Abstract
Introduction
Technological advances and the emergence of artificial intelligence (AI) are beginning to have an impact on the healthcare industry, sparking ongoing debates regarding their influence on work efficiencies, ethical considerations, and employment opportunities (Davenport & Kalakota, 2019). AI, as defined by the Oxford Dictionary (2021), refers to “the capacity of computers or other machines to exhibit or simulate intelligent behavior” and utilizes machine learning to analyze complex data, identify patterns, problem-solve, and make decisions (Meskó & Görög, 2020). This innovative technology has the potential to transform various aspects of patient care and influence occupational therapy assessments and interventions.
As AI and technological innovation continue to shape healthcare practice, research suggests that society is entering a “Fourth Industrial Revolution” (Liu, 2018). Recent studies have demonstrated the potential of AI to improve patient outcomes by enabling more accurate and timely diagnoses and personalized treatment plans (Topol, 2019). Additionally, AI has been shown to reduce healthcare costs by automating repetitive tasks, minimizing the risk of medical errors, and enabling care delivery in non-traditional settings (Davenport & Kalakota, 2019). Given the rapid advancements of AI and technology, the need for traditional manual occupational therapy assessments and interventions may gradually decrease.
The healthcare industry is increasingly adopting AI to enhance the quality and accuracy of medical decision-making, diagnosis, and treatment (Lambert et al., 2023). For example, AI algorithms have successfully detected Diabetic Retinopathy with accuracy comparable to trained ophthalmologists. Other studies have demonstrated that AI-powered systems in radiology accurately detect lung cancer from CT scans with high sensitivity (Mathew et al., 2020). AI has also been utilized to analyze electronic health records, predicting patient outcomes and identifying potential health risks (Xiao et al., 2018). Although healthcare professionals, such as surgeons and physicians, currently have varied understandings on AI, most generally have positive perspectives toward technology implementation in healthcare (Dave & Patel, 2023; Mousavi Baigi et al., 2023).
AI has also been used in occupational therapy. For example, AI has been implemented in upper extremity functional assessments, prediction of spasticity scores using wearable arm sensors, smart technologies for driving, and robotic devices for pain relief in premature babies (Adams et al., 2019; Classen et al., 2019; Holsti et al., 2019; Wang et al., 2020). However, the perceptions of AI use in the field of occupational therapy remain unclear. Understanding the experiences, perspectives, and outlooks of occupational therapists regarding AI is crucial to ensure the field is well-prepared to implement these technological changes.
This study aims to explore occupational therapists’ current perceptions and opinions regarding AI. Investigating these perspectives is essential for understanding the willingness to adopt technology and the potential impact of AI on patient care. The study seeks to gain insights into the current perceptions and uses of technology and AI in practice and the possible implications for future healthcare applications. Obtaining a deeper understanding of these perspectives may enable healthcare authorities across Canada to justify technology funding, guide the implementation of systemic changes for technological adoption, and most importantly, support training practices and education for occupational therapists.
Method
Study Design
Our study employed a sequential explanatory mixed methods design (Creswell & Creswell, 2018), utilizing surveys (quantitative) and focus groups (qualitative). To gather the opinions and perceptions of registered Canadian occupational therapists, a nationwide online survey was conducted in English and French using Qualtrics©. Initial findings from the surveys were then used to design and conduct online focus groups in English via a secured Zoom© platform.
Participants
Participants were recruited through convenience sampling via provincial regulatory bodies, educational programs, social media, and national and provincial professional occupational therapy associations. In order to be eligible for inclusion in the study, participants had to be registered occupational therapists practicing within Canada. The recruitment materials provided an overview of the study and links to the online survey. At the end of the survey participants had the opportunity to express interest in participating in the focus groups.
Ethics
The study received ethical approval from the Behavioural Research Ethics Board of the University of British Columbia (ref. #H21-02088). The online survey was designed using the University of British Columbia Survey Tool, Qualtrics. Qualtrics stores all data in Canada and adheres to Canadian privacy and security standards. Participants were presented with information about the survey and informed consent for participation.
