Abstract
Objective:
In low tuberculosis (TB) incidence countries, linguistic and cultural dissonance between families experiencing infectious TB and TB health care providers is a barrier to effective communication and successful treatment. The purpose of this research was to explore infectious TB education and counselling from the perspective of patients and family members who are foreign-born.
Design/Setting:
One component of a multiphase, qualitative case study conducted in Calgary, a large city in western Canada.
Method:
Data were collected through semi-structured interviews, chart review and field notes and analysed thematically. Eight families were represented in the 6 patient and 13 family member participants who had recently experienced infectious TB.
Results:
Three themes were generated from the data: ‘learning about TB from many sources’, ‘reassurance and connection’ and ‘missing information’. Participants described learning about TB in different ways, feeling reassured once they knew more and sharing information with others. Overall, participants expressed satisfaction with education and counselling received. However, there were indications that communication problems had occurred. Participants asked questions during the interview, described areas of lingering confusion and shared TB-related behaviours incongruent with medical understanding. Knowledge gaps often increased isolation.
Conclusion:
Gaps in infectious TB education and counselling have negative impacts on patient and family member well-being. Education and counselling can be improved using multiple modes of communication, proactively addressing common misperceptions and reducing barriers to patient participation. Improvements could empower families to better manage their own experience and share accurate TB information with their communities.
Current global tuberculosis (TB) elimination plans highlight the need to improve support for patients and families affected by TB (United Nations General Assembly, 2018; World Health Organization, 2014). In low TB incidence countries such as Canada, most people who become sick with TB are born outside the country (Pareek et al., 2016); thus, effective supports must be tailored to meet the needs of people who are foreign-born. Being ill with TB can be physically and psychosocially devastating. Symptoms are often prolonged and incapacitating; treatment is demanding and spans 6–24 months. Though TB is curable, patients are known to experience lasting social exclusion, catastrophic financial losses and a diminished sense of self (Courtwright and Turner, 2010; Juniarti and Evans, 2011; Tanimura et al., 2014). For people who are foreign-born, the negative impacts of TB often exacerbate pre-existing vulnerabilities associated with migration (Bender et al., 2010; Craig et al., 2017; Lönnroth et al., 2009). Family members of those with TB are also negatively affected through secondary stigma (Juniarti and Evans, 2011), shared financial losses (Tanimura et al., 2014) and an increased risk of TB disease (Moran-Mendoza et al., 2010). Yet little is known about the TB experience of family members, particularly in low incidence countries.
TB health care providers (TB HCPs) are a key source of support for patients and family members managing infectious TB (Chalco et al., 2006; Gerrish et al., 2013). Not only do TB HCPs facilitate diagnosis and treatment, they also provide emotional support, health information and referrals for outside assistance. TB HCPs must communicate effectively with patients and family members to fulfil this important role. Unfortunately, multiple barriers exist which challenge effective communication between TB HCPs, patients and family members. In low TB incidence countries, linguistic dissonance and discordant expectations for health care interactions are two important obstacles (Greenhalgh et al., 2006; Yeheskel and Rawal, 2019). Linguistic dissonance, even when bridged by professional interpreters, impairs communication by increasing stress and risk for misinterpretation (Meuter et al., 2015). Discordant expectations between providers and patients often stem from implicit differences in belief about the origins of disease and corresponding appropriate treatments (Galanti, 2014). Patients who are foreign-born base their understandings of TB on the culture, health care and health promotion messages in their country of birth. TB HCPs, trained to think biomedically and prioritise public health, can fail to adequately assess and respond to patient and family information needs (McEwen, 2005).
Research has demonstrated that education and counselling on latent tuberculosis infection (LTBI) provided by TB HCPs often fails to meet patient and family members’ information needs (Clarke et al., 2021; McEwen, 2005). LTBI is a non-infectious condition central to TB epidemiology in low TB incidence countries. Most patients who develop active disease in low TB incidence countries become ill after the activation of an asymptomatic infection acquired pre-migration (Pareek et al., 2016). Family members of infectious patients are routinely offered LTBI assessment and treatment to prevent future disease (Rea and Rivest, 2014); however, research has shown that people who are foreign-born have limited awareness of LTBI (Gao et al., 2015; Wieland et al., 2012).
