Abstract
Highly regulated industries such as healthcare can reap significant benefits from new digital technologies. However, due to institutional constraints, adopting such technologies is a slow and difficult process. Technology providers need to legitimize their underlying technologies to the customers and other stakeholders in the field. Drawing on multiple case studies in the healthcare industry, this article demonstrates how technology providers deploy two legitimizing practices: solution selling and issue selling. These activities lead to the emergence of open innovation ecosystems that help technology providers overcome adoption barriers.
Thus far, innovation research has mainly looked inside the organization to explain the adoption problem of radically new technologies. This literature has identified individuals’ and organizations’ reasons for internal resistance 7 and the contradictions and challenges involved in digital transformation. 8 However, new digital innovations do not typically emerge from inside the incumbent firm or organization. Instead, they are sourced from outside the firm through technology providers (e.g., tech startups or established firms) 9 who develop and introduce new technologies to customers and other external stakeholders, thus engaging in an open innovation (OI) process. OI refers to the processes that enable firms to source technologies externally, or commercialize internally developed technologies externally, thus leveraging external stakeholders to co-innovate beyond their boundaries. 10 Accordingly, the classic OI lens views OI as consisting of outside-in, inside-out, and coupled (combination of the previous two modes) innovation processes.
However, the classic OI lens cannot fully explain the digital technology adoption issues witnessed in highly regulated industries because it is mainly focused on knowledge exchange that occurs in inter-firm settings 11 or between firms and users in crowdsourcing contexts. 12 We also need to understand how external stakeholders (e.g., users, public authorities, professionals, and regulators) influence each other in the adoption of digital technologies. To this end, we adopt the broader open innovation ecosystem lens—a recent extension to the OI literature that also incorporates the outside-out innovation mode. 13 Outside-out innovation essentially means recognizing the role of external stakeholders, beyond the innovator or technology provider, who interact independently with each other, share knowledge, and co-create the processes relevant to the innovation adoption. While outside-out interactions are beyond the technology providers’ direct span of control, such dynamics can still be affected by a variety of legitimation activities that aim to make the new technology more plausible, comprehensible, and acceptable among the relevant stakeholders.
How do technology providers facilitate the legitimation and adoption of new digital innovations? We conducted an exploratory multiple-case study in the healthcare industry to uncover how technology providers not only offer new digital solutions but also build legitimacy for their underlying technologies, such as IoT and AI. We identify two important practices—solution selling and issue selling—that help technology providers legitimize new digital solutions in healthcare. Solution selling is a demonstration of the plausibility of the new technology by highlighting its practical value in terms of functional feasibility and economic viability of a given technological solution to customers. In contrast, issue selling focuses on gaining buy-in by building the comprehensibility and acceptance of the digital technology among both the customers and other stakeholders. We show how such issue selling—at both customer and field levels—can build trust and approval of the merits of the new digital technology and lead to cognitive and normative legitimacy among the adoption-side stakeholders.
Our findings suggest that it is not sufficient for managers of technology providers to merely focus on selling the functional utility of digital solutions; they must also concentrate on convincing and educating customer firms and wider stakeholders of the relevance, safety, and credibility of their underlying technologies. Our findings also integrate ecosystem thinking into OI studies, 14 advancing the notion of an open innovation ecosystem that highlights the role of outside-out innovation. 15 In contrast to previous studies that primarily examine B2C ecosystems, 16 our insights are applicable to B2B ecosystems that involve dominant industrial players in heavily regulated industries. 17
Conceptual Background
OI Challenge for Digital Technology Adoption in Highly Regulated Industries
Research has stressed the ongoing difficulties firms face in executing digital innovation, 18 especially when radical in nature. 19 Radical innovation is broadly defined as the novelty of the innovation across different dimensions, such as the novelty of the technology itself, the novelty of the innovation in the market, and also the novelty of the business model needed to utilize the technology. 20 The radical nature of innovation may lead to significant adoption barriers, especially among the external stakeholders involved in OI. 21 Thus, an important step in overcoming this OI challenge is to enhance the perceived legitimacy of the technology solutions, that is, their plausibility, credibility, and acceptability in the eyes of the relevant stakeholders. 22 Attaining technology legitimacy is critical, and yet challenging as stakeholders often have concerns over the uncertainty, viability, and ambiguity surrounding radical innovation. 23 This is especially the case in highly regulated industries where existing rules, norms, and belief systems are institutionalized, 24 and hence the adoption of a novel technology might require changes to socio-technical systems. 25 There is thus a particular need to overcome the legitimacy gap between the status quo and the desired new digital innovations. However, overcoming this gap is a challenge for OI since the legitimation of a new solution requires efforts and buy-in not only from the technology provider, but from many other external stakeholders.
In practice, selling a digital solution to a large institutional customer, such as a healthcare district or hospital, initially follows the classic coupled innovation mode 26 where both inside-out and outside-in innovation takes place. However, such customers further rely on numerous important stakeholders within and around their organization and in their institutional environment—for instance, in healthcare, these may include hospital administration, individual doctors and other medical professionals, public sector administrators, regulators, health insurance companies, medical associations, and more. Therefore, “outside-out” innovation is also needed. Outside-out innovation represents a core tenet of the OI ecosystem lens 27 and broadens the outlook to relevant external stakeholders.
Traditionally, the concept of OI primarily focused on inside-out, coupled, and outside-in knowledge flows between organizations, as outlined by Enkel et al. 28 This conventional OI framework offered a straightforward perspective, explaining the innovation of new products or services as the exchange of knowledge between two organizations—an innovator and a benefactor—or the joint knowledge creation between two organizations. 29 The underlying assumption within this model was that the success of knowledge exchange or co-creation depended solely on the capabilities and intentions of the involved parties, the formal agreements they forged, and the trust they established in each other.
