Abstract

Demand exceeds supply for hospital care
The Australian debate on the provision of inpatient care has progressed in recent years. Previously, policy makers considered Australia to have too many psychiatric beds, leading to a 2014 recommendation by the National Mental Health Commission (NMHC) that AUD$1 billion should be redirected from public hospitals to primary and community mental health services (Allison and Bastiampillai, 2015). This included major reallocations of $250 million in 2020–2021 and a further $300 million in 2021–2022, potentially reducing acute beds by 15%. However, the Australian Federal Government declined the NMHC’s 2014 recommendation to cut future funding for psychiatric beds. This is especially fortunate, as two subsequent major Australian Commissions have indicated that demand for acute hospital mental healthcare far exceeds supply.
Recent reports from the Productivity Commission into Mental Health (2020) and the State of Victoria, Royal Commission into Victoria’s Mental Health System (2021) reveal that public hospital mental health units are underfunded, and in disarray. Australia does not have too many beds – in fact the nation has considerably fewer beds than most other high-income countries (Allison and Bastiampillai, 2015). This is illustrated in Figure 1 which compares Australia and Victoria’s psychiatric beds per capita to countries in the Organisation for Economic Cooperation and Development (OECD). In 2014, the OECD reported specific concerns about Australia’s low numbers of psychiatric beds per capita, which risked worsening symptoms before patients could be admitted, and subsequently, the situation has only deteriorated, despite Australia’s large investment in primary care and community-based mental health services (Allison and Bastiampillai, 2015).
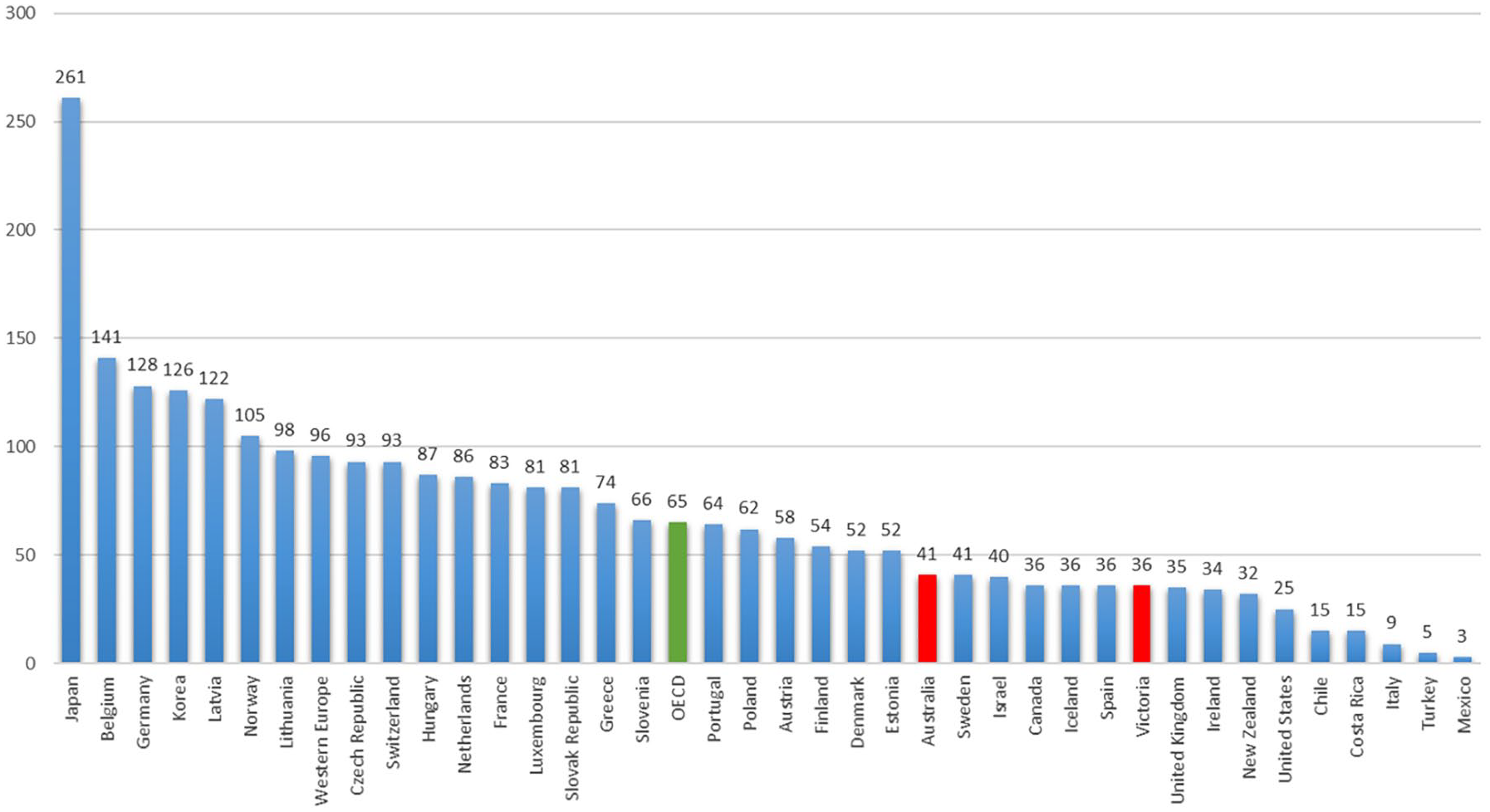
Comparison of psychiatric bed numbers in Organisation for Economic Co-operation and Development (OECD) countries.
In particular, there are long-standing concerns about Victoria’s psychiatric inpatient capacity to meet acute emergency department (ED) demand, particularly for the general adult population (aged 18–64). Victoria has by far the lowest public sector general adult bed numbers (acute and non-acute beds) of all the states, with 28% fewer general adult beds than the national average in 2018/2019 (23.1 beds vs 32.1 beds per 100,000 – the Australian national average: https://www.aihw.gov.au/reports/mental-health-services/mental-health-services-in-australia/report-contents/specialised-mental-health-care-facilities). The effects of Victoria’s low adult bed base are clear from key hospital metrics, including falling inpatient length of stay, with demand significantly exceeding the supply of beds.
The Victorian Royal Commission acknowledges that ready access to inpatient care is lacking in many regions of the state. Thus, the Commission’s interim report immediately targeted additional acute beds to the worst-affected regions, where the bed-building programme has been most significantly neglected despite Victoria’s high population growth. The final report recommended further acute beds across the system, and hopefully the number of these will be optimised by the new regional commissioning boards.
Community services and hospital avoidance
Both the National Productivity and Victorian Royal Commissions along with the NMHC expect that extra community services will significantly substitute for acute beds, thereby reducing pressure on public hospitals. However, this indirect approach is challenging to implement in already low-bedded countries like Australia, where only essential acute admissions occur. Moreover, in high-income countries, higher levels of community care are associated with greater hospital capacity, partly because better case-finding by community services reduces the treatment gap, bringing more people into mental health treatment systems (Allison et al., 2020).
Facing overwhelmed hospital services in England, associated with low and declining provision of hospital psychiatric beds (Figure 1), the Royal College of Psychiatrists (RCPsych) examined the evidence from recent systematic reviews as to whether additional community services might reduce hospital use (Wyatt et al., 2019). The RCPsych found that there was very little evidence that community services prevented or avoided acute hospital admissions. Accordingly, the RCPsych report specifically advocated for immediate additional acute psychiatric hospital beds in the highest priority areas (Wyatt et al., 2019). This report indicated that more than 1000 additional inpatient beds would be required to meet the recommended 85% bed occupancy rate target for underfunded regions.
