Abstract
Introduction
Social participation is essential for health, well-being, and quality of life (Law et al., 1998; Levasseur et al., 2022). For individuals living with dementia, opportunities for social participation are, however, often disrupted, leading to social isolation and loneliness. Prevailing narratives surrounding dementia often emphasize deficits and portray individuals as unfit to perform in social situations, which contributes to their exclusion (Birt et al., 2020; Kotwal et al., 2024). The cognitive and behavioral changes associated with this diagnosis, combined with social environments that fail to support inclusion, further contribute to restricted social participation (Craig, 2017). Lonely and socially isolated individuals face a range of health-related consequences, including memory decline and increased anxiety (Azevedo et al., 2021), decreased overall well-being (Kotwal et al., 2024), a higher risk of mortality, and greater healthcare utilization, such as more frequent visits to the emergency department (Bartley et al., 2024). Social isolation and loneliness can also be a shared experience between persons living with dementia and partners who would also benefit from tailored interventions (Kotwal et al., 2024).
To promote participation in society and engagement in meaningful activities to individuals living with dementia, it is important to intervene accordingly (Górska et al., 2021; Smith et al., 2022). Traditionally, these interventions have focused on middle or later stages of this disease. Increasing attention is, however, being given to earlier interventions, such as educational approaches that promote health and support individuals in adapting to and managing their diagnosis (Testad et al., 2020; Kajander et al., 2024). Early interventions may reduce stress and need for health services (King et al., 2024), which can occur due to uncertainties about the diagnosis and a lack of information regarding what to expect. Considering that, by 2030, approximately one million Canadians will be living with Alzheimer's disease or other forms of dementia, a number that is expected to double by 2050 (Alzheimer's Society Canada, 2022), it is therefore crucial to develop effective interventions that foster participation in everyday activities for this population to support individuals as soon as they receive the diagnosis.
Journeying through Dementia (JtD), an occupation-based community program developed for older adults living with early-onset dementia, is an example of an intervention that supports meaningful participation (Mountain & Craig, 2012). The focus on the preventive role of occupation as an intervention resembles the Lifestyle Redesign® program, one of the first evidence-based occupational therapy programs delivered in the community for older adults (Clark, 2015), which supports continued participation in meaningful activities.
JtD is grounded in occupational science and is based on the belief that “it is through one's immersion in the world of occupations that new discoveries about one's potential and a forward movement of one's life takes place” (Jackson et al., 1998, p. 329). This program was developed in the United Kingdom in partnership with individuals diagnosed with early-onset dementia and their care partners (Mountain & Craig, 2012). Based on participants’ views on how quality of life could be maintained after a dementia diagnosis, five key themes formed the foundation of the program: (a) Enhancing daily living, (b) Adapting everyday environments, (c) Maximizing psychological well-being, (d) Optimizing physical well-being, and (e) Supporting families and carers as equal partners. Each theme consists of several modules, used by occupational therapists during group sessions (e.g., enabling environments, technology, memory maintenance). Participants collaborated in shaping the program's delivery mode, which includes 12 group sessions, individual meetings with an occupational therapist, and group outings. Participants emphasized that it was important for the program to focus on practical strategies and hands-on activities that they could apply in their everyday lives rather than following a more educational approach.
The JtD aligns with the World Health Organization (WHO, 2021) initiative aimed at improving communities’ understanding of dementia and creating dementia-inclusive societies, that is, “where people with dementia can live meaningfully, safely and with dignity” (WHO, 2021, p. iv). The implementation of JtD is considered an essential aspect of occupational therapy practices in the United Kingdom. It is also aligned with national priorities outlined in Scotland's Dementia Strategy (Gray et al., 2023), and is recommended as a core role of occupational therapy (Gray et al., 2023). In Quebec, there is a lack of community-based programs for older adults living with early dementia that focus on promoting meaningful participation.
