Abstract
Objective:
To control a second-wave COVID-19 outbreak, the state of Victoria in Australia experienced one of the world’s first long and strict lockdowns over July–October 2020, while the rest of Australia experienced ‘COVID-normal’ with minimal restrictions. We (1) investigate trajectories of parent/child mental health outcomes in Victoria vs non-Victoria and (2) identify baseline demographic, individual and COVID-19-related factors associated with mental health trajectories.
Methods:
Online community sample of 2004 Australian parents with rapid repeated assessment over 14 time-points over April 2020 to May 2021. Measures assessed parent mental health (Depression, Anxiety and Stress Scales-21), child depression symptoms (13-item Short Mood and Feelings Questionnaire) and child anxiety symptoms (four items from Brief Spence Children’s Anxiety Scale).
Results:
Mental health trajectories shadowed COVID-19 infection rates. Victorians reported a peak in mental health symptoms at the time of the second-wave lockdown compared to other states. Key baseline predictors, including parent and child loneliness (standardized regression coefficient [β] = 0.09–0.46), parent/child diagnoses (β = 0.07–0.21), couple conflict (β = 0.07–0.18) and COVID-19 stressors, such as worry/concern about COVID-19, illness and loss of job (β = 0.12–0.15), predicted elevated trajectories. Effects of predictors on parent and child mental health trajectories are illustrated in an online interactive app for readers (https://lingtax.shinyapps.io/CPAS_trend/).
Conclusion:
Our findings provide evidence of worse trajectories of parent and child mental health symptoms at a time coinciding with a second COVID-19 outbreak involving strict lockdown in Victoria, compared to non-locked states in Australia. We identified several baseline factors that may be useful in detecting high-risk families who are likely to require additional support early on in future lockdowns.
As they enter the second year of the COVID-19 pandemic, many countries have imposed stricter and longer lockdowns (i.e. stay at home requirements) to limit the spread of the virus. Australia’s experience in 2020 provides a rare natural experiment for understanding the differential impact of COVID-19 outbreaks and associated lockdowns. The whole country experienced an 8-week national lockdown over April–May 2020. Then from June, most states experienced a period of low infection rates and minimal restrictions. In contrast, the state of Victoria (6·4M residents, 25% of Australia’s population) experienced a COVID-19 outbreak in late June, and went on to experience one of the longest and strictest lockdowns in the world (at that time), extending 4 months over July–October 2020, and requiring citizens to stay in their houses except for essential shopping (1 household member, once per day) and a maximum of 1 hour of daily exercise within a 5 km radius of their house, mandatory mask-wearing (indoor and outdoor) for those aged 12 years or more and a night-time curfew (8 pm to 5 am). Early childhood education centres and schools were closed. Altogether, Victorians were in hard lockdown for 176 days in 2020, compared to 56 days of less stringent rules for non-Victorians. Australia’s stratified experience of the COVID-19 pandemic, and the otherwise similar cultural, political and economic context across Australian states and territories, provide an unusual opportunity to assess mental health impacts of the strict second-wave lockdown in Victoria compared to the ‘COVID-normal’ control conditions experienced by the rest of Australia.
Around the world, COVID-19 lockdowns have posed particular risk for (1) parents, who have been required to juggle paid work from home while caring for children and/or supporting children’s remote learning from home (Achterberg et al., 2021; Chung et al., 2020; Dickerson et al., 2020; Romero et al., 2020); (2) children, in many cases removed from their usual education, care and social environments (Duan et al., 2020; Liu et al., 2020; Oosterhoff et al., 2020; Patrick et al., 2020; Rosen et al., 2020; Xie et al., 2020); and (3) high-risk groups, such as families with pre-existing mental health conditions (Asmundson et al., 2020; Dickerson et al., 2020) and/or financial stress (Amerio et al., 2020; Wang et al., 2020b) (pre-existing or COVID-19-related). However, data investigating the mental health outcomes for parents and children, specifically, during the present pandemic have been scarce. Studies have tended to assess static outcomes, either using cross-sectional data or longitudinal data with outcomes only measured at one time-point (Dickerson et al., 2020; Gotlib et al., 2021); or they have used a limited number of repeated measures (i.e. usually four or fewer time-points, and with small sample sizes) (Achterberg et al., 2020; Hussong et al., 2021). These designs limit the ability to examine within-person stability or change in symptoms across the period of the pandemic. Given the fast-moving and rapidly changing nature of COVID-19-related restrictions and lockdowns, it is important to understand whether the mental health impacts of the pandemic have also changed over time. Latent growth models enable sensitive assessment of within-person change over time (Sterba and Bauer, 2010).
To promote recovery, there is a need to prospectively examine the effects of prolonged, restrictive lockdowns on parents and children and to identify the most vulnerable families. There is also a need to identify high-risk families early in future crisis events, to ensure prompt and appropriate care, and thereby minimize long-term mental health impacts. Evidence consistently shows increased rates of mental health problems during the pandemic associated with pre-existing socio-economic disadvantage (Duan et al., 2020; Fisher et al., 2020; Oosterhoff et al., 2020; Patrick et al., 2020); sudden disadvantage related to the pandemic (e.g. through job loss) (Chung et al., 2020; Duan et al., 2020); worry/concern about the virus (Chung et al., 2020; Duan et al., 2020; Liu et al., 2020; Oosterhoff et al., 2020; Rosen et al., 2020; Xie et al., 2020); use of news media (Rosen et al., 2020); and pre-existing factors, such as chronic health conditions and mental health problems (Rosen et al., 2020; Wang et al., 2020a); and child neurodevelopmental conditions (Joseph et al., 2019; Skokauskas and Gallagher, 2012). Furthermore, other factors, such as personality and the quality of housing, may also be influential, given families have been restricted to their homes for extended periods.
The current study draws on data from an online community sample of 2004 parents followed over 14 time-points from April 2020 to May 2021 (Westrupp et al., 2020b). We aim to:
Investigate trajectories of parent and child mental health outcomes over the COVID-19 crisis in Victorian families experiencing strict second-wave lockdown, compared with families in the rest of Australia experiencing COVID-normal minimal restrictions.
Identify families at increased risk of poor mental health trajectories based on baseline factors, including: (a) demographic factors; (b) individual parent and child factors, such as pre-existing mental or physical health diagnoses, loneliness and couple verbal conflict; and (c) COVID-19-related stressors, including job loss and COVID-19-related illness.
Method
Design and recruitment
This study uses 13.5 months of data, collected over 14 time-points, from the COVID-19 Pandemic Adjustment Survey (CPAS) (Westrupp et al., 2020b), an online community sample of 2365 Australian parents of a child 0–18 years. CPAS was approved by the Deakin University Human Ethics Advisory Group (HEAG-H 52_2020). Participants were recruited via paid and unpaid social media advertisements over 8–28 April 2020, during the first-wave national lockdown (i.e. stay at home requirements) in Australia, targeting specific groups via postcodes/demographic factors to increase the representativeness of the sample. Participants responded about their oldest child aged 0–18, and were followed over 14 time-points, until 19 May 2021. Participants were eligible if they resided in Australia and were aged ⩾18 years, English speaking and a current parent of a child aged 0–18 years.
