Abstract
Objective:
To assess the effects of psychological, psychosocial, educational and alternative interventions on mental health outcomes of Indigenous adult populations in Australia, Canada, New Zealand and the United States and the Indigenous involvement and content in each study.
Methods:
We systematically searched databases, key journals and gray literature, for records until June 2020. Eligible studies were in English or French and examined the impact of interventions on mental health outcomes including anxiety disorders, posttraumatic stress disorder, depression, psychological distress or stress for Indigenous adults (⩾16 years). Data were extracted using a modified Cochrane Data Extraction Form and the Template for Intervention Description and Replication. Quality was evaluated using the Effective Public Health Practice Project quality assessment form.
Results:
In total, 21 studies were eligible, comprising 8 randomized controlled trials, 10 single-group pre–post studies and 3 pre–post studies with comparison groups. Twenty studies had Indigenous individuals or organizations involved in some decision-making capacity, though extent of involvement varied widely. In total, 9 studies were rated moderate and 12 weak in the Effective Public Health Practice Project quality assessment. Eight studies measuring depression, three measuring posttraumatic stress disorder, three measuring psychological distress and two measuring stress showed statistically significant improvements following the intervention.
Conclusion:
A wide range of interventions demonstrated mental health improvements. However, it is difficult to draw generalizable conclusions on intervention effectiveness, given heterogeneity among studies. Studies should employ a thorough assessment of the Indigenous involvement and content of their interventions for reporting and for critical consideration of the implications of their research and whether they address Indigenous determinants of mental health.
Introduction
Indigenous peoples have been displaced from their ancestral lands (United Nations, 2009). Vital cultural connections to the land were and continue to be disrupted, creating ‘near total psychological, physical and financial dependency on the state’ (Alfred, 2009: 42), inhibiting Indigenous self-governance, as well as creating an experience of collective, historical and intergenerational trauma which contribute to adverse health outcomes (Alfred, 2009; Kirmayer et al., 2000; Nielsen and Robyn, 2003; O’Neill et al., 2018). Consequently, Indigenous populations in colonial states such as Canada, the United States, Australia and New Zealand often have disproportionately high rates of mental illnesses. Off-reserve First Nations and Métis populations have a higher prevalence of mood and anxiety disorders compared to non-Indigenous populations (Rotenberg, 2016; Statistics Canada, 2016) which has also been observed in American Indian and Alaska Native populations (Bassett et al., 2014; Beals et al., 2005). Māori adults in New Zealand also have a higher prevalence of anxiety and mood disorders and an increased likelihood of psychological distress compared to non-Māori adults (Baxter et al., 2006; Ministry of Health—Manatu Hauora, 2020a) similar to Aboriginal and Torres Strait Islander People in Australia (Calma et al., 2017; Markwick et al., 2014). In turn, calls for political changes have been made, including the return of Indigenous lands, self-determination, self-governance and community development for the improvement of mental, physical, spiritual health and the economic well-being of Indigenous peoples (Alfred, 2009; Kirmayer et al., 2000; Tuck and Yang, 2012).
Despite calls for structural changes to address root causes of mental health disparities between Indigenous and non-Indigenous populations (Australian Government, 2019; Ministry of Health—Manatu Hauora, 2020b; Public Health Agency of Canada, 2020; US Department of Health and Human Services, 2020), programs have focused on ameliorating individual symptoms using psychological, psychosocial, educational or alternative interventions. Such approaches to mental health have then been critiqued for their harmful colonial perspectives or cultural ‘inappropriateness’, so instead, culturally sensitive, culturally competent, to culturally safe approaches have been developed (Brascoupé and Waters, 2009; Curtis et al., 2019; Wilson et al., 2013). Furthermore, cultural healing and continuity, connection to land, inclusion of community strengths and leadership are known to be protective and promotive elements of mental health for Indigenous peoples (Auger, 2016; First Nations Health Authority, 2018; Kelly et al., 2009; MacDonald et al., 2013). As a wide array of mental health interventions exist, it is important to summarize information and identify strengths and limitations of current research to inform future program and intervention planning.
While existing systematic reviews have examined mental health interventions for Indigenous populations, the most recent publications in these reviews are from 2015 (Antonio and Chung-Do, 2015; Leske et al., 2016; Pollok et al., 2018; Pomerville et al., 2016). Furthermore, none have conducted an extensive assessment to examine Indigenous involvement and content. Therefore, our review examines (1) the effect of psychological, psychosocial, educational and alternative interventions on mental health outcomes for adult Indigenous populations and (2) the cultural content and Indigenous involvement in the research and intervention processes. Our review leads to a discussion on considerations for research on mental health interventions for Indigenous populations.
Methods
Information sources and search strategy
The Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines (Liberati et al., 2009) and the protocol (PROSPERO registration # CRD42018087994) were followed. A systematic search was conducted in MEDLINE, Embase, PsycINFO, CINAHL, Cochrane and Scopus as well as in the Bibliography of Native North Americans and Native Health Database. Gray literature was identified through Grey Matters and additional articles from a manual search of the International Journal of Indigenous Health, Journal of Indigenous Wellbeing, Journal of Indigenous Research, AlterNative: An International Journal of Indigenous Peoples and American Indian Quarterly. Controlled vocabulary was identified along with keywords to search for mental health outcomes of interest AND interventions AND Indigenous populations (Supplemental Table S1). After consulting a librarian, the search was completed on 1 June 2020.
Screening and eligibility
Covidence was used to screen titles and abstracts, and for the full-text review, successively. Screening was done independently by two reviewers, and conflicts were resolved by a third reviewer and through discussions. If the full text of an eligible abstract could not be located, its authors were contacted to confirm whether an article was published. If authors did not respond within 2 weeks, the abstract was excluded.
Titles and abstracts were excluded if they did not include (1) Indigenous people from Canada, the United States, New Zealand or Australia; (2) a mental health intervention; and (3) mental health outcome(s). Eligible studies for full-text screening were experimental, quasi-experimental or observational; written in English or French; and examined how an intervention impacted the following mental health outcomes: anxiety disorders, posttraumatic stress disorder (PTSD), depression, psychological distress or stress. If these studies also included general and strength-based mental health outcomes, these were extracted. Study participants’ age were greater or equal to 16 years or 16 years on average. The research setting was limited to Canada, the United States, New Zealand or Australia which share similar histories of colonization and racism against Indigenous peoples (Paradies, 2016). Studies employing psychological, psychosocial, educational, alternative interventions or cultural interventions were included. Solely pharmacological interventions were excluded.
