Abstract
Objective:
There is substantial research examining insight in psychotic disorders and in some nonpsychotic disorders. However, there has been little attention given to many nonpsychotic disorders. Research on insight in psychosis distinguishes between cognitive and clinical insight. In most studies examining insight in nonpsychotic disorders, definitions and assessments of insight vary significantly. The purpose of this review is to suggest a definition of insight in nonpsychotic disorders such that it can be used across different disorders.
Method:
We systematically review the extant literature of insight in nonpsychotic disorders and analyze the assessments used in order to determine how well they capture these two types of insight. Then, we discuss how these two constructs can provide better understanding of the phenomenology of insight in nonpsychotic disorders.
Results:
The systematic search resulted in 99 articles. These articles used 17 different methods of measuring insight, containing 127 questions. Results of the content analysis of items suggested that measures of insight used in nonpsychotic disorders do not distinguish between cognitive and clinical insight, but that most questions (90%) can indeed be reliably differentiated.
Conclusion:
We provide a multidimensional model of cognitive and clinical insight in nonpsychotic disorders, emphasizing the complexity of assessment and the importance of accurately defining insight. Such definitions have important theoretical and clinical implications, offering a better understanding of the concept of insight in nonpsychotic disorders.
Introduction
Researchers have studied insight extensively in the context of schizophrenia and bipolar disorders (see reviews by Latalova, 2012; Lysaker et al., 2018). In recent years, researchers have also explored insight in the context of nonpsychotic disorders such as obsessive-compulsive disorder (OCD; Ozkiris et al., 2015), body dysmorphic disorder (BDD; Phillips, 2004) and eating disorders (EDs; Konstantakopoulos et al., 2011). As a result, diagnostic criteria of these disorders have been modified to include insight specifiers (Leckman et al., 2010; Phillips et al., 2010, 2013). However, research on insight in other nonpsychotic disorders, including anxiety disorders and major depression disorder (MDD), is limited.
Researchers studying insight in nonpsychotic disorders frequently use different terms and assessment tools to describe and evaluate insight’s role, which can lead to confusion about its definition. Moreover, most literature on insight in nonpsychotic disorders has not attempted to distinguish or specify the different types of insight. To present a comprehensive definition of insight in nonpsychotic disorders, we propose a transdiagnostic model and systematically review the assessments and definitions used to describe and measure insight in studies to date in order to determine how well they capture these types.
Definition of insight
Schizophrenia and psychosis
Researchers often distinguish between two types of insight in schizophrenia: clinical insight and cognitive insight (e.g. Van Camp et al., 2017). Typically, clinical insight in schizophrenia is multidimensional and is viewed as a continuous construct (Amador et al., 1993; Baier et al., 1998; David, 1990; Ghaemi and Pope, 1994). The definition of clinical insight in psychosis includes commonly used dimensions relating to awareness of having symptoms, mental illness, necessity for treatment, efficacy of medication, consequences resulting from the mental illness and attribution of symptoms to a mental disorder (Amador and David, 2004; Amador et al., 1993; David, 1990; Reddy, 2015).
Whereas clinical insight focuses on the awareness of illness, cognitive insight is defined as individuals’ capacity to evaluate their thoughts by isolating themselves from cognitive distortions and considering different perspectives (Beck et al., 2004; Beck and Warman, 2004; Van Camp et al., 2017). Cognitive insight consists of two dimensions: self-reflectiveness and self-certainty. Good insight is characterized by high degree of self-reflectiveness (e.g. ability to acknowledge different points of view and assess alternatives to make a decision) and lack in self-certainty (e.g. conviction that beliefs are true; Beck et al., 2004). Similarly, it is important to distinguish between the belief and values to accurately assess insight. According to Veale (2002), the belief (e.g. fear of contamination in OCD) is typically related to the values (e.g. caring and protecting others), thus over-valued ideation suggests a fixity and overinvestment in one value at the expense of others.
Although clinical insight and cognitive insight are proposed as separate constructs, some studies suggest that they are fundamentally related and complementary (Buchy et al., 2010; Perivoliotis et al., 2010; Riggs et al., 2012). For example, Riggs et al. (2012) suggested that cognitive insight is a metacognitive skill that could contribute to the development of clinical insight. Similarly, Greenberger and Serper (2010) proposed that individuals who are more self-reflective are more likely to have clinical insight and that measures of cognitive insight and clinical insight also positively correlate with one another.