Though low levels of TB awareness in the foreign-born population have been well-documented (e.g. Tomás et al., 2013), there is an important gap in the literature regarding patient and family members’ experiences with TB education and counselling. We are not aware of other studies which have qualitatively explored the information and support needs of this population. The purpose of this research was to explore infectious TB education and counselling from the perspective of patients who are foreign-born and their family members.
Setting
The study was undertaken as part of a larger qualitative case study (Abma and Stake, 2014; Stake, 1995), organised according to social-ecological levels (McLeroy et al., 1988). The overall study was directed at improving the infectious TB experience of patients who are foreign-born and their family members through education and counselling in Calgary, Canada. Information on other components of the case study is available elsewhere (Bedingfield et al., 2021a, 2021b).
The Calgary TB Clinic is the sole provider of TB care for a population of approximately 1.4 million residing in the city and surrounding areas (Alberta Health Services, 2020). In 2019, 124 people were diagnosed with active TB, 93% of whom were born outside of Canada (Alberta Tuberculosis Program, 2020). Families experiencing advanced infectious TB (as indicated by smear positive sputum status) are often more deeply affected than other families experiencing TB because of patients’ advanced symptoms and increased infectiousness. In Calgary, care for such families is based on national and provincial guidelines (Menzies et al., 2014). Education and counselling for patients and family members experiencing infectious TB is provided through a series of telephone calls and appointments with physicians and registered nurses. A telephone and video language interpretation service is available at the clinic. Clinic staff are encouraged by organisational policy to use the service whenever they deem it necessary to mitigate linguistic dissonance or when requested by patients. Several patient education pamphlets are available in nine languages including English. Clinic staff do not routinely promote online learning about TB (Bedingfield et al., 2021b).
In most circumstances, patients are asked to isolate at home for their infectious period, which is often 3 weeks. Patients are seen at the clinic to initiate treatment within 2–3 days of diagnosis (Alberta Health Services, 2017). Patients are not asked to engage in extra cleaning or distance themselves from others in the home because such practices do not reduce transmission of this exclusively airborne disease (Long and Schwartzman, 2014). Care for other household members begins with a contact investigation interview, ideally completed within 3 days of treatment initiation (Calgary Tuberculosis Clinic, 2020). Household members, often family, are contacted, counselled and assessed according to their age, symptoms and health history. Care is expedited for children under 5, symptomatic contacts or immunocompromised contacts. Healthy adults should be assessed within 1 week of identification (Calgary Tuberculosis Clinic, 2020).
Methods
Eligibility, sampling and recruitment
Participants were recruited from Calgary TB Services. The first author (N.B.) determined eligibility by reviewing patients’ electronic files for the following criteria: 18 years of age or older, born outside of Canada, diagnosed with smear positive pulmonary TB in the preceding 3–9 months and had at least one close contact whom they identified as family. Family members were eligible to participate if they were 18 years of age or older and identified themselves or were identified as a family member of an eligible patient. To strive for maximum variation within the sample, participants of varying ages, family roles, ethnocultural backgrounds and family sizes were recruited. Staff from the Calgary TB Clinic introduced the study to potential participants. Staff forwarded contact information for those who indicated interest to N.B., who made contact by phone, provided further information and arranged interviews with agreeable participants. Research activities were approved by the University of Calgary/Alberta Health Services Conjoint Health Research Ethics Board (REB19-0366).
Data collection
Semi-structured interviews were the primary mode of data collection with supplementary data obtained from chart review and field notes. Patients were interviewed individually. If more than one family member from a household participated, family members were offered a choice between an individual or small-group interview. N.B., a Canadian-born nurse of European descent, and experienced cross-cultural qualitative researcher, conducted all interviews. Fifteen individual and two group interviews were conducted between November 2019 and April 2020. Initial interviews were conducted in-person, often at the participants’ home. Follow-up interviews were conducted with three participants by phone.
Certified, professional interpreters who had signed confidentiality agreements facilitated interviews for 10 participants with limited English proficiency. 1 N.B. began interviews by introducing the study and her own background, followed by the informed consent process which was conducted in the participant’s chosen language and documented on a written consent form. When introducing the study, N.B. emphasised the value of critical feedback to the research and procedures used to protect participant confidentiality in an attempt to minimise social desirability bias (Bergen and Labonté, 2020). The interview guide, revised iteratively during data collection, was directed at exploring participants’ experience of infectious TB and their perspective on the education and counselling. It was developed with input from the research team (i.e. listed co-authors) who collectively possess expertise in TB, qualitative methods and cross-cultural research. N.B. frequently asked probing and confirmatory questions during the interview to reduce misinterpretation related to linguistic and cultural dissonance.