Data Collection
The construction of survey and focus group questions was based on previous studies investigating the perspectives of AI among radiologists and surgeons (Coppola et al., 2021; van Hoek et al., 2019) and in discussion with key stakeholders (e.g., researchers, occupational therapists).
The survey obtained data on participant demographics, current perception and definition of AI, occupational therapists’ opinions toward AI, and the potential therapeutic benefits and risks of AI. Various question types, including multiple choice, 7-point Likert scale, and short answer, were utilized throughout the survey (Supplementary Appendix A). Participation in the anonymous survey was voluntary, and no incentives were provided.
Focus groups were scheduled based on participants’ preferred availability. Each group lasted approximately 60 to 75 minutes, using an interview guide exploring various aspects of AI in OT practice (Supplementary Appendix B). Focus groups were conducted exclusively in English as the researchers involved were proficient only in this language.
Data Analysis
Quantitative Data
Descriptive statistics were generated using IBM SPSS Statistics software (Version 28.0). Participant responses were included in the analysis if they completed at least 85% of the questions, as this completion rate ensured meaningful responses beyond demographic information.
Qualitative Data
Thematic analysis was employed to identify common themes expressed by the focus group participants. Data from the focus groups were transcribed verbatim from the Zoom audio transcripts. Four researchers independently conducted initial coding of the focus group data, following the guidelines by Clarke and Braun (2017). Codes were generated by highlighting exact words from the text that captured key thoughts or concepts.