Given the unique and unprecedented context of the pandemic, we developed a ‘rapid repeated assessment’ paradigm, designed to maximize the frequency of data capture while minimizing burden related to intensive research participation. We collected data every 2–4 weeks (10-min online survey), in order to reflect constantly changing conditions, but planned for intermittent participation across multiple time-points. From time-point 4, we conducted phone or text/SMS follow-up only if participants had not completed 3+ consecutive time-points. Our approach was guided by the strengths of our trajectory modelling approach, which is robust to missing data and utilizes all available data from each participant (e.g. even if individuals participate at just 2–3 time-points). Additionally, our approach maximized coverage over time, with a proportional spread of data over the time-points of the study. Supplemental eFigure 1 shows participation rates across the study relative to the two lockdown periods: 72% of our final sample participated in 3 or more time-points; 60% participated in 4 or more; and 62% participated during the second-wave Victorian lockdown.
Participants
Current analyses used data from 2004 (of 2365 recruited) participants who provided at least one time-point of data. Compared to included participants, those excluded were younger, more likely to report low household income and a chronic physical health condition (see Supplemental eTable 1). We tested the effect of intermittent participation (see Supplemental eTable 2). Lower and earlier participation were both associated with male/non-binary parent gender, younger age, renting, overseas birth, financial deprivation, COVID-19 environmental stressors, lower household income and having a child with attention-deficit hyperactivity disorder (ADHD) or autism spectrum disorder (ASD). In contrast, parents with a chronic physical condition, or who had a child at home while working, were more likely to participate more often and later. Otherwise, parents participating more often were less likely to report baseline depression, anxiety, stress, loneliness and couple conflict. Parents participating later in the study reported lower baseline anxiety, depression, couple conflict and more satisfaction with their home.
Measures
Parents reported on their own and their child’s mental health. Table 1 details our measures of parent and child mental health outcomes over time-points 1–14, and baseline factors related to parent and child demographics, individual factors and COVID-19-related stressors.
Study measures.
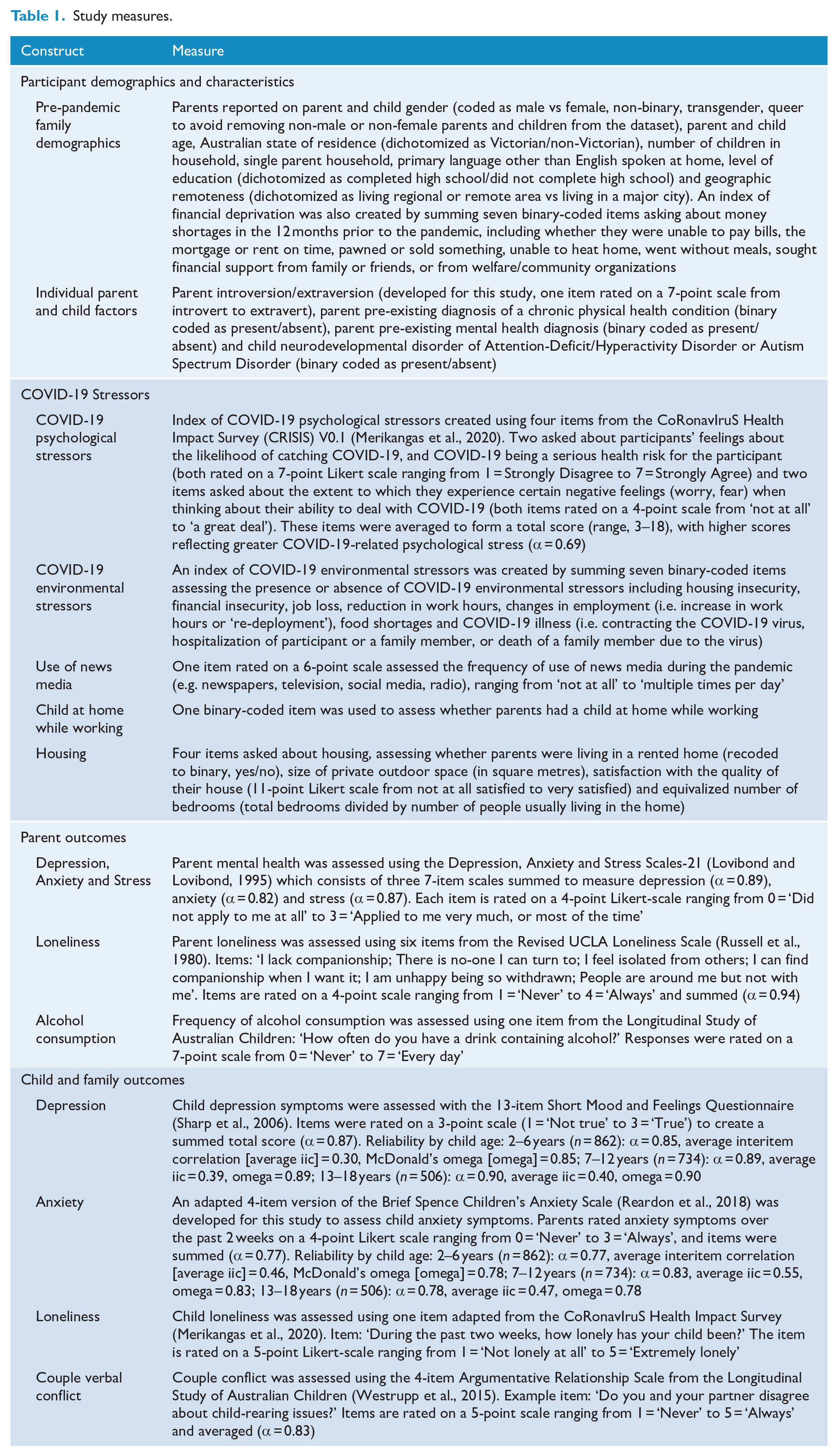
Data analysis
Data were cleaned in Stata version 16 and analysed in Mplus version 8·4. Multilevel modelling was used as the basis for all analyses, allowing us to estimate the trajectories of each parent and mental health outcome over time, using full-information maximum likelihood estimation to include all available data. To determine an appropriate trajectory shape, we first examined the trajectories for each outcome using the full sample of participants. To assist in estimation and avoid collinearity, time was centred at the mean of 113 days, rather than 0 days. A series of models were estimated including latent indicators of growth, from linear (^1) to sextic (^6) polynomial change over time. An appropriate model for each outcome was determined based on model fit and visual inspection. Model fit was based on comparing each model to the previous (e.g. quadratic model vs linear model) via chi-square difference tests and change in Akaike information criterion (AIC) and Bayesian information criterion (BIC) scores (Supplemental eTable 3, Supplemental eFigure 2).