Data collection
Data were extracted by two authors independently using the Cochrane data collection form for randomized controlled trials (RCTs) and non-RCTs (Higgins and Green, 2011). Discrepancies were resolved by a third reviewer and through discussions. Bibliographic information, study design, setting and study period, recruitment, eligibility criteria, sample size, and response and follow-up rates were collected. The outcomes, measurement tools and relevant details of the analysis were extracted. The interventions were described using the Template for Intervention Description and Replication (TIDieR) checklist (Hoffmann et al., 2014). The intervention name; descriptions of the rationale, materials and procedures used; intervention facilitators and research training; how and where the intervention was executed; and its duration and frequency were extracted. Additionally, intervention tailoring and modification as well as fidelity and adherence were summarized.
Risk of bias assessment
The studies were appraised using the Effective Public Health Practice Project (EPHPP) quality assessment tool (Armijo-Olivo et al., 2012) by two independent reviewers, and conflicts were resolved with a third reviewer and through discussions (Supplemental Table S2). Assessment criteria were selection bias, study design, confounding, blinding, data collection, and withdrawal and dropouts. Sex, age, socio-economic status and co-morbidities were defined a priori as confounders. Each criterion was rated weak, moderate or strong. For the global rating, studies were weak if they had two or more criteria rated weak, they were rated moderate if they had one weak rating, or strong if they had no weak ratings.
Results synthesis
Qualitative synthesis was used to report the findings of the studies.
Assessment of Indigenous involvement and content
An assessment of Indigenous involvement and content in the studies was completed independently by two authors and information extracted was supported by prior literature (Huria et al., 2019). We assessed whether Indigenous individuals or groups had decision-making responsibilities at the study design level and were involved in conducting research activities or implementing the intervention. We also assessed whether the studies were specific to an Indigenous population(s) and had considered the population’s diversity and had general or localized Indigenous knowledge included in the intervention or research processes.
Results
Study selection
The search resulted in 67,207 articles and after removing duplicates, 57,826 articles remained. A total of 57,523 articles were excluded based on title and abstract review, and 303 full-text articles were assessed for eligibility. Of these, 283 articles were excluded based on the eligibility criteria (Figure 1) resulting in 21 articles for our review.
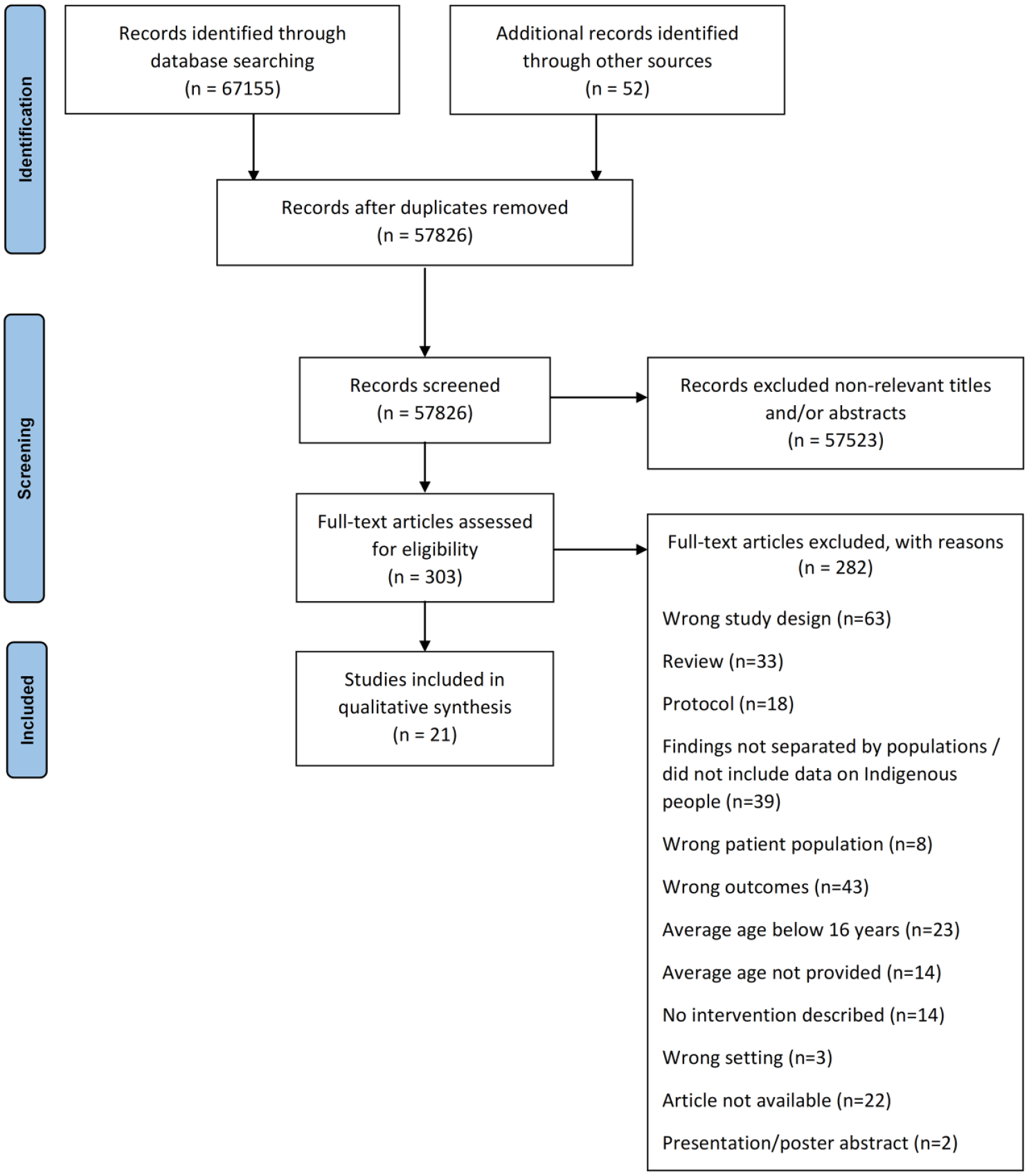
PRISMA flow diagram of the study selection.
Characteristics of included studies
Study characteristics are described in Table 1. Of the 21 studies included, there were 8 RCTs, 10 single-group pre–post designs and 3 pre–post designs with comparison groups. Studies were conducted in the United States (n = 9), Australia (n = 6), Canada (n = 3) and New Zealand (n = 3) and were published between 2009 and 2020. Sample sizes ranged from 10 to 365. Only nine studies reported response rates ranging from 9% to 97% and 19 studies had follow-up rates between 16% and 100%.