After reflection on identities and positionality, along with beliefs and biases through independent journaling, the researchers reached an agreement on the codes. Similar codes were subsequently grouped into categories based on their relationships and connections. The researchers described the related categories as potential themes. The themes were further reviewed by the whole team to ensure their applicability in relation to the codes. Ongoing analysis refined the number, name, and specifics of the themes (Clarke & Braun, 2017).
Finally, the quantitative findings were compared with the themes that emerged from the qualitative analysis (Hsieh & Shannon, 2005). These interpretive processes provided a context for the trends found in the quantitative analyses: the qualitative findings helped explain the quantitative findings (Creswell & Plano Clark, 2011; Klassen et al., 2012).
Findings
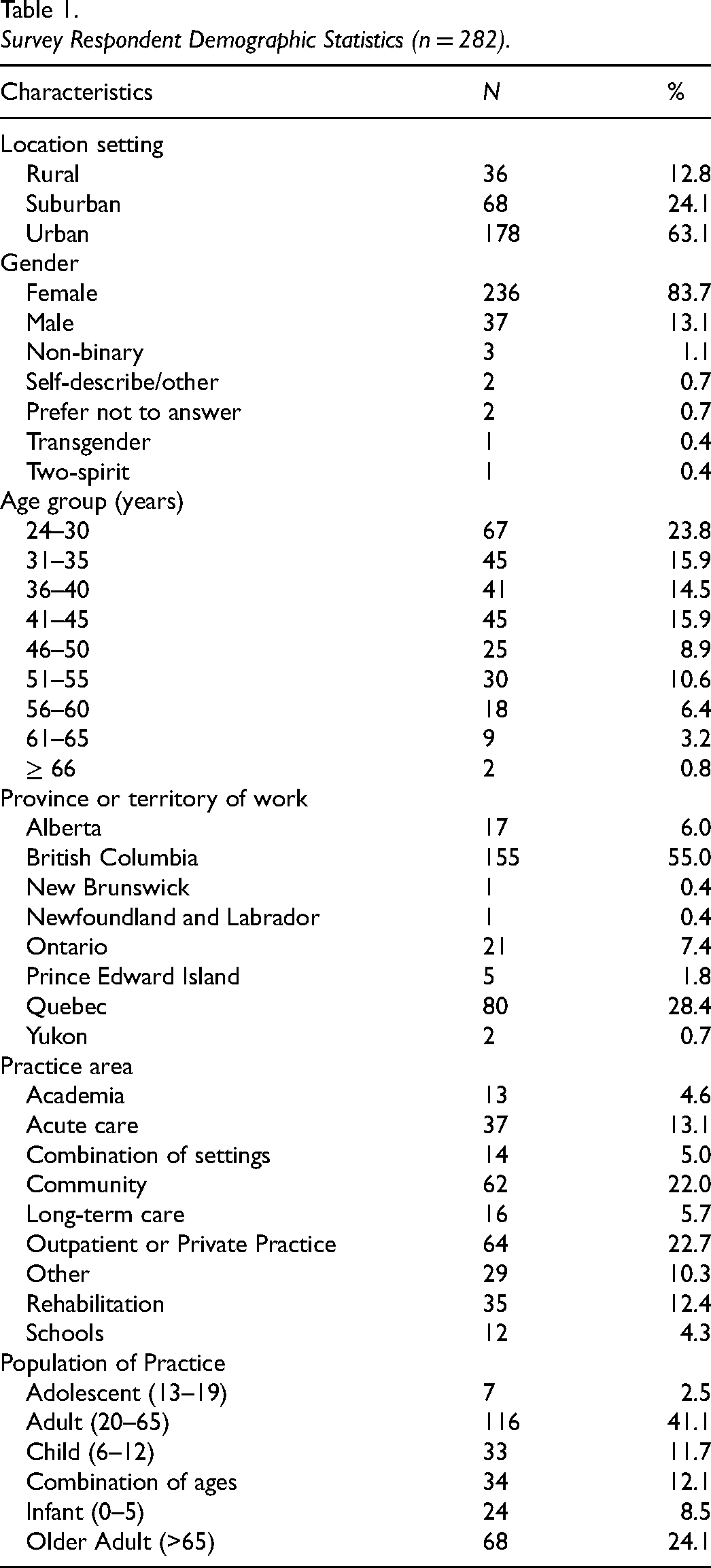
A total of 282 occupational therapists from across Canada participated in the study, with all participants completing the survey and 15 participants taking part in four separate online focus groups, ranging between 3 and 4 per group. Majority of survey participants were women, aged 24 to 40 years old, who practiced in urban settings (Table 1). Pediatric occupational therapists accounted for 20.2% of the sample, while the majority identified themselves as primarily working with adults (41.1%) (Table 1).
Survey Respondent Demographic Statistics (n = 282).
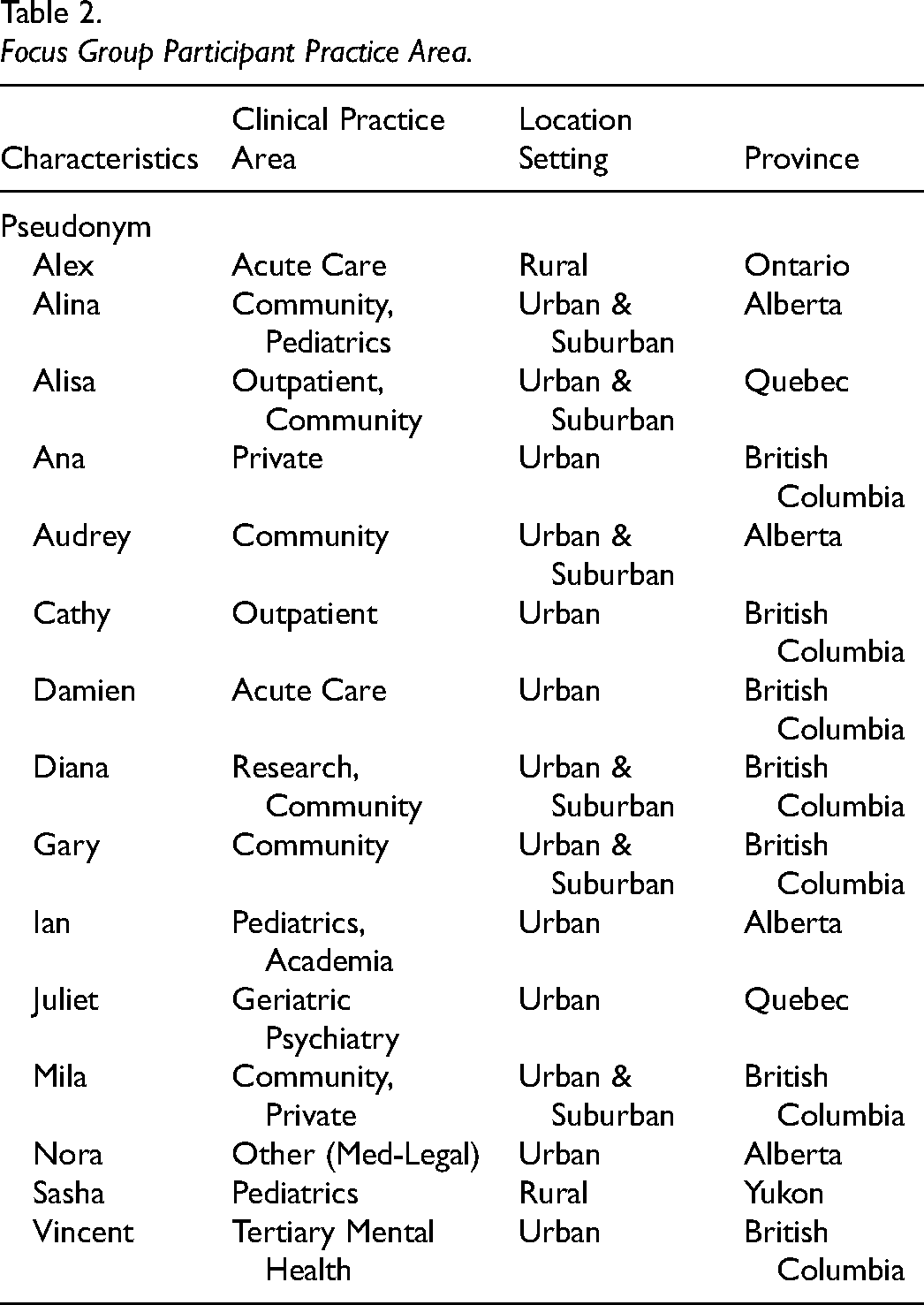
The 15 Canadian occupational therapists who participated in the focus groups are working in various practice settings. The majority of them were women practicing in urban areas representing five different provinces/territories (Table 2).
Focus Group Participant Practice Area.
Three main themes emerged, supported by both the quantitative and qualitative data, the first “AI Knowledge & Implementation” centered on understanding and experiences with AI, the second, “Use of AI in Occupational Therapy Practice” highlighting benefits, uses, and risks of AI use in practice, and the third, “Human vs. Machine” discussing impacts on client interactions, emotional intelligence, and potential threats to job opportunities. All names used in this section are pseudonyms, to maintain the focus group participants’ confidentiality.