To explore Aim 1, we estimated grouped multilevel models to compare trajectory shapes between participants residing in locked-down Victoria vs non-Victorian COVID-normal. Wald chi-square tests were used to examine differences in latent growth parameters. To address Aim 2, the models used for Aim 1 were repeated with each latent growth parameter regressed onto all exposure variables simultaneously. To obtain standardized estimates, we used a Bayes estimator for all regression models using default (non-informative) priors. Estimates and their 95% credibility intervals are reported in Supplemental eTables 5–14 (described later). The interpretation of each exposure’s effect was based on the influence on the overall trajectory shape and effect size (β) magnitude. Given the breadth of proposed exposures, we provide an interactive ‘shiny app’ as an online supplement to help readers visualize the impact of exposure variables on trajectories of these mental health constructs over time (https://lingtax.shinyapps.io/CPAS_trend/).
Results
Sample characteristics
Table 2 presents baseline characteristics of the full sample and of second-wave lockdown (Victorian, N = 1141, 51%) and COVID-normal (non-Victorian, N = 1112, 49%) samples. The majority of parents were female. Almost one-third of parents reported a chronic physical health condition, 41% reported a mental health condition and 15% had a child with ADHD or ASD. Most had a child at home while working from home, and less than one-third were renting their home. Demographic characteristics were fairly consistent across the samples. We have previously shown our sample is broadly representative of the Australian parent population in terms of geographic location, number of children, parents born overseas and single parent households, but note our sample are mostly mothers (underrepresenting fathers), and somewhat under-representative of families with a low income and low education (Westrupp et al., 2020a).
Baseline sample characteristics for the COVID-19 Pandemic Adjustment Survey.
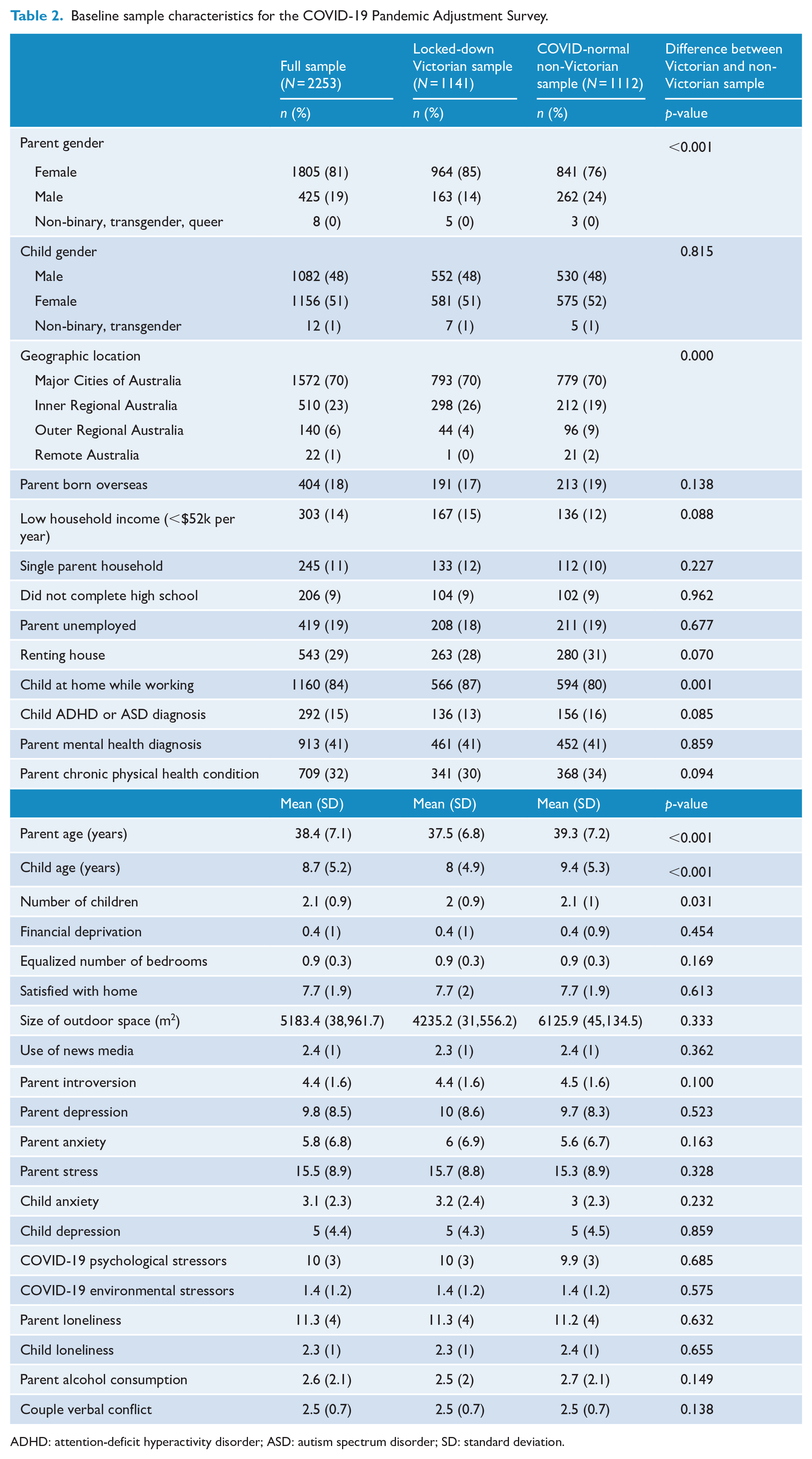
ADHD: attention-deficit hyperactivity disorder; ASD: autism spectrum disorder; SD: standard deviation.
Aim 1: parent and child mental health trajectories
Differences between participants experiencing second-wave lockdown (Victorian) and ‘COVID-normal’ (non-Victorian) on parent and child mental health outcomes are presented in eTable 4 (visualized in Figure 1). State differences were not evident during the first national lockdown (April–June 2020) but parents were in the ‘mild’ elevated range on parent depression, top of normal range for anxiety and in the ‘mild’ elevated range for stress based on clinical cut-points (Brumby et al., 2011). There were substantial state differences in the second Victorian lockdown period (July–October). Victorian parents reported a second peak in parent and child mental health symptoms from mid-July 2020, while non-Victorians’ symptoms recovered and remained relatively stable. Victorian symptoms recovered in a steep decline from about September 2020 (i.e. end of the Victorian lockdown), returning to the levels of other states, and the lowest level of symptoms, in early February 2021. Late 2020 to May 2021 was a fairly stable period for Australia-wide, with very low COVID-19 infections, and only brief region-specific lockdowns. However, a third peak in mental health symptoms was evident from early April to the end of the study in May 2021. State differences were not evident for parent symptoms, but symptoms of child depression and anxiety appeared to be higher for Victorian children at this time.