Interviews were audio recorded and lasted between 15 and 80 minutes. Field notes containing descriptions of the interview process, non-verbal communication and debriefing with language interpreters (when present) were recorded after each interview. English portions of the recording were transcribed verbatim. After the interviews had been completed, N.B. worked with one-on-one with bilingual research assistants (i.e. volunteer university students or professional interpreters not involved in the original interview), who had also signed confidentiality agreements, to verify the conceptual validity of language interpretation. At each of the seven verification sessions, N.B. played non-English segments of the recording to the assistant who interpreted and together with N.B., compared this interpretation to the English transcript. This procedure was followed for most segments longer than three lines in each reviewed transcript. In all cases, it was determined that the original interpreter had adequately captured the meaning of the participants’ responses. In a few instances, details such as mode of transport, numbers of medication and specific cultural references which had been summarised during the live interpretation were added from the recording.
Analysis
The steps for inductive thematic analysis outlined by Braun and Clarke (2006) were followed. Following listening and familiarisation, individual data segments were labelled with descriptive codes. Codes were then reviewed and refined. After review, codes relevant to infectious TB education and counselling were gathered and progressively collated until three themes were produced. An audit trail of the analysis was maintained using NVivo software and paper records. Several meetings among the research team were held to review data analysis, nascent themes and the need for further data collection. N.B. also discussed data interpretation with language interpreters and bilingual research assistants to add cultural context and minimise misinterpretation (Tsai et al., 2004).
Results
Eight families were represented among the 6 patients and 13 family members who participated. Participants were born in Africa, East Asia and South Asia. Four participants had completed high school, 12 had post-secondary education and 3 had completed post-graduate studies. Table 1 contains further description.
Description of participants.
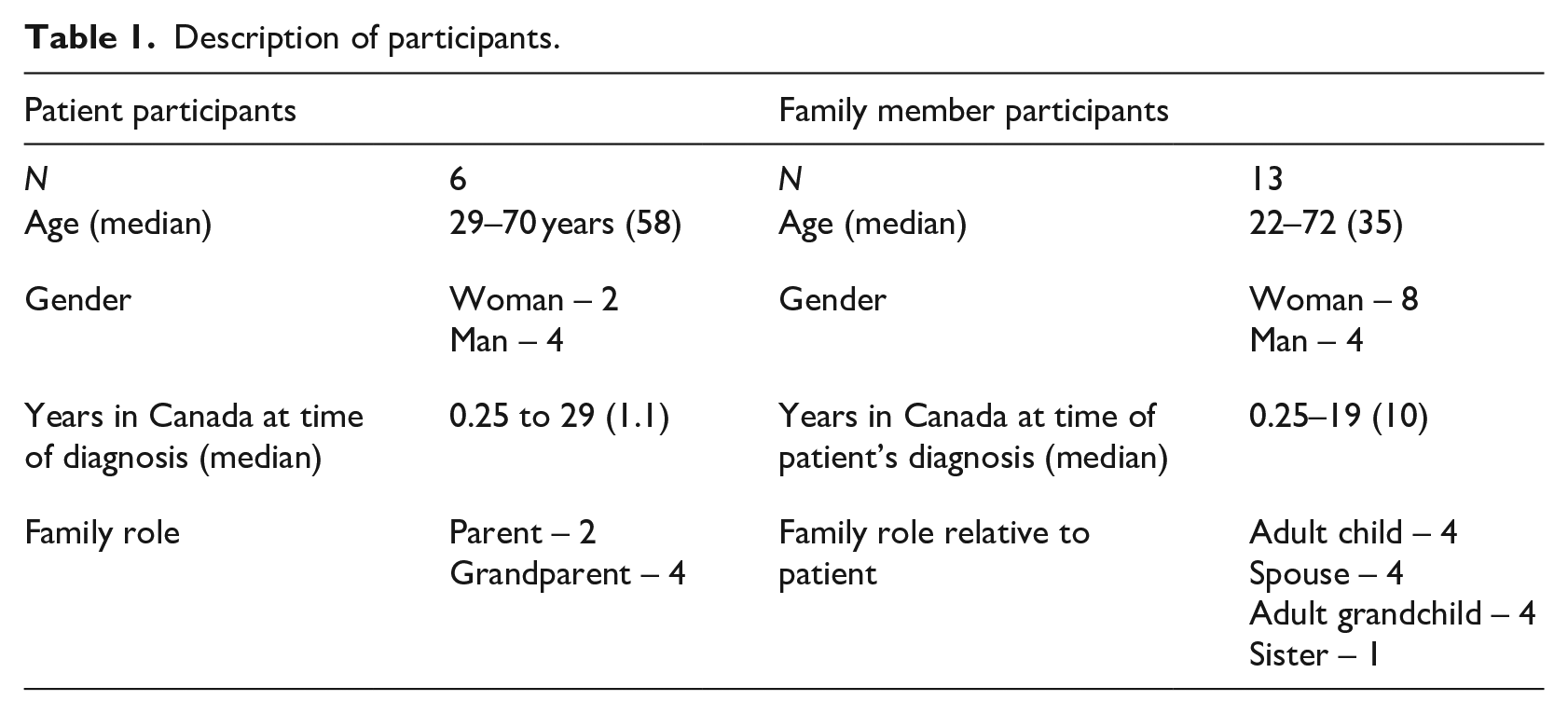