In terms of the research evidence, early intervention services are known to modestly reduce acute hospital care among young people with psychosis, but only for the period of the enriched treatment, usually 2 years (Wyatt et al., 2019). However, many of the other formal structural components of the community mental healthcare system lack clear evidence for reducing hospital use. Community mental health teams, police liaison and diversion, crisis resolution home treatment teams, crisis houses and peer support are all of uncertain or weak efficacy in preventing hospitalisation. Furthermore, day hospitals and acute day treatment units are considered ineffective in reducing hospital use.
Australia’s real-world experience is consistent with these findings. Major population-adjusted increases in the supplies of primary and secondary mental health services, including enhanced general practice, higher antidepressant use, Medicare subsidised psychology services and state-based community mental health services (as shown in Table 1), have not prevented the increased demand on public hospital EDs and for inpatient hospital admissions, adjusted for population growth (see Table 2; AIHW: https://www.aihw.gov.au/reports/mental-health-services/mental-health-services-in-australia/report-contents/summary-of-mental-health-services-in-australia). Instead, there have been significant increases in acute emergency and hospital inpatient demand since 2007/2008. In addition, increased primary and secondary mental health services have not reduced Australia’s population rates of very high and high psychological distress levels (Table 2), while there has also been a 22% increase in age-standardised suicide rates (between 2007 and 2019).
Australian primary mental health, community mental health and antidepressant population coverage.