Characteristics of included studies.
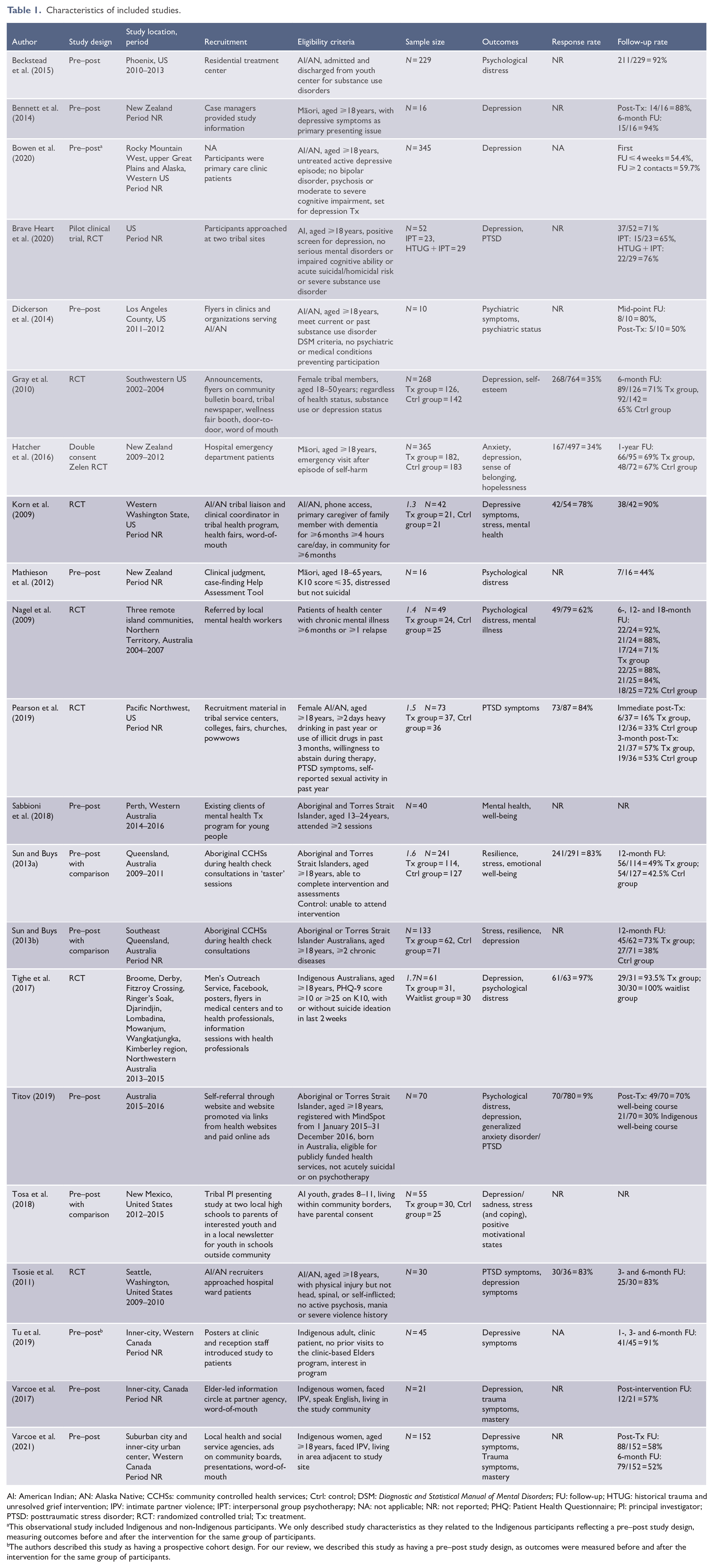
AI: American Indian; AN: Alaska Native; CCHSs: community controlled health services; Ctrl: control; DSM: Diagnostic and Statistical Manual of Mental Disorders; FU: follow-up; HTUG: historical trauma and unresolved grief intervention; IPV: intimate partner violence; IPT: interpersonal group psychotherapy; NA: not applicable; NR: not reported; PHQ: Patient Health Questionnaire; PI: principal investigator; PTSD: posttraumatic stress disorder; RCT: randomized controlled trial; Tx: treatment.
This observational study included Indigenous and non-Indigenous participants. We only described study characteristics as they related to the Indigenous participants reflecting a pre–post study design, measuring outcomes before and after the intervention for the same group of participants.
The authors described this study as having a prospective cohort design. For our review, we described this study as having a pre–post study design, as outcomes were measured before and after the intervention for the same group of participants.
Table 1 also includes the types of study participants and recruitment strategies. Some studies exclusively included women, patients enrolled in or frequenting health institutions, high school students and community event attendees. Recruitment strategies included flyers or posters, social media, websites and online ads and in-person approaches such as through community events, service providers or spaces, and door-to-door or word-of-mouth. One study did not recruit participants and instead used patient data from a clinical database (Bowen et al., 2020).
Description of studies
Supplemental Tables S3 and S4 describe the studies according to the TIDieR checklist and guide (Hoffmann et al., 2014).
Randomized controlled trials
The eight RCTs varied in treatment approaches. Brave Heart et al. (2020) incorporated psychoeducation on trauma and grief, and cultural healing practices with interpersonal group therapy. Tsosie et al. (2011) used individually tailored collaborative care management. Hatcher et al.’s (2016) intervention was based on problem-solving therapy. Another intervention used brief motivational care planning with principles of problem-solving therapy, motivational therapy and self-management (Nagel et al., 2009). Pearson et al. (2019) used trauma-informed cognitive processing therapy, and Korn et al. (2009) used polarity therapy. Tighe et al.’s (2017) trial delivered educational modules based on acceptance-based therapies delivered through an app (Shand et al., 2013). Gray et al. (2010) used cognitive-behavioral skills building with a culturally focused wellness intervention.