However, in highly regulated sectors, such as healthcare, framing the development of novel (digital) technology applications as knowledge flows between just two organizations does not cover all the relevant stakeholders. In fact, successful innovation in such settings is not solely reliant on how OI partners interact with each other; it is significantly influenced by other institutional stakeholders who decide on crucial aspects essential for innovation success. 30 For example, the successful introduction of digital healthcare innovations depends not only on the innovativeness of technology providers and their collaboration with clinicians and hospitals but also on various external stakeholders, such as public authorities, regulators, insurance companies, and financial service firms. These stakeholders can influence the removal of regulatory and legal barriers, the impact of insurance schemes, the efficiency of payment systems, the institutional willingness to experiment with innovative technologies, the ease of integrating digital services into existing digital infrastructure, and more. Thus, to account for these field-level stakeholders 31 in the OI process, the traditional OI framework must be expanded to include the outside-out mode of OI, 32 whereby knowledge flows occur outside the innovator firm’s boundaries but have a consequential impact on the firm.
As noted by Vanhaverbeke and Gilsing, 33 the outside-out perspective introduces new roles to the OI landscape beyond the innovator firm, including influencers, instigators, and orchestrators. These stakeholders may not be directly responsible for driving the innovation process, but they critically shape the broader context surrounding an innovation, which may be executed by another party. For example, technology providers and customers cannot single-handedly eliminate institutional barriers but instead must rely on external stakeholders to do so. Therefore, the traditional OI framework must evolve and incorporate the concept of OI ecosystems. This approach offers an expanded lens through which firms can manage their OI processes, taking into account not only the inter-firm dynamics, but also the interactions between the various types of stakeholders in the ecosystem. 34
In this study, we focus particularly on the role of technology providers in the healthcare industry and how such firms can navigate the challenge of building legitimacy in OI ecosystems with diverse stakeholders. These providers (and the managers working for them) need to communicate, sell, and deliver a variety of technology solutions to customer organizations, 35 and at the same time, convince other relevant stakeholders of the feasibility and credibility of their technology (e.g., in terms of functional features, safety, compliance). However, we lack nuanced insights into the deliberate actions they should undertake to legitimize digital technologies and implement OI. 36 This is of theoretical and practical relevance to understanding why the adoption of OI is likely to be heterogeneous. 37
Technology Legitimation in OI Ecosystems: Solution Selling and Issue Selling
There are two important dimensions for technology legitimation: selling the concrete benefits of the technology at a practical and operational level (i.e., demonstrating its practical value in terms of functional feasibility and economic viability to customers); and selling the benefits of adopting the new technology at a cognitive and strategic level (i.e., gaining trust, approval, and buy-in among a broader set of ecosystem stakeholders). Drawing on B2B marketing and strategic change literature, we label these two practices solution selling and issue selling.
First, solution selling relates to the efforts to concretize the value of the offered solutions, using different strategies to demonstrate how the solution could benefit the relevant stakeholders in the ecosystem, such as the customer firms or end users. 38 In the B2B literature, solution selling, and value-based selling are viewed as a practice that is inherently interactive and involves a joint iteration between members of the selling and the buying organizations. 39 In terms of selling new digital technology, technology providers use solution selling to concretize the practical value of the new technology to customers and end users. 40 Take, for instance, the case of remote-control devices in healthcare. These smart devices present significant advantages for patients, allowing them to stay at home instead of making regular visits to the hospital. Simultaneously, physicians benefit from more regular and real-time patient monitoring, and they can also allocate more time to in-person visits in the hospital. Additionally, hospitals can treat a greater number of patients more cost-effectively. Selling such solutions requires meetings, demonstrations, and concrete iteration of use cases between the technology provider and the potential users to jointly curate the practical features and benefits of the technological solution to enhance its functional feasibility and economic viability.
Second, issue selling is defined as a strategic process with the purpose of “selling” change in the organization through the cognitive processes of sensemaking and sensegiving that occur in everyday interactions with organizational members. 41 While researchers examining strategic change have established that issue selling is undertaken, only limited research has studied the practices or “moves” 42 that managers use to achieve issue selling. For example, healthcare providers may initially be hesitant to embrace remote monitoring devices. Their concerns often revolve around trusting and validating these digital devices as reliable medical tools, understanding how they integrate into their medical practices, and considering the need to acquire new skills and the potential effects on their income, position, or authority within the hospital. Issue selling also addresses the myriad considerations that influence the acceptance of digital technology among public authorities and regulators in healthcare. 43
Solution selling and issue selling are parallel yet different practices. Unlike solution selling, 44 which is focused on conveying the concrete benefits of the new technology, issue selling is aimed at convincing the customers and other stakeholders in the ecosystem of the benefits of supporting the adoption of the new technology. 45 While the solution is a concrete display of functional value to customers, issues are more perceptional and socially constructed in the interactions that take place over a prolonged period and with multiple stakeholders. 46
Research Design and Method
We adopted a multiple-case study approach to investigate the introduction of radically new technologies. The healthcare industry is not only highly regulated, 47 but it is also complex and heterogeneous. 48 These industry features lead to barriers that incumbent organizations face in the adoption of digital solutions. Therefore, this setting forms a relevant context for our research.
Data Collection
We collected and analyzed data in three phases over 41 months. Our dataset came from three sources: 49 semi-structured interviews with informants from digital technology providers, healthcare providers, payers, and consultants; archival data such as webinars, press releases, online speeches of managers, articles, business publications, and presentation files; and informal discussions and follow-up conversations. In this process, particular attention was paid to fulfilling the criteria of transparency and systematicity. 49
The first phase of six exploratory interviews with healthcare experts uncovered barriers to digital technology adoption and its disruptive potential. Phase two involved 35 semi-structured interviews with 33 informants from 30 organizations, with a deeper focus on the digital solution development, adoption barriers, and stakeholders involved. The deliberate efforts of technology providers to address adoption barriers emerged as a key insight in this phase. During the third phase of the data collection, we used purposeful sampling 50 to select six technology providers among the previously interviewed ones as potentially most informative for our research question. Our sample is based on three main characteristics. First, all six firms provided radically new digital healthcare solutions in the same national context (Belgium), controlling for key potential institutional confounds. Second, with a balanced range of different firm sizes, our sample was not biased toward either large organizations or startups. Despite their varying sizes, all technology providers in our sample dealt with relatively similar adoption barriers from a range of healthcare stakeholders. Third, our informants primarily consisted of managers who faced the necessity of overcoming such adoption barriers, as they were directly responsible for digital technology solution sales and implementation in healthcare, such as business development, client engagement, and sales management. These interviews, complemented by those with customers (professional users of the technology), validated previous findings and helped gain deeper insights into the legitimacy-building efforts of technology providers. Table 1 provides an overview of our case firms: their digital technology solution, what makes the solution radical, and the key stakeholders in the emerging OI ecosystems.
