Abstract
Background:
Exercise offers improvement to physical and mental health symptoms as well and cognitive function in patients with psychosis. However, patients with psychosis are often less ready to benefit from exercise intervention because of the difficulties in motivation. This study aimed to examine the effectiveness of adjunctive motivational coaching on exercise intervention in women with psychosis in Hong Kong.
Methods:
From a community mental health programme for women, patients with a diagnosis of psychotic disorder (within 5 years of first onset) were randomly allocated to receive 12 30-minute sessions of motivational coaching or psychoeducation in a group format. Both groups additionally received exercise intervention sessions consisting of yoga, stretching and high-intensity interval training. Primary outcome was the total physical activity level measured by the International Physical Activity Questionnaire.
Results:
Fifty-seven patients (mean [SD] age, 34.47 [12.44] years) were randomised into motivational coaching (n = 30) or psychoeducation (n = 27) treatment groups. The motivational coaching group had a significantly higher total physical activity level (4601.67 [686.59] vs 2524.82 [723.73] metabolic equivalent task-min/week, r2 = 0.473, p = 0.04) after the intervention and at 6 months post-intervention. Moderate and light physical activity levels were significantly higher in the motivational coaching group after intervention and at 6 months, respectively. Additionally, symptoms of bizarre behaviour were improved in the motivational coaching group at 6 months. Younger, unemployed, unmarried and those with longer durations of untreated psychosis generally showed larger improvements in the motivational coaching group.
Conclusion:
Motivational coaching may augment the effects of exercise interventions, as reflected by higher physical activity participation. Motivational coaching augmentation has the potential to further improve exercise intervention outcomes.
Introduction
In the past decade, exercise interventions have proven to produce positive outcomes in patients with psychosis, garnering the attention of health professionals (Chalfoun et al., 2016; Firth et al., 2015; Vancampfort et al., 2015). In addition to the physical health benefits through reducing the risk of cardiovascular disease (Chalfoun et al., 2016; Firth et al., 2015; Vancampfort et al., 2015), a meta-analysis reported moderate to significant effects in cognitive function improvement, mainly in working memory, social cognition, and attention or vigilance (Firth et al., 2017). The effects on cognitive function have been mostly reported with aerobic exercise and yoga, and also with resistance training, ball games and high-intensity interval training (HIIT) (Firth et al., 2017; Romain et al., 2019). Emerging evidence also reported small effect of aerobic exercise in improving negative symptoms, such as loss of emotional feeling and apathy, which are not improved by pharmacological treatments (Sabe et al., 2020).
Despite the proven benefits of exercise, patients with psychosis are more likely to lead a sedentary life compared to the general population. Several studies have reported difficulties in motivation as the reason (Beebe et al., 2011; Gorczynski and Faulkner, 2010; Soundy et al., 2014). The difficulties in motivation in patients with psychosis may be related to the severity of negative symptoms (Vancampfort et al., 2013) or the lack of knowledge of the benefits that exercise may have on their recovery (Rastad et al., 2014). Previous studies have shown that motivation is significantly associated with increased attendance (Archie et al., 2003), more active participation during the intervention (Beebe et al., 2012), improved self-efficacy (Beebe et al., 2011) and stronger autonomic regulation (Vancampfort et al., 2013), ultimately leading to an increase in physical activity (PA) levels. These findings highlight the importance of motivation for establishing and maintaining PA habits in patients with psychosis (Firth et al., 2016). Despite its importance, few studies have investigated the effects of motivational intervention on improving the efficacy of exercise interventions.
Coaching is a promising empowerment-based intervention, but its use in patients with mental health problems has not been widely studied (Bishop et al., 2018). Traditionally, coaching has been used in sports (Merian and Snyder, 2015) and business (Ladyshewsky, 2017) to improve trainee performance. In healthcare, coaching focuses on establishing and achieving health promotion goals that lead to changes in lifestyle-related behaviours, reducing health risks and improving quality of life (Van Ryn, 1997). The use of health coaches has increased in recent decades. The introduction of a health coach in primary care settings has led to a significant increase in exercise levels in more than half of healthy participants (Adelman and Graybill, 2005; Tidwell et al., 2004). The beneficial effects of coaching intervention or interventions with similar approach where development and implementation of patient-centred goal setting have also been reported in patients with psychosis, for weight control through modifying habits in PA and diet (Alvarez-Jimenez et al., 2006; Blouin et al., 2009; Curtis et al., 2016; Fredrikson et al., 2014; Lovell et al., 2014; Selby et al., 2021). While these studies provided evidence that coaching intervention can improve cardiometabolic risk in psychosis, its effect solely on PA engagement still requires further investigation.