Pre–post studies
Ten single-group pre–post studies included diverse therapeutic approaches. Beckstead et al. (2015) incorporated dialectical behavior therapy with cultural complements. Two were based on cognitive behavioral therapy (CBT); Bennett et al. (2014) adapted CBT to Māori values and another used a culturally adapted ultra-brief CBT intervention with problem solving (Mathieson et al., 2012). Sabbioni et al. (2018) used a mental health service model incorporating culturally appropriate strategies and care. One study included online assessments and treatment courses on well-being and CBT (Titov et al., 2017, 2019). Varcoe et al. (2017, 2021) used teaching circles with Elders and cultural activities. Drumming was at the core of Dickerson et al.’s (2014) intervention for healing and community cohesion. Tu et al. (2019) partnered with Elders as part of routine primary care. Bowen et al. (2020) studied the integration of collaborative care management in primary care. Among three pre–post studies with comparison groups, Tosa et al. (2018) used extreme sports as place-based teachings aligned with the sacred water cycle, and Sun and Buys (2013a, 2013b) used a community singing program with culturally relevant songs.
Quality assessments
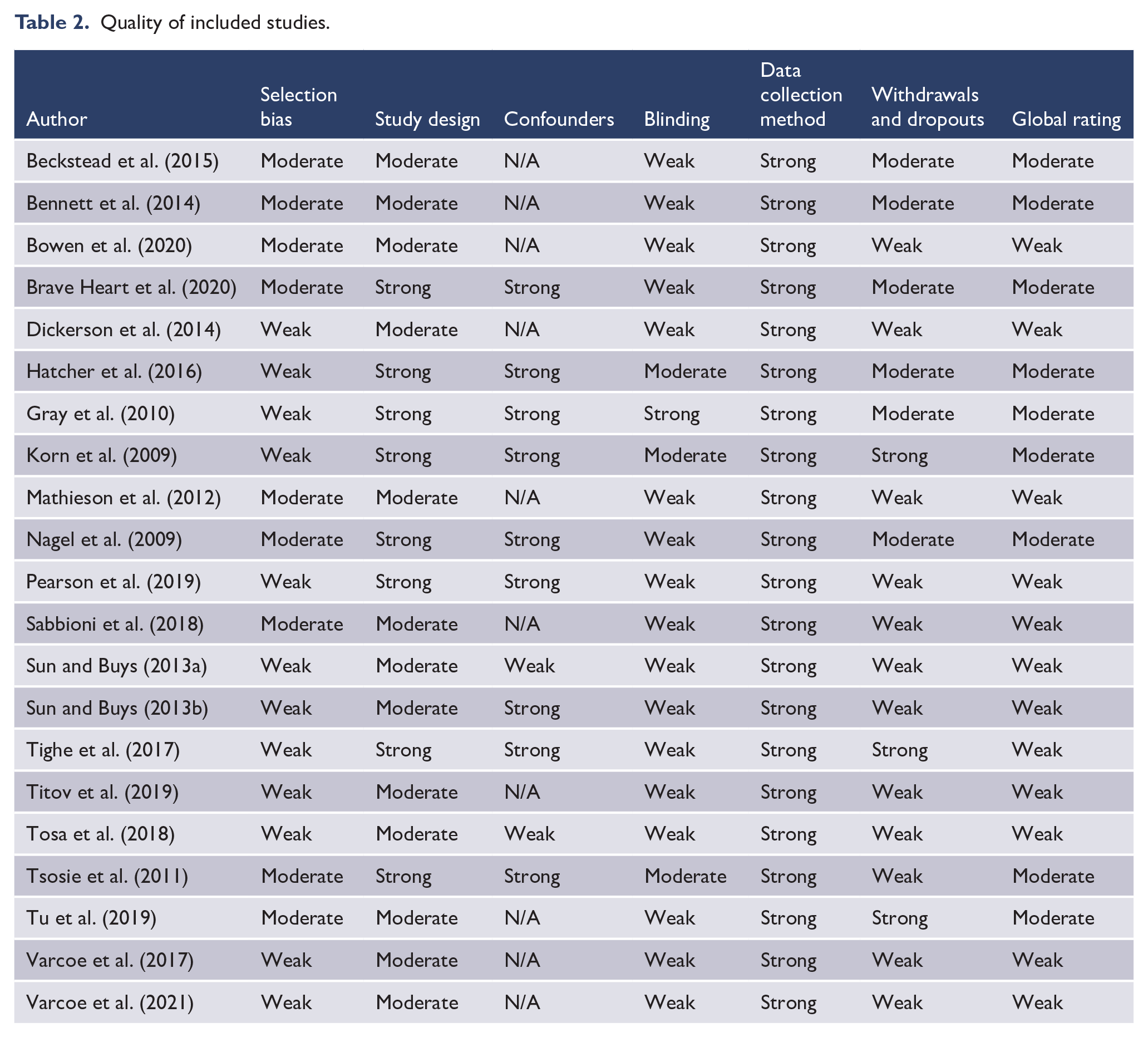
Quality was appraised using the EPHPP Quality Assessment Tool (Table 2). A total of 8 studies had a moderate global rating and 13 a weak global rating. For selection bias, 12 were rated weak as participants were unlikely to be representative of the target population or had a response rates less than 60%. Nine studies were moderate as participants were somewhat likely to be representative of the target population and had a 60–79% response rate, or were representative of the target population with no information on response rates. In total, 8 RCTs received strong ratings for study design and 13 pre–post studies were rated moderate. Ten studies were given a ‘N/A’ for confounders as they were single-group pre–post studies, two were weak for controlling for less than 60% of confounders and eight were strong for controlling all confounders in either the design (e.g. RCT) or analysis. All studies were rated strong for data collection as they employed validated and reliable measures. Three studies were rated strong for withdrawals and dropouts, with follow-up rates 80% or higher and describing reasons for withdrawals and dropouts. Six were rated moderate, meaning a 60–79% follow-up rate or non-applicability due to study design, and the remaining 12 were weak as they provided no reasons for their withdrawals and dropouts or because follow-up rates were less than 60%.
Quality of included studies.