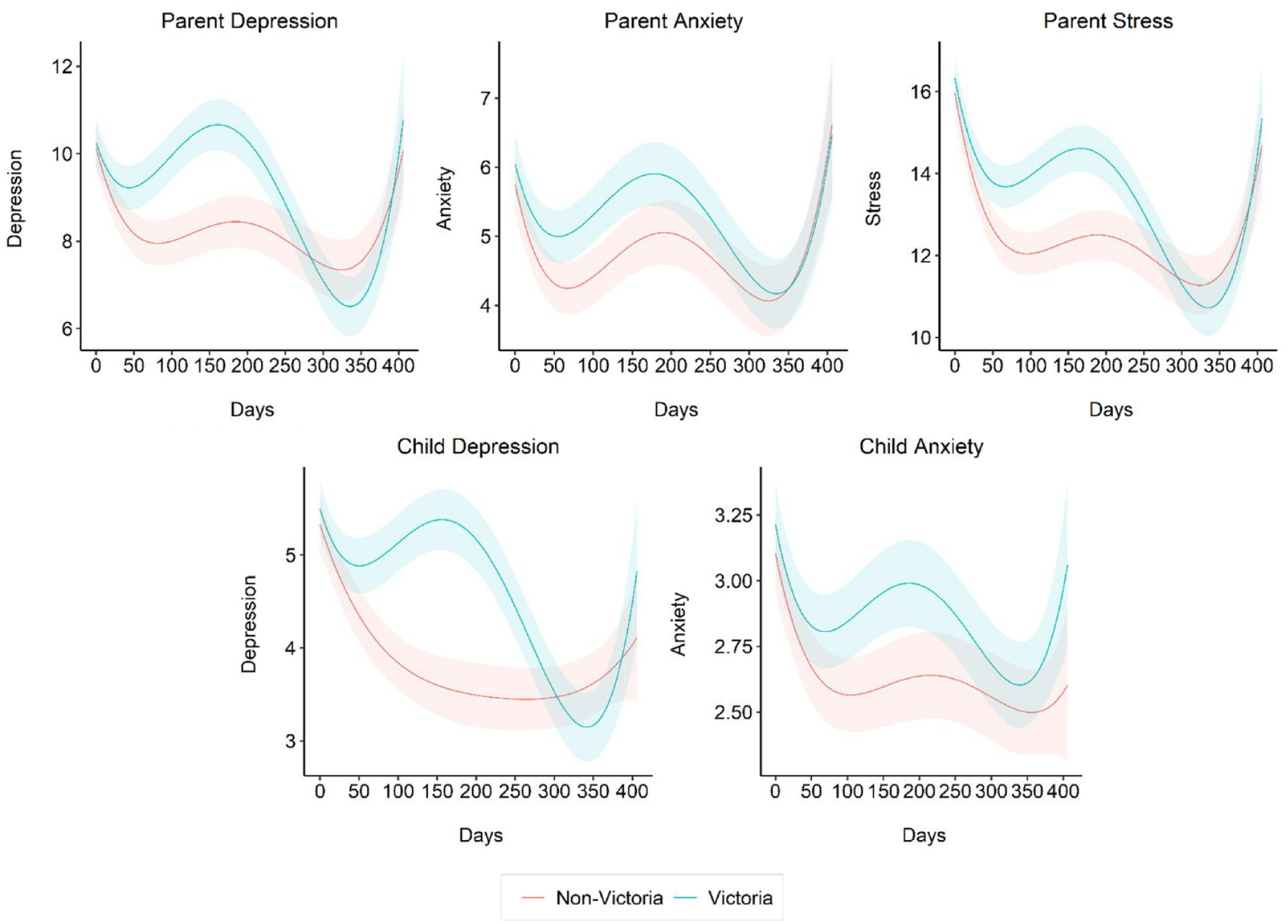
Estimated second-wave Victorian lockdown and COVID-normal non-Victorian trajectories of parent and child mental health outcomes with 95% confidence intervals. Notes: Model fit statistics used in the model building process for the full sample are presented in eTable 3. The first national lockdown occurred between days 1 and 45 (April–May 2020); the COVID-19 infection rate Victoria increased in late June 2020 (around day 74) and the second-wave Victorian lockdown occurred between days 85 and 180 (until 5 October 2020). There were easing restrictions from 180 days to approximately 300 days (early February 2021), when there was a third brief lockdown 11–18 February 2021), followed by easing restrictions to the end of the study.
Aim 2: predictors of parent and child mental health trajectories
Figures 2 and 3 summarize effect sizes for the associations between predictors and the five latent growth parameters for each outcome based on standardized regression coefficients from multilevel models. Full model output is presented in eTables 5–14. Our interactive online app (https://lingtax.shinyapps.io/CPAS_trend/) allows users to interact with model predictors to view effects on mental health trajectories in comparison to infection rates over time.
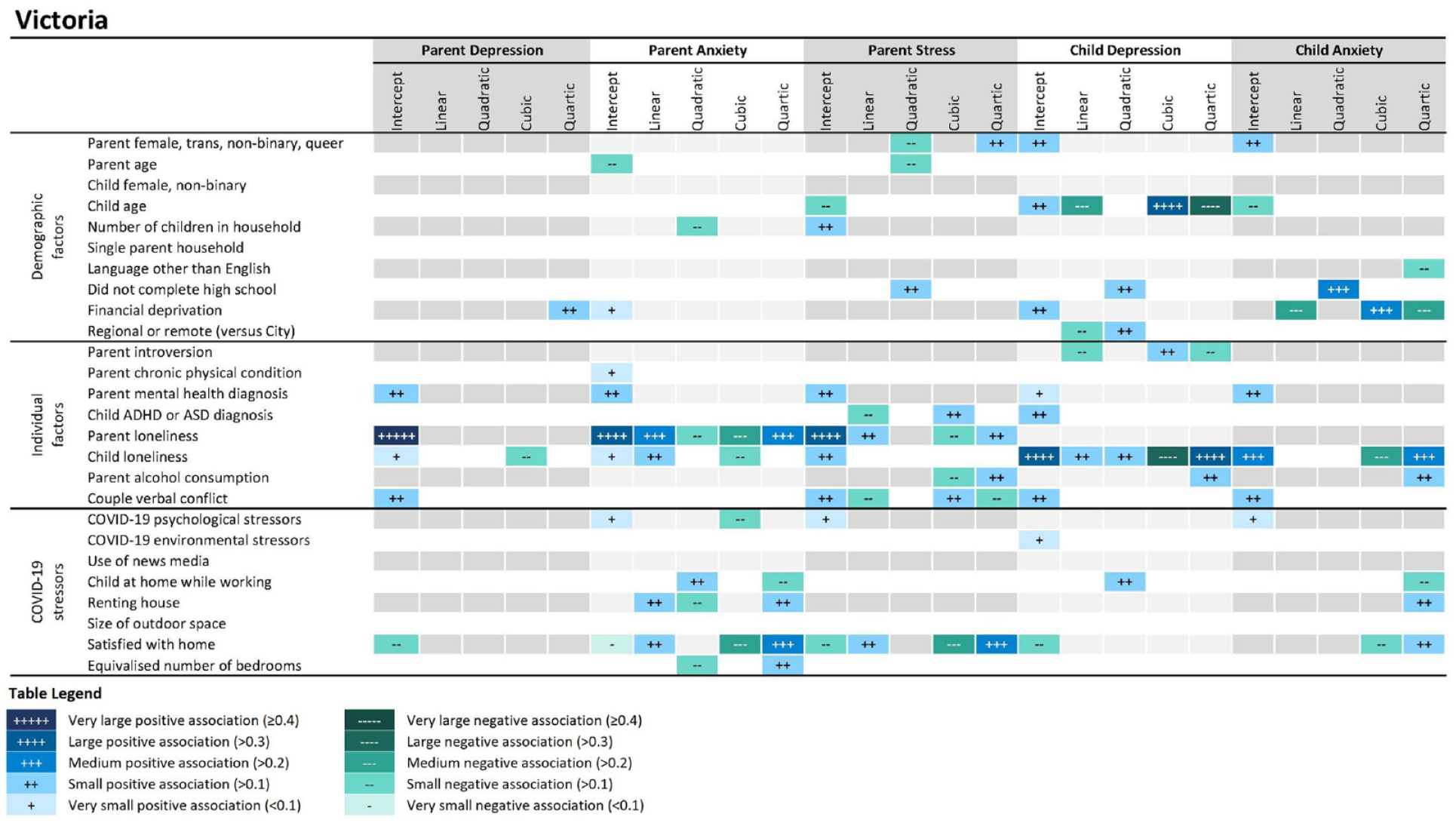
Second-wave locked-down Victorian parents: Effect sizes show the strength of associations between baseline predictors and growth parameters for parent and child mental health outcome. Notes: COVID-19 psychological stressors: parents’ feelings about the likelihood of catching COVID-19, and negative feelings when thinking about their ability to deal with COVID-19. COVID-19 environmental stressors: housing or financial insecurity, job loss, reduction/changes in employment, food shortages and COVID-19 illness in parent or family.