This study focused on women with psychotic disorders because the negative consequences of the disorder may spread more to others around them, as they are often the principal caregivers for children, the elderly and the sick in a family (Sharma et al., 2016). The disability associated with psychosis can interfere with the quality of care. A previous study also revealed that married women with schizophrenia were less likely to be cared for by their husband than men with schizophrenia who were cared for by their wife (Thara, 1998). In this study, we proposed to investigate motivational coaching (MC) as an adjunct to exercise interventions to address the difficulties in motivation to exercise in women with psychotic disorders. Women, who often play a caring role, may easily focus on the distress ahead and overlook the resources available to them or the capacity they possess (Hirst, 2005). It is believed that MC could be particularly useful in reminding them of the resources that they have and how to make good use of them.
In this study, the MC intervention was examined against psychoeducation (PE) which is one of the most commonly used pharmacological and cost-effective approaches to intervene patients’ health-related behaviours (Fernandez-Abascal et al., 2021). The primary objective of the current study was to examine the effects of MC and PE on PA level. The secondary objective was to explore whether any subgroup would show better improvement after receiving MC as an augmentation treatment. The PA level was set as the key domain of interest, instead of the exercise level (which means a more structured, planned, repetitive and intentional movement), because it is more commonly reported in the literature and the guidelines available for patients with psychosis mainly describes PA (e.g. Firth et al., 2015). This approach should facilitate our discussion of how our findings compare with those in the literature.
We hypothesised that compared to the PE group, the MC group would engage more in PA and demonstrate greater improvement in the severity of psychotic and mood symptoms. We also hypothesised that the better overall function at post-intervention could be maintained for a longer term.
Methods
Study design
This study was a prospective, two-arm, parallel-group, open-label randomised controlled trial conducted as part of the Jockey Club Mental Wellness Project for Women (JCWOW) organised by the University of Hong Kong (ClinicalTrials.gov Identifier: NCT03751852). The study was conducted from October 2018 to March 2021. Eligible women diagnosed with psychotic disorders who provided written informed consent were randomly assigned to the MC or PE group. Participants received no financial compensation. Ethical approval was obtained from the Research Ethics Committee, Kowloon West Cluster Hospital Authority in Hong Kong (Reference no.: KW/EX-16-041 (96-23)). This study was conducted according to the Consolidated Standards of Reporting Trials (CONSORT) reporting guidelines.
Participants
Research staff invited female patients from the outpatient clinic at the psychiatry unit in Kwai Chung Hospital (KCH) to participate in this study. Community partners in the KCH catchment area treating patients with psychosis could also refer potential participants to our research staff by telephone. Eligibility criteria included women between 18 and 64 years of age, with a previous diagnosis of schizophrenia, schizoaffective disorder, schizophreniform disorder, brief psychotic disorder, psychosis not otherwise specified or delusional disorder (as defined by the Diagnostic and Statistical Manual of Mental Disorders, 5th ed.), with the first onset of symptoms in the past 5 years. Additionally, the ability to communicate in Cantonese and physical fitness, as defined by negative responses to all seven conditions listed in the Physical Activity Readiness Questionnaire (PAR-Q), were required. Exclusion criteria included participants with severe physical illness or other contraindications to exercise, comorbid substance dependence, organic brain disease, known history of intellectual disability or attendance to special needs schools, or other mental conditions requiring treatment prioritisation, such as suicidal ideation.
Eligible subjects who agreed to be randomly allocated to receive MC or PE and participate in a yoga-based, stretching and HIIT exercise intervention programme were required to provide written informed consent and complete a baseline assessment interviewed by the research staff. Following these procedures, participants were individually randomised 1:1 to receive MC or PE via centralised computer-generated allocation sequences.
Interventions
The MC group received 12 (eight weekly, followed by four biweekly) 30-minute MC sessions in a group format with three to four participants (see Supplementary Material for details). The PE group received PE at the same frequency as the MC group (see Supplementary Material). In both groups, each session was followed by 30 minutes of full body stretching and HIIT focusing on cardiovascular functions (e.g. marching, jogging, skipping) and muscle strengths (e.g. forward lunges, chair plank, squat) (see Supplementary Material). The abovementioned MC, PE and exercise sessions were delivered by trained researcher and social workers. Additionally, weekly yoga sessions were offered to participants, by licensed yoga instructors, in both groups for 16 weeks on a different day from the primary intervention.