Case Firm Description.
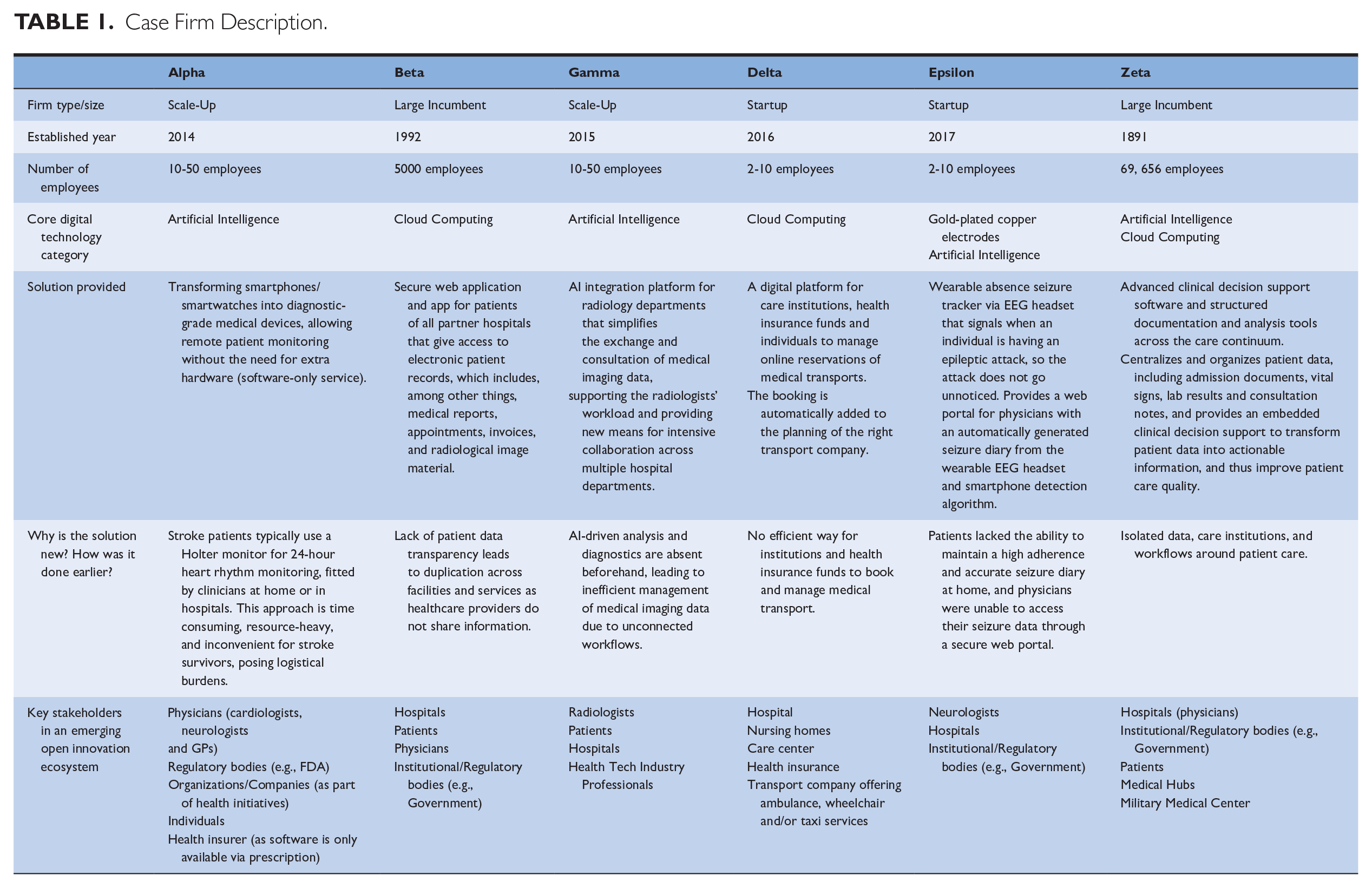
All interviews were recorded and transcribed. Collecting the data in three phases over 41 months increased accuracy. Although our level of analysis is the technology provider, we incorporated a range of stakeholder perspectives 51 to help with holistic understanding and triangulation of insights, ensuring the internal validity of our research. Several interview techniques (e.g., event tracking and non-directive questioning) were used to yield accurate information from informants. 52 In addition, highly knowledgeable industry experts were used as independent data sources. Archival data such as articles, web page captures, analyst reports, and business publications complemented our interviews. These enabled us to better understand digital healthcare applications and get different perspectives on the adoption challenges. The use of multiple data sources also helped us address potential informant bias as we could triangulate real-time data with retrospective data from secondary sources. 53
Data Analysis
Our inductive case analysis involved multiple cycles of confrontation between literature and data analysis, as well as data analysis and data collection. The first round of coding helped us identify the stages of digital technology-centered OI and related barriers to adoption in healthcare. In iterating between data and theory to discern how our emergent insights could be grounded in extant research, 54 it emerged that technology providers play an active role in overcoming these adoption barriers. This led us to engage with the literature on B2B marketing and strategic change to code our data and decipher themes. 55 We then aggregated first-level themes into theoretical constructs, deciphering customer-focused solution selling, customer-focused issue selling, and field-level issue selling as practices deployed by technology providers. The next iteration of coding led us to introduce the classic conceptualization of legitimacy and its classification as pragmatic, cognitive, and normative legitimacy 56 and to unpack how technology providers legitimize digital technologies. 57 A key step in this analysis was to develop a narrative history of the six case firms and how they overcame barriers to adoption. From this, we developed our final theoretical framework (see Figure 1).