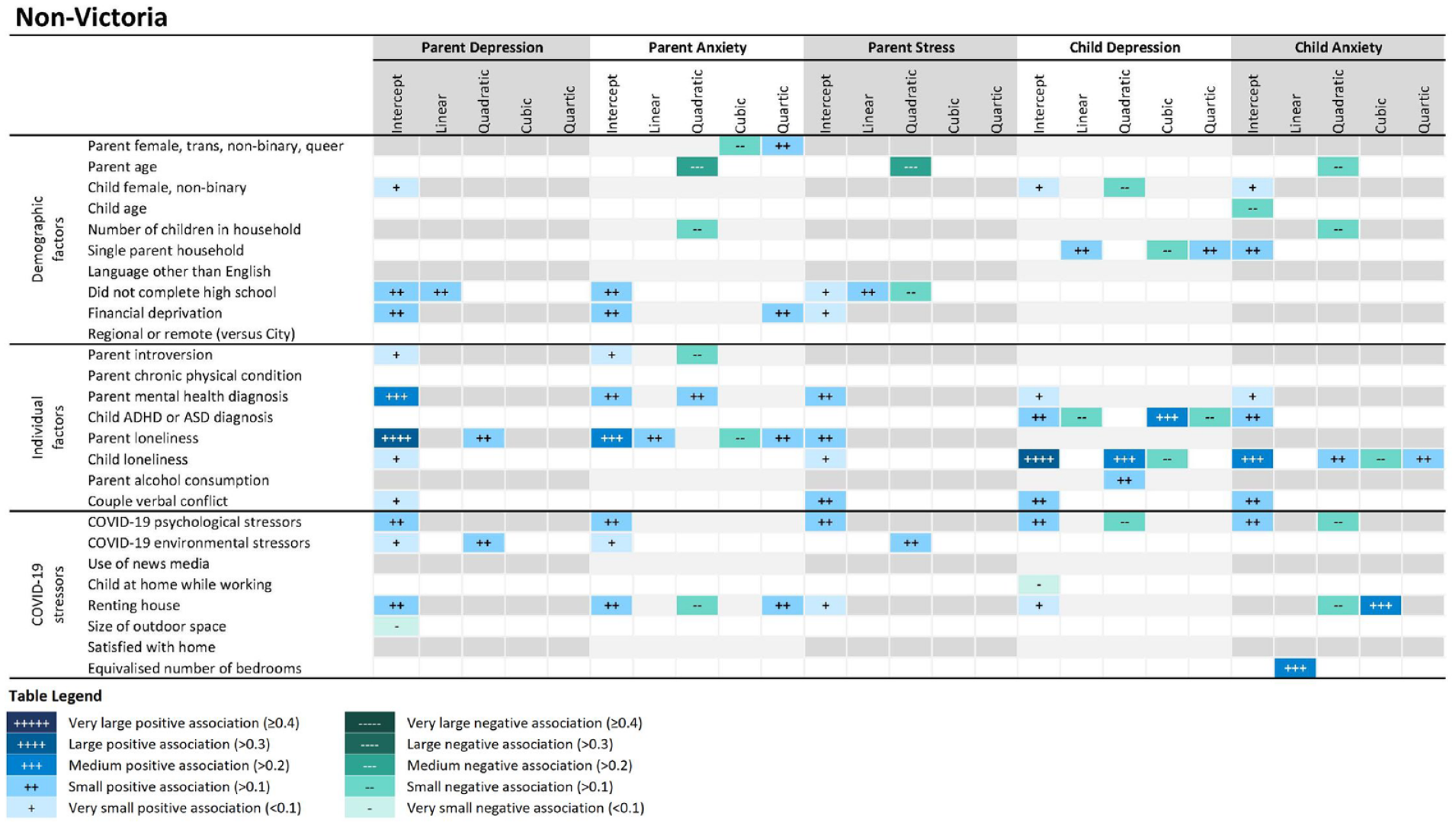
COVID-normal non-Victorian parents: effect sizes show the strength of associations between baseline predictors and growth parameters for parent and child mental health outcome. Notes: COVID-19 psychological stressors: parents’ feelings about the likelihood of catching COVID-19, and negative feelings when thinking about their ability to deal with COVID-19. COVID-19 environmental stressors: housing or financial insecurity, job loss, reduction/changes in employment, food shortages and COVID-19 illness in parent or family.
Demographic factors
For families in second-wave lockdown in Victoria, demographic predictors of parent and child mental health symptoms included parent gender, i.e. female, transgender, non-binary or queer gender, herein referred to as female/non-binary (parent stress; child depression, anxiety); younger parent age (parent anxiety, stress); younger child age (parent stress, child anxiety); older child age (child depression); larger family size (parent anxiety, stress); higher education (parent stress, anxiety); lower education (child anxiety); and financial deprivation (parent depression, anxiety; child depression, anxiety). Broadly, demographic risks were associated with increases in the overall trajectory, an elevated second peak in symptoms associated with the second-wave lockdown, and/or less recovery of symptoms into 2021. On demonstration in our interactive online app, financial deprivation and larger family size were particularly influential in worsening parents’ symptom trajectories. Furthermore, parents living in regional/remote areas (with a less restrictive lockdown compared to Melbourne city) reported a higher first peak and a lower second peak in child depression. Trajectories of child anxiety were somewhat lower in families speaking a language other than English.
For non-Victorian parents experiencing ‘COVID-normal’, parent female/non-binary gender (parent anxiety); younger parent age (parent anxiety, stress, child anxiety); child female/non-binary gender (parent depression; child depression, anxiety); younger child age (child anxiety); smaller family size (parent/child anxiety); single parent household (child depression, anxiety); low education (parent depression, anxiety; stress); and financial deprivation (parent depression, anxiety, stress) predicted worse symptom trajectories.