Three themes were generated from the data. The first, learning about TB from multiple sources, pertained to how participants learned about TB and the impact of this information. The second, reassurance and connection, comprised findings related to participants’ suggestions for improved education and counselling. Finally, missing information and incongruent accounts, pertained to TB questions and confusion which emerged during interviews. Participants whose quotes appear below are identified by pseudonyms; additional demographic information on these participants is presented in Table 2.
Description of quoted participants.
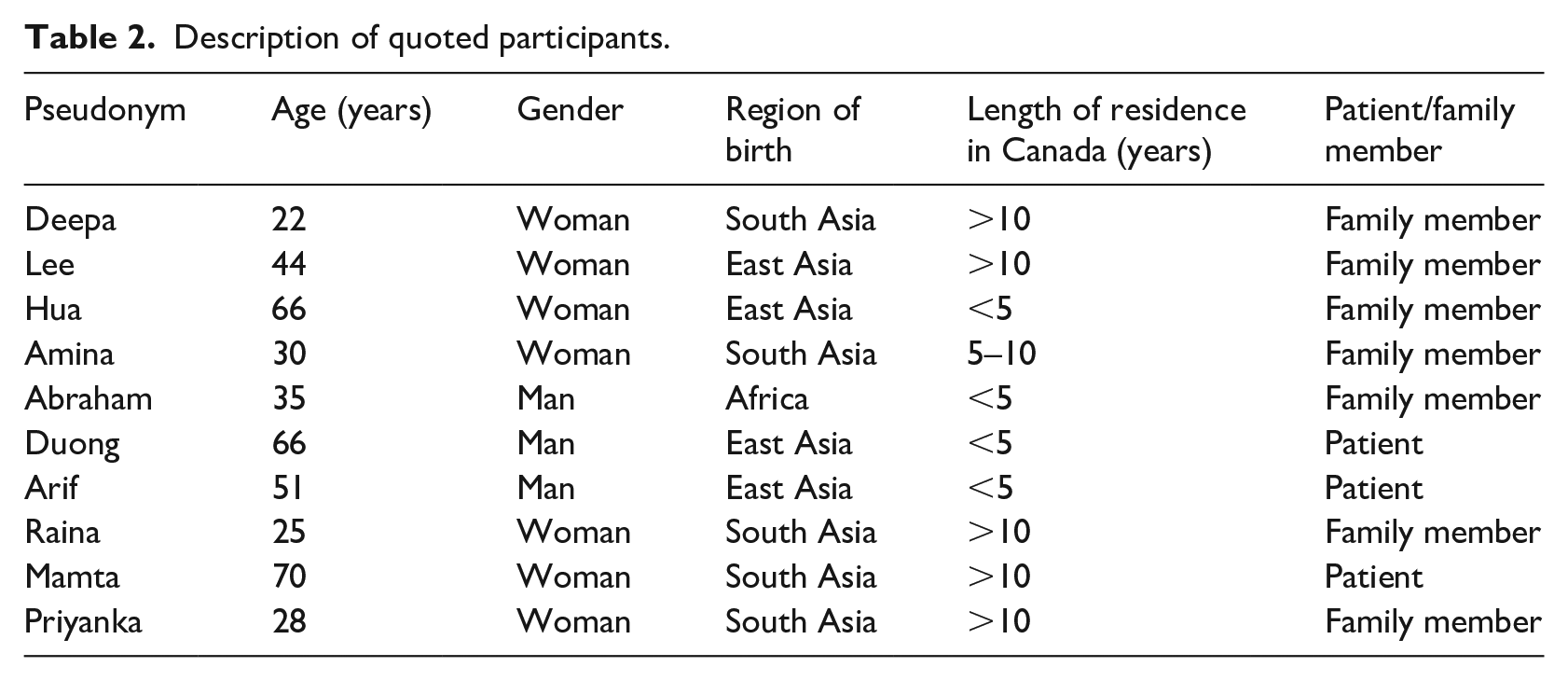
Learning about TB from multiple sources
Participants’ level of TB knowledge at the time of patients’ diagnosis varied greatly. Participants who knew little about TB were very afraid of an imminent death in the family; however, those more familiar with TB had less fear. Concerns about TB transmission were more common than concerns of fatality, particularly regarding transmission to young children in the home. After the patient’s diagnosis, participants received/obtained TB information from many sources and felt less afraid once they had learned more. The Internet, other family members and TB HCPs were important sources. Participants gained confidence in their understanding when they were able to interpret consistent messages from multiple sources. Deepa, a family member, described how knowledge reduced her fear for the patient’s well-being: I was told that it (TB) could not be cured, and then I found out about my grandma( ‘s diagnosis). . . . That was very scary. The first thought in my head was: ‘Is she going to live more?’ So when I did my (online) research, I spoke to my dad, and then I spoke to the doctors or nurse at the clinic, I was more relieved
In early stages, when fear and information needs were high, participants found online sources valuable because of their convenience. However, some found online sources frightening, untrustworthy or irrelevant. This was particularly true for participants with limited English who could only access online information in their first language. Participants also learned a great deal about TB from each other. Those who had experienced TB treatment were able to reassure other family members with stories of recovery. Family members also acted as conduits, passing on messages and information from TB HCPs to other family members. This occurred because some family members were able to communicate more closely with TB HCPs due to flexible daytime schedules and/or strong English proficiency.