Outcome measures
Baseline, post-intervention and 6-month post-intervention outcomes were measured using standardised interviews conducted by the research staff. Data collected included demographics, diagnosis, psychotic symptoms, functioning, duration of untreated psychosis (DUP), psychiatric comorbidities, previous hospitalisations and current PA level.
Participant data on psychiatric diagnosis, psychiatric comorbidities and history of hospitalisations were obtained from centralised hospital records. DUP was determined using the Interview for the Retrospective Assessment of the Onset of Schizophrenia (Häfner et al., 1992).
The primary outcome was the total PA level, measured with the International Physical Activity Questionnaire (IPAQ) (Craig et al., 2003) after the intervention. The IPAQ is a 27-item self-report questionnaire where participants report the duration (minutes) and frequency of PA for the past 7 days at light, moderate and vigorous intensities. The total PA level was reported in metabolic equivalent task-minute per week (MET-min/week) according to the scoring protocol (Ipaq Research Committee, 2005).
Secondary outcomes included the total PA level measured at 6 months post-intervention and the following measures immediately and 6 months after the intervention: PA levels aggregated into light, moderate and vigorous intensities, measured by the IPAQ, psychotic symptoms, functioning and mood at both time points. Psychotic symptoms were measured using the Positive and Negative Syndrome Scale (PANSS) (Kay et al., 1987), the Scale for the Assessment of Positive Symptoms (SAPS) (Andreasen, 1984) and the Scale for the Assessment of Negative Symptoms (SANS) (Andreasen, 1989). The Social and Occupational Functioning Assessment Scale (SOFAS) was used to measure participant’s overall functioning (Goldman et al., 1992). Mood symptoms were measured using the Calgary Depression Scale for Schizophrenia (CDSS) (Addington et al., 1996) and Young’s Mania Rating Scale (YMRS) (Young et al., 1978).
Statistical analysis
Since there was no comparable study in the literature at the time this study was designed, the sample size was calculated by estimating that the post-intervention total PA level in the MC group would be 15% higher than in the PE group. The sample size needed to demonstrate that this difference was calculated to 38 (power 80%, significance level 5%). The total sample size was estimated to be 54, with a 30% attrition.
Statistical analyses were performed using SPSS Statistics version 26.0 software (IBM Corp. Released, 2019). All tests were two-sided, with p < 0.05 considered statistically significant. Intention-to-treat analyses included all participants who were randomised. Missing data were treated using the ‘last observation carried forward’ approach. Baseline comparability was assessed using the chi-square test for categorical variables and the independent t-test for continuous variables or the appropriate nonparametric test when normality assumption was violated. Analysis of covariance (ANCOVA) was performed by adjusting the corresponding baseline values of the outcome measure and variables with baseline differences to examine the between-group differences. Multiple testing correction was performed using the Benjamini–Hochberg procedure with a false discovery rate of 5%.
Two-way ANCOVAs were used for subgroup analyses to examine whether the effects of MC were more pronounced in specific demographic and clinical subgroups. Factors examined included age (below vs equal to or above 30), diagnosis (schizophrenia vs non-schizophrenia), education (below vs above tertiary), employment (yes vs no), marital status (single vs other) and DUP (below vs above median). The findings of the subgroup analysis should help us understand which demographical or clinical subgroups of patients may be more benefitted by the MC intervention.
Results
Participant characteristics
From 15 November 2018 to 31 December 2019, a total of 192 women diagnosed with psychosis were screened for inclusion. Of these, 57 were randomly assigned to the MC (n = 30) or PE (n = 27) group (Figure 1). Retention rates were 64.9% at immediate post-intervention and 82.5% at 6 months post-intervention follow-ups. No differences in retention rates were observed between groups.