Theme 1: AI Knowledge & Implementation—“The Learning Curve Can be Large”
Participants had varying levels of understanding of AI and different definitions of it. Some expressed uncertainty about what AI entailed and its applications in their practice setting. For example, Alex described AI as “a computing or electronic device that has been programmed and fed information, then it's able to utilize that information to make its own decisions, and formulate thoughts or artificial ideas.” Others agreed that AI involves predictable data sets, machine learning, applied statistics, and the use of algorithms to recognize patterns and make decisions. When asked about their understanding of AI, 88.3% of survey respondents agreed that they had a good understanding, with fewer participants, yet more than half of them (57.8%, 163/282) choosing to describe AI as “the simulation of human intelligence,” which aligns with our study definition.
The topic of AI education was also discussed among the participants. Most believed that education on AI should be included in the university curriculum to increase familiarity with its application and utilization with clients. They emphasized the importance of understanding how AI works and being familiar with its capabilities and limitations to use it appropriately before entering the profession. However, there were differences in opinions regarding the timing of AI education in occupational therapy practice. Some participants expressed interest in AI education throughout schooling, while others believed that education would be most beneficial if AI is currently integrated in their workplace. Nonetheless, most (84.1%) of the participants had responses ranging from somewhat agree to strongly agree when asked about the implementation of AI in OT practice.