To collect preliminary data to support the planning of future trials, this study thus aimed to explore the feasibility of future implementation of the JtD program in Quebec, and given differences in cultural context between the United Kingdom and Quebec, it was necessary to assess how the program would be received locally. Specifically, the study explored: (a) their acceptability of the program; (b) appropriateness of its content and modes of delivery; (c) their adherence and retention to the program; (d) suitability of recruitment strategies, and (e) appropriateness of outcome measures.
Methods
Study Design
Guided by the Medical Research Council (MRC) framework for developing and evaluating complex interventions (Skivington et al., 2021), a single-site exploratory feasibility study was conducted. Exploratory studies are important for generating preliminary evidence needed to determine whether and how to proceed with a larger-scale intervention. One key objective of exploratory studies is to assess the feasibility of the intervention (Moore et al., 2018).
The MRC framework considers a broader range of contextual and implementation questions. In line with our study's objective we focused on five feasibility criteria, the first following three based on the intervention: (a) Acceptability (i.e., the extent to which program recipients were satisfied with the program and found it appropriate for their needs), (b) Program content and delivery (i.e., how participants responded to the content and mode of delivery of the intervention), (c) Adherence and retention (i.e., participants engagement including the number of sessions attended, tasks completed, and number of participants that completed the study). The remaining two criteria relate to the study design: (d) Recruitment (i.e., evaluating the strategies used to recruit participants into the study), and (e) Outcome measures (i.e., examining whether participants were able to complete the outcome measures, their understanding of the questions, level of fatigue during completion, and assistance required). The study was approved by the Comité d’éthique de la recherche vieillissement-neuroimagerie of the Centre intégré universitaire de santé et de services sociaux (CIUSSS) du Centre-Sud-de-l’Île-de-Montréal and the Institutional Review Board for the Faculty of Medicine and Health Sciences at McGill University.
Participants and Recruitment
Participants were referred to this program by a support service manager from a community organization that provides services for individuals living with a diagnosis of dementia and their partners. The service manager was familiar with the participants from other activities within the organization and understood the program's objectives. She identified individuals who could benefit from the program and referred them to the study coordinator, who later contacted them for interviews. The inclusion criteria were as follows: self-reported diagnosis of dementia, the ability to provide informed consent, living in the community, being willing to commit to an 8-week program, and being able to communicate in English. To avoid the limitations associated with using cognitive tests as a cutoff for inclusion (Brijnath, 2011), eligibility for the program was determined by the professional judgment of the services manager at the community organization. An occupational therapy student further validated this decision during the first interview. In line with an exploratory feasibility study, we initially anticipated recruiting a group of six participants to allow for a more in-depth exploration of their experiences.
The program was initially designed for care partners to attend only the first and last sessions, provided their partners consent. However, after participating in the first session, the care partners expressed a desire to stay involved throughout the program. Since the program allowed for some flexibility in its structure, we were able to accommodate their request for ongoing participation as detailed below.
Intervention
For the feasibility study, dyads met weekly for 8 group sessions covering the following modules: (a) Welcome and introductions, (b) Health, well-being, and activities, (c) Making the most of routines, (d) Outing in the community, (e) Maintaining community connectedness, (f) Enabling environment and technology, (g) Memory maintenance, and (h) Moving forward: celebrating and ending. Each session began with a light lunch during the first 30 minutes, bringing together participants, the facilitator, and the research team. Following lunch, the session continued for approximately 1.5 hours. All sessions were held at the research center and conducted in English. Table 1 describes the session flow.
Flow, Topics, and Attendance of Sessions.
