Abstract
Introduction
First introduced in the United Kingdom in the 2000s (Vidovic et al., 2021), social prescribing (SP) is a person-centred practice that uses prescriptions to improve the health and well-being of people with complex socioeconomic or psychosocial needs (e.g., poverty, loneliness, social isolation). Social prescribing typically follows a three-step process involving: (1) a referral from a healthcare professional, often in primary care, (2) a consultation with a link worker to assess needs and cocreate a plan, and (3) a connection to local nonclinical resources in the community (e.g., community gardening, museums, social clubs) or statutory sector (e.g., behaviour and self-management programs; Polley et al., 2017). Recognized as a vital tool in achieving integration of health and nonhealth services (World Health Organization (WHO), 2022), SP is gaining global interest among researchers, policy makers, and practitioners for addressing chronic diseases and health inequalities (Htun et al., 2023), optimizing resources, and enhancing community support (Mulligan, Bhatti et al., 2020). However, little is known about the relevance of this practice for occupational therapists (OTs), and how it can tie in with proven interventions to support occupational participation.
Prescribing activities to improve well-being and self-care (Polley et al., 2017) is not new for OTs, who, back in World War I (1914–1918), used occupations to help people thrive and carry on with their lives (Thew et al., 2017). This common ground with the aims of SP underscores the relevance of the subject for occupational therapy and the importance of critically reviewing it to better situate its contribution. Rooted in health promotion, SP could support a professional transition away from dominant trends of individualization and biomedicalization of health, which conflict with the values and ethics of the profession (Whalley Hammell, 2020). By fostering a practice that meets the needs of individuals and communities in terms of preventing decline, reducing loneliness and adapting to situations of adversity, SP could thus extend the role of OTs beyond traditional interventions and support their engagement in more preventive and adaptive approaches, including with people who have no occupational or health dysfunctions. The growing interest in SP also creates momentum, inviting OTs to assume a transformative leadership role (Backman, 2022). Whether by engaging in the conversation or seizing opportunities for learning, research or the development of new clinical roles (Bradley & Scott, 2021), OTs could, through SP, help access, initiate and maintain occupational participation. Combined with lessons learned during and following the COVID-19 pandemic, such as the importance of maintaining social interactions, promoting health and strengthening social safety nets (WHO, 2021), SP could also serve as an intervention framework.
Despite these premises which support SP practices, the evidence needs to be critically synthesized. Although it shares affinities with foundations, values, and objectives of occupational therapy, and its characteristics (e.g., structured referral) could generate synergies with other innovative interventions, the role of OTs in SP practices and possible linkages with other occupational therapy interventions with a social scope remain largely unexplored. Positioned as a theoretical contribution, this paper aims to present SP, review supporting evidence, and describe it using Lifestyle Redesign's (LR) areas of compatibility and tension. To foster equitable opportunities for occupational participation, particularly in times of adversity and among people in situations of vulnerability, this article also aims to highlight the potential contribution of OTs in the implementation of these two practices. The structure of this paper draws on a selective synthesis of conceptual and empirical literature, informed by foundational publications (e.g., Polley et al., 2017) and inspired by conceptual reflections such as Backman's (2019) on occupational therapy's role in social interventions. The structure follows progression from conceptual and contextual foundations to empirical findings, critical analysis, and theoretical connections to occupational therapy.
