Abstract
Objective:
This study explored medical trainees’ understanding of collaborative writing sessions in the Dominican Republic as a strategy to strengthen their technical writing and critical analysis skills in health education and communication.
Method:
We conducted semi-structured interviews with seven medical trainees who participated in a series of collaborative writing sessions and published their articles in medical journals. Thematic analysis was used to study coded notes and identify salient themes with quotations and a conceptual model.
Results:
Five perceived individual- and programme-level enabling factors of the collaborative writing sessions were described: (1) detailed agenda, (2) direct mentorship, (3) effective teamwork, (4) personal investment and dedication, and (5) future vision.
Conclusion:
Study findings highlight that collaborative writing sessions with direct mentorship offers medical trainees a unique opportunity to acquire key written communication and analytical competencies and publish their articles, as part of their professional development. The incorporation of these valuable health education training exercises for health professional students can help develop an academic culture of writing and publishing on emerging global health topics.
Introduction
As future leaders of national health systems, health professional students should remain up to date on clinical and community health priorities, contribute to research protocols and publications, and lead the delivery of relevant evidence-based health education messages for community engagement. Recognising the multifaceted challenges leading to the 2030 Agenda for Sustainable Development, the One Health concept – which highlights the complex interactions of the human–animal–environment nexus and underscores the need for multidisciplinary collaborations to address emerging health threats – can offer a holistic framework for students to analyse existing knowledge gaps (One Health High-Level Expert Panel (OHHLEP) et al., 2022; World Health Organization, 2020). By applying the One Health concept, they can expand innovative inquiry and foster scientific debate and collaboration to manage challenges reported by leading health agencies. By mastering skills in scientific writing and critical appraisal of the literature, they can advance the knowledge base, strengthen partnerships with community stakeholders, form academic networks for collaboration and feedback, establish faculty–trainee mentorship and gain professional recognition for scholarly contributions in health education and communication (Azer et al., 2014).
Collaborative writing, which focuses on connections between the writer and writing team to produce a scholarly product, is one approach to developing fundamental skills for technical writing and critical appraisal (Ramani et al., 2022). As writers keep abreast of the literature and seek potential collaboration opportunities, they engage with writing team members to create a ‘common document’ over an established timeline (Lingard, 2021). To support this capacity development, institutions have formed supportive faculty writing groups on manuscript, grant and narrative writing for faculty members (Boudreau et al., 2012; Chai et al., 2019; Remein et al., 2022; Steinert et al., 2008); workshops on op-ed and letter to the editor writing for medical trainees (van der List et al., 2022; Whittaker et al., 2020); and workshops on case report writing for medical trainees and clinician-educators (Sridhar et al., 2008). Journal clubs integrated into health professions curricula have helped students gain self-confidence, learn research and literature review techniques, and acquire key scientific knowledge and critical analysis skills (Honey and Baker, 2011; McLeod et al., 2010).
Due to the comprehensive curriculum of scientific competences in basic and clinical sciences, critical analysis adapted for technical writing has been inconsistently prioritised across health professions schools, especially in low- and middle-income countries. Limited information exists on the overall impact of collaborative writing activities for health professional students (Chen and Forbes, 2014; de Oliveira et al., 2011; Kusurkar, 2022; Manian, 2020). In addition, research training has been incorporated engaged with variably in medical schools, and the best pedagogical format or timeline for incorporating this content into established curricula is unknown (de Oliveira et al., 2011; Murray et al., 2022).
The Dominican Republic (DR), a country with 11 million residents, has 11 medical schools in 5 cities around the country, offering high-quality, robust and professional medical curricula to strengthen the formation of DR physicians with international competencies in medicine and public health. Although each medical school hosts distinguished faculty with national leadership who help support academic curricula to foster students’ learning and professionalism during their clinical and community training at diverse health centres, there is inconsistent research training across DR medical schools. To address this gap, the Dominican Medical Student Organization (Organización Dominicana de Estudiantes de Medicina, ODEM) was established in 2012, to fortify medical education with professional development opportunities, including acquiring skills on clinical and public health topics, research and public speaking, and team collaborations (https://ifmsard.com/).