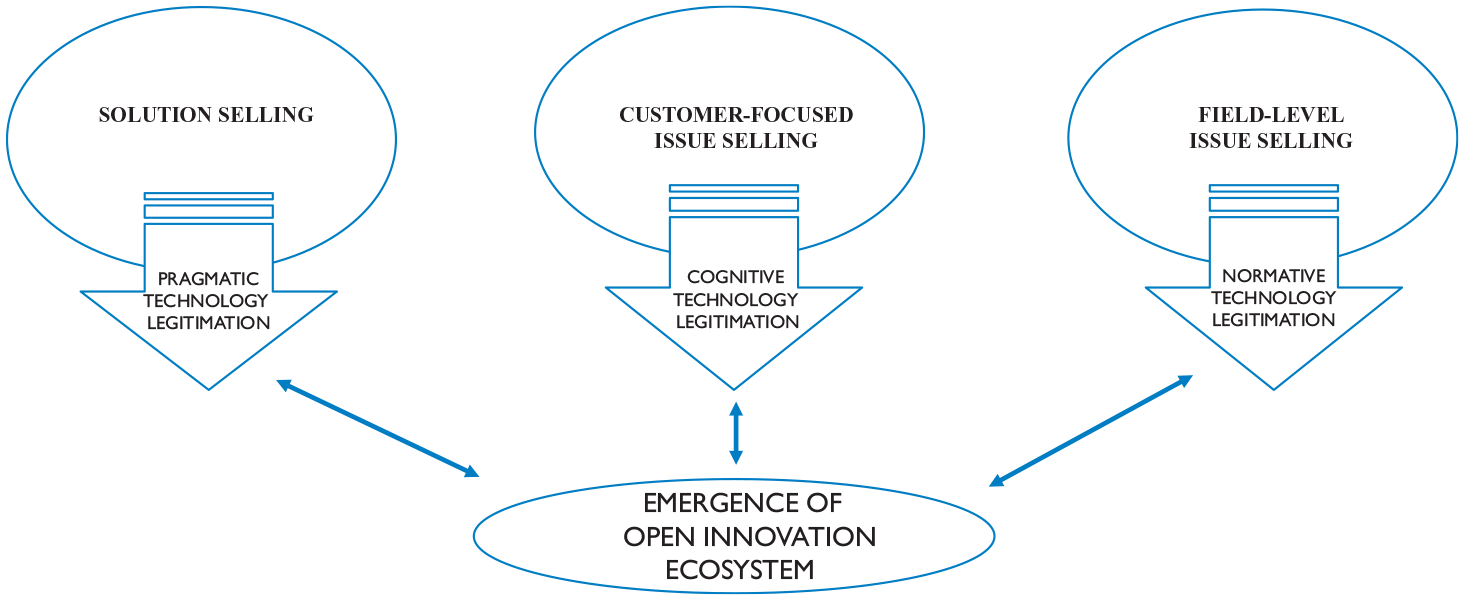
Practices for digital technology legitimation.
Findings
Our findings uncover three practices technology providers use in driving digital technology legitimacy: solution selling, customer-focused issue selling, and field-level issue selling.
Solution Selling and Pragmatic Technology Legitimation
The legitimation process starts with solution selling to the customer organizations. As part of this process, technology providers worked closely with the customer to co-create the value related to the solution. This ensured that technology providers could jointly curate the practical features and benefits of the technological solutions with the customer firms or end users, and that the solutions could practically benefit these stakeholders in the ecosystem, resulting in what we term pragmatic technology legitimation.
Solution selling was often deployed through pilot projects to identify and refine the solutions together with the customers and, eventually, co-develop the digital value proposition. In some cases, the providers also co-developed use cases and minimum viable products together with professional users (e.g., clinicians, nurses, or radiologists). For example, Alpha turns smartphones and smartwatches into diagnostic-grade medical devices to allow remote patient monitoring. It co-developed digital solutions based on this technology with customer teams of professional users and domain experts, with IT developers, and with logistics and analyst team members. They were asked about problems they had or how to solve those problems. Alpha had dedicated implementation specialists: “The gateway person [who] collects that information, [takes it] to the product manager and makes sure that we can implement these learnings we have had.” An Alpha customer confirmed the usefulness of this process in developing effective use cases, highlighting that “it will take at least six months to a year to come up with an ideal [use case] from the idea to implementation,” Overall, this approach helped technology providers develop a “long-term relationship with customers.”
Beta, which developed an application for partner hospitals to access consolidated electronic medical records, has around 40 working groups of multidisciplinary teams from different hospitals who focus on specific domains such as radiology, intensive care, or emergency room. In workshops, applying agile methodologies in experimental and iterative ways, these working groups were asked what “the main requirements are in the software to make a minimum viable product and proof of concept.”