Key Issues
Exploring Social Prescription
Although no official definition exists, the Alliance for Healthier Communities (AHC, 2024) describes SP as a person-centered approach combining social and medical models of health and well-being. Social prescribing is part of a formal trajectory that can be used by healthcare professionals to address the determinants of health. Notably, SP enables healthcare professionals to refer clients to navigators, that is, link workers who support the person in assessing needs and coconstructing a social prescription using community resources likely to improve their health and well-being (Polley et al., 2017). A cornerstone of SP is health equity which includes the reduction of barriers to occupational participation (AHC, 2024). By building on the individual's capabilities and facilitating access to health-promoting resources, SP places the individual at the center of care decisions, shifting paradigm from a medical to a salutogenic model (Howarth et al., 2020). While open to all, SP primarily targets people with mental health, social, or chronic conditions (Cartwright et al., 2022). Although older adults have diverse capacities, opportunities, and motivation to engage (Percival et al., 2022), SP could help address their unmet needs, particularly in terms of leisure and social participation (Levasseur et al., 2014). The main reasons for referral to SP services include managing physical and psychological symptoms, adapting to change, social isolation, loneliness, and work or financial issues (Cartwright et al., 2022). Although often described as innovative, SP's novelty lies mainly in developing structured access pathway integrating primary care and community resources (Mulligan, Bhatti et al., 2020). Specifically, these trajectories include three key components: (1) the healthcare professional (prescriber), (2) the navigator, and (3) community resources (Polley et al., 2017). Doctors, nurses, or pharmacists generally act as prescribers, referring their patients to navigators. Since they are in contact with people in situations of vulnerability, disadvantage, multimorbidity, social isolation, or loneliness, OTs could also act as prescribers. Skilled at navigating existing and emerging resources, navigators are generally nonprofessional caregivers attached to the healthcare system or a community organization (Polley et al., 2017). In Quebec, although their role does not follow a defined trajectory, the social geriatrics approach uses the navigator concept to identify current and potential problems (Guénette, 2023). Community workers supporting vulnerable older adults, an essential component of Quebec's action plan and policy, share many similarities with navigators, particularly in their role of referring individuals to community resources (Gouvernement du Québec, 2018). The intensity of support offered by navigators varies from providing information (signposting) to light, moderate or holistic support (Kimberlee, 2015). The more holistic the support, the more navigators maintain formal collaboration with prescribers (e.g., referrals, follow-ups), and provide ongoing support based on comprehensive need assessment (Kimberlee, 2015). In more intensive cases, navigators therefore meet with individuals to assess their needs, cocreate a personalized plan, facilitate access to meaningful community resources, and offer ongoing support to help them reach their goals (Drinkwater et al., 2019). Given their knowledge of resources and their cocreation skills, navigators are key players in SP. Yet, when social prescription falls short, for example, due to mismatches between the person and the activity, OTs can contribute by conducting in-depth occupational analysis and helping make occupational opportunities truly accessible and meaningful (Backman, 2019), particularly for those with complex needs or facing social exclusion. Beyond their support and referral, navigators can help develop new services based on gaps between customer needs and community resources (Polley et al., 2017). Community resources are activities offered locally, such as arts, physical activity, volunteering, learning, and connection with nature. Whether or not they involve interactions, activities to which clients are referred to are relational by nature, that is, linking people to each other and their environment (e.g., social, cultural, nature-oriented; Laliberte Rudman et al., 2022). By offering opportunities to meet, reflect, grow, and connect with others, nature and one's community (Howarth et al., 2020), these activities can provide an important source of motivation for occupation (Whalley Hammell, 2020) and help promote health and well-being (Bradley & Scott, 2021).
Social Prescription in Worldwide Health and Social Service Systems
In the United Kingdom, SP is being widely deployed, despite cuts in public spending (Polley et al., 2020), with targets of hiring over 1000 navigators to reach 900,000 people by 2023–24 (National Health Service (NHS), 2019). Inspired by these developments, SP initiatives are also underway in Canada (Mulligan, Hsiung et al., 2020), USA (Alderwick et al., 2018), Australia (Aggar et al., 2021), Spain (Calderón-Larrañaga & Braddick, 2021), Brazil (Younan et al., 2020), and Scandinavia (Jensen et al., 2016). In Canada, the Rx Community pilot study in Ontario was the first SP initiative implemented between 2018 and 2020 across 11 community health centers serving different populations (urban, rural, northern, English- and French-speaking; Mulligan, Hsiung et al., 2020). Building on this, the Canadian PaRx program (www.parkprescriptions.ca), launched in December 2020 and its Quebec version Precri-Nature prescribing “forest bathing” in the national parks across several provinces, also aim to formalize the act of prescribing nature in the same way as medication. More recently, the ClicSocial initiative (www.clicsocial.ca), developed through a partnership between a center for social justice and aging and a regional public health and social services center, is piloting an SP platform. Hosting a database of local community organizations, the platform enables healthcare and community workers to register as prescribers, generate social prescriptions, and connect individuals with appropriate resources. Although they do not all involve navigators, these initiatives are in line with the spirit of SP by targeting places of socialization and belonging that can help reverse the negative consequences of loneliness and social isolation (Howarth et al., 2020), which were exacerbated during and following the pandemic (Wister & Kadowaki, 2021).