Indigenous individuals or groups with decision-making responsibilities at the study design level
Indigenous individuals or groups with decision-making responsibilities were described at the study design level (Supplemental Table S5). Decision-making at the design level occurred in Indigenous health settings and by Indigenous service providers (Beckstead et al., 2015; Bennett, 2009; Bennett et al., 2014; Dickerson et al., 2014; Korn et al., 2009; Mathieson et al., 2012; Nagel et al., 2009; Pearson et al., 2019; Sabbioni et al., 2018; Sun and Buys, 2013a, 2013b; Tighe et al., 2017; Titov et al., 2019; Tu et al., 2019), cultural leaders (e.g. Elders, Medicine Man, spiritual counselor) (Beckstead et al., 2015; Bennett, 2009; Bennett et al., 2014; Sabbioni et al., 2018; Sun and Buys, 2013a, 2013b; Tsosie et al., 2011; Tu et al., 2019; Varcoe et al., 2017, 2021), Indigenous community members (Dickerson et al., 2014; Gray et al., 2010; Mathieson et al., 2012; Nagel et al., 2009; Pearson et al., 2019; Tighe et al., 2017; Titov et al., 2019; Tosa et al., 2018) and research team members (Dickerson et al., 2014; Mathieson et al., 2012; Nagel et al., 2009; Titov et al., 2019; Tosa et al., 2018; Varcoe et al., 2017, 2021). Decision-making also involved Indigenous research ethics boards (Beckstead et al., 2015; Brave Heart et al., 2020; Pearson et al., 2019; Tighe et al., 2017; Tu et al., 2019) and other groups (e.g. governing or tribal bodies; advisory, consultation, steering, and reference groups, committees, or boards) (Beckstead et al., 2015; Bennett, 2009; Bennett et al., 2014; Brave Heart et al., 2020; Dickerson et al., 2014; Gray et al., 2010; Hatcher et al., 2011, 2016; Mathieson et al., 2012; Pearson et al., 2019; Titov et al., 2019; Tu et al., 2019; Varcoe et al., 2017, 2021). Decision-making by Indigenous individuals or groups was not reported in one study (Bowen et al., 2020).
Involvement in the study design included adapting or determining the intervention content in all but seven studies (Bowen et al., 2020; Hatcher et al., 2011, 2016; Korn et al., 2009; Sabbioni et al., 2018; Sun and Buys, 2013a, 2013b; Tu et al., 2019), approving, endorsing or informing the study proposal or protocol (Bennett, 2009; Bennett et al., 2014; Brave Heart et al., 2020; Dickerson et al., 2014; Gray et al., 2010; Mathieson et al., 2012; Pearson et al., 2019; Sabbioni et al., 2018; Sun and Buys, 2013a, 2013b; Tosa et al., 2018; Tu et al., 2019; Varcoe et al., 2017, 2021), and implementing or overseeing implementation of the intervention (Gray et al., 2010; Sun and Buys, 2013a, 2013b; Varcoe et al., 2017, 2021).
Specificity and diversity of Indigenous population and Indigenous-specific content in the intervention and research process
The specificity of the studies to Indigenous populations is described in Supplemental Table S6. All studies were specific to Indigenous populations, but only two studies considered the populations’ diversity by engaging specific communities (Nagel et al., 2009; Tighe et al., 2017). Indigenous-specific content (e.g. ceremonies, oral and musical traditions, and weaving and crafting) was described in all but two studies (Bowen et al., 2020; Sun and Buys, 2013b). Nine studies explicitly included Indigenous worldviews or values into the intervention (Bennett et al., 2014; Brave Heart et al., 2020; Hatcher et al., 2011, 2016; Mathieson et al., 2012; Nagel et al., 2009; Pearson et al., 2019; Sabbioni et al., 2018; Varcoe et al., 2017, 2021). Five studies used Indigenous-specific measures or measures validated for use in Indigenous peoples (Brave Heart et al., 2020; Dickerson et al., 2014; Hatcher et al., 2011, 2016; Pearson et al., 2019; Sun and Buys, 2013b) (Supplemental Table S6).
Indigenous peoples’ involvement in conducting research activities and implementing the intervention
We identified five potential study stages for Indigenous involvement (Supplemental Table S7). Indigenous people set the study aims in four studies (Bennett et al., 2014; Hatcher et al., 2016; Tosa et al., 2018; Tu et al., 2019). Six studies had Indigenous involvement in recruitment (Gray et al., 2010; Korn et al., 2009; Tighe et al., 2017; Tosa et al., 2018; Tsosie et al., 2011; Varcoe et al., 2017). Indigenous health service providers and personnel (Gray et al., 2010; Korn et al., 2009; Tighe et al., 2017), research team and administrative personnel (Tosa et al., 2018; Tsosie et al., 2011), and cultural leaders (Korn et al., 2009; Varcoe et al., 2017) were involved in recruitment. In five studies, recruitment took place in Indigenous settings (e.g. clinics, service centers, pow wows, tribal health programs, health fairs) (Korn et al., 2009; Pearson et al., 2019; Sun and Buys, 2013a, 2013b; Tu et al., 2019). Only eight studies involved Indigenous peoples in the data collection (Mathieson et al., 2012; Sabbioni et al., 2018; Tighe et al., 2017; Tosa et al., 2018; Tsosie et al., 2011), analysis (Tosa et al., 2018; Tu et al., 2019) or sharing (Dickerson et al., 2014; Tosa et al., 2018; Tu et al., 2019) stages. Fifteen studies had Indigenous service providers delivering the intervention (Beckstead et al., 2015; Brave Heart et al., 2020; Dickerson et al., 2014; Gray et al., 2010; Hatcher et al., 2016; Nagel et al., 2009; Sabbioni et al., 2018; Sun and Buys, 2013a, 2013b; Tighe et al., 2017; Tosa et al., 2018; Tu et al., 2019; Varcoe et al., 2017, 2021) and Indigenous staff coordinating and administering the intervention (Hatcher et al., 2016; Sun and Buys, 2013a, 2013b; Tsosie et al., 2011). Six studies included research training opportunities exclusively for Indigenous persons on facilitating the intervention (Beckstead et al., 2015; Brave Heart et al., 2020; Gray et al., 2010; Tosa et al., 2018), data collection and analysis (Tosa et al., 2018) and on trauma (Varcoe et al., 2017, 2021).
Synthesis of mental health outcomes
The mental health outcomes measured included mood and anxiety disorders, PTSD and trauma symptoms, and general mental health measures (Table 3).
Summary of findings.