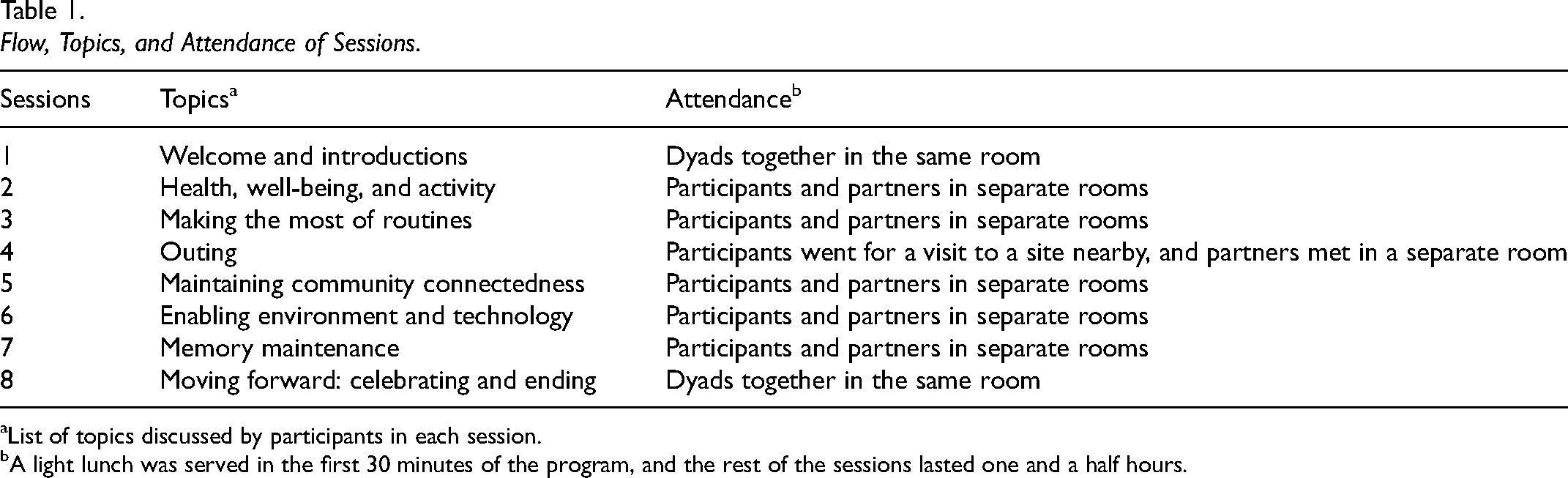
List of topics discussed by participants in each session.
A light lunch was served in the first 30 minutes of the program, and the rest of the sessions lasted one and a half hours.
From sessions 2 to 6, care partners began meeting in a separate room following the shared lunch. These informal gatherings, facilitated by a member of the research team, provided a supportive space for care partners to discuss the challenges and opportunities they face following their partner's diagnosis.
As the JtD was codeveloped with individuals living with dementia and family members and aligns with key priorities identified in the literature—such as engagement in everyday activities, peer support, and access to education and coping strategies (Belchior et al., 2023) – no adaptations were carried out before the start of the program. This study aimed to determine whether context-specific modifications were necessary, without altering the content, while also testing key feasibility components before further implementation studies.
Program Facilitator
The occupational therapist who led the program had over 10 years of experience working with older adults diagnosed with neurocognitive disorders and expertise in group dynamics. Due to his background, he only required a brief training period, which consisted of three 1-hour sessions with one of the co-authors (CG), who was involved in the development of the JtD program. During this training, the occupational therapist was informed about the program structure and the materials used for its delivery.
Data Collection
Outcome measures: Three questionnaires were selected to assess outcomes of interest in the study. The first is the Canadian Occupational Performance Measure (COPM) (Law et al., 1990), which is designed to identify and evaluate individuals’ perceived performance in everyday activities related to self-care, productivity, and leisure. It uses a semi-structured interview to help clients prioritize meaningful goals and rates both performance and satisfaction on a 10-point scale. The second is the Dementia Quality of Life Questionnaire (DEMQoL), specifically designed to assess the quality of life for individuals with dementia (Smith et al., 2007). The third is the General Self-Efficacy Scale (Schwarzer & Jerusalem, 1995), which measures individuals’ belief in their ability to perform in everyday situations. Additionally, one questionnaire was administered to partners and was developed to evaluate burden: the Zarit Burden Scale (Zarit et al., 1980). Finally, the occupational therapy student took field notes during the sessions to document the steps of program delivery.