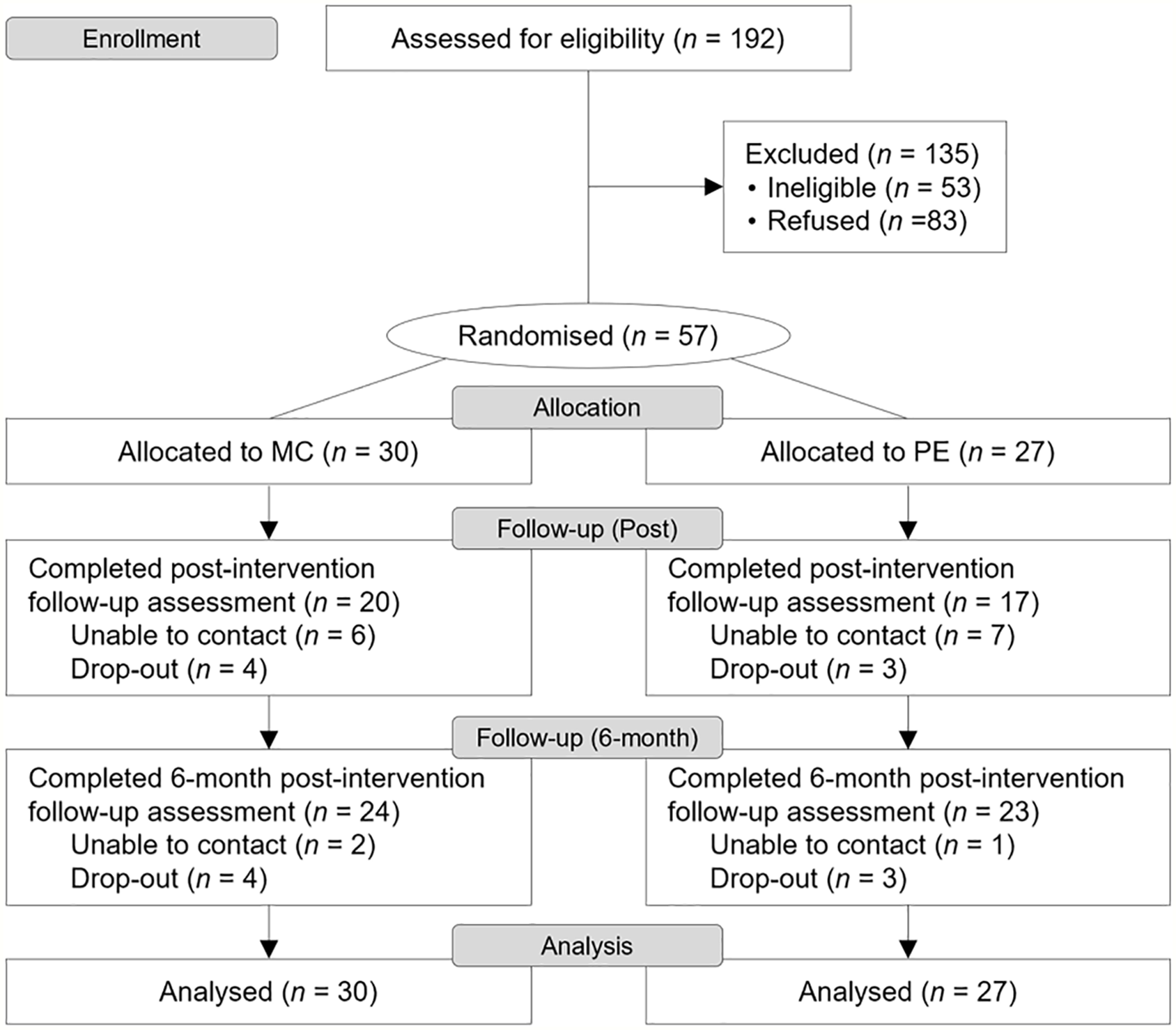
CONSORT diagram of participant flow through the trial.
The groups were demographically matched at baseline (Table 1). Mean (SD) age was 34.47 (12.44) years, and mean (SD) education was 13.60 (2.45) years. Thirty-seven (64.9%) participants were single, and 25 (43.9%) were employed. Thirty-seven (64.9%) participants met the DSM-5 diagnostic criteria for schizophrenia, and nine (15.8%) had comorbid disorders in multiple domains (e.g. anxiety and depression). The median DUP was 4 months (range, 0.56–22.21 months), and the majority of participants had at least one previous hospitalisation (n = 41, 71.9%). The two groups were clinically similar at baseline, except for a higher SANS alogia score (mean = 2.61 [SD = 0.88] vs 0.37 [0.26], p = 0.02) and lower SOFAS score (59.10 [1.88] vs 65.81 [2.02], p = 0.02) in the MC group and a higher SAPS hallucination score (3.48 [SD = 1.16] vs 0.96 [0.67], p = 0.007) in the PE group. PA levels for both groups were similar at baseline (Table 1).
Participant baseline characteristics.