Challenges participants identified related to implementing AI as it relates to knowledge. One challenge discussed was the personal barriers occupational therapists may face in learning how to use AI. Participants acknowledged their responsibility to understand the processes behind AI to effectively use it for clinical decision-making. However, they noted that understanding how AI works could be difficult for clinicians depending on their level of familiarity with technology, as described by Sasha: “One of the biggest barriers is therapist capacity. So the therapist being able to learn how to use it in order to facilitate somebody else using it or even recommend it, the learning curve can be large.”
Another challenge discussed was the justification of using AI to other healthcare professionals. Participants questioned whether healthcare professionals, such as physicians, would be receptive to recommendations from occupational therapists if AI was used as an aid for decision-making. Concerns were raised about the acceptance of AI by healthcare professionals who may already be hesitant to adopt existing technologies.
Participants also highlighted the challenges of implementing AI within the current healthcare system, as Audrey recognized the challenges of being limited by healthcare policies: I mean there's always [going to] be a learning curve and there's going to be red tape from higher ups and healthcare systems and what you can and can’t use right? That's just one of the facts when it comes to the healthcare system.
Participants mentioned that Canada has been slow to adapt technology and lacks systems to support AI or innovation in healthcare. Despite these challenges, a majority of survey respondents (84.0%, 237/282) expressed support for the implementation of AI in occupational therapy practice. All in all, participants agreed that learning to use AI within occupational therapy practice would be worthwhile, even if existing policies present barriers to its implementation in the healthcare system.
Theme 2: Use of AI in Occupational Therapy Practice—“It Could Help With Caseload Management and Prioritization”
Participants discussed the potential applications of AI that could benefit occupational therapy practice. These included using AI for initial referrals and screenings, standardized assessments, prediction and pattern identification, evidence-based recommendations, and streamlining documentation.
Participants noted that AI could fill a gap in the healthcare system and reduce the wait time for initial assessments. Survey respondents also identified potential advantages of AI in practice, including increased efficiency of daily work (58.9%, 166/282), reduced administrative time and costs (49.3%, 139/282), reduced wait times for occupational therapy services (48.2%, 136/282), and higher accuracy with lower rates of error (45.7%, 129/282). Participants agreed that AI could provide support to alleviate pressures in caseloads. Alex expressed a potential benefit of AI stating: It could help with caseload management and prioritization, not saying to fully replace the clinician, but I know, for me, sometimes I get thrown a caseload of 50 patients that I have to figure out who I have to see, and I only have so many hours in a day.
Diana wondered about the potential of using AI for screening stating: “perhaps AI could screen those initial referrals, and then could pass them along to the therapists who might be interested in taking on those specific clients based on their availability, preferences, etc.” Audrey supported this idea, as she explained: I think it could be really helpful in that sense, in terms of maybe filling a gap in the healthcare system, like there's such a long wait for initial assessments, and sometimes even you do the assessment and you think “oh this isn’t even an OT referral, this is psych or social work.”
The value of AI in assisting with standardized assessments was also discussed. Participants suggested that AI could play a role in administering standardized assessments, such as the Montreal Cognitive Assessment, and providing basic analysis of the results. The ability of AI to identify patterns and make predictions was another topic of discussion. Participants explored the potential of using AI to predict readmission rates for patients, allowing occupational therapists to provide better support for clients at home. Ian, a pediatrics occupational therapist, mentioned the usefulness of AI in collecting visual motor information and generating predictive data based on hand writing stating: You’d be able to easily get a lot of data and information from multiple aspects, because you’re collecting visual motor information, you’re collecting written outputs … even the stroke marks, there's so much rich data in a stroke mark of just analyzing a kid's written output and making assumptions about it.
The use of AI in making recommendations for assistive devices was considered by participants as well. Mila agreed and noted that while occupational therapists currently take measurements of clients, AI could potentially provide accurate measurements and reminders for skin degradation as she stated: “[it] can measure, well record your wheelchair angle, and then remind you when you've been sitting at that angle for too long, so you will be reminded to tilt it back and relieve that coccyx area.” Some participants noted that AI and technology could be useful as an addition to a clinician's decision-making. For example, Damien discussed how AI may be useful in providing appropriate equipment options explaining: It can help us with decision making, as to what kind of like mattress let's say, that would be beneficial for this patient, because sometimes there are certain, sometimes we do miss out on certain things and I do feel like artificial intelligence will kind of help us out in, you know, making sure that we tick all the boxes when we're providing care for our patients.