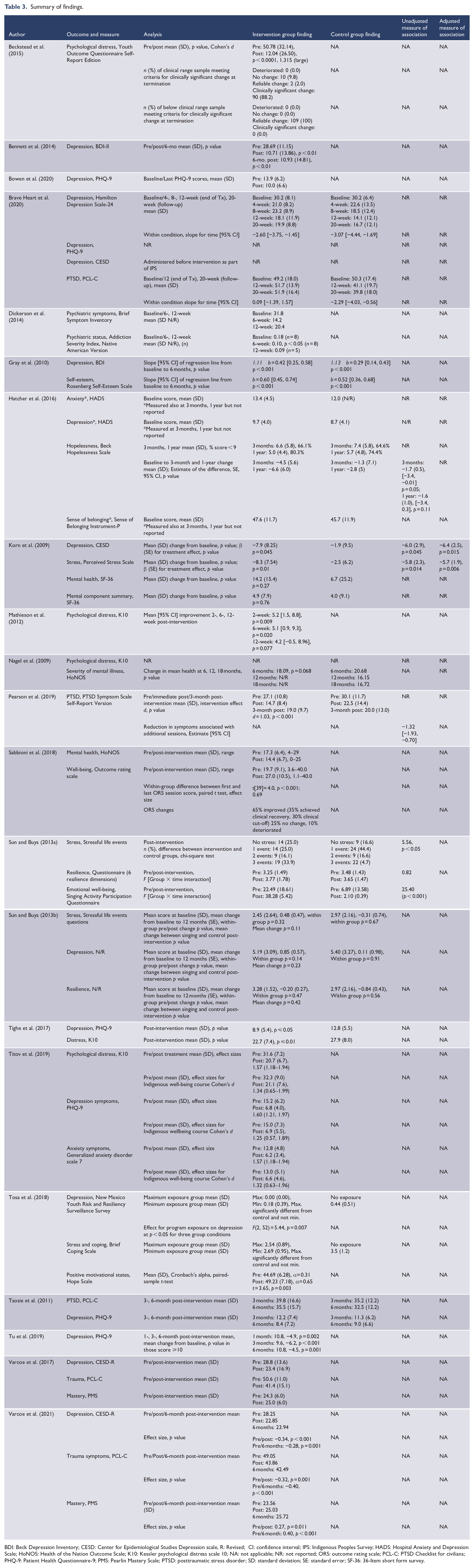
BDI: Beck Depression Inventory; CESD: Center for Epidemiological Studies Depression scale, R: Revised; CI: confidence interval; IPS: Indigenous Peoples Survey; HADS: Hospital Anxiety and Depression Scale; HoNOS: Health of the Nation Outcome Scale; K10: Kessler psychological distress scale 10; NA: not applicable; NR: not reported; ORS: outcome rating scale; PCL-C: PTSD Checklist for civilians; PHQ-9: Patient Health Questionnaire-9; PMS: Pearlin Mastery Scale; PTSD: posttraumatic stress disorder; SD: standard deviation; SE: standard error; SF-36: 36-Item short form survey.
Mood and anxiety disorders
Among six RCTs evaluating depressive symptoms, two measured statistically significant reduced symptoms immediately post-intervention (Korn et al., 2009; Tighe et al., 2017) and one at 6 months after baseline in both arms (Gray et al., 2010). One trial measured statistically significant lower depression scores at 20 weeks after baseline (Brave Heart et al., 2020). Depression scores were not reduced in one RCT (Tsosie et al., 2011) and one trial did not report their scores (Hatcher et al., 2016). Among six single-group pre–post studies assessing depression, three studies showed statistically significant reductions in depression immediately post-intervention and at 6-month follow-up (Bennett et al., 2014; Tu et al., 2019; Varcoe et al., 2021) as well as at 1- and 3-month post-intervention (Tu et al., 2019). In the three remaining pre–post studies, depression was reduced immediately post-intervention, but statistical significance was not provided (Bowen et al., 2020; Titov et al., 2019; Varcoe et al., 2017). One pre–post study with comparison group showed statistically significant lower depression scores immediately post-intervention (Tosa et al., 2018), but the other study did not (Sun and Buys, 2013b).
Anxiety was measured in an RCT and a pre–post study. In the RCT, anxiety scores were not reported (Hatcher et al., 2016). The pre–post study measured a statistically significant decrease in scores immediately post-intervention using a measure for anxiety, panic and PTSD (Titov et al., 2019).
Psychological distress was assessed in two RCTs and three pre–post studies. One RCT had a statistically significant lower mean distress score post-intervention (Tighe et al., 2017), and the second RCT did not report their results (Nagel et al., 2009). In two pre–post studies, lower mean distress scores were statistically significant immediately post-intervention (Beckstead et al., 2015) and at 2- and 6-week post-intervention (Mathieson et al., 2012). In the third study, distress was lower immediately post-intervention, but statistical significance was not calculated (Titov et al., 2019).
PTSD or trauma symptoms
Three RCTs examined PTSD symptoms. One trial had a statistically significant reduction in mean PTSD symptom scores immediately and 3 months post-intervention (Pearson et al., 2019), and in the intervention arm for two RCTs, symptoms were not reduced (Brave Heart et al., 2020; Tsosie et al., 2011). Among three pre–post studies, one study had a statistically significant reduction in PTSD (Titov et al., 2019), and a second study showed decreased trauma symptoms at post-intervention, but statistical significance was not calculated (Varcoe et al., 2017). In a third study, trauma symptoms were statistically significantly lower immediately post-intervention and at 6 months (Varcoe et al., 2021).
General mental health measures
In one RCT, mental health score changes were not statistically significant (Korn et al., 2009). A pre–post study found reduced mental health scores immediately post-intervention, but statistical significance was not calculated (Sabbioni et al., 2018).
A measure of well-being showed statistically significant improvements immediately post-intervention in one pre–post study (Sabbioni et al., 2018). Social and emotional well-being measured in two pre–post studies with comparison groups using the same intervention (Sun and Buys, 2013a, 2013b) showed statistically significant improvement in well-being in only one of the studies (Sun and Buys, 2013a).
One RCT measured a statistically significant reduction in perceived stress scores in the intervention arm (Korn et al., 2009). Among three pre–post studies with comparison groups, two studies using the same intervention measured fewer stressful events in the intervention group (Sun and Buys, 2013a, 2013b), but statistical significance was only measured in one of the studies (Sun and Buys, 2013a). In the third study, stress and coping scores were statistically significantly improved in the intervention group (Tosa et al., 2018).
Psychiatric symptoms and status were assessed in one pre–post study and statistically significant reduction in status only was observed at 6 and 12 weeks (Dickerson et al., 2014).
Other strength-based mental health outcomes
One RCT saw a statistically significant reduction in hopelessness in the intervention at 3-month follow-up, and although it measured sense of belonging only, the baseline measure was reported (Hatcher et al., 2016). Another RCT demonstrated statistically significant improvements in self-esteem at 14-week follow-up in both arms (Gray et al., 2010). Two pre–post studies of the same intervention observed increased mastery (Varcoe et al., 2017, 2021), but statistically significant improvements immediately post-intervention and at 6-month follow-up were only measured in one study (Varcoe et al., 2021). Two pre–post studies of the same intervention with comparison groups measured resilience and did not show statistically significant changes in the intervention group (Sun and Buys, 2013a, 2013b). Another pre–post study with comparison showed a statistically significant improvement in positive motivational state immediately post-intervention (Tosa et al., 2018).