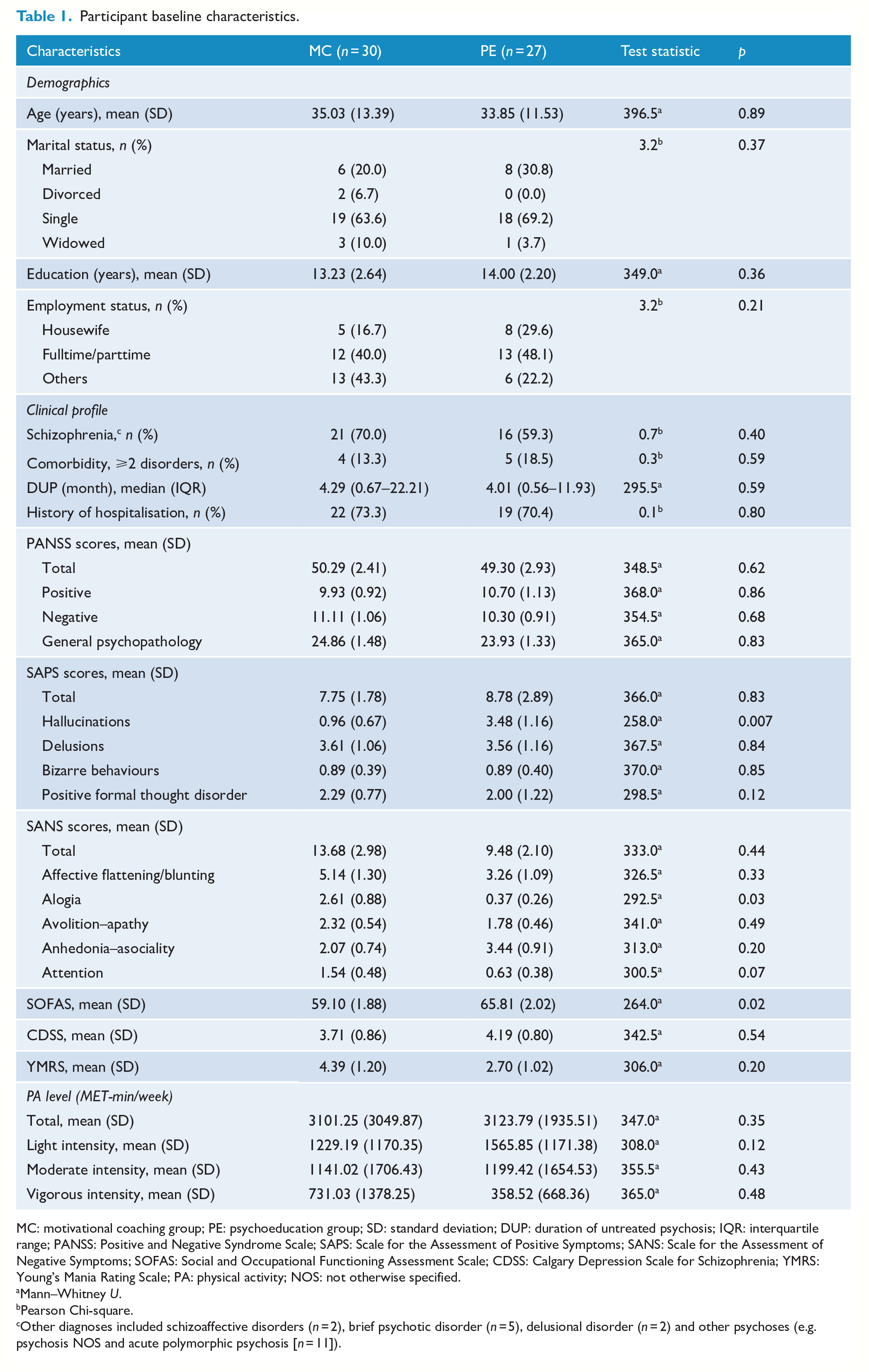
MC: motivational coaching group; PE: psychoeducation group; SD: standard deviation; DUP: duration of untreated psychosis; IQR: interquartile range; PANSS: Positive and Negative Syndrome Scale; SAPS: Scale for the Assessment of Positive Symptoms; SANS: Scale for the Assessment of Negative Symptoms; SOFAS: Social and Occupational Functioning Assessment Scale; CDSS: Calgary Depression Scale for Schizophrenia; YMRS: Young’s Mania Rating Scale; PA: physical activity; NOS: not otherwise specified.
Mann–Whitney U.
Pearson Chi-square.
Other diagnoses included schizoaffective disorders (n = 2), brief psychotic disorder (n = 5), delusional disorder (n = 2) and other psychoses (e.g. psychosis NOS and acute polymorphic psychosis [n = 11]).
Primary outcome measure
Post-intervention, the MC group had a higher total PA level than the PE group (4601.67 [686.59] MET-min/week vs 2524.82 [723.73] MET-min/week, r2 = 0.473, p = 0.04) after adjusting for the baseline total PA level, SAPS hallucination score, SANS alogia score and SOFAS score (Figure 2).