Regarding the usage of AI, 96.4% (272/282) of survey respondents agreed that if AI achieves high assessment accuracy, it should be used with sporadic or constant occupational therapy supervision. Participants stressed the importance of including justification for AI-generated recommendations, particularly for less common assessments and interventions. Diana noted that having access to evidence on how recommendations were made would increase the usability and trustworthiness of AI in occupational therapy practice highlighting: if we did get that kind of evidence of how AI gave you that assessment or intervention recommendation, I think it would help people use it a lot better and increase the usability… because I think as humans, we kind of want to see the reasoning behind everything.
Similarly, if AI achieves high intervention accuracy, 95.7% (270/282) of survey respondents believed it should be used with sporadic or constant occupational therapy supervision/presence. Most participants felt that AI should be used in collaboration with the clinician's work, as opposed to an isolated option. Alex elaborated on this as she stated: “AI can impact rapport and the sense of trust that a client feels. As professionals we set a standard that AI may not be able to replicate, I think it is important to use technology with oversight to keep everyone safe.”
Theme 3: Human Vs. Machine—“Everyone has that Initial Fear that We’re Going to beRreplaced”
Participants emphasized the importance of being able to relate through lived experience and utilize therapeutic use of self in occupational therapy practice. Audrey highlighted the significance of emotional intelligence and relatability in her role as an occupational therapist, stating: “There's that understanding and relatability that we can have to one another as practitioners and humans that I think AI just wouldn't be able to fully grasp.”
Participants expressed that technology and AI could impact rapport and the sense of trust clients feel. They noted that as professionals, they set a standard that AI may not be able to replicate. However, Diana raised a question: “What if AI can become so good that it could have those soft skills?”
Participants emphasized how that relatability and empathy were crucial factors to build rapport and relationships with clients, indicating that unique human experiences could not fully be recreated by AI. Others also discussed how humans can observe and actively react to cues related to body language, voice, tone, and inflection. Many agreed that misinterpretation in communication could lead to ethical issues, for example, individuals with dementia or cognitive impairments may not understand that AI is being used for their healthcare. In fact, many of survey respondents highlighted potential risks associated with the use of AI technology including increased ethical concerns 63.8% (180/282), and reduced human interaction (57.8%, 163/282).
Participants debated ethics, and the ability of AI to recognize when to make false statements to reduce distress and create positive interactions. Regarding a patient's ability to provide consent, Ana wondered: “What if they give consent in the earlier stages of dementia, but as it progresses, how would that change? Would patients truly understand the use of technology?” While some felt it might be appropriate for individuals with dementia, they acknowledged that it could create challenges for people who have difficulties with social interaction and understanding emotional cues. Overall, most participants voiced concerns regarding the ability for AI to adjust to specific scenarios, build rapport, and adjust interventions based on the needs of patients.
Participants expressed that the current use of technology with people with dementia, such as robotic stuffed animals and constructing home environments to resemble the 1960s-70 s, generally had a positive impact on improving quality of life and reducing psychological distress. This speaks to survey results with 98.9% (279/282) of respondents agreeing that further exploration of ethical concerns is necessary, prior to implementation. When asked about responsibility in case of an error made while using AI, the occupational therapist was the most frequently chosen response with 52.8% (149/282). Overall, participants believe that AI may not be suitable for all environments or populations.
Given the high variability and interactive nature of the occupational therapy profession, the participants did not anticipate that the implementation of AI would lead to a decrease in job opportunities in the future. They believed that AI could be utilized in current occupational therapy practice for tasks that were repetitive, predictable, and automatable. Gary shared his perspective: “There are so many factors… the occupations that seem to be at risk or losing their work involve tasks that are very predictable, that are very stable, and that can be automated.”
