Abstract
Globally, youth mental health services are evolving, with Australia’s
Many countries, including Australia, are engaged in building new models of youth mental health care (McGorry et al., 2022, 2024). These are appropriate responses to the epidemiology of adolescent-onset mental disorders (McGrath et al., 2023), and they reflect global recognition of the long-term neglect of indicated prevention, early intervention and secondary prevention by traditional mental health services in this age group (McGorry et al., 2022, 2024; Uhlhaas et al., 2023).
Australia is at the forefront of these new models due largely to the pioneering work from Orygen, the National Centre of Excellence in Youth Mental Health (McGorry et al., 2022; Uhlhaas et al., 2023). In the 1990s, Orygen developed and evaluated early intervention for first-episode psychosis (McGorry et al., 2002, 2008). This led to the global transformation and revitalisation of early intervention services for young people with emerging and first episodes of psychosis (Uhlhaas et al., 2023).
In 2007, with the establishment of
As of 2020, 16% of Australians (4.1 million individuals) were aged 12–24 years, with the most recent evidence indicating that 39% of those aged 16–24 years had a 12-month mental disorder (Australian Bureau of Statistics, 2023), up from 26% in 2007 (Australian Bureau of Statistics, 2008). Correspondingly, in 2021, 32% of youth aged 12–24 years received a Medicare-subsidised mental health service (this includes general medical and specialist psychological and psychiatric services), up from 28% in 2019. In addition, state-based mental health expenditure on youth aged 16–24 (largely hospital-based) has grown substantially in recent years ($3.64 per capita in 2010–2011 to $43 per capita in 2019–2020), with emergency department (ED) presentations for 18–24 year olds now reaching 209.3/10,000 in 2019–2020 compared with 121.61 for all ages. So, as psychological distress among young people continues to rise, and the demand for mental health services continues to grow rapidly, providing equitable and affordable access to high-quality care is increasingly challenging. These trends are clear in Australia, and globally (McGorry et al., 2024).
Given the emphasis in Australia on increasing access through enhanced primary care-based mental health services, the aim of this article is to present a variety of data sources, and analytic approaches, that report the differing demographic characteristics, clinical features and functional outcomes of young people who present across the network of
headspace as the national primary care platform for youth mental health services
The original intentions of
develop a national network of enhanced primary care-based mental health services that could provide diagnostic assessment and a clear pathway to the range of medical and psychological services relevant to early stages of anxiety and depression;
facilitate access to appropriate specialist or emergency care for those with more advanced, complex or enduring mood or psychotic disorders, through appropriate partnerships with local state-funded or Medicare-supported services;
facilitate access to other health services for young people, notably for sexual health and alcohol and other substance misuse; and
link young people to appropriate education, employment, training and other relevant psychosocial or welfare services.
Enacting this last point was never going to be easy given Australia’s historic lack of investment in psychosocial services (i.e. funding being at around 6% of total mental health expenditure) (Rosenberg and Harvey, 2021). Prior to
While other networks of alcohol and substance misuse and sexual health services existed, many lacked capacity for mental health assessment or interventions for young people.
headspace national reporting of who attends, clinical characteristics, services delivered and outcomes achieved
The development of regionally based
The most recent independent review, published in June 2022 by KPMG (2022), notes that
Of all episodes of care, 36% entail just a single occasion of service, and only 19% are associated with six or more occasions of service. This is consistent with the emphasis on expanding access via the provision of very brief psychological support, rather than more comprehensive medical, psychological, sexual health, alcohol or drug or psychosocial services.
Regarding outcomes, the KPMG report describes a shift away from the initial clinical focus on early intervention and secondary prevention for the early stages of major mental disorders. It now lists alternative ‘intermediate outcomes’ including increased mental health literacy, increased early help-seeking, increased access to required services and a focus on delivering each of these outcomes for ‘hard-to-reach’ groups (Aboriginal or Torres Strait Islander, culturally and linguistically diverse, LGBTQIA+, those with disability). These ‘intermediate outcomes’ are then differentiated from service system outcomes (e.g. advocacy, reducing stigma, improving care pathways), user experience outcomes (e.g. culturally appropriate and inclusive, family support, youth participation) and psychosocial outcomes (e.g. improving mental health and wellbeing, considering clinical outcomes and improving psychosocial outcomes).