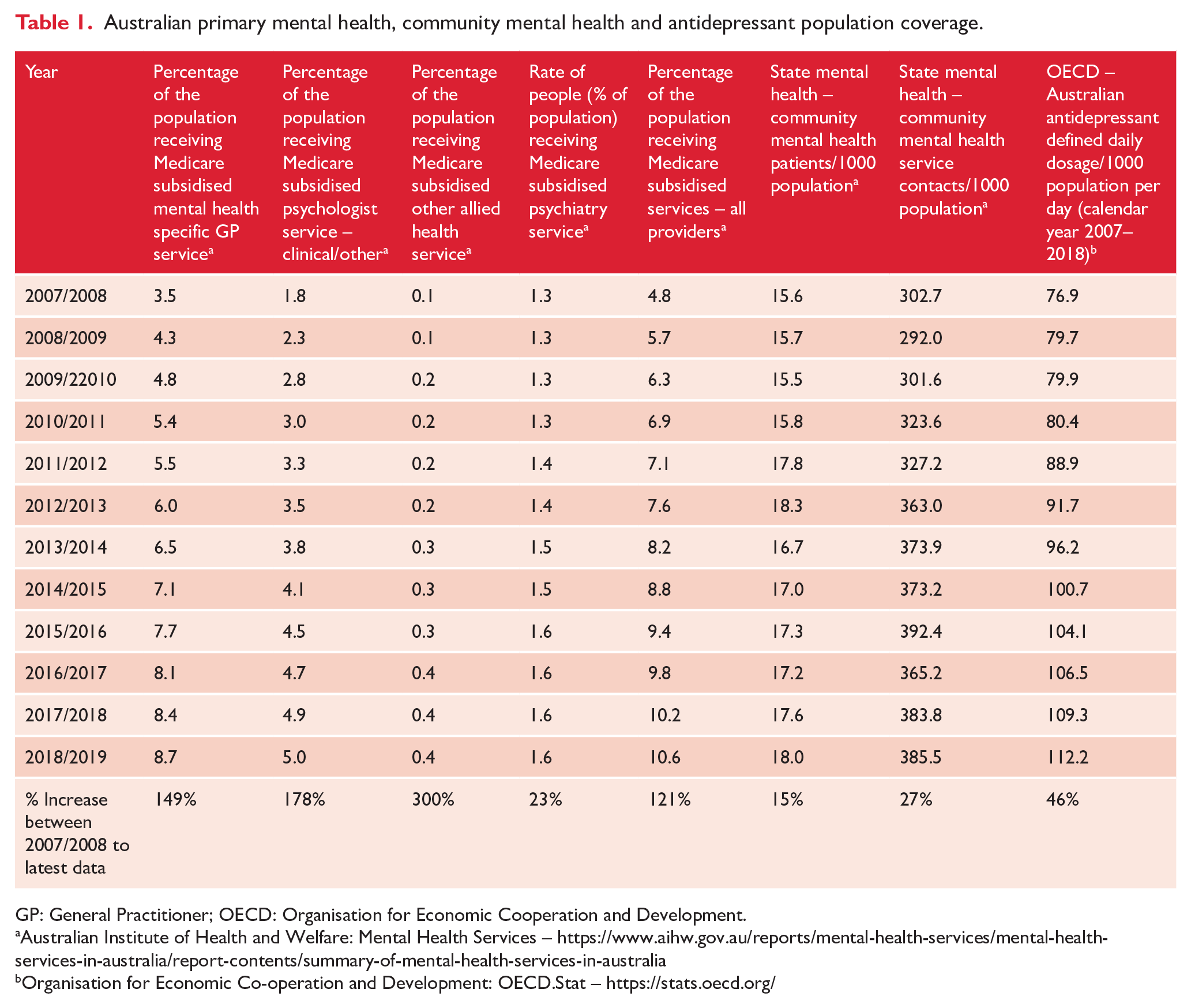
GP: General Practitioner; OECD: Organisation for Economic Cooperation and Development.
Australian Institute of Health and Welfare: Mental Health Services – https://www.aihw.gov.au/reports/mental-health-services/mental-health-services-in-australia/report-contents/summary-of-mental-health-services-in-australia
Organisation for Economic Co-operation and Development: OECD.Stat – https://stats.oecd.org/
Australian psychological distress levels, psychiatric hospitalisation use and suicide rates.
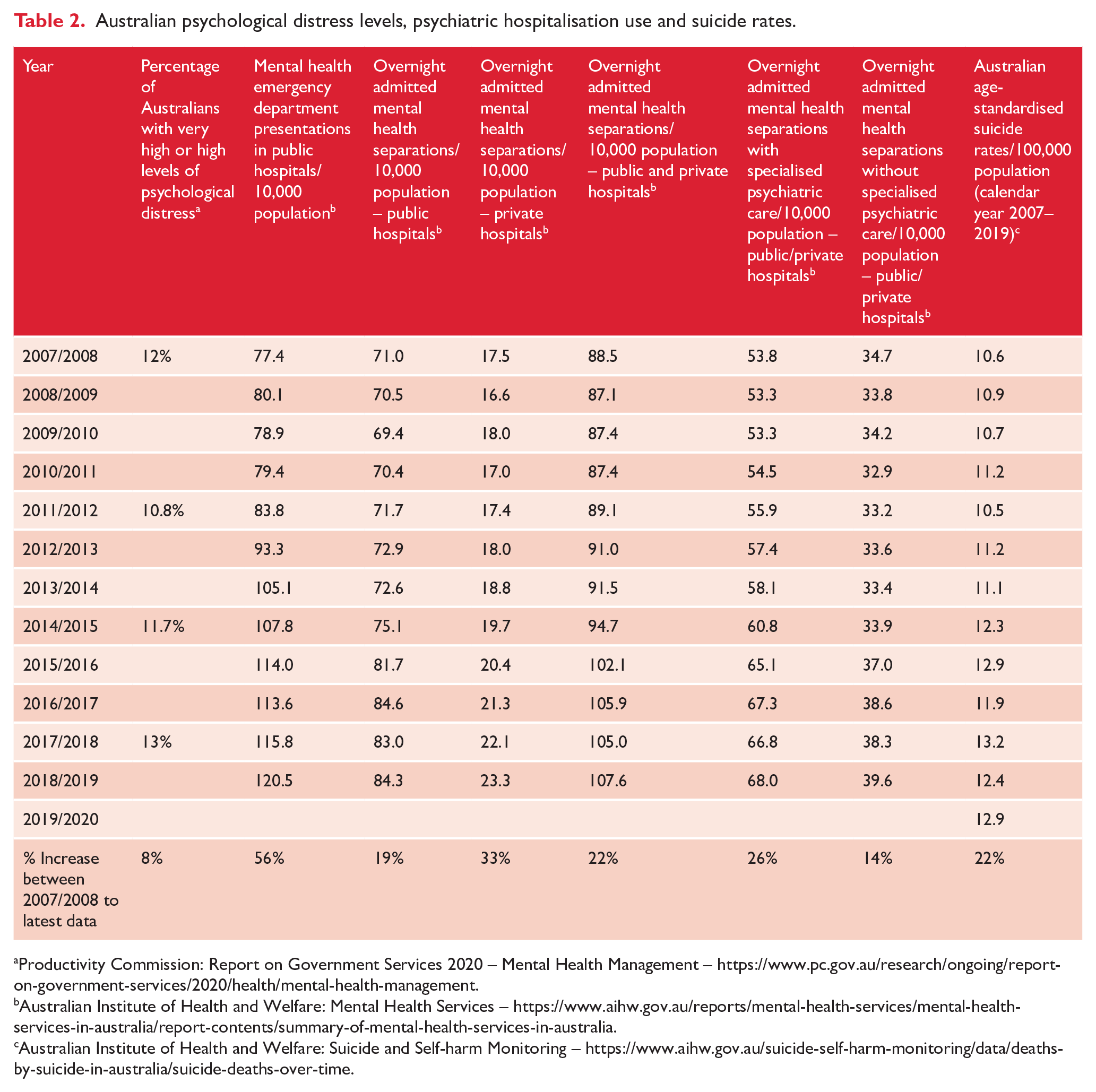
Productivity Commission: Report on Government Services 2020 – Mental Health Management – https://www.pc.gov.au/research/ongoing/report-on-government-services/2020/health/mental-health-management.
Australian Institute of Health and Welfare: Mental Health Services – https://www.aihw.gov.au/reports/mental-health-services/mental-health-services-in-australia/report-contents/summary-of-mental-health-services-in-australia.
Australian Institute of Health and Welfare: Suicide and Self-harm Monitoring – https://www.aihw.gov.au/suicide-self-harm-monitoring/data/deaths-by-suicide-in-australia/suicide-deaths-over-time.
There may be underlying secular and sociological factors contributing to increased population acuity and hospital presentations, including increased awareness of the appropriate role for (and a decreased stigmatisation of), seeking psychiatric care. For example, from 2007 to 2019, the percentage of the population with high and very high levels of psychological distress only increased by 8%, while ED mental health presentations increased by 56% (Table 2).
Demand continues to outstrip supply despite enhanced community care