Most participants indicated that talking with TB HCPs was valuable because information was relevant, and the source was trustworthy. Pamphlets distributed by TB HCPs were well-received, especially translated versions. Many participants shared their TB experience with others outside of the immediate family. Some participants described sharing newly acquired TB knowledge freely, whereas others were more selective in sharing. Few participants discussed TB stigma directly during the research interviews, but the impact of stigma could be inferred in participants’ willingness (or not) to share information about their TB experience.
Sharing TB information allowed some participants to help others. In one instance two sisters were sought out for peer support by a friend, also experiencing TB in her family. Lee, another family member, described how she photocopied and distributed a translated pamphlet: ‘Even my Dad’s friends, they were so scared too. But when they come to visit my Dad, I give the paper and they read it and after that they feel OK’.
Reassurance and connection
Satisfaction despite barriers
Overall, participants were satisfied with the education and counselling received from TB HCPs. Deepa spoke of the education her family received this way: ‘They were very supportive . . . they gave (my grandma) a lot of information . . . they answered our questions which was very good’. As seen in this (interpreted) quote from Hua, the high level of personal attention was appreciated: ‘Here, we feel friendly . . . we are feeling warm, because maybe in China it’s impossible to receive a call from the clinic’.
Participants mentioned several barriers to effective communication with TB HCP. Barriers included linguistic dissonance, lack of transport to get to appointments, difficulty missing work to attend appointments and rushed or non-responsive HCPs. Facilitators to effective communication included rapport development, home visitation and involvement of other family members. Although linguistic dissonance was often mentioned, not all participants felt it posed a communication problem which negatively impacted their care. These participants felt that mitigation strategies, which included managing with limited English, communicating via family, and use of professional interpreters were effective. Conversely, other participants felt apprehensive or frustrated by an impaired ability to communicate despite the use of interpreters.
