steps needed to take for recovery. In this way, HeadsUpGuys functions as a means of permission and practicality for men seeking mental health care, by helping them to overcome significant barriers to accessing support (Rice et al., 2020). This help connects men’s ability to self-manage their mental health with informal supports and professional services, aligning with previous work pointing to strengths-based approaches for empowering and upskilling men to manage their own health while norming the inclusion of others to support their health management (Seidler et al., 2019; Sharp et al., 2022). Indeed, a significant proportion of men indicated they were more likely to seek help from both peers and professionals after visiting the site. The importance of shaping more positive help-seeking attitudes among men cannot be over-stated (Oliffe et al., 2020).
The positive impact of shifting men’s perspectives on personal mental health care and psychological help-seeking appears to be reflected in the fact that the overwhelming majority of men reported being satisfied with the HeadsUpGuys resource and would recommend it to others. Indeed, 20% of men said they had already shared the resource with others. With men often needing other men to norm distress disclosures and help-seeking (Vickery, 2021), the sharing among men of useful mental health resources can be regarded a form of mutual support – critical to promoting men’s mental illness. The growth of peer mutual help may well be attributable to resources such as HeadsUpGuys – wherein the sharing of useful resources among men does not transgress masculine norms for directly asking about or disclosing mental health challenges. That said, HeadsUpGuys and similar resources may be an important conversation starter for catalysing men’s mutual peer help.
Influencing factors
Exploratory analyses revealed that increased frequency of visits to the HeadsUpGuys website was associated with an improvement in all of the visitor impression variables, which is consistent with the conclusions from a recent systematic review and meta-analysis that found that the more users engaged with digital interventions, the greater their improvements in mental health outcomes (Gan et al., 2021). In the present study, men’s mental health literacy improved and their stigmatised beliefs about depression were reduced. Furthermore, returning visitors also reported greater hope for recovery, greater inspiration for taking action towards recovery and greater satisfaction. These findings point to the importance of creating content that encourages visitors to come back. Due to the design of the present study, it is not known what drew visitors to HeadsUpGuys to return.
It also emerged from the exploratory analyses that age was associated with each of the visitor impression variables, pointing to greater benefit among younger men. Younger participants may be more likely to engage with digital mental health resources than older men due to their higher familiarity and comfort with technology. Younger generations, having grown up with virtual environments, tend to be more adept at navigating online programmes and more inclined to use digital health resources (Lehtimaki et al., 2021). Although the digital divide between generations has narrowed (Elena-Bucea et al., 2021), some older men may still lack experience with and access to digital tools, and might therefore face barriers to the effective engagement with, and use of some digital technologies (Woerner et al., 2022). Nevertheless, older adults are motivated to use digital technologies to improve their mental health, but the design and promotion of resources for them should strategically build trust, buy-in and support to maximise the likelihood of their engagement and sustained benefits (Lattie et al., 2022).
E-health design considerations
When designing e-mental health programmes for men, several key considerations can enhance user engagement and benefit. The website should have a user-focused design with intuitive navigation and a responsive layout to ensure accessibility across different devices (Opozda et al., 2024a). The aesthetic should be clean and professional, avoiding overly clinical or stereotypically masculine themes that might alienate some users (Rice et al., 2018). Content should address common challenges experienced by men, including work stress, relationship challenges, depressive symptoms, anxiety and issues related to work–life balance (Seidler et al., 2016), using non-technical, active and empowering language that resonates with men’s experiences (Balcombe and De Leo, 2022). Interactive elements including self-assessment tools, goal-setting modules and progress tracking can enhance user engagement (Vial et al., 2022). Anonymity and privacy features are crucial, as men often hesitate to seek help due to stigma (Ringrose and Wang, 2022). Testimonials and success stories can motivate users and help reduce the stigma associated with seeking mental health support (Keum and Ogrodniczuk, 2023). Stakeholder-centred design, with collaboration between men with lived experience of mental health problems, family and friends who support these men, mental health professionals and researchers, will help ensure that the content is relevant and evidence-based (Bond et al., 2023).
Limitations
Limitations of the study include the use of survey items developed for the purpose of this study, and thus lacking previous empirical testing. In addition, the study did not use a formal pre–post experimental design that would permit conclusions of attribution. Furthermore, the study lacked a comparison group; thus, it is not known whether HeadsUpGuys is potentially more effective at influencing mental health literacy, stigma and help-seeking among men than other types of mental health resources. Regarding help-seeking, the study only assessed intention, and not actual help-seeking behaviour, although help-seeking intention is highly predictive of actual behaviour (Sagar-Ouriaghli et al., 2019). The study also asked respondents to reflect on self-perceived changes in the study constructs instead of assessing actual change across time. It also lacked a baseline assessment of depression; thus, it is not known how many participants may have been experiencing depressive symptoms, nor do we know how the severity of depression may have influenced participants’ experiences of visiting HeadsUpGuys. It would also have been beneficial to assess an array of participant characteristics to explore factors that might have influenced their experience of using the site.
Considering the preliminary nature of the present study and the limitations noted above, a future validation study should include a pre–post experimental, randomised trial design that utilises standardised measures of mental health literacy, self-stigma, help-seeking attitudes and behaviours, as well as visitor characteristics, such as depression severity and conformity to masculine norms, that may shape visitor engagement and experiences using an eHealth resource like HeadsUpGuys. Such a study could be complemented by the collection of qualitative data to provide nuance and depth to the study findings.
Conclusion
HeadsUpGuys was created in the absence of male-focused mental health resources a decade ago, establishing a first point of contact for those who would likely be unserved. Its position as a practical and anonymous eHealth service has been vital to its success in providing men with an access point to the information, support and professional services they need to manage their depression and oftentimes concomitant suicidal thoughts. It is important to note that HeadsUpGuys has attracted ongoing industry and philanthropic support to scale and sustain the resource. While the commercial determinants of health draw much debate (see Maani et al., 2022: 416), financial sponsorships of interventions and their marketing are valuable to realise the full potential of the catalytic research funding that seeds these innovative programmes.
As evidenced by the results of the present study and the continuously growing number of men engaging with the site (Ogrodniczuk et al., 2022), HeadsUpGuys has the potential to bring about legitimate change in the lives of men who may otherwise not receive the care they require. Furthermore, by way of its success, HeadsUpGuys is working to dismantle pervasive narratives surrounding men’s neglect of their mental health by demonstrating that in gender-responsive contexts, they will readily engage with mental health services. By supporting the autonomy of men in the self-management of their depression, and by offering accessible avenues for further engagement, HeadsUpGuys is continuing to transform the way we address men’s mental health promotion and illness management, providing evidence for the utility of its online presence and reshaping our approach to mental health care for men.