Individual parent and child factors
Individual factors predicting parent symptoms were fairly consistent across groups. For locked-down Victorian parents, parent extroversion (child depression); a chronic physical condition (parent anxiety); pre-existing parent mental health diagnoses (all outcomes); parent loneliness (parent depression, anxiety, stress); child loneliness (all outcomes); parent alcohol consumption (parent stress; child depression, anxiety); and couple conflict (parent depression, stress; child depression, anxiety) predicted higher mental health trajectories. Child ADHD/ASD diagnosis was associated with a later peak in parent stress and a higher overall trajectory of child depression. In COVID-normal Australia, parent introversion (parent depression, anxiety); pre-existing parent mental health diagnoses (all outcomes); child ADHD/ASD diagnosis (child depression, anxiety); parent loneliness (parent depression, anxiety, stress); child loneliness (parent depression, stress; child depression, anxiety); parent alcohol consumption (child depression); and couple conflict (parent depression, stress; child depression, anxiety) predicted worse trajectories. Across all states, the most marked effects consistently observed in the shiny app were for parent and child loneliness, pre-existing parent/child mental health conditions and couple conflict, increasing overall trajectories and second peaks for locked-down Victorians.
COVID-19-related stressors
For locked-down Victoria, predictors of symptom trajectories included COVID-19 psychological stressors (parent anxiety, stress; child anxiety); COVID-19 environmental stressors (child depression); renting (parent and child anxiety); and housing dissatisfaction (all outcomes). Parents juggling a child while working from home had a sharp increase in parent anxiety and a slight increase in child anxiety at the end of the second lockdown. In COVID-normal Australia, predictors included COVID-19 psychological stressors (all outcomes); COVID-19 environmental stressors (parent depression, anxiety, stress); renting (all outcomes); and smaller outdoor space (parent depression). Having a larger house with more bedrooms was associated with a slightly higher second peak in child anxiety. The most influential predictors were the effects of COVID-19 psychological and environmental stressors and housing (satisfaction, renting) on locked-down Victorians (see online app).
Discussion
The current study investigated Australia’s stratified experience of the COVID-19 pandemic during 2020. Using an online community sample, our findings provide evidence of substantially worse trajectories of parent and child mental health symptoms at the time of a second-wave COVID-19 outbreak and associated long-term, restrictive lockdowns. Trajectories shadowed 2020–2021 COVID-19 infection rates, with a first nation-wide peak in mental health symptoms matching the first national lockdown (April–June, 2020). A second, larger peak in symptoms was specific to Victoria occurring during the second-wave lockdown in July–October 2020, while the rest of Australia, in ‘COVID-normal’ conditions (minimal restrictions) showed relatively flat symptom trajectories over the same period. There was a steep recovery in Victorian mental health symptoms in late 2020 and early 2021, but then another substantial increase in parent (nation-wide) and child (particularly Victorian children) mental health symptoms in April–May 2021.
In examining baseline predictors of mental health trajectories, our findings provide means to identify high-risk parents and children early in future lockdowns and crisis events. Female/non-binary parent gender, large family size, parent and child loneliness, pre-existing parent/child mental health conditions, couple conflict, quality of housing (satisfaction, renting) and COVID-19 stressors (particularly psychological stressors) were consistently associated with worse overall symptom trajectories, an elevated second-wave peak in symptoms for Victorian parents and children, and a higher third peak in 2021.
We found specific indicators of increased risk. Mothers, in particular, experienced deterioration in their mental health. Evidence from around the world shows that women have been more likely to shoulder caregiving or distance education responsibilities associated with lockdowns (Collins et al., 2021). We didn’t test interactions, but an important next step will be to assess whether mothers are disproportionately affected by lockdowns compared to men. Our data also demonstrate the importance of psychological factors. Other pandemic studies have shown increased mental health risks for adults with pre-existing mental health conditions (Rosen et al., 2020; Wang et al., 2020a); our findings extend this literature by demonstrating these patterns in parents specifically and longitudinally. Pre-pandemic evidence also shows increased mental health symptomatology for children with ADHD and ASD (Joseph et al., 2019; Skokauskas and Gallagher, 2012); we showed worse mental health trajectories during lockdown in these children. Consistent with longitudinal UK parent data (Dickerson et al., 2020), we found worse trajectories associated with parent and child loneliness. Finally, increased rates of family conflict/violence have been well document during the pandemic (Holland et al., 2021; Usher et al., 2020). Our findings suggest broader detrimental effects, where couple conflict consistently predicted worse trajectories of mental health for both children and parents.
COVID-19 environmental stressors, related to housing or financial insecurity, employment, food shortages and COVID-19 illness, predicted worse mental health trajectories for parents but not children. Our findings align with previous findings in general adult populations (Duan et al., 2020; Fisher et al., 2020; Oosterhoff et al., 2020; Patrick et al., 2020), demonstrating these impacts specifically in the parent population, while also suggesting that these parents may be successful in shielding children from impact (Singh et al., 2020). Furthermore, aligned with evidence from mainly cross-sectional studies (Chung et al., 2020; Duan et al., 2020; Oosterhoff et al., 2020; Rosen et al., 2020; Xie et al., 2020), we found that COVID-19-related psychological stressors, such as parents’ worry, fear and concern, were associated with worse mental health trajectories for both parents and children. We also contribute the first pandemic research showing that housing factors, such as larger outdoor space and housing satisfaction, were protective and associated with lower peaks in parent and child mental health symptoms in both lockdown periods, consistent with pre-pandemic evidence (Knöchelmann et al., 2020).
The Australian natural experiment demonstrates short-term increased risk for parent and child mental health at the time of the second-wave COVID-19 outbreak in Victoria. There is potential for long-term public health impacts, given the cascade of known consequences associated with child/adult mental health problems, including healthcare costs and reduced work productivity (Knapp et al., 2011). After initial recovery in mental health symptoms at the end of 2020, we unexpectedly found that parent and child symptoms deteriorated again in March–May 2021. This time frame did not align with further extended lockdowns, but may represent increasing public uncertainty or weariness, particularly in light of Delta outbreaks around the world at that time. We also note that state differences in mental health symptoms cannot be causally linked to lockdown measures per se; international evidence shows a range of economic and social impacts of COVID-19 outbreaks independent of public health orders (Demirgüç-Kunt et al., 2021). We identified a set of factors that community/school workers and general practitioners could use to identify families most vulnerable to deterioration in mental health symptoms, including demographic (parent gender, family size, housing) and individual factors (pre-existing diagnoses, loneliness), and COVID-related stressors. Linked to these risks, our findings suggest the possible need for additional supports/interventions that can be delivered online, to provide (1) surveillance and supports for parents/children with pre-existing diagnoses (Kahl and Correll, 2020); (2) support to strengthen family relationships and reduce conflict (Braithwaite and Holt-Lunstad, 2017); and (3) strategies for increasing social connections to reduce loneliness. In regard to policy, our findings build empirical evidence for increasing financial support for financially stressed parents during and in the wake of the pandemic (Broadway et al., 2020), and investment in high-quality social housing. Finally, our data demonstrate the specific risk of lockdowns for mothers, and particularly those with multiple children. Public policy must consider how to mitigate long-term, cascading impacts related to socio-economic and employment/career gender inequalities, and ongoing mental health risks for women.