One ODEM professional development activity took the form of collaborative writing sessions, which incorporated 3-hour introductory workshops and 3-month supervised practical sessions, for recent medical graduates and current medical students (Chapman and Veras-Estévez, 2023). As products of these sessions, medical trainees prepared letters to the editor for subsequent submission to medical journals. In this article, the authors used a qualitative design to examine medical trainees’ understanding of these collaborative writing sessions, as a mechanism to advance technical writing and critical analysis skills in health education and communication. Study findings can help guide health leaders in developing innovative health education training programmes that can instil the academic culture of writing and publishing on emerging global health topics.
Materials and methods
Setting and sample
Between December 2021 and January 2022, a qualitative study was conducted with a purposive sample of seven medical trainees (six women, one man), who attended one 3-hour introductory workshop and completed one 3-month supervised practical session in pairs, between 2017 and 2020. Inclusion criteria were medical trainees (⩾18 years of age) and active ODEM members who published their letters to the editor in medical journals. Only one medical student from each participating student group was included in this study.
Workshop and practicum design
Between 2017 and 2020, the first author (a general physician trained in the DR) and the medical trainee team (leaders of ODEM’s Standing Committee on Medical Education) organised and led five 3-hour publication workshops for ODEM members, with 15–50 trainees per session (Chapman, 2019, 2020). The workshop agenda included three elements: (1) an orientation towards the key skills required in the writing process, (2) a detailed review of the content of two letters to the editor published by the first author, and (3) an overview of the 3-month supervised practical session format. After completion of the introductory workshops, interested trainees registered to participate in the supervised practical sessions, which were organised and led by the first author. Student pairs were assigned one scientific article, and the first author provided weekly assignments and maintained email and video teleconference communications with teams (Chapman and Veras-Estévez, 2023). Of the 61 medical trainees (32 groups) who completed the supervised practicums, 47 trainees (26 groups) submitted their letters to the editor and 16 trainees (10 groups) of this total published their articles in 4 medical journals (The Clinical Teacher, MEDICC Review, European Sting and British Columbia Medical Journal).
Data collection
In this study, we used three frameworks to help guide our research design, approach and thematic analysis related to how medical trainees perceived the overall impact of this professional development opportunity, as part of their medical education. First, we used the socio-ecological model to examine the processes related to intrapersonal (individual characteristics), interpersonal (social networks), institutional (organisational rules), community (relationships among community organisations and networks) and public policy (laws and policies) levels (McLeroy et al., 1988). Second, we integrated the four-level Kirkpatrick Evaluation Model (reaction, learning, behaviour, results), where the first three levels helped guide the chronological training process from the introductory workshop (e.g. trainees perceive the added value of the training) to the supervised practical session (e.g. trainees acquire skills and identify knowledge gaps, trainees aim to refine their skills) as well as identify strengths and limitations of this academic training (Kirkpatrick and Kirkpatrick, 2006). Third, we utilised the Consolidated Criteria for Reporting Qualitative Studies (COREQ) to ensure the comprehensive review of the three domains (research team and reflexibility, study design, analysis and findings) specified in this checklist (Tong et al., 2007).
Using the scientific literature and consensus of medical students, we developed a 9-question demographic survey (e.g. year of academic studies, previous experiences in technical writing and critical analysis) as well as a semi-structured interview guide of 13 questions in Spanish, to permit an open discussion about technical writing and critical analysis for DR medical trainees. Question topics included (a) engagement in ODEM activities, (b) engagement in and perspectives on technical writing and critical analysis in health education, (c) perspectives related to participation in the introductory workshop and supervised practical session and (d) perspectives on the role of skills-based exercises in health education and communication. Interviews were conducted virtually in Spanish by the first author and audio recorded via a virtual platform. Field notes were prepared after each interview. Data saturation was reached when the authors observed no new prominent themes during data collection (Charmaz, 2014).
Data analysis
Interview data transcripts were transcribed and de-identified by the first author, and content was verified by the second author. Based on knowledge and experiences in medical education and research, the authors developed preliminary codes before data collection. They coded the data transcripts separately and then united to discuss each code and discrepancy to improve inter-observer reliability. They used thematic analysis to analyse coded notes and identify emerging themes with quotations (Ryan and Bernard, 2003; Sandelowski and Barroso, 2003). Participant feedback was elicited via three focus groups on a virtual platform in order to enhance reliability and validity during the analysis (Lincoln and Guba, 1985; Ryan and Bernard, 2003; Tong et al., 2007). A conceptual model was designed to depict the salient themes related to technical writing and critical analysis in health education.