Nonpsychotic disorders
Different terms (e.g. poor insight,
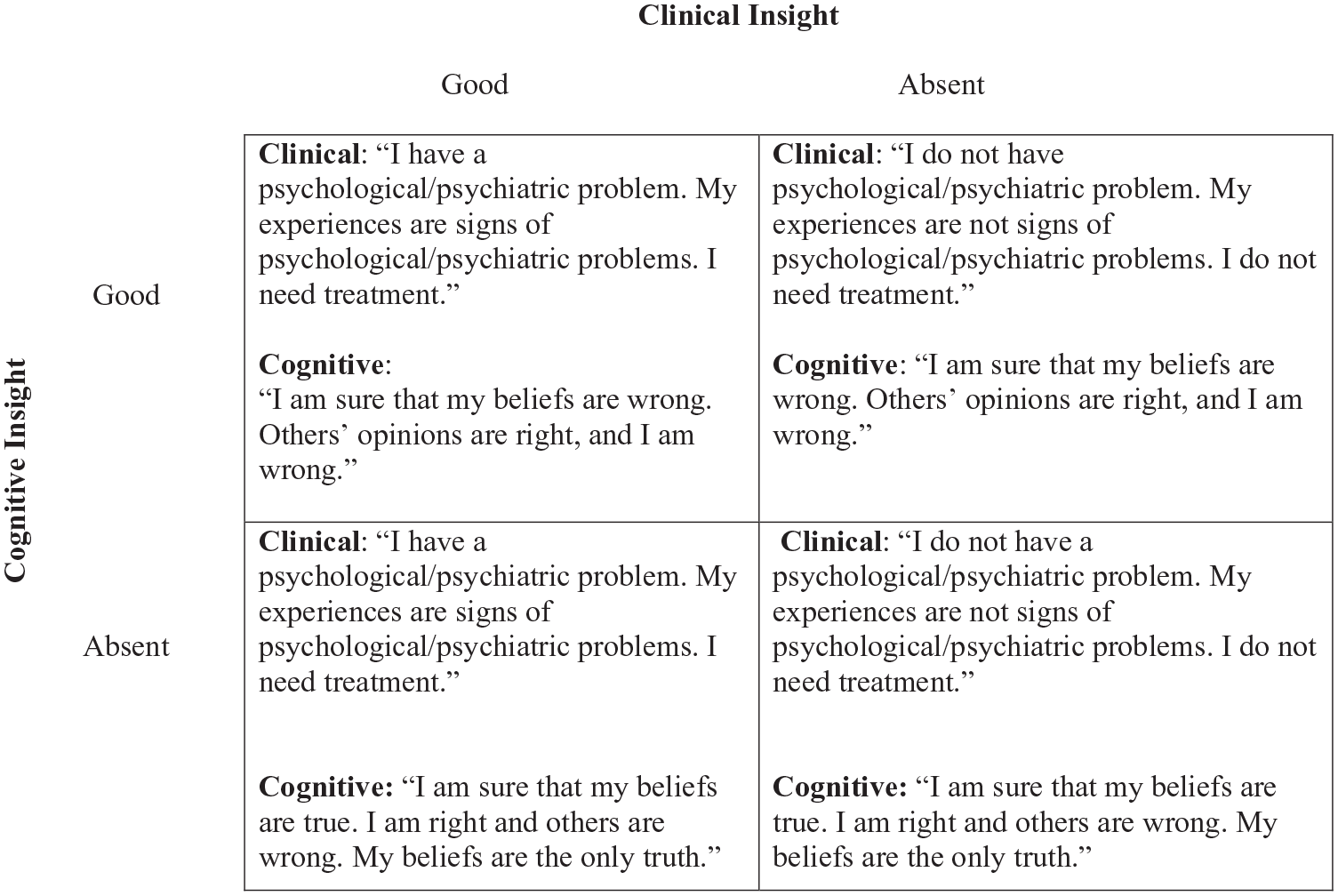

General model of insight in nonpsychotic disorders. The model presents two distinct types of insight (clinical; top of each box, and cognitive; bottom of each box). As both types of insight in the model are dimensional, this figure represents the extreme levels of each type of insight; either excellent or absent. The matrix results in four different subtypes of insight: (a) good clinical and good cognitive insight, (b) good clinical and absence of cognitive insight, (c) absence of clinical and good cognitive insight and (d) absence of clinical and absence of cognitive insight.
Cognitive insight in this model is based on Beck et al.’s (2004) definition; however, in our model, the definition is more specific by relating thoughts and behaviors to the experiences of the disorder as opposed to general experiences. Clinical insight in our model is based on the definition of clinical insight proposed by Amador et al. (1993) and David (1990; e.g. insight regarding symptoms, illness and the need for treatment); however, in our model, we refer to insight regarding psychological or psychiatric problems and not to having an illness. This is because we believe that the notion of mental illness is typically more related to having a diagnosis of psychosis or bipolar disorder. For example, an individual who suffers from social anxiety disorder might not believe that he or she suffers from a mental illness, but might acknowledge that they have a psychological issue and that that this problem requires treatment. Figure 2 provides a more detailed example of clinical and cognitive insight in OCD,
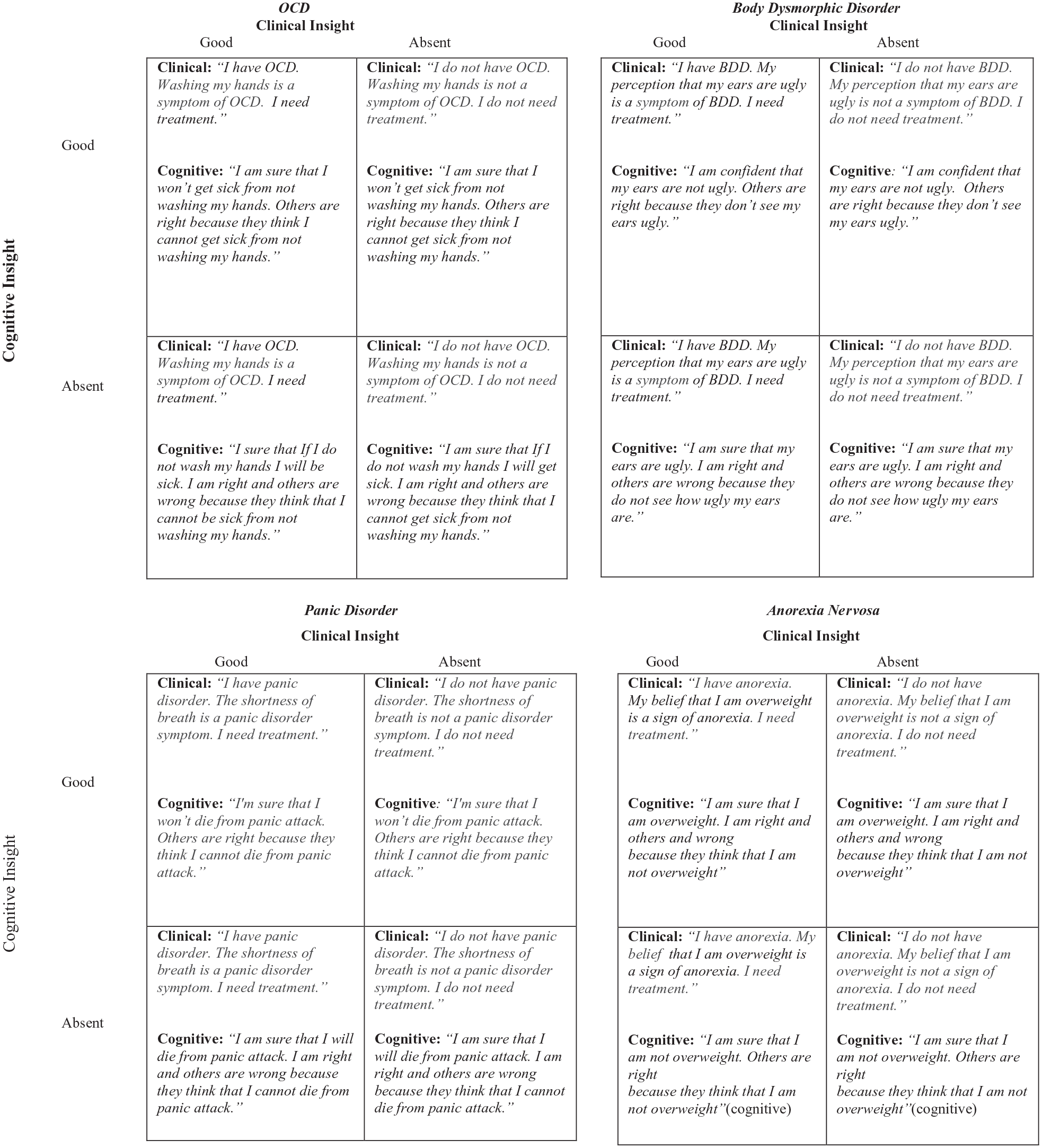
Insight in OCD, BDD, panic disorder and anorexia nervosa. Proposed model of insight in nonpsychotic disorders. Insight includes two constructs: (a) clinical insight and (b) cognitive insight, and each construct is on a continuum from good to poor to absent. The examples represent the extremes of either good or absent clinical or cognitive insight in various disorders. Clinical insight refers to awareness regarding psychological or psychiatric problems and the need for treatment, and cognitive insight refers to certainty and reflectiveness regarding thoughts and behaviors related to the experiences of the disorder.