Discussion
Summary of results
This is one of the largest systematic reviews to date on mental health interventions for Indigenous populations. It demonstrates that interventions are mostly effective in improving mental health outcomes in the short term, but the extent to which they engage communities in the research and intervention can vary widely. Meta-analysis could not be conducted due to the heterogeneity of the study designs. Depression was the most frequently examined outcome and 8 of 14 studies observed statistically significant improvements. Three of the six studies that assessed PTSD symptoms showed statistically significant improvements. Three of five studies examining psychological distress and two of four studies on the impact on stress showed statistically significant improvements. Only two studies looked at anxiety and one showed a statistically significant decrease. Six of the fourteen other studies all examining various general mental health or related outcomes (e.g. resilience, mastery) reported statistically significant positive results associated with the interventions.
Comparisons to other systematic reviews
Four similar systematic reviews have been published between 2015 and 2018 (Antonio and Chung-Do, 2015; Leske et al., 2016; Pollok et al., 2018; Pomerville et al., 2016) with the latest article being from 2015. Articles in our review were published between 2009 and 2020 and 11 of 21 between 2016 and 2020. Among the four reviews, four unique articles overlapped (Beckstead et al., 2015; Dickerson et al., 2014; Mathieson et al., 2012; Nagel et al., 2009).
Pollok et al. (2018) evaluated experimental studies of behavioral and pharmacological interventions for depression in any setting, whereas Leske et al. (2016) examined pharmacological, psychological and educational interventions for both mental and substance use disorders in Australia, Canada, New Zealand and the United States. Pomerville et al. (2016) aimed to understand the landscape of empirical work on psychotherapies for Indigenous populations in Australia, Canada, New Zealand and the United States, specifically understanding how much research exists, the types of research and their key findings. Antonio and Chung-Do (2015) examined mental health and substance use disorder interventions for Indigenous adolescents and assessed the degree to which an intervention was culturally tailored. Articles in these reviews were ineligible for our review as they were pharmacological interventions or had qualitative designs, irrelevant outcomes (e.g. tobacco and alcohol dependence) or no/lower age requirements. Our review builds on these efforts and few existing reviews have completed such a systematic, extensive examination of Indigenous involvement or content of interventions.
Indigenous involvement in interventions and research
Assessment and reporting of Indigenous involvement and content, whether in the context of original research or reviews, is important for many reasons. As observed in this review, studies varied greatly in this regard and perhaps most apparently so, in the reporting. Not only were actual involvement of Indigenous peoples and organizations and their roles often unclear, wording to describe involvement also varied greatly. Thus, conducting such assessments and reporting the results in original research can encourage accountability throughout the research process and transparency for readers. Researchers can consider using tools such as the CONSolIDated critERtia for strengthening the reporting of health research involving Indigenous Peoples (CONSIDER) statement to strengthen their reporting of health research involving Indigenous Peoples (Huria et al., 2019) or the Aboriginal and Torres Strait Islander Quality Appraisal Tool, a research assessment tool from Indigenous perspectives (Harfield et al., 2020).
Of course, these are only aides for researchers to critically reflect on the purpose and implications of their research beyond the ‘outcomes of interest’. Also, assessing Indigenous involvement can speak to the quality of the intervention and study, their effectiveness and feasibility (e.g. improved health outcomes, study participant recruitment, community engagement, uptake of research activities, self-determination, data sovereignty). In terms of quality, all the studies had either a weak (n = 12) or moderate (n = 9) global rating. Increased engagement of Indigenous people throughout the research process may have improved several quality assessment domains such as selection bias (i.e. response rate and recruitment) and withdrawals/dropouts. Our findings showed limited Indigenous involvement in recruitment which could have impacted the sample size to detect clinically or statistically significant outcomes (Faber and Fonseca, 2014). Also, perhaps greater involvement would have led to the collection of more information on reasons for dropouts and withdrawals important factors in determining the rating of this domain. Understanding the motivation of Indigenous people to participate in research has been shown to differ from non-Indigenous people and can largely be met by engaging Indigenous people. For example, the motivations for Indigenous people to participate in research included benefits to the community, the expression of specific values (e.g. reciprocity, respect, honesty) in the research process, as well as the selection of meaningful outcomes and research interests (Guillemin et al., 2016; Nadalin et al., 2010). Finally, Indigenous involvement in capacity building activities such as conducting the research and implementing interventions may sustain positive mental health outcomes beyond the duration of the research. Trained Indigenous persons living in the community may integrate intervention activities and skills acquired into programming or services. CONSIDER and the Aboriginal and Torres Strait Islander quality appraisal tool speak to outcomes that are beneficial at a community level versus solely individual level measures (Harfield et al., 2020; Huria et al., 2019). They also consider the use of Indigenous methodologies in contrast to western research principles (Harfield et al., 2020; Huria et al., 2019). We have developed an exploratory table (Supplemental Table S8) which should be reviewed cautiously given that future studies should conduct in-depth investigations into the level and duration of Indigenous involvement for example, as well as other yet to be identified factors that may be more meaningful to Indigenous peoples and communities. In fact, our supplementary Tables S5–S7 are important Indigenous-specific outcomes that only arise through Indigenous involvement that are as equally meaningful as improved mental health outcomes (Harding and Oetzel, 2019; Harfield et al., 2020; Huria et al., 2019).
With a(n) (ongoing) history of medicine and research being used as tools of continued colonial violence (Hawkes et al., 2017; Hyett et al., 2018; Smylie, 2005; Tuck, 2009), it is imperative that non-Indigenous researchers consider and address implications of their research given their positionality and answer whether the research should be conducted in the first place (Kwaymullina, 2016). Also whether institutionalized research ethics frameworks and practices of universities and colonial state governments agencies are truly aligned with reciprocity and respect within Indigenous epistemologies (Hawkes et al., 2017). In addition, it is important to consider whether these frameworks and practices are aligned with national and local Indigenous-defined research ethics for each country (Canadian Institutes of Health Research, Natural Sciences and Engineering Research Council of Canada and Social Sciences and Humanities Research Council, 2018; Hayward et al., 2021; National Health and Medical Research Council, 2018).