Ethical aspects
This study was approved by the Institutional Review Board of the Hospital Regional Universitario José María Cabral y Báez (Santiago de los Caballeros, DR). Study participants provided verbal informed consent.
Results
Interviews ranged from 22 to 48 minutes (average of 37 minutes) in duration. The seven participants (six women, one man), between the ages of 23 and 26, included one fifth-year medical student, one sixth-year medical student and five general physicians completing their 1-year required medical internship (Pasantía Médica de Ley 146-67). They represented five DR medical schools (Universidad Organización y Métodos, O&M; Universidad Nacional Pedro Henríquez Ureña, UNPHU; Universidad Iberoamericana, UNIBE; Universidad Autónoma de Santo Domingo, UASD; Instituto Tecnológico de Santo Domingo, INTEC). Perceived enabling factors were described as: (1) detailed agenda, (2) direct mentorship, (3) effective teamwork, (4) personal investment and dedication and (5) future vision (Chapman and Veras-Estévez, 2023). Figure 1 shows the conceptual model of the perceived factors that positively influenced how medical trainees successfully prepared their letters to the editor.
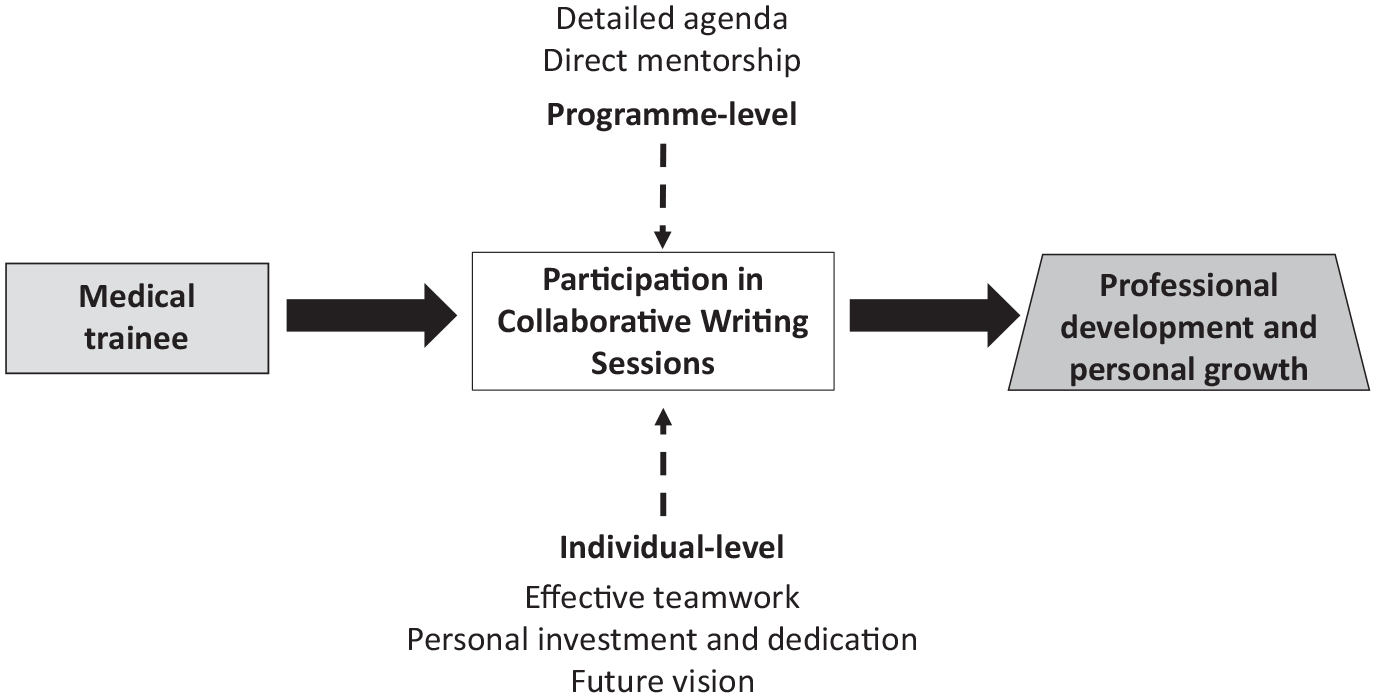
Conceptual model of the perceived enabling factors associated with medical trainees’ article preparation, as part of their participation in the collaborative writing series.