Accurately assessing insight and distinguishing between cognitive vs clinical insight has a number of important clinical and research implications. From a research standpoint, in order to understand the variables associated with insight, it is essential to have clear definitions and make distinction to determine factors that are related to each construct of insight. For example, factors that are related to acknowledging or denying having psychological problem (e.g. stigma) may be very different than factors that are related to maintaining basic beliefs (e.g. cognitive inflexibility). Furthermore, it is possible that one type of insight is more predictive of outcomes than another, and without clear definitions, operationalization and measurement of the distinct constructs, the ability to determine correlates of each construct as well as impact of such constructs on outcomes will be impeded.
Clinically, having a clear definition of these concepts can impact treatment seeking, assessment and outcomes. Specifically, good clinical insight can impact a patient’s motivation to seek treatment and need for change. Assessing clinical insight before treatment might be especially important for patients with poor clinical insight. Those patients can benefit from motivational intervention before treatment to gain from treatment. Cognitive insight may impact case conceptualization and become a specific target in treatment, via cognitive restructuring or other methods of cognitive change in cognitive behavioral therapy (CBT). Importantly, these are empirical, testable questions that can lead to better clinical decision making via more person-centered, tailored interventions. Degree of clinical and cognitive insight can vary from one patient to another, and they can each have potential clinical impact on assessment and treatments.
Poor clinical insight might be less prevalent in anxiety, mood and related disorders, as distress is central to these disorders. There is also less stigma to having a mood or anxiety disorder in comparison with psychotic disorders. On the contrary, given that many of the experiences in mood and anxiety disorders are on a continuum, individuals may be more likely to consider their symptoms as normative even when they have become excessive or clinically significant. Cognitive insight, however, may vary greatly, with some significant proportion of people with anxiety or mood disorders exhibiting poor cognitive insight. Individuals with a mood or anxiety disorder can be very convinced that their beliefs or fears are accurate, that their internal/emotional experiences reflect a truth that others cannot know and that there is little reason to consider alternatives.