Our study has limitations. First, our study used an online recruitment approach, which on post hoc analysis yielded a close to representative sample on key baseline demographics, with the possibility of higher representation of parents with mental health problems or COVID-19 worries. While online samples may overrepresent participants from vulnerable subpopulations (Batterham, 2014), our final sample was somewhat more advantaged than the original recruited sample and were mostly mothers, thus may have under-represented outcomes for less advantaged families and fathers. Second, our study focused on baseline time-invariant predictors. Investigation of time-varying factors, such as changes in family circumstances and functioning over the pandemic, may provide additional insights into parent and child mental health. Third, given small numbers of children/parents identifying as non-binary, trans and queer gender, and to avoid excluding these parents, we combined these groups with female parents/children. This approach prevented a meaningful examination of mental health trajectories for non-binary/trans/queer gender parents/children. These groups have unique profiles of mental health risk (Russell and Fish, 2016), and in future should be examined separately. Fourth, for practical reasons, we were unable to collect child-reported or objective data for child mental health problems, which may have resulted in biased estimates of child mental health. Furthermore, we made necessary pragmatic decisions to select measures suitable for a wide age span of children. Although the internal reliability estimates for our measures of child depression and anxiety in younger children were relatively strong, these measures have not specifically been validated children under 6 years.
Our findings illustrate potential for substantial and increasing effects of strict lockdowns on parent/child mental health over time. These results may inform the management of lockdowns in regions still grappling with high prevalence of COVID-19, as well as insights for future crisis events. We identified several baseline factors, including parent and child loneliness, parent/child diagnoses, couple conflict and COVID-19 stressors, with utility for detecting high-risk families who are likely to require support early on in future lockdowns. Finally, there was a steep recovery in Victorian mental health symptoms after the second lockdown, and state differences disappeared for parent symptoms. Nevertheless, state differences appeared to remain for child symptoms, and there was another substantial increase in parent (nation-wide) and child (particularly Victorian children) mental health symptoms in April–May 2021. Thus, it is important that future longitudinal research monitors symptom recovery throughout the pandemic to determine whether mental health impacts are transitory or more enduring.
Supplemental Material
sj-docx-1-anp-10.1177_00048674211065365 – Supplemental material for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia
Supplemental material, sj-docx-1-anp-10.1177_00048674211065365 for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia by Elizabeth M Westrupp, Christopher J Greenwood, Matthew Fuller-Tyszkiewicz, Craig A Olsson, Emma Sciberras, Antonina Mikocka-Walus, Glenn A Melvin, Subhadra Evans, Mark A Stokes, Amanda G Wood, Gery C Karantzas, Jacqui A Macdonald, John W Toumbourou, Samantha J Teague, Julian W Fernando, Tomer S Berkowitz, Mathew Ling and George J Youssef in Australian & New Zealand Journal of Psychiatry
Supplemental Material
sj-docx-10-anp-10.1177_00048674211065365 – Supplemental material for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia
Supplemental material, sj-docx-10-anp-10.1177_00048674211065365 for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia by Elizabeth M Westrupp, Christopher J Greenwood, Matthew Fuller-Tyszkiewicz, Craig A Olsson, Emma Sciberras, Antonina Mikocka-Walus, Glenn A Melvin, Subhadra Evans, Mark A Stokes, Amanda G Wood, Gery C Karantzas, Jacqui A Macdonald, John W Toumbourou, Samantha J Teague, Julian W Fernando, Tomer S Berkowitz, Mathew Ling and George J Youssef in Australian & New Zealand Journal of Psychiatry
Supplemental Material
sj-docx-11-anp-10.1177_00048674211065365 – Supplemental material for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia
Supplemental material, sj-docx-11-anp-10.1177_00048674211065365 for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia by Elizabeth M Westrupp, Christopher J Greenwood, Matthew Fuller-Tyszkiewicz, Craig A Olsson, Emma Sciberras, Antonina Mikocka-Walus, Glenn A Melvin, Subhadra Evans, Mark A Stokes, Amanda G Wood, Gery C Karantzas, Jacqui A Macdonald, John W Toumbourou, Samantha J Teague, Julian W Fernando, Tomer S Berkowitz, Mathew Ling and George J Youssef in Australian & New Zealand Journal of Psychiatry
Supplemental Material
sj-docx-12-anp-10.1177_00048674211065365 – Supplemental material for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia
Supplemental material, sj-docx-12-anp-10.1177_00048674211065365 for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia by Elizabeth M Westrupp, Christopher J Greenwood, Matthew Fuller-Tyszkiewicz, Craig A Olsson, Emma Sciberras, Antonina Mikocka-Walus, Glenn A Melvin, Subhadra Evans, Mark A Stokes, Amanda G Wood, Gery C Karantzas, Jacqui A Macdonald, John W Toumbourou, Samantha J Teague, Julian W Fernando, Tomer S Berkowitz, Mathew Ling and George J Youssef in Australian & New Zealand Journal of Psychiatry
Supplemental Material
sj-docx-13-anp-10.1177_00048674211065365 – Supplemental material for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia
Supplemental material, sj-docx-13-anp-10.1177_00048674211065365 for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia by Elizabeth M Westrupp, Christopher J Greenwood, Matthew Fuller-Tyszkiewicz, Craig A Olsson, Emma Sciberras, Antonina Mikocka-Walus, Glenn A Melvin, Subhadra Evans, Mark A Stokes, Amanda G Wood, Gery C Karantzas, Jacqui A Macdonald, John W Toumbourou, Samantha J Teague, Julian W Fernando, Tomer S Berkowitz, Mathew Ling and George J Youssef in Australian & New Zealand Journal of Psychiatry
Supplemental Material
sj-docx-14-anp-10.1177_00048674211065365 – Supplemental material for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia
Supplemental material, sj-docx-14-anp-10.1177_00048674211065365 for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia by Elizabeth M Westrupp, Christopher J Greenwood, Matthew Fuller-Tyszkiewicz, Craig A Olsson, Emma Sciberras, Antonina Mikocka-Walus, Glenn A Melvin, Subhadra Evans, Mark A Stokes, Amanda G Wood, Gery C Karantzas, Jacqui A Macdonald, John W Toumbourou, Samantha J Teague, Julian W Fernando, Tomer S Berkowitz, Mathew Ling and George J Youssef in Australian & New Zealand Journal of Psychiatry
Supplemental Material