Social Prescription in Time of Adversity
The COVID-19 pandemic affected lifestyles, with immediate and ongoing effects on physical and mental health. In Québec, where some of the most restrictive health measures were applied, surveys showed reduced physical activity and increased sedentariness (Camirand et al., 2023), in people aged 65 and older or those in situations of vulnerability. Similarly, both the prevalence (Kirkland et al., 2023) and level of loneliness (Lara et al., 2023) increased during COVID-19. As loneliness and social isolation are linked to disease and premature death (Holt-Lunstad et al., 2015) as well as reduced access and use of health services (Khattar et al., 2022), these issues are now public health concerns, spurring the development of effective interventions (Institut national de santé publique du Québec, 2020). By facilitating access to resources and programs (e.g., focused on exercise, nutrition, bereavement support) and promoting engagement in activities that foster social participation and new routines, SP supports social interactions and lifestyle change (Pollard et al., 2023) while helping mitigate exacerbated health adversities during and following the pandemic. However, SP faced significant challenges during the pandemic (Fixsen et al., 2021), including (1) care model shifting to simple signposting (light approach); (2) navigators’ focusing on counseling and advocacy for complex issues such as poverty, food insecurity, psychological distress, and suicide risk; and (3) new work conditions such as remote working, changing demands, lone work, and reduced resources (Westlake et al., 2022). Despite these challenges, several SP interventions have been adapted for remote delivery (e.g., online tablet groups; Vidovic et al., 2021), showing benefits notably for those with less complex health conditions, living in privileged areas or being in advantaged social positions. Therefore, a light approach to SP was sometimes insufficient for people experiencing hardship or digital illiteracy/inaccessibility during the lockdown (Morris et al., 2022). Without adequate training and support, these new tasks, technologies, and complexities may cause confusion, isolation, and burden, affecting link workers’ health and well-being, and posing risks for service users (Westlake et al., 2022). In this context, collaboration with healthcare professionals like OTs who have medical knowledge, communication skills, and expertise in activity adaptation is valued by link workers (Simpson et al., 2020) and helps protect service users, including in case of future pandemics.
Overall, the COVID-19 pandemic revealed both the importance and difficulty of SP. The crisis not only exposed flaws in health and social systems but also showed innovation was possible (Westlake et al., 2022). In a post-pandemic context, SP could contribute to healthier communities better equipped to recover from a crisis by promoting social bonding: a key factor in well-being and resilience (Vidovic et al., 2021). To avoid exclusion and inequalities, access to SP, link workers interactions, and the scope of community activities must be considered (Westlake et al., 2022).
Effects of SP
Documented from five systematic reviews enhanced and updated by expert work from National Academy of Social Prescribing (NASP), SP can have effects on individuals, communities, and healthcare systems (Table 1). To include an aging perspective, two other systematic reviews specific to SP with older adults were considered (Grover et al., 2023; Percival et al., 2022).
Documents Used to Summarize the Effects of Social Prescription (n = 10).