Detailed agenda
Participants enthusiastically shared their enjoyment of the clear weekly assignments, which offered a step-by-step guide to each task. One trainee commented, ‘Each assignment offers a “piggyback” on the previous assignment, and they are all weaved together in a logical manner’ (Participant 2, sixth-year medical student). Another trainee stated, ‘The agenda was very detailed. Even universities have never shared such a detailed agenda [for a course], including for my current thesis project’ (Participant 1, fifth-year medical student).
One participant expressed that the agenda was achievable for medical trainees with a busy schedule and limited technical writing skills in health education, but most importantly helped encourage them to complete tasks: The assignments are achievable, logical, direct, clear, and short, and I believe that the division of weekly assignments was what allowed us to prepare our article. These ‘baby steps’ made the assignments feasible for us because there were so many tasks to complete, many things that we had not done before . . . this is what allowed us to not be overwhelmed so that we had the strength and motivation to continue forward. (Participant 7, general physician)
Another trainee remarked on the time schedule for each assignment: ‘For me, the agenda was very well designed because you had sufficient time to complete each assignment’ (Participant 4, general physician). Another participant shared, The agenda offered flexibility, where you could get ahead and not fall behind. This is what I liked a lot. We were able to work at the pace of the agenda, and immediately when the practicum ended, we were able to complete the letter to the editor. We did not need any extra time. (Participant 6, general physician)
They also noted that each assignment was helpful with navigating their critical analysis on key health education topics. One trainee said, The agenda offered specific questions that helped you understand the next steps to prepare your article. You would respond to these specific questions as you were reading the article. (Participant 4, general physician)
Direct mentorship
Participants stated that the mentorship received throughout the practical session was distinct from that provided in other university courses. Specifically, they vocalised that they had not received such direct mentorship during their thesis or other course projects, since faculty frequently are assigned more than 20 students per academic course. Hence, trainees expressed feelings of achievement and satisfaction with their investment in the practical session. One trainee commented, ‘I feel that I have achieved my goals, and thanks to the workshop, I feel more confident about my technical writing’ (Participant 5, general physician). Another participant described hos she had left her comfort zone during the writing process: When the workshop facilitator gave us the opportunity to revise our articles [based on editorial feedback], we had to leave our comfort zone and think about how we wanted to revise the content. It is not the same situation when someone makes the respective edits for you as when you make the edits. (Participant 1, fifth-year medical student)
Trainees remarked that they appreciated the direct and rapid feedback for each assignment during the editorial process, which presented an opportunity to learn from the suggested revisions each week. One trainee said, The direct follow-up influenced everything, because it allowed us to understand what was written well and poorly and revise the content accordingly. I liked the follow-up because it was not just a required follow-up that told us what to do, but instead it provided suggestions that we could consider with what we wanted to emphasise, and we made the respective revisions. For me, the follow-up was the best part of the workshop because it taught me how to write from a scientific point of view (laughs). (Participant 6, general physician)
Finally, one trainee highlighted the value of mentorship during these skills-based exercises, to help articulate the key objective of the scholarly product: Unless you have mentorship, it will be difficult to understand how to complete the scientific writing tasks. It is like a black cloud, very intimidating, something that you cannot physically touch (laughs). I believe that it was about learning and discovering the world of publications and research. To have someone hold my hand and show me, well it is not as intimidating now, I am no longer afraid. It does not seem unreachable or strange. (Participant 7, general physician)
Effective teamwork
Most participants described the direct connections and synergies with group members that helped them finalise assignments in a timely manner. They expressed how they learned new concepts and skills about how to communicate their writing objective through the steep learning process. One trainee confided that her group had limited experiences in technical writing, especially in English: Neither of us had previous experience, so we were learning how to write in a language that is not our native language along the way. This was a little complicated at times, but [the process] helped us significantly. (Participant 3, general physician)
Six participants accredited the group dynamics as an essential element to the completion of weekly assignments. One trainee mentioned that her team displayed empathy, gained confidence and recognised the value in this academic collaboration: We both offered our ideas, without any fear, of what the other could not say. We also always worked thinking about how each of us could contribute our best so that the article could continue to improve beyond its current form. (Participant 3, general physician)
One participant commented on the timing of the synergistic interactions with her group member: ‘We worked well together because she knew my strengths and weaknesses, and I knew her strengths and weaknesses, and we complemented each other’ (Participant 1, fifth-year medical student).