sj-docx-15-anp-10.1177_00048674211065365 – Supplemental material for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia
Supplemental material, sj-docx-15-anp-10.1177_00048674211065365 for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia by Elizabeth M Westrupp, Christopher J Greenwood, Matthew Fuller-Tyszkiewicz, Craig A Olsson, Emma Sciberras, Antonina Mikocka-Walus, Glenn A Melvin, Subhadra Evans, Mark A Stokes, Amanda G Wood, Gery C Karantzas, Jacqui A Macdonald, John W Toumbourou, Samantha J Teague, Julian W Fernando, Tomer S Berkowitz, Mathew Ling and George J Youssef in Australian & New Zealand Journal of Psychiatry
Supplemental Material
sj-docx-16-anp-10.1177_00048674211065365 – Supplemental material for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia
Supplemental material, sj-docx-16-anp-10.1177_00048674211065365 for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia by Elizabeth M Westrupp, Christopher J Greenwood, Matthew Fuller-Tyszkiewicz, Craig A Olsson, Emma Sciberras, Antonina Mikocka-Walus, Glenn A Melvin, Subhadra Evans, Mark A Stokes, Amanda G Wood, Gery C Karantzas, Jacqui A Macdonald, John W Toumbourou, Samantha J Teague, Julian W Fernando, Tomer S Berkowitz, Mathew Ling and George J Youssef in Australian & New Zealand Journal of Psychiatry
Supplemental Material
sj-docx-2-anp-10.1177_00048674211065365 – Supplemental material for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia
Supplemental material, sj-docx-2-anp-10.1177_00048674211065365 for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia by Elizabeth M Westrupp, Christopher J Greenwood, Matthew Fuller-Tyszkiewicz, Craig A Olsson, Emma Sciberras, Antonina Mikocka-Walus, Glenn A Melvin, Subhadra Evans, Mark A Stokes, Amanda G Wood, Gery C Karantzas, Jacqui A Macdonald, John W Toumbourou, Samantha J Teague, Julian W Fernando, Tomer S Berkowitz, Mathew Ling and George J Youssef in Australian & New Zealand Journal of Psychiatry
Supplemental Material
sj-docx-3-anp-10.1177_00048674211065365 – Supplemental material for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia
Supplemental material, sj-docx-3-anp-10.1177_00048674211065365 for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia by Elizabeth M Westrupp, Christopher J Greenwood, Matthew Fuller-Tyszkiewicz, Craig A Olsson, Emma Sciberras, Antonina Mikocka-Walus, Glenn A Melvin, Subhadra Evans, Mark A Stokes, Amanda G Wood, Gery C Karantzas, Jacqui A Macdonald, John W Toumbourou, Samantha J Teague, Julian W Fernando, Tomer S Berkowitz, Mathew Ling and George J Youssef in Australian & New Zealand Journal of Psychiatry
Supplemental Material
sj-docx-4-anp-10.1177_00048674211065365 – Supplemental material for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia
Supplemental material, sj-docx-4-anp-10.1177_00048674211065365 for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia by Elizabeth M Westrupp, Christopher J Greenwood, Matthew Fuller-Tyszkiewicz, Craig A Olsson, Emma Sciberras, Antonina Mikocka-Walus, Glenn A Melvin, Subhadra Evans, Mark A Stokes, Amanda G Wood, Gery C Karantzas, Jacqui A Macdonald, John W Toumbourou, Samantha J Teague, Julian W Fernando, Tomer S Berkowitz, Mathew Ling and George J Youssef in Australian & New Zealand Journal of Psychiatry
Supplemental Material
sj-docx-5-anp-10.1177_00048674211065365 – Supplemental material for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia
Supplemental material, sj-docx-5-anp-10.1177_00048674211065365 for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia by Elizabeth M Westrupp, Christopher J Greenwood, Matthew Fuller-Tyszkiewicz, Craig A Olsson, Emma Sciberras, Antonina Mikocka-Walus, Glenn A Melvin, Subhadra Evans, Mark A Stokes, Amanda G Wood, Gery C Karantzas, Jacqui A Macdonald, John W Toumbourou, Samantha J Teague, Julian W Fernando, Tomer S Berkowitz, Mathew Ling and George J Youssef in Australian & New Zealand Journal of Psychiatry
Supplemental Material
sj-docx-6-anp-10.1177_00048674211065365 – Supplemental material for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia
Supplemental material, sj-docx-6-anp-10.1177_00048674211065365 for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia by Elizabeth M Westrupp, Christopher J Greenwood, Matthew Fuller-Tyszkiewicz, Craig A Olsson, Emma Sciberras, Antonina Mikocka-Walus, Glenn A Melvin, Subhadra Evans, Mark A Stokes, Amanda G Wood, Gery C Karantzas, Jacqui A Macdonald, John W Toumbourou, Samantha J Teague, Julian W Fernando, Tomer S Berkowitz, Mathew Ling and George J Youssef in Australian & New Zealand Journal of Psychiatry
Supplemental Material
sj-docx-7-anp-10.1177_00048674211065365 – Supplemental material for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia
Supplemental material, sj-docx-7-anp-10.1177_00048674211065365 for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia by Elizabeth M Westrupp, Christopher J Greenwood, Matthew Fuller-Tyszkiewicz, Craig A Olsson, Emma Sciberras, Antonina Mikocka-Walus, Glenn A Melvin, Subhadra Evans, Mark A Stokes, Amanda G Wood, Gery C Karantzas, Jacqui A Macdonald, John W Toumbourou, Samantha J Teague, Julian W Fernando, Tomer S Berkowitz, Mathew Ling and George J Youssef in Australian & New Zealand Journal of Psychiatry
Supplemental Material
sj-docx-8-anp-10.1177_00048674211065365 – Supplemental material for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia
Supplemental material, sj-docx-8-anp-10.1177_00048674211065365 for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia by Elizabeth M Westrupp, Christopher J Greenwood, Matthew Fuller-Tyszkiewicz, Craig A Olsson, Emma Sciberras, Antonina Mikocka-Walus, Glenn A Melvin, Subhadra Evans, Mark A Stokes, Amanda G Wood, Gery C Karantzas, Jacqui A Macdonald, John W Toumbourou, Samantha J Teague, Julian W Fernando, Tomer S Berkowitz, Mathew Ling and George J Youssef in Australian & New Zealand Journal of Psychiatry
Supplemental Material
sj-docx-9-anp-10.1177_00048674211065365 – Supplemental material for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia
Supplemental material, sj-docx-9-anp-10.1177_00048674211065365 for Parent and child mental health trajectories April 2020 to May 2021: Strict lockdown versus no lockdown in Australia by Elizabeth M Westrupp, Christopher J Greenwood, Matthew Fuller-Tyszkiewicz, Craig A Olsson, Emma Sciberras, Antonina Mikocka-Walus, Glenn A Melvin, Subhadra Evans, Mark A Stokes, Amanda G Wood, Gery C Karantzas, Jacqui A Macdonald, John W Toumbourou, Samantha J Teague, Julian W Fernando, Tomer S Berkowitz, Mathew Ling and George J Youssef in Australian & New Zealand Journal of Psychiatry
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship and/or publication of this article: E.M.W., A.M.-W. and G.C.K. were supported by Deakin Faculty of Health Mid-Career Fellowships. E.S. was supported by an NHMRC Career Development Fellowship (1110688) and a veski Inspiring Women’s Fellowship.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