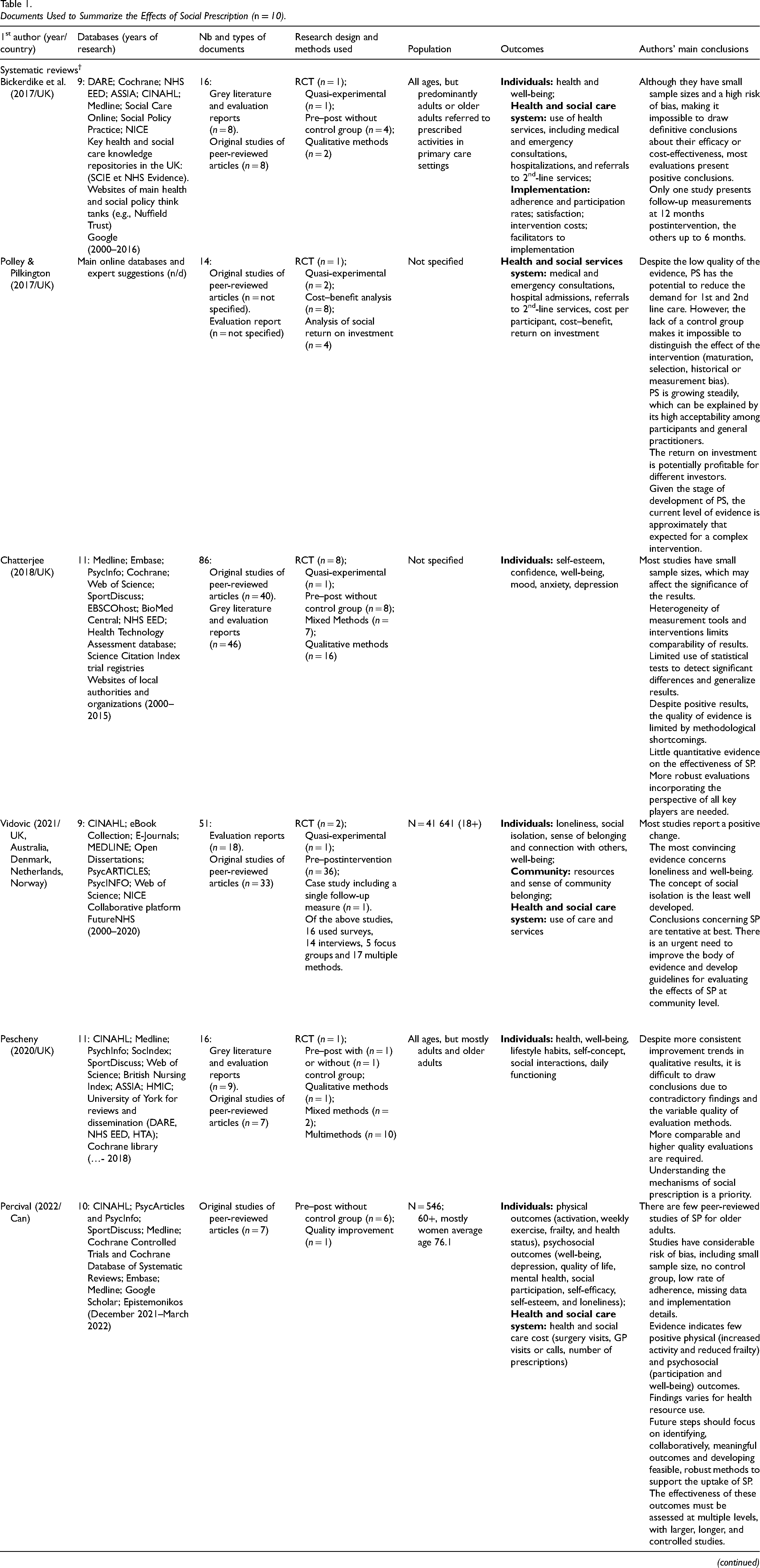
Studies include overlapping articles.
ASSIA = Applied Social Sciences Index & Abstracts; Can = Canada; CINAHL = The Cumulative Index to Nursing and Allied Health Literature; DARE = Database of Abstracts of Reviews of Effects; HMIC = Health Management Information Consortium; N/A = not applicable; NASP = National Academy for Social Prescribing; NHS EED = National Health System Economic Evaluation Database; NICE = National Institute for Health and Care Excellence; n/d = no date; RCT = randomized controlled trial; SP = social prescribing.