The purpose of this review is to suggest a definition of insight in nonpsychotic disorders (OCD, BDD, EDs, anxiety disorders, hoarding disorder [HD] and MDD) such that it can be used across different disorders. To this end, we systematically identified the assessments (interviewer-administered and self-report) used to measure and describe insight, and analyzed the content of the assessments to determine what dimensions of insight they relate to. By determining a definition of insight, we intend for researchers to clearly identify the types of insight they intend to measure as well as to aid clinicians in determining which types of insight to address in assessment and treatment.
Method
Literature search
We followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) for reporting our systematic review (Moher et al., 2009). We used PubMed and PyschINFO to systematically search for articles reporting insight measures in samples with OCD, BDD, EDs, anxiety disorders, HD and MDD. We used multiple terms associated with insight to search these databases, including ‘poor insight’, ‘cognitive insight’, ‘clinical insight’, ‘overvalued ideation’, ‘fixity of beliefs’, ‘delusional thinking/beliefs’, ‘conviction’, ‘impaired insight’, ‘lack of insight’, ‘awareness’, ‘illness denial’ and others. We combined these terms with those related to diagnoses or disorders (e.g. ‘OCD’, ‘OC*’, ‘GAD’, ‘panic disorder’, ‘anxiety symptoms’, ‘anxiety’, ‘agoraphobia’, ‘PTSD’, ‘social anxiety’, ‘phob*’, ‘BDD’, ‘dysmorphobia’, ‘body image disorder’, ‘anorexia nervosa’, ‘bulimia nervosa’, ‘body image’, ‘eating disorder’, ‘depression’, ‘depress*’, ‘hoarding behavior’, ‘hoarding compulsions’ and others) and with terms related to insight assessments, including ‘insight assessment’, ‘Brown Assessment of Beliefs Scale’, ‘Beck Cognitive Insight Scale’, ‘Overvalued Ideas Scale’, ‘Fixity of Beliefs Questionnaire’, ‘item 11 of Y-BOCS’, ‘DSM insight’, ‘Scale to Assess Unawareness of Mental Disorders’, ‘The Schedule for the Assessment of Insight’ and others. Studies included in this review had to meet the following criteria: (a) they had to be published in a peer-reviewed journal after 1987; (b) they had to be published in the English language; (c) they had to have a sample diagnosed with a
Literature selection
Selecting articles to review included multiple steps. We first searched abstracts in PubMed and PyschINFO, in addition to seeking out other articles using additional online sources and references of included articles. Thereafter, collected articles were imported into a reference database manager. We then uploaded the references to Endnote X8.2 and removed duplicates. Then, we removed irrelevant articles based on their titles and screened the abstracts of the remaining articles for inclusion criteria. The primary author downloaded and reviewed the full text of potentially eligible articles. A second reviewer independently checked 50 articles randomly selected from the 183 full texts for reliability and to ensure that only relevant articles were included. Once the final articles were identified, the first author extracted each item of each of the assessments used in order to examine the content and categorize it according to thematic dimensions and larger potential constructs.