Participants emphasized that the current level of technology or AI would not replace occupational therapists or diminish their job prospects in the next 10 to 20 years. While 81.2% (229/282) of participants disagreed with the statement that there would be fewer job opportunities for occupational therapists in the future due to AI, the majority of survey respondents (76.3%, 215/282) believed that AI would have an impact on their careers within the next 5 to 20 years. They saw AI as a tool that could support their role in various settings and contexts. Survey data highlighted various benefits of AI in occupational therapy practice. The majority of respondents (65.6%, 185/282) agreed that AI could increase work efficiency. Additionally, 65.2% (184/282) of respondents believed that the benefits of AI outweigh the risks in OT practice. Yet, most acknowledged that people may have fears associated with losing job prospects due to AI, as Audrey stated: “Everyone has that initial fear that we're going to be replaced… as soon as you say AI, I feel like most people who don't work with AI regularly; most people generally will think of a robot or a talking computer.”
Discussion
The study focused on exploring the perspectives of occupational therapists on AI in healthcare. Previous research has primarily examined the views of physicians and radiologists, indicating that AI can be advantageous in reducing diagnostic errors and optimizing workflow but may negatively affect professional reputation from the public (Blease et al., 2019; Coppola et al., 2021; van Hoek et al., 2019). However, there is a notable lack of literature exploring the perspectives of occupational therapists on AI, highlighting a knowledge gap in this area (Villamil et al., 2019).
Results of this study provide insights into occupational therapists’ understanding and opinions of AI, as well as the perceived benefits and risks associated with its implementation. Generally, occupational therapists recognize the potential of AI to improve patient outcomes, streamline workflows, and reduce decision-making errors. These findings show similarities with previous research, as physicians, surgeons, and radiologists highlight the potential of AI to lower diagnostic errors and improve their work optimization (Blease et al., 2019; Coppola et al., 2021; Dave & Patel, 2023; Mousavi Baigi et al., 2023; van Hoek et al., 2019). These similarities may be attributed to the universal nature of challenges and opportunities AI presents across health professions, including concerns about ethics, integration into workflows, and the need for adequate training.
Findings from this study also suggest concerns regarding the current lack of education around technology, the possibility of AI replacing healthcare workers, leading to job loss, as well as the ethical implications of AI-driven medical decisions. Other healthcare professionals reported similar hesitancies due to the lack of education and training on AI technologies, and the uncertainty around the responsibility in case of AI errors (Blease et al., 2019; Coppola et al., 2021; van Hoek et al., 2019). Despite these concerns, previous findings showcase that physicians, radiologists, and surgeons overall express a positive perspective toward the implementation of AI (Blease et al., 2019; Coppola et al., 2021; Dave & Patel, 2023; Mousavi Baigi et al., 2023; van Hoek et al., 2019).
This research contributes to the existing literature on the use of AI in standardized assessments in occupational therapy. Previous research by Fong et al. (2020) demonstrated the potential of machine learning algorithms in improving the accuracy of functional capacity evaluations by providing direct numerical measurements through robotic systems. This study expands on these findings, showing that occupational therapists believe AI can enhance standardized assessments by offering performance summaries, scoring, and basic data analysis. This indicates a willingness among occupational therapists to adopt AI technology to improve assessment precision and accuracy.
Occupational therapists also identified the benefits of using AI in their practice, particularly in terms of increased efficiency in tasks such as charting and documentation. This aligns with the development of natural language processing (NLP) within machine learning, which enables automatic speech recognition, information extraction, and image captioning (van Buchem et al., 2021). NLP has been utilized to develop clinical voice assistants for transcribing patient visit information into electronic health records, reducing the time spent on documentation and allowing clinicians to focus more on patient care (van Buchem et al., 2021). Occupational therapists expressed interest in using AI to identify patterns in chart notes and extract relevant patient information during chart reviews, which is consistent with the capabilities of NLP and machine learning technologies. Although this type of technology is currently being implemented for physicians throughout hospitals in Canada (van Buchem et al., 2021), it remains unclear why AI integration in professions such as occupational therapy appears to be slower. Thus, additional research is required to explore this area further.