Limitations
There are several limitations in our review. First, mental health is also encompassed by and conceptualized through the term ‘social and emotional wellbeing (SEWB)’ in Australia. Aboriginal and Torres Strait Islander Peoples’ concept of SEWB emphasizes connections to family, kin, community, land, spirituality and health and is contextualized in the broader sociopolitical context in which these connections have been disrupted (Gee et al., 2014). As our search terms did not include ‘social and emotional wellbeing’, relevant studies from Australia may have been missed. However, it is important to note that we did include other terms such as ‘wholeness, wellness, wellbeing’ that may have been keywords or MeSH terms of articles of interest in our search strategy (Supplemental Table S1). Also, ‘mental health and mental disorder’, keywords in our search strategy, were keywords in articles on SEWB (Calma et al., 2017; Gee et al., 2014). As in the systematic reviews described above on similar topics, we have included Indigenous peoples from Canada, the United States, Australia and New Zealand. Therefore, our findings cannot be generalized across Indigenous populations in different countries and within the Indigenous populations of a country which is why we have ensured that our review specifies the Indigenous populations and their communities if reported (Supplemental Table S6).
Second, our assessment of Indigenous involvement and content was restricted to the information written in the articles. It is not yet commonplace to describe Indigenous relationships or involvement in research in journal articles. Authors make subjective decisions on what to include or exclude and are limited by academic journals’ publication requirements like word counts or editing processes. We did not conduct external searches to investigate the studies, unless the article in our review directed readers to another publication to increase information on the protocol. We noted whether there were Indigenous primary authors/investigators, but if this was not explicitly described in the articles (Brave Heart et al., 2020), they were not recorded.
One final limitation may be that our review lacks more ‘rigorous’ studies, as indicated by the lack of ‘strong’ quality studies. However, as discussed above, there are legitimate questions around whether existing, non-Indigenous assessment tools are appropriate as standalone tools for evaluating ‘quality’ of research involving Indigenous peoples. Furthermore, we recognize the challenges in implementing more resource-intensive and rigid RCT designs.
Implications and recommendations
The observations in our review support the establishment and uptake of reporting guidelines for Indigenous health research to improve both the implementation and description of research. It is particularly important to understand power relations, accountability and reciprocity in Indigenous health research in the context of colonial states, where medicine, public health and ‘knowledge production’ more generally have facilitated and reinforced colonial systems (Schnarch, 2004).
Through the cultural assessment, we learned that six interventions trained community members (Beckstead et al., 2015; Brave Heart et al., 2020; Gray et al., 2010; Tosa et al., 2018; Varcoe et al., 2017, 2021) (where applicable, given some were retrospective or observational), extending the impact of the intervention beyond the study period. Hiring and training community members can be beneficial since clinical skills are transferrable beyond the duration of the intervention and financial resources are directed to the community. Funding and resources are integral to supporting self-determination and cultural continuity in many Indigenous communities (Auger et al., 2016; First Nations Health Authority, 2018). Any positive impacts of interventions may be better sustained if researchers were committed to also providing a plan for what happens after the ‘completion’ of the intervention and research. To the best of our knowledge, most of the studies did not report a plan to follow-up with the community after the intervention, ways to disseminate findings, or plans to apply findings to future program or policy.
Cultural continuity, understood as intergenerational cultural connectedness, is a determinant of Indigenous health (Auger, 2016). Self-determination and governance are crucial in improving Indigenous health at the population level (Alfred, 2009; Auger et al., 2016; Chandler and Lalonde, 1998). Therefore, interventions and policy changes for improving Indigenous mental health should aim to promote cultural continuity, self-determination and self-governance. Most studies in this review addressed cultural continuity by facilitating the transmission of cultural knowledge or incorporating Indigenous values and healing practices as part of the intervention. Self-governance and self-determination were rarely the goal for these interventions, likely because mental health interventions tend to focus on treating or improving an individual’s symptoms. One study (Tosa et al., 2018) had participating youth lead a project to address an issue from their community as part of the intervention, which could potentially address self-determination to some degree.
Cultural continuity and self-determination also have micro- and macro-level dimensions (Auger, 2016; Auger et al., 2016) and therefore their operationalization may differ vastly. Interventions here do not address self-determination and self-governance in the macro-, structural sense. Here, we recognize the challenges in that public health ‘interventions’ are questionable instruments to address deeply embedded structural injustices. In turn, there are tensions in how public health is implicated in this context—as colonial governments continue to invest in public health research and interventions, they simultaneously continue to disregard and actively preserve root causes of health inequities.
Conclusion
A wide range of interventions identified in our review demonstrated mental health improvements. However, it is difficult to draw generalizable conclusions on intervention effectiveness, given study heterogeneity. Future studies should first consider the appropriateness of actually conducting their research and intervention. Then, researchers should thoroughly assess the Indigenous involvement and content of their interventions throughout the research process. Finally, it is important to consider the implications of the research, whether and how they address important social and structural determinants of mental health for Indigenous peoples.
Supplemental Material
sj-docx-1-anp-10.1177_00048674221089837 – Supplemental material for Systematic review of Indigenous involvement and content in mental health interventions and their effectiveness for Indigenous populations
Supplemental material, sj-docx-1-anp-10.1177_00048674221089837 for Systematic review of Indigenous involvement and content in mental health interventions and their effectiveness for Indigenous populations by Rachel Seungyun Lee, Hilary K Brown, Sarah Salih and Anita C Benoit in Australian & New Zealand Journal of Psychiatry
Footnotes
Acknowledgements
We would like to thank Vincci Lui, Librarian from the University of Toronto, for contributing to the development of our search strategy as well as Catherine Moses and Priya Prabhakar who contributed to developing the search strategy and for screening titles and abstracts. Nadine Eltayeb also screened titles and abstracts.
Author Contributions
A.C.B. and H.K.B. developed the study concept. S.S. contributed to developing and conducting the database search and coordinated the screening of titles and abstracts. A.C.B. and R.S.L. also screened titles and abstracts. All authors conducted the full-text screening and data extraction. A.C.B., H.K.B. and R.S.L. conducted the data analyses and contributed to the write-up and review of the manuscript. S.S. provided feedback on the manuscripts. The funders had no involvement in the data extraction, analysis and writing of the manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship and/or publication of this article: A.C.B. is supported by a Canadian Institutes for Health Research (CIHR) Ontario HIV Treatment Network (OHTN) New Investigator Award; Rachel S. Lee, Catherine Moses and Priya Prabhakar are supported by a CIHR Operating Grant (CBA 144834); H.K.B. is supported by a Tier 2 Canada Research Chair; S.S. is supported by a Canadian Institutes for Health Research (CIHR) Operating Grant (CBA 144384) and from Dr Brown’s Canada Research Chair.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