Education and counselling priorities
Participants were asked to provide suggestions for TB HCPs when counselling other patients in similar situations. Participants overwhelmingly responded by saying that TB HCPs should provide reassurance by explaining that TB was curable for the patient and manageable for the family. These messages should be provided quickly to counter high levels of fear in the family, expected after TB diagnosis. Amina described how lack of reassurance could affect patient well-being: ‘Some people think it’s not curable and then they go into like stress, depression. If people can get more awareness (that) it is a curable disease’. Abraham, a father of two small children, described the importance of quickly communicating the care plan: even at the point where it was discovered that this is TB, I think it would . . . be better for the doctors to say . . . OK for the kids, for yourself, there’s the risk that this could have been passed. . . . OK these are the things that we’re going to do, were gonna test you . . . if you have it, immediately treatment is gonna commence. This communication (should be) made at this very stage.
Participants were asked about their preferences for health care interactions. Though there was a continuum of responses, several participants indicated that having an opportunity to provide input was not a priority for them. Most participants who did not prioritise participation went on to explain that they believed it was their role to adhere with the treatment plan formulated by experts. Duong conveyed his perspective through an interpreter as follows: In my opinion, I respect the doctor’s opinion very much. I don’t ask a lot of questions, I just describe my symptoms and my feelings to the doctor, then doctor is the person to make decision to about the treatment. So yeah, I follow up doctor’s opinion.
Missing information
Despite the high level of satisfaction expressed by participants regarding the education and counselling received, there was considerable evidence that communication problems had occurred. Participants often asked questions during research interviews, described areas of persistent confusion or gave accounts of their experience which were inconsistent with their medical records or current TB infection prevention practices. In some cases, participants were aware of the gaps in their TB knowledge and could articulate questions. In other cases, participants were not aware, and incongruent accounts provided evidence of ineffective education.
Questions regarding the genesis of TB were common. For many, the patient’s disease seemed to appear out of nowhere. Arif, who had been in Canada less than a year, explained his confusion through an interpreter: ‘He has no idea how he got tuberculosis because when he came here, he had x-rays . . .. it showed nothing, (his) system (was) clear’. Participants also had questions about treatment. A patient with mono-drug-resistant TB was unsure why his treatment had not followed the originally described trajectory for drug-susceptible disease. Raina described her confusion at being offered LTBI treatment: the medication that they give you for non-active TB . . . they say . . . it’s not necessary that you take (it), but its good to have it. So, I don’t know what (that) means . . . Why is it not a must thing?
Inconsistencies often pertained to personal or family diagnoses, and household infection prevention practices. One mother was unaware that her child, who thankfully did not become seriously ill, had been diagnosed with primary TB. Many participants described health behaviours undertaken to prevent TB transmission which went above and beyond clinic recommendations. These practices included distancing and masking in the home, separating the patient’s dining ware, and increased cleaning. Mamta described her motivation for household cleaning through an interpreter: ‘She would make sure everything is cleaned up because she was really worried that it would get onto her family members, onto her grandkids’. Having learned during the interview that fomites do not play a role in TB transmission, Priyanka expressed how learning this information earlier would have facilitated connection in her family: Yeah, see, like, we didn’t have knowledge about that, right? So . . . especially guests coming in, they don’t know. They just think like they can’t even sit on the sofa because the bacteria is embedded in there and they’re going to get it.
Whenever possible, N.B. attempted to address patient knowledge gaps by sharing TB information during the research interview; patients were encouraged to contact their TB HCP for information on diagnoses.
Discussion
Participants in the study felt reassured by learning about TB and were largely satisfied with their education and counselling experience. Despite overall satisfaction, participants were missing key pieces of information about TB, as demonstrated by statements made during the interviews. Based on these findings, we highlight what key pieces of information are missing and explore the impact of this missing information on patients and families. We also discuss the tension between participants’ missing information and overall satisfaction with education and counselling. Finally, we offer our recommendations for improvements rooted in patient and family member experiences.
Impact of missing information
Participants in this study had been engaged with TB care for several months. However, many were nevertheless missing information about family diagnoses, TB transmission and treatment. As a result, participants felt confused, experienced unnecessary isolation and did extra, ineffective work at an already stressful time. Many participants in this study described distancing themselves from other family members in an attempt to prevent TB transmission. Concern for others and fear of TB were at the heart of these health behaviours which may have increased intra-family stigma and weakened support for patients. Family support is key for patients experiencing active TB (Gerrish et al., 2013) and armed with a fuller understanding of TB transmission, families may have felt more connected to each other and been better able to manage the not-insignificant demands of advanced infectious TB. In other words, participants may have had a more negative experience than necessary because of gaps in education and counselling. Additional details on the inferred impacts of education and counselling gaps may be found in Table 3.