A Beta manager elaborated: We always first show [customers] the [technology] roadmap [for] setting the scene. And then we show them the new functionalities on the roadmap. So, we get direct feedback: Okay, I see that you’re going that way, but maybe it’s better to go that way. So, we can adapt to that. (Beta)
Beta engaged in different project-based working groups with customers at different maturity levels in their digital transformation journey. In these working groups, some “mature users” asked “a lot of questions about what is on the [technology] roadmap” and shared ideas on “what is to change,” while others “come just to listen to the functionalities” or to “learn from those working groups.” As a Beta manager further explained: We did [a] sprint every two weeks with our customers, where we showed them a demo of the new functionalities [and] asked for input . . . We go very deep into the functionalities, and most of the time, we do it with two or three hospitals. In this working group, [we] ask for feedback . . . they tell us the [digitalization] process in their hospital. Show us the papers that they’re using so we can get [them] matched to a digital license. (Beta)
This customer-centric process led to concrete changes to the functionalities based on customers’ needs. Beta’s manager explained that they used to develop solutions without customer consultation but changed the approach after they realized the importance of achieving fit with the customer’s problem, rather than focusing solely on technology: [Now] we get a lot of information in the working groups. So, we can see what’s new and what can we use from the new developments. You have the opportunity to talk directly to the [customer] teams. We take everything into account before we start developing, and [customers] really like that—that they can give their inputs. (Beta)
Another company, Gamma, an AI integration platform for radiology departments, followed a similar approach. Once the technology was incorporated among professional users, feedback was gathered from nearly a thousand radiologists. A customer of Gamma explained the critical role of technology providers in this process, emphasizing the experimental approach where specific use cases are developed to address significant problems. Pilots are then conducted based on these use cases, overseen by a project manager who communicates with various stakeholders including radiologists, healthcare providers, data privacy officers, and the IT department of the hospital. Another customer concurred, adding that this needs to be an ongoing and iterative process: To give feedback about the solution, we communicate with [the providers], we tell them, “Okay, this is not working well,” or “[this is] making too many errors,” or “there are too many delays.” So, there will always be a relationship with the vendor because they need our feedback. The process never stops. It’s a long-term process. (Professional user/customer of Gamma)
Offering an example, the same customer raised the concern that a technology solution utilized for analyzing CT scans may face compatibility issues when integrating with a new scanner. Therefore, solution selling is also about monitoring and verifying such compatibility to ensure that the solution maintains its effectiveness over time. This highlights the importance of considering long-term relevance beyond initial solution implementation. Thus, solution selling enhances the practical, pragmatic, and operational value of the digital technology, developing the functional feasibility and economic viability of the technology solution. When this is accomplished, solution selling leads to pragmatic technology legitimation.
Customer-Focused Issue Selling and Cognitive Technology Legitimation
Besides solution selling, technology providers also deploy customer-focused issue selling—a strategic process to sell the benefits of adopting the new technology. This helps build credibility and buy-in for the technology among customers, resulting in cognitive technology legitimation.
For example, Alpha’s software turns consumer-grade digital devices (e.g., smartphones or smartwatches) into medical instruments, allowing remote patient monitoring without the need for extra hardware. An Alpha manager highlighted the need for issue selling, especially to professional users: It doesn’t mean that if [a technology] is available, [it] will be used, and that’s an interesting learning we had. So, the credibility of what we’re doing is still a barrier. (Alpha)
This lack of credibility poses a particularly challenging adoption barrier for Alpha’s radically new digital technology, a software that makes a diagnosis using a signal that is yet unknown to physicians. Alpha’s manager explained: When you are a cardiologist, you will have been trained during your entire education to use a particular signal for electrocardiograms, and [you] know how to read this. This is like a signal that actually explains what goes wrong in the heart. And they’ve never ever heard of a photoplethysmogram (or PPG signal). And since these people have a specific vision of this technology, they will say, “Sorry, it is not the same.” It doesn’t mean that it doesn’t perform as well, but it’s not the same for them. So, what we’ve mainly had to overcome is to find the credibility on the healthcare professional side. (Alpha)
To overcome this resistance among professional users (e.g., doctors, nurses, radiologists), technology providers framed the new digital technology as a complement to their existing competence and expertise. By signaling a synergistic approach, the technology providers safeguarded against immediate resistance from customers.
58
One approach was to allow professional experts to actively reflect on how the technology could augment rather than displace or substitute the work conducted by them. Alpha’s manager described disseminating education as a required pre-phase and a “convincing step,” emphasizing that [the physicians] are completely unaware of what the technology is and what it is capable of doing. We have to invest in education to make them aware of how to look at [the technology]. That is the next discussion to have: understanding where the data does [create] value.
As part of this issue selling, Alpha started the Alpha Academy, “where we are really investing in making sure we train photophysiologists and actually put in a different framing perspective.” This involved unlearning the current practices of professional users and then relearning what they could do with Alpha’s technology, which helped create awareness that the professionals’ own knowledge and judgment can be augmented by the technology or data-based claims (e.g., AI/ML-powered diagnosis). 59 Thanks to this, Alpha’s manager opined, “We can start having much more inflection.”
Another approach that technology providers adopted was to strategically withhold radical functionality of their technologies to prevent the professional users from feeling threatened in their expertise and role. At the same time, they also promoted desirable aspects of the technology. 60 They did this by demonstrating the compatibility of the digital innovation with the strategic goals of the customer organizations. A manager at Epsilon outlined how they approached this with prospective customers. They highlighted the typical delays associated with obtaining medical devices due to limited availability. They then contrasted those delays with Epsilon’s new technology, a software solution accessible via smartphones, which can significantly reduce waiting lists in hospitals, streamline efficiency, and decrease costs compared to physical devices, leading to increased operational margins for hospitals.
Framing an issue convincingly requires in-depth knowledge of the customers and their priorities to make appropriate choices. As Alpha’s manager said: “It’s really knowing the business of your customers. You have to talk to your customers and know the different layers of your customers.” A senior manager at Beta clarified their approach, highlighting their use of a customer advisory board where senior managers from five customers convened annually for two days for strategic discussions on the financial interests of hospitals and patient safety. This approach allowed Beta to align its lower-level working groups with the hospitals’ strategic objectives and adapt solutions accordingly. Moreover, this enabled them to showcase to customers how their technology roadmap would address strategic goals in the upcoming years, emphasizing the importance of this issue-selling practice.