The data trends presented in Tables 1 and 2 raise questions about whether further substantial increases in primary and secondary mental health services will reduce the acuity of mental illness in the population and thereby lower hospital demand. Hence, even if the recommendations of the Productivity Commission and Victorian Royal Commission were fully implemented, a community-care-centred approach, without sufficient complementary acute hospital beds, will likely prove ineffective (Allison et al., 2020). In fact, based on previous data over the last decade, increased community services might be associated with increased hospital use, rather than the reverse, related to a reduction in the treatment gap.
In conclusion, the Australian debate about the provision of acute inpatient care has progressed from the NMHC’s 2014 recommendation to cut funding for psychiatric beds to the Royal Commission’s (State of Victoria, 2021) acknowledgement that there are insufficient beds in many regions of Victoria. Given these findings, timely reporting of the relevant hospital key performance indicators at the regional level would be an important step in transparency and accountability, in relation to the deterioration of public hospital mental health services. Policy makers and regional planners need to monitor closely whether emergency presentations and psychiatric admission rates continue to increase and inpatient length of stay continue to fall. If so, effective measures should be urgently taken to improve the supply-side of public hospitals by commissioning more psychiatric beds. Finally, Australia requires a national standard for optimal hospital psychiatric beds per capita, and a mandatory maximum ED length of stay before admission, together with the commissioning of additional psychiatric beds across the nation, in order to meet these standards.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