Results
The initial search resulted in 11,549 articles, and after removing duplicates, 4378 remained. Screening of titles determined that 3878 articles were irrelevant and 505 articles were included. Out of the 505 articles, 322 were excluded after reviewing abstracts (see Figure 3 for reasons). The final 183 full articles were examined and from those 84 articles were excluded, and 99 relevant articles were included. A PRISMA flow chart (Moher et al., 2009) of the study selection is represented in Figure 3. The articles that were included in the review are listed in Supplemental Appendix 1.
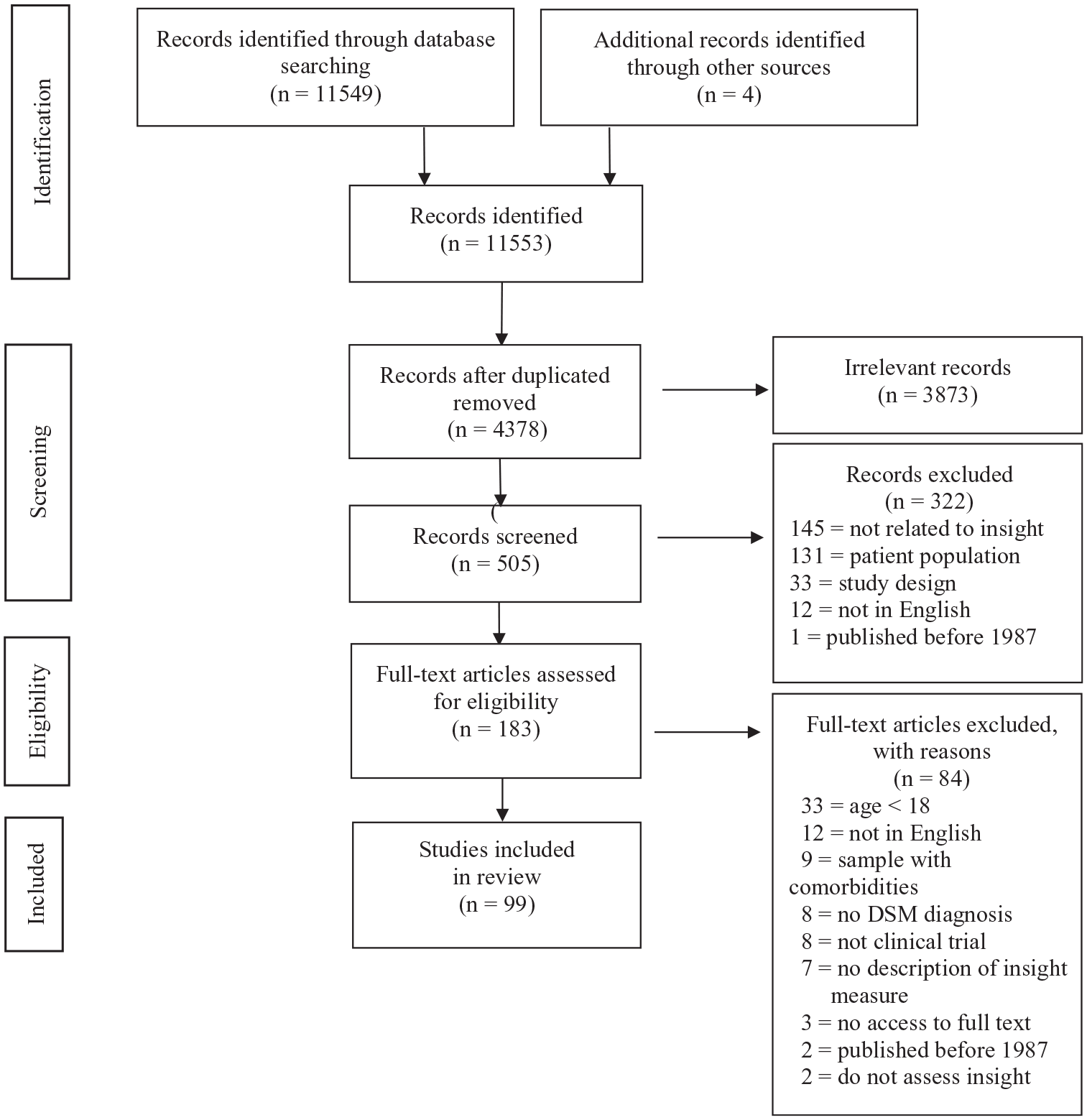
PRISMA flow diagram of studies included in the systematic review.
The systematic review revealed 17 different measures used to assess insight in nonpsychotic disorder samples. Overall, studies examined OCD in 69 studies, BDD in 20 studies, MDD in 8, EDs (anorexia and bulimia) in 5 studies, mixed anxiety in 1 study and Social Anxiety Disorder (SAD) in 1 study. Table 1 provides details about each measure and the number of studies in which it was used. The results suggest that the common insight measures used to examine insight in nonpsychotic disorders are the Brown Assessments of Beliefs Scale (BABS, Eisen et al., 1998), item 11 of the Yale-Brown Obsessive Compulsive Scale (Y-BOCS; Goodman et al., 1989), the Over-Valued Ideas Scale (OVIS; Neziroglu et al., 1999) and the DSM-IV insight criteria (APA, 2000). The results also reveal that some studies (9 out of 99) used measures of insight developed for psychosis, including the Beck Cognitive Insight Scale (BCIS; Beck et al., 2004), the Scale for assessing Unawareness of Mental Disorder (SUMD; Amador et al., 1993), the Schedule for Assessment of Insight (SAI; Kemp and David, 1997) and the Insight Scale (IS; Birchwood et al., 1994) (see Table 1).
Summary of the systematic review of insight measures and analyses of types of insight in nonpsychotic disorders.
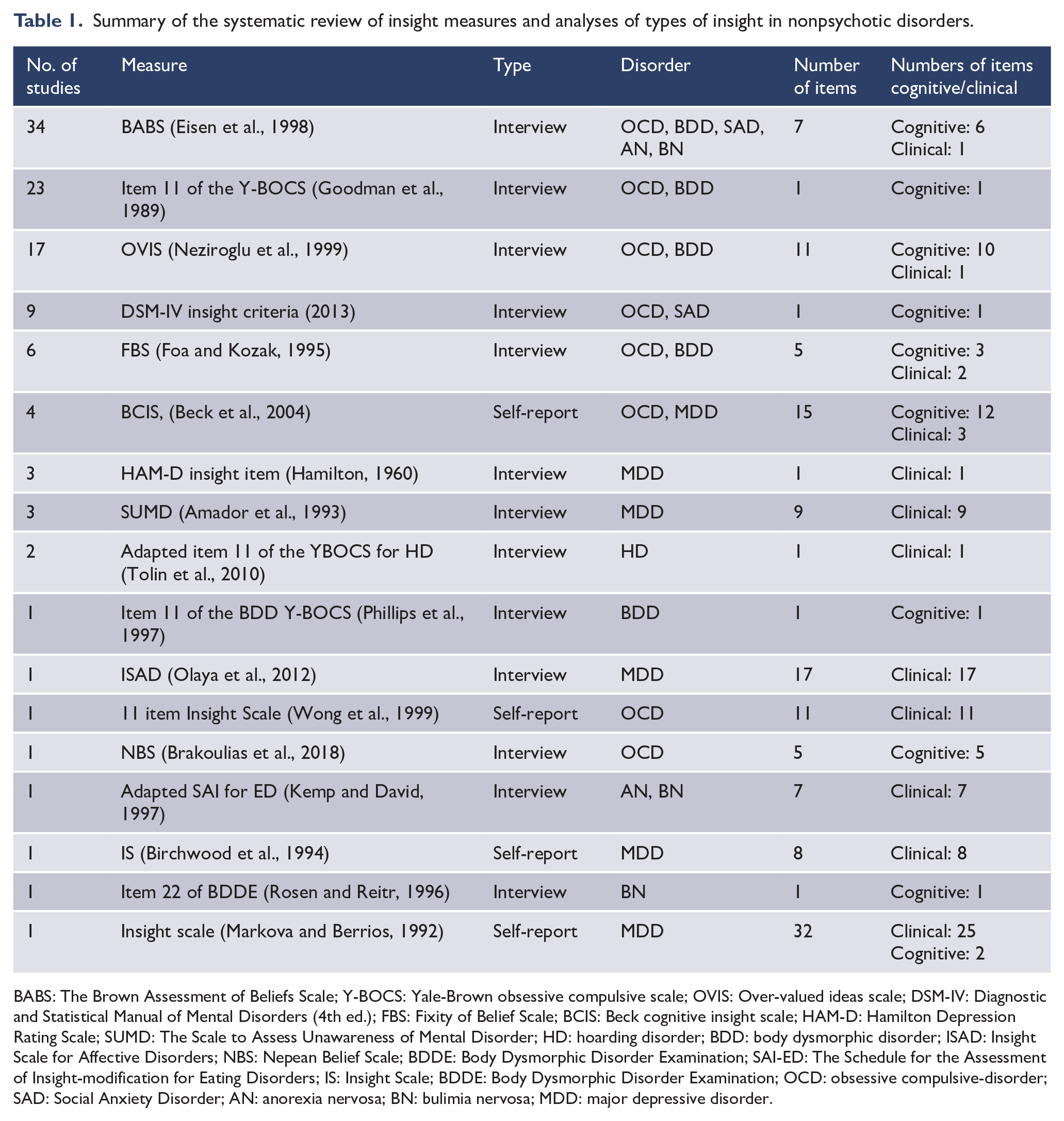
BABS: The Brown Assessment of Beliefs Scale; Y-BOCS: Yale-Brown obsessive compulsive scale; OVIS: Over-valued ideas scale; DSM-IV: Diagnostic and Statistical Manual of Mental Disorders (4th ed.); FBS: Fixity of Belief Scale; BCIS: Beck cognitive insight scale; HAM-D: Hamilton Depression Rating Scale; SUMD: The Scale to Assess Unawareness of Mental Disorder; HD: hoarding disorder; BDD: body dysmorphic disorder; ISAD: Insight Scale for Affective Disorders; NBS: Nepean Belief Scale; BDDE: Body Dysmorphic Disorder Examination; SAI-ED: The Schedule for the Assessment of Insight-modification for Eating Disorders; IS: Insight Scale; BDDE: Body Dysmorphic Disorder Examination; OCD: obsessive compulsive-disorder; SAD: Social Anxiety Disorder; AN: anorexia nervosa; BN: bulimia nervosa; MDD: major depressive disorder.