Impact of missing information on patient and family member experience.
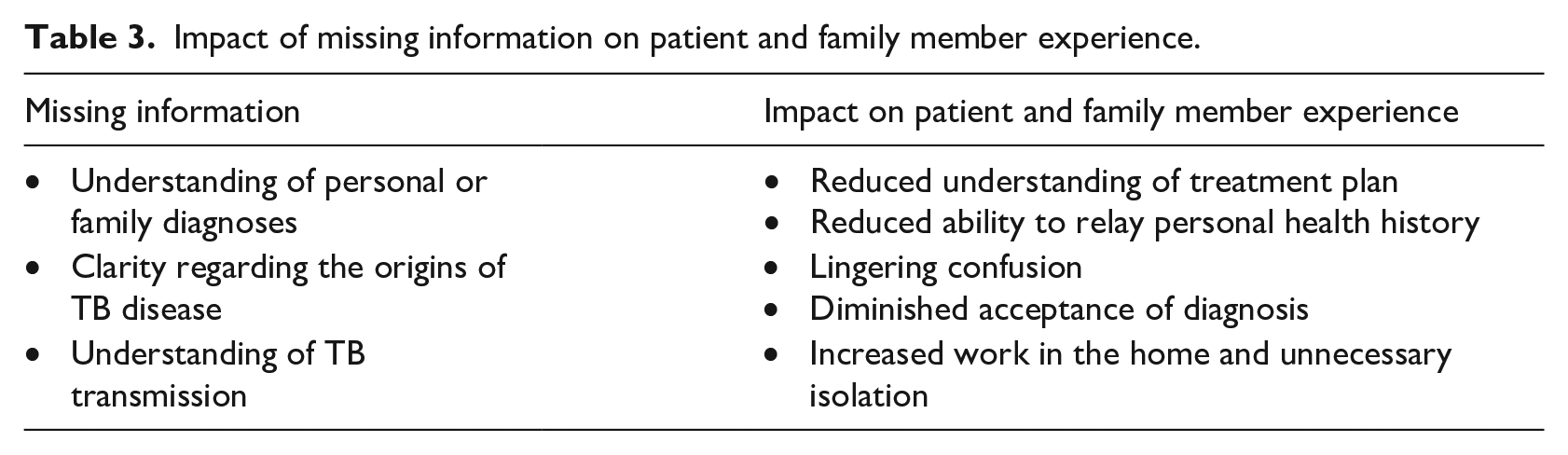
There are many potential reasons for participants missing key pieces of information; one may be that TB HCPs used a high proportion of instructions and a low proportion of explanations when providing education and counselling. Other researchers (e.g. Brumwell et al., 2018; McEwen, 2005; Moodley et al., 2020) have demonstrated that TB education and counselling can be imbalanced, containing a strong focus on biomedical instructions at the expense of more fulsome explanations which help patients and family members understand TB and manage the impacts on their everyday lives.
Researchers have also expressed concern that the excessive focus on adherence in TB has resulted in clinical communication which reinforces power inequities between patients and TB HCPs (Brumwell et al., 2018; Dick and Lombard, 1997; Dick et al., 1996; Gao et al., 2015). A similar communication pattern has been noted among HCPs working with linguistic and culturally diverse patients. In their systematic review, Schouten and Meeuwesen (2006) revealed a trend also documented by other researchers (e.g. Greenhalgh et al., 2006; Suurmond and Seeleman, 2006). Schouten and Meeuwesen found that HCPs made more directive statements and fewer informative, reassuring statements when working ‘ethnic minority patients’ (with and without language barriers) compared to white patients. HCPs’ time pressures, paternalistic attitudes as well as patient preferences have been offered as explanations for this communication style (Brumwell et al., 2018; Greenhalgh et al., 2006; Suurmond and Seeleman, 2006), but regardless of the cause, HCPs, particularly TB HCPs, require training and resources to incorporate more informative, empowering statements in their teaching.