A third approach technology providers deployed was to help doctors and other professionals deal with the changes in their roles and workflow, alleviating their potential worries about how the technology would work in their everyday practice. As Alpha’s senior manager described: There’s no one size fits all. Healthcare needs to be tailor-made. The moment technology starts to ask for effort and time, that’s the moment that your technology will start to fail. You can make sure that [it] is not a burden but actually a relief for them. So, this [sales] person is actually interacting with the nurses [and] also the physicians to make sure they want to work with [the technology] because [the technology] should fit seamlessly in[to] their workflow. (Alpha)
To facilitate such issue selling, Alpha used a clinical implementation specialist as a “configurator.” One service that Alpha developed through this process is pre-analyzing both machine-processed and human-processed data by their technicians. This approach aimed to facilitate a smooth and augmented workflow for their customers, guiding them through the learning-by-doing approach with the goal of minimizing barriers to adoption. Gamma’s manager reiterated that such issue-selling practices helped professional users (who are often the “gatekeepers”) deal with the opacity and complexity of digital technologies and reconcile the threat to their professional expertise: The moment [the healthcare professional] can start trusting the technology, I would say we can tick that box. That’s an important one. (Gamma)
Zeta, which developed an advanced clinical decision support software, also partnered with its customers to ensure that the technology would work for them and that they could confidently use the new functionalities. Notably, the customer perceived similar benefits, as “they know that it will make their operation more efficient. It saves them time. . .it makes their life easier.”
Overall, the variety of customer-focused issue-selling practices helped demystify the technology and improve its credibility among customers, leading to cognitive technology legitimation. 61
Field-Level Issue Selling and Normative Technology Legitimation
In addition to customer-focused issue selling, digital providers also promoted wider acceptance of the technology among different field-level stakeholders 62 through field-level issue selling. This resulted in what we label normative technology legitimation.
One approach was to create coalitions and communities of supporters to steer a core agenda and enhance its impact. For example, technology providers targeted professional associations, such as radiological societies and other scientific societies, to advocate the benefits of digital technology and pursue a normative agenda around its ethical application in healthcare. The aim is to “trigger these societies to stimulate education in this domain” (Gamma). For example, Gamma’s manager collaborated with American radiological societies on an ethics-related publication, intending to generate interest in the subject. It brought stakeholders together to foster broader understanding and discussion on ethical questions within the field. Epsilon’s manager also articulated the benefits of “making a coalition with those stakeholders who have similar interests.” The same manager also spoke of working with patient organizations to capture patient data to benefit the healthcare ecosystem.
Another important approach was to facilitate partnerships to co-develop solutions with relevant market players, such as pharmaceutical or medtech companies, and “build something together that is seen as strategic” (Epsilon). Partnerships were also sought with insurance companies, which were seen as key complementors. As a Delta manager explained: “Especially in Europe, physicians don’t like to prescribe something that is a cost to the person with the condition. So, reimbursement is definitely very important.” Having “as many partnerships as possible” with market and non-market stakeholders was deemed essential, as were lobbying and having representatives in the right places.
Besides the formation of coalitions and partnerships, technology providers also focused on signaling the appropriateness of the new technology through multiple channels. The primary channel was to secure various regulatory approvals to ensure acceptance of their technology in the market. Indeed, Alpha’s manager emphasized that market access and commercialization of technologies should never be hindered by the lack of necessary approvals. Moreover, the manager highlighted the importance of technology providers actively participating in shaping field-specific norms and guidelines for long-term success. The company noted that physicians typically adhere to established guidelines, and being included in the development of new guidelines is crucial for gaining acceptance as a reputable reference in the field. Alpha has focused on adoption efforts, particularly in relation to atrial fibrillation guidelines expected in 2024, and it sees positive indications that its technology (app) will be recommended by the guidelines. Beta’s manager also explained how coalescing with standard-setting bodies enables adoption as the resulting standards mean “everybody talks the same language.”
Another channel was to build acceptance through collaboration with reputable institutions to convey institutional credibility. According to Epsilon’s manager, the clinical validation trial they initiated with a leading Children’s Hospital and an international University marked an important stride toward industry and market acceptance. Additionally, they noted the reputational benefit associated with partnerships with entities like living labs, research institutes, and pharmaceutical companies, which enhances connections and credibility.
A third channel was to use social media and networks of advocates for a cause. For example, Gamma managers talked about being on LinkedIn, attending conferences, and talking to friends and colleagues to give a certain issue greater exposure. Epsilon’s manager highlighted the importance of influential stakeholders: So many digital innovations or technology innovations. . .will come to market via sports idols [who] will wear them when going on to the court or going on to the fields. And therefore, youngsters will want to have the same devices in those forms. And it’s that awareness that solves the issue. (Epsilon)
Finally, some also used their own personal role and stature to signal appropriateness. For example, a Gamma customer (who was an early adopter of AI and also a visiting professor at a university) initiated topics for bachelor’s and master’s theses focused on AI in medicine. This was a proactive start to enhance physicians’ confidence and understanding of these technologies, as they will inevitably need to utilize them in their practice.
Overall, these different field-level issue-selling practices led to normative technology legitimation through the cumulative and mutually reinforcing acceptance of technology among different field-level gatekeepers such as regulators, key experts, communities, and other wider (non-)market stakeholders.
Technology Legitimation and the Emergence of OI Ecosystems
The multi-layered and multi-stakeholder process of technology legitimation facilitates the emergence of OI ecosystems. Ultimately, the adoption of a particular technology among ecosystem stakeholders creates mutually supportive synergies. 63
External stakeholders working collectively led to outside-out OI dynamics that promoted complementarities at an ecosystem level. For example, the manager from Zeta elaborated on how multiple hospitals utilized the digital innovation collectively to scale adoption. They emphasized the importance of local champions within each hospital forming partnerships with counterparts in other hospitals to facilitate joint efforts in implementing the technology. Additionally, Zeta highlighted their collaboration with a network of 28 hospitals, which worked together and pooled resources. They mentioned being approached by the chairman and staff director of this hospital group to discuss Zeta’s extensive healthcare digitalization initiatives.