Effects on Individuals
Results indicate positive effects on health, well-being, and social interactions (Table 1), including physical health, lifestyle habits, self-esteem, communication skills, motivation, and meaning in life. Reduction in anxiety and depressive symptoms, isolation and loneliness, and new knowledge and interests is also reported (Grover et al., 2023; Polley, Chatterjee, Asthana, Cartwright et al., 2022). Studies using standardized tools, all supported improved health or well-being (Bickerdike et al., 2017). However, quantifying improvements was difficult, in part due to lack of control groups (Bickerdike et al., 2017).
In their recent work, Polley, Chatterjee, Asthana, Cartwright, et al. (2022)) and Vidovic et al. (2021) reported that the majority of studies included measures of quality of life and well-being (69/83; 83.1%), almost half concerned social ties (e.g., loneliness; 39/83; 46.7%), and only a few (4/32; 12.5%) focused on physical (e.g., frailty) and mental health. Specifically, 44 studies (44/69; 60.8%) reported improvements in quality of life and well-being. According to Polley, Chatterjee, Asthana, Cartwright, et al. (2022), nine studies (9/27; 33.3%) reported positive trends, and a further two (2/27; 7.4%) found mixed effects (Table 1). Of the seven reporting the longest follow-up measures (4–10 months), one indicated a trend toward improved well-being at 3 and 6 months postintervention but a decline in quality of life at these same measures, and two others reported improvements in well-being immediately following the program as well as at 2, 3, and 6 months postintervention (Polley, Chatterjee, Asthana, Bertotti et al., 2022). For older adults, Percival et al. (2022) found similar results indicating some positive effects on well-being with 4/5 (80.0%) studies reporting significant improvements.
Regarding loneliness and social interaction, the latest evidence (Polley, Chatterjee, Asthana, Cartwright et al., 2022; Vidovic et al., 2021) reports improvements in more than a third of studies (14/39; 35.9%) and improving trends in 7 others (7/16; 43.8%). According to Polley, Chatterjee, Asthana, Cartwright, et al. (2022), two studies (2/16; 12.5%) observed mixed results, and another (6.3%) documented an increase in group membership at 4 months postintervention, followed by a decline at 6 and 9 months. Reviews on older adults, both qualitative and quantitative, indicates improvements for loneliness and social isolation (Grover et al., 2023; Percival et al., 2022), including building social connection, establishing new friendships, and developing a sense of community (Grover et al., 2023).
Findings on physical and mental health are mixed. Of six recent studies, five found positive changes in frailty and physical activity (Percival et al., 2022; Polley, Chatterjee, Asthana, Cartwright et al., 2022), and one in mental health (Polley, Chatterjee, Asthana, Cartwright et al., 2022). Older adults also reported better management of health, including depressive or anxiety symptoms (Grover et al., 2023).
Effects on Health and Social Services System
Effects on health service use are mixed: one study found a 28% reduction in the average number of medical consultations and a 24% reduction in emergency department visits reported compared to the control group (Polley & Pilkington, 2017), while other studies found no change (Kimberlee, 2016). These reductions, likely attributable to SP, were greater in younger people and high-service users (Kimberlee et al., 2022). The only randomized clinical trial (Grant et al., 2000) found similar consultation rates, fewer specialist referrals and more drug prescriptions in the intervention group. Similarly, Percival et al. (2022) reported mixed results in three studies of older adults, including no change in GP visits and calls, and a nonsignificant decrease in prescriptions. Although SP may reduce service demand, further studies are needed to confirm system-level benefits (Table 1).