As all participants acknowledged the challenging academic coursework and clinical rotations, they confirmed often alternating between in-person and virtual meetings to complete weekly assignments. One trainee believed that in-person meetings were beneficial: ‘The fact that we always saw each other in person [on campus] was very important because it helped us advance quickly . . .’ (Participant 6, general physician). Another participant shared, Many of our meetings were in person, where we met at each other’s house . . . Many times, according to our schedule, we also worked virtually and completed the same agenda. (Participant 5, general physician)
Several trainees highlighted the essential role of team communication in completing weekly assignments. One participant stated, Time was limited . . . We always communicated [about task delegation], like ‘If you want, you can complete the assignment this week, and I will complete the assignment next week’ . . . We talked frequently and we did not encounter any negative situation. (Participant 6, general physician)
Another trainee emphasised that successful team interactions were dependent on each trainee reviewing the practicum material prior to their group meeting: Honestly, we often completed each assignment individually in order to benefit from our group work. For example, I would read the article, then you would read the article . . . You are going to read it and note the important points that you understand . . . and I will read the article and take important notes that I understand, and then we will combine our notes together. (Participant 4, general physician)
Personal investment and dedication
Participants stressed how their commitment to the supervised practical sessions allowed them to acquire and refine valuable technical writing and critical analysis skills for their career development. As they reflected on their participation in the collaborative writing sessions, they acknowledged that their inexperience with technical writing on an array of health topics resulted in the steep learning curve. One trainee commented that this experience had opened her eyes to the writing process: The entire process was a significant challenge because it is something that we had never experienced, something intimidating, something that seemed unreachable. It was something that I had never even thought about before for my professional development. (Participant 7, general physician)
Another participant elaborated on the steep learning curve by noting that students were familiar with reading and summarising assignments, rather than critically analysing the content: At the beginning, it was very challenging because I was confronted with many skills that I did not have. No one ever talked to me about these [technical writing] skills, so it was not unlearning to learn, but rather learning from zero. For example, we are accustomed to preparing summaries and transcribing what you hear or read (laughs). (Participant 5, general physician)
Participants provided feedback on their individual learning process of tangible skills, including analytical techniques. One trainee emphasised the importance of flexibility during the writing process: It taught me to be more flexible and understand that the research process is not always linear, but that many times you start with an idea that you may not be able to follow, and you have to learn to reinvent and develop a new idea or modify the original one. (Participant 5, general physician)
Participants mentioned that these skills were not only complementary to their medical training but also served as life skills for their next career steps. One trainee stated, ‘I acquired skills [through this workshop] that my university did not offer, but I will need them in the workplace after graduation’ (Participant 1, medical student). Another participant attested to the personal challenge he had faced, but remarked that all medical students can learn these skills: At the beginning, it was challenging because we did not master the skills to complete a scientific publication. Moving forward, any medical student can prepare a publication after acquiring these skills. (Participant 4, general physician)
Future vision
All participants agreed that physicians are community leaders who should be knowledgeable on their clinical specialty, aware of community health needs, possess research skills and be talented with oral and written health education and communication skills. Participants stressed that physicians have a leadership role and should contribute their knowledge to advancing the scientific literature of their discipline. One trainee commented, I believe that technical writing shows how we communicate, whether we are in the Dominican Republic, China or the United States, and that we speak the same language. This is important, not only to understand what other people have contributed to the field, but also the possibility that you contribute something new, whether an approach [or trend] used in your country, whatever you want to share with the world. (Participant 2, sixth-year medical student)