Furthermore, a rural hospital network’s initiative to develop an app for physician-patient communication also delivered significant value. Zeta emphasized the benefits of joining forces with the network, noting that a recent agreement aimed at standardizing solutions and expediting processes offered mutual advantages for all parties. Thus, the advantages of outside-out dynamics are clear.
Furthermore, as Zeta observed, “You can become successful if and only if you have hospitals [and] insurers linking up as an ecosystem.” OI ecosystem complementarities also helped manage various adoption-side stakeholder requirements as in the case of patient reimbursements. As Delta’s manager explained, the health insurance funds are always linked to the government. The involvement of health insurance funds and government in-patient reimbursements meant that “you have multi-stakeholder management that needs to take place, which is quite complex in your sales cycle.” Zeta’s manager described the benefits of stakeholder synergy in outside-out OI: Any health insurance wants the same as [the technology provider] wants. They want the same as the hospitals want: digitalization of care and also to keep it affordable and to have the right care at the right place. So, we all embrace this model. And now it’s more about how you get it implemented. And we understand that we can’t do it alone. (Zeta) The message is clear: Come in our ecosystem, you can join. So that’s how I bring it together. Outcome related and also working together in an ecosystem [with adoption-side stakeholders]. (Zeta)
Beta’s manager also stated that stakeholders “are only doing [what] is complementary to what we are doing. What we now preach is that we want to be open.” For example, Beta initiated working groups bringing medical directors and data privacy officers of their customer hospitals together to address matters concerning ethics and patient safety that they are responsible for. By facilitating these discussions, Beta triggered the formation of coalitions to pursue a normative agenda around ethical conduct and regulatory issues in healthcare.
Furthermore, Delta’s manager highlighted the crucial role of coalitions across multiple institutional stakeholders, including regulators and professional associations, to “guide projects so that you can implement it on a hospital-wide level” (Delta). These allowed demand-side stakeholders to drive cumulative adoption through outside-out OI.
These findings illustrate the importance of outside-out OI, where stakeholders, who are not directly involved in developing digital innovations for the healthcare industry, are still crucial to mutually reinforce the legitimation and acceptance of these new digital innovations. Epsilon’s manager remarked that “there is interest from the market to find that [collective] solution that really helps us as an organization, but also the users.” Thus, leveraging outside-out OI to find a collective solution was not only valuable for technology providers, but also yielded benefits for the ecosystem as a whole.
Discussion and Implications
OI in highly regulated industries is very challenging, as rigid institutional structures, regulations, and practices hinder the adoption of new technologies. Our study in the healthcare industry reveals two practices—solution selling and issue selling—that help technology providers legitimize new digital technologies among customer organizations and relevant field-level stakeholders. Table 2 summarizes and further illustrates these key findings of the study.
Three Types of Technology Legitimation Practices.
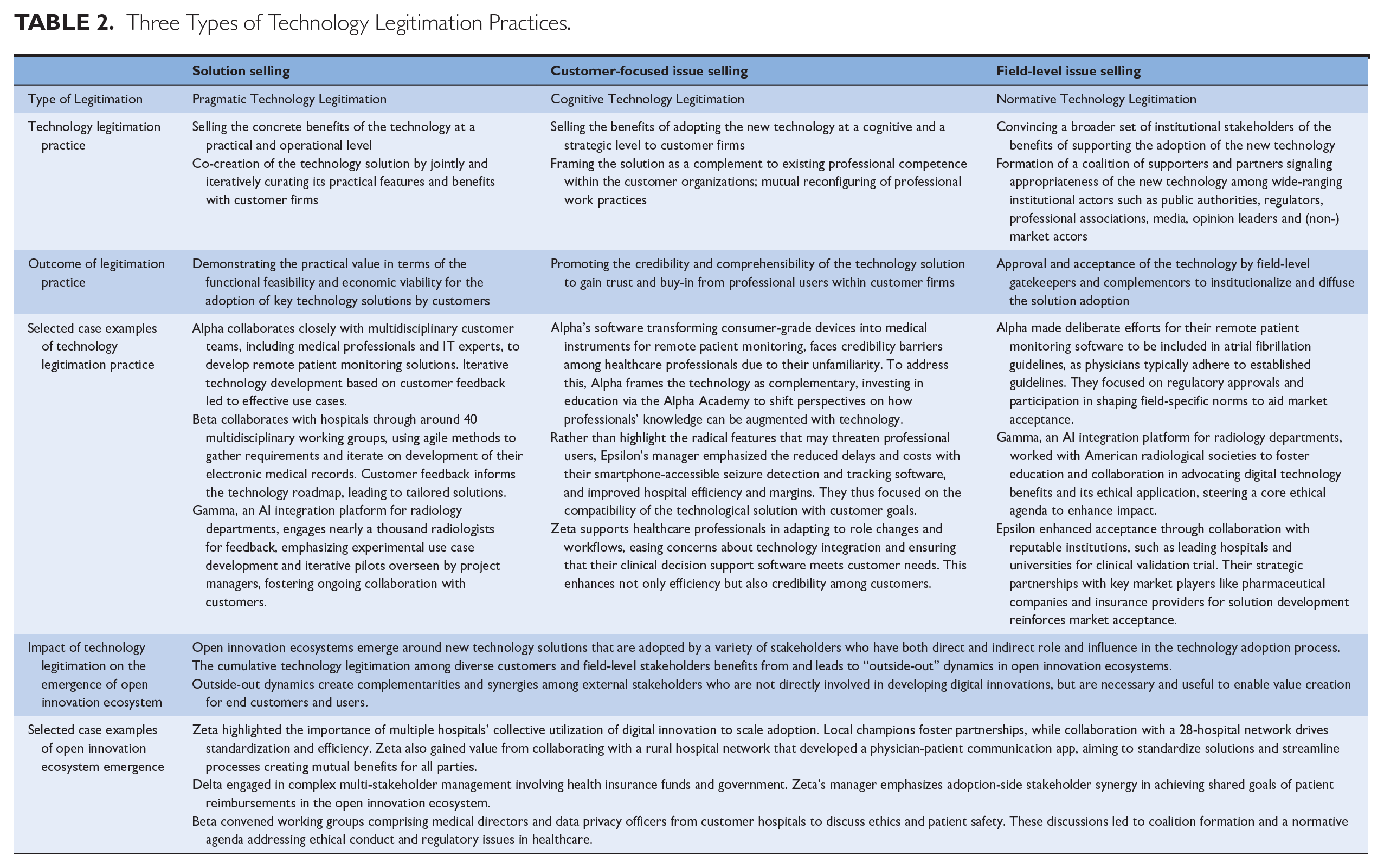
We show that while solution selling leads to pragmatic legitimacy, issue selling—at both customer and field levels—leads to cognitive and normative legitimacy, central concepts in the legitimacy literature. Importantly, we illustrate how technology legitimation with the customers and wider set of stakeholders plays a cumulative role in fostering an OI ecosystem around the new digital technology. Such ecosystems feature mutually supportive complementarities among stakeholders and align with the concept of outside-out knowledge flows relevant to OI processes.