Cost-Effectiveness
Despite some assessments of cost-effectiveness, cost–benefit, and return on investment (Table 1), SP initiatives rarely undergo economic analysis. Their uniqueness (Kimberlee, 2015) and monetization of different variables (Kimberlee, 2016) hinder comparison. For holistic SP initiatives, health worker costs per client ranged from C$365 to C$1362 (Kimberlee, 2015). The only RCT reported higher costs of care for the intervention group but did not calculate the cost–benefit ratio (Grant et al., 2000). Returns on investment ranged from $1.96 to $9.13 per dollar invested (Kimberlee et al., 2022; Percival et al., 2022) benefiting users, communities and health and social services system as early as year 1 (Kimberlee et al., 2022). In year 2, one program reported sufficient added value to cover intervention cost (Dayson et al., 2016). As SP effects may take time, overall savings are expected to grow in later years (Kimberlee et al., 2022). One analysis found cost per quality-adjusted life year at $3206, well below the National Institute for Health and Care Excellence threshold of $32,666, indicating cost-effectiveness (Kimberlee et al., 2022). Sustainability of these results over time is unknown or to what extent changes in health-related quality of life are attributable to SP. Although SP may reduce primary care pressure and generate savings (NASP, 2021), economic evidence for SP remains limited and further studies are needed.
Criticism of Social Prescription
Despite significant political (NHS, 2019) and professional (Royal College of Occupational Therapists & Royal College of Psychiatrists, 2021) support, SP faces criticized. First, its paternalistic connotations and complex terminology (e.g., “navigators”) may deter engagement (Brown et al., 2021). Because prescription stems from a medical model, it may also be viewed as authoritarian, imposing ways of being (Bradley & Scott, 2021). Aware of this connotation, some practitioners view “prescription” as an “evocation”: an opportunity to discuss various treatment options, especially to develop healthy lifestyles and connect with others, culture and nature (Fixsen & Polley, 2020). While found useful for some clients, lighter-touch approaches have limited capacity to improve conditions or health of those living in the most disadvantaged circumstances, and thus to mitigate the social determinants of health or reduce inequalities (Pollard et al., 2023).
Although often presented as a solution to complex problems, SP must not obscure the reality of social and health inequalities (Calderón-Larrañaga et al., 2022) or create an appearance of action when more complex or costly solutions should be preferred. For instance, areas with limited community resources may face challenges in supporting SP initiatives, potentially exacerbating existing inequities (Brown et al., 2021). To ensure that identified needs do not go unmet due to insufficient services, investment in the community sector is necessary (Alderwick et al., 2018). Some scholars also highlight that SP may fail to reach the most marginalized, perpetuating their isolation (Cartwright et al., 2022). As funding usually covers referrals and not activities, financial constraints may restrict access and sustainability of engagement beyond the short term of SP programs (Pescheny et al., 2018). Beyond equity and inclusion, SP must better address older adults’ needs facing structural or social disadvantages (Cousins, 2023) by tailoring programs to values and priorities such as autonomy, connectedness, trust, and personalization (Yu et al., 2024).
The evidence in support of SP is, in turn, considered insufficient (Calderón-Larrañaga et al., 2022), due mainly to methodological weaknesses limiting the establishment of a causal link (Husk et al., 2019) as well as research methods not adapted to the evaluation of complex interventions (Calderón-Larrañaga & Braddick, 2021) or not allowing comparison with a control group. Along with small sample, high attrition and imprecise selection criteria (Bickerdike et al., 2017), studies use numerous variables, sometimes poorly defined and often chosen for political concerns such as individual effects and cost-effectiveness (Polley et al., 2020). The multiplicity of outcomes also raises questions about their relevance and usefulness (Husk et al., 2019). Long-term follow-up measurements are rarely carried out (Table 1), making it impossible to determine whether positive effects are maintained over time. Finally, heterogeneity in SP practices may undermine quality of services by promoting fragmented (e.g., need-specific), transactional (guidance vs. support) or inequitable interventions (Calderón-Larrañaga et al., 2021).