The study coordinator met with participants at three points during the study. The initial meeting was conducted either at the participants’ homes or at the research center. During this session, participants completed baseline outcome measures. The midpoint check-in consisted of a brief phone call to monitor progress and collect impressions about their experiences with the program thus far. The final interview was conducted in person. During the final interview meeting, participants were also asked a series of questions to gather their perception about the program. These questions were informed by the key feasibility criteria explored in this study, specifically focusing on acceptability, content, and delivery, and included questions such as: “What is your overall impression of the program?”, “To what extent did the program address your needs?”, “Did you experience any benefits from participating in the program?”, “Did you experience any frustration with the program?”, “How willing would you be to continue participating in a program like this?”. All participants chose to invite their partners to take part in the interviews. The partners provided valuable insights, having attended portions of the program. Their contributions were therefore included in the analysis as they had also provided consent to be part of the study.
Specifically, data for acceptability, program delivery, and compliance were collected through semi-structured interviews and field notes. Data for recruitment and retention were collected through field notes. Finally, data for outcome measures were collected through questionnaires and field notes. Efforts were made to ensure that the questions were easy to understand, thereby minimizing participant fatigue. Questionnaires were administered both before the program began and at its conclusion.
Data Analysis
Data were analysed using a primarily deductive approach, guided by feasibility domains (Skivington et al., 2021). We used Miles et al. (2020), which served as a guide to structure the thematic content analysis. First-level codes were developed inductively to capture participants’ specific experiences (e.g., “impression about the program,” “safe space,” “demystifying dementia”). These codes were then grouped into second-level themes corresponding to the predefined feasibility domains, which served as the thematic categories.
Results
Four participants were recruited, but one withdrew because of a schedule conflict. As a result, three participants completed the study. All participants were white men, aged between 63 and 79 [P1 (65), P2 (63), and P3 (79)], held university degrees, currently retired, lived with their partners, and had received their diagnosis within the past 5 years.