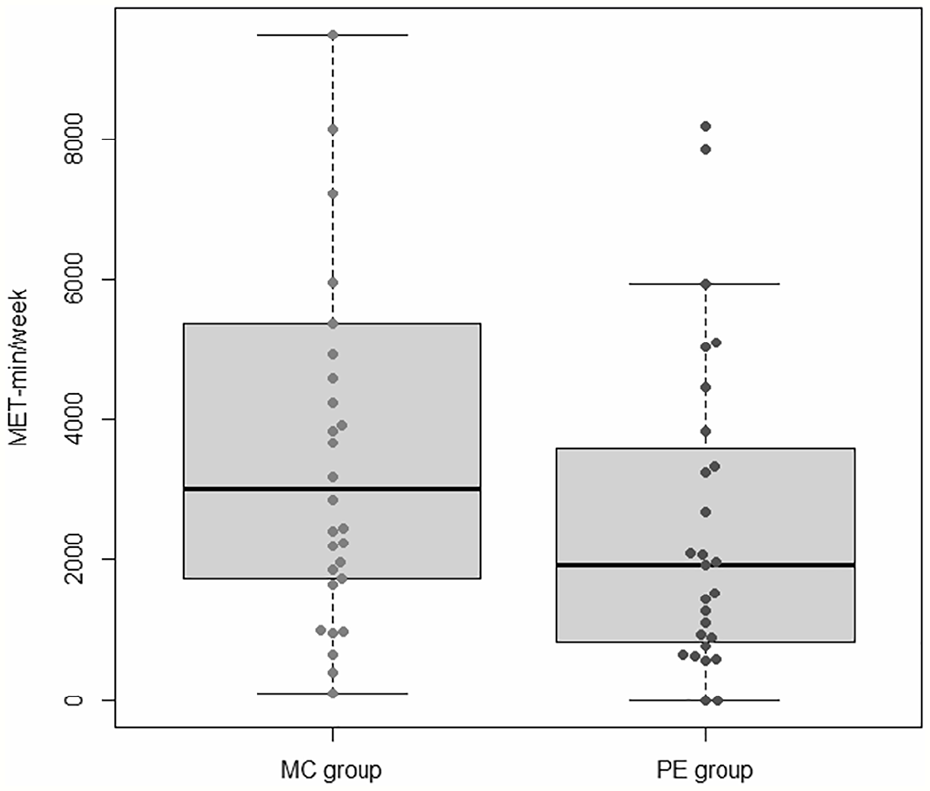
Total post-intervention physical activity level (primary outcome).
Secondary outcome measures
After the intervention, the MC group had significantly higher moderate-intensity PA levels (1249.38 [1566.94] vs 504.08 [932.52] MET-min/week, r2 = 0.364, p = 0.02) (Table 2).
Secondary outcome measurements.
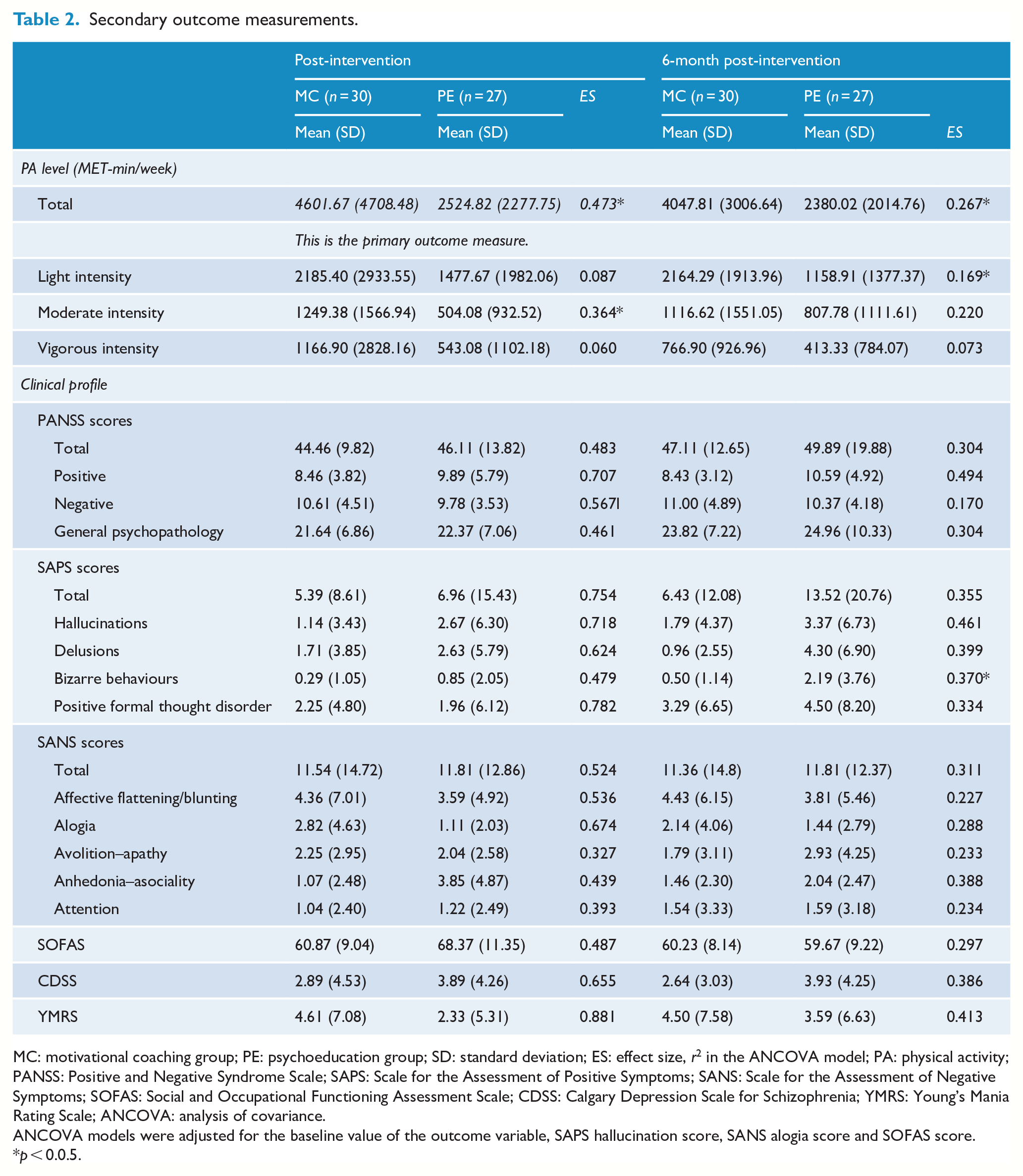
MC: motivational coaching group; PE: psychoeducation group; SD: standard deviation; ES: effect size, r2 in the ANCOVA model; PA: physical activity; PANSS: Positive and Negative Syndrome Scale; SAPS: Scale for the Assessment of Positive Symptoms; SANS: Scale for the Assessment of Negative Symptoms; SOFAS: Social and Occupational Functioning Assessment Scale; CDSS: Calgary Depression Scale for Schizophrenia; YMRS: Young’s Mania Rating Scale; ANCOVA: analysis of covariance.
ANCOVA models were adjusted for the baseline value of the outcome variable, SAPS hallucination score, SANS alogia score and SOFAS score.
p < 0.0.5.
At 6 months post-intervention, the MC group had significantly higher total PA levels (4047.81 [3006.64] vs 2380.02 [2014.76] MET-min/week, r2 = 0.267, p = 0.02) and light-intensity PA levels (2164.29 [1913.96] vs 1158.91 [1377.37] MET-min/week, r2 = 0.169, p = 0.03) and lower scores on the SAPS bizarre behaviour (0.50 [1.14] vs 2.19 [3.76], r2 = 0.370, p = 0.01).
Subgroup analyses
Subgroup analyses examined the effects of age, education, employment, marital status, diagnosis and DUP on outcome measures. Participants with a better response to the MC intervention were younger, unemployed, unmarried and had longer DUP. These participants showed significant improvement in PA engagement, psychotic symptoms and mood symptoms (Supplementary Material S2, S5, S6 and S7). The education and diagnosis subgroup results were inconclusive in this sample (Supplementary Material S3 and S4).
Discussion
This study revealed that women diagnosed with psychosis in Hong Kong engaged in an average of 40.3 minutes of moderate-to-vigorous PA (MVPA) per day, which has met the beneficial amount of MVPA on physical and mental health outcomes in schizophrenia patients suggested by Firth et al. (i.e. 90 minutes of MVPA per week) (Firth et al., 2015). This finding implies that any interventions that help our participants maintain baseline levels of MVPA would lead to better health outcomes. However, the amount of MVPA achieved by our participants is approximately 15% lower than the overall rate found in a previous meta-analysis in mixed-gender patients (i.e. 47.1 minutes/day) (Stubbs et al., 2016), suggesting that our study participants may be at higher risk for physical health and recovery compared to patients with psychotic disorders in other study cohorts.