Tensions and Opportunities Between Social Prescription and LR
The SP and LR share several affinities, including their preventive aims and holistic approach. Lifestyle Redesign is an occupational therapy intervention framework that promotes awareness of the relationship between everyday activities and health. It guides individuals in analyzing and restructuring their daily occupations, habits, and routines to enhance physical, mental, and social well-being. Lifestyle Redesign is delivered by occupational therapists through individualized and group sessions using techniques such as occupational self-analysis, narrative reasoning, didactic education, and collaborative problem-solving. The framework emphasizes client autonomy and the therapeutic use of occupation to develop sustainable, health-promoting performance patterns. Applicable to both prevention and chronic condition management, LR is adaptable across diverse populations, settings, and modes of delivery, including telehealth (Pyatak et al., 2022). As part of a biopsychosocial model, SP aligns with occupational therapy and LR. For OTs, these two approaches are client-centered and promote occupational participation: key elements of their professional ethos. Occupational therapists are therefore key players in LR and natural partners in SP approaches, as both share a preventive vision, promote healthy lifestyles, and fill gaps in illness-focused systems. By addressing social determinants of health, these approaches promote a broader vision of healthcare services.
However, the two approaches differ in terms of their integration into the healthcare system, their referral trajectory and their target clientele. Unlike SP, a key element of UK health policy, LR's influence on US health policy and practice, is considered suboptimal (Clark et al., 2013), mainly because of the lack of implementation plans. In Quebec, despite support from the Professional Order of Occupational Therapists (Ordre des ergothérapeutes du Québec, 2017) and local projects (Lagueux et al., 2021; Levasseur et al., 2019), LR is absent from recent health recommendations and action plans (Ministry of Health and Social Services, 2021). Inspired by the United Kingdom, integrating LR into Canadian health policies, particularly for preventing deconditioning, could propel more preventive and community-based occupational therapy practices.
In its current form, LR lack a structured referral trajectory and navigators, key differences from SP. Indeed, while the SP referral path is established (Mulligan, Bhatti et al., 2020), that of LR has yet to be defined in a service use model. Although LR could include self-referral, medical prescription, or intersectoral entry points, ensuring equitable and nondiscriminatory access to the program is essential (Lévesque et al., 2025).
Unlike SP, which targets a sicker or socially vulnerable clientele (Cartwright et al., 2022), LR adopts a universal vision that is aimed at everyone. Although developed for people with a high probability of having health problems, LR also reaches independent older adults who are unknown from the health and social services system, but who are not immune to losses associated with aging. Compared with SP, LR emphasizes intervening upstream of major health problems (Clark et al., 2021; Pyatak et al., 2022), a important aspect in planning services for aging societies facing overlapping crises such as climate (WHO, 2023), housing (Minister of Housing Infrastructure and Communities, 2024), ageism (Lagace, 2013), and loneliness (Office of the U.S. Surgeon General, 2023).
In contrast with SP, sometimes limited to guidance and advice to meet specific needs or to a narrow range of activities (e.g., physical), LR is a holistic approach offering personalized support based on strengths, self-analysis of occupations, discovery of meaning and action (Pyatak et al., 2022). In addition to being well-suited to address the needs and priorities of older adults, including those being structurally or socially marginalized, the approach's emphasis on helping participants find purpose and to be included is a key aspect for those engaging in SP.
Finally, and as synthesized by Pyatak et al. (2022), LR is a professionally led intervention optimizing occupations, habits, and routines to promote health and well-being. It may therefore address complex needs (e.g., life transitions), reduce barriers to participation (e.g., community mobility; Simpson et al., 2020), and support behaviour change through theories and techniques (e.g., goal setting and follow-up; Percival et al., 2022), all shortcomings noted in SP studies. Occupational therapists have the medical knowledge to adapt to changing conditions, provide appropriate support for participation, adjust to the person's literacy, and maintain a therapeutic relationship. By analyzing the interactions between the person, occupation, and environment, OTs apply a broad socioecological vision to identify or offer integrative, context-specific solutions. This creates opportunities for OTs and link workers to collaborate and advance SP.
Possible Linkages Between SP and LR
Because of their many affinities, SP and LR offer several possible linkages, three of which are presented below: (1) LR as an intervention included in the SP offer, (2) a navigator dedicated to LR, and (3) the occupational therapist as navigator.