To better define the concept of insight in nonpsychotic disorders and provide a more comprehensive definition, we analyzed the content of each individual item of the 17 measures to extract the types of insight each captures. We determined whether questions were related to clinical insight based on the definitions described in the literature on psychosis (Amador and David, 2004; Amador et al., 1993; David, 1990; Reddy, 2015) or cognitive insight (Beck et al., 2004). We categorized all items except for items 15, 19, 20, and 27–29 on the Insight Scale (Markova and Berrios, 1992). These items relate to psychotic experiences regarding thought control and hallucinations that are unlikely to be related to insight in nonpsychotic disorders. Consequently, we decided not to include these items in our analysis.
Table 1 also describes for which disorders each measure has been used to assess insight and summarizes the type of insight it captures based on the numbers of items. Eleven individuals (3 OCD experts, 7 PhD students and 1 BA student) categorized each item of the 17 measures to clinical or cognitive insight. An inter-rater reliability (IRR) analysis was performed to determine whether the items could be categorized reliably into clinical or cognitive insight. The marginal distributions of ratings did not indicate prevalence or bias problems, suggesting that Cohen’s (1960) kappa was an appropriate index of IRR (Di Eugenio and Glass, 2004). Kappa was computed for each coder pair and then averaged to provide a single index of IRR (Light, 1971). The resulting overall kappa indicated overall moderate agreement, κ = 0.43 (Landis and Koch, 1977), κ = 0.47 for clinical and κ = 0.55 for cognitive insight. Reliability per item ranged from κ = 0.20 to 1.0, with the majority of the items having moderate or better reliability (114 items with κ ⩾ 0.40). In other words, raters agreed on whether the items were or were not cognitive or clinical in nature 87% of the time: 86% for clinical insight and 88% for cognitive insight. Of the 127 questions, there was moderate to excellent agreement on 114 of the questions (90%). The IRR analysis suggested that coders had moderate to excellent agreement, which indicates that it is possible to categorize the items into two constructs of insight: clinical and cognitive.
In addition to looking at the overall IRR of all items, we also looked at the items that had a low agreement, k < 0.40, to understand why the coders had difficulty agreeing on the construct of insight the question captures. There were 13 items (10%) that had poor IRR. When examining these items more closely, we determined a number of factors that may attribute to the complication in categorizing these items as clinical vs cognitive insight.
First, the coders had difficulty categorizing the items that included the word ‘experiences’ or ‘problem’, (
Second, some items (
Third, some questions appeared to be more complicated to categorize. The items (
Thus, we can conclude that most of the items (90%) measure either cognitive or clinical insight in a differentiable fashion, which supports our proposed model and the distinction between clinical and cognitive insight. However, categorizing some items on existing measures is complicated. It is therefore important to consider our points when using existing measures and write items clearly without confusing the constructs when developing a new measure of insight.