Many participants concurred that learning about technical writing and critical analysis was essential for their future medical careers, vocalising that they would be less competitive without these skills. One trainee articulated, ‘If we do not develop technical writing as health professionals, we are a step behind the market or the workforce competition’ (Participant 6, general physician). Another participant said that medical trainees must possess a ‘crystal ball’, as a window into the future, so that they can identify and complete essential skills-based training for their professional journey: It is not a skill that you will keep hidden, but that you will use it for the future, your medical residency, your work . . . with more skills, you will have more opportunities. (Participant 1, fifth-year medical student)
Another trainee shared the value of critical analysis as an integral part of clinical responsibilities: Critical analysis represents our job . . . the baker makes bread, the professor teaches, the physician makes decisions. To make decisions, you not only have to have the knowledge, but you also have to employ critical analysis to be able to understand where the information comes from and how to use it. Critical analysis is what helps physicians avoid becoming automatic machines in the workplace. (Participant 7, general physician)
All participants felt that their skills acquired from these collaborative writing sessions would accompany them for their lifetime and that they could continue to build upon this skill set. Remarkably, three participants commented that they were considering pursuing doctoral-level training in health research. One trainee stated, Before the workshop, research and public health were things that did not excite me at all (laughs) . . . Our professors did not inspire me adequately so that I would be interested in exploring this area . . . I joined this workshop to see if it would interest me. It motivated me with another passion, and after this workshop, I could see that really enjoyed it and could combine it with clinical practice. (Participant 5, general physician)
However, all participants agreed that medical trainees experience challenges, including acquiring new concepts, the inability to apply these concepts during clinical rotations and erroneous perceptions related to publishing. One trainee said that she would not have been brave enough to prepare an article, if the workshop had not been offered as an ODEM professional opportunity. Another participant remarked that traditional medical education does not utilise journal club courses as a space to discuss research article formats (e.g. letter to the editor, perspective, original research) and designs (e.g. descriptive, analytical). Another trainee shared, ‘During our training, professors refer to the topic [research] as something very far off and difficult, as an unrealistic option for us’ (Participant 5, general physician). One participant expressed feeling empowered to become involved in research activities during the writing process: ‘I learned that it is not necessary to have a professional title to be able to publish as students’ (Participant 6, general physician).
Discussion
This is the first known study to explore the impact of a series of collaborative writing sessions on medical trainees in the DR. In a country with 11 medical schools, the Dominican Association of Faculties and Schools of Medicine (Asociación Dominicana de Facultades y Escuelas de Medicina, ADOFEM) deans and directors meet monthly to discuss ongoing priorities and activities to strengthen medical education, address challenges and pave the way for best practices. In a rapidly changing world where rigorous scientific inquiries and analyses are essential, developing timely and relevant continuing education courses can complement medical curricula and training of future physicians in health education and communication skills.
In this study, participants stressed the importance of the detailed workshop agenda, which facilitated the learning curve and the development of their letters to the editor. Detailed agendas served as valuable tools that offer tangible tasks and timelines to achieve training objectives (Fuller, 2013). Understanding trainees’ motivation for pursuing training programmes can help educators and mentors align workshop goals and content (Camacho Lizarraga, 2018). This workshop followed the learner-centred approach, defined as a technique to present new information (scientific writing) and build upon the trainee’s frame of knowledge (learner), and set a plan with clear objectives and tangible weekly assignments (Neilson, 2013).
Participants articulated that the direct mentorship with regular feedback using virtual communication technologies (e.g. email, Google documents, Skype, WhatsApp, Zoom) allowed them to strengthen their skills-based competencies in health education throughout the writing process. Their expressed self-confidence in their writing skills represents one of many potential benefits of mentee–mentor relationships (Chapman and Veras-Estévez, 2021; Nimmons et al., 2019). These findings align with one study that explored direct faculty interactions with student dyads and triads for a one-semester mentored undergraduate research practicum, where students exhibited higher levels of scholarly productivity, science self-efficacy and scientific identity (Joshi et al., 2019). Hence, guided research can serve as a significant step to integrating students and trainees into health research programmes and contributing to editorial boards, noting disparities (‘leaky pipeline metaphor’) among gender (Sarna et al., 2020) and low- to middle-income countries (Dotson, 2012; Kusurkar, 2022; Tutarel, 2004).