Lifestyle Redesign as an Intervention Offering Within Social Prescription
As an occupational therapy intervention offering opportunities to explore new activities in group or individual settings, along with practical, motivational, and personalized support, LR could be integrated into the SP offer. In the postpandemic context, and since it acts on the development of coping strategies (e.g., resilience) and social network, LR could help mitigate psychological stressors and social consequences associated with COVID-19 (Johnson, 2022). Including LR in a group format within the SP offer could also help older adults’ better cope with depressive symptoms (Dingle et al., 2021).
Dedicated Navigator to LR
A dedicated navigator for LR, supported by a consulting occupational therapist, could better reach older adults at risk of vulnerability, deconditioning, or low well-being and strengthen their connection with community resources. With strong local knowledge, the navigator would help direct participants toward resources that align with their needs, interests, and abilities, based on the occupational therapist's initial assessment. Occupational therapist would facilitate the navigator's work by first identifying the person's characteristics, meaningful activities, and levers and barriers to participation. During individual meetings, the navigator could support change by helping identify meaningful goals for the older adult, maintaining their motivation toward achievement, and developing a Personal Engagement Plan (PEP). Through community ties, a dedicated navigator could facilitate outings, partner conferences, intervention groups and civic actions. If barriers to action arise, the navigator could also help older adults take the first steps. At the end of the program, the navigator could follow up with the prescriber, facilitate transitions to other resources, and support those who wish to continue meeting informally.
Occupational Therapists as Navigators
With their expertise in coaching, engagement, coordination and advocacy, as well as their in-depth knowledge of person–occupation–environment interaction, OTs are well-suited for SP interventions, aligning with their expected role in prevention and health promotion(ACOTRO et al., 2021). As healthcare evolve, OTs are increasingly called to focus on health promotion. They can also act as navigators, supporting people needing professional intervention. Social prescribing then becomes part of the therapeutic process, positioning OTs as intermediaries between public health services and the community. Elements from LR, such as PEPs, could enhance individualized recommendations and facilitate referral to other community services and resources. As described in the Well Elderly model of Lifestyle Redesign® (Clark et al., 2015), PEPs remain a recognized component of this original conceptualization, although they may not be included in more recent implementations (Pyatak et al., 2022). As this practice takes time, its relevance and legitimacy must be justify to managers, notably through accountability statistics. Despite their role is often poorly understood and underutilized in the community (Bradley & Scott, 2021), OTs’ integration into family medicine groups and community organizations would be an avenue to explore as part of this emerging practice (Thew et al., 2017). More specifically, emerging practices focused on SP and LR could help strengthen community connections while supporting evidence-based practices that can reach populations at risk for chronic disease, disability, and isolation.
Implications
By addressing social determinants of health preventively, SP complements occupational therapy interventions, extends its scope and support adaptation, especially in times of adversity or for people experiencing situations of vulnerability. Despite emerging evidence, notably for older adults (Grover et al., 2023; Percival et al., 2022), SP is not a universal solution nor always advantageous. Further studies are needed to improve the quality of the evidence and better understand how, why, and at what cost SP works across populations and contexts. Research approaches that are better adapted to assessing complexity, such as realist review and evaluation and pragmatic trial design, are therefore encouraged. Finally, fighting isolation and social and health inequalities requires multilevel approaches, and mobilizing health and social systems as well as government to develop preventive structures enabling individuals and communities to thrive while improving their health and well-being. By drawing on their expertise to support occupational participation, strengthen engagement beyond simple referrals, and enhance alignment between individuals, occupations, and community resources, OTs can help implement SP in a way that is more equitable and meaningful.
Key messages
Although not a universal solution, SP may offer a better way to address the social determinants of health.
SP and Lifestyle Redesign® are complementary and aligned with the profession's priorities regarding occupational justice and participation.
To better address situations of adversity, including loneliness and social isolation, SP should be part of occupational therapists’ strategic considerations.
Footnotes
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Canadian Institutes of Health Research, Fonds de Recherche du Québec - Santé, Molson Foundation, (grant number 148466).