Tensions in patient satisfaction
At the heart of these findings lies a tension between participants’ missing information about TB on one hand, and their overall satisfaction with education and counselling on the other. This seemingly contradictory finding is consistent with those in other research exploring patient satisfaction both inside and outside the field of TB. In their systematic review on patient satisfaction with TB care in low- and middle-income countries, Cazabon et al. (2020) found higher than expected rates of satisfaction, despite widespread evidence of poor-quality care. Similarly, Mukasa et al. (2015) found Australian patients of non-European descent were less likely to be dissatisfied with their TB care compared to Australian patients of European descent. From outside the field of TB, Fryer et al. (2013) found many patients with limited English proficiency did not express frustration with rehabilitation counselling rendered partially inaccessible by language barriers. Accustomed to managing with limited English, many participants felt that they had understood all the ‘major things’. The authors disagreed, arguing that participants had received only enough information to follow instructions and not enough to fully engage in recovery.
Patient satisfaction is fundamental to culturally safe, patient-centred care; however, it is highly influenced by patient expectations and can be difficult to measure and interpret (Kahan and Goodstadt, 1999). This is particularly true for patients who may have formed expectations based on pre-migration experiences with poorly resourced health care systems. TB programmes must measure and carefully balance patient satisfaction with other objective metrics of quality when evaluating progress towards equitable, acceptable care for people who are foreign-born.
Practice recommendations
In keeping with best practice in patient education, infectious TB education for patients and family members who are foreign-born should incorporate multiple modes of communication (Friedman et al., 2011). It was natural for participants in this study to learn about TB from many sources and TB HCPs should build upon this behaviour by intentionally providing information on multiple occasions through different modes of communication. This practice would reinforce challenging concepts and capitalise on the advantages of different approaches. For example, links to multilingual online information could be easily shared with families at the time of diagnosis, followed by individual and/or family counselling, and distribution of translated materials.
Regardless of the mode of communication, TB HCPs should proactively address common misperceptions. Topics which would have benefitted participants in this research included additional explanation about personal and family diagnoses, the TB latency cycle and TB transmission – key for dispelling stigma-informed myths about household infection prevention. This list is by no means comprehensive, and we agree with Brumwell et al. (2018) that consensus is needed on a list of essential education and counselling topics in TB. However, such a list is insufficient without efforts to strengthen patient and family member participation in education and counselling.
Unfortunately, patients who are foreign-born face considerable barriers to participation in Western health care interactions. Patients who are racialised may be reluctant to engage with HCPs due to previous negative experiences (Ben et al., 2017; Wiltshire et al., 2006). Patients with limited English proficiency are vulnerable to misinterpretation, and being cut short by time constraints (Greenhalgh et al., 2006). Some patients from non-Western cultures may simply not expect or desire a high level of participation (Lee and Lin, 2010; Mantwill and Schultz, 2018). Thus, it is essential that TB HCPs proactively attend to language barriers and take time to listen (Pérez-Stable and El-Toukhy, 2018).
Strengths and limitations
A strength of this research was that the topic was explored from the patient and family perspective which begins to fill a critical gap in the TB literature. Authenticity in the research process was strengthened when N.B. shared TB information with participants during research interviews. Despite efforts to minimise the limitations associated with cross-cultural research, linguistic and cultural dissonance may have dampened the depth of participant responses and the nuance of researcher interpretations. Perceived power dynamics and social desirability bias may also have influenced participants’ positive evaluation of TB care. Future research on this topic could incorporate conversation analysis to empirically assess the proportion of strategic and communicative messages used by TB HCPs interacting with people who are foreign-born.
Conclusion
It is critical that infectious TB education and counselling for patients and their family members who are foreign-born be oriented not simply towards medication adherence but towards empowering patients and families. Comprehensive, effective counselling is needed to reach this goal. Participants in this study felt reassured when they learned more about TB and also shared their knowledge with others. Engaging with the recommendations described here could not only support patient and family self-management but also increase the dissemination of accurate TB information. TB health promotion in linguistically and culturally diverse communities can be difficult (Gibson et al., 2005; Wieland et al., 2012) and patients and family members, able to share accurate knowledge and positive experiences, can play a powerful role in efforts to end TB in their communities.
Footnotes
Acknowledgements
We are grateful to the patients and family members who took the time to share their experiences. We would also like to thank staff and management at the Calgary Tuberculosis Clinic for their efforts to facilitate this research.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship and/or publication of this article: The Lung Association (Alberta & North West Territories Branch) Studentship Award and the Robert Cowie Fund for Tuberculosis and Non-Tuberculous Mycobacterial Research.