Discussion
Insight has been the topic of extensive research in the area of psychosis, with many researchers and clinicians determining that there are two main types of insight: clinical and cognitive insight. This distinction, while not without controversy (see below), has helped direct research into the phenomenology, psychopathology and treatment implications of insight in psychosis. However, much less research has been conducted on insight in nonpsychotic disorders. Indeed, in our systematic review of empirical studies examining insight nonpsychotic disorders, we found that 89% of studies examining insight in examined OCD or BDD, whereas only one study examined SAD, and one examined insight in other anxiety and related disorders such as panic disorder, agoraphobia, generalized anxiety disorder or PTSD. The large majority of these studies did not systematically distinguish between cognitive and clinical insight and used assessment measures that mixed cognitive and clinical insight. Nevertheless, our evaluation from the raters found that all could reliably differentiate these two constructs. These results suggest the need for development of clear measure of cognitive and clinical insight, and a clear framework for considering insight in nonpsychotic disorders.
Our analysis suggests that most of the assessments reflected various dimensions of insight relating to clinical (awareness of mental illness, symptoms, need for treatment) or cognitive (self-reflectiveness and self-certainty) insight. Supplemental Appendix 2 includes a detailed table of each measure and types and dimensions of insight each item captures. Additionally, during this analysis, we determined that several items (e.g. item 11 of Y-BOCS, DSM-IV insight criteria, item 2 of the OVIS, item 5 of NBS, item 4 of the 11 item insight scale and item 7 of the SAI for ED) did not reflect the dimensions as defined in the literature. Therefore, we propose two new dimensions, one for cognitive insight (rationality of belief) and one for clinical insight (emotional awareness of having a psychological/psychiatric problem). Rationality of belief refers to the meta-awareness of the internal logic of the belief. We contend that beliefs fall within the realm of cognitive insight, somewhere between self-reflectiveness and self-certainty.
Emotional awareness of psychological/psychiatric problems refers to the emotional reaction or expression of emotion when thinking about or being aware of having psychological/ psychiatric problems (and therefore a form of clinical insight). The focus in this dimension is on the way people ‘feel’ about their problem/experiences and not what they ‘think’ about their problem/experiences; in BDD, ‘I am sad when I think that my ears are ugly’.
In order to provide a comprehensive definition of insight, including the dimensions, we propose a more detailed model that presents the types of insight and their dimensions based on the analyses of the scales’ items. This transdiagnostic model is based on factor analytic studies and reviews of measures of insight in schizophrenia (e.g. Konsztowicz et al., 2018; Lincoln et al., 2007), with additional changes to make the model relevant to nonpsychotic disorders. The model presents the two types of insight (clinical and cognitive) as distinct, though each type has various dimensions that may overlap. Clinical insight is proposed to have three dimensions: (a) intellectual awareness of psychological/psychiatric problems and their consequences; (b) emotional awareness of psychological/psychiatric problems and their consequences; and (c) awareness of the need for psychological/psychiatric treatment (evidence-based and/or commonly recommended by psychiatrists or psychologists). In contrast with the suggestion of Konsztowicz et al. (2018), we believe that individuals with nonpsychotic disorders can be aware of their experiences but can lack insight regarding the need for treatment. Cognitive insight is proposed to have three main dimensions: (a) self-reflectiveness, (b) self-certainty and (c) rationality of belief (a meta-awareness of the belief’s internal logic).
In this model, we suggest that both types of insight are on a spectrum, which means they can range from excellent to poor to absent. For example, an individual with excellent insight might have awareness of all dimensions of clinical insight and cognitive insight, whereas an individual who lacks insight entirely might not have any awareness regarding any of the dimensions. Furthermore, individuals with poor insight may have awareness of certain dimensions of clinical insight and/or cognitive insight, while lacking insight in additional dimensions. Importantly, there are different dimensions in the model relating to various aspects of psychopathology that can exist and vary from one individual to another or within an individual over time. The combination of the dimensions can result in a picture of mixed insight; therefore, it is important to evaluate insight based on multiple dimensions.
Complexity of assessing insight and its multiple dimensions
Although we attempted to theoretically and systematically distinguish among the different domains of the scales mentioned in the literature, it is worth noting the complexities in making this distinction. Considering that not all patients believe they have illness, understanding patients’ perceptions or thoughts regarding their symptoms is complex. Unlike physical disease, mental illness does not exhibit symptoms that enable completely objective identification and treatment. Ever since Szasz (1960), some have suggested that mental disorders are partially (e.g. Wakefield, 1992) or completely (e.g. Dowbiggin, 2009) socially constructed. For example, Dowbiggin (2009) suggested that social anxiety is a socially accepted response to social stresses and that society sets rules to determine whether anxiety is normalized. Although extreme views are in the minority, most professionals acknowledge the psychological and social construction of mental illness. Ultimately, the lack of objective, observable criteria for most mental illness requires the clinician to label with care. This is true of diagnostic labels including insight. In order to assess insight accurately, it is important to evaluate what the social, cultural and personal factors are that contribute to the perception of one’s experiences and how they impact the conceptualization of disorder vs nondisorder. It is important to consider one’s professional opinion as well as the opinion of the patient. Therefore, using self-report measures and multidimensional structured interviews can help to assess insight more accurately.