The report concludes that these intermediate goals (e.g. improved mental health literacy) have been achieved to varying degrees. However, key challenges remain for achieving effectiveness in area-level outcomes, managing wait times, connecting with ‘hard-to-reach’ groups, connecting with the wider mental health service systems or achieving reliable or clinically significant improvements in most clients. Importantly the report concludes that ‘
Elsewhere in the same report, there is the following statement ‘
The headspace national data set: cross-sectional and longitudinal reports
There are several academic reports of the
In the most comprehensive data now available on 58,223 clients, 23.57% are reported to have no significant psychological symptoms and no risk factors, and a further 25.64% are reported to have risk factors only (Rickwood et al., 2023). This means that
Of the presenting psychological symptoms (reported in
By contrast, another academic report on 76,021 individuals accessing 113 different services in 2018–2019 has recently appeared (Gao et al., 2024). It provides a somewhat different perspective on the needs of those who attend, while also suggesting that there may be important differences between sites. Over 50% of persons were rated as having very high levels of distress (Kessler Psychological Distress Scale [K10] >30) and 46% had significantly impaired function (Social and Occupational Functioning Assessment Scale [SOFAS] <61). Using a data-driven approach, the authors conclude that at least 60% of attendees have at least moderate levels of complexity, with 20% being rated as highly complex. However, the dataset on which these analyses were based has limitations, particularly with regard to the extent that they relied on ratings of clinical staging and formal diagnoses by site staff.
Instruction to staff by
On the basis of the complexity score developed by Gao et al. (2024), the proportion of youth rated as having low complexity (for whom a brief intervention or indicated prevention approach may be most appropriate) was recognised as 40% (range: 21–64% across centres), meaning that 60% had more complex needs (range: 36–79%) and were likely to require more substantive clinical interventions. This estimate (but not the range) is consistent with earlier work by the BMC group (Capon et al., 2023a) which also used an empirically based approach, and found that 49% of attendees had more complex needs, while another 27% were in need of significant early intervention. Using a standardised and reliable data collection method, we have estimated the range across
The longitudinal data reported by
Those followed in the short-term comprised 38% (22,349 of 58,223) of presenting clients. When considering how many had positive outcomes from service engagement, ‘reliable change’, indicative of ‘improvement’, was reported in 24.5% for psychological distress (self-reported K10), 29.9% for functioning (clinician-rated SOFAS) and 30.1% for self-reported quality of life (measured by
These data were interpreted as demonstrating the effectiveness of
The BMC experience and evidence from 2007 to 2022
Our first academically affiliated centre was established in Campbelltown in 2007 and the second in Central Sydney from 2012. From the outset, these centres have been committed to continuous reporting on who is seen at these sites, their demographic and clinical characteristics (Capon et al., 2023b; Hamilton et al., 2011; Scott et al., 2012) and their clinical and functional outcomes (Burton et al., 2022; Iorfino et al., 2022a; Scott et al., 2019). Consistent with the BMC Youth Model (Hickie et al., 2019), these centres have been supported by academic and more specialised infrastructure since their inception. In addition, the BMC has supported clinical training and data collection and analyses from other urban and regional centres (Capon et al., 2023a, 2023b). Consequently, compared with most other
While these data are distinct from that reported by
Key characteristics of Brain and Mind Centre and
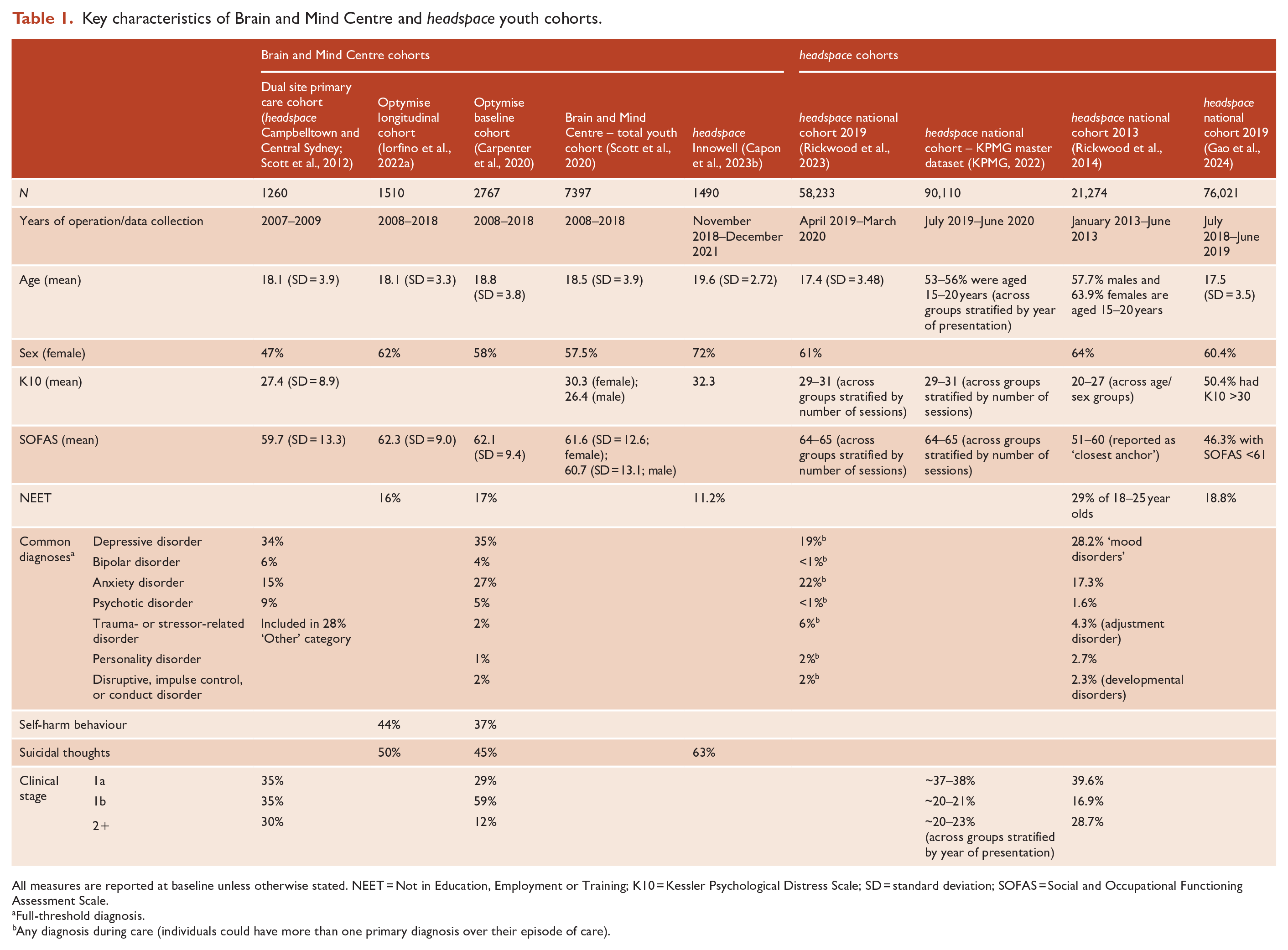
All measures are reported at baseline unless otherwise stated. NEET = Not in Education, Employment or Training; K10 = Kessler Psychological Distress Scale; SD = standard deviation; SOFAS = Social and Occupational Functioning Assessment Scale.
Full-threshold diagnosis.
Any diagnosis during care (individuals could have more than one primary diagnosis over their episode of care).
More recently, we have been able to access data directly from 11 other urban and regional sites. Generally, these non-academic sites are connecting with very similar cohorts, though with the trend towards regional sites having a higher proportion of younger clients and clients with more psychotic-like symptoms and risk of suicidal behaviour (Capon et al., 2023b). Interestingly, those from urban areas were more likely to have used other services previously and had higher rates of alcohol misuse.
Furthermore, it is clear that a large proportion of young people attending our centres do have formal diagnoses of anxiety, depression or other complex disorders, well-established functional impairment, and other neurocognitive impairments and neurodevelopmental difficulties (Crouse et al., 2020), elevated genetic risk for severe mood and psychotic disorders (Crouse et al., 2021) and prior presentations for care and experiences of other interventions (Table 1). Importantly, the data we have collected across various centres indicate that almost 50% of attendees have complex clinical needs (Capon et al., 2023a).
Longitudinal data sets and longer term multidimensional outcomes
Longer term data linkage studies have confirmed that this ‘early intervention’ youth cohort is at risk of premature death from all causes (notably suicide and accidents and injuries), with a five-times increased risk found for males and two-times increased risk for females (McHugh et al., 2023). In addition, over a 10-year follow-up period, the median number of presentations to state-based EDs for mental or physical health crises is three (Iorfino et al., 2023a). Almost a third (31%) had an ED presentation directly associated with mental illness or substance abuse. Furthermore, short-term studies of the brief interventions provided indicate that those with greater functional impairment do not improve to the same extent as those who present with little impairment (Cross et al., 2016).
In the most significant long-term study of those entering care through our
While there was significant individual variation in illness course in our long-term outcomes, several different trajectories were clear. These included early improvement followed by later deterioration, pre-existing impairment which does not change despite clinical interventions and pre-existing impairment which is then associated with progressive impairment. For two-thirds of this cohort, the brief psychological intervention model does not result in significant change to either illness course or functional outcomes. More recent work evaluating causal effects has demonstrated the importance of functional impairment as a direct and specific target for intervention with potential impacts not only on functioning, but also on suicide ideation, self-harm, suicide attempts and psychosis-like experiences (Iorfino et al., 2023b).
The use of clinical staging has been an important tool for understanding the risks of young people presenting to these services (Hickie et al., 2013). With regard to illness progression, 3% of those presenting as stage 1a as compared with 13% of those presenting as stage 1b (i.e. sub-threshold syndromes) progress to stage 2 (full threshold) of a major mood, psychotic or comorbid disorder (Iorfino et al., 2019). So, these cohorts likely contain a subgroup who are at significant risk of progression to major mental disorders.
The central notions of indicated prevention, or early intervention combined with secondary prevention, are that early access to effective strategies can reduce the transition rate from ‘sub-threshold’ or ‘early clinical stages’ to major mood or psychotic disorders. In our largest long-term cohort study (
In studies from this large youth cohort, we have detailed the extent to which physical illness or risk factors (notably metabolic dysfunction), as well as substance misuse, are not necessarily tied to clinical stage (meaning they often occur early in the course of illness; Capon et al., 2022; McKenna et al., 2024; Shin et al., 2024; Wilson et al., 2023). Further, some factors such as circadian disturbance and functional impairment are not only predictive of illness progression (Iorfino et al., 2019; Scott et al., 2022), but may also be a consequence of that progression (Capon et al., 2022). Altogether, this work illustrates the level of complexity already present among these cohorts.
Diverging narratives
Given the changing epidemiology of adolescent-onset mental disorders, the development of enhanced primary care-based ‘
As large-scale controlled trials of these new service platforms are unlikely, we must learn as much as possible about their effectiveness from systematic and detailed monitoring, as well as from selected but much more detailed evaluations (Hilferty et al., 2016; Muir et al., 2009). The data from the centres operated directly by the BMC, and affiliated networks, provide valuable insights that have not been readily available from the
It is a concern, however, that two diverging narratives have developed over the life of the
The
This narrative may well be appropriate for young people experiencing largely transient distress, with very low rates of clinical disorders, self-harm or suicidal ideation, physical ill-health, other comorbidities (e.g. abnormal eating behaviour) and little evidence of functional impairment, estimated by
The BMC narrative that emphasises the more significant needs of the majority of those attending
These more detailed analyses have major implications for the future design of youth mental health services. The BMC model of care places a much clearer focus on highly personalised and skilled assessment on entry to services, followed by measurement-based care. That is, it prioritises detailed clinical and multidimensional assessment to facilitate the delivery of a range of appropriate evidence-based psychological, psychosocial and medical interventions. This service delivery model is not tied to the traditional primary-secondary or specialist care divide, or simple stepped-care (or ‘fail-first’) models, but instead leverages infrastructure that supports an alternative ‘right care, first time’ care model (Hickie et al., 2019; Rosenberg et al., 2020). Such rapid access to appropriately coordinated specialist care is also more likely to deliver significant population-level benefits, in cost-effective ways, as compared with our current stepped-care models (Crosland et al., 2024; Skinner et al., 2023; Vacher et al., 2023).
When established in 2007,
Conclusion: ways forward
As the demand for more personalised and effective care options rises, and the limitations of a very narrow focus on low levels of complexity and indicated prevention rather than genuine early intervention and secondary prevention are recognised, a new range of service care models are urgently required. Much of the BMC-led clinical and population-based work has focused on the promotion of regionally focused service planning and the development of person-centred and organisationally relevant infrastructures to underpin effective triage, service prioritisation and short- and longer term tracking of clinical and functional outcomes (Crosland et al., 2024; Rosenberg et al., 2023). This requires the development of real partnerships with local youth and welfare services, maintaining and fostering clear partnerships with more specialised mental health services, so that a range of clinical and psychosocial needs can be met. Consequently, what we need is a national network of youth services that overtly respond to the unmet needs of young people in the early stages of major disorders, who already have moderate levels of clinical and psychosocial complexity. Providing early, effective, equitable, appropriate, evidence-based and affordable care to Australia’s young people surely ranks among our highest priorities for mental health reform.
Footnotes
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: IBH is the Co-Director, Health and Policy at the Brain and Mind Centre (BMC) University of Sydney. The BMC operates an early-intervention youth services at Camperdown under contract to
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The funders played no role in study design, data collection, analysis and interpretation of data, or the writing of this manuscript. IBH is supported by a NHMRC L3 Investigator Grant (GNT2016346). JJC is supported by an NHMRC Emerging Leadership Fellowship (GNT2008197). WC is supported by an Australian Government Research Training Program (RTP) Scholarship. FI was supported by the Bill and Patricia Richie Foundation and an NHMRC EL1 Investigator Grant (GNT2018157).