Overall, the program was perceived as acceptable by participants, with both content and modes of delivery considered appropriate (Table 2). Adherence and retention rate were high, indicating strong engagement with the intervention. While recruitment presented some challenges, valuable insights were gained regarding potential barriers (Table 2).
Summary of Key Feasibility Criteria and Outcomes.
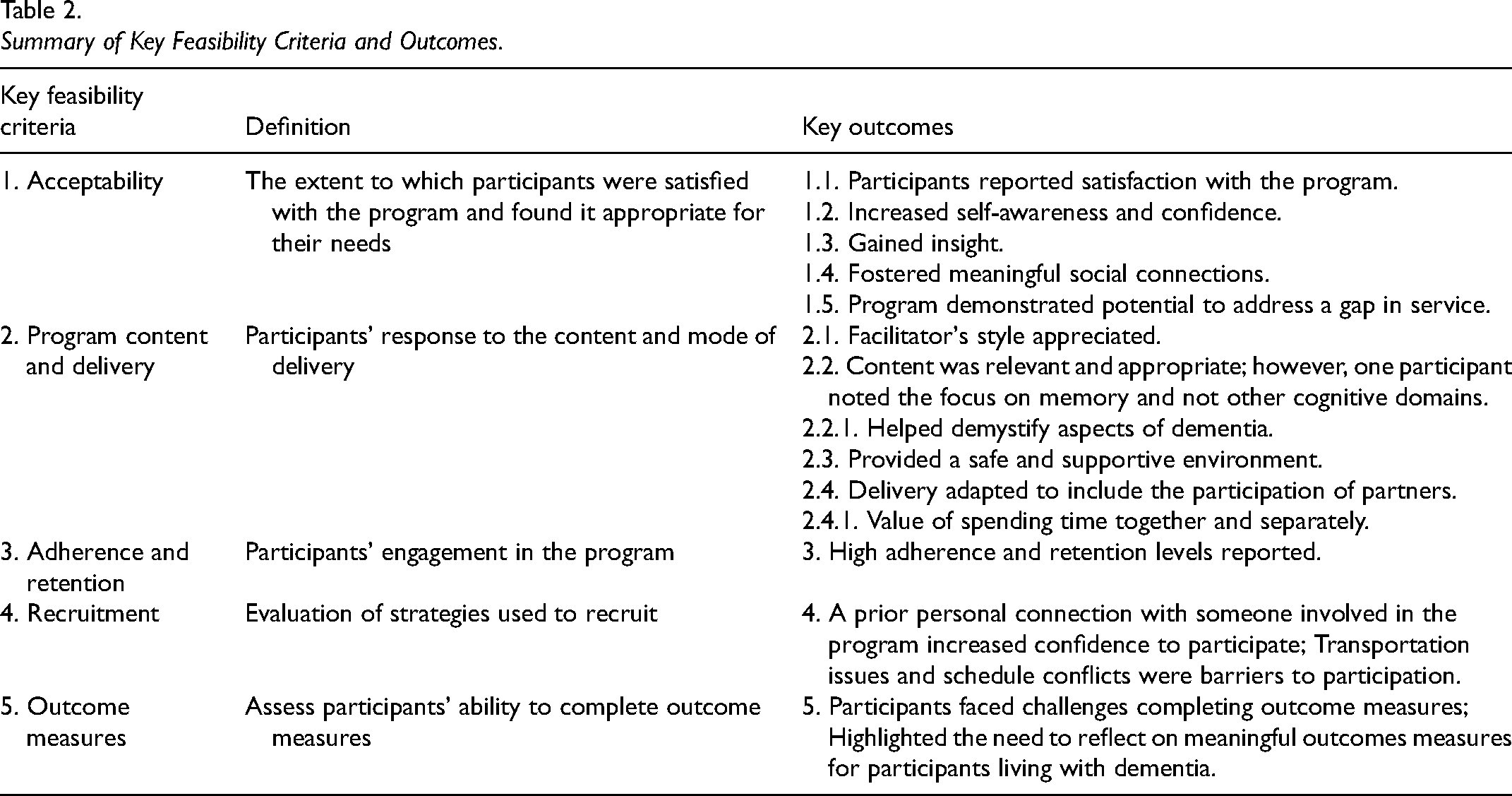
During the program, two participants chose to engage in volunteering activities (Table 2). One participant found that the program boosted his confidence, leading him to volunteer alongside his partner at a program that provides physical activities for individuals with mobility issues. He enjoyed his volunteer work, as it provided an opportunity to continue learning, as he reported: “I think the learner cycle, part of that learning is learning from the people who have challenges” (P3).
I have judgment issues… [when] I find myself in and some of the environments, including the Internet, my judgment leaves me sometimes as a victim (P1); I see a difference in you after the group, in the last couple of weeks. More of a reflection. You did not want to talk about it, but you were thinking, and then coming out with things. Because you’re a person who is very reflective, I’m seeing that when you come out of the group. More a calmness (PP1).
The first thing is that I’m not alone. Even though we have problems with Alzheimer's, there are three people living with it, and we have interesting things to share. People different from us have other ways of being, and it gives ideas to make life more enjoyable (P2).
Participants also found it relevant that the program was centered around the idea of maximizing well-being and provided concrete steps (Table 2), as mentioned by one partner: This theme of living your best life, we used to talk about it [at home] and in the group, that was the focus a lot, but in a very concrete way. It was very good. I got a lot of benefit from that (PP1).
Participants felt that their discussions were enriching, and they learned something new each week, as expressed by one participant: For us to be able to create this environment and have that type of substantive discussion (P3).
I found that people felt safe enough if they wanted to speak. We did not know each other, but everyone felt comfortable enough to participate, contribute, share, and help (P3).
Partners reported that participating provided them with an opportunity to understand the program with their spouse: “I like the fact that we were together, came home together, and we understand this program together” (PP1). They also noted how meaningful it was to see participants connecting with one another at the end of each session, as highlighted by one partner: It was also nice to see the other gentleman, what their face was like when they got out of that meeting, banter and joking a little. You could tell that they were also connecting […]. It just happened and I felt a kinship (PP2).
Having them together reassured individuals living with dementia that their partners were also taken care of and that their issues were also being addressed, which was important to them, as mentioned by one participant: I really think that I was going to be by myself, and I thought that [my partner] would be telling me the stories after I got home. As it turns out, that was a very good, and that might have also been felt by the other guys (P1).
I have been in that type of situation before, and I enjoy it. This was very good at the beginning, where we are all together just as the little groups, like the couples […] It was really important for me (PP1).
One participant expressed that it also helped to understand what other couples living in similar situations were dealing with in their everyday lives, although it took some time to feel comfortable opening up: “Because we exchanged, we understood what the other one was typically doing with his wife. It took time to exchange frankly and openly, I feel that it took many meetings” (P2).
Because[the service manager] thought we would be a good fit, and indeed she had a good sense for it, but it's not just because you have the diagnosis that you’re going to [enjoy] it (P2).
The recruitment represented some challenges. In addition to the person who withdrew before the program started, another individual expressed great interest but was unable to attend due to transportation issues (Table 2). Moreover, another potential participant had prior commitments that conflicted with the program's schedule.
Discussion
The goal of this study was to explore the feasibility of implementing the Journeying through Dementia program in the Quebec context to gather preliminary data to support planning of future trials. Feasibility was assessed using five indicators (Skivington et al., 2021): acceptability, program content and delivery, adherence and retention, recruitment, and outcome measures. Three dyads participated in an 8-week program, which involved weekly 2-hour sessions. Overall, this study supports the feasibility of using the Journeying through Dementia program in Quebec and offers insights to guide future adaptations and ongoing implementation research.
Overall, participants were satisfied with the program and experienced positive benefits. Participation in the program provided a sense of self-awareness, confidence, and insight. It also created an environment in which participants could connect with others and build supportive relationships, which demonstrates the potential of this program to address social participation. The importance of supportive social environments for the well-being of people living with dementia has also been highlighted in previous research (Sturge et al., 2021). Starting new activities, meeting others, and building trust have been reported to create feelings of normalcy and self-worth; these were elements in this program that could have contributed to the positive results. Our findings align with previous research that has demonstrated that empowerment in people living with dementia is fostered through interactions within their social environment, particularly through communication about their needs and wishes, as well as enabling shared decision-making and reciprocal relationships. (Ziebuhr et al., 2023).
Another benefit reported by participants was the program's potential to address a gap in existing services by offering tailored and flexible support. In this context, the program stands out as a promising approach to addressing this need. As highlighted by King et al. (2024), the current service landscape is characterized by fragmented infrastructure, limited resources, and an inconsistent understanding of dementia. The challenges in accessing services post diagnosis have also been documented elsewhere (Ramakrishnan & Malhotra, 2025; Parsons et al., 2025; Zhang et al., 2025).
In relation to the program content, participants felt that the topics were overall appropriate and relevant to their needs. The focus of the program on “living your best life” instead of focusing on losses and decline conveyed a broader and more hopeful outlook on life, which was appreciated. While the meaning of living well may differ among individuals and change over the course of the disease, one recent study has identified six common factors that contribute to this experience (Quinn et al., 2022), which has also alignment with our results: (a) a positive outlook on life (e.g., participants expression that even though they have Alzheimer's they still have interesting things to share); (b) physical fitness and health; (c) social engagement and connectedness (e.g., connection among participants and among partners); (d) independence in daily activities; (e) quality of interpersonal relationships (e.g., feeling more like a couple and less like a “caregiver”), and (f) perceived social standing and societal role (e.g., feeling that they are not alone). (Quinn et al., 2022). These factors were introduced in the program and also contribute to supporting participants’ social participation.
This perspective necessitates a shift from the traditional medical model, which primarily focuses on symptom control, to a more holistic approach. Participants also described the program as destigmatizing, possibly due to the reframing of dementia as a manageable condition rather than focusing only on losses. This approach can also contribute to shifting the label of “caregiver” to a “partner,” a change that was valued by participants. The term “caregiver” can be unsettling, as it can imply a shift in personal identity that not all partners are comfortable with. One partner expressed that the label of a caregiver feels imposed upon her, and this label risks shifting her identity as a woman and wife, overshadowing her own needs (Hooper & Collins, 2019). One proposed adaptation to the program would be the inclusion of content addressing cognitive changes beyond memory. As memory maintenance is covered, but other cognitive domains were not explicitly addressed, which was remarked by one participant.
In terms of the delivery of the program, an important adaptation in this study was the participation of the participants’ partners in all sessions, rather than only the first and last as in the original program. In the first session, partners expressed a desire to participate in the meetings and form their own group to address their own needs. Participants observed that this experience helped them better understand the program together. In fact, the concepts of “together” and “separate” emerged as metaphors for their experiences, symbolizing their simultaneous shared and individual journeys through dementia. Viewing this experience from a relational lens, instead of focusing only on the person living with dementia, allowed for a more nuanced understanding of their journey, as also suggested by Demers (2022). Partners’ ability to successfully orchestrate their lives to meet their occupational needs, along with persons diagnosed with dementia, is essential for well-being (Hooper & Collins, 2019).
The program also provided partners with a sense of belonging, addressing their loss of social connection. It created a space where they could experience mutual support in their roles (Hooper & Collins, 2019). In fact, there is an increased recognition of the importance of supporting couples’ relationships through the dementia journey, but the community-based programs in this area remain largely unexplored (Bannon et al., 2025; Colloby et al., 2022).
This study suggests that when the social environment is adapted to meet the needs of both individuals living with dementia and their partners, they can also have positive experiences in the role of care partners (Demers, 2022). “Understanding of caregiver experience embedded within an occupational participation approach to explore caregiver and care recipient occupations could produce ‘double-well-being’” (Demers, 2022, p. 228). It is important to note that the recruitment strategy did not intentionally focus on recruiting dyads; the occurrence of dyads was coincidental and contributed to the outcome. While other group compositions may yield different results, future research could benefit from intentionally organizing specific groups for partners and also focusing on their relationships.
In terms of recruitment, participants’ prior relationship with the organization helped them feel safe joining the study. This was important as individuals in the early stages of the disease may not be ready to participate in such programs, as they might still be coming to terms with the diagnosis. In fact, the stigma associated with a diagnosis of dementia often leads individuals to conceal their diagnosis or avoid social situations that might make them feel vulnerable (Xanthopoulou & McCabe, 2019). In addition, shame and guilt related to its symptoms, which can be worsened by negative societal attitudes (Kotwal et al., 2024), can contribute to reluctance in joining new groups.
One barrier encountered was transportation, which seems to be a challenge for participants at the organization overall. For many potential participants, driving may not be an option, and using public transportation can be challenging. Lamanna et al. (2020) suggest that alternative transportation solutions should be considered alongside the development of community-based programs, as this is a common issue.
The next feasibility criteria explored were related to study design. In terms of adherence and retention, participants attended all the sessions, with a 100% attendance rate, which could demonstrate the impact of the program on their daily lives. This can also attest to the satisfaction and positive benefits experienced by participants. From the very first session, there was a strong sense of belonging and connection among the group. All participants recognized that feeling safe was a crucial factor in enhancing their engagement in the program.
Our findings regarding the challenges participants faced in completing outcome measures are consistent with previous research. A recent narrative synthesis reviewed the use of standardized self-report measures in studies involving individuals living with dementia (Gridley et al., 2024). It revealed that incomplete assessments and missing data are common in these studies. These issues are often associated with factors such as participant burden or emotional distress caused by the assessment process. However, such challenges are seldom documented or discussed in published research (Gridley et al., 2024).