In terms of cognitive insight, cultural factors can affect how one defines or relates to cognitive insight. Studies indicate differences in the factor structure of BCIS between Asian cultures and Western societies (Jacob et al., 2019), suggesting that this difference could be linked to the difference in cultural elements that can impact cognitive insight. This likely leads to different results regarding patient’s cognitive insight depending on their culture, which complicates the measurement of cognitive insight.
Furthermore, assessing insight accurately requires a clear definition of insight and its dimensions. Various questions can be asked to determine the level of insight within a dimension and wording the questions based on the dimension one is attempting to assess is important. For example, many patients might ‘feel’ that their belief is true, even though they ‘know’ or ‘think’ it is not. This idea is related to the concept of rational-emotional dissociation (RED; Stott, 2007) which refers to a dissociation between beliefs and emotions. In other words, holding a rational belief but feeling the opposite about it, where both ideas are held with total conviction. Whereas there are some items related to the RED in measures of clinical insight, measures of cognitive insight to date do not include such a distinction, more work is needed to further examine this in future research. It is important to point out that RED is not the same as the proposed emotional awareness dimension. Emotional awareness refers to the emotional reaction or expression of emotion when thinking about or being aware of having a problem (e.g. ‘I am concerned that I do not go out of the house because I am afraid of seeing a dog’) and RED refers to an aspect more related to cognitive insight: the feeling that the rational belief is true despite knowing it is not (e.g. ‘I feel that the dog will bite me’).
In addition, we suggest that the belief may fluctuate with anxiety/mood and may not necessarily be an indication of poor cognitive insight. For example, assessing the self-certainty dimension during an interview is different than assessing it during a panic attack; insight decreases in the peak of an emotional experiences. Therefore, it is crucially important to consider the context of belief when assessing insight. Such experiences and their relationship to overall insight and treatment outcome should be studied.
The different terms used in the literature of nonpsychotic disorders often reflect similar constructs that could make their use redundant or require further specification to make their differentiation clearer. For example, in the case of conviction and fixity of beliefs, we believe that conviction is similar to high self-certainty and fixity is similar to low self-reflectiveness within the dimensions of cognitive insight proposed by Beck et al. (2004).
The complexity of the dimensions themselves can add to the complications of measuring insight. For example, distinguishing between awareness of the need for treatment and willingness to seek treatment is important. Patients may be aware that they are having problems and may think they need treatment, but they may be unwilling to seek or engage in treatment for economic (e.g. inability to afford treatment), personal (e.g. concerns about side effects), religious (misattributing religious symptoms of OCD to religiosity or panic attacks to demons), cultural (negative stereotypes and stigmatization; Belvederi Murri and Amore, 2019) or other reasons. This does not necessarily mean that the patient lacks insight about the need for treatment.
It is important for researchers to be clear about what dimension of insight they are attempting to measure especially when wording the insight questions. For example, based on our content analysis, item 11 of the Y-BOCS and the adapted versions for BDD and HD (Phillips et al., 1997; Tolin et al., 2010) did not appear to capture the same dimensions. Therefore, it is important for researchers to be clear about what dimension they are attempting to measure.
Limitations
It is important to point out that our content analysis of insight measures was qualitative/theoretical and not empirical. We believe this is an important first step, which organizes the existing measures and literature. Future research should focus on empirical studies using factor analysis in order to create a comprehensive measure of insight. Furthermore, it would be useful to survey experienced clinicians to determine if there are other dimensions of insight that are not captured in the current review.
Conclusion
Based on our systematic review and content analysis, we conclude that there is a dearth of research on insight in nonpsychotic disorders. Hardly any studies have attempted to examine insight in adults with EDs, anxiety disorders and other nonpsychotic disorders. However, it is likely that insight varies within all disorders and should be considered for both research and clinical purposes. Furthermore, the existing studies of insight in nonpsychotic disorders do not reflect a comprehensive assessment to distinguish between types and dimensions of insight. Therefore, we suggest that using multiple measures is important to capture types and multiple dimensions, and we further advocate for the development of new insight tools that capture both concepts of cognitive and clinical insight with the aim of obtaining a better understanding of the concept among patients with nonpsychotic disorders. In attempting to better define the concept of insight in nonpsychotic disorders, we propose a new, transdiagnostic model of insight to analyze the relationships among the two types of insight and their different dimensions. Indeed, we suggest that constructs of cognitive and clinical insight can be applied across nonpsychotic disorders, even though this has not typically been done to date. Thus, future research is necessary to better understand cognitive and clinical insight and to identify their role in the phenomenology, etiology, prognosis and treatment outcomes in nonpsychotic disorders.
Supplemental Material
sj-docx-1-anp-10.1177_00048674211025722 – Supplemental material for Insight in nonpsychotic disorders: A new model of insight and a systematic review of measures
Supplemental material, sj-docx-1-anp-10.1177_00048674211025722 for Insight in nonpsychotic disorders: A new model of insight and a systematic review of measures by Asala Halaj and Jonathan D Huppert in Australian & New Zealand Journal of Psychiatry
Supplemental Material
sj-docx-2-anp-10.1177_00048674211025722 – Supplemental material for Insight in nonpsychotic disorders: A new model of insight and a systematic review of measures
Supplemental material, sj-docx-2-anp-10.1177_00048674211025722 for Insight in nonpsychotic disorders: A new model of insight and a systematic review of measures by Asala Halaj and Jonathan D Huppert in Australian & New Zealand Journal of Psychiatry
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