While AI has the potential to transform healthcare delivery and improve outcomes, concerns and drawbacks should be addressed. Privacy and security risks, ethical considerations, and the need for healthcare professionals to maintain their expertise and judgment in the face of increasing automation are among the concerns associated with AI use (Dave & Patel, 2023). Disparities in access to care and job displacement among healthcare workers are potential consequences of AI implementation in healthcare. Further research is needed to understand the impact of AI on healthcare delivery, develop ethical frameworks, and establish regulatory systems that ensure responsible and beneficial AI use in occupational therapy and other healthcare settings (Topol, 2019; Davenport & Kalakota, 2019). In addition, the question of who is responsible for providing education and preparing occupational therapists on how to use AI in practice remains unknown and must be explored.
Strengths and Limitations
This study is the first to be conducted on the opinions and perspectives of occupational therapists on AI within Canada. It utilized a mixed-methods approach with an online survey and focus groups to facilitate the exploration of various perspectives from Canadian occupational therapists. Through these platforms, this study explored the experiences of therapists from varying backgrounds and practice areas.
Technical difficulties were encountered during some focus groups due to connectivity issues, and language barriers were present as the groups were conducted exclusively in English. Additionally, the sample may not have been fully representative of all Canadian occupational therapists, as self-selection bias may have impacted their ability to participate. Response rates also varied across different provinces and territories, potentially impacting the generalizability of the findings. These limitations underscore the necessity for future research to address these issues and broaden the scope of the study.
Implications for Practice and Policy
Given the limited research examining occupational therapists’ viewpoints on AI, this study holds relevance for occupational therapists and other healthcare professionals seeking to comprehend their colleagues’ understanding of AI, concerns regarding its implementation, and perspectives on its current and potential uses in occupational therapy practice. As AI continues to integrate into healthcare systems, educating healthcare professionals, including occupational therapists, about AI can support in preparing for forthcoming changes in healthcare processes, addressing preconceived notions, and promoting interprofessional collaboration while upholding evidence-based practice. Furthermore, this research can help identify potential barriers and limitations in the implementation of AI in healthcare and inform companies developing AI technology about the perspectives of end-users. Overall, the findings from this study can serve as a guide for expanding educational opportunities, increasing access to diverse communities, and understanding the ethical considerations of AI in clinical practice.
Future Research
Future research in this area could delve into exploring perspectives on specific AI technologies and its application in greater detail. Additionally, investigating potential barriers to the adoption and implementation of AI, understanding the utilization of AI across different practice areas, and comparing AI use among urban, suburban, and rural communities can contribute to a more comprehensive understanding of AI's impact. Longitudinal studies could be conducted to assess how occupational therapists’ perspectives on AI evolve over time as technology advances and integrates further into healthcare systems. Moreover, research could explore the potential impact of AI on the occupational therapy profession, including the emergence of new roles and responsibilities, changes in job demand, and implications for education and training. Finally, cross-disciplinary research involving other healthcare professionals should be conducted to examine their perspectives on AI, fostering enhanced collaboration among interdisciplinary teams in the development and implementation of AI technologies in clinical practice.
Conclusion
This study aimed to investigate the opinions and perspectives of occupational therapists regarding AI and its potential impact on clinical practice. The findings, derived from focus groups and survey data, revealed that occupational therapists have varying levels of understanding on AI and its capabilities within their current practice. Some therapists have limited experience with AI and are open to its use, recognizing potential benefits such as increased work efficiency and reduced wait times. However, challenges in implementing AI were also identified, including personal barriers to learning, uncertainties about the perceptions of other healthcare professionals, and ethical concerns. While occupational therapists acknowledge the potential of AI to enhance their practice, they consider their therapeutic use of self and lived experiences as irreplaceable. Most believe that job opportunities will not be limited by the use of AI and instead it would enhance their practice. These findings provide valuable insights for future research and the development of AI technology in occupational therapy, contributing to the improvement of services. This study can be utilized by therapists, healthcare professionals, health management and policy stakeholders, and AI technology developers. Overall, the opinions of occupational therapists on AI expressed in this study are instrumental in enhancing the future use of AI in clinical practice, understanding its impact on the care provided to recipients, and identifying areas for further research.
Footnotes
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Dr. JS received funding from the Michael Smith Health Research BC (Scholar Award).
Supplemental Material
Supplemental material for this article is available online.
Author Biographies
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