Therefore, besides the classic and direct inbound and outbound dynamics, a comprehensive analysis of OI should consider how a diverse range of external stakeholders affect the focal innovation and technology legitimation, adopting a “wide lens” of OI ecosystems. 64 The OI ecosystem lens is particularly relevant in B2B ecosystem contexts, which involve complexities, multiple customers (including consumers and end users), and significant institutional considerations. Unlike existing research that has largely focused on B2C ecosystem orchestration, 65 our study examines the emergence of B2B digital ecosystems in which powerful industrial incumbents converge without a central orchestrator, especially in highly regulated industries. 66
Following are recommendations for practitioners in technology companies aiming to commercialize and diffuse novel digital technologies in highly regulated contexts. Table 3 shows how managers can engage in a technology legitimation process to overcome key adoption barriers in regulated industries.
Managerial Practices for Digital Technology Legitimation to Overcome Open Innovation Challenges.

Managerial Takeaway: In Engaging with Customers in Highly Regulated Industries, Technology Providers Must Combine Solution Selling with Issue Selling
Solution selling is a direct and transparent process where technology providers collaboratively shape the practical value, functional feasibility, and economic viability of digital solutions through ongoing interactions with customers. This iterative co-creation ensures that customer firms grasp the operational advantages of digital technology solutions tailored for specific tasks. However, healthcare providers often perceive digital technologies as novel, potentially disruptive, and threatening, with ramifications for professional workflows, business processes, and skill acquisition.
For example, in the integration of AI into digital imaging, the introduction of the new technology not only alters the workflow of radiologists, but also significantly impacts diagnostics and treatment recommendations for patients. This necessitates a re-evaluation of the collaboration between radiologists and prescribing clinicians, which presents a challenge to a smooth transition in work practices. 67 Resistance may arise, particularly from prescribing physicians who might perceive a loss of autonomy or influence with AI integration into radiology practices. To address such challenges, technology providers must use customer-focused issue selling to bridge the legitimacy gap. By collaborating closely with customers and articulating the core benefits of their technology offerings, technology providers ensure that their solutions are trusted, understood, and perceived as useful by customer firms.
Technology providers must actively engage in issue selling not only with customers, but also with a broader set of stakeholders in the field. This involves influencing and building acceptance among external stakeholders such as government regulators, professional associations, and insurers. The process begins by establishing the suitability of the digital solution within the given regulatory context, followed by forming a coalition of various stakeholders to influence (rather than impose) a broader agenda. This approach creates alignment among stakeholders toward a collective value proposition that emphasizes value creation for the users beyond just commercial interests.
A concrete example is the Belgian reimbursement scheme implemented in 2021. It enables patients to be reimbursed for using new mobile health apps. The validation process, represented by a “validation pyramid,” allows for the early reimbursement of patients’ telemedicine purchases. 68 Without the coordinated efforts of multiple stakeholders, mobile health services would remain unreimbursed, rendering digital applications unviable for patients due to their high costs.
Policy Takeaway: Policymakers Are in a Key Position to Facilitate Digital Healthcare Solutions and Reduce Barriers to Adoption, and This Requires Collaboration with Ecosystem Stakeholders
Governments and other public authorities are key enablers of digital healthcare since they have the power to level the playing field by dismantling regulatory and financial barriers entrenched in institutional practices. By streamlining legal and regulatory frameworks, public authorities can create an environment conducive to innovation and adoption of healthcare technologies. For this to happen, the digital readiness of public authorities themselves is necessary. Such readiness differs across governments, regions, and sectors so it is important for public authorities to not only share best practices, standards, and regulations among each other, but also to engage in co-creative policy work with technology providers, hospitals, healthcare providers, and other private sector stakeholders.
In fact, our key practical recommendation for public authorities is active engagement with technology providers and other stakeholders to understand the benefits and challenges of digital healthcare adoption. By fostering collaboration and coalition-building efforts, while also making sure that the developed technologies follow the relevant standards and safety regulations, public authorities can create synergies that facilitate the acceptance and diffusion of digital solutions. Furthermore, in addition to supporting the technology development and adoption among different firms and organizations, policymakers can create incentives and support for scaling up solutions for digital healthcare among end users.
Footnotes
Funding
The author(s) received financial support for the research, authorship, and/or publication of this article: This research was funded partially by the Australian Government through the Australian Research Council (ARC). Professor Krithika Randhawa is the recipient of an ARC Discovery Early Career Award DE240101364 funded by the Australian Government.
Notes
Author Biographies
Krithika Randhawa is an Associate Professor of Strategy, Innovation, and Entrepreneurship and ARC Research Fellow at the Business School at the University of Sydney, Australia (email:
Wim Vanhaverbeke is a Professor of Digital Strategy and Innovation at the University of Antwerp. (email:
Paavo Ritala is a Professor of Strategy and Innovation at LUT Business School, Finland. (email:
