Abstract

Access to timely and effective care is a primary goal for mental health services. However, chronic shortages in Australia’s psychiatric workforce continue to plague effective service provision. Current projections conservatively predict an alarming undersupply of 124 psychiatrists by 2030, with 43% of psychiatrists intending to retire in the next decade (Department of Health, 2017). The recruitment of overseas psychiatrists has long been used to fill these gaps, yet this remains an unsustainable long-term strategy. While the government’s recent AU$1 million investment into 30 new psychiatry training positions partly addresses these gaps, these additional positions will need to be matched with increased numbers of trainees. In this article, we describe factors that draw medical students and prevocational doctors into psychiatry and outline evidence-based recommendations that may increase overall recruitment numbers.
The decision to pursue psychiatry is made before, during or after medical school (Figure 1). A survey of 29,713 American medical students found that 50.2% of those who intended to pursue psychiatry when entering medical school maintained that choice by graduation (Goldenberg et al., 2017). In our experience, medical students and prevocational doctors are drawn to psychiatry by positive learning experiences and mentorship during their psychiatry term, comparatively better working conditions and involvement in extracurricular enrichment activities. However, one systematic review reported that students and doctors may be discouraged from psychiatry due to a perceived lack of evidence base for diagnoses, poor patient prognoses and a stigmatised image of psychiatry from the public and other specialties (Choudry and Farooq, 2017).
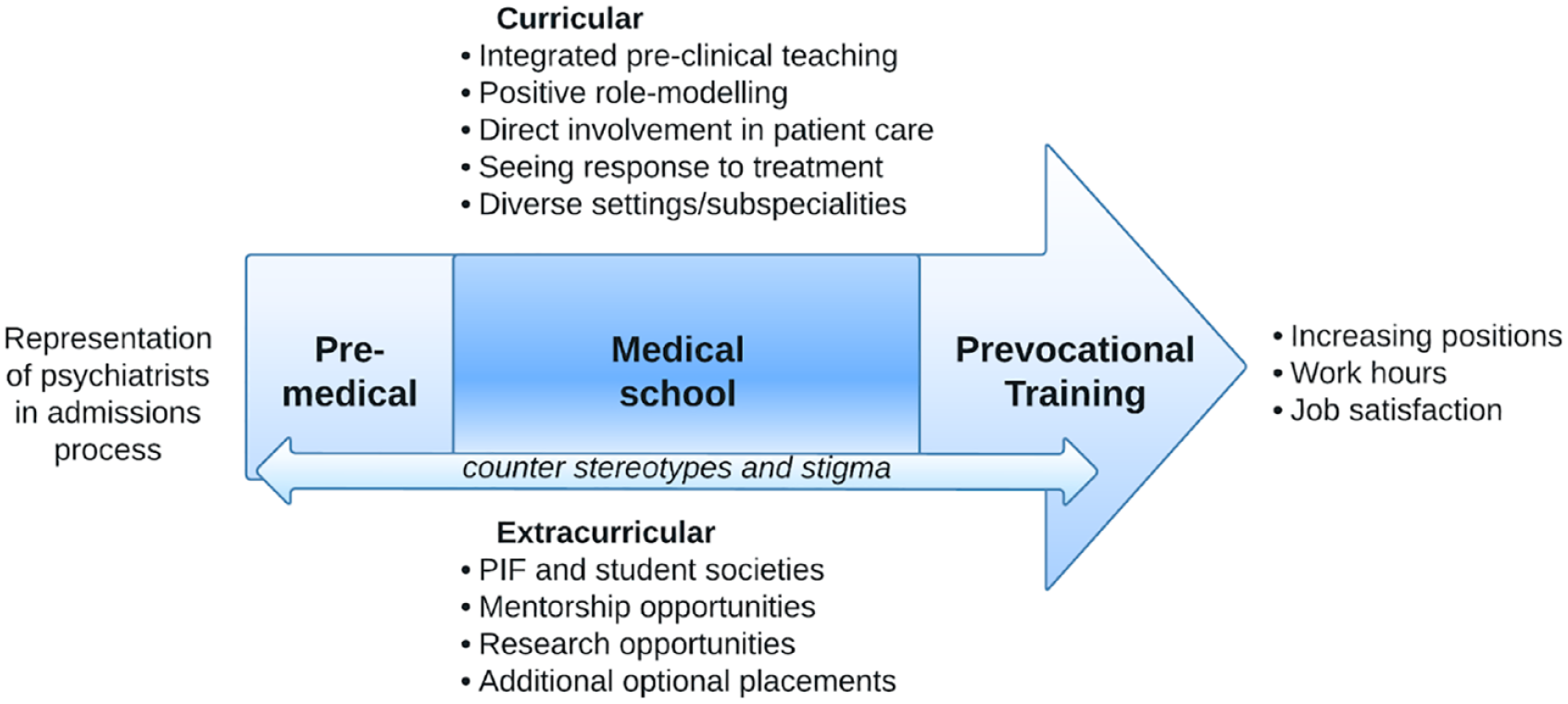
Increasing recruitment into psychiatry before, during and after medical school.
Strategies that improve recruitment in psychiatry must be informed by its drawing cards. From initial intake into medical school, psychiatrists should be appropriately represented in the interview and admission process to encourage selection of applicants with diverse backgrounds and educational interests (Goldenberg et al., 2017). During medical school, students should be introduced to psychiatry early in the curriculum alongside other specialties. Academic psychiatrists in leadership positions need to advocate for appropriate curricular changes that emphasise the morbidity of mental illness across the lifespan and highlight the relevance of psychiatry across all medical specialties. Given early experiences in psychiatry have been positively associated with interest in pursuing psychiatry (Lyons, 2017), we suggest integrating relevant modules such as basic psychiatric history-taking, behavioural science and neuroscience into the pre-clinical curriculum. Such modules may also identify students with an interest in psychiatry early on. These students should be offered formal or informal mentorship opportunities by academic psychiatrists or near peer-mentoring by registrars (Hewson et al., 2021).
Simultaneously, recruitment strategies must also address factors that dissuade medical students from pursuing psychiatry. Students may be deterred from psychiatry before commencing their psychiatry placement due to stigmatising attitudes about mental health from the public and other specialties. These attitudes must be acknowledged and challenged across the curriculum through further formal teaching or programmes such as Mental Health First Aid, which may reduce stigma by facilitating exposure to those with lived experience of mental illness. Acquiring a fundamental understanding of mental illness through early and in-depth exposure may allow students to consider psychiatry with a more open mind before beginning their placement.
During their placements, students should be given opportunities for direct involvement in patient care in diverse settings. Expanding placement opportunities to private and community mental health settings gives students more opportunities to find a subspecialty of interest. Given seeing patients respond to treatment has been cited as an important reason for pursuing psychiatry (Choudry and Farooq, 2017), providing exposure to settings where there are less restrictive modes of care and a stronger focus on recovery compared with acute public inpatient units may help increase interest and recruitment in psychiatry. During placement, students should also receive teaching from clinicians who are genuinely passionate about psychiatry and are able to convey the benefits of pursuing the specialty (Goldenberg et al., 2017). High-achieving and interested students identified on placement should be encouraged to pursue psychiatry and offered further opportunities to cultivate their interest.
Promoting extracurricular enrichment activities is another important avenue for increasing recruitment in psychiatry. The Royal Australian and New Zealand College of Psychiatrists (RANZCP) established the Psychiatry Interest Forum (PIF) in 2013 to improve recruitment, challenge common misconceptions and foster the interest of medical students and prevocational doctors into pursuing psychiatry. PIF initiatives are wide-ranging and have included career information sessions, essay competitions and conference scholarships. PIF also sponsors initiatives by student-run psychiatry interest societies. As of June 2022, 6409 medical students and prevocational doctors have become PIF members, with 79% of new psychiatry trainees in 2021 being previous PIF members (RANZCP, personal communication, 8 July 2022). Although a proportion of members may have joined PIF with clear vocational intentions to pursue psychiatry, in our experience, many join PIF to simply engage and learn more about the profession. PIF has been successful in promoting psychiatry and engaging those with interest in the field, and deserves further longitudinal evaluation to map its full impact on recruitment.
Longitudinal evaluations of faculty-led electives and summer schools have found that up to 70% of students attending these programmes ended up pursuing psychiatry training (Lyons, 2017). One component of these initiatives may include one-to-one mentoring programmes offered by trainees and consultants. This may provide benefits such as personalised career advice, information about working as a psychiatrist and additional placement or research opportunities to students considering psychiatry as a career (Hewson et al., 2021). An evaluation of a university-led mentoring scheme in the United Kingdom found that the programme had either increased or maintained interest in psychiatry across a vast majority of mentees (Hewson et al., 2021). However, further research must elucidate whether these initiatives translate into increased recruitment rates.
Those who decide to pursue psychiatry after graduating medical school may have fewer opportunities to gain exposure to psychiatry. Increasing the number of positions for prevocational doctors in psychiatry rotations would provide adequate clinical exposure, informal mentorship opportunities and a better picture of what working life in psychiatry may look like. Local health districts and programmes like PIF should also proactively advertise pathways into psychiatry and encourage prevocational doctors to apply for the training programme.
While numerous strategies have been suggested, there remain ongoing barriers to effective recruitment. Extracurricular and enrichment activities are mostly sought after by medical students already interested in psychiatry and do not adequately target all students. Increasing recruitment requires engaging students who may not have considered psychiatry at first or who remain undecided about their career pathway. Moreover, the pervasive stigma and stereotypes that have been associated with psychiatry for decades remain another barrier for effective recruitment. We believe sufficient exposure to mental health early on may provide enough academic context to understand the shortcomings of these stigmatising views. Unfortunately, existing medical curricula leaves little room for integrating further teaching into psychiatry. Part of the solution to this issue requires more academic psychiatrists in faculty positions to advocate for such changes.
In conclusion, Australia is projected to encounter a gross undersupply of psychiatrists over the next decade, which will require not only more training positions but also an increase in the number of trainees. Sustainable recruitment strategies begin with medical students and continue to prevocational doctors. Appropriate investment into implementing such reforms will effectively promote interest in mental health and ultimately recruit more psychiatrists in the future.
Footnotes
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship and/or publication of this article: T.P.N. and P.S. are both members of the RANZCP’s Psychiatry Interest Forum.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