Participants also highlighted the valuable aspects of teamwork during the writing process, where student pairs coordinated in-person (preferred) and virtual meetings, worked on writing tasks and expressed reduced stress associated with the steep learning process of acquiring technical writing skills. Commitment to dyads was observed, in line with Tuckman’s four stages of development – forming (learning about each team member), storming (managing conflict), norming (open discussion among team members) and performing (achieving mutual trust and collective performance) (Tuckman and Jensen, 1977). Notably, two medical education reports underscore the need to increase physician engagement in teamwork training activities. First, the National Academies of Medicine shared five principles (shared goals, clear roles, mutual trust, effective communication, measurable processes and outcomes) that were needed for team-based health care (Mitchell et al., 2012). Second, the 2010 Flexner Report described the 21st-century physician as a team player with six needed skills (acquire and use knowledge, interdisciplinary research teams, collaborative, share accountability, interdisciplinary teams, coordination of patient-centred care), differing from the focus on the individual achiever in the 1910 Flexner Report (Morrison et al., 2010).
Although participants expressed their inexperience with scientific writing due to limitations in medical curricula, their dedicated efforts were evidence of their desire to acquire this important skill as future physicians. With unanticipated learning experiences, participants translated their reflections into clinical and public health practice (Mann et al., 2009). The act of reflection, defined as a metacognitive process to better self-understanding and lifelong learning, is now frequently integrated into training curricula (Mann et al., 2009; Sandars, 2009) and aligns with the framework of the Kolb learning model (experience, reflection, conceptualising, action) (Ménard and Ratnapalan, 2013). Incorporating reflective practices into writing workshops can also positively impact faculty–student relationships, support high-quality teaching practices and connect theoretical concepts to practice (Mann et al., 2009).
With emerging global health risks, future physicians should master clinical and public health competencies in the evidence-based literature and skills in technical writing and critical analysis (Chapman and Veras-Estévez, 2020). According to the World Health Organization, one urgent health challenge – improving public trust – can be addressed by health professionals’ talents in oral and written communication of pressing health concerns (World Health Organization, 2020). By refining these skills, medical trainees can identify knowledge and practice gaps, promote the One Health concept to advance scientific research and recommend relevant health promotion strategies to strengthen health system resilience.
Limitations
This study had a few limitations. First, although the study had a small sample size, saturation was met when no new emerging themes were observed (Charmaz, 2014). Second, as the first author was the ODEM founder and facilitator of the collaborative writing series, she cautiously stressed the importance of constructive critique of this academic intervention and noted that their collective feedback would be incorporated into future training. Third, interviews were conducted via a virtual platform during the COVID-19 pandemic, which may have hindered capturing all non-verbal cues during interviews. Finally, both authors analysed the data and recognised that alternate approaches to analyse and interpret qualitative data may exist (Miles et al., 2014).
Conclusion
Using a qualitative approach, this study offered an in-depth look at how medical trainees perceived their participation in collaborative writing sessions, as a benefit for their professional training and personal growth. The approach, which incorporated a feasible agenda, peer interactions and direct mentorship with timely feedback, was perceived as an effective way to reinforce technical writing and critical analysis skills in health education. These direct connections with the facilitator and team member during the collaborative writing sessions were fundamental to brainstorm, discuss and ultimately prepare innovative scientific articles for publication. By integrating this kind of academic training into health professional education, future health leaders will be better prepared to identify emerging One Health risks and lead and contribute to multidisciplinary health teams that develop novel health messaging and real-time solutions to mitigate risk to population health.
Footnotes
Acknowledgements
We thank study participants for their time and enthusiasm in sharing their experiences and perspectives related to these collaborative writing sessions. We commend the leadership of the Dominican Medical Student Organization (Organización Dominicana de Estudiantes de Medicina, ODEM) for their dedicated efforts to support key continuing education courses. We also appreciate the support of the deans and directors representing the Dominican Association of Faculties and Schools of Medicine (Asociación Dominicana de Facultades y Escuelas de Medicina, ADOFEM) and mentorship by O&M University (Universidad Organización y Métodos, O&M) Medical School and Two Oceans in Health leadership.
Declaration of conflicting interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship and/or publication of this article: The views expressed herein are those of the authors and do not reflect the official policy or position of the George Washington University or the Universidad Católica del Cibao. H.J.C. is the founding member of the Dominican Medical Student Organization (Organización Dominicana de Estudiantes de Medicina, ODEM), who continues to offer professional development seminars at no cost in support of medical education and training in the Dominican Republic.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