Some researchers argue there might be value in evaluating the immediate or short-term effects of the intervention, even section by section, instead of focusing on more long-term outcomes (Smith et al., 2022; Reilly & Harding, 2025), as previous research has highlighted the importance of “being in the moment” for individuals living with dementia. This is significant because their experiences of the condition can fluctuate, making reports on “last month” or “last week” not relevant (Smith et al., 2022).
There is a growing call to develop and validate new approaches for assessing psychosocial outcomes in individuals living with dementia (Reilly & Harding, 2025). While most existing assessment tools focus primarily on symptom reduction, this does not always reflect those with lived experiences. When asked, individuals living with dementia often emphasize experiences such as feeling valued and respected, being able to laugh with others, and staying engaged in meaningful activities they enjoy (Reilly & Harding, 2025). If outcome measures fail to reflect these priorities, there is a risk of measuring the wrong things. This is supported by studies that have reported discrepancies between qualitative measures and standard assessments, which can risk failing to capture the real benefits of interventions (Reilly & Harding, 2025).
Lastly, because there are currently no specific assessments available to measure meaningful participation for individuals with dementia, researchers often rely on proxy outcomes, which was the case in this study. However, these outcomes may not reflect what is truly important to those living with dementia. Therefore, further research is necessary to develop a meaningful way to assess outcomes in this population.
Limitations
One limitation of the study is the small sample size; however, the qualitative data collected provided detailed and rich accounts that offer valuable insight into participant experiences. Additionally, home visits—originally planned as part of the intervention—were not conducted due to the occupational therapist's limited availability within the study timeframe, making it logistically unfeasible to deliver this component. Given that this was an exploratory feasibility study primarily focused on assessing key feasibility indicators, we proceeded without the home visits. Lastly, the lack of demographic data on participants’ partners may be seen as a limitation, as it restricts our ability to explore how partner characteristics may have shaped their experiences with the program.
Nonetheless, despite these limitations, the study offered meaningful insights into participants’ experiences with the intervention. These findings contribute important knowledge that can inform the design and delivery of future programs and research aimed at similar populations. Finally, given the exploratory nature of this study, these limitations did not significantly compromise the overall aims related to feasibility.
Conclusion and Next Steps
This exploratory feasibility study supports the feasibility of using the Journeying through Dementia program in Quebec and offers insights to guide future adaptations and ongoing implementation research. The program was well-received by participants, and adherence and retention were successful within the small-scale context of the study. Participants continued to meet at the community organization even after the program ended, demonstrating both sustained engagement and a critical need for this type of intervention. Noted adaptations for the next phases are the inclusion of partners in the program and refining the outcome measures. We recognize that the experiences of people living with dementia are very diverse, and the findings from this exploratory study may not represent the experiences of all groups. A diagnosis of dementia is not without challenges, but this study demonstrated that with the appropriate support, individuals can still have meaningful experiences. Nevertheless, this study has provided relevant information to inform the planning of future work.
As a next step, we are collaborating with a community organization to build on the insights gained from the feasibility study and deliver the program in the community. This will allow us to gather further information on potential barriers and facilitators to implementation. A complementary step will be to translate the program into French—the predominant language spoken in Quebec, Canada—in preparation for a larger-scale evaluation. Together, these efforts aim to inform future implementation of the program.
As a concluding note, in this study, we use the term “people living with dementia” as it reflects the name of the program and is commonly used in the field. However, we recognize that not all individuals diagnosed with dementia identify with this term, and while alternatives like “neurocognitive disorders” are also used, many people are not familiar with this terminology. We strive to use language that respects individual preferences.
Key Messages
Preliminary results support the feasibility of conducting further implementation studies of the Journeying through Dementia program in Quebec.
This exploratory study showed that recognizing people living with dementia and their care partners as equal collaborators should be taken into consideration when developing programs.
Footnotes
Acknowledgements
Kami Sarimanukoglu
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Canadian Occupational Therapy Foundation (COTF); CIUSSS Centre-sud-de-l’île-de-Montréal- Programme d’appui à des Projets de recherche stratégiques et structurants (PRSS).