The importance of motivation for exercise and its subsequent benefits for patients with severe mental illness is well established (Firth et al., 2016). This study is among the few that have explored the issue of difficulties in motivation in exercise interventions which warrants further investigation. In this study, total PA levels at post-intervention were higher in participants who received MC than those who received PE, and the effect could still be observed 6 months later. This finding is consistent with a previous pilot reporting that coaching, which emphasises the setting of a self-identified goal, can increase total PA levels in patients with severe mental illness (Williams et al., 2019). Our findings are also in line with studies reporting that the support granted through coaching may encourage patients to continue exercising when they encounter challenges (Carpiniello et al., 2013; Firth et al., 2016). With MC, participants could gain support from other group members, potential barriers to achieving PA goals could be discussed and solutions could be considered. Additionally, participants could benefit from the support provided by the coach by gaining confidence in creating and maintaining PA habits (Soundy et al., 2014). Having someone to ‘give you a push’ and ‘go with you’ can also help patients cope with self-infliction and keep themselves physically active (Rastad et al., 2014).
Our finding that the effects of MC last up to 6 months suggests that MC may be a suitable adjunctive intervention to maintain the beneficial effects of exercise interventions for a longer term, as Firth et al. (2018) had previously reported that the effectiveness of the exercise intervention on PA engagement might decline over time. Our findings have added value to the literature by demonstrating that MC might help sustain the effect of the exercise intervention for 6 months. We hypothesise that the sustained effects on our participants resulted from greater encouragement to create PA habits in the MC group. Based on this positive finding, further studies with a longer follow-up period (e.g. 12 months) are highly recommended.
Subgroup analyses revealed that patients who were younger, unemployed, unmarried and had DUP > 4 months had better improvement after receiving the MC. Given this finding, future MC interventions could target these groups given that they have been shown to be more effective in these groups. While it is well known that prolonged DUP is associated with poorer prognosis and health outcomes (Marshall et al., 2005; Norman et al., 2005), our findings suggest that MC as an adjunct to exercise intervention can potentially improve the long-term outcomes in patients with prolonged DUP.
Our study has several limitations. First, due to limited resources, the current study used a self-report measure of PA level instead of using an objective measurement device, such as actigraphy. Thus, results may be biased by participants’ subjective perceptions of their PA behaviours. Second, a post-intervention attrition rate of greater than 30% suggests that survival bias may have been present, and the results should be interpreted with caution. Third, the sample size for the subgroup analysis may have been too small, and further studies with bigger samples are needed to confirm the observed results. Fourth, because this study focused on female patients, the generalisability of the results to male patients with psychosis remains unclear. Future studies evaluating the MC intervention in male patients are warranted. Finally, the inconclusive results in subgroup analysis on education and diagnosis warrant further investigation. Concerning education level, a previous study reported that participants with higher education levels had a better sense of control over their PA habits (Droomers et al., 2001) and had better PA levels. While perceived control has been reported in the past as a strong predictor of behaviour change (Landau, 1995; Tai, 2009; Thompson and Spacapan, 1991), it may be more difficult for people with lower education and with severe mental illness, who often have a lower sense of control, to achieve this lifestyle behaviour change (Landau, 1995; Tai, 2009). Nevertheless, such a relationship should be tested in the future using a larger sample.
To conclude, MC may augment the effects of exercise interventions, as reflected by higher PA participation. MC has the potential to improve health outcomes in patients with prolonged DUP.
Supplemental Material
sj-docx-1-anp-10.1177_00048674211061496 – Supplemental material for Motivational coaching augmentation of exercise intervention for early psychotic disorders: A randomised controlled trial
Supplemental material, sj-docx-1-anp-10.1177_00048674211061496 for Motivational coaching augmentation of exercise intervention for early psychotic disorders: A randomised controlled trial by Yi Nam Suen, Lik Hang Lincoln Lo, Edwin Ho-Ming Lee, Christy Lai-Ming Hui, Sherry Kit Wa Chan, Wing Chung Chang and Eric Yu Hai Chen in Australian & New Zealand Journal of Psychiatry
Footnotes
Acknowledgements
We would like to thank the late Jenny for her considerable assistance in developing the motivational intervention that made this work possible. We would also like to thank all participants and collaborating partners, the Hong Kong Hospital Authority, Caritas Hong Kong, Hong Kong Federations of Women’s Centers, New Life Psychiatric Rehabilitation Association and Early Psychosis Foundation.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship and/or publication of this article: The study was funded by the Hong Kong Jockey Club Charities Trust (grant number 2017/0104).
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
